That bridge is looking quite appealing
1/236
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
237 Terms
What do T cells recognize when bound to a MHC protein?
Antigens
What type of protein do antigens bind to on the plasma membrane of cells that allow for T cells to recognize them?
Glycoproteins
What does MHC stand for?
major histocompatibility complex
What are the glycoproteins on the surface of plasma membranes produced by?
major histocompatibility complex (MHC) gene
Are the MHC proteins unique to each individual?
Yes; except for identical twins
What do MHC proteins bind to on the plasma membrane of body cells?
Antigens
What are the two major Classes of MHC proteins?
Class 1 MHC proteins & Class 2 MHC proteins
Where are Class 1 MHC proteins found?
The plasma membrane of all nucleated cells
Where are Class 1 MHC proteins not found?
Red blood cells
What is an antigen presenting cell?
They engulfing pathogens, digesting them into small peptides, and displaying these antigens on their surface via class 2 MHC proteins to activate T-lymphocytes
Where are class 2 MHC proteins found?
The plasma membrane of Antigen presenting cells (Dendrites, macrophages, B cells) and lymphocytes
What are the two main types of macrophages?
Fixed and floating
What are examples of structures that house antigen presenting cells?
lymph nodes and spleen
What determines what type of MHC protein a T cell can bind to?
Cluster of differentiation (CD) markers
What are the two Cluster of Differentiation (CD) Markers?
CD8 markers & CD4 markers
Where are CD8 markers found?
On Cytotoxic T cells and regulatory T cells
What type of MCH protein do CD8 markers respond to?
Class 1 MCH markers
What cells are CD4 markers found?
Helper T cells
What type of MHC protein do CD4 markers respond to?
Class 2 MHC proteins
What happens when T cells become activated by the MHC protein with an antigen they recognize?
They undergo mitosis producing identical clone cells
What are the types of T cells that have CD8 markers that are activated by class 1 MHC proteins and react quickly?
Cytotoxic T cells, and Memory T cells
What are the types of T cells that have CD8 markers that are activated by class 1 MHC proteins and react slowly?
Regulatory T cells
What do cytotoxic T cells attack and destroy?
Infected and abnormal cells displaying antigens
What type of T cells are highly mobile cells that roam throughout injured tissues?
Cytotoxic T cells
What are the three ways that Cytotoxic T cells attack and destroy infected and abnormal cells displaying antigen?
Perforins, cytokines, and lymphotoxin
What happens when cytotoxic T Cells release perforins?
forms pores on the plasma membrane of target cell
What happens when cytotoxic T Cells release cytokines?
activate genes for apoptosis (programed cell death)
What happens when cytotoxic T Cells release lymphotoxin?
Kills target cell
During the first exposure to an antigen how long is the response from a cytotoxic T Cell?
It takes a significant amount of time, 2 days to reach sufficient levels.
What is produced when T cells with CD8 markers are activated?
Memory T cells
What happens when a Memory T cell is re-exposed to an antigen?
They differentiate into cytotoxic T cells and produce a rapid and effective response
How do regulatory T cells moderate the response of other T cells and B cells?
By secreting inhibitory cytokines called suppression factors
What are cytokines?
signaling proteins released by immune cells
Why does the response of regulatory T cells take longer than the response of Cytotoxic T cells
Because they take longer to activate and their are fewer that are activated.
What do activated CD4 T Cells produce?
Active Helper T cells & Memory Helper T cells
What do the cytokines secreted by activated helper T cells do?
stimulate cell-mediated and antibody mediated immunity
(☆ ask slide 15 vs 16) What do the Cytokines of inactive Helper T cells do?
Promote Activation of B cells
Attract and stimulate Cytotoxic T Cells
Attracts and stimulates macrophages
Stimulates T cell division that produce memory T cells
Speeds up the maturation of Cytotoxic T cells
How many different populations of B cells does the human body contain?
Millions
What do B cells carry?
thousands of unique antibody molecules bound to its plasma membrane
What happens to an antigen when its in the presents of its antibody on the plasma membrane of a B cell?
Binds to the B cell
How does a B cell become sensitized?
1) The inactive B cell has antigens attach to it’s antibodies
2) The antigens are brought into the B cell through endocytosis
3) The antigen binds to the Class 2 MHC protein and goes to the cell membrane.
4) A helper T cell can now activate it
What has to happen for a Helper T cell to activate a B cell?
The B cell has to be sensitized
How does a Helper T cell activate the sensitized B cell?
Helper T cells bind to the B cells class 2 MHC protein then secretes cytokines that promote B cell activation
What’s produced by an activated B cell?
Plasma and memory B cells
What does the activated B cell do to create plasma and memory B cells?
It divides several times producing daughter cells that differentiate into plasma cells and memory B cells
What do plasma cells do?
Plasma cells synthesize and secrete large quantities of antibodies
Which antigens can the antibodies produced by the plasma cells recognize?
same antigens as the antibodies on the plasma membrane of the activated B cell
How many antibodies can a plasma cell secrete hourly?
100 million antibody molecules
When is inflammation triggered?
From physical trauma, intense heat, irritating chemicals, or infection by viruses, fungi or bacteria.
What are the beneficial effects of inflammation?
Prevents spread of damaging agents, Disposes of cell debris and pathogens, Alerts adaptive immune system, and Sets stage for repair
What are the four major signs of acute inflammation?
Redness, heat, swelling, and pain
What causes the release of inflammatory chemicals?
Tissue injury & immune cells
What is a key component of the inflammatory response and releases histamine?
Mast cells
What is released by Mast cells that is of note during the inflammatory response?
Histamine
What are the inflammatory chemicals?
Histamine, Kinins (Bradykinin), prostaglandins, and complement proteins
What is the effect that inflammatory chemicals have on the body?
They dilate local arterioles, make local capillaries leakier, and attract leukocytes to the area
During the inflammatory response what is responsible for the redness and heat?
Vasodilation through increasing blood in the area
What does vasodilation cause in the inflammatory response?
Redness and heat
What is the fluid containing clotting factors and antibodies that leaks from the capillaries into the tissue?
Exudate
What is exudate?
The fluid containing clotting factors and antibodies that leaks from the capillaries into the tissue
What does Exudate during the inflammatory response cause?
produces swelling (edema) and pain through increased pressure on nerve endings
What is edema?
Swelling produced by exudate which puts excess pressure on nerve endings causing pain.
What is produced by bacterial toxins within the inflammatory response?
The release of prostaglandins and kinins which produce pain.
What does sensitization do during the inflammation response?
It lowers the pain threshold, amplifying pain, causing the release of prostaglandins and kinins
How does Aspirin and other anti-inflammatory drugs work?
They inhibit prostaglandins, which in turn reduces pain
How does exudate aid the immune response in tandem with the lymphatic system?
the surge of protein rich fluids in the tissue washes the foreign material into lymphatic vessels causing the lymphatic system to respond.
How do the contents of exudate aid the immune response?
It delivers important proteins to the area. Complement proteins, and clotting factors that isolate the injured area and prevents the spread of the foreign material.
What are the four steps that allow the mobilization of phagocytes to injured areas?
Leukocytosis, Margination, Diapedesis, & Chemotaxis
What is Leukocytosis?
First step of the mobilization of phagocytes to injured area. When leukocytosis inducing factors is released form damaged cells it induces neutrophils to enter blood from red bone marrow
What causes Leukocytosis?
leukocytosis inducing factors
What is Margination?
Second step of Mobilization of Phagocytes to Injured Area. Cell adhesion molecules on endothelial cells of inflamed tissue signal the site of injury. When the Cell adhesion molecules on neutrophils are activated by inflammatory chemicals they bind to the endothelial cells of capillaries
What is diapedesis?
Third step of Mobilization of Phagocytes to Injured Area. The neutrophils flatten and squeeze through the endothelial cells of the capillary wall.
What is Chemotaxis?
The last step of phagocytes moving to injured areas. Neutrophils and other WBCs migrate up gradient of chemotactic agents released during inflammation.
How long does it take for neutrophils to gather at a site of injury from the start of inflammation?
Within the hour
How do monocytes get to an injured area?
They follow the neutrophils
After a monocyte leaves the blood how long does it take for it to differentiate into a macrophage?
Within 12 hours
What type of protein enhances the innate response?
Antimicrobial Proteins
What are the two most important antimicrobial proteins?
Interferons and complement proteins
What produces interferons?
Cells infected by viruses
Whats the function of interferons?
They are released from the infected cell and bind to the receptors in near by cells. This binding stimulates the cell to produce antiviral proteins that block viral protein synthesis and degrade viral RNA
What do the proteins that are produced by interferons stimulating cell receptors do?
They interfere with the normal function of viruses by blocking protein synthesis, and degrading viral RNA
Are Interferons virus specific or non-specific
They are not virus specific
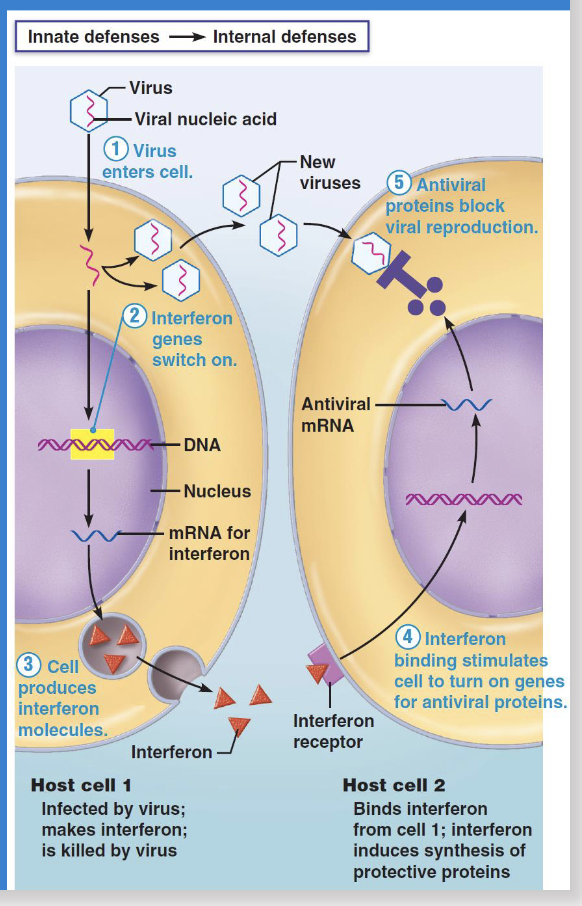
What is this?
The interferon’s function cycle
What are the three types of interferons?
Alpha (α), Beta (β), and Gamma (γ)
Whats the effect of an alpha interferon?
Has antiviral effects, and activates natural killer cells
What do beta interferons do?
Has antiviral effects, and activates natural killer cells
What are Gamma interferons secreted by?
T cells and NK cells
What do gamma interferons do?
Activates macrophages
How many different plasma proteins that circulate in blood are apart of the complement system?
Over 20
What proteins are included in the complement system?
C1-C9, Factors B, D and P, & Regulatory proteins
When the complement system is do to inflammation?
Enhances inflammation
What makes up the adaptive defense system?
T cells & B cells
What makes the adaptive defense system special?
It is specific, systemic, and has memory
What does it mean for the adaptive defense system to be specific?
It targets specific pathogens
What does it mean for the adaptive defense system to be systematic?
It is not restricted to initial infection site.
What does it mean for the adaptive defense system to have memory?
Mounts a faster and stronger defense against pathogens previously encountered.
What do the B cells do within the adaptive defense system?
Involved in the humoral antibody-mediated immunity. It’s Antibodies produced through humoral immunity circulate in blood and lymph
binding to extracellular pathogens
What do T cells do in the adaptive defense system?
They are involved with cell-mediated immunity and when activated T cells attack cells infected with pathogens directly
What are the four primary types of T Cells?
Cytotoxic, Helper, Regulatory, & Memory T Cells.
What do Cytotoxic T cells (Tc) do?
Directly attack antigen presenting cells