Lecture 10: Collateral and Multiple Ligament Injury/Meniscal Injury
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
collateral ligament injury
complete or partial tear of medial or lateral collateral ligament
ligament injury =
sprain
muscle tendon unit =
strain (no grading)
what is the function of the medial and lateral collateral ligament?
limit varus-valgus motion of stifle joint
injuries to medial or lateral collateral ligaments occur with
injury to other primary and secondary restraints of stifle joint
multiple ligament injuries result from
severe trauma to stifle joint
PE findings for collateral ligament injury
based on palpation
stifle joint extended to examine for collateral injury
the valgus stress test evaluates the
medial collateral ligment
the varus stress test evaluates the
lateral collateral ligament
valgus stress test
patient in lateral recumbency
one hand stabilizes femur while other hand grasps distal tibia and applies upward force (abduction)
if medial joint restraints are torn → see opening of medial joint line
varus stress test
patient in lateral recumbency
one hand stabilizes femur while the other hand grasps distal tibia and applies inward force (adduction)
if lateral restraints are torn → see opening of lateral joint
radiographs for collateral ligament tear
determines if bone fragments are associated with ligament damage
craniocaudal and medial-lateral radiographs confirm
presence of absence of bony avulsions
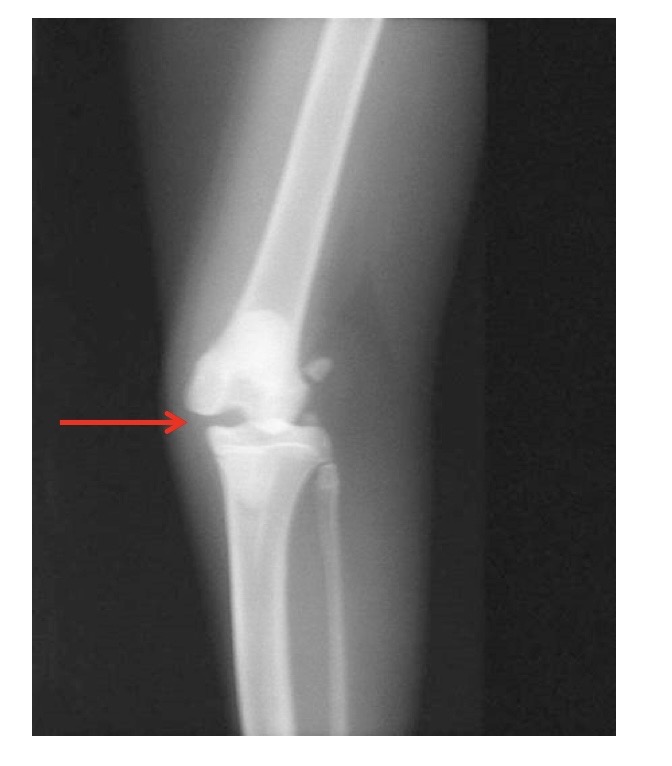
what is this showing?
valgus stress applied to joint → MCL injury
differential diagnosis for collateral ligament tear
muscle strains
cranial or caudal cruciate ligament tears
nondisplaced physeal fractures in immature animals
conservative or surgical treatment for isolated collateral ligament injury is based on
degree of injury
what is an indication for conservative treatment/1st degree sprain?
minimal swelling and only slight opening of joint space with stress test
what indicates greater injury to collateral restraints/2nd to 3rd degree sprains?
moderate to severe swelling and significant opening of joint space with stress test
surgical treatment for 2nd or 3rd degree sprains?
reconstruction of collateral ligaments, meniscocapsular ligaments, and joint capsule
primary repair of collateral ligaments is done if
point of failure is origin or insertion of ligament
an intrasubstance tear with large segments of ligament intact
preoperative management to prevent additional damage to articular cartilage or menisci
place modified robert jones bandage on limb
limit activity to leash walking
preop management for patients with injuries by HBC
thoracic, cardiovascular, and abdominal evaluation
perioperative antibiotics and preemptive pain management
NSAIDs
opioids
epidural analgesia
medial collateral ligament anatomy
originates from medial femoral epicondyle
runs distally to insert onto proximal tibial metaphysis
as ligament crosses medial joint line → strong attachment to joint capsule and medial meniscus
lies deep to caudal sartorius muscle
lateral collateral ligament anatomy
originates from oval area on lateral femoral epicondyle
runs distally to insert onto fibular head
lies deep to fascia lata
what do you need to preserve when dissecting near the lateral collateral ligament?
peroneal (fibular) nerve
peroneal nerve
branch of sciatic nerve
obliquely crosses distal aspect of stifle joint
superficial to gastrocnemius muscle
sends articular branch to lateral collateral ligament
patient positioning for lateral collateral ligament injury
lateral recumbency with affected leg up
patient positioning for medial collateral ligament injuries
dorsal recumbency
patient positioning for multiple ligament tears
dorsal recumbency to facilitate exposure to both sides of limb
suspend limb and prepare for aseptic surgery
where should the incision go for repair of a medial restraint injury?
the insertion of the caudal head of sartorius muscle and deep fascia along craniomedial border of proximal tibia
if ligament injury is intrasubstance tear
primary repair by suturing ligament ends with locking-loop suture pattern
supplement primary repair with screws and figure-eight support
repair of a lateral restraint injury
craniolateral approach to expose lateral collateral ligament
make proximal to distal parapatellar incision through fascia lata
continue incision distally 4cm below tibial crest parallel to joint line → protect peroneal nerve
reflect fascia lata caudally → expose collateral ligament and lateral joint capsule
repair ligament as described for MCL
prognosis for isolated collateral ligament tears
good to excellent
prognosis for multiple ligament tears
fair
multiple ligament injuries
injuries where cranial or caudal cruciate ligaments and collateral ligaments are damaged simultaneously
caused by HBC or other major trauma
surgical anatomy of multiple ligament tears
moderate to severe swelling and bruising of soft tissue surrounding joint seen
torn collateral ligaments difficult to identify because often encased in edematous connective tissue
menisci often displaced from normal positions and folded cranially or caudally
what structures are commonly injured with multiple ligament derangement of the stifle joint?
cranial and caudal cruciate ligaments and disruption of the medial restraints
common triad of multiple ligament injuries include
cranial and caudal cruciate ligament tears
failure of primary and secondary medial restraints
peripheral medial meniscal tears
deranged stifle
when there are multiple ligamentous injuries
often with meniscal injury → resulting in luxation of stifle joint
locations of release of medial meniscus
transection of meniscotibial ligament
transection of midbody of meniscus
meniscal release
means of protecting medial meniscus following surgical stabilization of stifle
developed in association with TPLO
uncertain efficacy
by transecting the meniscus, the function of the meniscus is
compromised by elimination of hoop stresses
midbody release or transection of meniscotibial ligament
femoral condyle increases contact with articular cartilage of tibial plateau → contributes to OA
impairs functions of meniscus to provide stability and congruence
no clinical studies demonstrate efficacy of meniscal release in
decreasing incidence of post TPLO meniscal injury, but technique remains in widespread use
why is conservative treatment not an option for meniscal injuries?
continued back and forth sliding of torn meniscus → causes severe pain, will not improve
accelerates DJD
methods of surgical treatment for meniscal injuries
partial meniscectomy
primary repair of peripheral meniscal injuries
total meniscectomy
medial meniscectomy is easiest to perform through a
medial surgical approach
partial meniscectomy
removal of torn section of meniscus
experimentally → carries less morbidity than a total meniscectomy
treatment of choice for bucket handle tears of medial meniscus
primary repair of peripheral meniscal injuries in dogs
reserved for peripheral tears
uncommon
total meniscal removal induces
severe DJD in stifle
total meniscectomy
considered only when peripheral rim of meniscus is so damaged that primary suturing of meniscocapsular tissue not possible
the more meniscal tissue removed, the more rapidly OA develops