CH 31: Vascular Disorders
1/29
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
30 Terms
A patient with atherosclerosis asks why smoking cessation is important. What should the nurse respond to this patient?
1. “Tobacco toxins increase your HDL-C.”
2. “Tobacco reduces the effects of cholesterol in the body.”
3. “Tobacco causes the blood pressure to drop and changes the cells within the arteries.”
4. “Tobacco smoke speeds the growth of atherosclerosis in coronary arteries, aorta, and the legs.”
ANS: 4
atherosclerosis is the damage of the artery lining/ thjis leads to decreased blood flow due to the narrowed arteries.
it is then accurate that it will affect coronary arteries, aorta and the legs.
The nurse provides education to a patient who is diagnosed with atherosclerosis. Which patient statement indicates a need for additional teaching?
1. “I will decrease my intake of folic acid.”
2. “I will eat a low-fat, low-cholesterol diet.”
3. “I will increase by daily activity to decrease by blood pressure.”
4. “I will quit smoking because nicotine increases the buildup of plaque.”
ANS: 1
folic acid needs to be increased because it helps decrease the different proteins that
increases blood clot risks
damages artery linings
*The nurse is preparing teaching material to help a patient with atherosclerosis manage lifestyle changes. What should the nurse emphasize in this teaching?
1. “You need to limit cigarette smoking.”
2. “You need to follow a low-fat, low-cholesterol diet.”
3. “You should consider adopting an active lifestyle.”
4. “You may have dizziness at times which is expected.”
ANS: 2
a low-fat, low-cholesterol diet lessens the LDL, and lowers the risk of artery damage.
cigarettes should not JUST BE LIMITED, it needs to be stopped
NOT CONSIDER an active lifestyle is highly encouraged
DIZZINESS is somethjing that should be reported and not normalized
A patient’s blood pressure is 140/86 mm Hg; however, previous measurements have been within normal limits. The patient denies any other complaints. Which intervention would be appropriate for this patient?
1. Refer the patient to the emergency department for treatment.
2. Prepare teaching on antihypertensive medications.
3. Schedule an additional measurement in a few weeks.
4. Instruct on the effects of hypertension on major body organs.
ANS: 3
diagnosing hypertension needs to have 2+ high readings on different days, and needs to be rechecked in a few weeks.
although the patient is having hypertension symptoms, these are the following that needs to be followed before giving antihjypertensive medicine.
In administering a calcium channel blocker to patient diagnosed with primary hypertension, the nurse correlates a decrease to which mechanism of action of this medication?
1. Blocks formation of angiotensin II, a potent vasoconstrictor
2. Blocks the action, not the formation, of angiotensin II
3. Decreases blood vessels’ ability to contract and cause vasoconstriction
4. Relaxes the muscles of the blood vessels
ANS: 4
calcium channel blockers relaxes the muscxles of the blood vessels. which means it VASODILATES.
1 and 3 has the words “vasoconstrict”
2 is not related
*The nurse provides education to a patient who is prescribed the DASH diet. Which patient statement indicates a need for additional teaching?
1. “I will eat four servings of fruit each day
2. “I will eat one serving of nonfat dairy each day.”
3. “I will eat five servings of vegetables each day.”
4. “I will eat at least three whole-grain foods each day.”
ANS: 2
the patient needs to have 2-3 servings a day of DAIRY.
The nurse monitors for which early clinical manifestation in the patient admitted with Buerger’s disease?
1. Bounding pulses
2. Claudication
3. Gangrene in affected extremity
4. Pitting edema in the lower extremities
ANS: 2
claudication or pain while moving is an early manifestation of buerger’s disease/
gangrene is a late sign.
1 and 4 is not related because Buerger’s disease is about the inflammation and blotting of the small vessels, which is strongly linked to smoking
Which assessment finding in patient with Raynaud’s phenomena requires an immediate intervention by the nurse?
1. Pitting edema in the lower extremities
2. Leg pain when ambulating
3. Numbness and tingling in the lower extremities
4. Weak distal pulses audible by Doppler only
ANS: 4
weak pulses is an EMERGENCY beecuase it means arterial insufficiency. this is a HIGH RISK because it can lead tto permanent tissue loss.
The nurse formulates the following diagnosis: “Impaired Tissue Perfusion related to Acute inflammation and thrombosis in arteries and veins in the hands and feet.” This nursing diagnosis is most relevant to which disease process?
1. Buerger’s disease
2. Raynaud’s disease
3. Secondary hypertension
4. Deep vein thrombosis
ANS: 1
buerger’s disease is specifically for inflammation and clotting of small vessels this counts the arteries and veings
raynaud’s disease: is specifically for artery contraction during the cold
secondary hypertension is not related
deep vein thrombosis is specifically for the legs and targets the veins
Which statement by the patient with Raynaud’s disease indicates that teaching was effective?
1. “Mittens are better than gloves to prevent episodes.”
2. “I need to decrease cigarette smoking.”
3. “I will need to take blood thinners for life.”
4. “I will need to limit fluid intake.”
ANS: 1
since raynaud’s disease is triggered by the COLD, mittens are much more effective in protecting the hands comapred to just gloves.
In completing an admission assessment on a patient admitted for evaluation of peripheral arterial disease (PAD), which statement by the patient correlates with stage III PAD?
1. “The pain usually goes away when I lie down.”
2. “The pain frequently awakens me at night.”
3. “I do not feel sharp objects when I step on them.”
4. “The pain is the same when I take long walk.”
ANS: 2
“pain awakens me at night” is stage 3 because the patient WILL feel pain at rest, which is contradictory to option 1 (pain goes away when lying down)
The nurse is monitoring a patient with peripheral arterial disease (PAD). Which clinical manifestations does the nurse correlate to stage III PAD?
1. Decreased pedal pulses
2. Pain, burning, and leg cramping relieved by rest
3. Pain, numbness and burning in the legs/feet at rest
4. Ulcers and blackened tissue on the toes
ANS: 3
(1) decreased pedal pulses = stage I
(2) indirectly stage II. this stage is specifically CLAUDICATION
(3) pain at rest = stage III
(4) ulcers and blackened tisue of toes = stage IV
The nurse is monitoring a patient with peripheral arterial disease (PAD). Which clinical manifestations does the nurse correlate to stage IV PAD?
1. Pedal pulses are decreased.
2. Muscle pain experienced with exercise.
3. Numbness and tingling of the extremity.
4. Tissue that is blackened on the great toe.
ANS: 4
(refer to q12)
The nurse reviews the ankle-brachial index for a patient admitted for treatment of peripheral arterial disease (PAD). What is the significance of a value of 0.50?
1. Normal
2. Borderline PAD
3. Mild to moderate PAD
4. Severe PAD
ANS: 3

*In administering hemorheological agents to a patient with peripheral arterial disease, the nurse correlates this treatment to which mechanism of action?
1. Anticoagulation
2. Diuretic
3. Platelet aggregation inhibitor
4. Vasodilator
ANS: 3
platelet aggregation inhibitor (stops blood clumping with e/o). since PAD narows the arteries and decreases bloodflow to the legs, having a platelet aggregation inhibitory factor. helps increase blood flow
*The nurse monitors for which complication in the patient with carotid atheroembolization?
1. Shortness of breath
2. Tachycardia
3. Change in level of consciousness
4. Upper extremity edema
ANS: 3
carotid atheroembolization is a concept where a plaque breaks off and clogs small arteries IN THE CAROTID ARTERY.
RESULT: less blood in the brain
(3) change in level of consciousness. the BRAIN IS VERY SENSITIVE TO OXYGEN if there is even one artery clog to oxygen distribution, it wiull lead to confusion. this is an early sign of stroke
A patient is diagnosed with carotid artery disease. The nurse monitors the patient for which potential complication of this disease process?
1. Stroke
2. Diabetes mellitus
3. Hypertension
4. Dyslipidemia
ANS: 1
stroke is a major complication of CAD
Based on an auscultated bruit over a patient’s carotid artery, the nurse explains to the patient which test as the most commonly ordered noninvasive diagnostic test to evaluate atherosclerotic plaque?
1. Carotid angiography
2. Carotid duplex ultrasound
3. Magnetic resonance angiography
4. Computed tomography angiography
ANS: 2
carotid duplex ultrasound is non invasive.
1,3,4 angiography: this is INVASIVE. it inserts a catheter to the area where the xray is happening
In monitoring a patient immediately after a carotid endarterectomy (CEA), the patient demonstrates impaired swallowing. The nurse correlates this finding to compression of which cranial nerve (CN)?
1. CN VII, Facial
2. CN X, Vagus
3. CN XI, Spinal accessory
4. CN XII, Hypoglossal
ANS: 2
CEA is a surgical procedure that removes plaques in the carotid artery of the neck (a treatment for CAD).
IMPAIRED SWALLOWING = vagus nerve / CN X
A patient recovering from a carotid endarterectomy (CEA) has a blood pressure of 90/48 mm Hg. What should the nurse do first?
1. Raise the head of the bed
2. Lower the head of the bed
3. Assess cranial nerve function
4. Place the head in neutral position
ANS: 2
lowering the head of the bad = laying flat. this helps with increased brain perfusion. because low blood pressured with CEA treatment is related to the CAD diagnosis that may lead to decreased blood flow to the brain
neuttral position: is standing up, aligned everything. this does not help with blood pressure.
In admitting a patient with a vascular disorder, the nurse correlates which clinical manifestation to femoral vein thrombosis?
1. Calf pain
2. Tenderness in the foot
3. Thigh swelling to the knee
4. Entire leg swollen and painful
ANS: 3

*Which statement by the patient discharge on warfarin (Coumadin) indicates the need for further teaching?
1. “I can take acetaminophen for pain.”
2. “I need to limit intake of green leafy vegetables.”
3. “It is okay if I see a little blood in my stool.”
4. “I need to take the medications at the same time every day.”
ANS: 3
blood in the stool, urine, or sputum NEEDS TO BE REPORTED vecause it has as high possibility that it is an INTERNAL BLEEDING, which is quick to make a paatient’s condition worse
In reviewing healthcare provider admission orders for a patient admitted for treatment of a deep vein thrombosis of the left lower leg, which order should the nurse question?
1. Compression stockings on both legs
2. Sequential compression devices on both legs
3. Elevate the left leg 10 to 20 degrees above the heart
4. Encourage fluid intake
ANS: 2
SCD: this device that pumps blood in the legs, may dislodge a clot if the patient has DVT. we don’t want that to happen cause it may travel. to the heart.
In reviewing diagnostic results for a patient, which values are consistent with a diagnosis of atherosclerosis? Select all that apply.
1. Decreased homocysteine levels
2. HDL-C 30 mg/dL
3. LDL-C 120 mg/dL
4. Triglycerides 175 mg/dL
5. HgbA1c 5%
ANS: 2,3,4
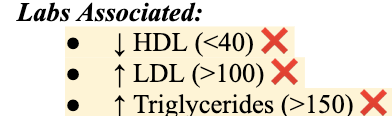
((1) “decreased” homocysteine levels = needs to be high for atherosclerosis
In providing care to a patient who is diagnosed with hypertension, which assessment data are risk factors for this disease process? Select all that apply.
1. Current age 45 years
2. Body mass index 28 kg/m3
3. A history of cigarette smoking
4. Glomerular filtration rate 58 mL/min
5. Concurrent diagnosis of diabetes mellitus
ANS: 3.4,5
(2) BMI 28 = needs to be 30 or higher as a risk , because it meands obesity
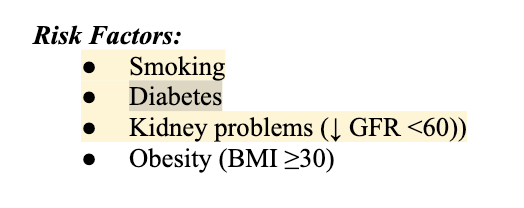
The nurse is preparing material about peripheral artery disease (PAD) for a community fair. What should the nurse include about modifiable risk factors for the disease? Select all that apply.
1. History of chronic obstructive pulmonary disease
2. Smoking
3. Hypertension
4. Family history of cardiovascular disease
5. Sedentary lifestyle
ANS: 2,3,5
modifiable risk factors: any factors of PAD that can still be changed
1 & 4 are history of the patient. they cannot be changed anymore
The nurse monitors for which clinical manifestations in the patient with carotid artery disease. Select all that apply.
1. Dizziness
2. Difficulty talking
3. Sudden vision changes
4. Upper extremity edema
5. Sudden weakness on one side of the body
ANS: 1,2,3,5
CAD clinical manifestations are stroke symptoms.

Which statements by a 70-year-old patient about elective surgery for repair of an abdominal aortic aneurysm indicate that teaching was effective? Select all that apply.
1. “The size of my aneurysm is not a factor.”
2. “I have a greater risk of rupture because I have hypertension.”
3. “Because my aneurysm is 7 cm, the risk of rupture is greater that the risk of dying during surgery.”
4. “My risk of rupture is greater because my aneurysm is 7 cm wide.”
5. “My age is really not a consideration at this time.”
ANS: 2,3,4

The nurse correlates which pathophysiological processes to Virchow’s triad? Select all that apply.
1. Vasodilation
2. Stasis of blood flow
3. Hypercoagulability
4. Leukocytosis
5. Endothelial injury
ANS: 2,3,5

In providing care to a patient with a deep vein thrombosis (DVT), which findings in the patient’s history are contraindications for tissue plasminogen activator (tPA)? Select all that apply.
1. History of osteoarthritis
2. Being treated for hemophilia
3. Previous surgery for spinal stenosis
4. Symptoms of a DVT present for a week
5. Diagnosis of DVT made upon symptoms
ANS: 2,4,5
(5) DVT diagnosis from symptoms: it needs to be A CONFIRMED DIAGNOSIS. if it just ASSUMPTIONS, it is a.contraindication.
