NURS2001 - Wk 3 Lec Pharmacodynamics
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms

Pharmodynamics
What the drug does to the body
Where do drugs bind
Ligand binds to a receptor to initiate an action (eg. opening a channel one macromolecule)
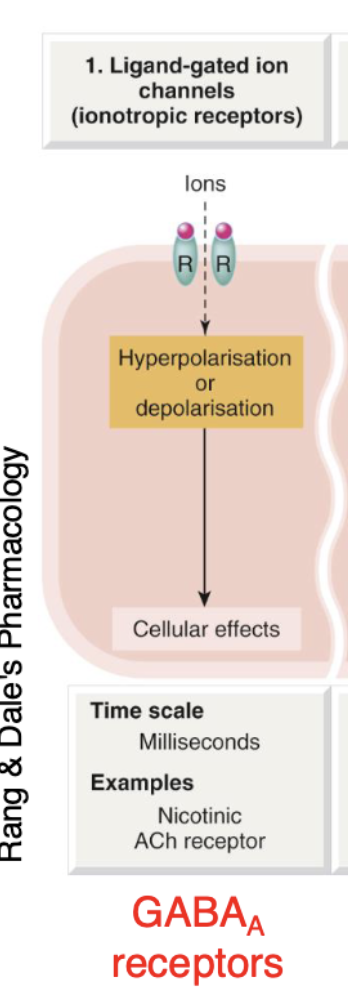
Ionotronic receptors
Ligand-gated ion channel
Ligand = drug
drug binds to receptors
Then a channel opens which initiates ions to enter the cell
Process causes hyperpolarisation or depolarisation of cell
Changing the charge of the cell membrane
This process occurs very quickly (milliseconds)
eg. GABA a Receptors
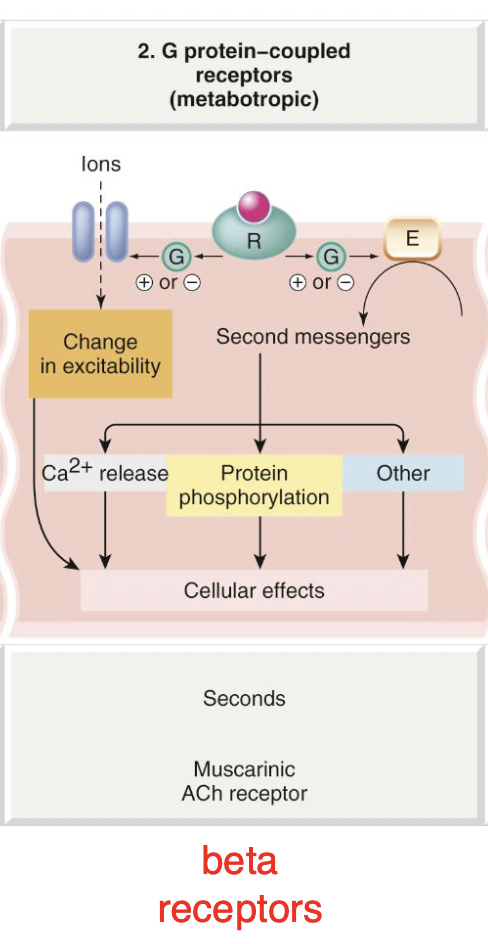
Metabotropic Receptors
G protein-coupled receptors
Ligand binds to receptors
Activates the action of G-proteins
Causing a cascade of effects eg. multiple enzymes changing etc.
Occurs in seconds
eg. Beta receptors
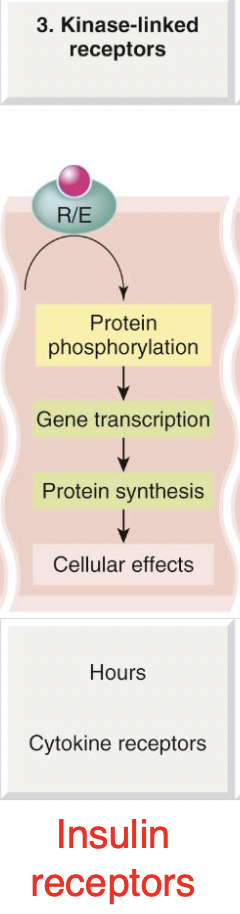
Kinase-linked receptors
Receptor is both intracellular and extracellular
intracellular receptor = enzyme
Extracellular receptor is bind by a ligand triggering phosphorylation of the interior enzyme within the cell
causing gene transcription and then protein synthesis
This process takes Hours
eg. Insulin receptors
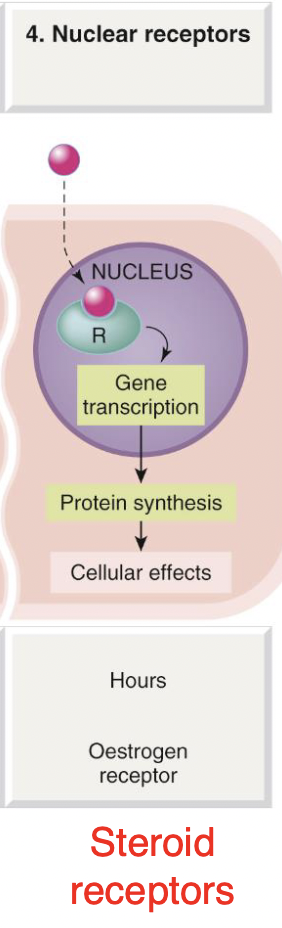
Nuclear receptors
Drug (ligand) must go past cell membrane and into nucleus of the cell
Initiating gene transcription and then protein synthesis
This process takes the longest (more hours)
eg. steroid receptors
IMPORTANT TO NOTE
Fastest to slowest responses to drugs (how fast the effect of a drug takes)
Isotronic receptors, Metabotropic receptors, Kinase-linked receptors, Nuclear receptors
Isotronic > Beta blockers etc. > Insuline/cytokine receptors > Steroids / oestrogen receptors
Ion channels (other places drugs/ligands may bind to)
eg. Local anaesthetics inhibit voltage gated sodium channels
Essentially, these drugs jam and block the receptor channel to prevent a signal from going through
Carriers (other places drugs/ligands may bind to)
eg. LDL (pts w high cholesterol often have high low-density lipoprotein) bind to LDL receptors which causes metabolism within the cell
Enzymes (other places drugs/ligands may bind to)
NSAIDs (eg ibuprofen) inhibit cyclooxygenase enzymes to trigger the anti-inflammatory effect
Agonist
Bind to receptors to produce a response (mimicking endogenous ligands that naturally produce a response)
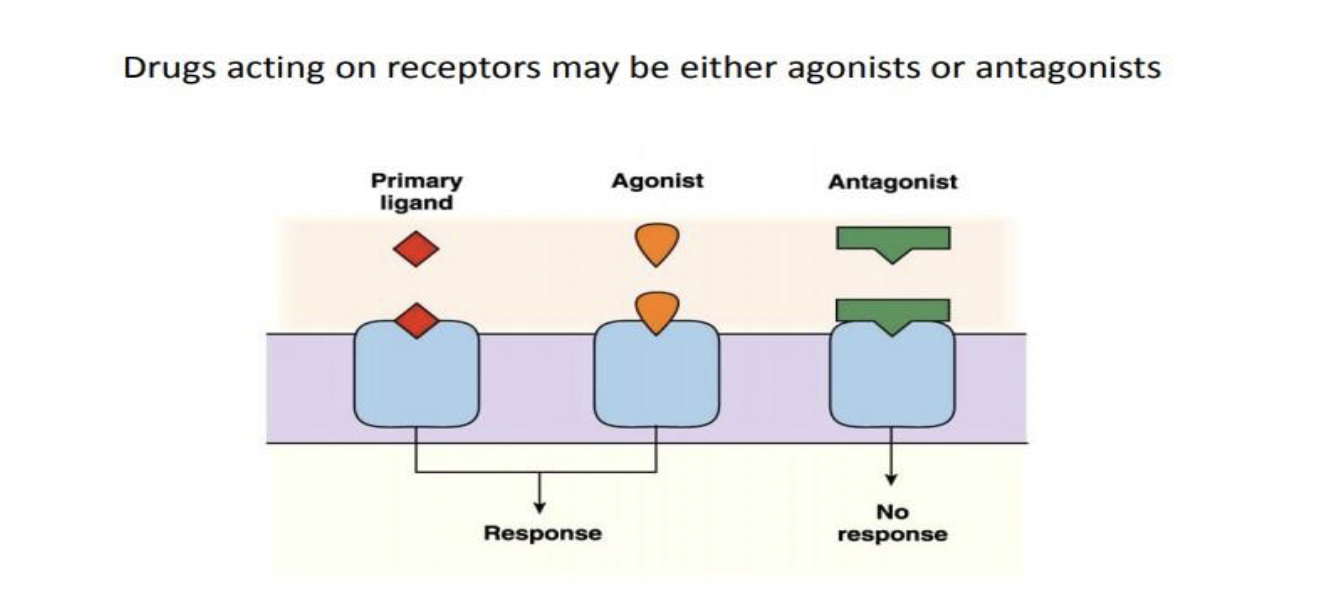
Antagonist
Bind to receptors to prevent/inhibit a response by blocking the receptor from natural ligand binding activity
Affinity
Drug binding to the receptor
The ability of a drug to bind to a receptor
Efficacy
Ability of drug to activate the receptor once bound
Even though a drug can bind, it’s efficacy is dependent on whether it can produce a response
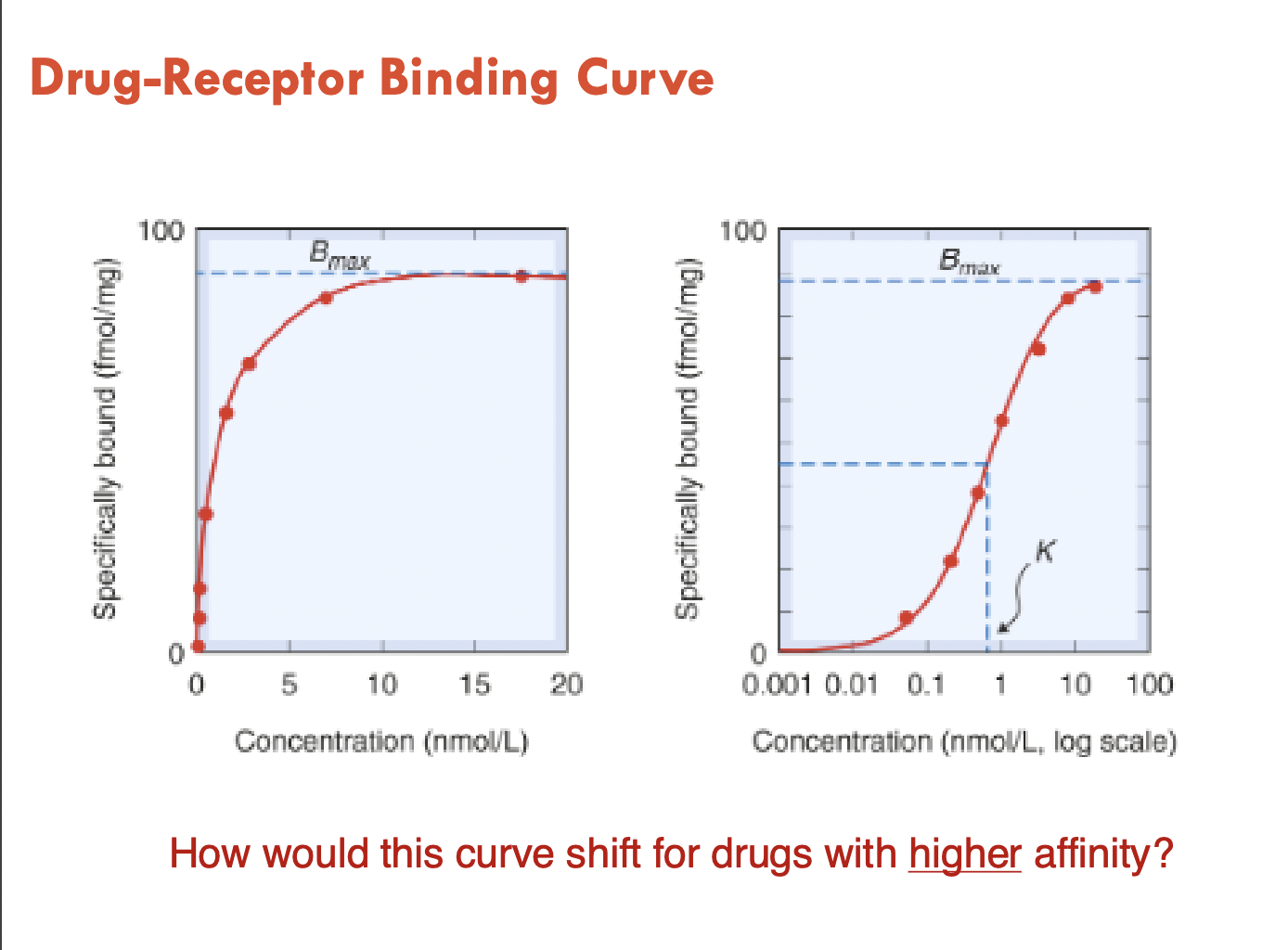
Drug receptor binding curve
Higher affinty = curve will shift to the left since it takes less concentration for drug to reach its max bound capacity
Bounding quicker
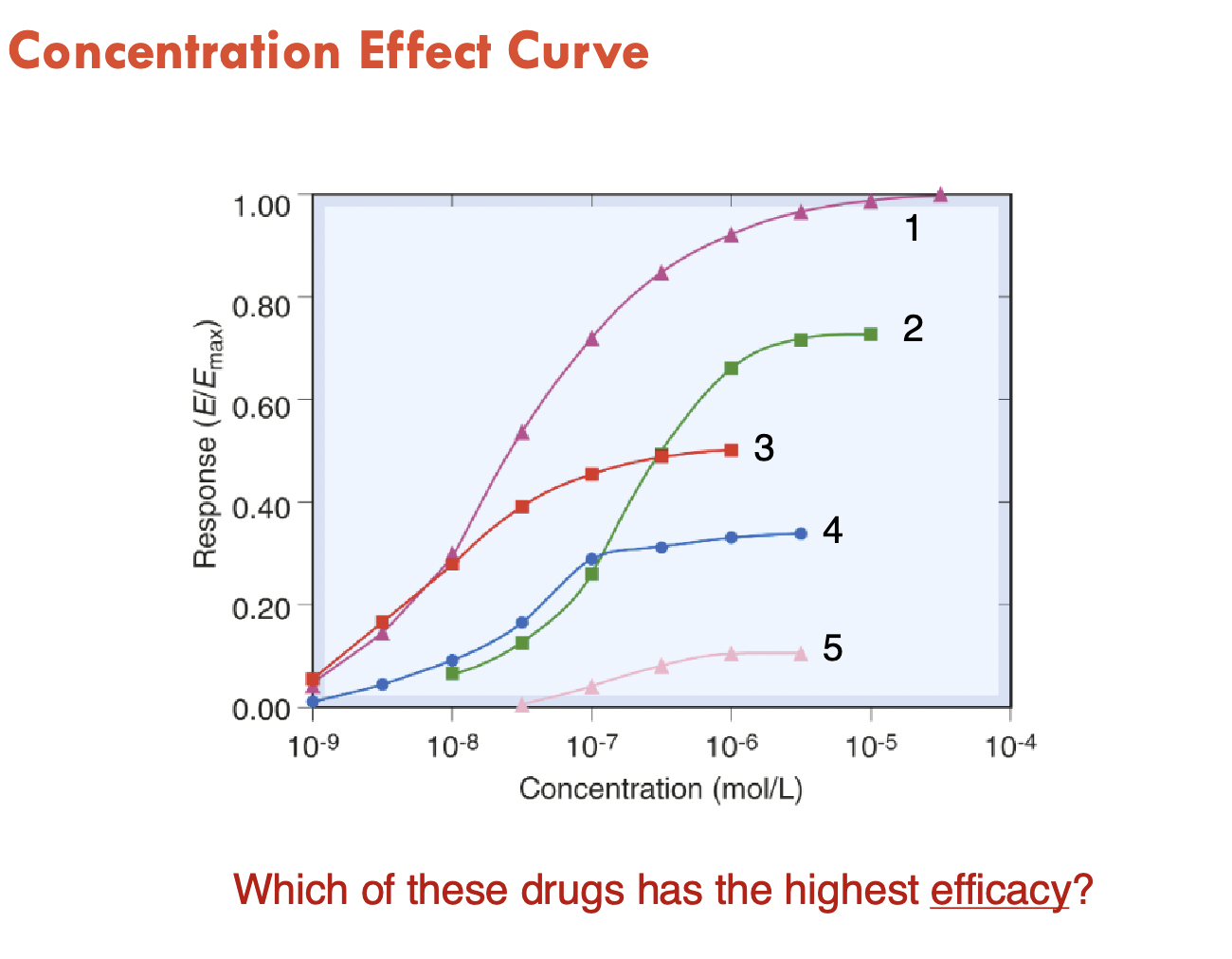
Concentration effect curve
Higher efficacy = higher response
Dose response relationship: efficacy
Max effect = Full agonist
Sub-max effect = Partial agonist
eg. Buprenorphine = partial agonist as although it has a high affinity, its ability to create a max response is limited, thus a partial agonist
Potency
Concentration or amount of drug required for a max response
eg. drug A can reach max (or same) response with a lower conc compared to drug B, thus drug A has a higher potency
Although they have the same efficacy, their potency is different
Selectivity
How selective and specific a drug is when binding to a receptor
eg.
Propranolol = non selective Beta blocker
Metoprolol = selective beta blocker
Therefore, propranolol is more likely to cause adverse effects such as bind to beta 2 receptors in the lungs
—> This in turn can cause bronchial restriction, impacting patients with asthma etc.
Higher dose = more likely to bind to more variety of receptors no matter if selective or non selective
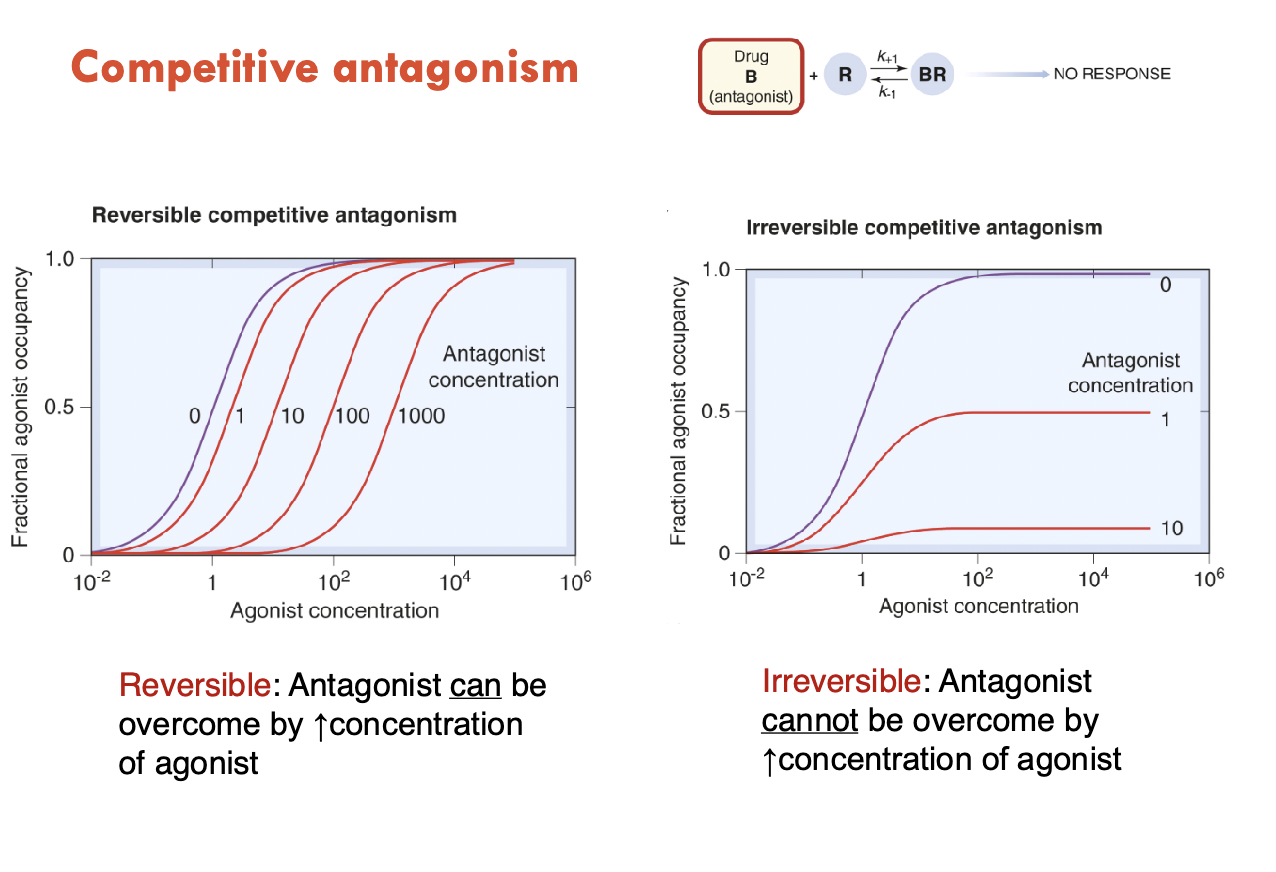
Competitive antagonism
Higher conc of antagonist = higher conc of agonist required to overcome and reach max agonist occupancy
—> this is reversible competitive antagonism as you can still combat the antagonism
Higher conc of antagonist = higher conc of agonist required, however conc of agonist occupancy decreases as antagonist conc increases
—> therefore irreversible competitive antagonism
Drugs
All have some form of side effects (eventually)
Adverse drug event
Medication errors
Adverse drug reactions
Can occur with everything happening well, but still something happens
Adverse drug reaction
Unintended
Type A = Predictable and dose-dependent (eg. side-effect, toxicity/overdose)
Type B = Hypersensitive reaction, unpredictable and not dose dependent (eg. allergic reaction, intolerance)
Risk of ADR
Age
Sex (females)
Disease
genetic factors
history of adverse reactions
How to prevent ADRs?
Accurate medication history
Pt interview and reviewing of Pt
Therapeutic drug monitoring (measuring conc of drugs)
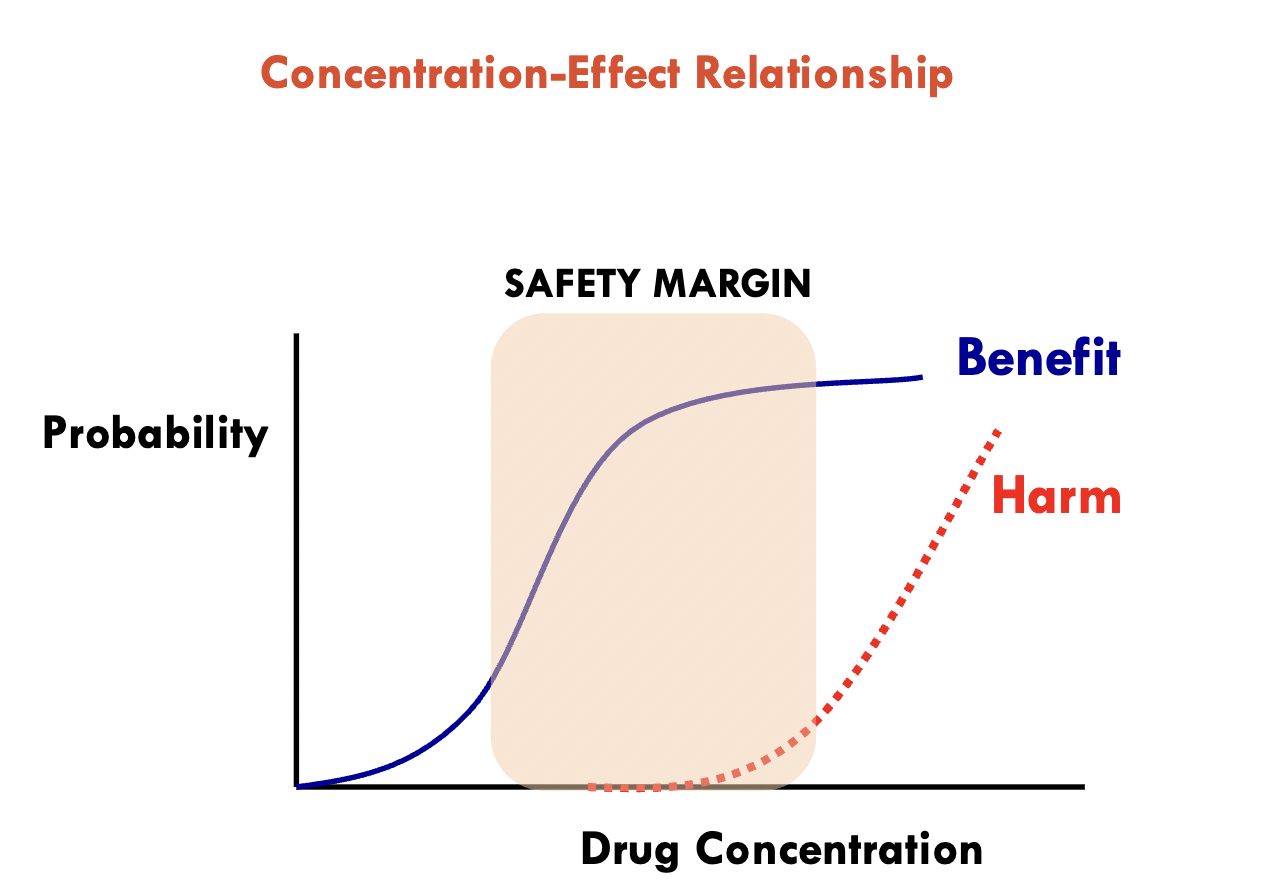
Therapeutic index (range)
Margin of safety
The gap between the the drug response and the time it takes to have adverse effects
Thinner gap = lower margin of safety
Physiochemical interactions
Physical incompatibility
Eg. drugs may not be compatible to be mixed in IV mixtures (eg crushing and mixing 3 drugs in mixture)
Can lose activity ability or cause adverse effects
Pharmokinetic
ADME
Absorption = Normal food-interactions
Distribution = Protein binding
Metabolism = Cytochrome P450 (CYP450)
Elimination = ????
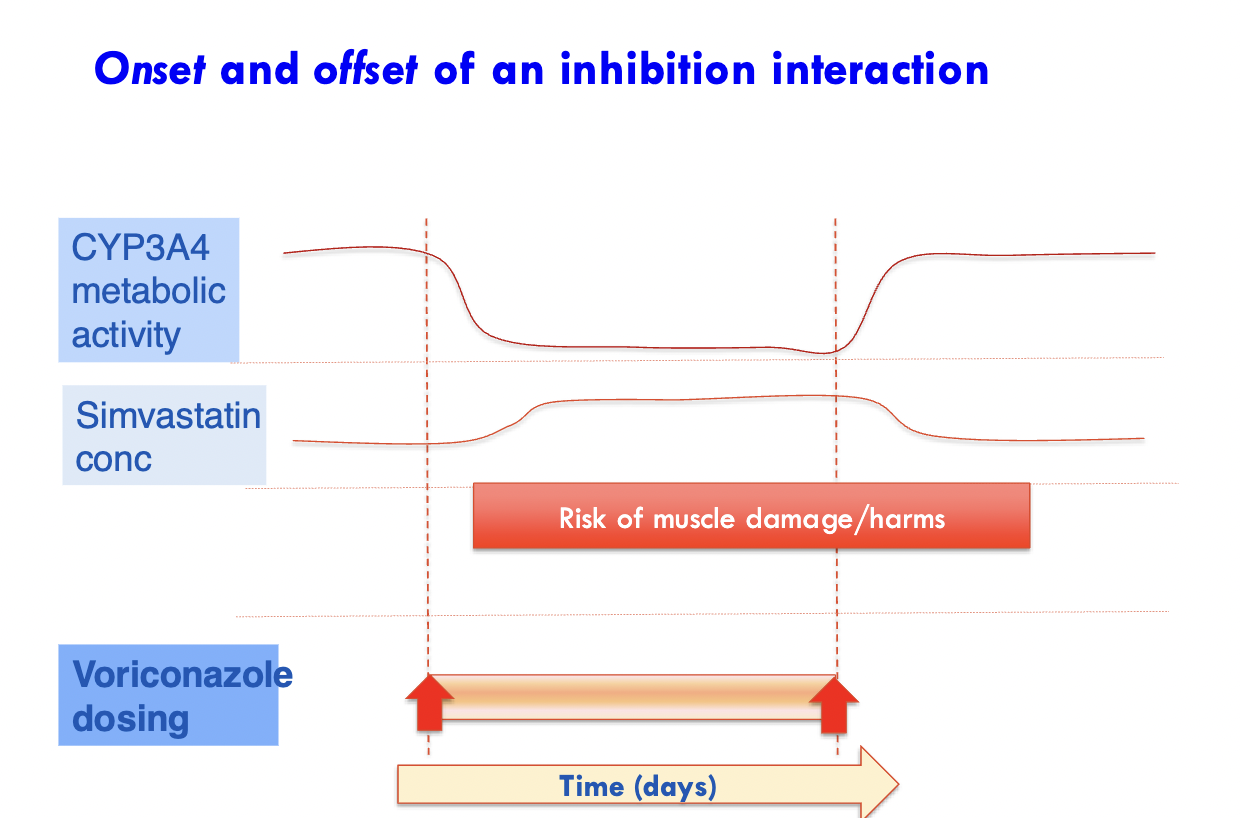
Onset —> offset of inhibition interaction of a drug
Increased dosing = increased other drug conc, decreased enzyme activity (eg. CYP3A4) and HARM
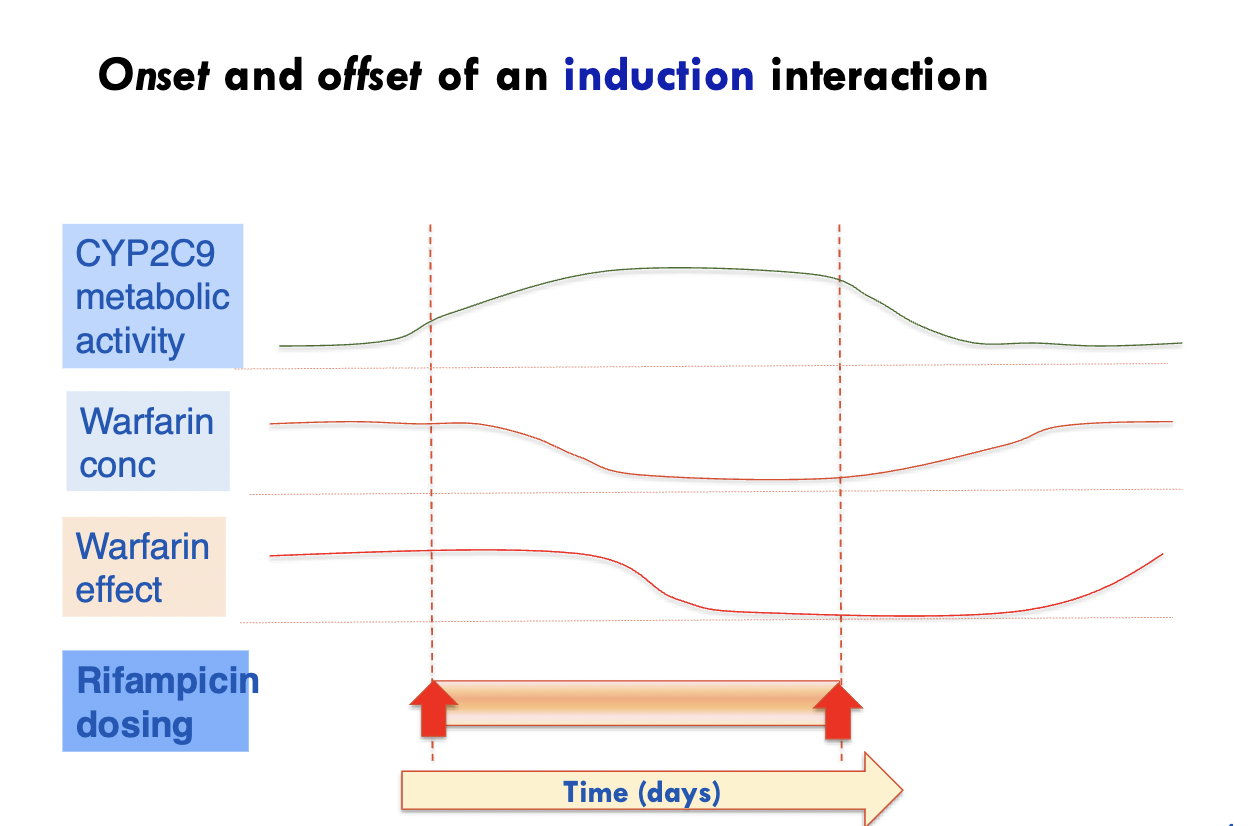
Induction reaction
Increased dosing = decreased other drug conc and its effect, while increase enzyme metabolic activity (eg. CYP2C9)
Pharmacodynamic interactions
Drugs with similar mechanisms of action and pharmacological effects
Antagonist and agonists
Examples of Enzymes
Inducers = Phenytoin
Inhibitor = Clarithromycin