Pharmacodynamics & Introduction to Autonomic Control
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
28 Terms
what is a drug
any substance or product that is used or intended to be used to modify or explore physiological systems or pathological states for the benefit of the recipient
how do drugs cause its effects
the target the drug interacts with
how the drug binds to the target site(s)
how binding translates to a biological effect
what are the 4 main ways a drug may interact in the body
May interact through:
receptors - ligand/receptor interaction
ion channels
enzymes
carrier channels/transporters
what is a ligand & what aspects determine its binding
substance that binds to a receptor, can be a ‘drug’ or endogenous factor
binding depends on:
shape & size
how does affinity of a drug effect its binding
forces of attraction
weak & reversible:
hydrogen bonds
ionic bonds
dispersion forces
strong & potentially non-reversible
covalent
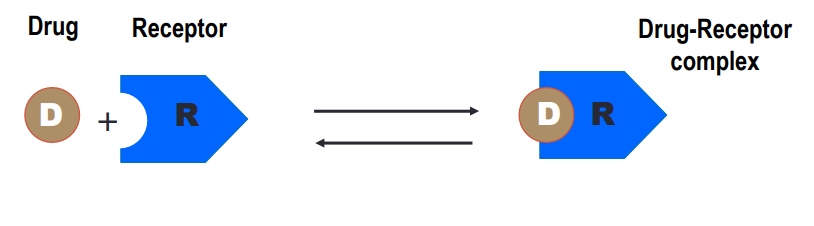
how does the law of mass action relate to drug-receptor binding
the principle that the rate of a chemical reaction is proportional to the concentrations of the reacting substances / reactants
more drug (limiting reagent) + receptor = drug-receptor complex
what are the different K values for the drug-receptor complex
Kon = association
Koff = dissociation
therefore, [D] x [R] x Kon = [DR] x Koff (this is true at equilibrium)
NOTE: ↑ [DR] = ↑ response
what is measure of affinity
when 50% of receptors are occupied: [R] = [DR]
therefore, [D] = Kd = measure of affinity
e.g. Kd = 1nM (means that only 1nM is required to occupy 50% of receptors)
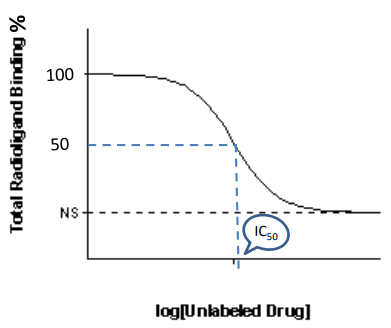
what are competition binding assays/experiments
experiments used to determine the Kd/IC50 (inhibitory curve at 50%)
starts with a radioligand (radioactive ligand) mixed with a sample of receptors until saturated
drug of interest (non-radioactive) is added to the mixture, the drug displays the radioligands thus decreasing the % of radioligands bound
this is illustrated by a graph (inhibitory curve)
NOTE: IC50 = Ki = Kd
how are Ki valves reported
as pKi values:
pKi = -log10(Ki)
higher pKi = greater affinity
what are some of the different receptor types
ligand-gated ion channels
G-coupled protein receptors
kinase-linked receptors
nuclear responses
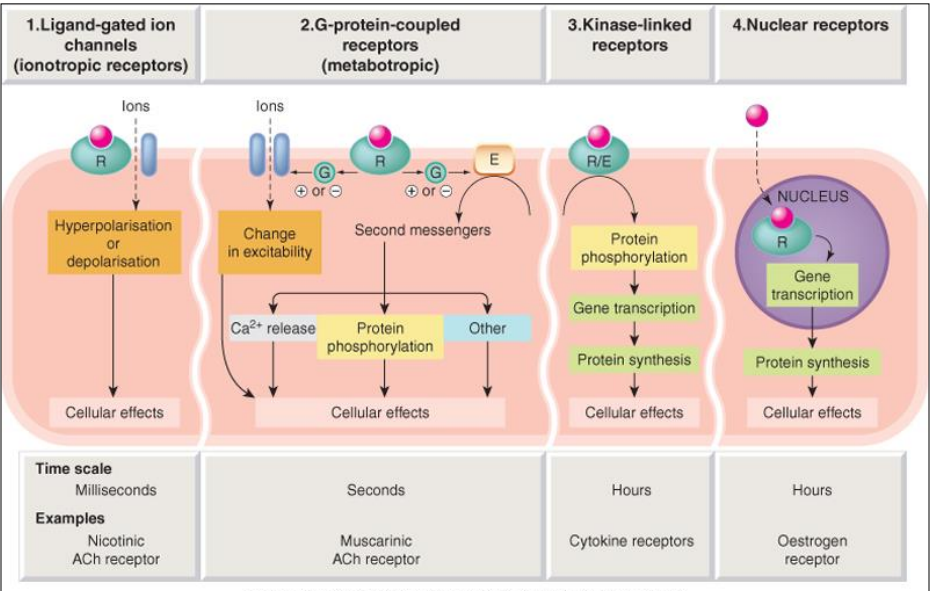
what are agonists & antagonists
agonist - a drug/molecule that activates a receptor (denoted: DR*), mimics the effect of original ligand
antagonist - a drug/molecule that inhibits the activation of a receptor
has affinity but NO efficacy
what is efficacy
the ability of a drug, once bound, to activate the receptor to cause a response
refers to effect as a result of receptor activation
what is clinical efficacy
refers to the therapeutic effect of a drug
what are concentration-response curves
curves that display the relationship between [D] & % response
Emax = maximum response = efficacy
EC50 = agonist concentration that produces a response 50% of maximum = potency
![<p>curves that display the relationship between [D] & % response</p><ul><li><p>E<sub>max</sub> = maximum response = efficacy</p></li><li><p>EC<sub>50</sub> = agonist concentration that produces a response 50% of maximum = potency</p></li></ul><p></p>](https://knowt-user-attachments.s3.amazonaws.com/c3c74134-7d8d-40ac-b883-f8a136e76f5d.png)
what is potency & how is it measured
measure of how much of a drug is required to produce a particular effect
measured as pEC50 = -log10(EC50)
greater pEC50 = greater potency
what is selectivity
the degree to which a drug acts on a given site relative to other sites.
e.g. a drug has high selectivity for kidney but low for brain
what is therapeutic index
relates the dose causing adverse effects to the dose causing desired effect
i.e. dose that cause good effects vs dose that causes bad effects
what is the natural state of receptors
normally in the inactive form but become active via a ligand that forces a conformational change in shape
what is important to note about the location of sympathetic nerves
located within the spinal cord, in which axons branch out to differnet parts of the body
how is noradrenaline formed
formed from tyrosine which enters neuron via a transporter
tyrosine → DOPA (tyrosine hydroxylase)
DOPA → dopamine (DOPA carboxylase)
dopamine is moved into VMAT vesicle
dopamine → noradrenaline (dopamine β-hydroxylase - only in synaptic vesicles)
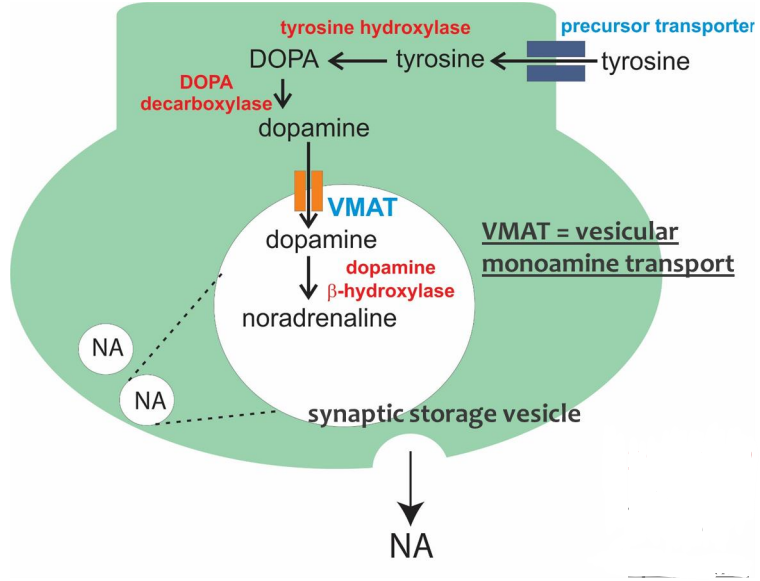
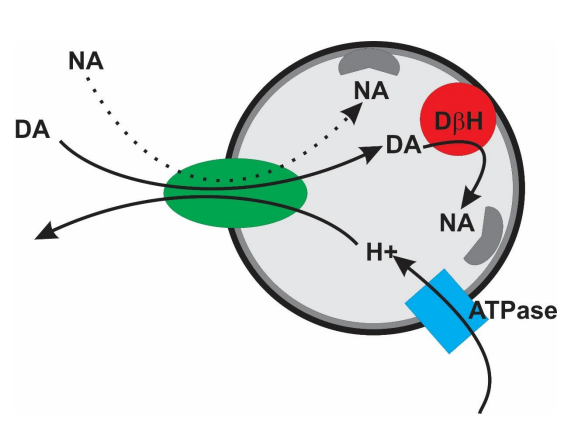
what is vesicular monoamine transport (VMAT)
storage vesicle that takes up dopamine (& noradrenaline) for storage & re-release
ATPase drives H+ into vesicle
H+ is released for vesicle in exchange for dopamine
NA formed is bound to the membrane of the vesicle
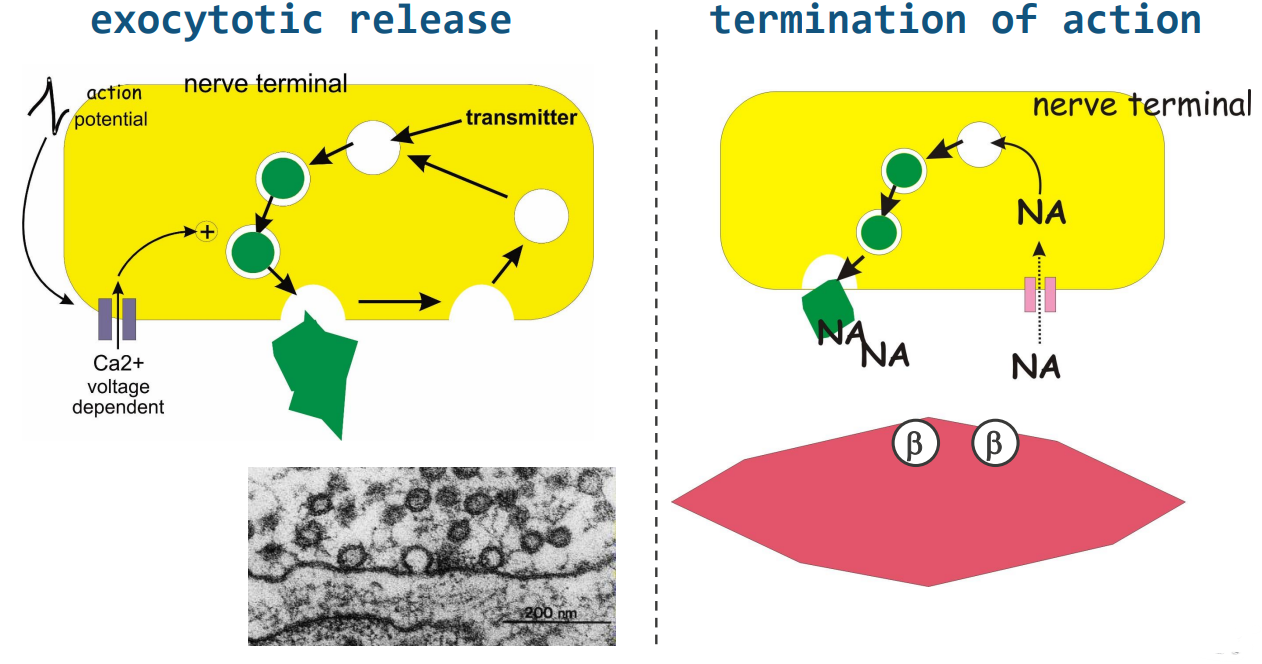
what is the process of NA release & recycling
exocytotic release:
AP propagates through cell activating Ca2+ channels
calcium facilitates the movement of VMAT to nerve terminal where its released
termination/recycle:
NA in synaptic cleft is taken up by a transporter
NA is reloaded into VMAT vesicles ready for re-release
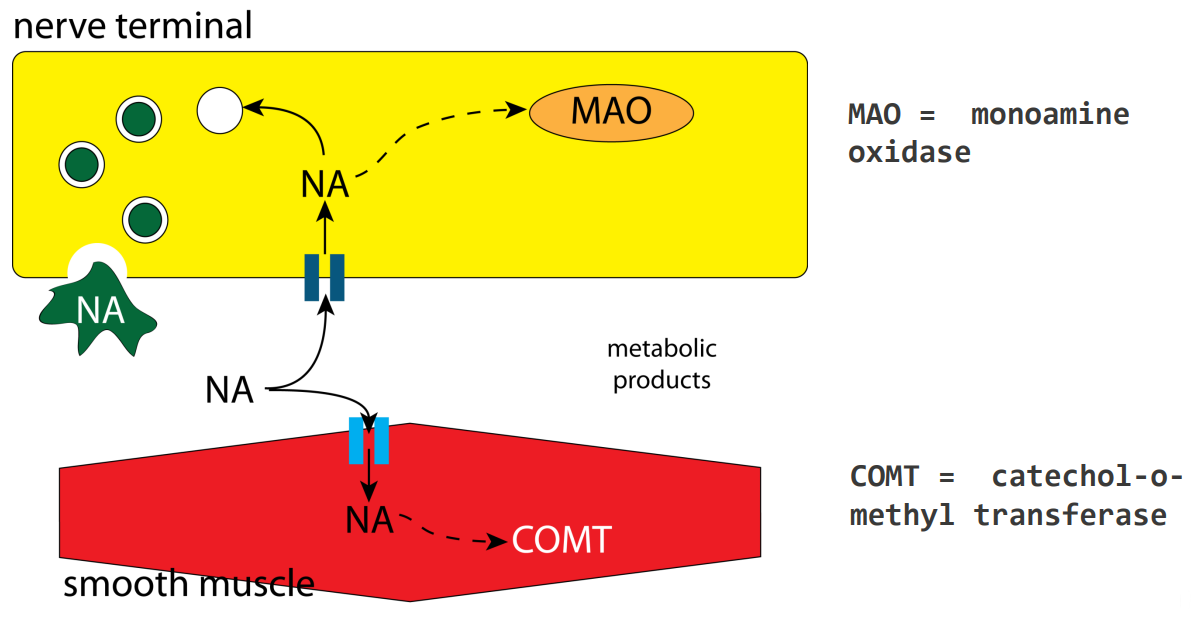
what enzymes breakdown or degrade NA
MAO = monoamine oxidase
found in nerve terminal
degrades NA
COMT = catechol-o methyl transferase
metabolises NA that is taken up by the smooth muscle cell
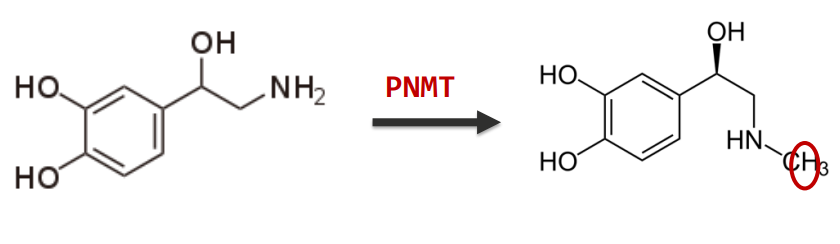
what is adrenal
a hormone from the medulla of the adrenal glands
travels through bloodstream to act on structures like the bronchi
synthesised from noradrenaline by PNMT (phenylethanolamine N methyltransferase)
what are some differences between α & β receptors
α-receptors: noradrenaline >= adrenaline
mainly regulated cardiovascular system: contracts vessels
β receptors: adrenaline >= noradrenaline
heart rate (increases force & rate)
gut activity (slows & relaxes)
smoot muscle (dilates to increase blood flow)
what are some different β-receptors
β1-receptors: cardiac muscle, liver, skeletal (↑force & rate)
β2-receptors: lungs, blood vessels (relaxation ↑blood flow & O2 delivery)
β3-receptors: adipose tissue (lipolysis)
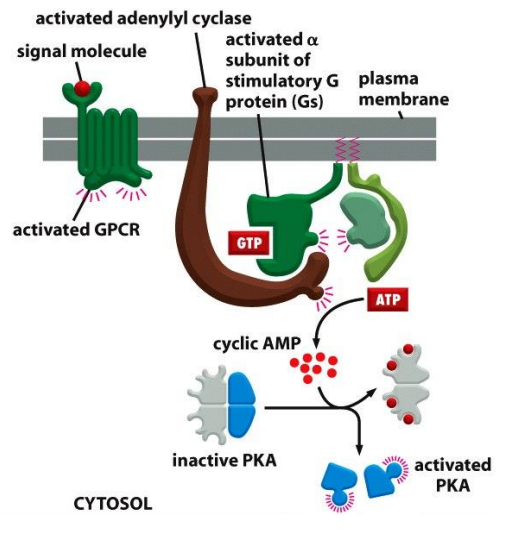
what type of receptor is β adrenoceptors:
G-protein coupled receptors
thus β adrenoceptors activate adenylyl cyclase
this produces cAMP
cAMP activates protein kinase A
protein kinase A phosphorylates activates other enzymes
NOTE: this examples why receptors on different cell cause different effects since they phosphorylate different intracellular proteins