[OB Exam 1 2/4] MAIN CONTENT
1/185
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
186 Terms
Chapter 4: Prenatal Care
QEBP
Prenatal care dramatically reduces infant and maternal morbidity and mortality rates by early detection and treatment of potential problems. A majority of birth defects occur between 2 and 8 weeks of gestation.
QS
Client History Assessment for Prenatal Care includes Any hazardous environmental exposures; current work conditions.
QPCC
Birth Plan: A nurse ascertains what a client’s goals are for the birthing process. The nurse should discuss birthing methods, such as Lamaze, and pain control options (epidural, natural childbirth).
Preconception and prenatal education emphasizes healthy behaviors that promote the health of the pregnant client and their fetus.
The nurse anticipates reviewing prenatal education topics with a client based on their current knowledge and previous pregnancy and birth experiences. The client’s readiness to learn is enhanced when the nurse provides teaching during the appropriate trimester based on learning needs. Using a variety of educational methods (pamphlets, videos) and having the client verbalize and demonstrate learned topics will ensure that learning has taken place
QTC
Assist the provider with the gynecological examination. This examination is performed to determine the status of a client’s reproductive organs and birth canal. Pelvic measurements determine whether the pelvis will allow for the passage of the fetus at delivery.
Client History (Initial Assessment)
Reproductive & Obstetrical History – Contraceptive use, STIs, gynecological conditions, previous pregnancies.
Medical History – Chronic illnesses, surgeries, immune status (rubella, hepatitis B).
Nutritional History – Identifies deficiencies or dietary risks affecting fetal growth.
Family History – Genetic conditions or hereditary risks.
Recent or Current Infections – Any illnesses that may impact pregnancy.
Current Medications & Substance Use – Includes alcohol, tobacco, and illicit drugs.
Psychosocial History – Emotional well-being, support system, history of depression, domestic violence.
Environmental & Occupational Exposures – Workplace risks, chemical exposures.
Exercise & Lifestyle – Impact on pregnancy health.
Abuse History or Risk Factors – Screen for physical, sexual, or emotional abuse.
Birth Plan Discussion
Patient’s goals for labor & delivery (e.g., natural birth, epidural).
Childbirth education & pain management options (Lamaze, breathing techniques).
Lamaze
A childbirth technique that helps pregnant women prepare for labor and delivery. It is also known as the psychoprophylactic method.
Prenatal Assessments
First Visit (Initial Prenatal Visit, within 12 weeks)
Determine EDD (estimated due date) using Naegele’s Rule.
Obtain vital signs, baseline weight, pelvic exam.
Order lab work: Hemoglobin, hematocrit, blood type & Rh, rubella titer, urinalysis, STI screening, HIV, Hepatitis B, Pap smear, toxoplasmosis, RPR/VDRL (syphilis).
Ongoing Prenatal Visits (Follow Schedule)
16-28 weeks: Every 4 weeks.
28-36 weeks: Every 2 weeks.
36 weeks to birth: Every week.
Ongoing Prenatal Visits (Follow Schedule)
16-28 weeks: Every 4 weeks.
28-36 weeks: Every 2 weeks.
36 weeks to birth: Every week.
Ongoing Care & Assessments
Monitor Weight, BP, Urine for Protein/Glucose (Gestational HTN & Diabetes screening).
Assess for Edema & Fetal Development
FHR (fetal heart rate) heard by Doppler at 12 weeks.
Fundal Height Measurement – Between 18-30 weeks, fundal height in cm = gestational age.
Fetal Movement felt by 16-20 weeks.
Patient Education
Common discomforts: Nausea, back pain, heartburn.
Danger signs: Severe headache, vision changes, decreased fetal movement.
Nursing Interventions
Perform Leopold Maneuvers
To assess fetal presentation & position.
Assist with Pelvic Exam
Ensures pelvis is adequate for delivery.
Administer Rhogam (RhO(D) Immune Globulin)
Given at 28 weeks if Rh-negative to prevent Rh incompatibility.
When must Rh- mothers receive Rhogam to prevent complications?
28 weeks
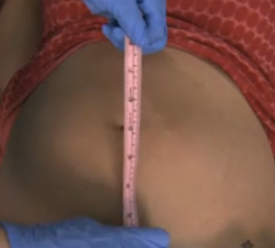
Fundal Height Measurement
Measurement correlates with gestation weeks (+-2)
ONLY ACCURARE 18/20 - 31/32 weeks
Blood Tests
Blood Type & Rh Factor: Screens for Rh incompatibility
Rh-negative mothers need Rhogam at 28 weeks.
CBC (Complete Blood Count): Detects infection and anemia.
Hgb Electrophoresis: Identifies sickle cell anemia & thalassemia.
Rubella Titer – Checks immunity to rubella
Live vaccine cannot be given during pregnancy
Hepatitis B Screen – Identifies carriers of hepatitis B.
Infection Screening
Group B Streptococcus (GBS) – Vaginal/rectal culture at 36-37 weeks
Antibiotics needed in labor if positive.
Pap Smear (Pap test) – Screens for cervical cancer, HPV, herpes simplex type 2.
Vaginal/Cervical Culture – Screens for STIs (gonorrhea, chlamydia, bacterial vaginosis, beta-hemolytic strep).
PPD (Tuberculosis Test) – Chest x-ray required after 20 weeks if positive.
VDRL/RPR – Syphilis screening (mandated by law).
HIV Screening – Offered at first visit (can be refused but recommended).
TORCH Screening (Toxoplasmosis, Rubella, CMV, Herpes) – Done if indicated (history of exposure).
Urinalysis & Glucose Screening
Urinalysis with Microscopy – Detects protein (preeclampsia), glucose (diabetes), ketones, infection.
hCG (Human Chorionic Gonadotropin) – Confirms pregnancy.
1-Hour Glucose Tolerance Test (24-28 weeks; no fasting) – If >140 mg/dL, follow-up needed.
3-Hour Glucose Tolerance Test (Fasting) – Confirms gestational diabetes if 1-hour test is abnormal.
Hemoglobin A1C – Used for pre-existing diabetes diagnosis (Normal: <5.9%).
Genetic & Fetal Abnormality Screening
Maternal Serum Alpha-Fetoprotein (MSAFP) (15-22 weeks)
Low levels → Possible Down syndrome.
High levels → Possible Neural tube defects (Spina bifida, anencephaly).
Quad Screen (AFP + hCG + Estriol + Inhibin A) may be used for better accuracy.
What is the relation tp protein in urine to hypertension/preeclampsia
Hypertension damages kidney function, leading to protein leakage into urine.
Proteinuria + high BP = possible preeclampsia → requires close monitoring.
Severe preeclampsia needs urgent intervention to prevent complications (eclampsia, HELLP syndrome, stroke).
Initial Prenatal Visit (First Trimester: Up to 12 Weeks)
Blood Type & Rh Factor – Determines Rh incompatibility (Rh-negative moms need Rhogam at 28 weeks).
CBC (Complete Blood Count) – Screens for infection and anemia.
Hgb Electrophoresis – Detects sickle cell anemia & thalassemia.
Rubella Titer – Checks immunity to rubella (live vaccine not given in pregnancy).
Hepatitis B Screen – Identifies carriers of hepatitis B.
HIV Screening – Recommended but can be refused.
VDRL/RPR – Syphilis screening (mandated by law).
Pap Smear (if needed) – Screens for cervical cancer, HPV, herpes simplex type 2.
Urinalysis with Microscopy – Detects protein (preeclampsia), glucose (diabetes), ketones, infection.
hCG (Human Chorionic Gonadotropin) – Confirms pregnancy.
TORCH Screening (Toxoplasmosis, Rubella, CMV, Herpes) – Done if indicated (e.g., history of exposure).
15-22 Weeks (Second Trimester)
Maternal Serum Alpha-Fetoprotein (MSAFP) OR Quad Screen
Low AFP → Possible Down syndrome.
High AFP → Possible Neural tube defects (Spina bifida, anencephaly).
Quad Screen (AFP + hCG + Estriol + Inhibin A) may be used for better accuracy.
24-28 Weeks
1-Hour Glucose Tolerance Test – No fasting required.
>140 mg/dL requires a follow-up 3-hour glucose test.
3-Hour Glucose Tolerance Test (If 1-hour test is abnormal) – Confirms gestational diabetes.
Hemoglobin A1C (if indicated) – Screens for pre-existing diabetes (Normal: <5.9%).
Indirect Coombs Test (if Rh-negative) – Checks if antibodies have developed; if negative, Rhogam is given at 28 weeks.
28 weeks
Rhogam Injection (If Rh-negative & Indirect Coombs Test was negative) – Prevents Rh sensitization.
36-37 Weeks
Group B Streptococcus (GBS) Culture – Vaginal/rectal swab to detect GBS.
If positive → IV antibiotics during labor to prevent neonatal infection.
40+ Weeks (Post-Dates Monitoring)
Non-Stress Test (NST) – Monitors fetal heart rate and movement.
Biophysical Profile (BPP) – Assesses fetal well-being (NST + ultrasound measurements).
Client Education
Health Promotion
Avoid unnecessary medications, supplements, alcohol, tobacco, and illicit substances.
Engage in 30 minutes of moderate exercise daily (walking/swimming) if no contraindications exist.
Avoid hot tubs and saunas due to the risk of overheating and neural tube defects.
Consume at least 8-10 glasses (2.3 L) of water daily.
Recommended Vaccinations
Influenza vaccine is recommended during pregnancy.
Tdap (Whooping cough) should be given between 27-35 weeks; family members should also receive it.
COVID-19 vaccine should be given according to CDC guidelines.
Risk Reduction
Encourage smoking cessation.
Treat existing infections to prevent complications.
Provide genetic testing and counseling if indicated.
Educate on the risks of exposure to hazardous materials.
Preparation for Pregnancy and Birth
Nursing Education Topics
Explain physical and emotional changes during pregnancy and interventions for relief.
Identify warning signs and complications that should be reported.
Discuss available birthing options and pain management choices.
Maternal Psychological Adaptation
Emotional lability, including mood swings, irritability, and tearfulness, is common due to hormonal changes.
Ambivalence about pregnancy is a normal response, often occurring early in pregnancy and resolving before the third trimester. This includes conflicting emotions such as joy, anxiety, and uncertainty.
Teaching Strategies
Use multiple education methods, including pamphlets, videos, and verbal discussions.
Assess the client’s readiness for learning based on their trimester and previous experiences.
Encourage the client to verbalize and demonstrate understanding to ensure knowledge retention.
First Trimester (Weeks 1-12) Key Topics
Physical and emotional changes
Common pregnancy discomforts and relief strategies
Healthy lifestyle habits (exercise, nutrition, stress management, safe sexual practices)
Avoidance of harmful substances (alcohol, tobacco, drugs, unsafe medications)
Warning signs of complications (preterm labor symptoms)
Early fetal growth and development
Importance of prenatal exercise
Routine laboratory testing
Second Trimester (Weeks 13-27) Key Topics
Benefits of breastfeeding
Managing pregnancy discomforts
Healthy lifestyle habits (posture, body mechanics, clothing, seat belt safety, travel)
Recognizing fetal movement
Possible complications (preterm labor, gestational diabetes, hypertension, prelabor rupture of membranes)
Childbirth preparation & education classes
Exploring birthing methods
Birth plan development (verbal or written preferences for labor & delivery)
Third Trimester (Weeks 28-40+) Key Topics
Childbirth preparation
Childbirth classes & birth planning
Coping strategies (breathing, relaxation, counterpressure, effleurage, water therapy, TENS, acupuncture)
Use of heat/cold, massage, aromatherapy
Pain management discussion (natural childbirth vs. epidural)
Role of a doula for labor support
Signs of preterm labor & active labor
Labor process & postpartum care
Fetal Movement & Kick Counts
Count fetal kicks daily to monitor well-being
Less than 3 movements per hour or no movement for 12 hours requires evaluation
Diagnostic Testing for Fetal Well-Being
Non-Stress Test (NST)
Biophysical Profile (BPP)
Ultrasound
Contraction Stress Test
How many kicks per hour requires evaluation?
Less than 3 or none in 12 hours
Diagnostic Testing for Fetal Well-Being
Non-Stress Test (NST)
Biophysical Profile (BPP)
Ultrasound
Contraction Stress Test
Prenatal Education by Trimester
First Trimester (Weeks 1-12)
Key Topics:
Physical and emotional changes
Common pregnancy discomforts and relief strategies
Healthy lifestyle habits (exercise, nutrition, stress management, safe sexual practices)
Avoidance of harmful substances (alcohol, tobacco, drugs, unsafe medications)
Warning signs of complications (preterm labor symptoms)
Early fetal growth and development
Importance of prenatal exercise
Routine laboratory testing
Second Trimester (Weeks 13-27)
Key Topics:
Benefits of breastfeeding
Managing pregnancy discomforts
Healthy lifestyle habits (posture, body mechanics, clothing, seat belt safety, travel)
Recognizing fetal movement
Possible complications (preterm labor, gestational diabetes, hypertension, prelabor rupture of membranes)
Childbirth preparation & education classes
Exploring birthing methods
Birth plan development (verbal or written preferences for labor & delivery)
Third Trimester (Weeks 28-40+)
Key Topics:
Childbirth preparation
Childbirth classes & birth planning
Coping strategies (breathing, relaxation, counterpressure, effleurage, water therapy, TENS, acupuncture)
Use of heat/cold, massage, aromatherapy
Pain management discussion (natural childbirth vs. epidural)
Role of a doula for labor support
Signs of preterm labor & active labor
Labor process & postpartum care
Fetal Movement & Kick Counts
Count fetal kicks daily to monitor well-being
Less than 3 movements per hour or no movement for 12 hours requires evaluation
Diagnostic Testing for Fetal Well-Being
Non-Stress Test (NST)
Biophysical Profile (BPP)
Ultrasound
Contraction Stress Test
Common Discomforts of Pregnancy and Nursing Interventions (First Trimester)
Nausea and Vomiting
Eat dry crackers or toast before getting out of bed.
Avoid an empty stomach, spicy, greasy, or gas-forming foods.
Encourage frequent fluid intake between meals.
Breast Tenderness
Wear a well-supportive bra for comfort.
Urinary Frequency
Empty the bladder frequently.
Reduce fluid intake before bedtime.
Perform Kegel exercises to strengthen pelvic muscles.
Fatigue
Encourage frequent rest periods.
Common Discomforts of Pregnancy and Nursing Interventions (Second and Third Trimester)
Urinary Tract Infections (UTIs)
Wipe front to back after urinating.
Avoid bubble baths and tight-fitting clothing.
Wear cotton underwear.
Drink plenty of water (at least 8 glasses/day).
Urinate before and after intercourse.
Urinate as soon as the urge occurs to prevent bacterial growth.
Notify the provider if urine is foul-smelling, contains blood, or appears cloudy.
Fatigue
Encourage frequent rest periods.
Heartburn
Eat small, frequent meals and avoid an empty stomach.
Avoid spicy or greasy foods.
Sit upright for at least 30 minutes after eating.
Check with the provider before taking antacids.
Constipation
Drink plenty of fluids.
Eat a high-fiber diet.
Exercise regularly.
Hemorrhoids
Use warm sitz baths.
Apply witch hazel pads and topical ointments.
Backaches
Exercise regularly and perform pelvic tilts.
Use proper body mechanics (lift with the legs instead of the back).
Use side-lying positions.
Shortness of Breath & Dyspnea
Maintain good posture and sleep with extra pillows.
Contact the provider if symptoms worsen.
Leg Cramps
Extend the affected leg, keeping the knee straight.
Dorsiflex the foot (toes toward the head).
Apply heat or massage to the muscle while the leg is extended.
Notify the provider if cramping persists.
Varicose Veins & Lower-Extremity Edema
Rest with legs and hips elevated.
Avoid constricting clothing.
Wear support hose.
Avoid prolonged sitting or standing.
Do not cross legs at the knees.
Exercise moderately to stimulate venous return.
Gingivitis, Nasal Stuffiness, & Epistaxis (Nosebleeds)
Brush teeth gently and maintain good oral hygiene.
Use a humidifier.
Use saline nose drops or spray if needed.
Braxton Hicks Contractions
Change positions and walk to see if contractions decrease.
If contractions become regular and increase in intensity, notify the provider.
Supine Hypotension
Avoid lying on the back, as the gravid uterus compresses the vena cava.
Encourage side-lying or semi-sitting positions.
Danger Signs During Pregnancy (First Trimester)
Infection Signs: Burning on urination, diarrhea, fever, or chills
Severe Vomiting: Could indicate hyperemesis gravidarum
Abdominal Cramping and/or Vaginal Bleeding: Could indicate miscarriage or ectopic pregnancy
Danger Signs During Pregnancy (Second and Third Trimester)
Signs of Preterm Labor & Fetal Distress:
Gush of fluid from the vagina: Possible rupture of membranes before 37 weeks
Vaginal bleeding: Possible placental problems (placenta previa or placental abruption)
Abdominal pain: Could indicate preterm labor, placental abruption, or ectopic pregnancy
Decreased fetal movement: Possible fetal distress
Signs of Gestational Hypertension & Preeclampsia:
Severe headaches
Blurred vision
Edema of face and hands
Epigastric pain
Signs of Infection & Other Medical Conditions:
Persistent vomiting (hyperemesis gravidarum)
Elevated temperature
Painful urination (dysuria) (possible urinary tract infection)
Signs of Blood Sugar Imbalance:
Hyperglycemia: Flushed dry skin, fruity breath, rapid breathing, increased thirst, frequent urination, headache
Hypoglycemia: Clammy pale skin, weakness, tremors, irritability, dizziness
Chapter 17: Postpartum Physiological Adaptations
It is important to provide comfort measures for the client during the fourth stage of labor.
This recovery period starts with delivery of the placenta and includes at least the first 2 hr after birth.
Also during this stage, parent-newborn bonding should begin to occur.
The main goal during the immediate postpartum period is to prevent postpartum hemorrhage.
Other goals include assisting in a client’s recovery, identifying deviations in the expected recovery process, providing comfort measures and pharmacological pain relief, providing client education about newborn and self-care, and providing baby-friendly activities to promote infant/family bonding.
QEBP
Determine whether the fundus is firm or boggy. If the fundus is boggy (not firm), lightly massage the fundus in a circular motion.
Enemas and suppositories are contraindicated for clients who have third- or fourth-degree perineal lacerations. Q
Postpartum Key Physiological Changes & Risks
Uterine & Cervical Involution
The uterus contracts and shrinks back to its pre-pregnancy size.
The cervix gradually returns to a closed position.
Lochia Flow (Vaginal Discharge)
A mix of blood, mucus, and uterine tissue expelled after birth.
Vaginal & Ovarian Function Changes
Decrease in vaginal distention.
Return of ovulation and menstruation depends on lactation status.
Cardiovascular, Urinary, Breast & GI Changes
Adaptations in fluid balance, blood volume, and hormone levels.
Hemorrhage (due to uterine atony or retained placenta).
Shock (caused by excessive bleeding).
Infection (such as endometritis, UTIs, or mastitis).
Postpartum period (Puerperium)
Involves both physiological and psychological adjustments.
Time: Between birth and the return of the reproductive system to its nonpregnant state
Traditionally lasts 6 weeks
Postpartum Hormonal Adjustments
After placental delivery, estrogen, progesterone, and placental enzyme insulinase drop, leading to:
Lower blood glucose levels (reversal of pregnancy-induced diabetes effects).
Breast engorgement and increased sweating (diaphoresis) & urination (diuresis) to eliminate excess fluid.
Reduced vaginal lubrication → may cause intercourse discomfort.
Higher muscle tone due to decreased progesterone.
hCG disappears quickly but can be detected for up to 4 weeks postpartum.
Oxytocin's Role Postpartum
Released from the pituitary gland to strengthen uterine contractions.
Breastfeeding stimulates oxytocin, which aids in uterine contraction.
Synthetic oxytocin may be given to enhance uterine tone.
Causes afterpains (painful uterine cramps), especially during breastfeeding.
Human chorionic gonadotropin (hcG)
Hormone produced by the placenta that forms around the embryo during pregnancy
Ovulation & Menstruation Resumption
Lactating Clients:
Elevated prolactin levels suppress ovulation.
Ovulation return depends on breastfeeding frequency, feeding length, & supplementation use.
First postpartum ovulation: ~6 months.
Nonlactating Clients:
Prolactin levels drop to pre-pregnant levels by ~3 weeks postpartum.
First postpartum ovulation: 7-9 weeks postpartum.
Menstruation Resumption: 12 weeks postpartum.
Postpartum Frequency of Assessments
First 2 hours
Blood pressure & pulse → Every 15 minutes (Q15×8)
Temperature → Every 4 hours
After 8 hours:
Temperature → Every 8 hours
Postpartum Assessment: BUBBLE-E
B: Breasts
Check for engorgement, redness, lumps, pain, or cracked nipples.
Assess latch and breastfeeding effectiveness (if applicable).
U: Uterus
Measure fundal height (should decrease daily).
Check uterine firmness → Should be firm, midline, and at or below umbilicus.
A boggy uterus may indicate postpartum hemorrhage.
B: Bowel & GI Function
Assess for constipation, hemorrhoids, and bowel sounds.
Encourage hydration and fiber intake to prevent straining.
B: Bladder
Monitor for urinary retention or burning sensation (UTI risk).
Encourage frequent voiding to prevent uterine displacement.
L: Lochia (Postpartum Bleeding)
Assess COCA:
Color: Rubra (red, 1-3 days), Serosa (pink, 4-10 days), Alba (white, 10-6 weeks).
Odor: Should be mild, foul odor = infection.
Consistency: Clots should be small; large clots may indicate hemorrhage.
Amount: Moderate to light flow; excessive soaking may signal PPH.
E: Episiotomy / Perineum
Check for redness, swelling, bruising (ecchymosis), and proper healing.
Encourage sitz baths and pain management if needed.
Vital Signs & Pain
Monitor temperature, heart rate, respiratory rate, and blood pressure.
Assess pain level and provide appropriate interventions.
Education & Teaching Needs
Educate on breastfeeding, self-care, and signs of complications.
Encourage hydration, ambulation, and emotional support.
H - Homan’s Sign (DVT assessment) (OUTDATED)
Assess for pain, redness, or swelling in the calves
Dorsiflex the foot → If calf pain occurs, it may indicate DVT (Deep Vein Thrombosis)
E - Emotional Status
Monitor for postpartum blues, anxiety, or signs of depression
Encourage open communication about mood, bonding with baby, and support system
Postpartum Laboratory Tests
Complete Blood Count (CBC)
Monitors:
Hemoglobin (Hgb) & Hematocrit (Hct) → Detects anemia due to blood loss.
White Blood Cell (WBC) Count → Elevated levels may indicate infection.
Platelet Count → Monitors clotting ability (important after birth).
Urinalysis
Checks for protein, glucose, and infection indicators (WBCs, nitrites, bacteria).
Detects postpartum complications like UTIs or kidney issues.
(Future Pregnancy Health)
Rubella Immunity Test (If status is unknown)
Why? If the mother is not immune, she may need a rubella vaccine postpartum to protect future pregnancies.
Rh Factor (Blood Type Compatibility)
If the mother is Rh-negative, testing ensures the newborn’s blood type is compatible.
If the newborn is Rh-positive, RhoGAM is given within 72 hours to prevent complications in future pregnancies.
Detects postpartum hemorrhage effects (low Hgb & Hct).
Prevents infections & complications (WBC count & urinalysis).
Ensures future pregnancy health (Rubella & Rh testing).
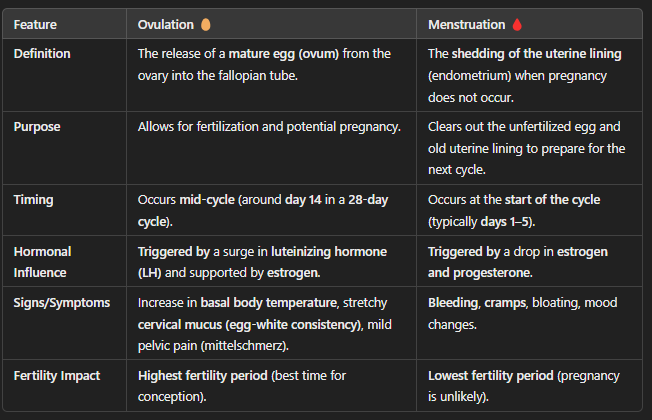
Ovulation vs Menstruation (Table)
The release of a mature egg (ovum) from the ovary into the fallopian tube.
Allows for fertilization and potential pregnancy.
Occurs mid-cycle (around day 14 in a 28-day cycle).
Increase in basal body temperature, stretchy cervical mucus (egg-white consistency), mild pelvic pain (mittelschmerz).
Highest fertility period (best time for conception).
The shedding of the uterine lining (endometrium) when pregnancy does not occur.
Clears out the unfertilized egg and old uterine lining to prepare for the next cycle.
Occurs at the start of the cycle (typically days 1–5).
Bleeding, cramps, bloating, mood changes.
Lowest fertility period (pregnancy is unlikely).
BUBBLE-E vs BUBBLE-HEE Acronym
(Adds two extra assessments!)
Everything in BUBBLE-E, plus:
H - Homan’s Sign (DVT assessment) (OUTDATED)
Assess for pain, redness, or swelling in the calves
Dorsiflex the foot → If calf pain occurs, it may indicate DVT (Deep Vein Thrombosis)
E - Emotional Status
Monitor for postpartum blues, anxiety, or signs of depression
Encourage open communication about mood, bonding with baby, and support system
Uterus (of BUBBLE-HEE): Fundal Assessment & Nursing Care
Assessment Guidelines
Frequency: Every 8 hours after the initial recovery period.
Steps:
Explain the procedure to the patient.
Position the patient supine with knees slightly flexed.
Use gloves and a lower perineal pad to observe lochia during assessment.
Palpation Technique
Use both hands: One above the symphysis pubis for support, the other to palpate the fundus.
NEVER palpate without support to prevent uterine inversion.
Fundal Documentation:
Above umbilicus: +1, U+1, 1/U
Below umbilicus: -1, U-1, 1/U
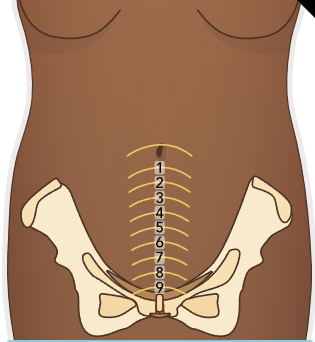
Uterus (of BUBBLE-HEE): Fundal Height Progression
Brief Ascent
Immediately after birth:
Firm, midline, and about 2 cm below the umbilicus.
1 hour post-birth: Rises to umbilical level.
12 hours post-birth: Can be palpated 1 cm above umbilicus.
Gradual Descent
Each 24 hours
Descends 1-2 cm per day.
By day 6: Fundus is halfway between symphysis pubis & umbilicus.
By 2 weeks: No longer palpable in the abdomen.
Uterine Involution (Image)
(Uterine Shrinking)
After birth, the uterus contracts to return to its pre-pregnancy size (involution).
Reduces from 1,000g (immediately postpartum) to 60-80g at 6 weeks postpartum.
Fundal height decreases by 1 cm per day until it is no longer palpable (~2 weeks postpartum).
Uterus (of BUBBLE-HEE): Postpartum Uterine Care
Medications to Promote Uterine Contractions
Oxytocin (Pitocin) - First-line drug
Methylergonovine (Methergine) - Avoid in hypertension
Carboprost (Hemabate) - Avoid in asthma
Misoprostol (Cytotec) - Prostaglandin used to prevent hemorrhage
Additional Nursing Interventions
Encourage early breastfeeding (stimulates natural oxytocin).
Encourage bladder emptying
Prevents uterine displacement.
Monitor for side effects:
Oxytocin & Misoprostol → Hypotension
Methergine & Carboprost → Hypertension
Lochia (BUBBLE-HEE): Assessing Lochia Amount
Amount of blood saturating a perineal pad:
Scant: Less than 2.5 cm / 1 inch (small spot of blood)
Light: 2.5 to 10 cm / 1-4 inch (small stain)
Moderate: More than 10 cm (covers a portion of the pad)
Heavy: One pad saturated within 2 hours
Excessive Blood Loss (Warning Sign!):
One pad saturated in ≤15 min
Pooling of blood under the buttocks
Lochia (BUBBLE-HEE): Assessing Lochia for Normal Appearance
Monitor lochia frequently to check for bleeding changes:
First hour: Every 15 minutes (x8)
Next 4 hours: Every 1 hour
Next 24 hours: Every 4 hours
After 24 hours: Every 4-8 hours, per facility protocol
Lochia flow pattern:
Typically trickles but may flow more steadily during uterine contractions.
Pooling under the client (especially when lying down) may indicate heavy bleeding.
Massaging the uterus or walking may cause a gush of lochia (normal)
Should return to a trickle.
Weighing pads helps estimate blood loss accurately.
Clients who had a C-section will have less lochia
The uterus is cleaned out during surgery.
Monitor for hemorrhage signs (excessive saturation or pooling).
Educate clients on expected vs. abnormal lochia patterns.
Encourage early movement to prevent clot formation
Lochia (BUBBLE-HEE): Abnormal Findings & Nursing Care
Report these findings immediately!
Bright red blood spurting from the vagina
Possible cervical or vaginal tear
Large clots & excessive bleeding (saturating a pad in ≤15 min)
Possible postpartum hemorrhage
Foul-smelling lochia
Infection (endometritis)
Persistent heavy lochia rubra beyond Day 3
Possible retained placental fragments
Lochia serosa or alba lasting too long (beyond expected duration)
Endometritis (inflamed inner lining especially if with fever, pain, or tenderness)
Nursing Interventions
Notify the provider immediately
Assess vital signs (watch for tachycardia & hypotension
Monitor fundal height & firmness
To rule out uterine atony
Encourage frequent bladder emptying
Prevent proper uterine contractions)
Administer prescribed medications (e.g., oxytocin, methylergonovine)
Prepare for possible surgical intervention (D&C for retained placenta)
Client Education
Change pads frequently
Perform hand hygiene after perineal care
Avoid tampons (higher risk of infection)
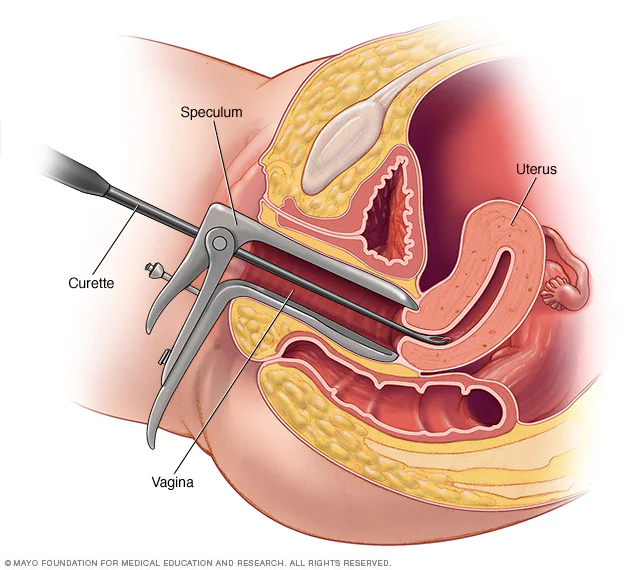
Dilation and curettage (D&C)
Surgical procedure that involves dilating (opening) the cervix and removing tissue from the inside of the uterus (endometrium)
Postpartum Changes: Cervix, Vagina, and Perineum
Cervical
Immediately after birth: Soft, edematous (swollen), bruised, and may have small lacerations
By 2-3 days postpartum:
Shortens, regains its firm shape, and gradually closes
Lacerations can reduce cervical mucus production
The external os shape changes from round to a slit-like opening
Vaginal
Stretched during birth, then gradually returns to prepregnancy size
Reappearance of rugae
folds in the vaginal wall) and thicker vaginal mucosa
Permanent muscle tone loss
Does not fully return to pre-pregnancy state
Breastfeeding mothers may experience increased vaginal dryness & atrophy
Low estrogen levels
Perineal
Redness (erythema) & swelling (edema) common
Especially near episiotomy or laceration sites
Pelvic floor muscles may be weak and overstretched
Hemorrhoids & hematomas may develop
Pressure and pushing during labor
Cervix Anatomy (Image)
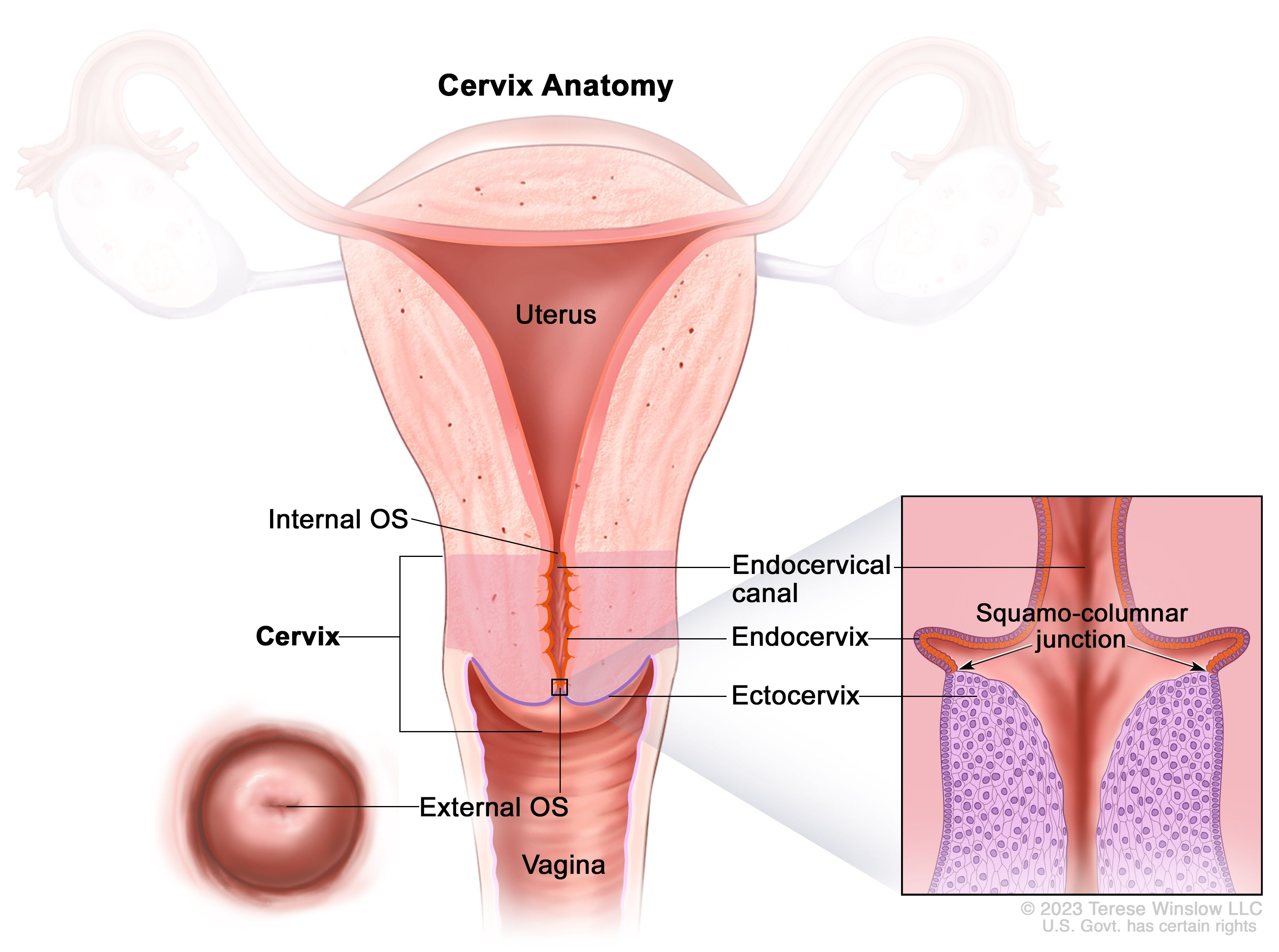
Postpartum Assessment & Care: Cervix, Vagina, and Perineum
Assessment
Monitor perineal healing for:
Redness (erythema), swelling (edema), and hematoma formation
Episiotomy/laceration site for approximation, drainage, bleeding, and healing
Bright red trickle of blood from episiotomy is normal in the early postpartum period
Healing Timeline:
Initial healing: 2 to 3 weeks
Complete healing: 4 to 6 months
Perineal Tenderness, Laceration, & Episiotomy Care
Ice/cold packs for first 24 hours
Reduce swelling and pain (do not apply directly to skin)
Heat therapy (hot packs, sitz baths, moist heat) for circulation & healing
Sitz baths (warm or cool) for 20 minutes, twice a day
Pain relief:
Nonopioid (Acetaminophen) & NSAIDs (Ibuprofen)
Opioids (Codeine, Hydrocodone) for severe pain
Topical anesthetics (Benzocaine spray) & witch hazel pads for pain & hemorrhoid relief
Infection Prevention:
Educate on proper perineal hygiene
Client Education
Wash hands before & after voiding
Use warm water or antiseptic squeeze bottle after each voiding
Blot dry from front to back (urethra to anus)
Avoid rubbing—instead, pat dry gently
Change perineal pad frequently, removing from front to back
Breasts (of BUBBLE-HEE)
Physical Change
Colostrum: Clear yellow fluid produced 2–3 days after birth
Milk Production: Begins 72 to 96 hours postpartum
Engorgement: Breasts become tight, tender, warm, and full due to increased blood flow and lymphatic circulation
Non-breastfeeding clients: Use breast binders, support bras, ice packs, or cabbage leaves to relieve discomfort
Breastfeeding clients: Frequent feedings and proper breast care help manage engorgement
Assessment
Redness (erythema), tenderness, cracked nipples, or mastitis (breast infection with flu-like symptoms)
Proper newborn latch to prevent nipple soreness
Ineffective feeding patterns (related to dehydration, discomfort, or poor positioning)
Patient-Centered Care
Encourage breastfeeding within 1–2 hours after birth
Early & frequent feeding stimulates oxytocin release, which helps with uterine contractions and prevents hemorrhage
Assist with comfortable breastfeeding positions:
Football hold (under the arm)
Cradle hold
Modified cradle hold
Side-lying position
Teach proper latching techniques (baby should take in part of the areola, not just the nipple) to prevent soreness
Clients who do not plan to breastfeed should avoid stimulation and expression of milk
Postpartum Cardiovascular and Vital Sign Changes
Blood loss during childbirth
Vaginal birth: 300–500 mL (~10% of blood volume)
Cesarean birth: 500–1,000 mL (~15–30% of blood volume)
Diaphoresis (sweating) and diuresis (urination): Eliminates excess fluid accumulated during pregnancy
Weight loss of ~19 lb (8.6 kg) occurs within the first 5 days postpartum
Hypovolemic shock is uncommon postpartum because:
The placenta is eliminated, reducing demand for blood flow
The uterus shrinks, redirecting blood back into maternal circulation
Blood Composition
Hematocrit (Hct) decreases for 3–4 days postpartum, then increases to normal by 8 weeks
Elevated white blood cell (WBC) count:
Common range: 20,000–25,000/mm³ (may reach 30,000/mm³)
This is called postpartum leukocytosis, a normal response to prevent infection and aid healing
Coagulation factors and fibrinogen levels remain elevated postpartum
Increases risk for blood clots (DVT, thrombophlebitis)
VS
Blood pressure (BP) remains stable, but a significant increase may indicate preeclampsia
Postural hypotension: Can occur when standing due to fluid shifts—advise sitting at the bedside before standing
Heart rate (HR) can drop to 40 bpm (postpartum bradycardia) within the first 2 days, returning to normal by 6–8 weeks
Elevated temperature up to 38°C (100.4°F) within 24 hours after labor is normal due to dehydration
Persistent fever after 24 hours may indicate infection
Assessment
Monitor cardiovascular and blood changes
Compare postpartum vitals to pregnancy baseline
Check pulses, skin turgor, and assess legs/feet for edema
Inspect lower legs for redness, warmth, swelling (signs of venous thrombosis)
Care
Encourage hydration to prevent dehydration and hypotension
Promote early ambulation to prevent blood stasis and clots
Apply compression stockings/SCDs to high-risk clients for DVT prevention
Administer medications (anticoagulants, pain relief) as needed
Laceration Tears (Image)
Enemas and suppositories are contraindicated for clients who have third- or fourth-degree perineal lacerations.
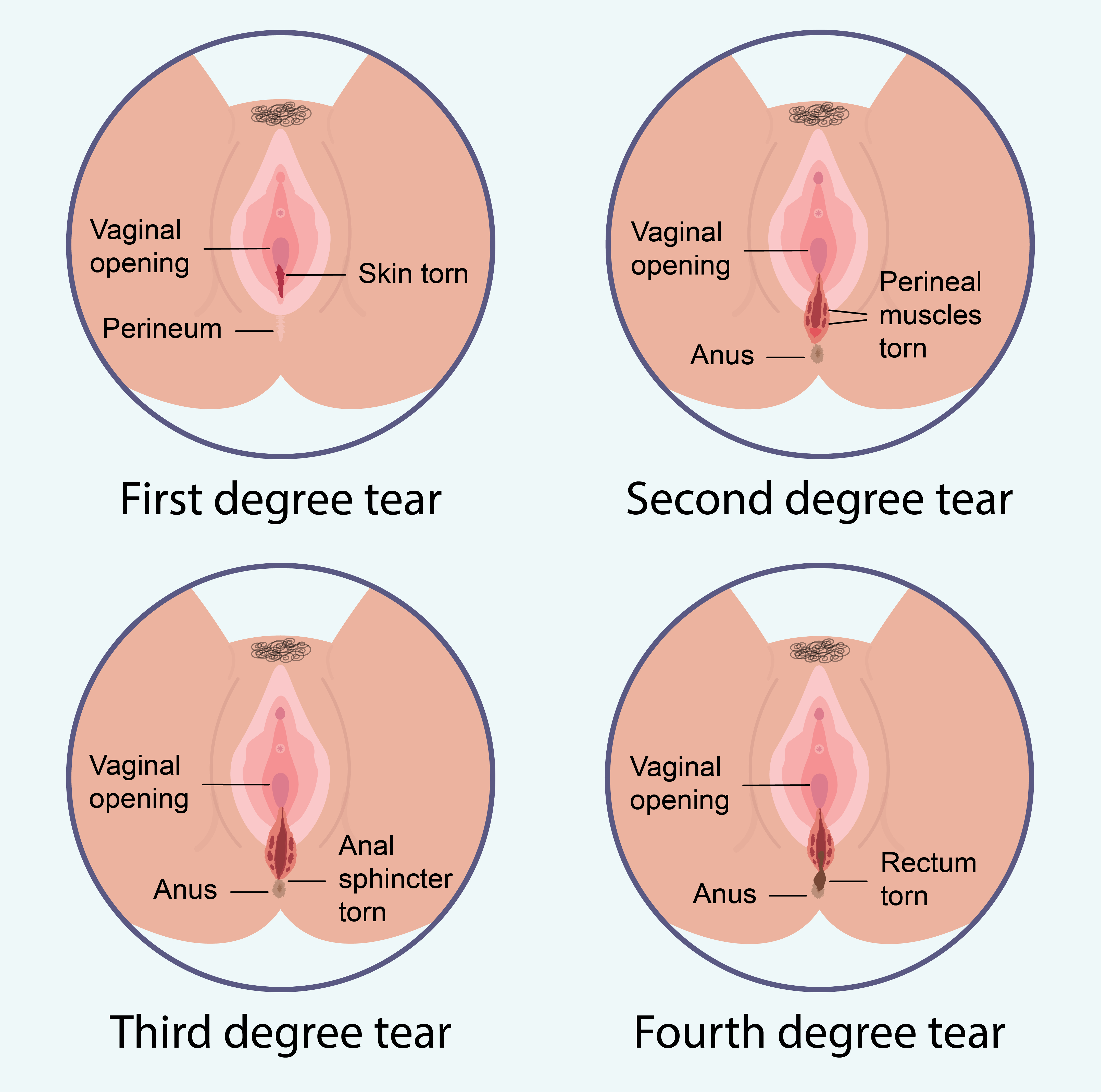
Bowels (of BUBBLE-HEE)
Physical Changes
Increased appetite immediately after birth
Constipation
Decreased peristalsis and muscle tone
Hemorrhoids (common)
From pushing during labor
Assessment
Hunger levels (clients will likely have a strong appetite)
Bowel sounds and function
Delayed bowel movement (2–3 days postpartum) is normal
Muscle tone changes, dehydration, or pain medications
Defecation discomfort
Perineal tenderness, episiotomy, lacerations, or hemorrhoids
Rectal area assessment for hemorrhoids or varicosities
Care
Encourage early ambulation, fluid intake, and high-fiber foods to improve bowel function
Administer stool softeners (docusate sodium)
Prevents constipation
Avoid enemas/suppositories in clients with third- or fourth-degree perineal lacerations
Manage gas pain (common after cesarean birth)
Encourage movement (rocking, walking) to relieve flatus
Avoid gas-producing foods
Anti-flatulent medications may be needed
Urinary (of BUBBLE-HEE)
Changes
Urinary retention may occur
Loss of bladder elasticity, decreased bladder sensation from trauma or anesthesia, and the effects of labor.
A distended bladder can lead to uterine displacement, increasing the risk of hemorrhage and infection.
Postpartum diuresis (increased urine output) typically begins within 12 hours after birth
Helps eliminate excess fluids retained during pregnancy.
Assessment
Check for pain or difficulty urinating due to perineal or urethral swelling.
Assess the elimination pattern
Eecessive urination over 3,000 mL/day is normal for the first 2-3 days
Look for signs of bladder distension, which may include:
Fundal height above the umbilicus or baseline level
Uterus displaced laterally
Visible or palpable bladder bulge
Excessive lochia (postpartum vaginal discharge)
Tenderness over the bladder area
Frequent voiding of less than 150 mL per urination
Can indicate urinary retention with overflow.
Care
Encourage urination within 6-8 hours after birth
If unable to void, catheterization may be necessary.
Promote frequent bladder emptying
Prevents uterine displacement and atony (lack of uterine tone).
Measure the first few voidings to ensure proper bladder emptying.
Encourage oral fluid intake to replace lost fluids and prevent dehydration.
Postpartum Musculoskeletal System
Changes
Joints stabilize and return to their normal state.
Feet may remain permanently increased in size.
Muscle tone begins to restore as progesterone levels drop after placenta delivery.
Abdominal muscles (rectus abdominis) and pelvic muscles (pubococcygeus) regain strength over time.
Assessment
Monitor musculoskeletal changes as the body recovers.
Assess for diastasis recti (separation of the abdominal muscles)
Usually resolves in 6 weeks.
Care
Fall prevention protocol
Client Education
Start with gentle postpartum exercises, gradually increasing intensity.
Delay abdominal exercises for 4 to 6 weeks after a cesarean birth (or follow provider recommendations).
Use proper body mechanics to avoid strain.
Ambulate early to improve circulation and muscle strength.
Perform Kegel exercises to strengthen pelvic muscles.
Postpartum Immune System Considerations
Rubella (MMR Vaccine)
Given postpartum to clients nonimmune to rubella or with a low titer.
Protects future pregnancies from congenital rubella syndrome.
Contraindication: Avoid pregnancy for 4 weeks (28 days) after vaccination.
Rh Factor (Rho(D) Immune Globulin)
For Rh-negative mothers who give birth to an Rh-positive newborn.
Administer IM within 72 hours postpartum to prevent maternal sensitization.
Nursing Considerations:
Check if the client has already been sensitized before administration.
Monitor for allergic reactions for at least 20 minutes post-administration.
Test immunity after 3 months to confirm effectiveness.
Varicella (Chickenpox Vaccine)
Given if the client has no immunity to varicella.
Avoid pregnancy for 1 month after vaccination.
A second dose is administered 4 to 8 weeks later.
Tetanus, Diphtheria, and Acellular Pertussis (Tdap) Vaccine
Recommended for clients who have never received it.
Also recommended for family members and caregivers who will be around the newborn.
Administer before discharge or as soon as possible postpartum.
Safe during breastfeeding.
Rubella (MMR Vaccine)
Given postpartum to clients nonimmune or with a low titer.
Protects future pregnancies from congenital syndrome.
Contraindication
Avoid pregnancy for 4 weeks (28 days) after vaccination.
Rh Factor (Rho(D) Immune Globulin)
For Rh-negative mothers who give birth to an Rh-positive newborn.
Administer IM within 72 hours postpartum to prevent maternal sensitization.
Nursing Considerations:
Check if the client has already been sensitized before administration.
Monitor for allergic reactions for at least 20 minutes post-administration.
Test immunity after 3 months to confirm effectiveness.
Varicella (Chickenpox Vaccine)
Given if the client has no immunity
A second dose is administered 4 to 8 weeks later.
Contraindication
Avoid pregnancy for 1 month after vaccination.
Tetanus, Diphtheria, and Acellular Pertussis (Tdap) Vaccine
Recommended for clients who have never received it.
Also recommended for family members and caregivers who will be around the newborn.
Administer before discharge or as soon as possible postpartum.
Safe during breastfeeding.
Postpartum Comfort & Psychosocial Well-being
Assessment & Interventions
Assess pain related to:
Episiotomy, lacerations, incisions
Afterpains (uterine contractions postpartum)
Sore nipples from breastfeeding
Assess pain location, type, and intensity to tailor interventions.
Administer prescribed pain medications.
Teach nonpharmacological pain relief:
Distraction techniques (e.g., music, imagery)
Heating pads, cold packs
Position changes
Psychosocial Adjustments
Clients may experience a wide range of emotions due to hormonal changes, adjusting to newborn care, and fatigue.
Assessment & Interventions
Encourage verbalization of feelings.
Assess emotional status.
Observe parent-newborn bonding.
Monitor for postpartum blues or depression, which may include:
Decreased appetite
Difficulty sleeping
Decreased social interactions
Lack of communication
Patient-Centered Care
Encourage skin-to-skin contact with the baby.
Document bonding interactions.
Encourage rooming-in (keeping the baby in the client’s room at all times).
Provide emotional support and refer for counseling if needed.
Chapter 18: Baby-Friendly Care
Importance of Bonding
Helps establish emotional connection between parent and baby.
Delaying nursing procedures (e.g., weighing, bathing) during the first hour after birth allows for skin-to-skin contact and early breastfeeding.
Immediate interaction enhances maternal role attainment and helps parents recognize any bonding difficulties.
Factors Affecting Bonding
Maternal Factors
Unwanted pregnancy or adolescent pregnancy
History of depression or previous traumatic birth experiences
Physical recovery challenges after labor
Neonatal Factors
Prematurity (requires NICU care, delaying bonding)
Congenital anomalies (may cause emotional distress)
Difficult birth leading to medical interventions
Social & Cultural Factors
Age and socioeconomic status
Cultural beliefs about newborn care and bonding
Nursing Interventions
Encourage skin-to-skin contact.
Promote breastfeeding within the first hour.
Provide emotional support for clients facing challenges.
Assess for signs of delayed bonding and provide early interventions.
Stages of Maternal Role Attainment
1. Dependent: Taking-In Phase
Duration: First 24 to 48 hours after birth
Characteristics:
Focuses on personal needs such as recovery, rest, and nutrition.
Relies on others for help, including family and nurses.
Excited and talkative, eager to share birth experience.
Processes birth experience to gain closure.
2. Dependent-Independent: Taking-Hold Phase
Duration: Begins on day two or three and lasts ten days to several weeks
Characteristics:
Shifts focus from self to baby care, including feeding, diapering, and bonding.
Wants to take control but still needs reassurance.
Open to learning and seeks guidance.
Can experience baby blues, including mood swings and anxiety.
3. Interdependent: Letting-Go Phase
Duration: Weeks to months postpartum
Characteristics:
Adjusts to new identity as a mother.
Balances family responsibilities and self-care.
Resumes partner intimacy and individual goals.
Nursing Interventions
Provide education on baby care and self-care.
Offer emotional support and assess for postpartum depression.
Encourage bonding activities such as skin-to-skin contact and eye contact.
Validate concerns and reassure the mother about her progress.
Dependent: Taking-In Phase (1 of 3 of Maternal Role Attainment)
Duration: Day 1-2
Characteristics:
Focuses on personal needs such as recovery, rest, and nutrition.
Relies on others for help, including family and nurses.
Excited and talkative, eager to share birth experience.
Processes birth experience to gain closure.
Dependent-Independent: Taking-Hold Phase (2 of 3 of Maternal Role Attainment)
Duration: Day 2/3 to 10 days OR several weeks
Characteristics:
Shifts focus from self to baby care, including feeding, diapering, and bonding.
Wants to take control but still needs reassurance.
Open to learning and seeks guidance.
Can experience baby blues, including mood swings and anxiety.
Interdependent: Letting-Go Phase (3 of 3 of Maternal Role Attainment)
Duration: Weeks to months postpartum
Characteristics:
Adjusts to new identity as a mother.
Balances family responsibilities and self-care.
Resumes partner intimacy and individual goals.
A client in the early postpartum period is very excited and talkative. They repeatedly tell the nurse every detail of the labor and birth. Because the client will not stop talking, the nurse is having difficulty completing the postpartum assessments. Discuss the action the nurse should take.
The nurse should give the client time to express their feelings and recognize that the client is excited about the birth of their baby by giving them the opportunity to discuss the birth. This also helps to develop rapport with the client and allows for therapeutic communication. NCLEX Connection: Health Promotion and Maintenance/Ante-/Intra-/Postpartum and Newborn Care
Positive Indicators of Bonding
The client considers the newborn a family member.
Maintains face-to-face contact and eye contact.
Interprets the newborn’s behavior positively.
Identifies the newborn’s unique characteristics.
Names the newborn, showing attachment.
Maintains physical contact like holding, touching, or skin-to-skin contact.
Provides physical care such as feeding and diapering.
Responds to the newborn’s crying.
Talks, sings, and smiles at the newborn.
Impaired or Absent Bonding Behaviors
Apathy when the newborn cries.
Displays disgust when the newborn voids, stools, or spits up.
Expresses disappointment in the newborn.
Turns away and avoids looking at the newborn.
Does not seek physical closeness.
Does not talk about or acknowledge the newborn’s features.
Handles the newborn roughly.
Ignores the newborn.
Does not refer to the newborn as part of the family.
Views the newborn as difficult or uncooperative.
Signs of Maternal Emotional Challenges
Mood swings, feeling "down," inadequacy, or anxiety.
Frequent crying, flat affect, or withdrawal.
Feeling unable to care for the newborn.
Nursing Interventions for Bonding
Encourage skin-to-skin contact and face-to-face positioning right after birth.
Support rooming-in to provide a quiet environment for bonding.
Promote early breastfeeding initiation and recognition of newborn feeding cues.
Educate on newborn care to improve confidence in parenting.
Encourage parents to interact through cuddling, feeding, bathing, and observing the newborn.
Provide praise, support, and reassurance to guide the client into their parental role.
Encourage parents to express feelings, fears, and concerns about newborn care.
Co-Parent Adaptation
The bonding and role adjustment a non-birthing parent experiences in caring for a newborn.
Engaging in skin-to-skin contact, holding the newborn, and making eye-to-eye contact.
Observing the newborn for similarities to their own features.
Talking, singing, and reading to the newborn
Assessment
Observe bonding behaviors such as holding, talking to, or feeding the newborn.
Assess if the co-parent is actively involved or feeling excluded from newborn care.
Look for signs of emotional distress such as frustration, sadness, or withdrawal.
Nursing Interventions
Provide education on newborn care for both parents.
Encourage a hands-on approach by allowing active participation in caregiving.
Assist in the transition to the parental role by offering guidance and support.
Promote communication between parents regarding their expectations and feelings.
Acknowledge emotions and reassure the co-parent that adaptation takes time.
Transition Phases in Co-Parenting
1. Expectations and Intentions
The co-parent wants to be emotionally and deeply connected with the newborn.
2. Confronting Reality
The co-parent realizes parenting is more challenging than expected.
Common feelings include sadness, frustration, and jealousy if they feel left out of newborn care.
May feel distanced from the birthing parent, who is focused on newborn caregiving.
3. Creating the Role of the Involved Co-Parent
The co-parent actively participates in newborn care and builds confidence.
4. Reaping Rewards
Parental involvement leads to newborn smiles, emotional fulfillment, and a sense of purpose.
Sibling Adaptation
Positive Responses (Indicate Good Adaptation)
Shows interest and concern for the newborn
Demonstrates increased independence
Adverse Responses (Indicate Difficulty in Adaptation)
Displays sibling rivalry and jealousy
Regression in toileting or sleep habits
Aggressive behavior toward the newborn
Attention-seeking behaviors such as whining or clinginess
Nursing Interventions
Familiarization
Take the sibling on a tour of the obstetric unit to introduce them to the newborn’s environment.
Parental Guidance & Involvement
Allow the sibling to be one of the first to see the newborn.
Encourage parents to give a gift "from the newborn" to the sibling.
Suggest dedicated one-on-one time with the sibling while the other parent cares for the newborn.
Allow older siblings to assist in newborn care with simple tasks.
Provide preschool-aged siblings with a doll to simulate baby care.
Chapter 19: Client Education and Discharge Teaching
Discharge teaching is an important aspect of postpartum care. It is important for a client to be able to perform self-care and recognize effects that suggest possible complications prior to discharge.
Discharge planning should be initiated at admission with time spent during the hospitalization on providing client education regarding postpartum self-care.
A nurse should use a variety of teaching strategies to promote learning. Return demonstrations are important to ensure that adequate learning has taken place.
QS
REPORT: Change in vaginal discharge with increased amount, large clots, change to a previous lochia color, such as bright red bleeding, and a foul odo
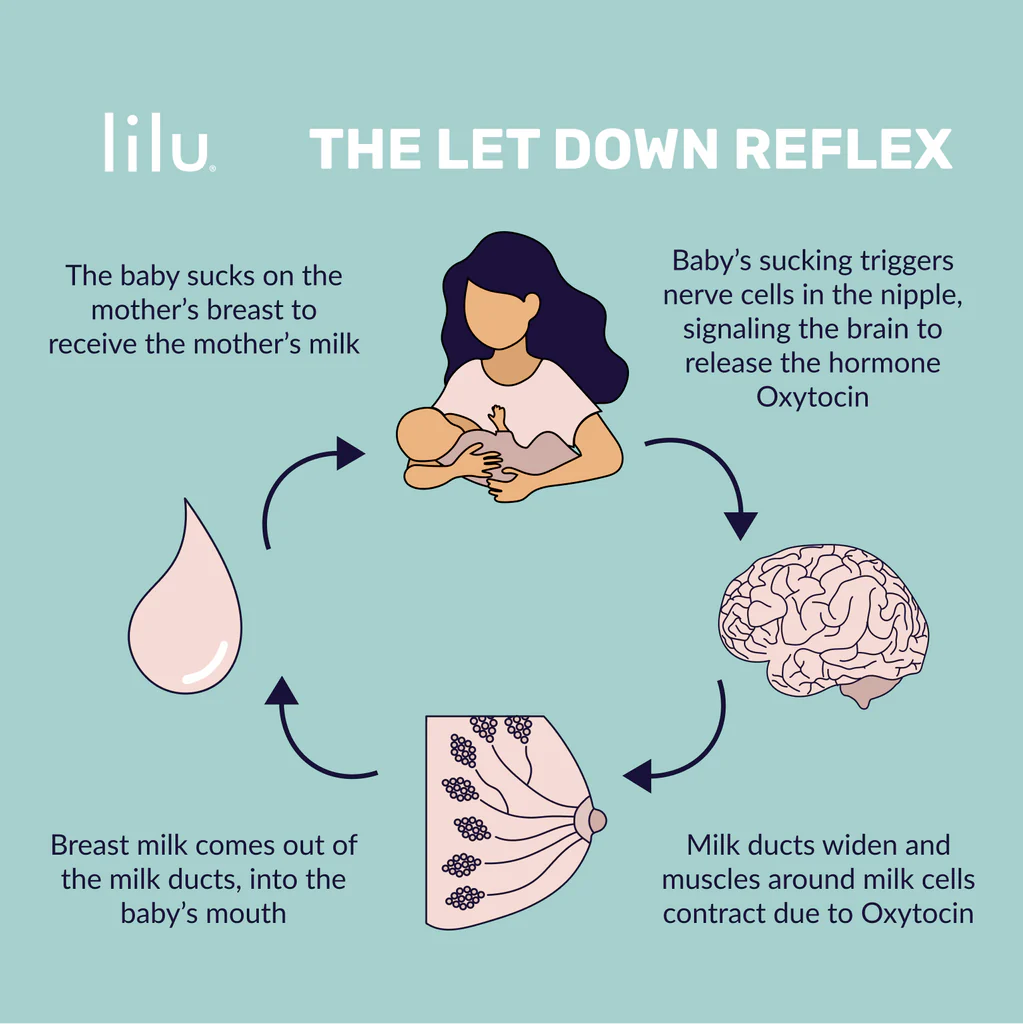
Letdown (Oxytocin) reflex
A physiological response that occurs in lactating women when their baby or a pump stimulates the breast.
Triggers the release of milk from the mammary glands into the milk ducts.
Oxytocin is produced more quickly than prolactin.
It makes the milk that is already in the breast flow for the current feed, and helps the baby to get the milk easily.
Prolactin vs Oxytocin
Signals the body to produce milk
Signals the body to release milk
A nurse is providing discharge instructions to a postpartum client following a vaginal birth with a 4th degree laceration. The client reports leaking urine every time they sneeze or cough. What interventions should the nurse suggest?
The nurse should recommend performing Kegel exercises because they consist of the voluntary contraction and relaxation of the pubococcygeus muscle to strengthen the pelvic muscles. This will assist the client in decreasing urinary stress incontinence that occurs with sneezing and coughing.
NCLEX Connection: Health Promotion and Maintenance, Ante-/Intra-/Postpartum and Newborn Care
Assessing a Client’s Knowledge of Postpartum Care
Evaluate Current Knowledge
Ask about self-care routines and any prior experience with postpartum recovery.
Assess Support System
Identify who will assist the client at home and involve them in education.
Determine Readiness to Learn
Ensure the client can verbalize or demonstrate postpartum care instructions.
Perineal Care
Cleanse the perineal area from front to back after each voiding or bowel movement.
Blot dry from front to back.
Replace perineal pads from front to back to prevent infection.
Breastfeeding Breast Care
Hand Hygiene
Wash hands before breastfeeding to prevent infections.
Client Education
Bra Fit: Wear a well-fitted, nonbinding bra for comfort and support.
Avoid underwire bras (risk of clogged ducts).
Leads to mastitis
Feeding Schedule: 8 to 12 times a day
Breast Engorgement Relief:
Before feeding: Apply warm compresses or take a warm shower to promote milk flow.
After feeding: Use cold compresses to reduce swelling.
Cracked Nipples: Apply prescribed breast creams or wear breast shells to prevent irritation.
Flat/Inverted Nipples: Use breast shells between feedings.
Hydration: Drink plenty of fluids to maintain milk production.
Non Breastfeeding Breast Care
Lactation Suppression
Wear a supportive bra continuously for 72 hours postpartum.
Avoid breast stimulation and warm water over the breasts.
Engorgement Relief
Apply cold compresses (15 minutes on, 45 minutes off).
Use fresh cold cabbage leaves inside the bra to reduce swelling.
Mild analgesics or anti-inflammatory medication can be taken if needed.
Postpartum Activity
Assess the client’s usual activity level to identify tasks that may be strenuous.
Encourage the client to accept help from others when needed.
Teach pelvic tilt exercises
Strengthens back muscles and reduce lower back strain.
These involve arching and straightening the back alternately.
Client Education
Pelvic Floor Strengthening: Perform Kegel exercises to regain pelvic muscle control, as these muscles assist in controlling urination.
Progressive Exercise: Begin with simple movements and gradually increase to more strenuous activities.
After Cesarean Birth:
Avoid strenuous, abdominal exercises, stair use for about 4 to 6 weeks
Stair Climbing Restrictions:
After vaginal birth, limit stair climbing for the first few weeks.
A general guideline: no more than one flight of stairs per day and avoid lifting more than 10 lbs for the first 2 weeks postpartum.
Rest and Recovery: Schedule at least one daily rest period and try to nap when the newborn naps to promote healing.
Postpartum Nutrition
Nonlactating clients
1,800 to 2,200 kcal/day.
Lactating clients
Increase caloric intake by 450 to 500 calories/day
Include calcium-rich foods.
Iron supplements may be prescribed for clients with low hemoglobin and hematocrit levels.
Client Education
Eat a nutritious, balanced diet high in protein for tissue repair.
Continue taking prenatal vitamins for six weeks after birth.
Postpartum Sexual Activity
Safe to resume intercourse within 2 to 4 weeks after birth
If bleeding has stopped and the perineum has healed.
Over-the-counter lubricants may be needed
During the first 6 weeks to 6 months.
Sexual response may be slower and less intense
For the first 3 months postpartum.
Postpartum Contraception
Discuss before resuming sexual activity.
Inform clients that pregnancy can occur even if menses has not returned while breastfeeding.
Client Education
Breastfeeding clients should avoid oral contraceptives until milk production is well established (around 6 weeks).
Nonlactating clients: Menses may not return for 4 to 10 weeks, but ovulation can occur as early as 1 month postpartum.
Lactating clients: Menses may not resume for 6 months or until breastfeeding ends.
Postpartum Signs of Potential Complications
Fever and Chills
Temperature greater than 38° C (100.4° F) for over 24 hours.
Abnormal Vaginal Discharge
Increased amount, large clots, or change in color (e.g., bright red bleeding).
Foul-smelling lochia could indicate infection.
Normal Lochia Flow Patterns:
Rubra: Dark red discharge (Days 1 to 3).
Serosa: Brownish-red or pink discharge (Days 3 to 10).
Alba: Yellowish-white discharge (Days 10 to 8 weeks).
Wound or Incision Complications
Pain from episiotomy, laceration, or incision that does not improve with pain medication.
Foul-smelling drainage, redness, or swelling at the incision site.
Pelvic or Abdominal Pain
Pain or tenderness that does not improve with medication.
Breast Pain or Infection Signs
Localized areas of pain, swelling, or tenderness.
Cracked, red, or bruised nipples, blisters, or fissures.
Leg Pain or Swelling
Calf pain, tenderness, redness, or swelling.
One leg is more swollen, red, or warm compared to the other.
Urinary Tract Symptoms
Pain, burning, frequency, or urgency when urinating.
Mental Health Concerns
Persistent feelings of sadness, anxiety, or apathy toward the newborn.
Difficulty providing self-care or newborn care.
Thoughts of harming self or baby.
Postpartum Discharge Instructions
Follow-up visit should be scheduled within 3 weeks after vaginal or cesarean birth.
Follow-up care should be ongoing and individualized for each client.
The appointment date and time should be written on discharge paperwork and discussed before leaving.
Chapter 24: Nursing Care of Newborns
Newborn care consists of stabilization and/or resuscitation. This can include establishing a patent airway, maintaining adequate oxygenation, and thermoregulation for the maintenance of body temperature. A physical assessment (physical examination, measurements, and monitoring laboratory studies) is done every 8 hr or as needed.
Nursing interventions and family teaching (umbilical cord care, prophylactic measures, newborn screening, newborn feedings and bathing, and fostering baby-friendly activities) are integrated into a newborn’s plan of care.
QEBP
Using the facility’s preferred pain assessment tool, conduct a pain assessment on the newborn with routine assessments and following painful procedures. Q
Newborn hearing screening is required in most states. Newborns are screened so that hearing impairments can be detected and treated early.
Provide family education and promote family-newborn attachment.
The newborn should be warmed slowly over a period of 2 to 4 hr. Correct hypoxia by administering oxygen. Correct acidosis and hypoglycemia.
QPCC
Decreased risk of penile cancer and cervical cancer in female partners (Circumcision)
QS
Identification (using two identifiers) is applied to the newborn immediately after birth by the nurse. It is an important safety measure to prevent the newborn from being given to the wrong parents, switched, or abducted.
Newborns sleep approximately 16 to 19 hr/day with periods of wakefulness gradually increasing. Newborns are positioned supine, “safe sleep,” to decrease the incidence of sudden unexpected infant death (SUID).
Newborn Physical Assessment
Vital signs should be checked frequently per facility protocol.
Daily weight should be measured at the same time using the same scale.
Umbilical cord should be inspected for bleeding and secured to prevent hemorrhage.
Observe periods of reactivity within the first 6 to 8 hours after birth:
First period of reactivity (first 30 min)
Newborn is alert, active, and makes sucking sounds.
Heart rate rises to 160-180 bpm, then stabilizes at 100-120 bpm.
Respiratory rate is elevated.
Period of relative inactivity (lasts 60 to 100 min)
Newborn becomes quiet, rests, and sleeps.
Heart rate and respirations slow down.
Second period of reactivity (2 to 8 hours after birth)
Newborn reawakens, becomes active again.
Gagging and choking on mucus may occur.
Can last from 10 minutes to several hours.
Conduct a pain assessment using the facility’s preferred pain assessment tool.
First period of reactivity (first 30 min after birth) (1 of 3)
Newborn is alert, active, and makes sucking sounds.
Heart rate rises to 160-180 bpm, then stabilizes at 100-120 bpm.
Respiratory rate is elevated.
Period of relative inactivity (lasts 60 to 100 min after birth) (2 of 3)
Newborn becomes quiet, rests, and sleeps.
Heart rate and respirations slow down.