Cardiovascular models
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
Non-clinical drug evaluation
Toxicology, pharmacokinetics, chemistry, safety pharmacology, and pharmacodynamics.
Species selection
Humans average 70 bpm with a 200 ms action potential and 93 mmHg.
Rats around 580 bpm and 111 mmHg.
Dogs around 105 bpm and 128 mmHg.
Mice around 340 bpm and 11 mmHg.
Non-clinical experimental models
Specific methodology applied on a biological system
In vivo: clinical data, animal models
Ex vivo: isolated organs
Ex vivo/in vitro: cellular models
In vitro: molecular models (biochemistry)
Pathological model
Mimic the pathology in experimental models
In vivo: genetic selection, genetic manipulation, administration of a toxic or pharmacological compound, surgery
Ex vivo: an organ from patients or an animal model
Ex vivo/ in vitro: primary cell culture from patients or animal models, cell lines, reprogrammed stem cells (iPS), engineered tissue
In vitro: modified recombinant protein with mutation
Proof of concept
Demonstrate efficacy of the therapeutic strategy in a non-clinical model of the pathology
Then, a 1st trial in humans
Organ perfussion
Driven by arterial blood pressure (Pa)
Right heart: low-pressure system
Left heart: high-pressure system

Blood pressure
Systolic pressure (120 mmHg, when blood is ejected into arteries)
Diastolic pressure (80 mmHg, pressure between heartbeats)
Hemodynamics recording (BP recording)
Invasive: catheterism
Non-invasive: sphygmomanometer
Catheterism
Advantages: direct mesurement, collection of blood samples
Limits: anesthesia may be required (influence heart rate and blood pressure), risk of complications: thrombosis, infection
Sphygmomanometer
Advantage: recording in vigil (non-anesthetized) animals
Limit: indirect mesurement
Catheterism method
Placing a fluid-filled catheter into an artery, connected to a pressure transducer.
Generates an arterial pressure trace providing systolic, diastolic, mean arterial pressure, pulse pressure, and heart rate.
Measure specific pressures, such as right ventricle systolic pressure in nicotine-exposed mice.
Tail cuff method (CODA system)
Tail-cuff placed on the tail to occlude the blood flow. Upon deflation, one of several types of noninvasive blood pressure sensors, placed distal to the occlusion cuff, can be used to monitor the blood pressure.
Animals are vigil.
Necessitates a habituation period (generally 5 consecutive days, with “real” measurement on day 6-7)
Limit: provides with a snapshot of BP value; no long-term monitoring
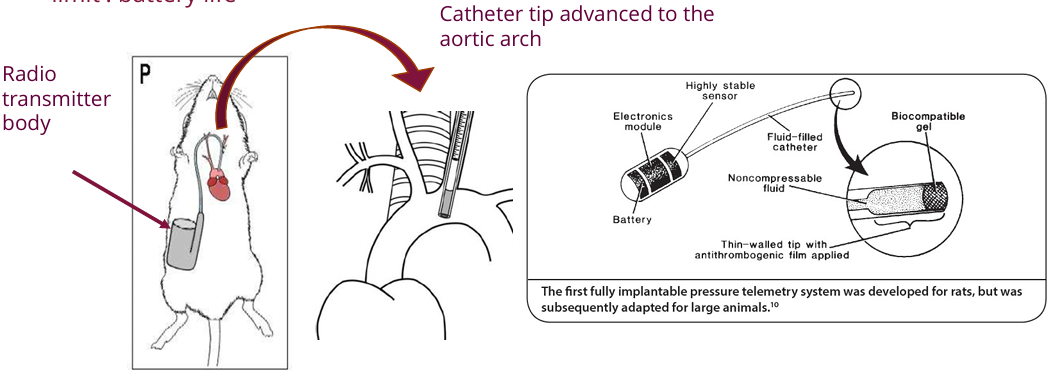
Radiotelemetry
Implanting a pressure probe and transmitter.
It allows for direct, continuous monitoring of blood pressure and circadian rhythms in conscious, free-moving animals
Limited by battery life.
Experimental designs using this method must carefully control treatment timing, doses, and positive controls.
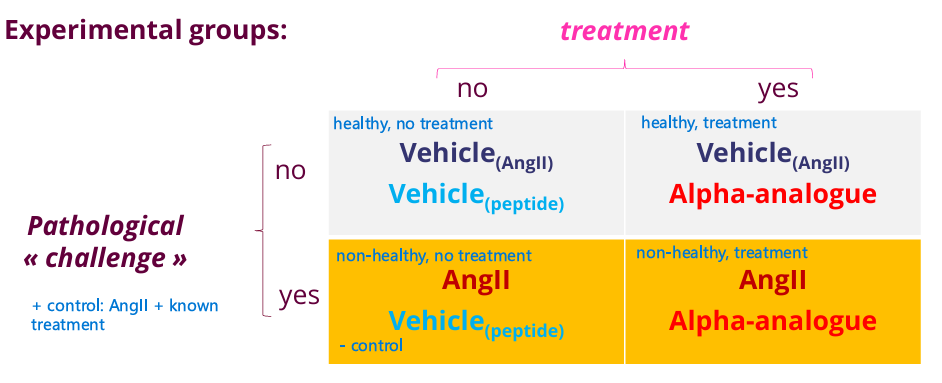
Experimental design
5 experimental groups
Treatment parameters: dose, route, frequency, vehicle, timing
Echocardiography
Non invasive technique to explore cardiac morphology and function using ultra sounds
A probe emits ultrasounds at high frequency (15-40 MHz) toward the organs
The probe receives back the echoes, which are translated in electrical signal and amplified.
Used for morphological exploration of the heart chambers and large vessels
Conducted on anaesthetized, unconscious animals (typically using isoflurane, a gaseous anaesthetics)
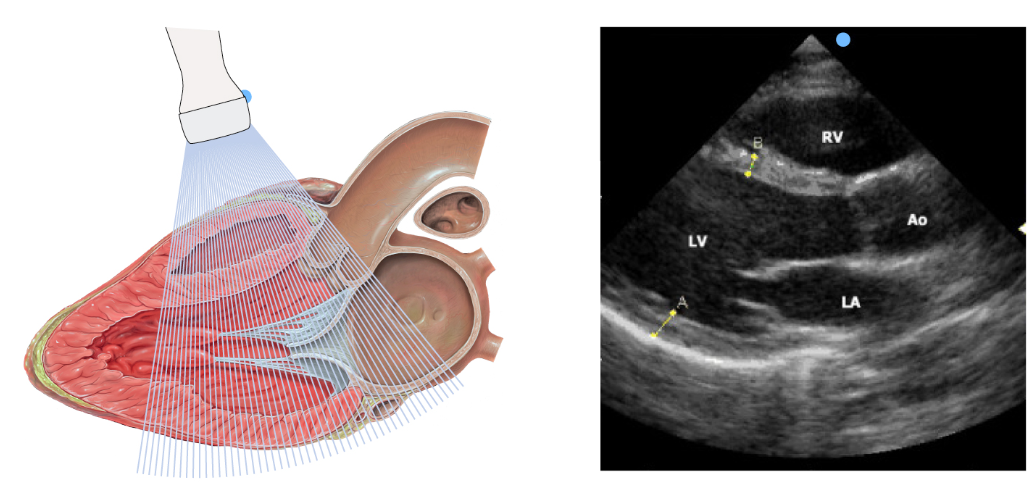
Echocardiography B-mode
2D morphological images to measure dimensions and calculate left ventricle (LV) volumes, LV mass, stroke volume, ejection fraction, and cardiac output.
Echocardiography M-mode
Motion mode displays the movement of the anterior and posterior walls over time, used to measure LV internal diameters during systole and diastole.
Echocardiography Doppler-mode
Uses pulse wave and color Doppler to visualize blood flow velocity, which serves as a crucial indicator of diastolic function
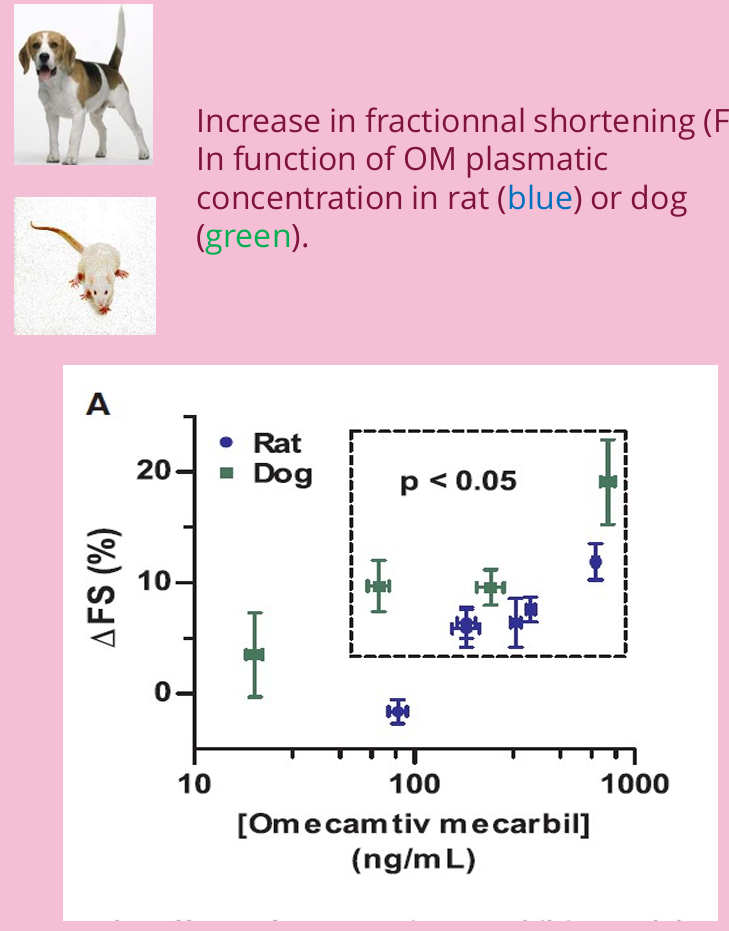
Echocardiograms uses
Measure the effects of inotropic drugs, like omecamtiv mecarbil, which increases fractional shortening in rats and dogs.
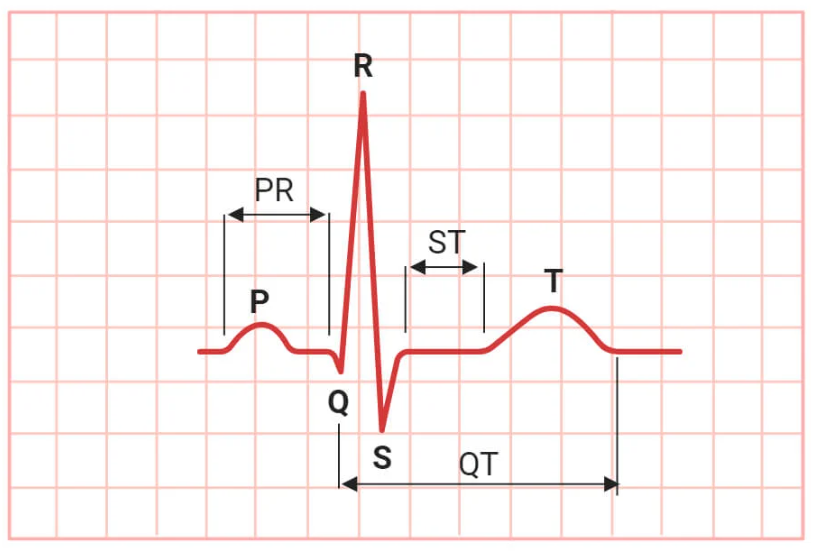
Electrocardiogram
Maps the heart's electrical pathways.
P wave represents atrial depolarization
QRS complex represents ventricular depolarization
T wave represents ventricular repolarization
ECG Recording
External electrodes or implanted radiotelemetry
Yields data on heart rate, arrhythmias, and ischemia

Safety pharmacology
Before human trials, investigates the potential unwanted effects of a drug at therapeutic and supra-therapeutic doses
A core battery of tests evaluates the central nervous system, respiratory function, and cardiovascular function, with a heavy emphasis on arrhythmogenic potential
Long QT syndrome
A slower cardiac action potential repolarization leads to a prolonged QT interval on an ECG
Trigger "Torsades de pointes" (a dangerous arrhythmia) and sudden death
Can be inherited or drug-induced (iatrogenic) by pharmacological inhibition of the hERG K+ channel, which blocks the repolarizing potassium efflux
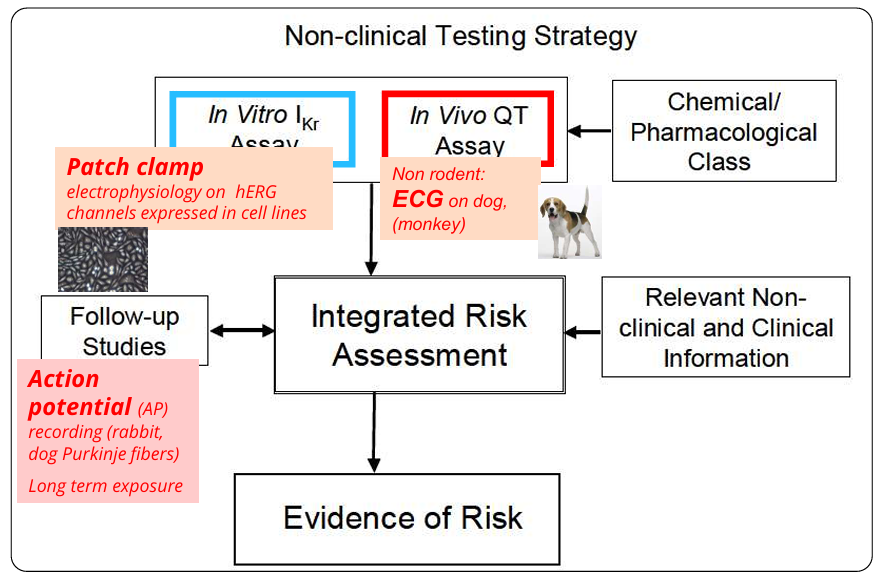
ICH S7B Guidelines
Risk evaluation of ventricular repolarization
Arterial hypertension
Hypertension is defined as systolic blood pressure > 140 mmHg and/or diastolic > 90 mmHg
Affects 30–45% of adults globally
Major risk factor for cardiovascular and renal events, ischemic heart disease, and stroke
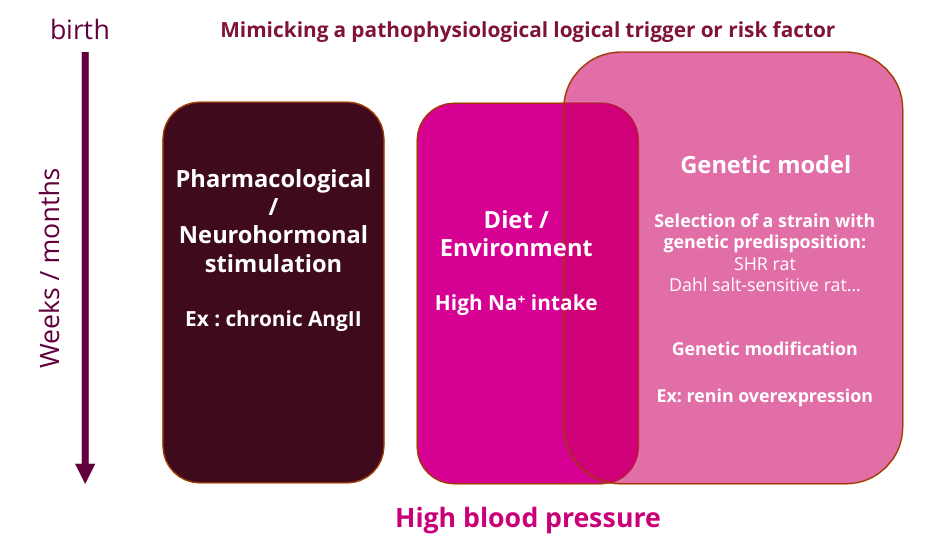
Models for arterial hypertension
Mimic this pathology using genetic selection, neurohormonal stimulation, dietary changes, or genetic manipulation
Spontaneous hypertensive rat (SHR)
Genetic model of hypertension that naturally develops chronic hypertension leading to left ventricular hypertrophy and ultimately heart failure over a period of two years
Hypertensive development begins around 5–6 weeks of age, reaching systolic pressures between 180 and 200 mmHg in the adult age phase.
Starting between 40 and 50 weeks, SHR develops characteristics of cardiovascular disease, such as vascular and cardiac hypertrophy
Control: Wistar-Kyoto rats
Stroke prone SHR (SHRSP)
Further development of SHR that has even higher blood pressure than SHR and a strong tendency to die from stroke
80% in males, 60% in females
Extensive arteriosclerosis
Control strain: Wistar Kyoto
Dahl salt-sensitive rat model
An inbred strain that develops hypertension and heart failure when exposed to high-salt diets, characterized by metabolic disturbances such as insulin resistance and dyslipidemia
Suppressed plasma renin activity (due to high Na reabsorption), low aldosterone
Diastolic heart failure, nephropathy
Control strain: normal rat, with a high salt diet
Mimics salt-sensitive HT in patients
Transgenic hypertension model
Transgenic rats, overexpression of a gene involved in BP regulation
TGR(mREN2)27 transgenic rat, resulting in severe hypertension
Double transgenic: human renin and angiotensinogen. Test antihypertensive effect of the human renin inhibitor
Advantage of studying conscious animals
Anesthetics actively influence and alter fundamental cardiovascular parameters, including heart rate and blood pressure
Studying conscious, "vigil" animals provides a much more accurate, unconfounded picture of the animal's true physiological baseline and the actual pharmacodynamic effects of the drug over an extended period
Important parameters to be examined to explore the effect of a drug on the cardiovascular system
Blood pressure: via catheter or tail cuff, asses wether a drug is a vasodilator (lowers BP) or a vasoconstrictor (raises BP)
Heart rate: via pressure tracing or electrocardiogram (ECG). Determine if a drug causes dangerous tachycardia (abnormally fast) or bradycardia (abnormally slow)
QT interval: via ECG. Total time for ventricular depolarization and repolarization. Prolongation of the intervals indicates a risk of fatal arrhythmias
Ejection fraction (EF) / stroke volume (SV): in vivo echocardiography. Evaluates drugs’ inotropic effect (how strongly it impacts the heart muscle’s ability to contract).
SV: amount of blood pumped per beat
EF: percentage of the blood the left ventricle pumps out with each contraction
Cardiac repolarization tests
Patch clamp: electrophysiology to study the drug's effect directly on specific ion channels expressed in cell lines
ECG: check for a prolongation of the QT interval or the onset of arrhythmias