cells to organisms lecture mcq 2
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
71 Terms
negative feedback
to return a variable to a normal range (eg temperature regulation, blood glucose regulation)
Positive feedback
amplifies a stimulus and only contributes to homeostasis in animals in a small number of functions (childbirth, blood clotting, electrical impulses in nerves)
feedforward
anticipatory responses to expected change (eg increased heart rate in anticipation of exercise; increased secretion of insulin before food is digested to yield glucose; stimulation of gastric secretions due to thought/smell of food)
homeostasis
Maintaining a relatively constant internal environment (steady state) in the face of dynamic change
endocrine versus nervous signalling

interaction and cooperation examples between endocrine and nervous sytems
1. Some nerves innervate endocrine glands eg.adrenal glands
2. Hypothalamus and pituitary are brain regions that regulate endocrine function
3. Blood pressure is regulated by nerves acting on the heart and blood vessels and by hormones acting on the kidneys to regulate blood volume
4. Glial cells (including immune cells) in nervous system play an important role in nervous function
role of sensory receptors
transduce stimulus energy and transmit signals to the central nervous system: complex processing of sensory information to build percepts
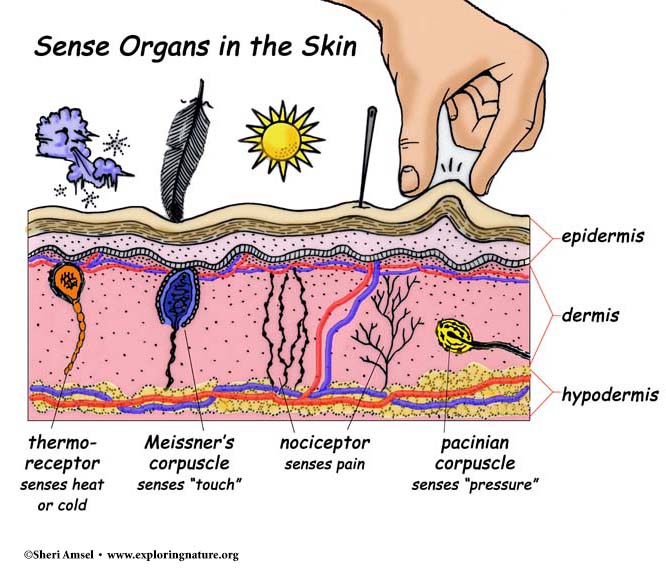
order of sensory processing
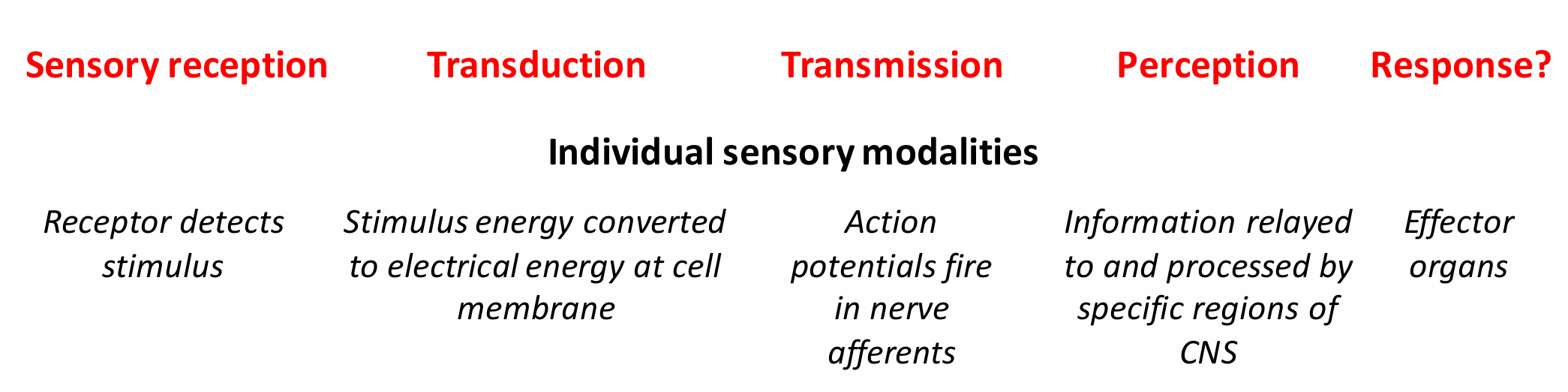
describe how information is relayed and processed regarding PNS and CNS
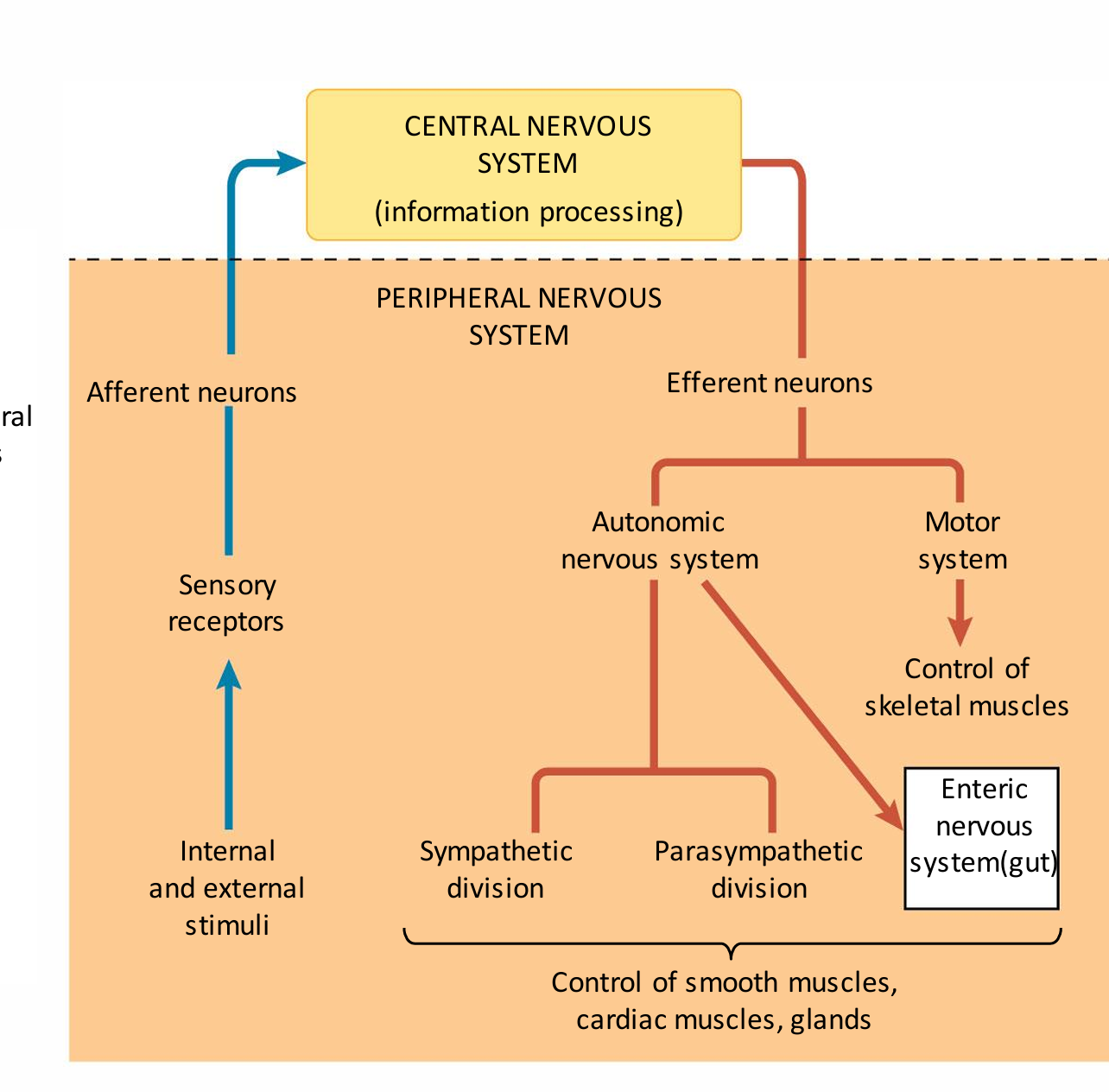
what is cerebrospinal fluid
surrounds the brain and spinal cord and fills the ventricles. It is modified blood plasma
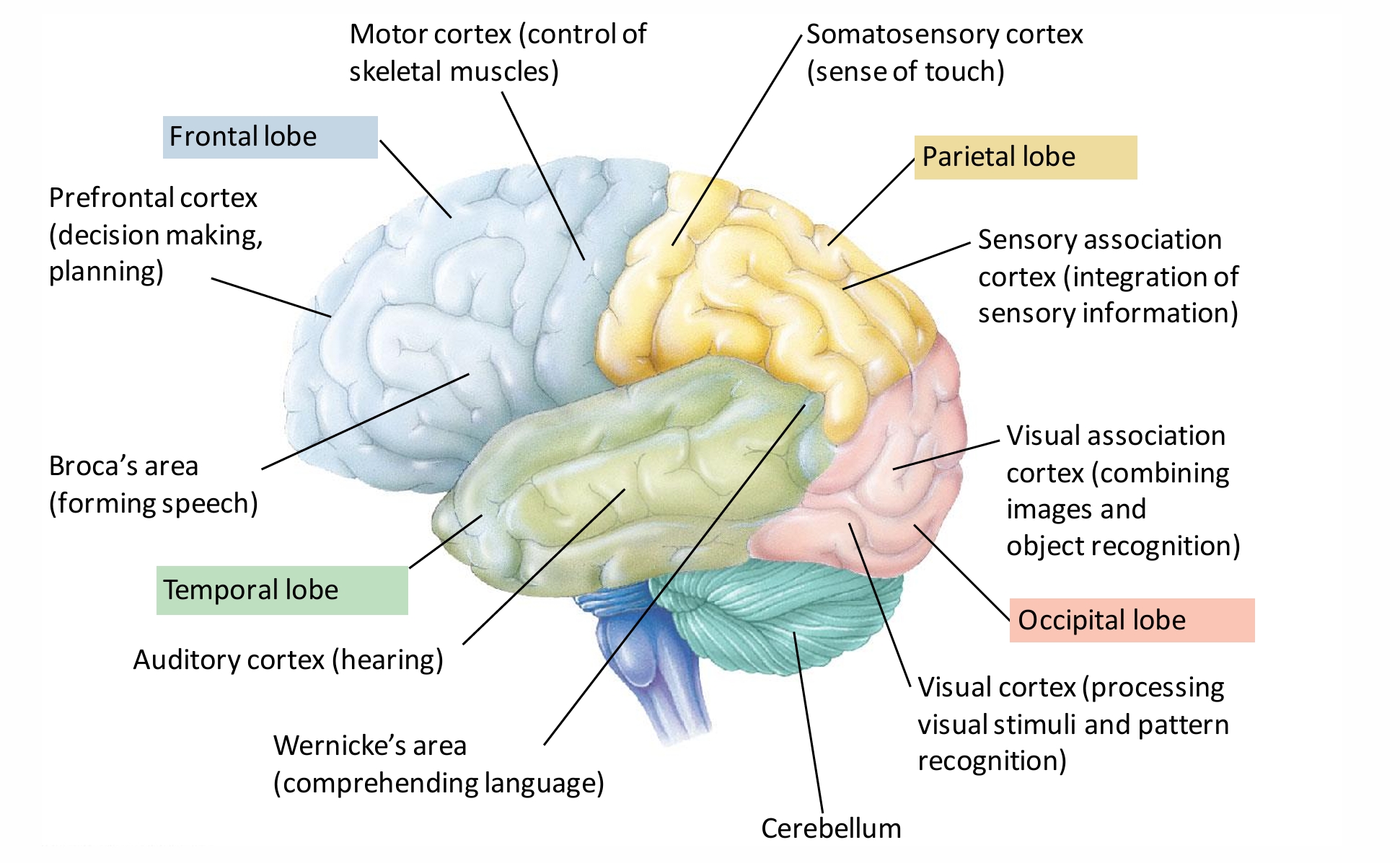
grey and white matter in the brain
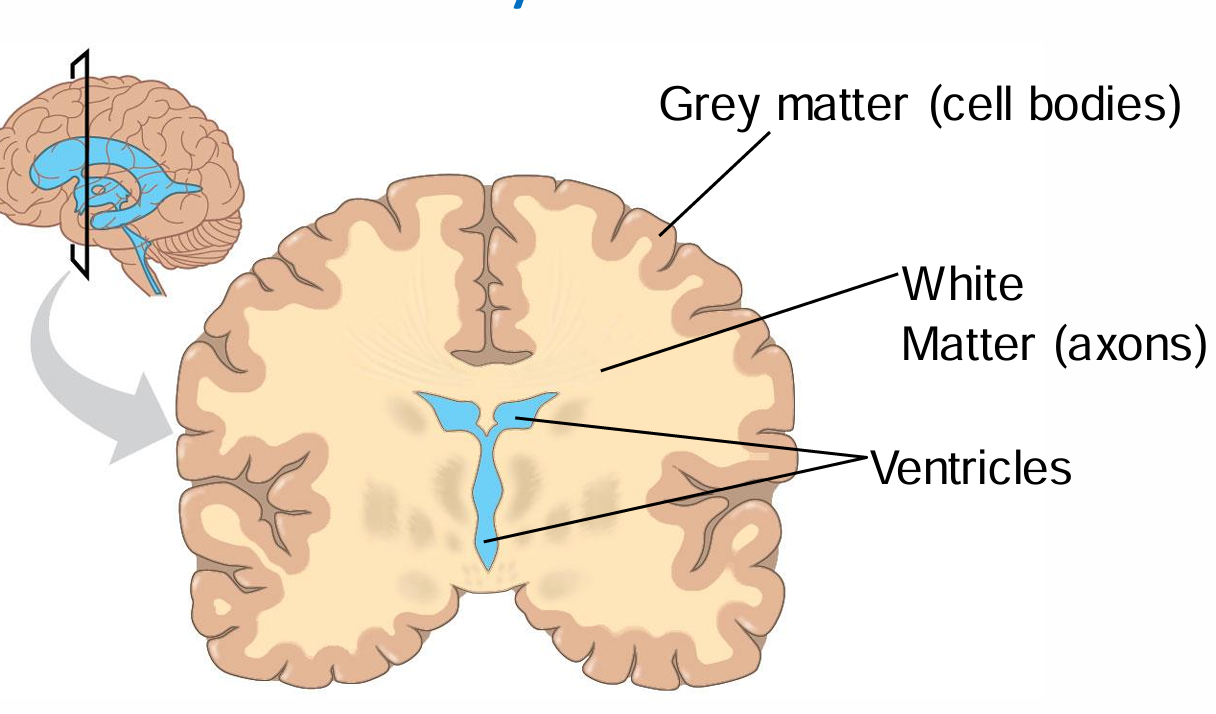
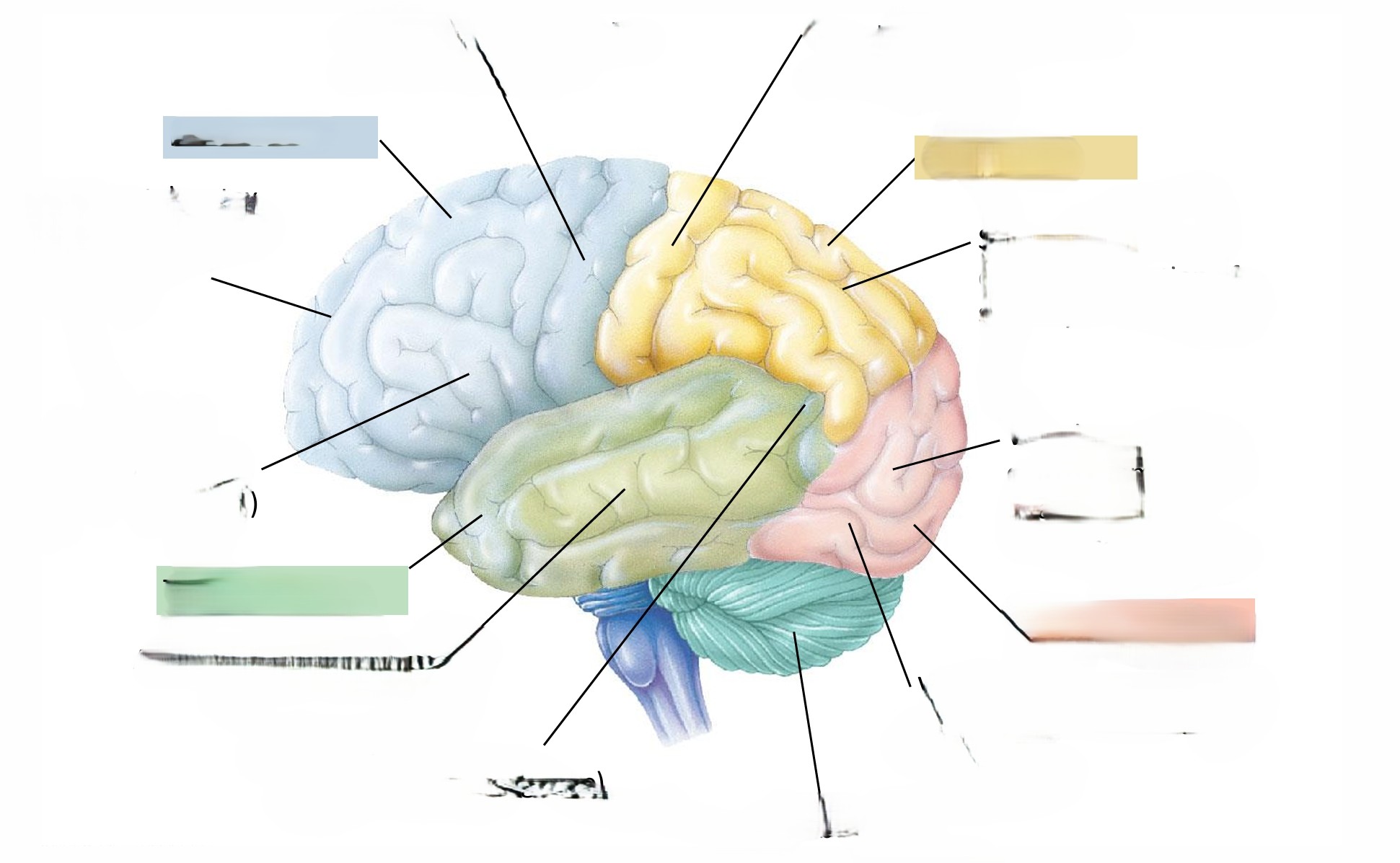
fill in the blank
function of the spinal cord
Neuronal link between brain and PNS Integrating center for spinal reflexes
31 pairs of spinal nerves emerge from spinal cord through spaces formed between vertebrae
what happens at the synapse
neurotransmittersdiffuse short distances and bind to receptors on target cells
what are NTs supported by
glia
visceral afferent versus sensory afferent
Visceral afferent: Incoming pathway for information from internal viscera (organs in body cavities)
Sensory afferent: Somatic (body sense) sensation: arises from body surface and proprioception(touch, pain, orientation of body and limbs)
what are the two efferent components of the PNS and their functions
the motor system : carries signals to skeletal muscles and is mainly voluntary (though note reflexes and also eg diaphragm in breathing
the autonomic nervous system: regulates smooth and cardiac muscles and is generally involuntary
the enteric: exerts direct control over the digestive tract, pancreas, and gallbladder
the autonomic nervous system has→
sympathetic division regulates arousal and energy generation (“fight-or-flight” response)
parasympathetic division has antagonistic effects on target organs and promotes calming and a return to “rest-and-digest”functions
describe the autonomic nerve pathway
Extends from CNS to an innervated organ
Two-neuron chain Preganglionic fiber (synapses with cell body of second neuron) Postganglionic fiber (innervates effector organ)
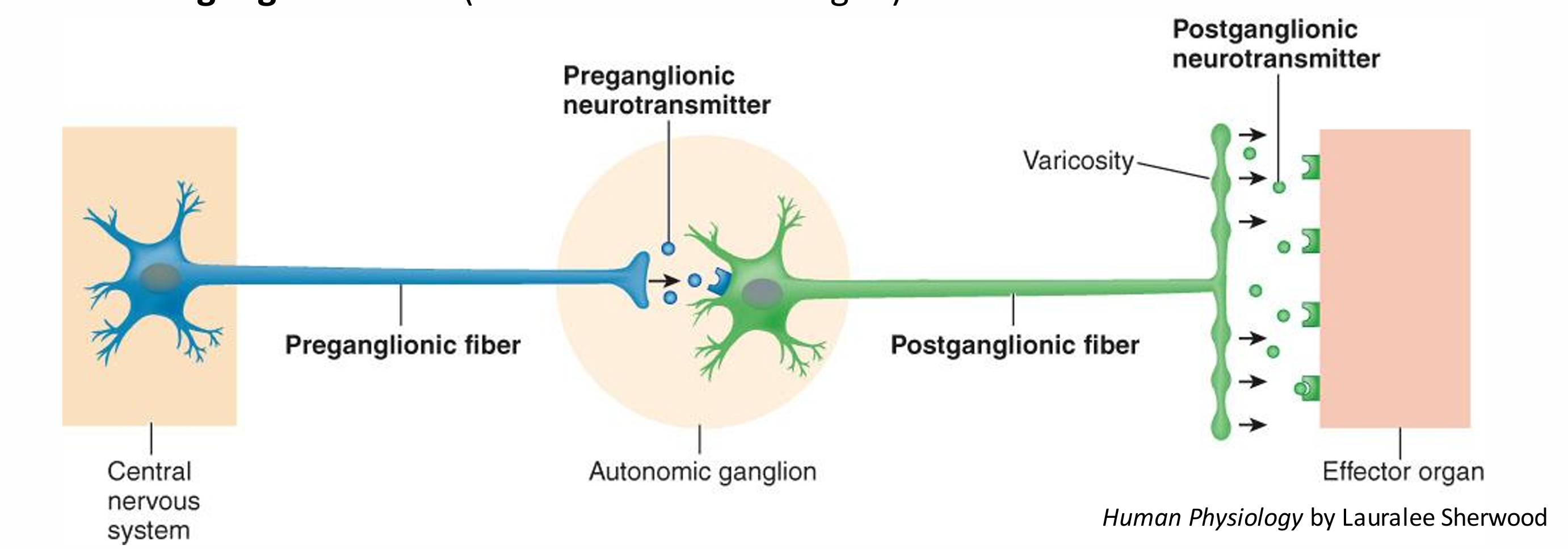
what is a ganglion
a collection of cell bodies in the peripheral nervous system The equivalent in the CNS is a nucleus
what are visceral organs innervated by
Most (but not all) visceral organs are innervated by both sympathetic and parasympathetic fibers (eg sweat glands only receive sympathetic innervation)
In general produce opposite effects in a particular organ
Dual innervation of organs by both branches of ANS allows precise control over organ’s activity
what does an increase in action potential frequency cause
Increase frequency: more neurotransmitter released: bigger effect on target cell
function of motor neurons
Motor neurons are final common pathway by which various regions of CNS exert control over skeletal muscle activity– areas include spinal cord, motor regions of cortex, basal nuclei, cerebellum, and brain stem
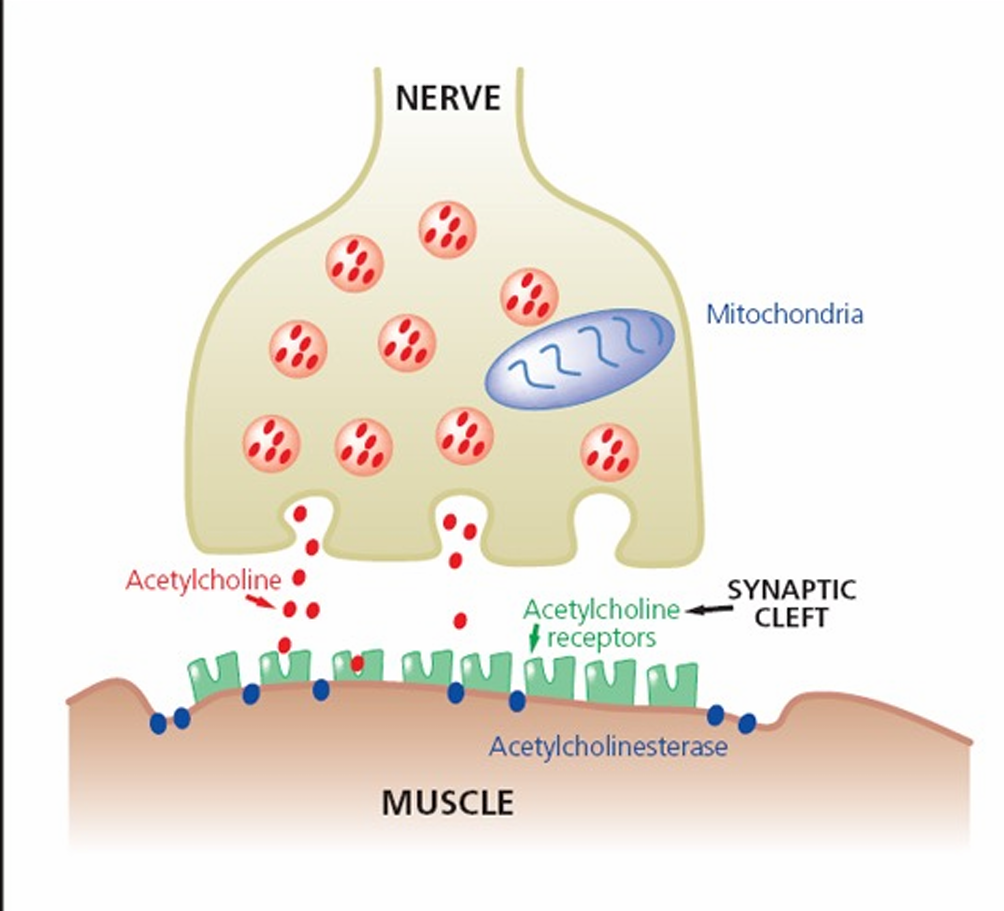
Acetylcholinesterase
inactivates ACh, ends the end-plate potential and the action potential and resultant contraction
Ach at the neuromuscular junction(NMJ)
nicotinic ie respond to nicotine
When ACh receptors are activated, ion channels open allowing influx of current and depolarization of cell (end-plate potential)
chemical agents NMJ is susceptible too
Black widow spider venom causes explosive release of ACh: prolonged depolarization: respiratory failure
Botulinim toxin (C. Botulinim) blocks release of ACh: causes flaccid paralysis Food poisoning; Medical use; Cosmetic use.
Curare blocks action of ACh at receptor sites (antagonist, competitive with ACh). Used as an arrow poison by indigenous peoples of S. America
Organophosphates (eg Sarin) prevent inactivation of ACh– lung muscle paralysis – death by suffocation. Used as chemical weapons
two neurotransmitters involved in autonomic nervous signaling
epinephrine=adrenaline and norepinephrine=noradrenaline
differences in NT release between sympthatic and parasympathetic
Sympathetic: ACh secreted from pre ganglionic; NAd secreted from post ganglionic Also causes release of Ad from adrenal gland
Parasympathetic: ACh released from both pre ganglionic and post ganglionic neurons
types of cholinergenic receptors
bind ACh
Nicotinic receptors– found on postganglionic cell bodies of all autonomic ganglia
Muscarinic receptors– found on effector cell membranes
Andrenergic receptors
bind noradrenaline and adrenaline
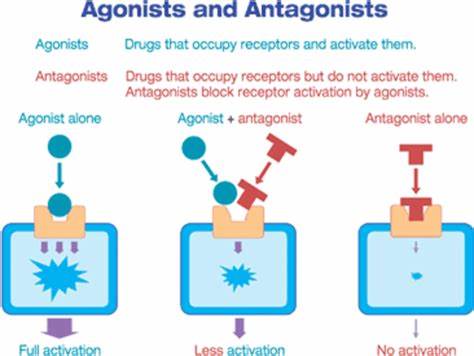
receptor agonists versus antagonists
Receptor agonists: Bind to same receptor as neurotransmitter Elicit an effect that mimics that of neurotransmitter
Receptor antagonists: Bind to receptor Block neurotransmitter’s response
Regions of CNS Involved in Control of Autonomic Activities
prefrontal cortex through its involvement with emotional expression characteristic of individual’s personality
Hypothalamus plays important role in integrating autonomic, somatic, and endocrine responses that automatically accompany various emotional and behavioral states
Medulla within brain stem is region directly responsible for autonomic output
Some autonomic reflexes, such as urination, defecation, and erection, are integrated at spinal cord level
bronchodilator
Eg salbutamol (β2-adrenergic agonist) β2-adrenergic receptors are predominant receptors on bronchial smooth muscle
Physiology: Sympathetic nerves innervate bronchial smooth muscle When they release NAd (eg during exercise): bronchioles widen, making it easier to breathe Bronchodilator drugs act on these receptors to mimic the effect of endogenous neurotransmitter, widening bronchioles and making it easier to breathe
metoprolol
n anti-hypertensive: blocks β1 adrenergic receptors in heart muscle cells ‘β-blocker’ class of drugs
Physiology: sympathetic nerves speed up heart rate β-blockers block the effects of sympathetic nerves, decreasing heart rate and helping to lower blood pressure
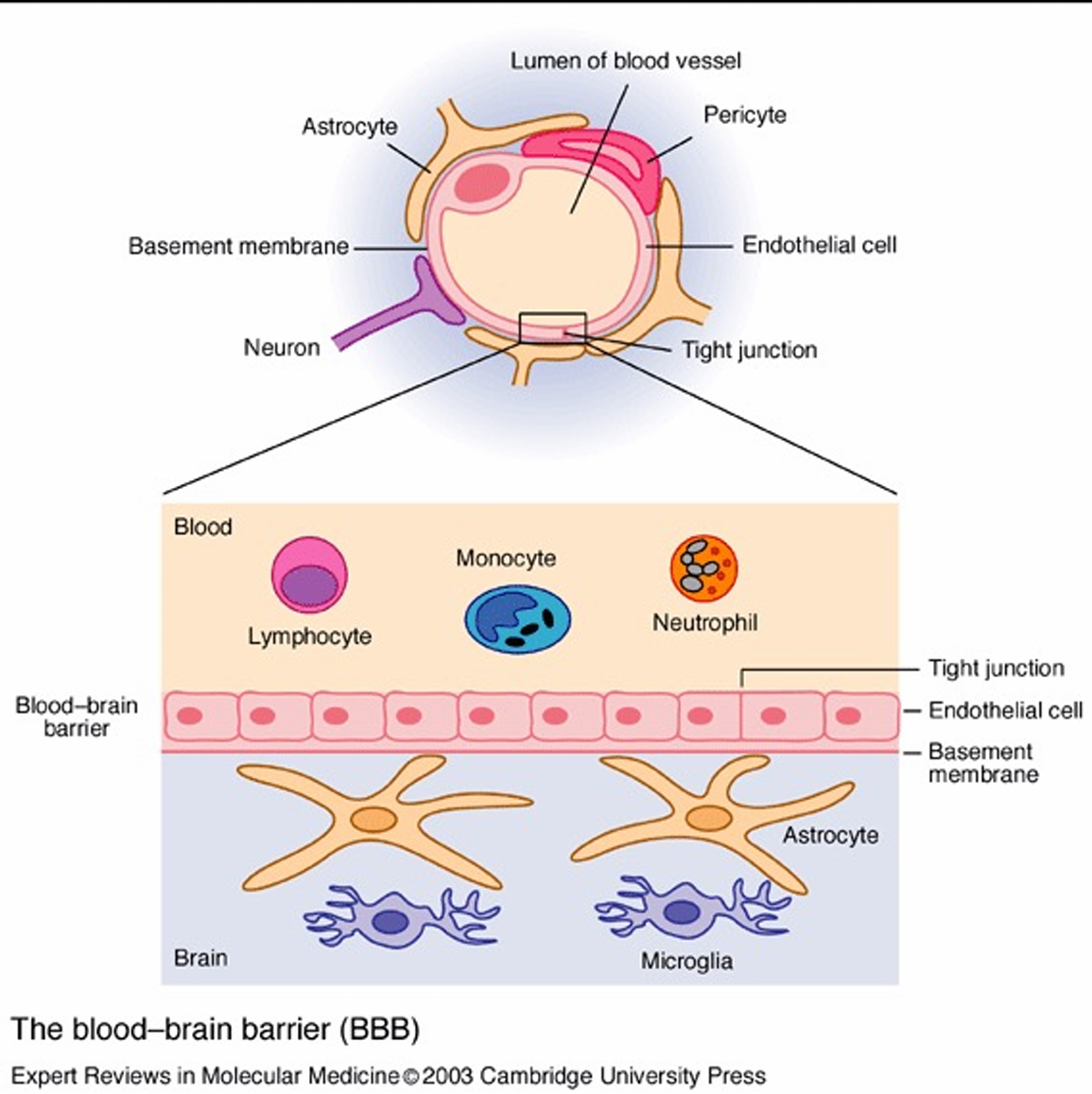
describe the blood brain barrier
Tight junctions between endothelial cells lining cerebral blood vessels Specific arrangement of glial cells Prevents easy passage of large macromolecules and pathogens between the circulation and the brain
effects of serotonin being complex

what is muscle activity a response to
input from the nervous system '
Muscle cell contraction relies on the interaction between thin filaments, composed mainly of actin, and thick filaments, staggered arrays of myosin
what does the skeleton provide for muscles
a rigid structure to which muscles attach
what are muscle composed by
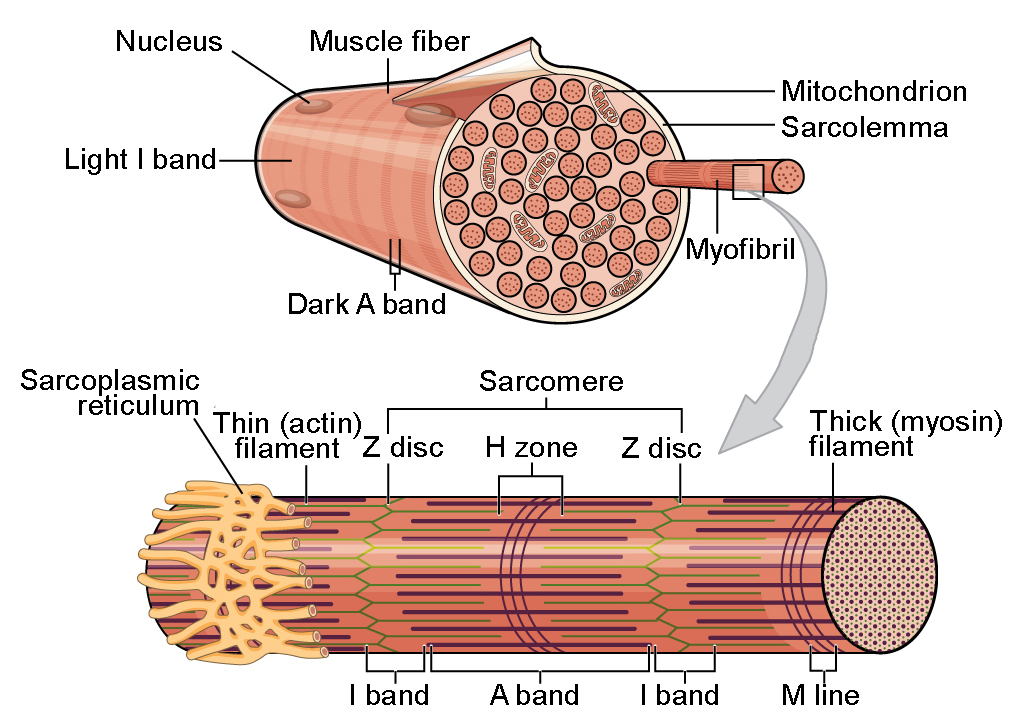
A skeletal muscle consists of a bundle of long fibres, each a single cell, running along the length of the muscle
Each muscle fiber is itself a bundle of smaller myofibrils arranged longitudinally
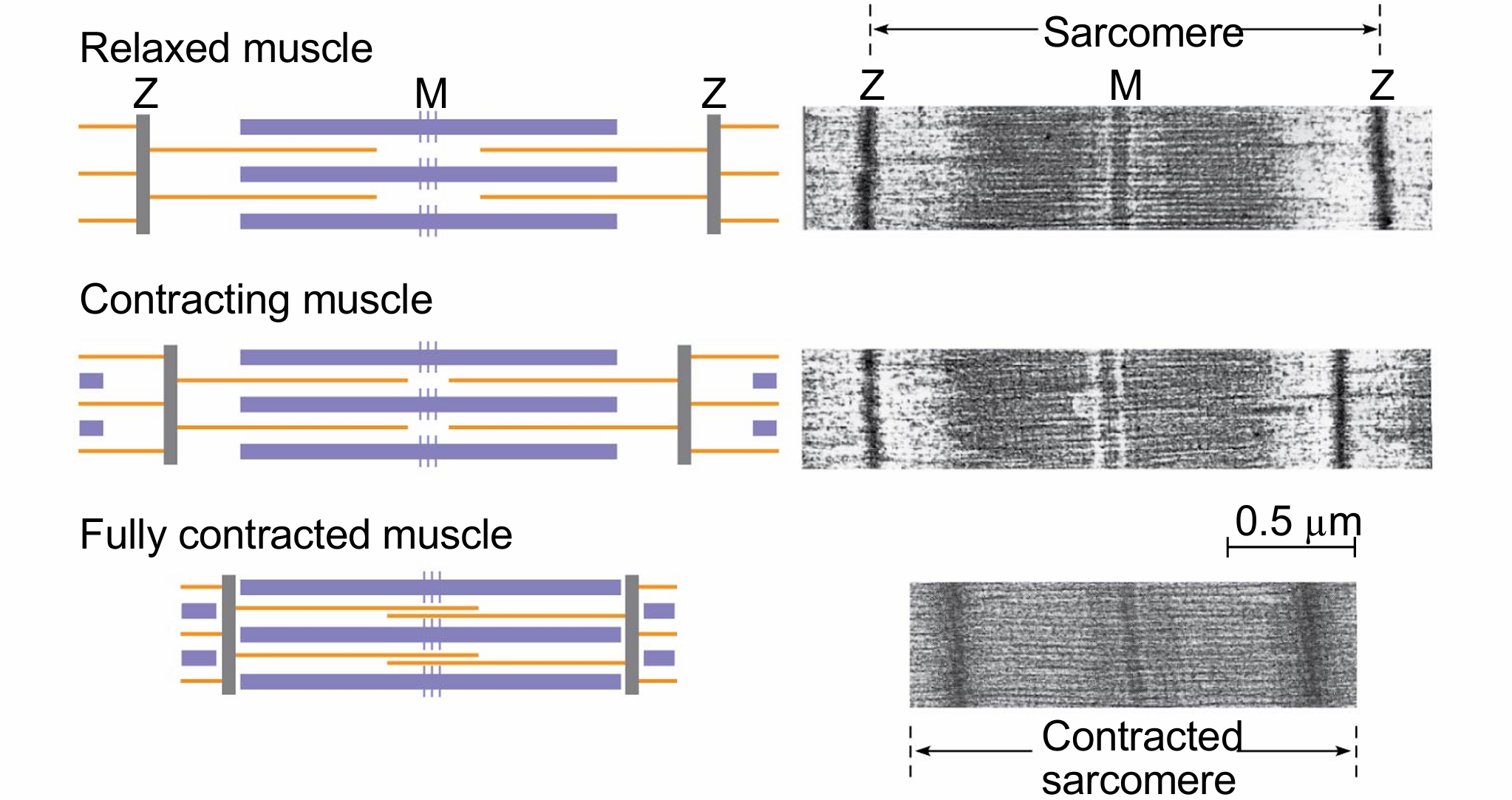
Skeletal muscle is also called striated (striped) muscle because the regular arrangement of myofilaments creates a pattern of light and dark bands
The functional unit of a muscle is called a sarcomere and is bordered by Z lines, where thin filaments attach
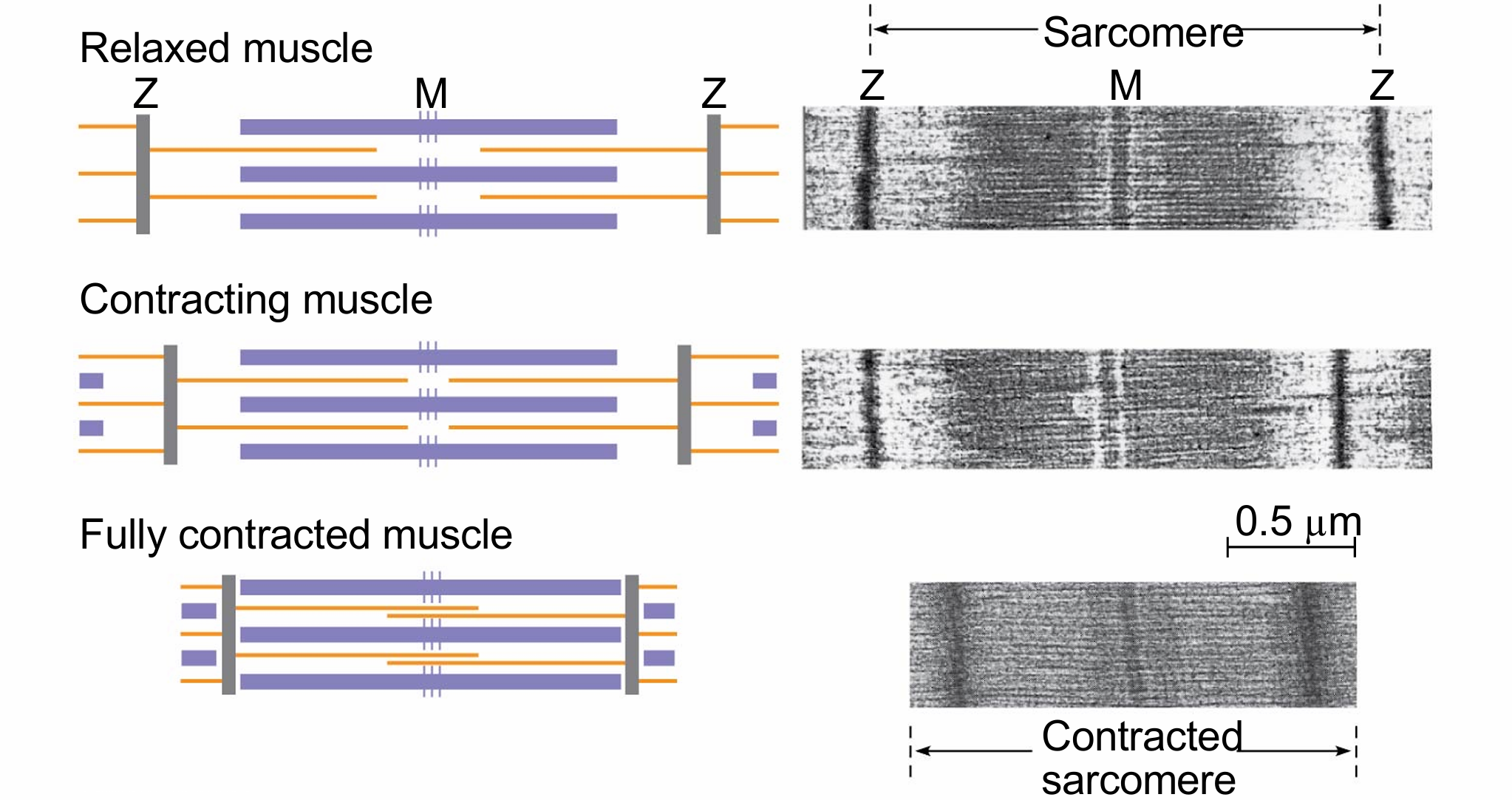
the sliding filament model
thin and thick filaments ratchet past each other longitudinally, powered by the myosin molecules – the muscle shortens
how does myosin facilitate muscle contraction
Each myosin has a long “tail” region and a globular “head” region
The head of a myosin molecule binds to an actin filament, forming a cross-bridge and pulling the thin filament toward the center of the sarcomere: the power stroke
Muscle contraction requires repeated cycles of this binding and release: “cross-bridge cycling”
why does muscle fatigue
Metabolic reasons: lack of substrate (ATP) or accumulation of metabolites that interfere with contraction Glycolysis and aerobic respiration generate the ATP needed to sustain muscle contraction During intense muscle activity, O2 becomes limiting & ATP is generated by lactic acid fermentation This activity generates less activity per glucose than glycolysis and can sustain contraction for only about 1 minute
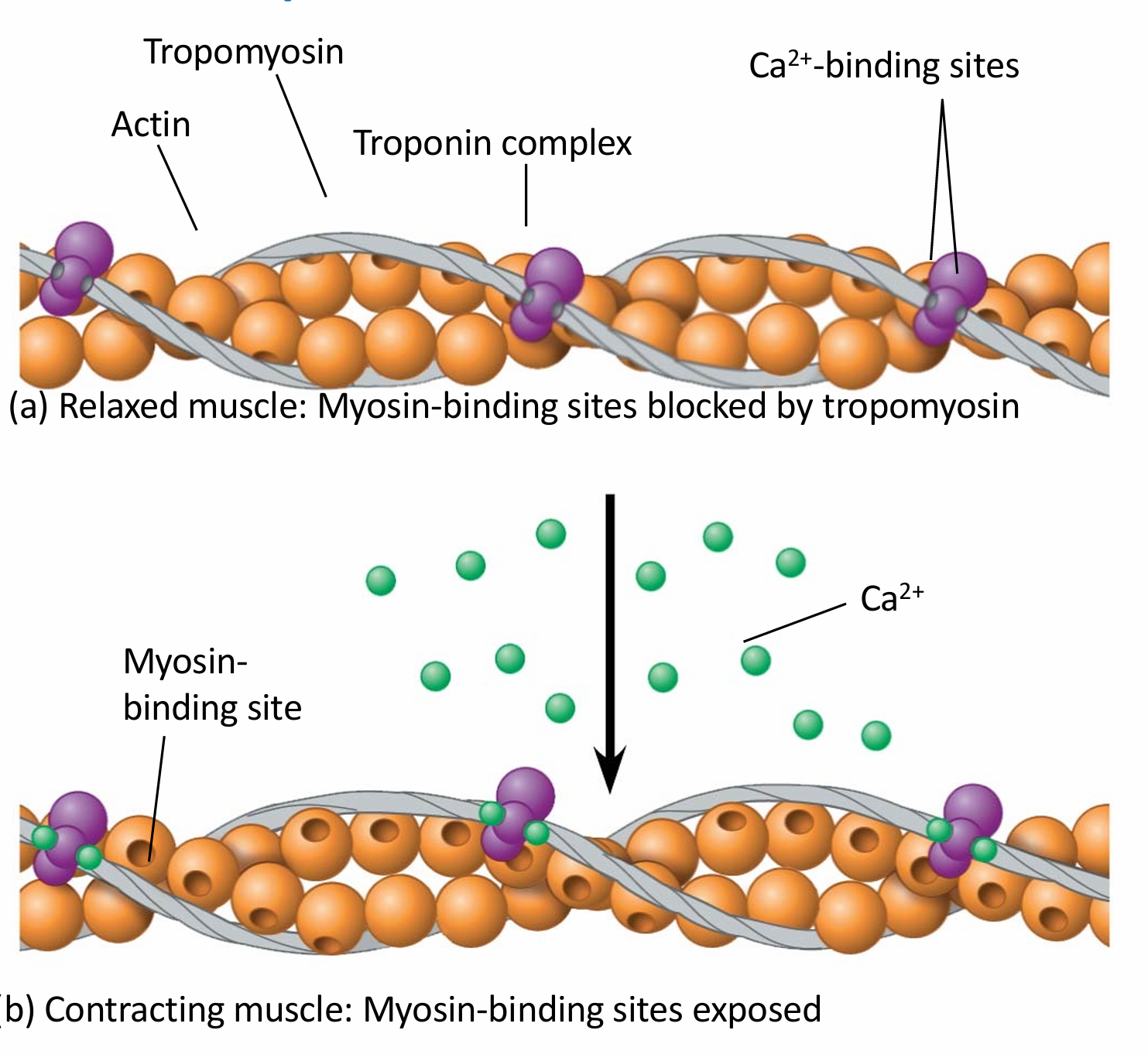
function of tropomyosin
The regulatory protein tropomyosin and the troponin complex, a set of additional proteins, bind to actin strands on thin filaments when a muscle fibre is at rest This prevents actin and myosin from interactin
how do muscle fibers contract
The regulatory protein tropomyosin and the troponin complex, a set of additional proteins, bind to actin strands on thin filaments when a muscle fibre is at rest
This prevents actin and myosin from interacting
For a muscle fibre to contract, myosin-binding sites must be exposed
This occurs when calcium ions (Ca2+) bind to the troponin complex and expose the myosin-binding sites
Contraction occurs when the concentration of Ca2+ is high; muscle fibre contraction stops when the concentration of Ca2+ is low
why are motor nerves vital for skeletal muscle contraction
The stimulus leading to contraction of a muscle fibre is an action potential in a motor neuron that makes a synapse with the muscle fibre
The synaptic terminal of the motor neuron releases the neurotransmitter acetylcholine (ACh) ACh depolarizes the muscle (end plate potential), causing it to produce an action potential
Action potentials travel to the interior of the muscle fibre along transverse (T) tubules, causing the sarcoplasmic reticulum (SR) to release Ca2+
The Ca2+ binds to the troponin complex, initiating the muscle fibre contraction
When motor neuron input stops, the muscle cell relaxes - transport proteins in the SR pump Ca2+ out of the cytosol - regulatory proteins bound to thin filaments shift back to their starting positions
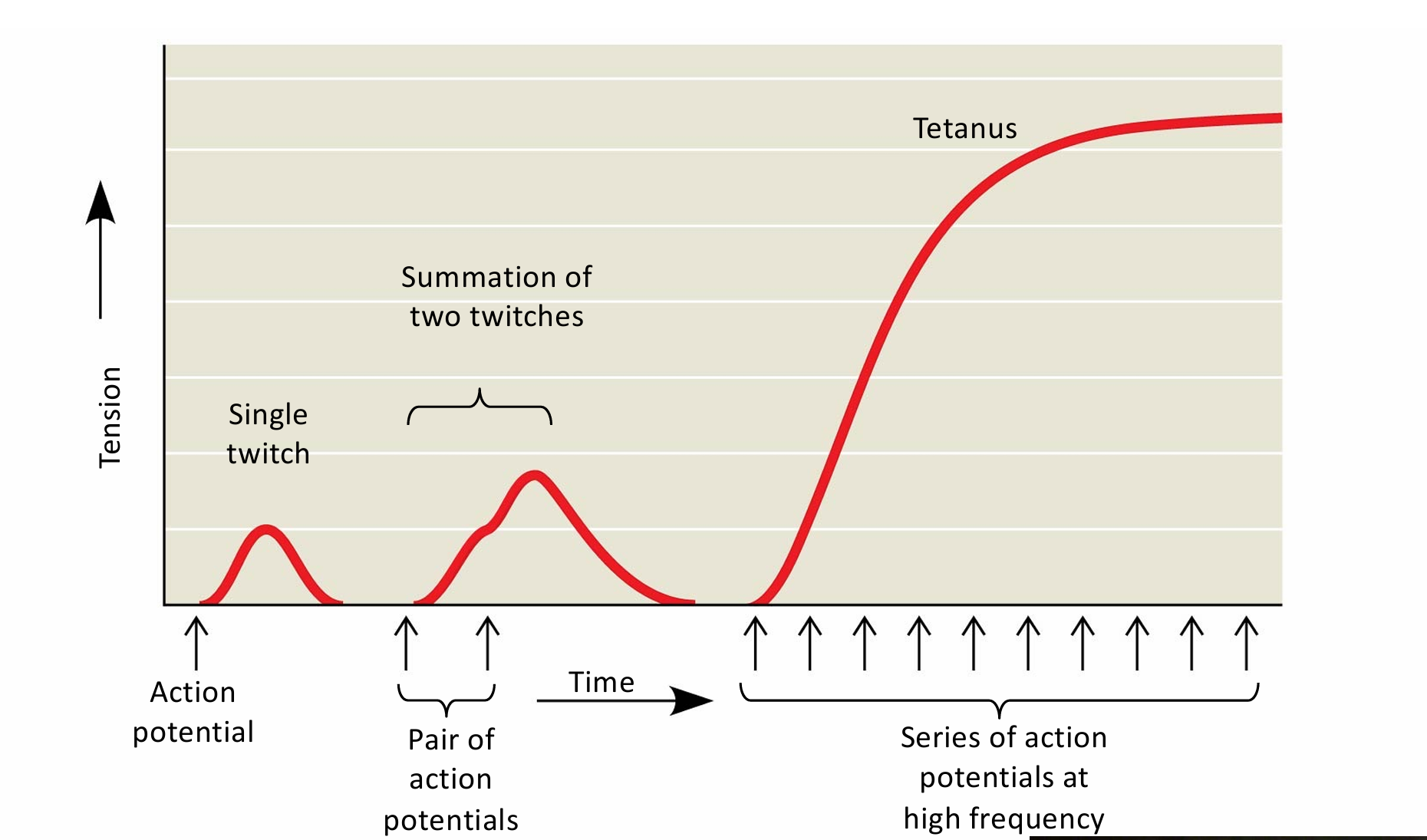
how are graded contractions produced
Contraction of a whole muscle is graded; the extent and strength of its contraction can be voluntarily altered 2 basic mechanisms by which the nervous system produces graded contractions
Varying the number of fibres that contract
Varying the rate at which fibres are stimulated
Each motor neuron may synapse with multiple muscle fibres, although each fibre is controlled by only one motor neuron
what does a motor unit consist of
a single motor neuron and all the muscle fibres it controls
tetanic muscle contraction
sustained muscle contraction, where a muscle doesn’t relax between contractions eg if you’re lifting a heavy weight.
skeletal muscle disorders
Amyotrophic lateral sclerosis/Motor Neurone Disease Unknown cause (genetics + environmental factors) Interferes with the excitation of skeletal muscle fibers; muscles atrophy and weaken. No cure or effective treatment
Multiple sclerosis Demyelinating disease with major immune component Unknown cause (genetics + environmental factors) Disorder of central nervous system
Myasthenia gravis An autoimmune disease that attacks ACh receptors on muscle fibres: muscle weakness (eye, limb, respiratory) 200-400 cases/million Treatments: cholinesterase inhibitors; immunosuppressants
Duchenne Muscular Dystrophy 1:5000 males at birth (X-linked) Genetic Lack of dystrophin (muscle protein) Muscles weaken and degenerate over time
what are cardiac gap junctions
electrical current spreads directly from one cell to another
what makes cardiac muscle unique
Cardiac muscle can generate action potentials without neural input (because of the pacemaker)
Cardiac muscle does NOT fatigue (lots of mitochondria)
No tetanic contraction
characteristics of smooth muscle
Smooth muscle is found mainly in walls of hollow organs such as those of the circulatory, digestive, and reproductive systems
Contractions are relatively slow and may be initiated by the muscles themselves
Contractions may also be caused by stimulation from neurons in the autonomic nervous system
Smooth muscle lacks striations because the actin and myosin are not regularly arrayed
Calcium ions enter the cytosol through the plasma membrane; smooth muscle contraction is regulated by Ca2+, but the mechanism is different
resistance versus endurance training on the heart
Endurance (aerobic) training: heart chambers increase in volume can pump more blood with each beat
Resistance training: heart chamber wall increases in mass: generates more force to pump against resistance
what happens to astronauts muscle in space
On earth we use anti-gravity muscles eg. calf (gastrocnemius, soleus), quadriceps, back, neck. Microgravity; little muscle contraction is needed; spacecraft physical work is undemanding. Without regular use and contraction of muscle, muscles weaken and deteriorate. Up to 20% loss of muscle mass on spaceflights lasting five to 11 days
Astronauts in the International Space Station (ISS) exercise for 2.5hrs/day to prevent muscle atrophy – even then it is not entirely successful and some atrophy still occurs
effect on astronauts heart
CVS function slows down in space Heart becomes more spherical in shape and loses muscle mass (use it or lose it)
Heart function is less efficient NASA study: 12 astronauts underwent ultra sound before, during and after spaceflight
Hearts become 9.4% more spherical Temporary change: shape reverted on return to earth
Consequences for blood circulation and fluid balance
what are the three classes of hormones and their descriptions
polypeptides, steroids, and amines
Polypeptides and most amines are water soluble
Steroid hormones and other largely nonpolar hormones are lipid soluble
Water-soluble hormones are secreted by exocytosis, travel freely in the bloodstream, and bind to cell-surface receptors
Lipid-soluble hormones diffuse across cell membranes, travel in the bloodstream bound to transport proteins, and diffuse through the membrane of target cells They bind to receptors in the cytoplasm or nucleus of the target cells
purpose of the hypothalamus
coordinates endocrine signaling It receives information from nerves throughout the body and initiates appropriate neuroendocrine signals
anterior versus posterior pituitary gland
At the base of the hypothalamus is the pituitary gland, composed of the posterior pituitary and anterior pituitary
The posterior pituitary stores and secretes hormones that are made in the hypothalamus Neural link (PP also known as neurohypophysis)
The anterior pituitary makes and releases hormones under regulation of the hypothalamus Vascular link (AP also known as adenohypophysis)
why does alchohol increase urine output
Alcohol inhibits secretion of ADH = increased volume of dilute urine
thyroid gland feedback loop
If thyroid hormone level drops in the blood, the hypothalamus secretes thyrotropin releasing hormone (TRH), causing the anterior pituitary to secrete thyroid-stimulating hormone (TSH) TSH stimulates release of thyroid hormone by the thyroid gland
goiter
Disruption of thyroid hormone production and regulation can result in serious disorders Thyroid hormone is the only iodine-containing molecule synthesized in the body Low levels of thyroid hormone, due to insufficient iodine, the pituitary continues to secrete TSH This causes the thyroid to enlarge, resulting in a goiter
function of the adrenal glands
The adrenal glands are located on top of the kidneys Each adrenal gland consists of two glands: adrenal medulla (inner) and adrenal cortex (outer)
Adrenal medulla secretes adrenaline and noradrenaline (fight, flight or freeze)
Adrenal cortex secretes corticosteroids – glucocorticoids and mineralocorticoids
Glucocorticoids eg cortisol, influence glucose metabolism and the immune system
Mineralocorticoids eg aldosterone, affect salt and water balance
type one versus type 2 diabetes
Type I diabetes Characterized by lack of insulin secretion (autoimmune destruction of b cells)
Type II diabetes Characterized by normal or even increased insulin secretion but reduced sensitivity of insulin’s target cells
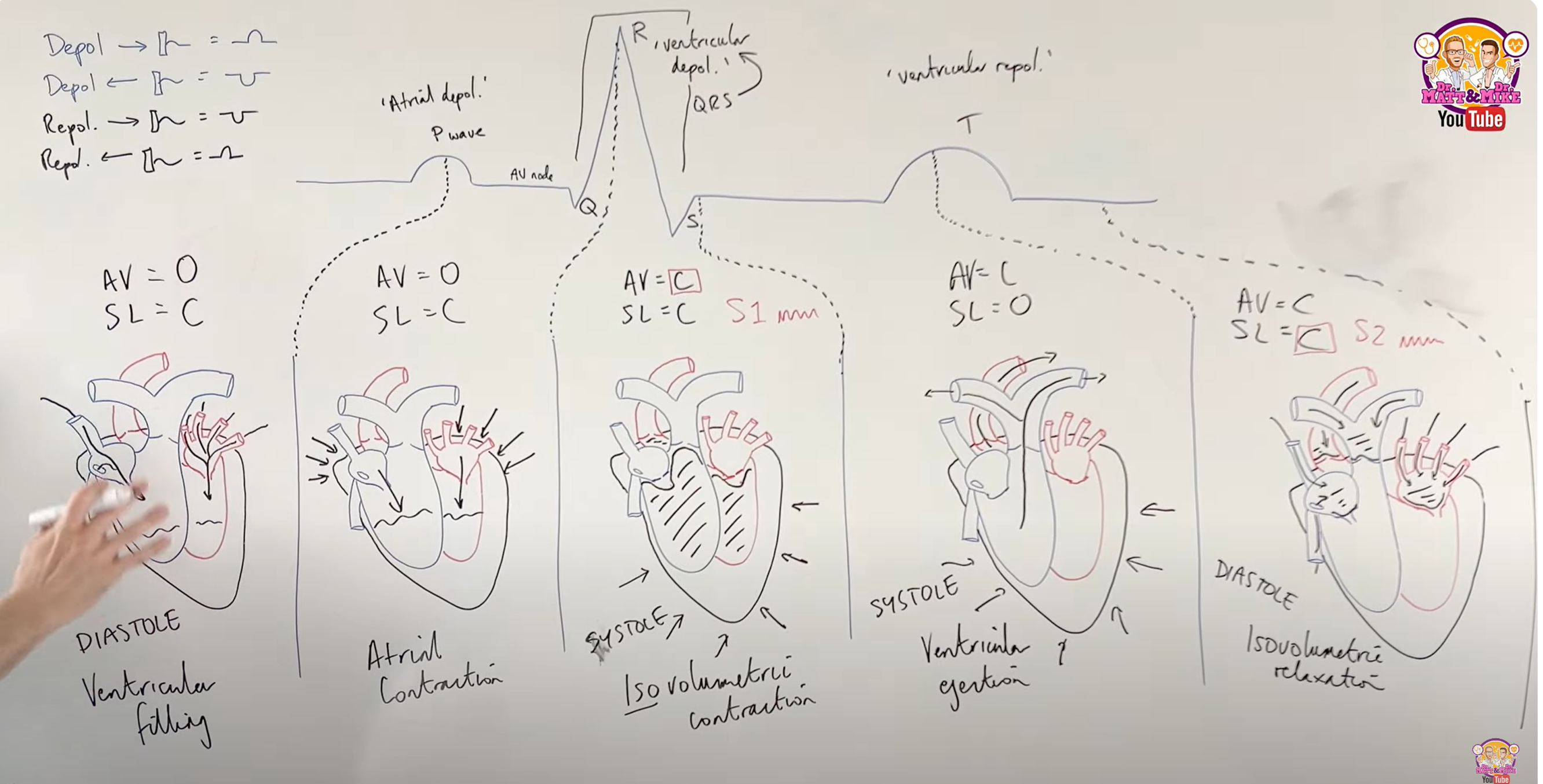
describe the cardiac cycle
how to find cardiac output
Heart rate (beats/min) x stroke volume (mls/beat)
Standard at rest: 70bpm x 70ml/beat = 4900ml/min Approx. 5L/min
Exercise: increases several fold.
Untrained person maybe 20(female) - 25(male) L/min
Miguel Indurain (elite cyclist): peak CO of 50L/min
atrial fibrillation versus ventricular fibrilliation
Fibrillation Loss of coordination of electrical activity.
Can be corrected by defibrillation
Atrial fibrillation – weakness
Ventricular fibrillation - death within minutes Damage to heart muscle
boyles law
At constant temp, pressure and volume are inversely related
inhalation versus exhalation
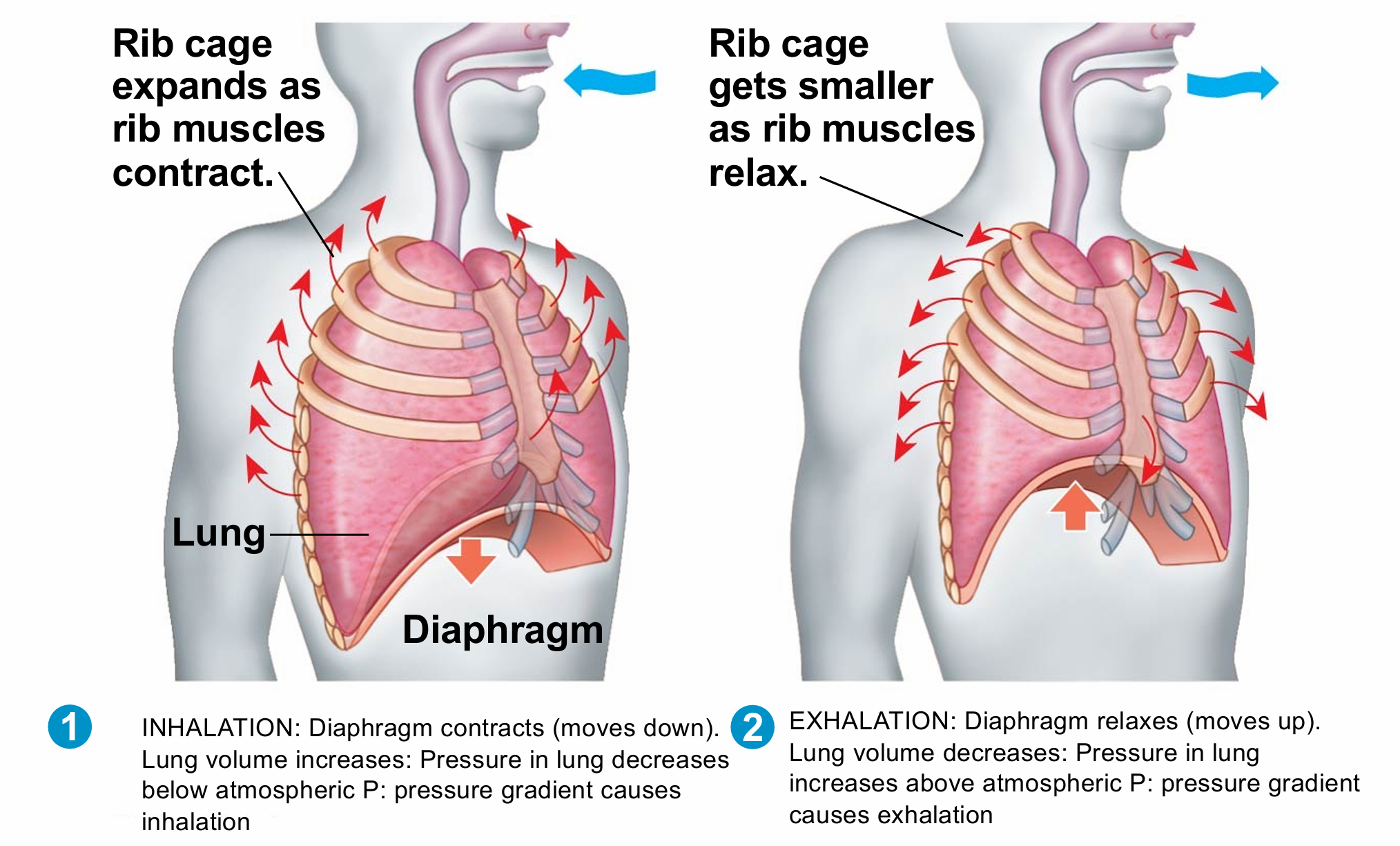
how does transport of oxygen versus carbon dioxide differ
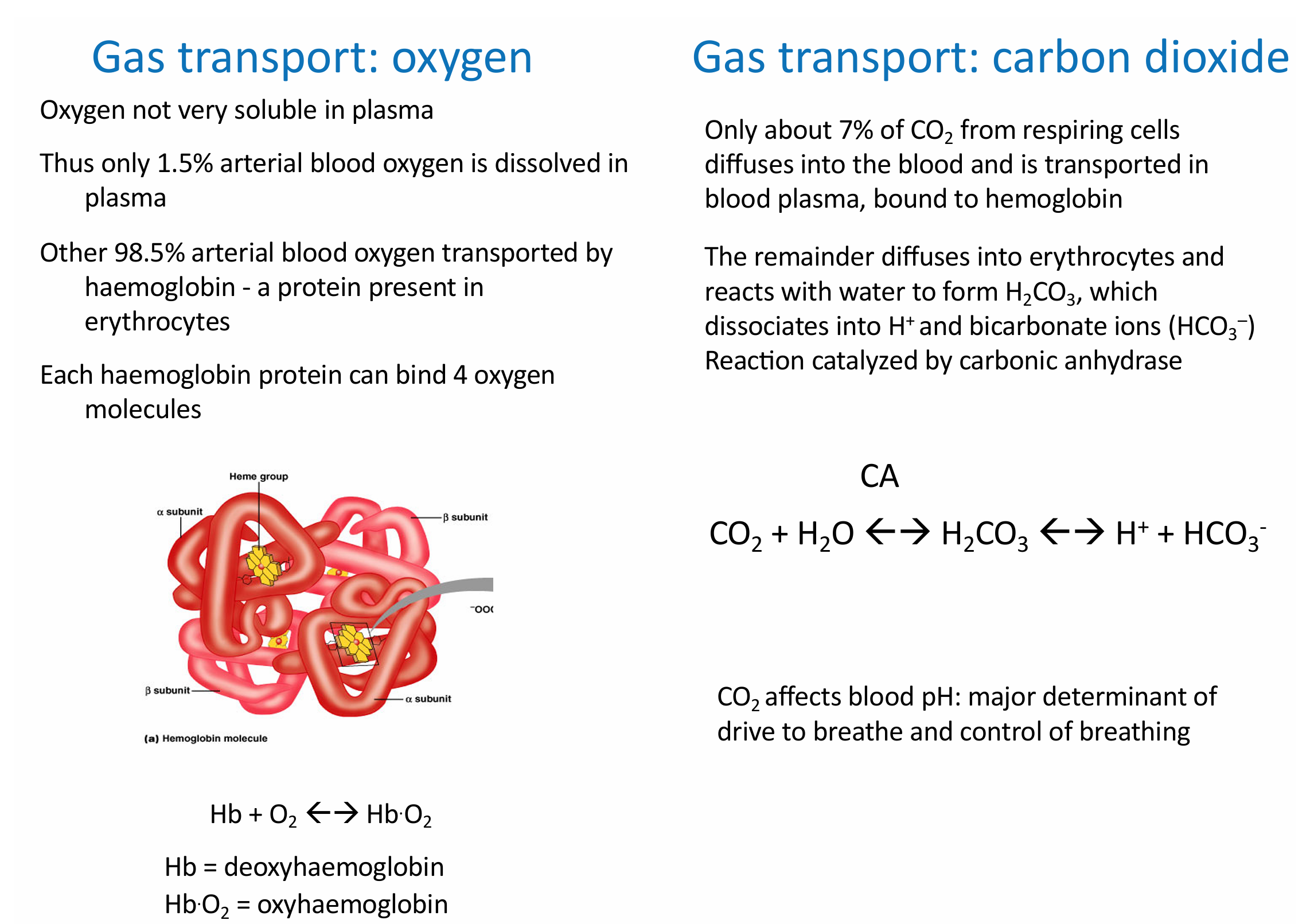
describe the Bohr shift
CO2 produced during cellular respiration lowers blood pH and decreases the affinity of hemoglobin for O2
describe Oedma
Build up of fluid in the interstitium , via Reduced [plasma proteins] Loss in urine (kidney disease) Reduced synthesis (liver disease) Dietary Increased capillary permeability Inflammation & allergic responses
Increased venous pressure
Uterine venous compression during pregnancy
Aeroplane flight (via decompression & immobility)
Lymph blockage Damage during surgery Parasitic infection
![<p>Build up of fluid in the interstitium , via Reduced [plasma proteins] Loss in urine (kidney disease) Reduced synthesis (liver disease) Dietary Increased capillary permeability Inflammation & allergic responses </p><p>Increased venous pressure </p><p>Uterine venous compression during pregnancy </p><p>Aeroplane flight (via decompression & immobility) </p><p>Lymph blockage Damage during surgery Parasitic infection</p>](https://knowt-user-attachments.s3.amazonaws.com/ac2b7c8d-57a0-45ef-a0c2-8d80e50a7a61.png)