MICR:3164 Microbe-Human Interactions
1/109
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
110 Terms
MecA
another route of beta-lactam resistance
antibacterial resistance gene
penicillin attacks peptidoglycan by binding to its target, PBP
mecA allows bacteria to make another version of target protein called PBP2a
what are microbe-host interaction?
contact between microbes and hosts
can be beneficial, neutral, or pathogenic
humans are constantly in contact with microbes, but why aren’t we constantly sick?
host defenses (immune system)
resident biota / normal flora
resident biota / normal flora
microbes colonized in/on a host that don’t normally cause disease
colonization
the act of microbes taking up long-term residence in a human host
infection
entry and multiplication of microbes in host tissues
disease
any deviation, including when a microbial infection damages or disrupts host tissues and organs
how do normal flora prevent intruder infection?
normal flora are colonized and unlikely to be displaced due to limited attachment sites
normal flora create a hostile environment for other organisms
normal flora keep each other in check, so that no singular species takes over and causes disease
normal flora preventing intruder infection is an example of what?
microbial antagonism
how do we acquire normal flora?
microbes present in utero
acquired during birth
breastfeeding/formula
shared from caregivers and family
environment
pathogenicity
an organism’s potential to cause disease
true pathogens
capable of causing disease in healthy people with normal immune defenses
opportunistic pathogens
cause disease when the host’s defenses are compromised
most infections are likely?
polymicrobialp
polymicrobial
multiple microbes contribute to the disease
ex. influenza and pneumonia
infection by influenza virus → lungs damaged
bacteria can easily colonize in wake of influenza
virulence
describes the severity of disease caused by a microbe
ability to establish itself in host
ability to cause damage
virulence factor
a characteristic or structure of a microbe that contributes to virulence
steps of establishing infection
portals of entry
attachment and interaction with microbiome
surviving host defenses
causing disease
vacating host
portal of entry
route by which a microbe enters a host
typically a cutaneous (skin) or membranous route
microbes adapt to use a certain portal of entry otherwise, entry won’t cause infection
infectious dose (ID)
the minimum number of microbes required to establish infection
adhesion
microbes need to gain a stable foothold on host tissues
how do microbes attach and interact?
adhesion
microbe may have specific requirements for attachments (eg receptors)
microbes may have special structures for attachment
why is firm attachment a requirement for microbes?
because many methods of detaching microbes from host tissues exist
how do microbes survive host defenses?
host immune system recognized “foreign” microbes
attacks with phagocytes, other immune cells, antibodies, etc.
microbes have ways to attack back (capsules, toxins, etc.)
how do microbes damage the host?
directly thru enzymes or toxins
indirectly by inducing host defenses and producing an excessive response
epigenetic changes made to host cells
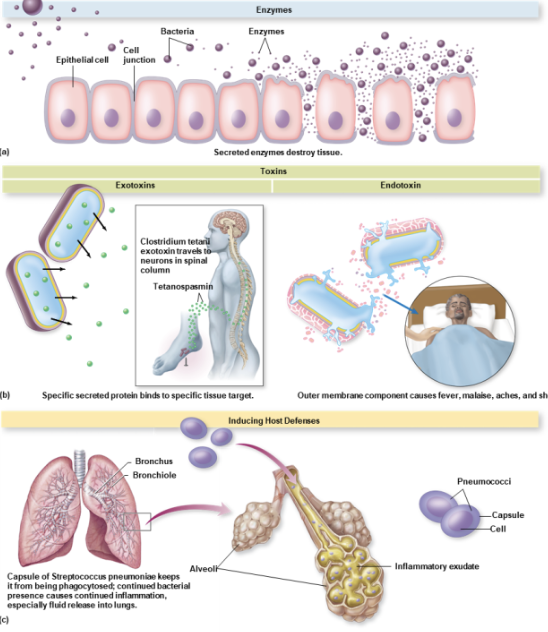
extracellular enzymes
exoenzymes
ex. mucinase (degrades mucous)
ex. coagulase (clots blood)
toxins
specific chemical products of microbes that are poisonous to other organismst
2 types of toxins
exotoxins and endotoxins
exotoxins
proteins with specificity for a target cell and powerful effects
ex. hemolysins lyse RBC
endotoxins
one molecule, LPS, causes a variety of effects on tissues and organs
ex. fever, inflammation, hemorrhage
many aspects of disease are caused by the host trying to what?
trying to rid itself of a pathogen (eg fever, inflammation)
are all responses directly due to something microbe does?
no, not all responses are directly due to something microbe does, but instead the responses it elicits
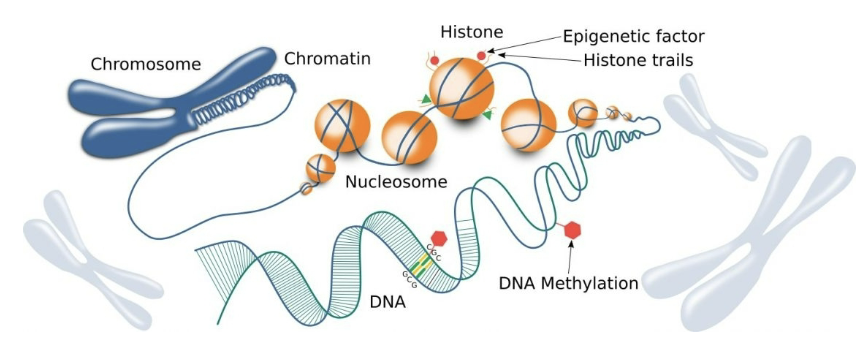
epigenetics
alterations to DNA that impact how or if a gene is expressed, but the DNA sequence doesn’t change
how do microbes cause epigenetic changes in host cells?
they secrete molecules that interact with DNA to shut off host genes
on the scale of likeliness to cause disease, most microbes fall somewhere in the middle. so what tips the scale?
microbe
virulence factors
infectious dose
correct portal of entry
host
genetic variability of host defense
previous exposure
general health
how do disease manifest in the body?
there are many different ways like localized infection, systemic, focal, primary, etc.
sign
any objective evidence of disease as noted by an observer
observed externally
symptom
subjective evidence of disease as sensed by the patient
observed internally
syndrome
when a disease can be identified or defined by certain signs and symptoms
what does inflammatory responses include?
cells and chemicals that respond nonspecifically to disruptions in the tissues
symptoms of inflammation
fever
pain
soreness
swelling
signs of inflammation
edema
granulomas and abscesses
lymphadenitis
edema
accumulation of fluid in tissue
granulomas and abscesses
walled-off collections of inflammatory cells and microbes in the tissues
lymphadenitis
swollen lymph nodes
signs of infection in the blood
changes in the number of white blood cells
presence of a microbe or its products in the blood
changes in the number of circulating WBC
leukocytosis
leukopenia
leukocytosis
increase in white blood cell countsle
leukopenia
decrease in white blood cell counts
presence of a microbe or its products in the blood
septicemia
bacteremia / viremia
septicemia
microbes are multiplying in the blood
bacteremia / viremia
these microbes are present in blood
infections that commonly cause no symptoms are called?
asymptomatic or subclinical infections
portals of exit
microbes are released from the host through secretion, excretion, discharge, or sloughed tissue
the more microbes released, the more likely…
infection is to spread
does recovery mean microbe is gone?
not always
latency
infectious agent retreats into a dormant state and may recur
sequelae
consequences in the form of long-term or permanent damage to tissues or organs
4 distinct phases of infection course
incubation
prodrome
acute
convalescence
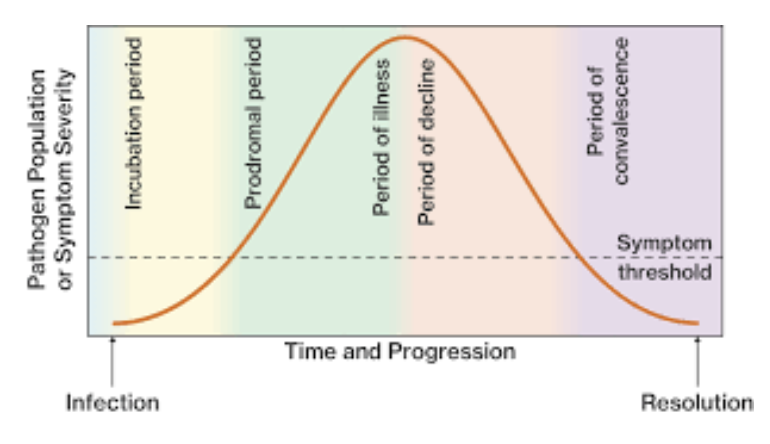
incubation phase
from initial contact to first symptoms
pathogen is multiplying
established timeline for most infections
usually 2-30 days
prodrome phase
earliest notable symptoms
vague discomfort, but may have specific symptoms
short period (1-2 days)
acute phase
microbe is multiplying quickly
greatest virulence
well established infection
fever, cough, rash, etc.
length is variable
convalescence period
recovery period
symptoms decline as body responds to infection
microbes are still present
continuation phase
only present in some infections
organism is present or symptoms continue
reservoir
primary habitat in the natural world where a potential pathogen makes its home
ex. living reservoir: humans, arthropods, animals / non-living: soil, water, air
carrier
an individual who inconspicuously shelters a pathogen and spreads it to others
types of carriers
asymptomatic
incubating
convalescent
chronic
passive
asymptomatic carrier
infected but no symptomsi
incubating carrier
spread infection during infection period
convalescent carrier
spread infection during convalescent period
chronic carrier
shelter an infectious agent for a long period because of latency or persistent infections
passive carrier
healthcare workers who handle heavily contaminated patient materials and pass infectious agents to other patients
zoonosis
an infectious agent usually present in animals spreads to humans
ex. rabies, influenza
can human transmit zoonosis to other humans?
usually dead-end hosts as human-human transmission does not occur
what percentage do zoonoses make up in new emerging diseases?
70% of all new emerging diseases
is eradicating of zoonosis diseases with reservoirs easy or hard?
difficult
communicable
when an infected host can transmit the infectious agent to another host and establish infection
contagious
when a disease is highly communicable
noncommunicable
infection and disease is not acquired through transmission of an infectious agent host-to-host
ex. infections acquired thru soil
horizontal vs vertical transmission
horizontal is to each other while vertical is to offspring
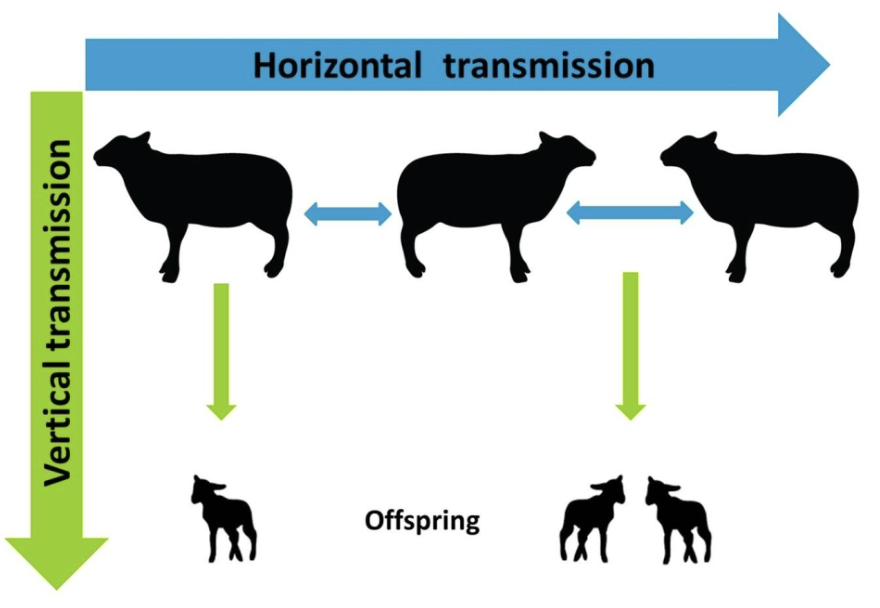
types of horizontal transmission
direct contact
indirect contact
vector-borne
foodborne
waterborne
direct contact transmision
coming into contact with saliva, mucous, blood, or feces containing germs
indirect contact transmission
coming into contact with areas that have been contaminated with germs
vector-borne transmission
being bitten by a tick or a mosquito carrying a disease-causing agent
foodborne transmission
eating food contaminated with germs
waterborne transmission
drinking or coming into contact with contaminated water
fomite
inanimate object that harbors and transmits pathogens like doorknobs, phones, faucet handles
vehicle
a natural, nonliving material that can transmit infectious agents like aerosols/droplets
aerosols/droplets
suspensions of dust or moisture in air
transmission aids
fomite
vehicle
healthcare-associated infections (HAIs)
nosocomial
infectious disease that are acquired or developed during a hospital or healthcare facility stay
patients are often immunocompromised and bring in infectious agents like pneumonia, GI illness, UTIs, bloodstream infections, and surgical site infections
etiologic agent
the precise, causative agent of disease
koch’s postulates
isolate hypothesized agent, inoculate naive population, and see the same disease
epidemiology
study of the frequency and distribution of disease and other health factors
goal of epidemiology
help public health departments develop prevention and treatment programs
reportable diseases
disease that must be reported to authorities by law like anthrax, cancer, foodborne diseases, petussis, tetanus, measles, HIV, lyme disease
prevalence
total number of existing cases in a given population
prevALence = ALl cases / population @ risk
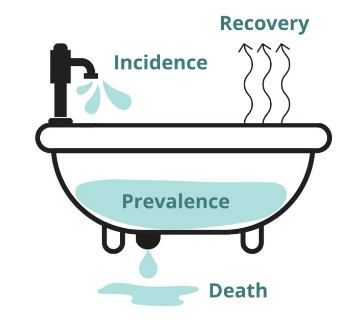
incidence
number of new cases over a certain time period
iNcidence = New cases / population @ risk
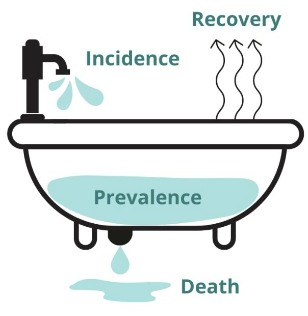
mortality rate
the total number of deaths in a population due to a certain disease
morbidity rate
the number of people afflicted with an infectious disease