PATHO: ch 13 - The Hematopoietic and Lymphatic Systems
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
Blood
A fluid connective tissue
Blood is composed of
Plasma and formed elements (3 formed elements)
What are the 3 formed elements
Erythrocytes (red blood cells)
Leukocytes (white blood cells)
Platelets
Purpose of Erythrocytes (RBCs)
Transport oxygen
What formed element is the most numerous in terms of cells?
Erythrocytes
How long do Erythrocytes survive
4 months (120 days)
Reticulocytes
Immature erythrocytes
How do Reticulocytes become mature erythrocytes
Mature in the bloodstream
What is Hemoglobin
Oxygen-carrying protein formed by the developing red cell
Hemoglobin is composed of how many subunits?
4 subunits (each consisting of heme and globin)
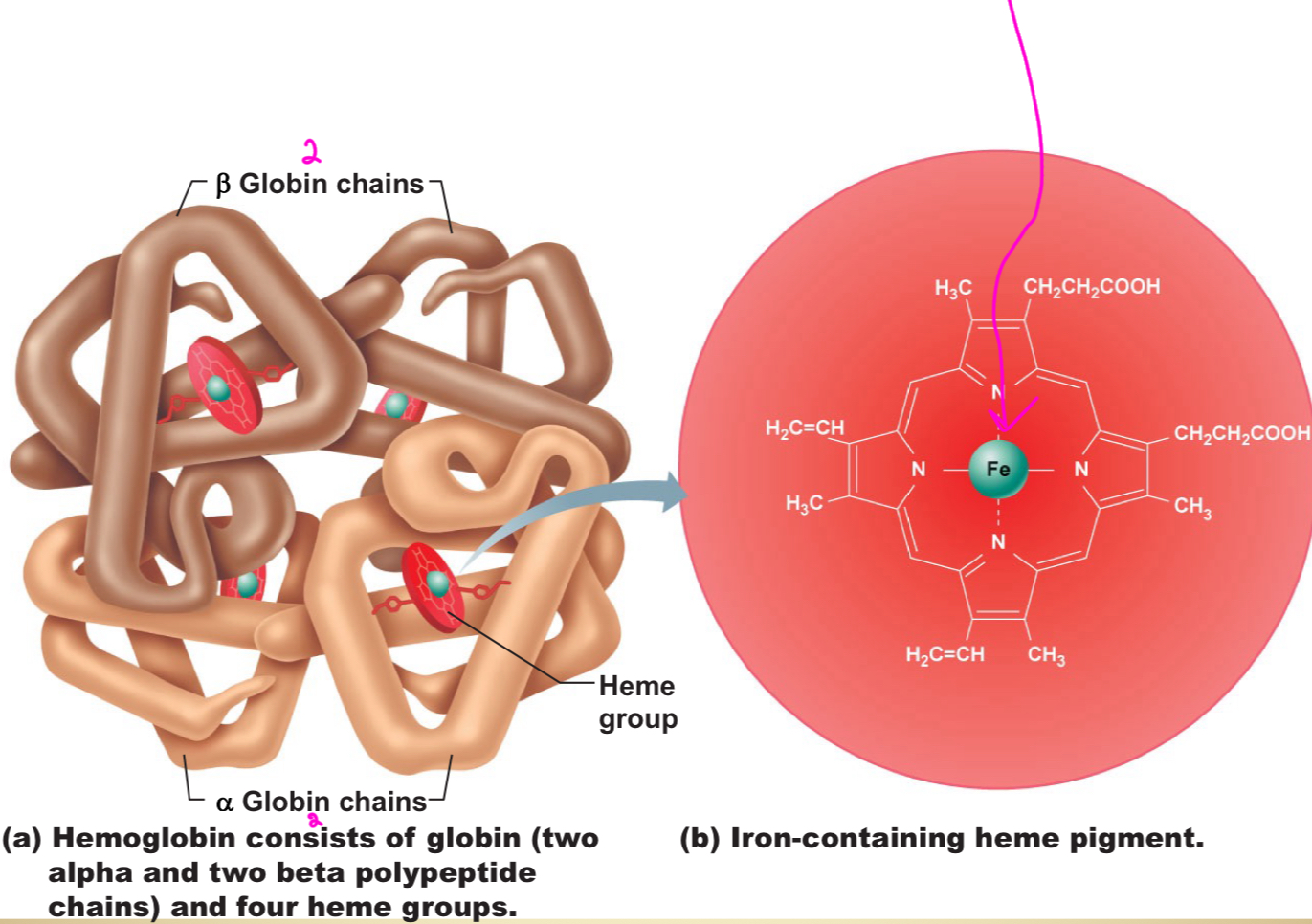
Heme contains what kind of atom?
an iron atom
Hematopoiesis
Formation and development of blood cells
What substances are necessary for hematopoiesis?
Protein
Vitamin B12
Folic Acid
Iron
Reticulocytes become mature…
Erythrocytes in the bloodstream
What is erythropoiesis?
The process of the body producing new red blood cells
What hormone stimulates erythropoiesis?
Erythropoietin (EPO)
What happens to worn out red blood cells?
They are removed in the spleen
How is hemoglobin degraded?
Globin chain are broken down and used to make other proteins
Iron is extracted and reused to make new hemoglobin
Heme degraded and excreted as bile by liver
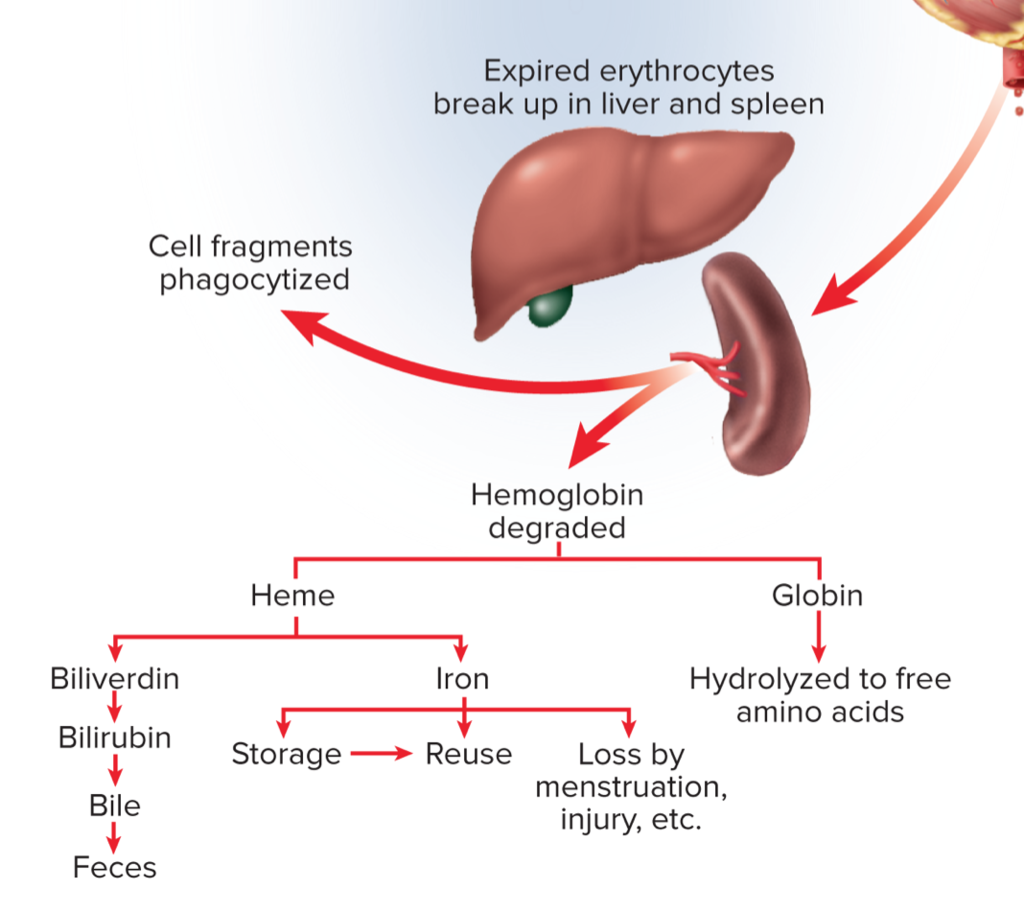
Anemia
Reduction in red blood cells or subnormal level of hemoglobin
What are considered raw materials?
Iron
Vitamin B12
Folic acid
Etiologic classifications of anemia
Insufficient raw materials
Inability to deliver adequate red cells into circulation
External blood loss (hemorrhage)
Shortened survival of red blood cells in circulation
What would cause the inability to deliver adequate red blood cells into circulation?
Marrow damage or destruction (aplastic anemia)
Replacement of marrow by foreign or abnormal cells
Why is it bad to have insufficient raw materials
Inadequate production of red blood cells
Normocytic anemia
Normal size and appearance
Macrocytic (megaloblastic) anemia
Cells are larger than normal
What causes macrocytic (megaloblastic) anemia
Folic acid deficiency
Vitamin B12 deficiency
Microcytic anemia
Cells are smaller than normal
What causes microcytic anemia
Iron deficiency
Normochromic anemia
normal hemoglobin content
Hypochromic anemia
Reduced hemoglobin content
What causes hypochromic anemia
Iron deficiency
Hyperchromic anemia
Increased hemoglobin content
Hypochromic microcytic anemia
smaller than normal and reduced hemoglobin content
What causes hypochromic microcytic anemia
Iron deficiency
Signs and symptoms of anemia
Fatigue
Pallor (light/gray skin)
Especially on conjunctiva (thin, mucous membrane lining inner surface of eyelids)
Dyspnea
Headache
Tachycardia (abnormally fast heart rate)
Weakness
Lethargy
Exercise intolerant
Diagnostic evaluations of anemia
Complete blood count (CBC)
Blood smear
Reticulocytes count
Lab tests
Evaluation of blood loss from gastrointestinal tract
Bone marrow study
Purpose of a complete blood count (CBC)
Assesses the degree of anemia, leukopenia, and thrombocytopenia
Purpose of a blood smear
Determine if normocytic, macrocytic, or hypochromic microcytic
Purpose of Reticulocyte count
assess rate of production of new red cells
If bone marrow is functioning properly, will more or less Reticulocytes become released into the circulation?
More Reticulocytes will be released
What is iron-deficiency anemia?
Iron absorbed from duodenum, transferrin, stored as ferritin
Most common type of anemia
Blood lacks sufficient amount of iron to produce hemoglobin
Pathogenesis of iron-deficiency anemia
Inadequate iron intake in diet
Impaired iron absorption
Inadequate reutilization of iron present in red cells due to chronic blood loss
Pathogenesis of iron-deficiency anemia in INFANTS
Occurs during periods of rapid growth
Pathogenesis of iron-deficiency anemia in ADOLESCENTS
Inadequate diet
How do cells of iron-deficiency anemia appear?
Hypochromic microcytic anemia (small cells and small hg content)
Iron-deficiency anemia laboratory profile
Low serum ferritin and serum iron
Higher than normal serum iron-binding protein
Lower than normal percent iron saturation
Treatment of Iron-deficiency anemia
Primary focus: learn cause of anemia
Administer supplementary iron
Examples of iron-deficiency anemia
Infant w/ history of poor diet
Adults: chronic blood loss from GIT
Women: excessive menstrual blood loss
What contains Vitamin B12?
Meat, liver, foods rich in animal protein
What contains folic acid?
Green leafy vegetables, animal protein foods
BOTH vitamin B12 and folic acid are required for…
Normal hematopoiesis and maturation of other cells (specifically DNA synthesis)
Vitamin B12 is needed for structural and functional integrity of the ________ system
Nervous
(Deficiency may lead to neurological disturbances)
Consequences of vitamin B12 or folic acid deficiency
Cell’s can’t divide
Enlarged RBCs (macrocytic, normochromic anemia)
Abnormal developmen of white cell precursors and megakaryocytes: leukopenia, thrombocytopenia
What is pernicious anemia?
Autoimmune condition
Vitamin B12 can’t be absorbed
Combines with gastric juice in stomach
Leads to a vitamin B12 deficiency
What is the cause of Pernicious Anemia
Autoimmune chronic gastritis
Gastric mucosal atrophy (thin stomach lining)
Gastric resection and bypass
Lack of intrinsic factor
Distal bowel resection or disease
Impaired absorption of Vitmain B12
Pernicious Anemia symptoms
Paresthesia (pins and needles)
Weakness
Headaches
Irritability
Altered vision
Lightheadedness
Tinnitus (ears ringing)
Maybe some neuropathy
Pernicious Anemia treatment
Monthly intramuscular injections of vitamin B12 during person’s ENTIRE lifetime
What is Folic Acid Deficiency Anemia?
Body has very limited stores which rapidly become depleted if not replenished continually
Vitamin B9 deficiency
What causes Folic Acid Deficiency Anemia?
Inadequate diet: frequent in chronic alcoholics
Poor absorption caused by intestinal disease
Occasionally in pregnancy - increased demand for folic acid
How is Folic Acid Deficiency Anemia diagnosed?
Presence of low serum folate
Treatment for Folic Acid Deficiency Anemia
Supplementary folic acid
What conditions depress bone marrow function (3)?
Bone marrow replacement anemia
Anemia of chronic disease
Aplastic anemia
What is bone marrow replacement anemia
Marrow infiltrated by tumor or replaced by fibrous tissue
What is anemia of chronic disease
Mild suppression of bone marrow function
Chronic infection
Some malignant tumors
What is aplastic anemia
Condition resulting from an insult to stem cells in the bone marrow resulting in destruction or inhibition of red bone marrow
What is reduced due to aplastic anemia
RBC, WBC, and platelet production is reduced
What causes aplastic anemia
Radiation
Chemotherapy
Chemicals
Autoantibodies
ALL kill stem cells
Treatment of aplastic anemia
Blood and platelet transfusions
Immunosuppressive drugs
Bone marrow transplant
In MANY cases, no specific treatment
What are hereditary hemolytic anemias?
Genetic abnormality prevent normal survival of RBCs
RBCs are destroyed prematurely
What causes hereditary hemolytic anemias
Hemoglobin abnormalities (most cases)
RBC enzyme disorders
Glucose-6-phosphates dehydrogenase deficiency
What is sickle-cell anemia
Defective gene codes for abnormal hemoglobin
RBCs become sickle shaped in low-oxygen situations
What causes sickle-cell anemia
Sickle shapes RBCs
What do sickle shaped RBCs do
Obstruct capillary flow
Leads to tissue hypoxia
Leads to obstruction and infarction
What populations is sickle-cell anemia prevalent in
Blacks of African origin
Sickle-cell anemia symptoms
Recurrent infections
Abrupt onset of pain curing crisis
Pain can affect any body part
Often involves abdomen, bones, joints, soft tissue
Jaundice
Sickle-cell anemia treatment
Oxygen administration
IV fluids
Narcotic analgesics
Hydroxyurea stimulates bone marrow to produce hemoglobin
CRISPR gene therapy
Blood stem cells start producing HBF
What is Thalassemias
Absent or fault globin chain synthesiS
What causes Thalassemias
RBCs are thin, delicate, deficient in hemoglobin
Microcytic, hypochromic anemia (small RBCs and reduced RBC count)
What populations are Thalassemias most prevalent in?
Those of Mediterranean descent (Greek and Italian ancestry)
What are acquired hemolytic anemias?
Normal red cells but unable to survive due to “hostile environment”
What causes acquired hemolytic anemias
Autoimmune Hemolytic Anemia
Destruction of red cells by mechanical trauma
What is autoimmune hemolytic anemia (type of acquired hemolytic anemia)
RBCs attacked an destroyed by antibodies
What is the destruction fo red cells by mechanical trauma (type of acquired hemolytic anemia)
Passing through enlarged spleen (splenomegaly)
In contact with some part of artificial heart vale
What is Polycythemia
Increased RBC concentration in blood
Result of increased blood viscosity
Increased tendency to thromboses (clotting)
Polycythemia symptoms
Headaches, dyspnea, irritability, mental sluggishness, dizziness, syncope, night sweats, weight loss, splenomegaly, clubbing of the fingers
What is polycythemia versus (primary polycythemia)
Overproduction of red cells, white cells, and platelets
Malignant RBCs do not require erythropoietin for growth
Primary polycythemia treatment
Marrow suppressed by drugs or radiation
What is secondary polycythemia
Increased erythropoietin production (RBCs)
What causes secondary polycythemia
Chronic lung disease
Congenital heart disease
Heavy smoking
Increased erythropoietin production by renal tumor
Blood doping (exogenous EPO)
Commonly used by athletes
Boosts RBC count
Improves oxygen to muscles
Enhances endurance
Secondary polycythemia treatment
Periodic removal of excess blood