OTC - Skin Conditions + childhood skin conditions
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
What are the symptoms of Acne
Whiteheads (closed comedones)
Blackheads (Open comedones)
Spots (Red Papules)
Pustules (small papules filled pus)
Common affected area = face, neck, upper back, shoulders and centre of chest
What is the referral criteria for Acne
- Children under 12 years old
- Adults over 25 for first time
- Acne rosacea (butterfly pattern) - reddening of cheeks with papules and pustules, Confined to face only, Common in middle aged - may be systemic lupus (erythematosus)
- Appears on back or chest or anywhere but face
- Medication ADR - (Lithium, Phenytoin and progestogens)
- OTC failure > 8 weeks
- Moderate - severe acne (may need antibiotics or stronger preparation)
How to tell the difference between Mild, Moderate and Severe acne
Mild Acne - confined to face, mainly blackheads, whiteheads, and small number of inflammatory lesions
Moderate Acne - many inflammatory lesions not confined to the face. Lesions can be painful and there is a possibility of scarring
Severe Acne - Also has nodules and cysts and is wide spread. Scaring is highly likely. Requires retinoids
What are the OTC products available for Acne
First line: Benzoyl peroxide (Acnecide, panoxyl) - Antibacterial, anti comedogenic, anti - inflammatory. Start at a low strength 2.5% or 5%, then gradually increase from OD to BD, then after few weeks increase up to 10%
How to apply benzoyl peroxide
Wash skin before applying with mild soap to remove excess sebum
Takes about 8 weeks for improvement - continue for 4 - 6 months for full effect
Apply to whole area affected by acne not just lesions and apply at night
What are the side effects of benzoyl peroxide
Bleaches clothes
Avoid direct sunlight - apply sunscreen
Photosensitivity - apply in evening
Stinging, dry, burning, red, peeling skin especially in initial stages - Stop for 1 -2 days and start again if side effects unbearable or reduce strength or frequency of application
What is an alternative to benzoyl peroxide
Nicotinamide (Freederm)
Has anti-inflammatory properties but evidence for use is limited
What advice can you give for acne
- There is no evidence to suggest certain food or poor hygiene can cause acne
- Use a mild antibacterial soap - Twice daily is sufficient do not over clean as it can irritate symptoms
- Do not overscrub - once daily is sufficient
- Do not squeeze spots - can lead to infections, scarring
- Avoid greasy oil based cosmetics (clogs pores - stick to water based cosmetics and remove makeup before bed
What virus causes cold sores
Herpes simplex virus 1
Once contracted it remains dominate in the body and never really goes away
What can trigger the herpes simplex virus outbreak
Night fatigue
Menstrual periods
How is the virus transmitted in cold sores
Close personal contact - kissing
What are the symptoms of cold sores
Tingling sensation or irritation (6 - 24 hours before blister)
Blisters on lips/around mouth (filled with white matter on top of sore inflammed skin) - these burst after a day or so to reveal open sores which form a yellowy brown crust - gradually disappear within 10 - 14 days
Self limiting
What is the referral criteria with cold sores
Painless (cancer?)
Babies/ Young children (more severe and potentially lethal)
Immunocompromised (risk of serious infections)
Uncertain diagnosis (impetigo)
Eye affected
Cold sores inside mouth
Cold sores > 2 weeks
Patients with atopic eczema (herpes infections more severe and widespread)
What are the OTC products available for cold Sores
At blister or tingle phase:
- Aciclovir (Zovirax Cold sore cream) - Apply 5 times daily for at least 4 days. Max 10 days - four hourly intervals
- Penciclovir 12+ (Fenistil cold sore cream) - Apply 8 times daily for 4 days. Two hourly intervals
Hydrocolloid patch (Compeed patch) - apply for 24 hours a day until it completely heals. Wound healing properties and acts as a virus shield to prevent contamination
Bland creams - Soothes and moistens skin to help reduce the risk of a secondary bacterial infection
What advice to give to patients with cold sores
HIGHLY CONTAGIOUS
No longer contagious after crusts form
Wash hands after applying cream or touching lesions
Infection is transferable to eye (avoid touching the eye or contamination to eye makeup)
Avoid kissing, oral sex, sharing cutlery
Recurrent episodes - cold sores have no cure and are for life (can be triggered by stress, sun exposure, periods)
What are the symptoms of corns and calluses
Yellow hyperkeratinised skin - caused by excessive pressure or friction on the skin. Common cause is wearing poor fitting shoes or high heels
Can be painful
What is the referral criteria for corns and calluses
Diabetes
Impaired circulations
Treatment failure
Soft corns
What are the OTC products available for corns and calluses
Padding or shielding -helps to relieve pressure
What advice to give to patients with corns and calluses
Wear appropriate well fitting shoes (high heels and poor fitting shoes cause them)
Use a pumice stone to gently remove hard skin
Dry you feet thoroughly after washing them
What is dermatitis
Inflammation of the skin
What is eczema and what are the symptoms
Eczema is atopic dermatitis - Genetic tendency to be hyperallergic
- Sore and inflammed rash
- Very dry and flaky skin
- Irritated and itchy skin
Commonly affected areas is the face, Hands and limb flexures e.g: behind the knees or inner elbows
What is contact dermatitis and what are the symptoms
Response to external factors
- Irritant - substance directly damages outer layer of skin e.g: soap detergent
- Allergic - substance causes immune response e.g: nickel allergy
The typically affected areas is where skin comes into contact with the offending substance
What is the referral criteria for dermatitis
Infected skin - weeping, crusty and spreading rash
Severe rash - widespread, bleeding, cracked skin
Broken skin
Face
Anogenital areas
OTC failure > 7 days
Undiagnosed eczema or no known cause
Symptoms > 2 weeks
What OTC products are available for dermatitis
Emollients: Hydrates and soothes - Apply as often as needed
- Lotions (e.g: dermol 500)
- Cream (e.g: aveeno, cetraben, E45)
- Ointment (e.g. Epaderm ointment) - Most lipid content and most hydrating
- Soap subsititues (e.g: Aqeuous cream)
- Bath additives (e.g: Oilatum bath oil)
Topical Steroids: reduces inflammation. Mild to moderate eczema/rashes
Apply thinly once or twice a day.
10+ Hydrocortisone - Mild potency
12+ Clobetasone - Moderate potency
Itch relief
- Calamine/ Crotamiton (Eurax)
What is the OTC licensing for steroid creams
Max, 15g pack size. Max use 7 days.
Not for broken or infected skin
Not for face or anogenital areas
Not for pregnancy
C/I in acne, rosacea, skin infections e.g: cold sores, athletes foot, impetigo, ringworm
What advice to give to patient OTC for dermatitis
Apply steroid sparingly - can cause skin thinning
Apply Emollient first - Wait 30 minutes to apply steroids
Use soap substitutes
Eliminate aggravating factors (Cold, harsh weathers, stress, central heating, house dust, pet fur, soaps, perfumed cosmetics, synthetic clothing, dairy and red meat
What are the symptoms of psoriasis
Plaque psoriasis
Red plaques
Well defined edges
Slivery scales
Areas affected include elbows, knees and scalp
What is the referral criterial of psoriasis
Undiagnosed
Moderate to severe
What are the OTC products for psoriasis
Emollients
12+ coal tar solution - Exorex, T/Gel shampoo, polytar
Can stain clothes and has an unpleasant smell.
Side effects: Photosensitivity and skin irritation
POM = Vitamin D (Calcipotriol), steroids, Dithranol
What advice can you give OTC for psoriasis
Limit stress
Not contagious
Sun exposure - can improve psoriasis
Give examples of tinea fungal infections
Athlete's foot - tinea pedis
Body ringworm - tinea corporis
Jock itch - tinea cruris
Scalp ringworm - tinea capatis
What are the symptoms of tinea pedis - athletes foot
White
Itchy
Flaky
Possibly macerated skin in web spaces between toes - looks soggy
Smelly
What are the symptoms of tinea corporis - body ringworm
Flat
Slightly raised circular rings with a distinctive red scaly border and can have a central clearing
What are the symptoms of tinea cruris - Jock itch
Fungal groin infection
Red brown rash with well defined edge on inner thighs and buttocks
What are the symptoms of tinea capatis - Scalp ringworm
Distinctive ring shaped rash with associated hair loss
Refer requires oral antifungal
What is the referral criteria for all tinea fungal infections
Ring worm that affects the face or scalp
Toenails also affected in athletes foot
Large area affected or with broken skin
Secondary bacterial infections
Diabetic/ immunocompromised
OTC Failure after 2 weeks
What are the OTC products available
Topical Imidazoles can be used to treat tinea infections:
- All ages: Clotrimazole (Canesten)
- Adults: Ketoconazole (Daktarin GOLD, Intensiv)
- All ages: Miconazole (Daktarin, Daktacort - 15g) - Daktacort licensing: 10+ 7 days use only. Thinly BD
Terbinafine (Lamisil 16+ Lamisil Once 18+)
OTC Licensing:
Spray, cream = Jock itch and athlete's foot
Gell = Jock itch, athlete's foot and body ringworm
Cutaneous solution (Lamisil Once) = Athlete's foot
Powders (Mycota, mycil)
- Can be used prophylactically for athletes foot
What advice can you give for Tinea fungal infections
Continue until at least 7 days after symptoms disappear
Contagious - Easily transferred from pets and animals
Avoid sharing towels - Avoid tight shoes, clothing and accumulation of sweat and heat
In athletes foot:
- Change socks regularly, Dry skin thoroughly, Wear flip flops in communal areas
What are the symptoms of fungal nail infection
Dull, yellow opaque (appearance starts at side of nail or beneath the tip and mainly affects toe nails)
Nail thickens and distorts
Brittle and crumbles away
What are the referral criteria for fungal nail infection
Other fungal nail infections - OTC treatment for mild DLSO
Nail breaking away (severe need systemic treatment with terbinafine)
Pre disposing patient groups
- Immunocompromised
- Peripheral circulatory disease
- Diabetes
What is the OTC Product available
POM to P swtich
Amorolfine 18+ (Curanail 5% nail lacquer)
For mild DLSO
Distal (beneath the nail tip)
Lateral (sides of nail)
Subungal (under nail plate)
Onchomycosis (fungal nail infection)
OTC Licensing: 18+
- No more than 2 nails affected.
- Only beneath tips or sides of nails affected
C/I in pregnancy and breastfeeding
What advice to give to patients with fungal nail infection
Keep using until all the affected nail tissue grows out
- Toenails take 9 - 12 months, Fingernails take 6 months
- One pack give 3 months supply
1. Apply Once weekly to affected nails
2. File down nail surface (use disposable nail file to prevent infection to healthy nails
3. Clean using disposable cleaning pads provided
4. Apply nail lacquer evenly and leave to dry. (Lacquer can be removed by solvents )
What virus causes Warts and verrucae
Human papilloma virus
What are the symptoms of Warts
Flesh colour
Raised
Cauliflower surface
Commonly occurs on the hands and fingers
Disappears naturally within 6 months to 2 years
What are the symptoms of verrucae (plantar warts)
Flat
Occur on sole of feet with black dots (blackened capillaries) in he middle
Can be painful if on weight bearing part of foot
Disappears naturally within 6 months to 2 years
What is the referral criteria for warts and verrucae
Facial warts (OTC products destructive, scarring)
Multiple warts
Anogenital warts (STI)
Diabetic patient - impaired circulation = delayed healing
Immunocompromised patients Itching/ bleeding warts
Change in appearance of wart: size and colour (skin cancer)
OTC Failure > 3 months - warts can take up to 12 weeks to disappear
What are the OTC products for Warts and verrucae
Salcyclic acid (Bazuka, verrugon, salactol)
- Treatment of choice. Softens + destory skin
- Some products contain lactic acid (keratolytic) enhances the availability of salicyclic acid
Cryotherapy (Wartner):
- Freezes warts, verrucae; comes off in 10 days
- Contain dimethyl ether propane
- Thought not to work as well as salicylic acid
Glutaralyydehyde (Glutatrol)
- More suited to treat verrucae
- Not first line ; useful in resistant cases
What advice to give to patients with warts and verrucae
Take up to 12 weeks to disappear with salicyclic acid or glutaraldehyde
Take steps to prevent spreading to others e.g: cover with plaster
When applying salicylic acid:
1. First soak affected area in warm water for 5 minutes to soften it
2. Apply daily, protect healthy skin using petroleum jelly i.e: vaseline
3. Remove dead skin every week with pumice stone/ emery board.
What virus causes chicken pox
varicella zoster virus
What are the symptoms of chicken pox
Small red spots --> very itchy and infectious blisters --> crusts
Small red spots first appear on chest or face before spreading to the limbs/ other body parts
Blisters form over the next 12 hours and then burst and scab over the next few days
Prodromal symptoms: up to 3 days before chickenpx erupts there may be fever, headahce, sore throat, myalgia and malaise
What is the referral criteria for chicken pox
Adults
Pregnant women
Weakened immune system
Infants under 4 weeks old - dangerous at risk of severe chickenpox
What is shingles
Reinfection of the varicella zoster virus and it is a nerve infection - immune system is low
It needs to be referred as it can be treated with possible antivirals (espically if over 50 years, pregnant, immunocompromised, severe rash or severe pain, eye involved, non truncal involvement)
What is the symptoms of shingles
Blisters appear on one side of the body usually the trunk and does not cross over the midline
Nerve pain - can last a month and up to a year after infection
What are the OTC products available for chickenpox
Itching:
Calamine lotion
Crotamiton (Eurax)
1+ Chlorphenamine (piriton)
Fever:
Paracetamol
AVOID IBUPROFEN - can cause serious skin reactions
What advice can you give OTC for chickenpox
Don not scratch lesion (cut nails short and clean to reduce risk of secondary bacterial infection and scarring)
Very contagious
- Infectious until lesions have crusted over.
(Chickenpox spreads through direct contact with blister exudates and air droplets e.g: coughing or sneezing)
Shingles spreads through direct contact only. cover rash with non adhesive dressing
Can catch chickenpox from someone with shingles if you haven't had it before
What is impetigo
Highly infectious bacterial infection that causes sores and blisters
What bacteria causes impetigo
Staphylococcus aureus
Streptococcus pyogenes
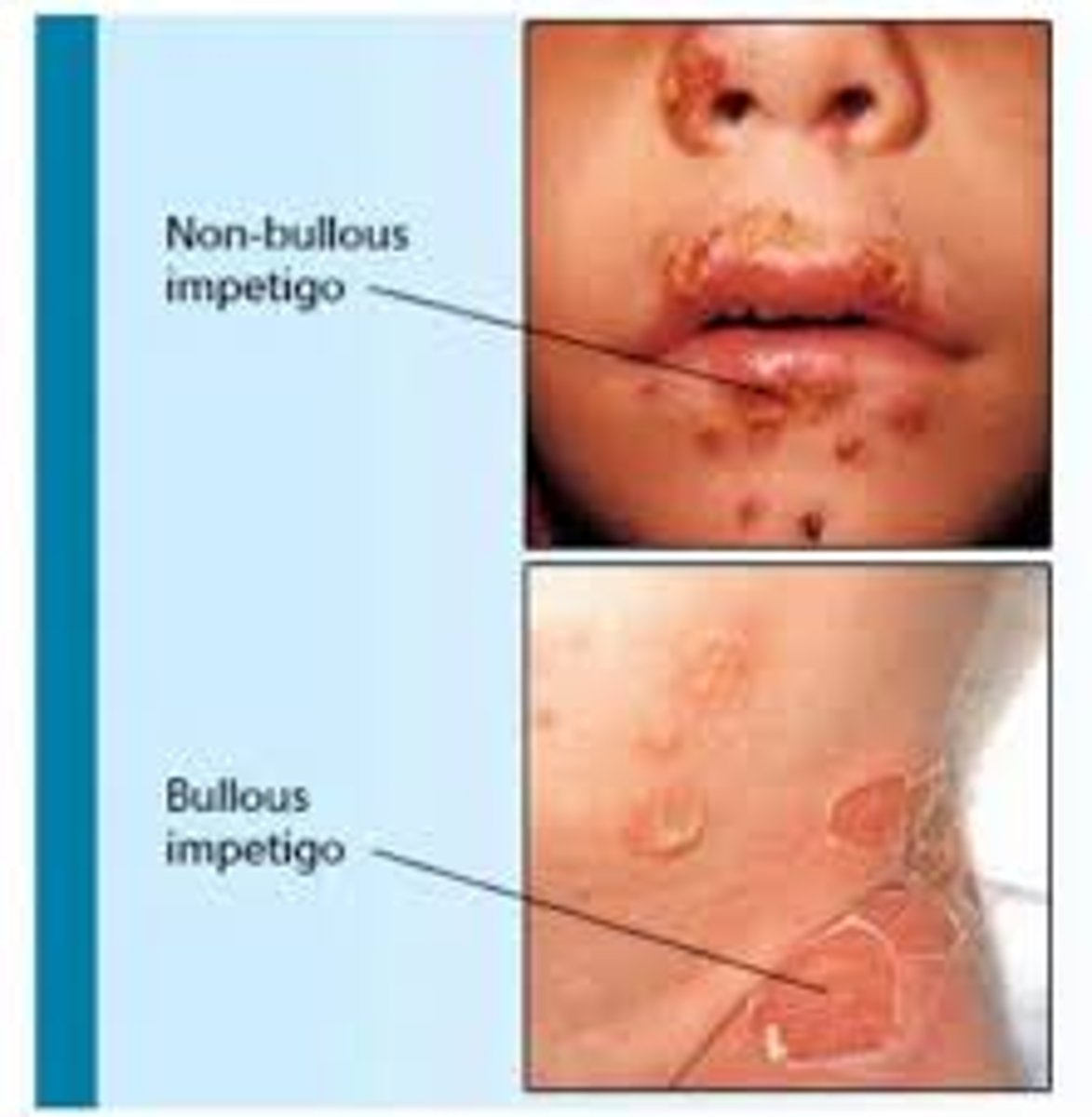
What are the symptoms of impetigo
Golden crust lesions in both
Non - bullous impetigo
- Starts as small red sores around the nose and mouth
- Quickly develops into blisters and bursts
- Can be itchy but otherwise asymptomatic; not painful
Bullous impetigo
- Common in neonates
- Starts as fluid filled blisters on trunk or arms/legs
- Quickly spreads before bursting
- Can be painful and itchy
- Fever and swollen lymph glands is more common
What is the referral criteria for impetigo
ALL CASES needs to be referred
They need antibiotics
- Topical fusidic acid cream for mild cases in small areas
- Oral flucloxacillin if severe or widespread
What are the OTC Products for impetigo
No OTC treatment for impetigo
Symptomatic treatment: if required e.g: paracetamol for fever or antihistamines for itching e.g: chlorpheniramine
What OTC advice can be given for impetigo
Contagious
- Stay away from school until rash clears
Hygiene measures
- Do not share towels. Do not touch lesions
- Cut nails short, scratching causes secondary infection and scarring
What is Meningitis and what bacteria causes meningitis
Infection of meninges which are protective membranes that surround the brain and spinal cord
Can cause life threatening septicemia and can lead to permanent damage to the brain or nerves
Neisseria meningitides - life threatening
Streptococcus pneumoniae
Viral meningitis is caused by the HSV virus - more common and less serious and a spontaneous recovery
When is the peak time for meningitis to occur
6 to 12 months
However can happen in children and adults
What are the symptoms meningitis
- Non blanching rash (pale, blotchy skin with widespread bruises which does not fade when pressed against a glass tumbler) - refer immediately
Non specific symptoms:
- Worsening flu like symptoms
- High fever
- Severe muscle ache
- Nausea and vomiting
More specific:
- Stiff neck
- Severe Headache
- Cold hand and feet
- Confusion, drowsiness
- Photophobia - dislike bright lights
- Seizures
What are specific symptoms specific to infants for meningitis
- Floppiness/ unresponsive
- Dislike being handled
- Refuse feeds
- Difficult to wake
- Rapid breathing/ Grunting
- Unusual cry or moan
- Bulging fontanelle
What should be done to all suspected meningitis cases
BE REFERRED
As required immediate hospital admission
What are the OTC products for viral meningitis
Usually mild, can be treated at home and has spontaneous recovery
Symptomatic relief:
- Paracetamol
- Ibuprofen
What advice can you give for meningitis
TRUST GUT INSTINCT - dont wait until rash develops
Bacterial meningitis is life threatening and may cause septicemia and necessitate limb amputations
What virus that cause MMR
Measles - Paramyxo virus
Mumps - paramyxo virus
Rubella - RNA virus
What are the symptoms for measles
Measles - Initial symptoms develop 1 - 2 weeks after infection with the paramyxo virus - these symptoms include cold like symptoms, red sore eyes, fever and classically koplick spots (greyish white spots that develop on the inside of the cheek)
Measle characteristics:
- Rash starts behind the ears and then spreads to the face, trunks and limbs. Red - brown confluent and blotchy rash
What are the symptoms of mumps
Initial symptoms of mumps develop 2 - 3 weeks after infection with the paramyxo virus
- General symptoms of fever, headache and malaise occur
Mumps characteristics:
Painful swelling on one or both sides of face given a person a distinctive hamster face appearance. - inflammation of the parotid glands
What are the symptoms of rubella
The initial symptoms of rubella develop 2 - 3 weeks after infection with the RNA virus
Symptoms: Swollen lymph glands at the back of neck is a tell tell symptom
Characteristics:
Pink - red macular non confluent rash - Rash starts on the face then spreads to trunks and limbs
What is the referral criteria for MMR
All cases of measles, mumps and rubella for confirmed diagnosis
MMR are notifiable disease
What are the OTC products for MMR
Symptomatic relief after seeing a doctor
- Paracetamol or ibuprofen
What OTC advice can you give for MMR
Plenty of bed rest
Keep hydrated
Keep children off school during contagious period
Avoid acidic drinks in mumps (irritates parotid glands)
Children with rubella should keep away from pregnant women
How long to keep children of school for in measles
Contagious for 4 days after rash appears
Most dangerous childhood illness: complications: otitis media, pneumonia, encephalitis
How long to keep children of school for in mumps
Contagious for 5 days after swelling appears
In adults risk of meningitis and sterility
How long to keep children of school for in rubella
Contagious for 6 days after rash appears
STAY AWAY FROM PREGNANT WOMEN - FETAL DAMAGE
What virus causes slapped cheek
Parvovirus
What are the symptoms of slapped cheek
Bright red rash on cheeks
Light pink, lace like itchy rash on trunk and milbs
Initial cold like symptoms - most contagious period
- Occurs a few days before the rash appears. The patient may have a slight fever, sore throat, headache, runny nose and malaise
What is the referral criteria
Mild infection that usually clears up by itself in 1 to 3 weeks and therefore referral is not required
Refer exposed patient groups urgently if they show symptoms
- Pregnant women - causes miscarriage or stillbirth
- Blood disorders - thalassaemia, weakened immune system, sickle cell anaemia = risk of severe anaemia
- Symptoms of severe anaemia - fainting, severe shortness of breath, ery pale skin, extreme tiredness
What OTC products can be used for slapped cheek
Symptomatic relief:
- Paracetamol or ibuprofen - helps with fever, headaches etc
- Antihistamines - eases itchy rash e.g: piriton
What advice can be given OTC for slapped cheek
Rest and plenty of fluid
Once rash appears it is no longer contagious - there is no need to stay away from school unless the child is feeling unwell
What bacterial causes scarlet fever
Group A streptococcus pyogenes
Usually affects under 10
What are the symptoms of scarlet fever
Follows a sore throat or impetigo
Initial symptoms before rash:
- Sore throat
- Headache
- High temperature
- Flushed cheeks
- Swollen tongue
Pink red itchy sandpaper rash - develops 12 to 48 hours after initial symptoms. First appears on the chest and stomach before spreading to other areas of the body
Other symptoms:
Red and swollen tongue (strawberry tongue)
Swollen lymph glands
Malaise
Loss of appetite
What is the referral criteria for scarlet fever
All cases of scarlet fever as they require antibiotics
Amoxicillin for 10 days - fever goes 24 hours after starting an antibiotic
What OTC products that can be used for scarlet fever
Symptomatic relief as GP referral
- Paracetamol - relieves high fever
- Antihistamine/ calamine lotion - relieves itching
What OTC advice can you give for scarlet fever
Scarlet fever is very contagious
Keep children off for at least 24 hours after starting antibiotic
Avoid sharing towels, clothes, bed linen, cups - spread through touching the skin of a person with streptococcal skin infection, such as impetigo
Cover mouth when sneezing, coughing - spread through air droplets