Physio Chapter 17 & 18 Endocrine System
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
Characteristics of the endocrine system
Composed of endocrine glands that secrete chemical messengers (hormones) into circulatory system to their target tissues (effectors), where they stimulate a specific response.
Works closely with the nervous system to achieve and maintain homeostasis.
Nervous and Endocrine System Similarities
Both systems have shared brain structures, specifically the hypothalamus.
May use same chemical messenger as neurotransmitter and hormone.
• For example, epinephrine.
Two systems are cooperative to regulate body processes.
Neurotransmitters and hormones can affect their targets through G protein-coupled receptors.
Nervous and Endocrine System Differences
Mode of transport: Axons release neurotransmitters directly onto target cells vs.
hormones are released into the blood to travel to target tissues.
Speed of response: Nervous – instant/milliseconds; Endocrine – delayed/seconds.
Duration of response: Nervous – milliseconds/seconds; Endocrine – minutes/days.
Modulation of signal intensity: Amplitude (concentration of hormones) vs. frequency (rate of action
potentials per unit time).
Growth and development
stimulate bone cells to secrete new matrix, neurons to form and strengthen synapses, enlargement of muscle fibers, and more.
Metabolism
stimulate cells to take up or release glucose, produce enzymes, modify heart rate, blood pressure, and respiration.
Blood composition
regulate kidney actions to conserve or secrete ions and water, regulate plasma pH, blood cell numbers and types, and plasma proteins.
Reproduction
key regulators of reproduction in the production of gametes and preparation of the female body to nourish offspring
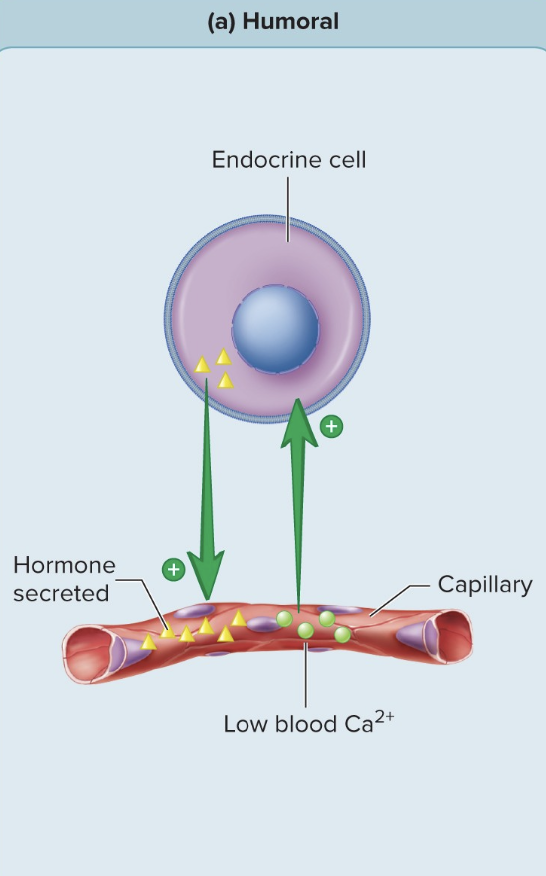
Humoral Stimuli
Stimulus is found in the blood - blood calcium and blood glucose are detected by chemoreceptors to tell the system how to respond
Some hormones are released when the blood levels of certain chemicals change.
Example – when blood calcium levels are low, parathyroid hormone is released.
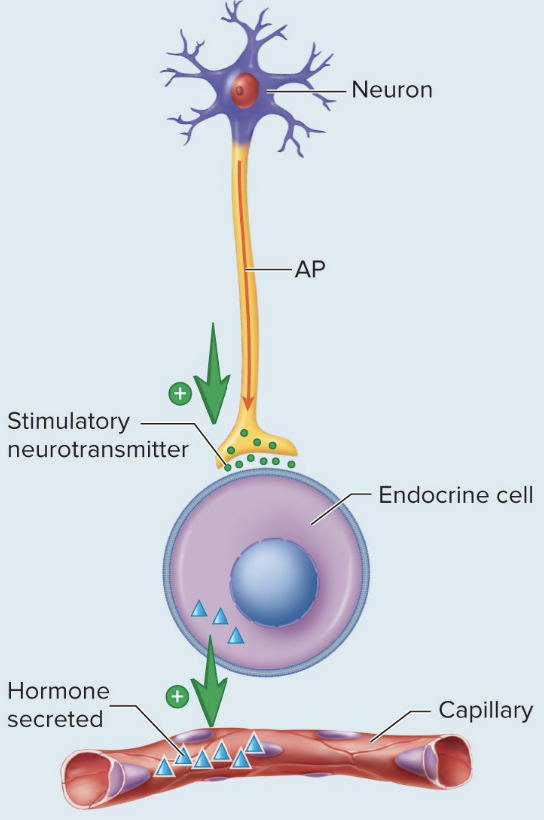
Neural Stimuli
Following an action potential, a neuron releases a neurotransmitter into a synapse with a hormone-producing cell that then secretes its own hormone.
Example: release of epinephrine and norepinephrine from the adrenal medulla from sympathetic stimulation
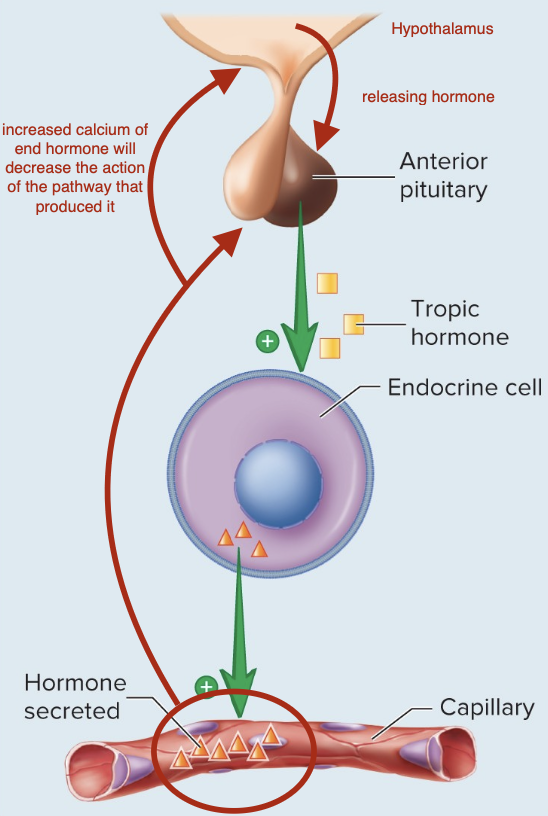
Hormonal Stimuli
Certain hormones are secreted in response to another hormone.
Most are tropic hormones from the anterior pituitary gland to the hypothalamus that act as releasing or inhibiting hormones.
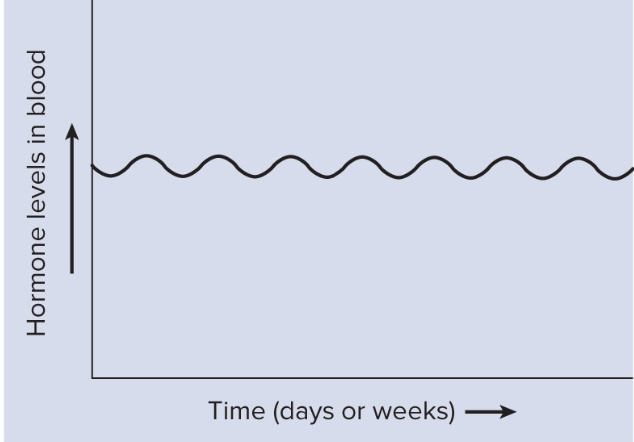
Chronic hormone secretion
Maintenance of relatively constant concentration of hormone in circulating blood for a fairly long period, up to several weeks.
Thyroid hormone
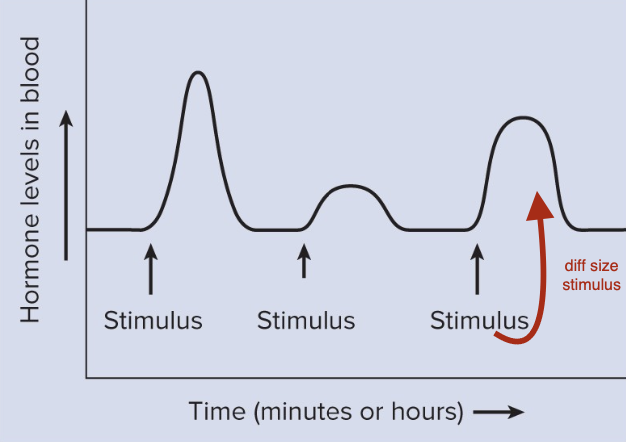
Acute hormone secretion
Concentration changes suddenly and irregularly as a result to a specific stimulus.
Epinephrine in response to stress.
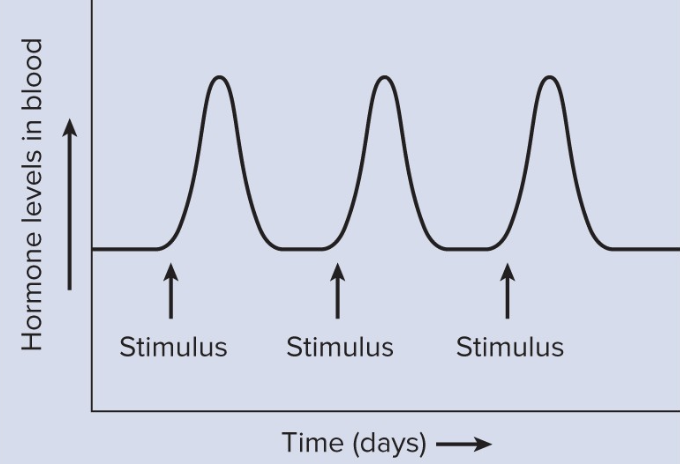
Episodic hormone secretion
Secreted in a fairly predictable pattern.
Female reproductive hormones
Lipid-soluble hormones
Nonpolar, including steroids, amino acid derivatives, thyroid hormone, and fatty acid derivatives.
Take longer for effects but effects last longer
Small lipid - can diffuse freely across the cellular membrane, bind to a nuclear receptor
Water-soluble
Polar, including proteins, peptides, and amino acid derivatives.
Large and bind extracellular receptors - act and decline quickly
Binding proteins
Due to hydrolytic enzymes in the blood, many hormones would be broken down soon after entering the bloodstream.
These hormones require a binding protein to deliver them to their target tissue.
Once bonded to a specific protein, they are called bound hormones; acts as a reservoir.
The process is reversible; then called free hormones; must be free to interact with target tissue.
Free hormones
Immediately activate target cells once they are delivered from the blood. Blood levels fluctuate.
Hormones degrade quickly
Bound hormones
Circulate in the blood longer and provide a chronic, stable supply of hormone
Can’t be broken down by the blood
Negative feedback of hormones levels in the blood
Most common regulatory mechanism. Hormone secretion is inhibited by the hormone itself; self-limiting.
Positive feedback of hormone levels in the blood
the hormone’s secretion is stimulated by the hormone itself; self-perpetuating.
Half-Life of Hormones
Hormone concentrations are stable in the bloodstream, though some hormones are more stable than others.
Larger more complex hormones are more stable than smaller, simpler hormones, but are degraded more quickly.
Half-life: the amount of time it takes for 50% of the circulating hormone to be removed from circulation and excreted. As concentration decreases, the hormone effect decreases.
Elimination of Hormones from the Bloodstream
All hormones are destroyed either in circulation or by enzymes at their target cells. This limits the time they are active.
Without binding proteins, lipid-soluble hormones would quickly diffuse out of capillaries and be degraded by enzymes of the liver or lungs, or be filtered out by the kidneys, and unable to effectively regulate their targets.
Conjugation: specific enzymes in the liver attach water-soluble molecules to the lipid-soluble hormones making them unable to reenter the blood. They are excreted by the kidneys and liver into the urine and bile.
Water-soluble hormones are broken down by enzymes called proteases in the bloodstream and the products removed by the kidneys.
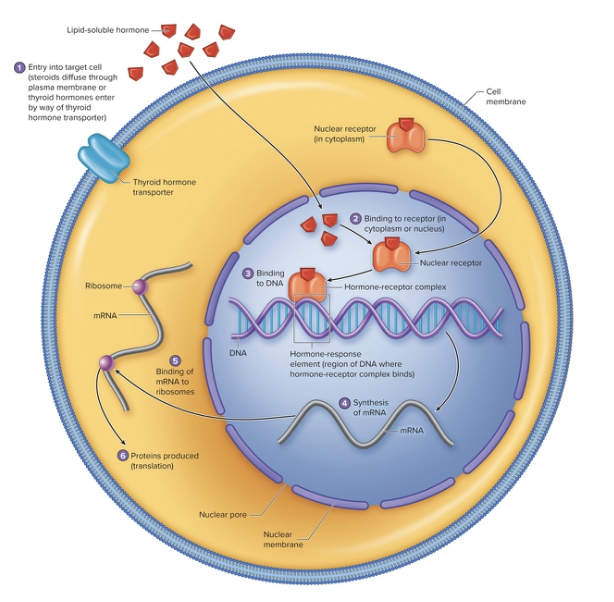
Action of Nuclear Receptors
After lipid-soluble hormones enter their target cell they bind to their receptors.
Lipid-soluble hormones either bind to cytoplasmic receptors and travel to the nucleus or bind to nuclear receptors.
The hormone-receptor complex binds to DNA to produce new proteins. The receptors that bind to DNA have fingerlike projections that recognize and bind to specific nucleotide sequences in the DNA called hormone-response elements. The combination of the hormone and its receptor forms a transcription factor.
When the hormone-receptor complex binds to the hormone-response element, it regulates the transcription of specific messenger RNA (mRNA) molecules.
Newly formed mRNA molecules move to the cytoplasm of the cell, and bind to ribosomes to be translated into specific proteins.
The new proteins produce the cell’s response to the lipid-soluble hormone.
Hormone-receptor complexes are degraded within the cell, limiting the time for hormone influence.
Types of membrane-bound receptors
For EC membrane-bound receptors
Ligand-gated ion channels
G protein-coupled receptors
Enzymatic receptors
G Protein-Coupled Receptors
GTP-binding proteins that allow for transduction of an extracellular signal into an intracellular signal through the use of second messengers
In a second messenger system, the hormone is the first messenger, which binds to its membrane receptor that is coupled to a 3 unit G protein that produces second messenger (intracellular) molecules when activated.
G Protein structure and Function
Subunits:
Alpha (α) – type of α subunit determines the specific cellular response. (drive 2nd messenger production)
Beta (β) and gamma (γ) subunits.
Alpha subunit deactivated by GTPase by removing a phosphate from the GTP and the α subunit rejoins the β and γ subunits.
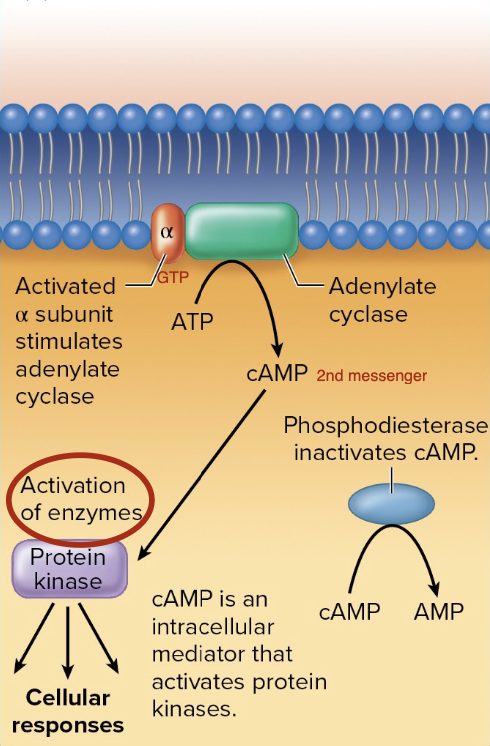
G Protein-Coupled Receptors - Αlpha subunits that increase cAMP
Increase by activating adenylate cyclase.
Activation causes the enzyme adenylate cyclase to convert ATP to the second messenger cAMP.
cAMP then binds to protein kinases to phosphorylate another molecule.
May increase or decrease the enzyme’s activity.
Phosphodiesterase breaks down cAMP to AMP.
Process used by glucagon, epinephrine, ADH, LH, and FSH.
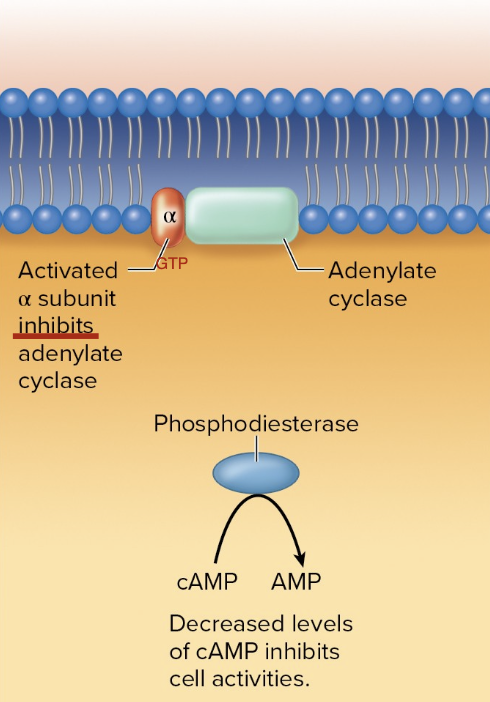
G Protein-Coupled Receptors - Alpha subunits that decrease cAMP
Decrease cAMP in cells where it is typically abundant - decreased cell activity
Activation inhibits adenylate cyclase, which results in a decrease in available cAMP.
Phosphodiesterase breaks down the cAMP that is available, further reducing
the cAMP.
Process used by epinephrine and prostaglandins.
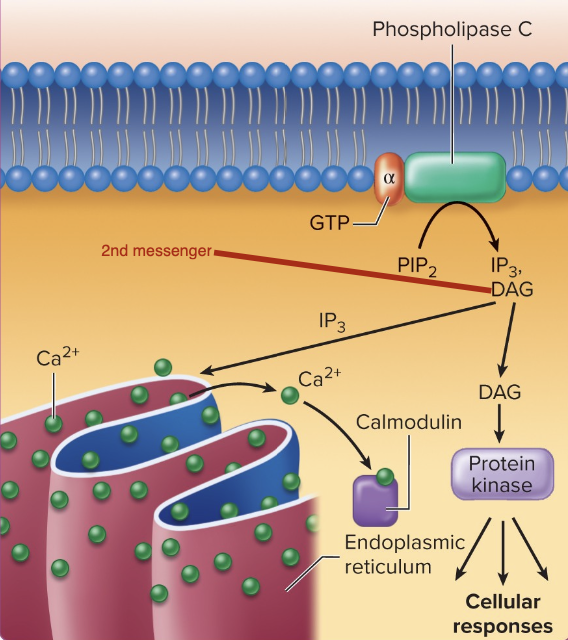
G Protein-Coupled Receptors - Alpha subunits that increase 2 Ca+
Activations stimulates the enzyme phospholipase C that converts PIP2 to the second messenger DAG.
DAG (diacyl glycerol) and inositol triphosphate (IP3).
DAG activates enzymes that synthesize prostaglandins to increase smooth muscle contractions.
IP3 releases Ca2+ from ER or opens 2 Ca2+ channels to increase contraction of smooth muscle.
Process used by oxytocin.
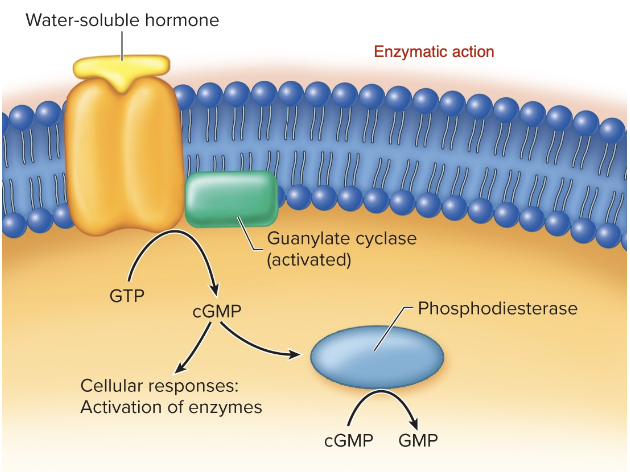
Enzymatic Receptors - Guanylate Cyclase Receptors
cGMP, a second messenger, is synthesized in response to a hormone binding to a membrane-bound receptor.
Activates the enzyme, guanylate cyclase that converts GTP to cGMP.
cGMP activates specific enzymes as the cell’s response.
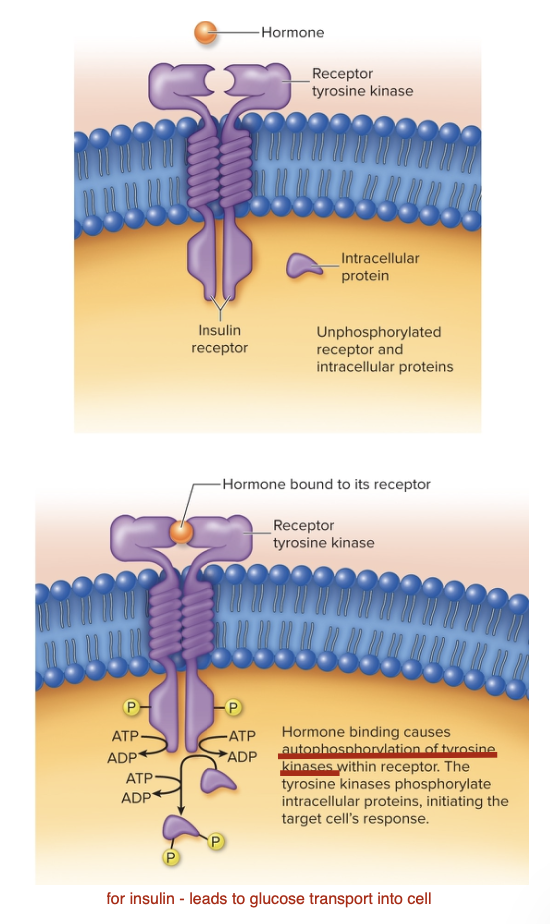
Enzymatic Receptors - Receptor Tyrosine Kinases
Insulin receptor is a receptor tyrosine kinase of four subunits.
Two units are extracellular, and two are embedded in the membrane and contain the enzymatic portion.
Binding of insulin to the extracellular portion causes a conformational change that ends with the tyrosine amino acids in the receptor to become phosphorylated and activated.
The receptor then phosphorylates cytoplasmic proteins to elicit the hormone effects.
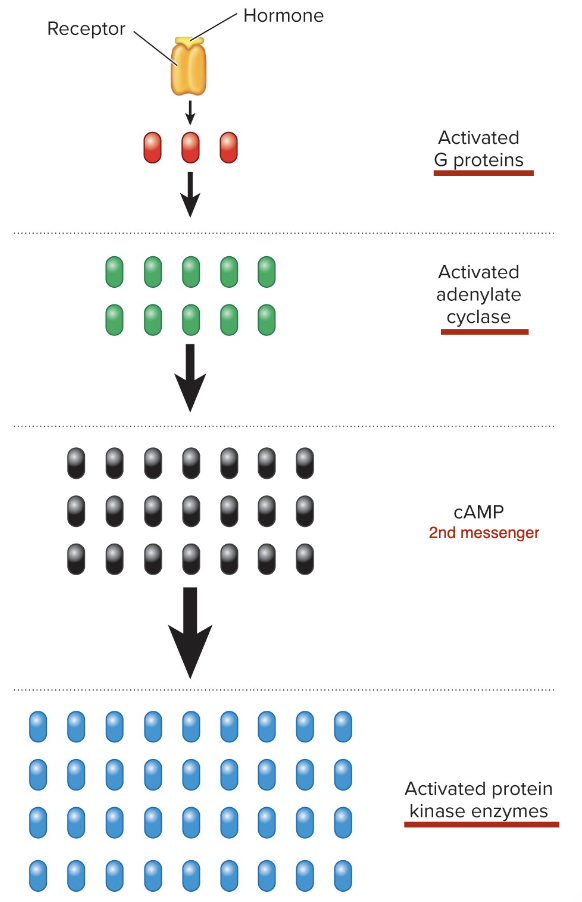
Signal Amplification
The rate and magnitude of a hormone’s response are determined by the mechanism of action at the receptor
Nuclear receptors activate protein synthesis which can take several hours
Hormones that use second messenger, respond quickly and with a greater magnitude.
Down-regulation
Desensitization
Rate at which receptors are synthesized decreases in some cells after the cells are exposed to a hormone.
Combination of hormones and receptors can increase the rate at which receptor molecules are degraded. This combined form is taken into the cell by phagocytosis and then broken down.
Up-regulation
Some stimulus causes increase in synthesis of receptors for a hormone, thus increases sensitivity to that hormone.
For example, FSH stimulation of the ovary causes an increase of LH receptors. Ovarian cells are now more sensitive to L H, even if the concentration of L H does not change. This causes ovulation.
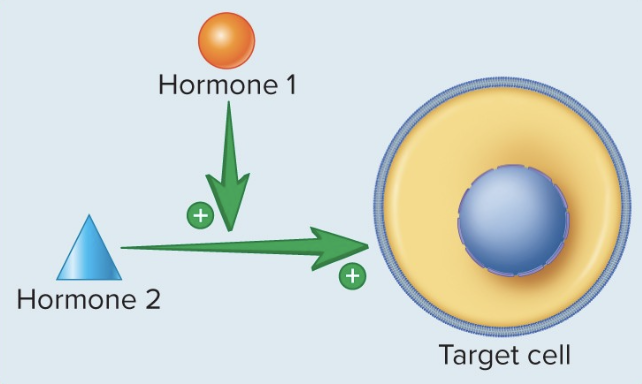
Permissive Interactions
Some hormones assist other hormones to have a stronger response.
Thyroid hormone promotes synthesis of receptors for epinephrine in the heart.
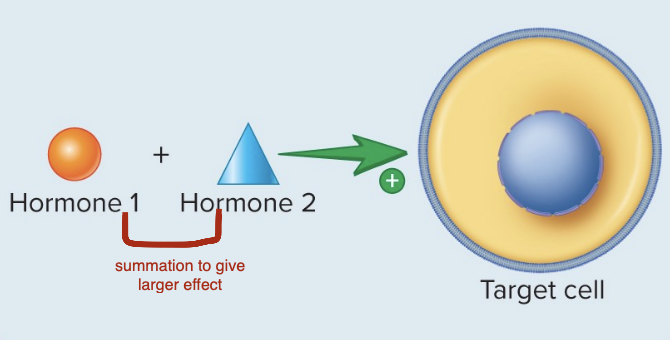
Synergistic Interactions
Two or more hormones exert their effects on a target tissue to greatly increase the response
Reproductive hormones
LH and FSH have a more potent affect when combined - drive ovulation, estrogen synthesis
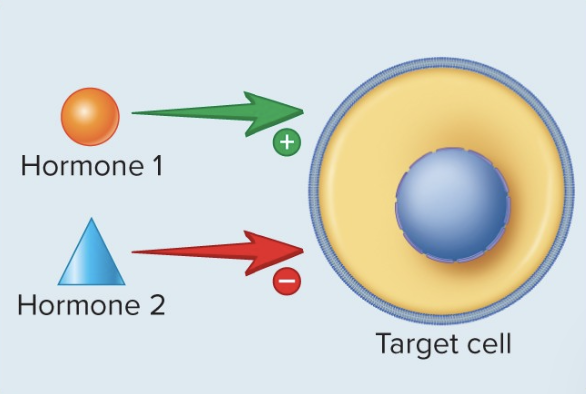
Antagonistic Interactions
Some hormones work in the opposite way from another to tightly regulate a response.
Calcitonin and PTH regulate 2Ca+ blood levels.
Insulin and glucagon regulate blood glucose levels.
Roles of the Endocrine System
•Regulates growth and development (e.g., growth hormone, thyroid
hormones)
•Controls metabolism (e.g., insulin, thyroid hormones)
•Maintains homeostasis (e.g., fluid balance, blood pressure via ADH and
aldosterone)
•Manages stress responses (e.g., cortisol, adrenaline)
•Supports reproduction (e.g., estrogen, testosterone, LH, FSH)
•Influences mood and sleep (e.g., melatonin, serotonin
Posterior Pituitary Hormones
Antidiuretic hormone (ADH)
Oxytocin
Antidiuretic hormone (ADH)
Also called vasopressin
Release triggered by:
Osmoreceptors in the hypothalamus detecting increase blood
osmolality. Increased concentration of solute in the blood and a decreased concentration of water.
Baroreceptors (carotid arch/aortic sinus) sense changes in blood
pressure (BP). Decreased water in blood, decreased BP
Oxytocin
Stimulate uterine contractions during labor. Allows for breast feeding.
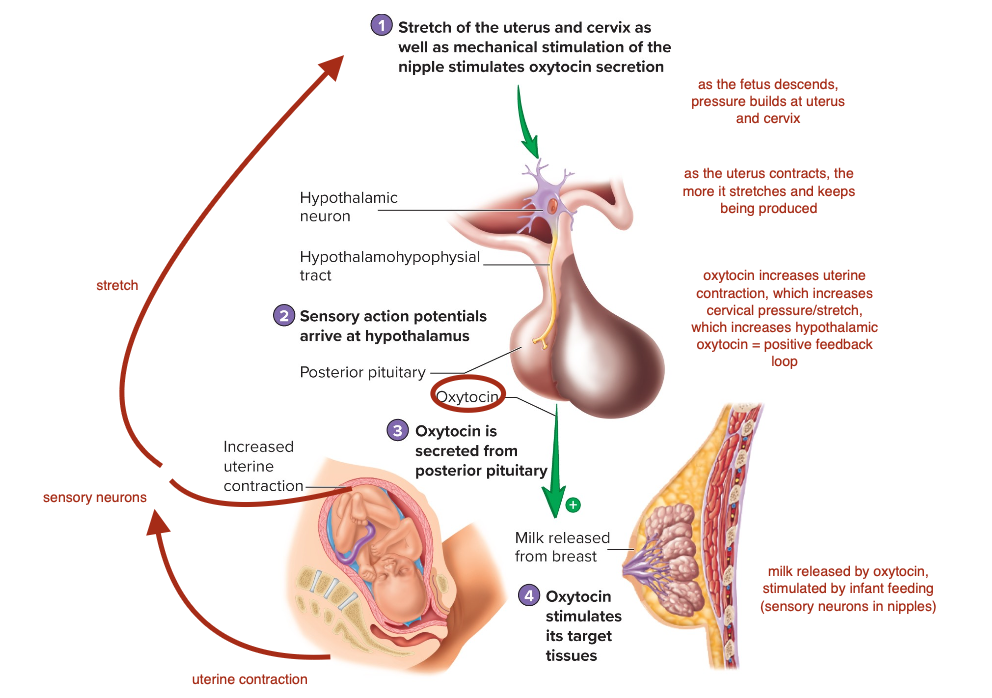
Control of Oxytocin Secretion
Stretch of the uterus and cervix as well as mechanic stimulation of the nipple stimulates oxytocin secretion.
Sensory action potentials arrive at the hypothalamus
Oxytocin is secreted from the posterior pituitary
Oxytocin stimulates its target.
Growth Hormone
•Stimulates growth: Promotes bone and muscle development, especially in children and teens.
•Regulates metabolism: Increases fat breakdown, supports protein synthesis, and can raise blood sugar.
•Supports tissue repair: Aids in healing and cell regeneration.
•Maintains bone density: Helps prevent osteoporosis.
•Deficiency: Causes stunted growth in children; fatigue and muscle loss in adults.
•Excess: Leads to gigantism in children, acromegaly in adults, and increased health risks.
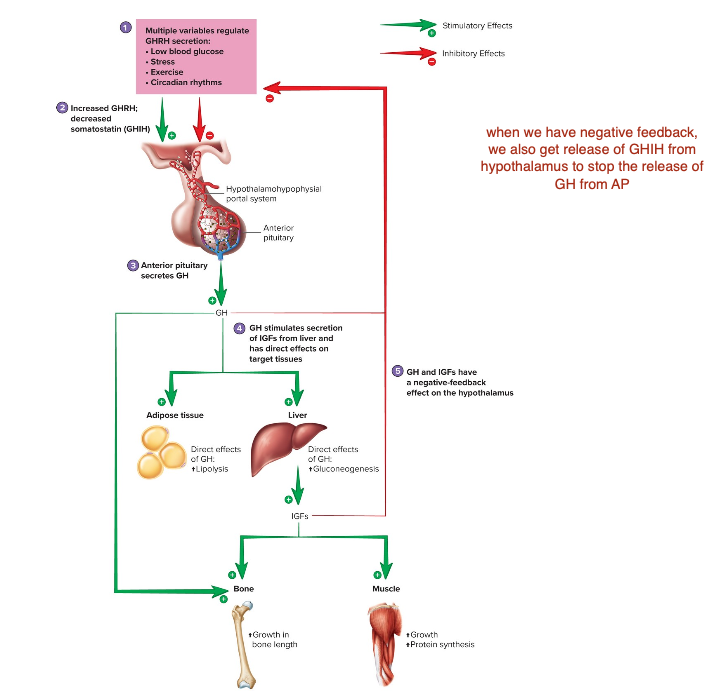
Control of Growth Hormone Secretion
Multiple variables regulate GHRH secretion:
Low blood glucose, stress, exercise, circadian rhythm
Increased GHRH; decreased somatostatin (GHIH)
Anterior pituitary secretes GH
GH stimulates secretion of IGFs from liver and has direct effects on target tissues
GH and IGFs have a negative-feedback effect on the hypothalamus.
Prolactin
Role in milk production, enhances progesterone secretion by ovaries, also contributes to regulation of the ion composition of blood, growth, development, behavior, metabolism, and immune function.
Regulation of secretion: prolactin-releasing hormone (PRH) and prolactin-inhibiting hormone or dopamine (PIH).
Causes milk production for the next nursing event (oxytocin causes release of milk during current nursing event)
Thyroid Gland Physiology
Follicular cells: secrete thyroglobulin into lumen of follicle
Parafollicular cells: secrete calcitonin
TSH (from anterior pituitary) is a glycoprotein hormone that causes secretion and storage of hormones T3 and T4 from and within the thyroid gland.
Iodine required to produce thyroid hormone
TSH receptors respond through a G protein mechanism that increases intracellular cAMP.
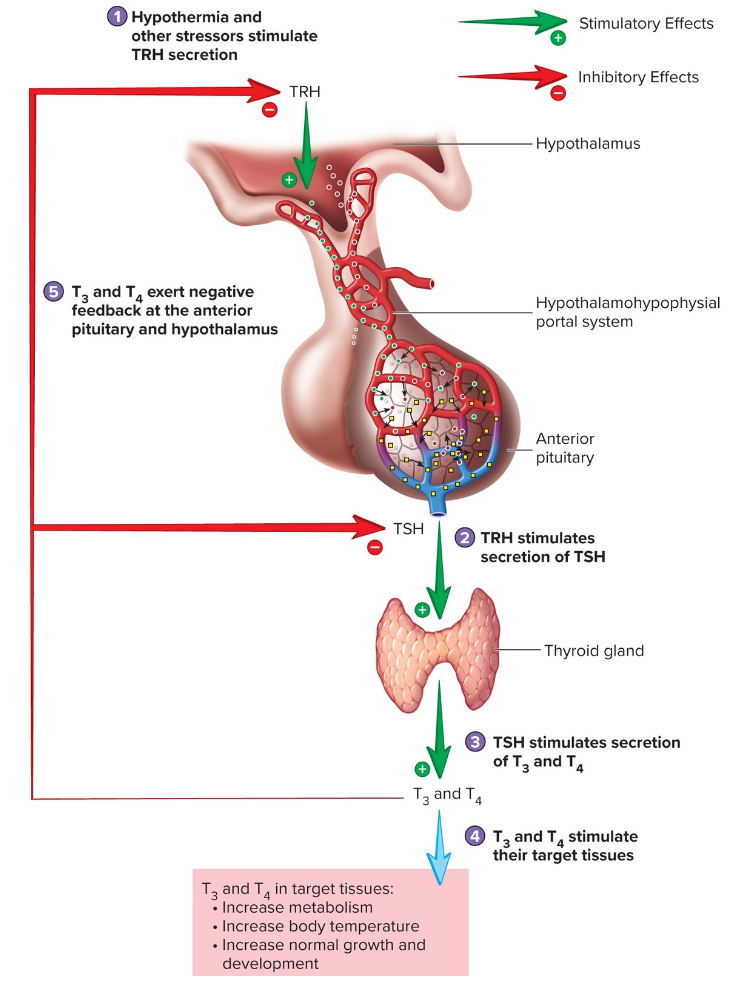
Thyroid Hormone (T3 and T4) Secretion
Hypothermia and other stressors stimulate TRH secretion
TRH stimulates secretion of TSH out of anterior pituitary
TSH stimulates secretion of T3 and T4 from thyroid gland
T3 and T4 stimulate their target tissues (increased metabolism, increased body temp, increased normal growth and development)
T3 and T4 exert negative feedback at the anterior pituitary and hypothalamus
Effects of T3 and T4
Boosts basal metabolic rate.
Enhances oxygen consumption and heat production.
Supports brain development, especially in infants.
Maintains cardiovascular, muscular, and digestive system function.
T3 is released as an active thyroid hormone – no further modification needed, not long-lasting
T4 is released as inactive thyroid hormone – needs further modification at the target, longer-lasting effect.
Adrenal Gland
Inner medulla; outer cortex.
• Medulla: formed from neural crest; sympathetic. Secretes epinephrine and
norepinephrine.
• Cortex: formed from mesoderm; consists of three zones.
Adrenocorticotrophic Hormone (ACTH)
CRH from hypothalamus causes release of ACTH from anterior pituitary which causes cortisol secretion from the adrenal cortex (a glucocorticoid from the zona fasciculata).
• Environmental stress is a key stimulus for ACTH secretion.
• Primary action is the release of cortisol that regulates stress.
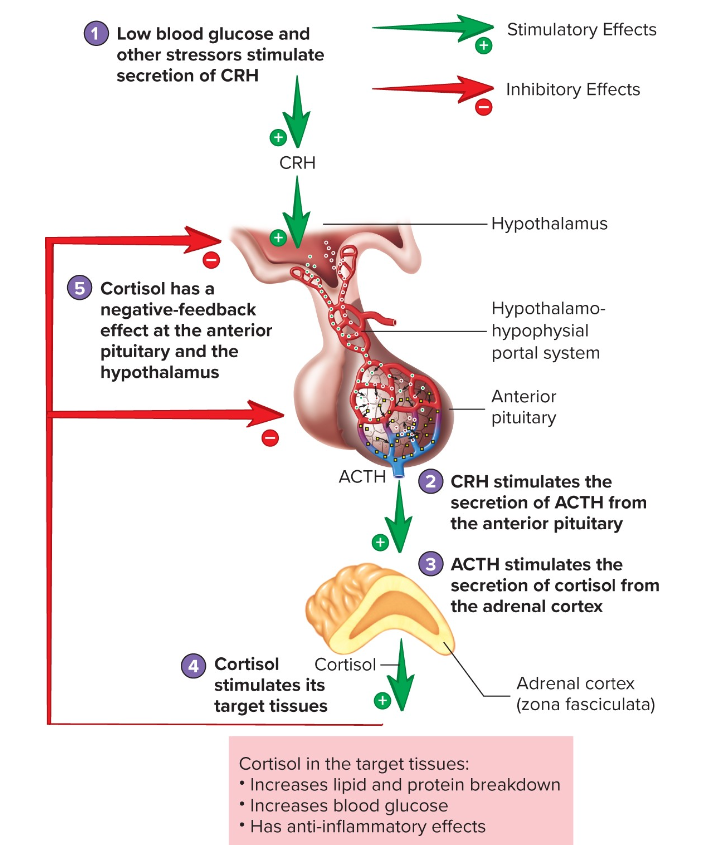
Regulation of Cortisol Secretion
Low blood glucose and other stressors stimulate secretion of CRH in hypothalamus
CRH stimulates the secretion of ACTH from the anterior pituitary
ACTH stimulates the secretion of cortisol from the adrenal cortex
Cortisol stimulates its target tissues
Cortisol has a negative-feedback effect at the anterior pituitary and the hypothalamus
Cortisol target tissues
Increases lipid and protein breakdown
Increases blood glucose
Has anti-inflammatory effects
Pancreas
Exocrine function: produces pancreatic digestive juices
Endocrine function: consists of pancreatic islets
Alpha cells (20%); secrete glucagon.
Beta cells (75%); secrete insulin.
Delta cells; secrete somatostatin.
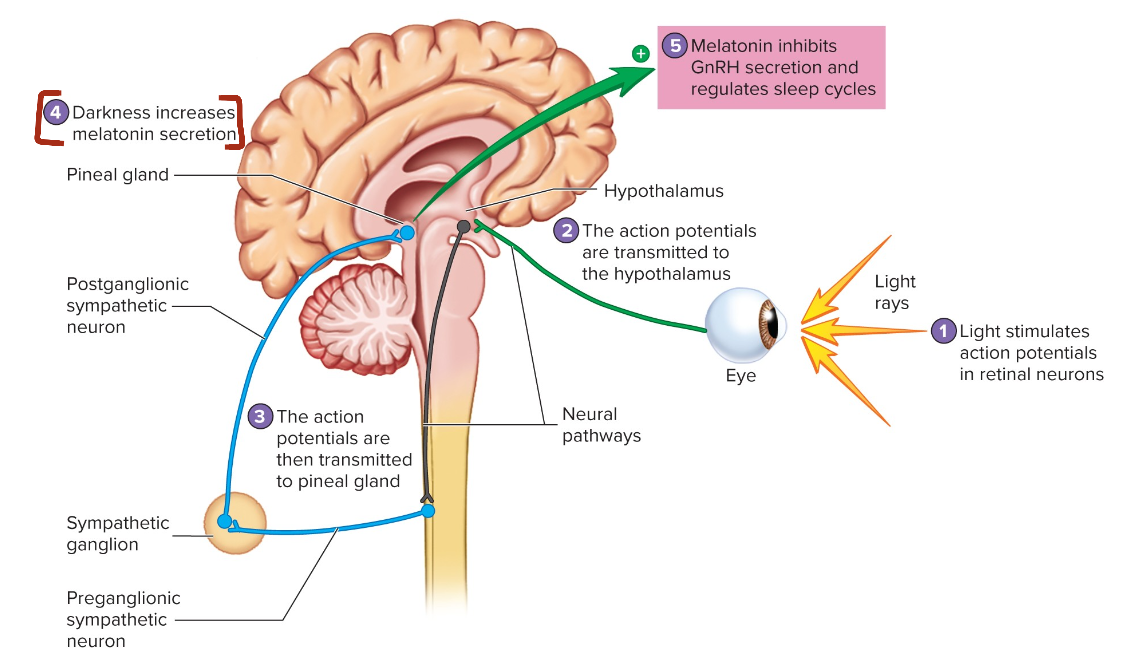
Regulation of Melatonin Secretion from the Pineal Gland
Light stimulates action potentials in retinal neurons
The action potentials are transmitted to the hypothalamus
The action potentials are then transmitted to pineal gland
Darkness increases melatonin secretion
Melatonin inhibits GnRH secretion and regulates sleep cycles
Other Hormones and Chemical Messengers
Hormones of the Thymus: Thymosin. Development of the immune system.
Hormones of the G I tract: Several hormones regulate digestion and enzyme secretion.