pnb 2265 exam 3 practice questions
1/92
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
93 Terms
What is the primary purpose of mechanical digestion in the mouth?
To chew food into smaller pieces, increasing surface area for digestive enzymes to work.
What are the components of saliva and their functions?
Water, fluoride, bicarbonate (neutralizes acid), lysozyme (breaks down bacteria), and salivary amylase (begins carbohydrate digestion).
What is a bolus?
Chewed food mixed with saliva.
What is the function of the lower esophageal sphincter (LES)?
It remains closed to prevent acid reflux and relaxes to allow food to enter the stomach.
What is achalasia?
A disorder where the lower esophageal sphincter fails to relax, preventing the bolus from entering the stomach.
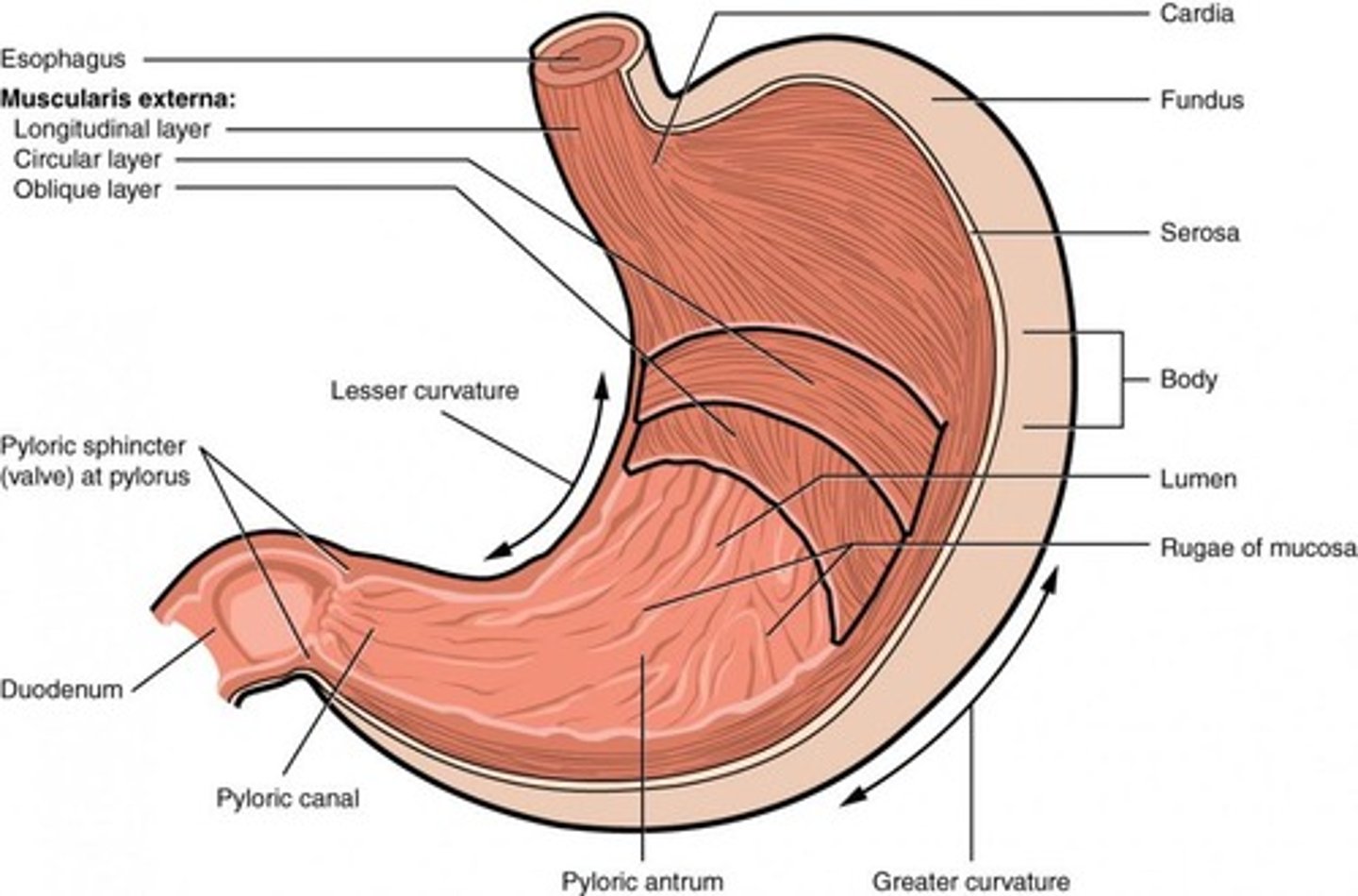
What is the function of the stomach's oblique muscle layer?
It provides extra force for mechanical digestion.
What do chief cells secrete?
Pepsinogen and gastric lipase.
How is pepsinogen activated?
It is converted into active pepsin when mixed with hydrochloric acid.
What is the role of intrinsic factor?
It helps the body absorb vitamin B12.
What is the function of the proton pump (H+/K+ ATPase) in parietal cells?
It uses ATP hydrolysis to secrete H+ ions into the stomach lumen to form hydrochloric acid.
What is the role of somatostatin in gastric acid regulation?
It acts as a negative feedback signal to inhibit acid production by parietal cells.
What is receptive relaxation in the stomach?
The process where the fundus and body of the stomach stretch to store food.
Why is the stomach not a primary site for nutrient absorption?
It lacks villi and a brush border, though it does absorb alcohol and aspirin.
What is the function of the alkaline mucus barrier in the stomach?
It protects the stomach mucosa from damage by hydrochloric acid.
What is the role of CCK (Cholecystokinin) in digestion?
It is released in response to fats to slow gastric emptying and stimulate pancreatic lipase.
What is the function of secretin?
It is released in response to low pH and stimulates the pancreas to secrete bicarbonate to neutralize stomach acid.
What is dumping syndrome?
A condition where stomach contents are emptied into the duodenum prematurely, often associated with gastric bypass surgery.
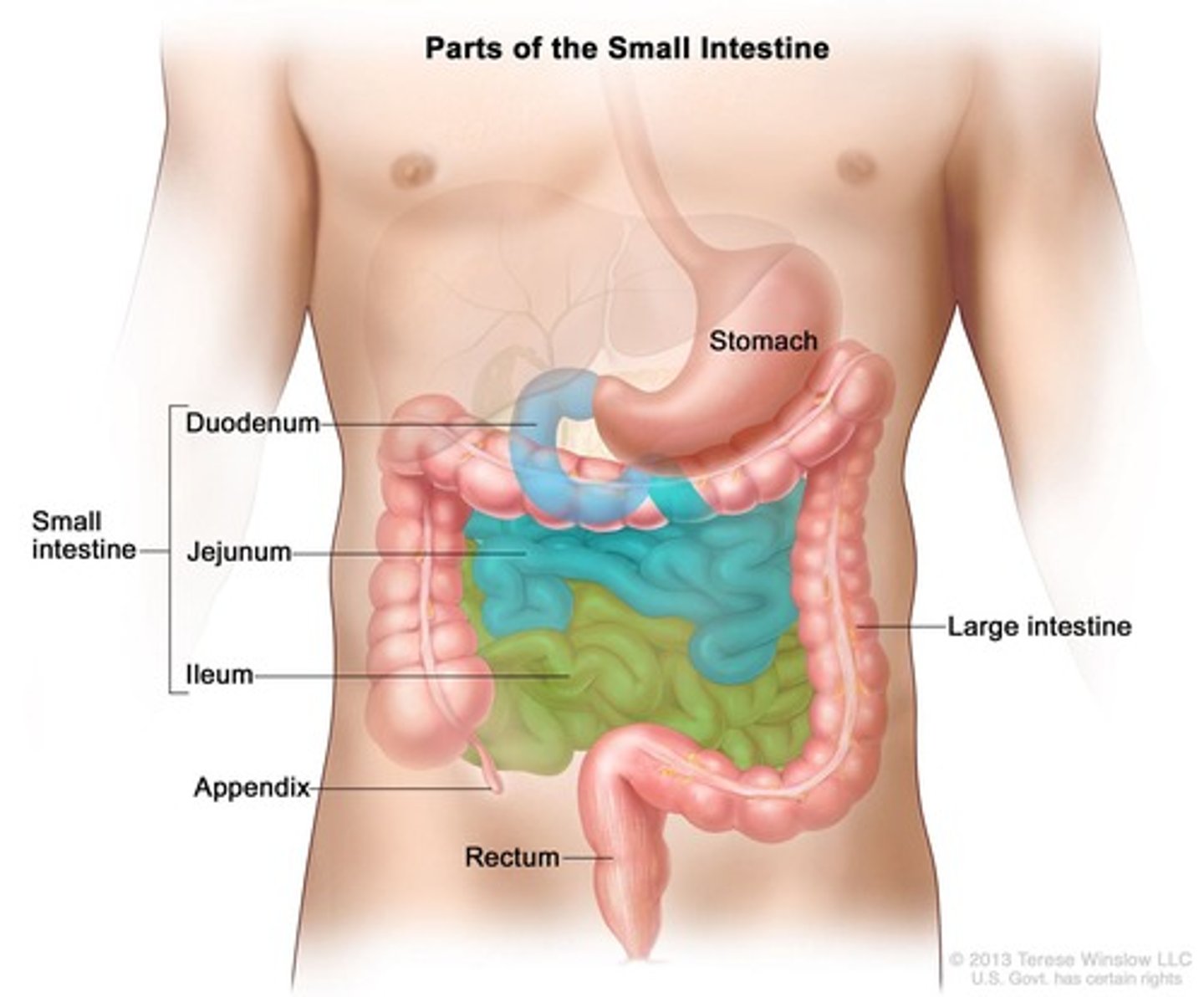
What are the three sections of the small intestine?
Duodenum, jejunum, and ileum.
What is the migrating motor complex?
A strong wave of peristalsis that occurs during fasting to clear the small intestine of remaining substances.
Why are pancreatic enzymes secreted as zymogens?
To prevent autodigestion of the pancreatic tissue.
What is the function of bile?
It is produced by the liver and stored in the gallbladder to emulsify fats.
What is the role of the common bile duct?
It carries bile from the liver and gallbladder to the duodenum.
What are haustra?
Small pouches in the large intestine caused by the contraction of the taeniae coli muscle bands.
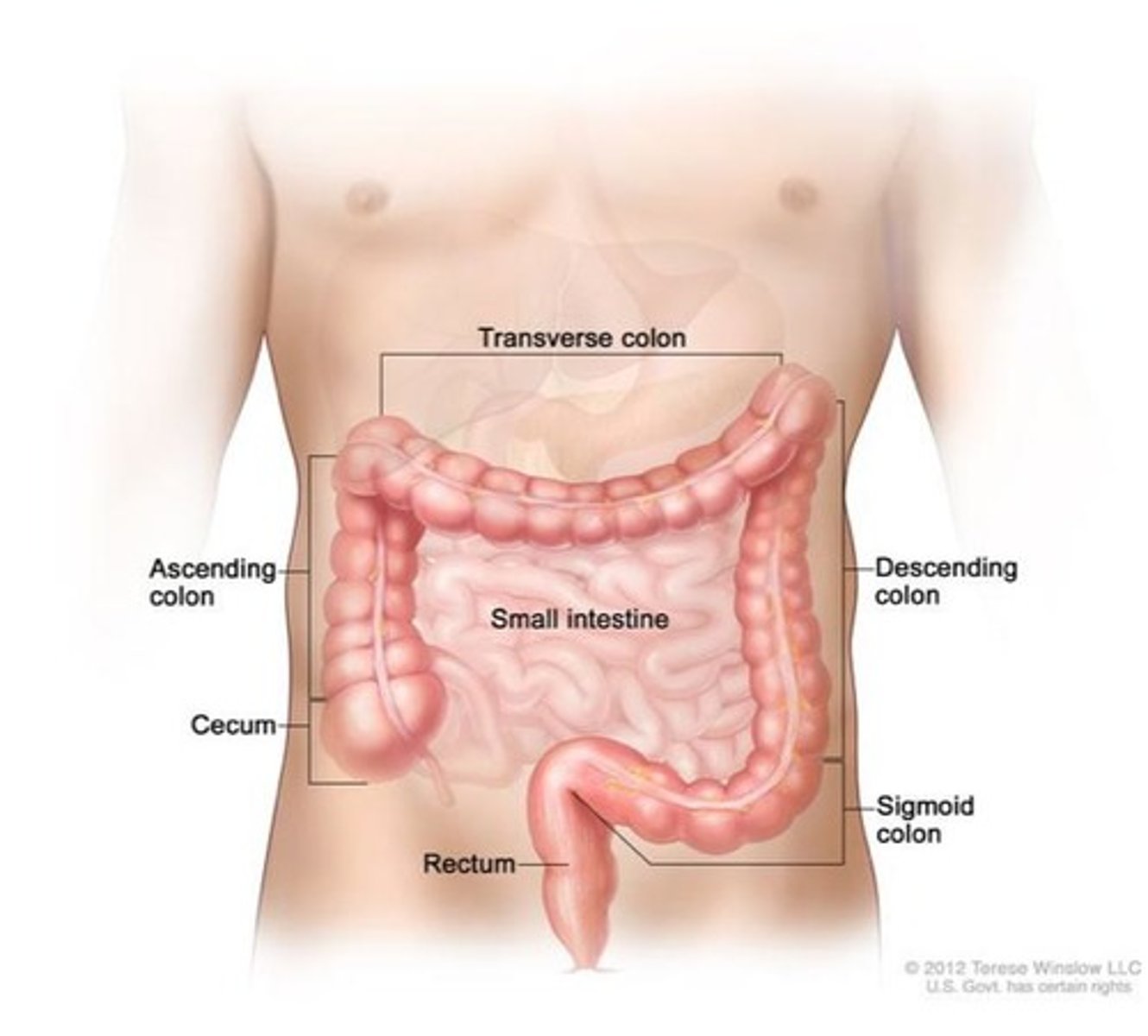
What is the primary function of the large intestine?
Absorption of water and electrolytes, and the formation of feces.
What triggers the defecation reflex?
The stretching of the sigmoid colon and rectum.
What is the difference between the internal and external anal sphincters?
The internal sphincter is smooth muscle under involuntary control, while the external sphincter is under voluntary control.
How does the stomach regulate gastric emptying?
By coordinating the contraction of stomach muscles with the relaxation of the pyloric sphincter via the nervous system.
Amino acids absorbed in the small intestine will follow what path?
Villus capillary - hepatic portal vein - liver lobule - hepatic artery
A pyruvate dehydrogenase (the enzyme that breaks down pyruvate) deficiency could be treated by
Ketogenic diet (increasing fat metabolism and ketone production to convert to ACH)
All of the following are true about leptin except
Leptin activates neurons in the solitary tract of the hypothalamus
2 multiple choice options
The majority of nutrient absorption in the digestive system occurs in the
jejunum
all of the following will lead to increased phosphorolation of the proton pump except?
Muscarinic receptor inhibition (somatostatin)
3 multiple choice options
In skeletal muscles, amino acids undergo betaoxidation to form ach
false
The "alkaline tide" is created by the _________________ on the ______________.
CL/HCO3 exchanger; basolateral membrane of parietal cells
The rate of gastric emptying can be increased by
inhibiting smooth muscle with vasoactive intestinal peptide (VIP)
Salivary amylase produces ____________; pancreatic amylase produces ___________
Disaccharides; disaccharides
Lipoprotein lipase is unique from pancreatic lipase because:
pancreatic lipase is found in the lumen of the small intestine
fructose crosses the apical membrane of enterocytes via _______ and rhe basolateral membrane via ______
DIffusion; diffusion
What structure is made from skeletal muscle
the UES
During the absorptive state, which of the following nutrients is NOT stored inside the body?
Protein
achalasia treatment
blocking smooth muscle calcium channels
Don Draper visited his primary care doctor, complaining of heartburn. His doctor explained that his habitual use of whiskey and cigarettes led to the development of ________________ caused by _______________.
reflux, reduced esophogeal pressure
is smooth muscle contraction stimulated by camp?
False
What vessel brings nutrients from the small intestine to the hepatocytes
hepatic portal vein
The absence of this would prevent the breakdown of EtOH (ethanol) into acetylaldehyde.
alchohol dehydrogenase
Haustra are produces by the contraction of
taenia coli
The fundus of the stomach relaxes as food enters. This process is called:
adaptive relaxation
Low density lipoprotein (LDL) transports cholesterol ____________________. If the levels of LDL become too _____________________, the risk of cardiovascular disease increases.
Away from the liver, high
what channel is located on the apical surface of a duct cell?
CFTR
Hydrochloric acid secretion ______________ when __________________ .
increases, calcium increases
What stimulates the mmc
fasting
Peristalsis is the result of ____________________ relaxation and ____________________ contraction.
distal, proximal
The sodium/hydrogen exchanger is located on the __________________ surface of _____________ cells.
basolateral, duct
chemical digestion begins during what phase
cephalic
The myenteric plexus is located in which of the following tissue layers
muscularis externa
Sequence the following digestive structures in the order that they would be encountered by a food particle
deudonum - 1
descending colon -2
ileium -3
pyloric sphincter - 4
chief cells are reponsible for secreting
endopeptidases
What is primarily associated with the post-absorptive state
gluconeogeneisis
Anatabuse is a drug used to treat alcohol use disorder. When taking this drug, indiduas that consume any alcohol have rapid responses that include headaches and vomiting. What enzyme does anatabuse inhibit?
acetylaldehyde dehydrogenase
what enzyme is associated with the absorptive state
glycogen synthase
As a component of her annual check up, leanes NP ordered a metabolic panel. the test results indicate abnormal cholesteral levels in her blood put her at risk for atherosclerosis and cardiovascular disease. What would explain this?
Abnormally low HDL
What creates involuntary changes in the anal and sphincter muscle?
decreased parasympathetic activity on the internal anal sphincter
breast fed indiviuals develop passive immunity to certain pathogens by ingesting antibodies. What digestive process is this?
endocytosis
Order these layers from apical to basolateral
1. circular layer
2. serosa
3. longitudinal layer
4. myenteric plexus
5. epithelial cells
cck _____ neurons in the arcurate nucleas and ______ neurons in the paraventricular nuclei
stimulates, inhibits
cck is released from the _____ and bind to ____ receptors
sm intestine, gallbladder
Blockage of what structure would most be likely to cause autodigestion
pancreatic duct
protein digestion beings in the _____, protein absorption begins in the _____
stomach, sm intestine
What transporter is responsible for moving glucose and fructose by facilitated diffusion
GLUT 2
Piper has started a new weight loss medication. this drug also binds to hydrogen ions, preventing them from reaching the brush border. what would most likely be the side effect
hypoglycemia
peristalsis is an example of ____ smooth muscle contraction. Segmentation is an example of _____ smooth muscle contraction
Phasic, Phasic
Activation of stretch receptors in the stomach leads to _____ relaxation. Activation of stretch receptors in the esophogus leads to ____ relaxation
adaptive, receltpive
insulin is released from ____ located in _____
beta cells, pancreatic islets
secretin release is stimulated by _____ and leads to ______
low ph, secretions from the pancreatic duct
smooth muscle contractions would be increased by
GQ coupled receptors
Secretory epithelia are found primarily in the ______________; Parietal cells are secretory epithelia in the _______________.
Mucosa; Stomach
which of the following is not a correct function of the digestive system?
the elimination of indigestible substances from the body through the kidneys
3 multiple choice options
What describes the small intestine?
The primary site where enzymes and bile complete digestion and nutrients are absorbed
What statement about accessory organs is false
The liver produces bile to emulsify fats, stores it, and releases it directly into the small intestine
3 multiple choice options
A surgeon is operating in the abdominal cavity and notices the outermost
layer of a digestive organ. Which of the following statements about this
layer is true?
. It protects the organ and reduces friction as it moves within the abdominal cavity
3 multiple choice options
A patient suffers damage to the muscularis layer of the small
intestine. Which of the following problems is most likely to occur
Impaired signaling to the brain about gut actvitiy
3 multiple choice options
During a biopsy, a patient is found to have damage to the lamina
propria of the small intestine mucosa, the layer directly beneath the epithelium. Which of the following problems is most likely to occur?
neither
3 multiple choice options
A patient has a genetic defect that disrupts transport proteins in the epithelial cells lining the small intestine. Which of the following is most likely to occur?
both
3 multiple choice options
Which of the following statements about where digestion of
macronutrients starts and ends is incorrect?
C. Fat digestion starts in the stomach with gastric lipase and ends
in the small intestine
2 multiple choice options
Which of the following correctly matches monosaccharides with their
transporters for absorption into the intestinal cell (apical side) and into the
blood (basolateral side)?
Glucose - SGLT1 into the cell, GLUT2 into the blood; Fructose - GLUT5 into
the cell, GLUT2 into the blood; Galactose - SGLT1 into the cell, GLUT2 into the
blood
2 multiple choice options
A patient has reduced saliva production due to damage to the
submandibular and parotid glands. Which of the following
problems is most likely to occur?
. Difficulty forming a bolus and initiating swallowing, increasing
the risk of choking
2 multiple choice options
A patient has impaired grinding and mixing of food in the stomach,
leading to poorly formed chyme entering the small intestine. Which of
the following structures is most likely affected
Antrum, which functions in grinding and mixing food before it passes
through the pyloric sphincte
3 multiple choice options
A patient undergoes a procedure that damages the distal portion of the stomach while leaving the proximal stomach intact. After eating, the stomach can still expand to accommodate food, but digestion is impaired. Which of the following is the most likely problem
Impaired grinding and mixing of food due to decreased strong
peristaltic contractions in the antrum
2 multiple choice options
A patient is given a medication that blocks histamine release from
enterochromaffin-like (ECL) cells in the stomach. Which of the following
effects is most likely to occur?
Decreased stomach acid production due to reduced stimulation of
parietal cells
3 multiple choice options
A patient is taking a drug that blocks somatostatin receptors on G
cells and parietal cells. Which of the following effects is most likely
to occur
Both A and B
2 multiple choice options
Regarding stomach motility and neural control during the gastric
phase, which of the following statements is incorrect?
The vasovagal reflex inhibits gastric acid and enzyme secretion
to prevent over-digestion
2 multiple choice options
A patient is diagnosed with dumping syndrome, where chyme moves
too quickly from the stomach into the small intestine. Which of the
following is the most likely cause?
Premature relaxation of the pyloric sphincter, allowing chyme to
enter the duodenum too quickly
2 multiple choice options
A patient has persistently high LDL levels and low HDL levels. Which of
the following statements about their lipid and ketone metabolism is
incorrect
Ketone bodies are produced from carbohydrates in the liver and can
be used by neurons as a backup fuel
3 multiple choice options