topic 11: cardiovascular pt. 1
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
57 Terms
how does the cardiovascular system play an important role in homeostasis?
ensures that oxygen, nutrients, and hormones reach every cell while at the same time is removing wastes
what does the cardiovascular system vital to?
regulating blood pressure
body temperature
immune response to keep body in balance
why is understanding cardiovascular physiology important?
crucial for recognizing how the heart and blood vessels function in health and disease, especially since heart-related conditions are among the leading causes of death worldwide
what are the parts in cardiac physiology?
heart - dual pump with valves
conduction system
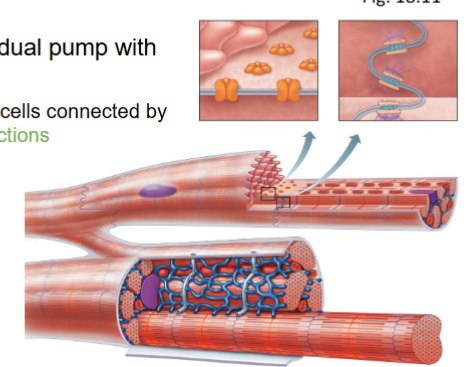
what is the heart?
dual pump with valves
muscle cells connected by gap junctions connecting 2 areas of ISF
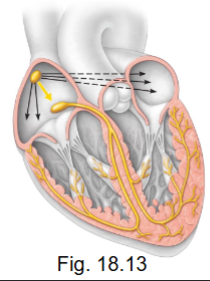
what is the conduction system?
non-contractile cardiac muscle cells - modified to initiate and distribute impulses (APs) throughout the heart
produce APs spontaneously (no stimulus) BUT at different rates (make faster and slower, space b/w AP)
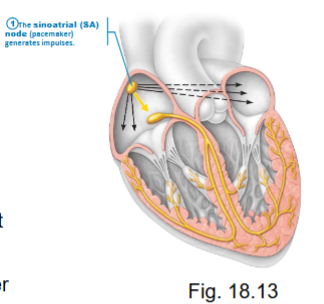
what are the parts of the conduction system?
sinoatrial (SA) node - right atrium
atrioventricular (AV) node - right atrium
bundle of HIS (AV bundle)
Purkinje fibers
how does the AV node contribute to the conduction system?
rate = 100 APs/min (modified by PSP to be 75 APs/min at rest)
produced APs faster than other areas therefore is the pacemaker
how does the AV node contribute to the conduction system?
rate = 50 APs/min
on its own, so can have HR with no SA node but it would be a slower heart rate
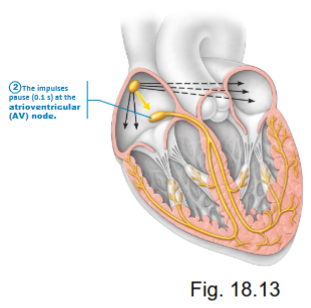
how does the bundle of HIS contribute to the conduction system?
originated at AV node
ONLY route for electrical activity to go from atria to ventricles and Bundle Branches (right and left)
30 APs/min (too slow to keep you alive)
CT is an insulator → cannot pass conduction through
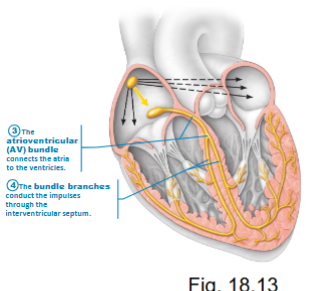
how does the Purkinje fibers contribute to the conduction system?
terminal fibers - stimulate contraction of the ventricular myocardium
30 APs/min
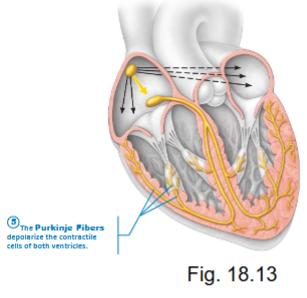
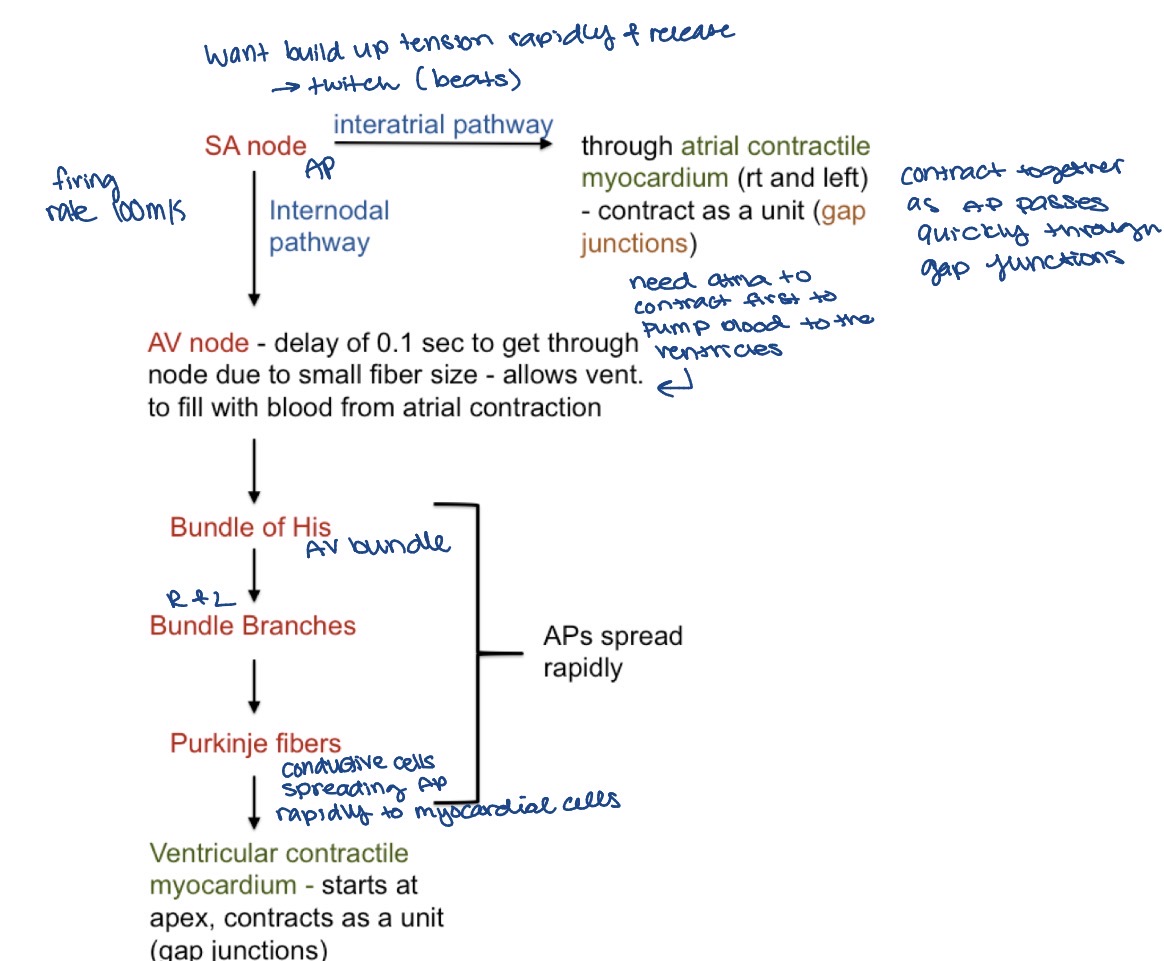
pathway of action potentials in the heart
what happens if the conduction system is damaged?
next fastest part becomes the pacemaker
if SA node is damaged, AV node takes over (atria may not contract + ventricles contract at AV speed = 50 bpm) ok but not good
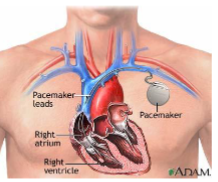
what are artificial pacemakers?
can be used when the conduction system fails
stimulus of SA or AV node damaged (sets up electrical current to reestablish HR)
action potentials of the SA and AV nodes
cells = non-contractile autorhythmic cardiac muscle (self-excitable, don’t have conscious control)
threshold = - 40mv
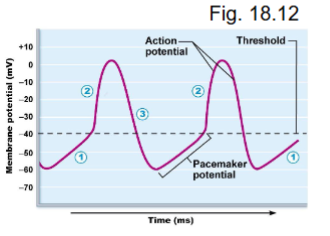
what are the phases of pacemaker activity?
pacemaker potential
AP depolarization
AP repolarization
Na+ channels open at -50mV
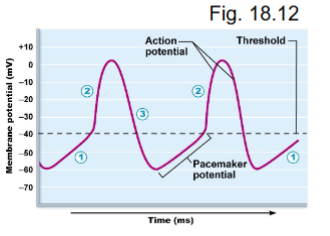
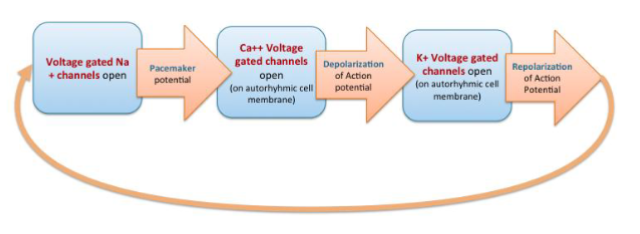
what occurs during pacemaker potential?
low K+ permeability (K+ voltage gates closed)
slow inward leak of Na+ (Na+ voltage gates open)
causes slow depolarization toward threshold (-40mV) (up to 0)
autorhythmic
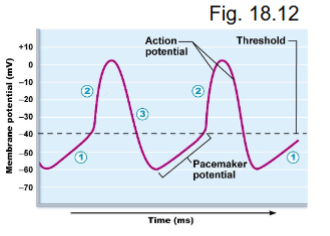
what occurs during AP depolarization?
at threshold → AP
Ca2+ voltage gates open - Ca2+ moves in → depolarization (Na+ voltage gates close at threshold so are NOT involved in AP)
Ca2+ voltage gates close at peak (~0mv) (sodium closes at -40mV)
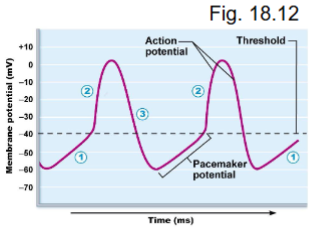
what occurs during AP repolarization?
K+ voltage gated open at peak K+ out → repolarize
K+ gates close below threshold
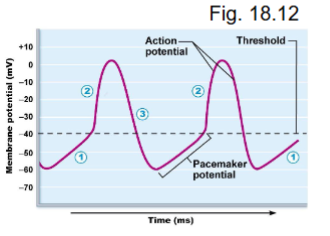
what occurs during the Na+ channels opening at -50mV?
starts pacemaker potential (1) again (continuous cycle)
self propagating APS
does the conduction system have a resting membrane potential?
NO
no relative refractory period because it is self regulating
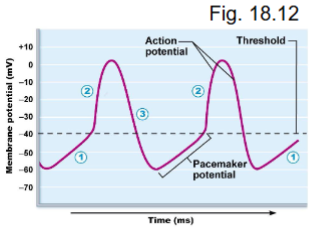
phases of pacemaker activity
APs in ventricular myocardium
cells = contractile
Purkinje fibers AP → ventricular (contractile, they DO have RMP) myocardial AP (spread cell to cell by gap junctions)
resting MP = -90mV
heart needs to relax otherwise would remain contracted
where are pacemaker cells (autorhythmic) found?
SA and AV node
non-contractile
generate AP automatically
where are contractile cells found?
most of heart
atria and ventricles
contract and pump blood
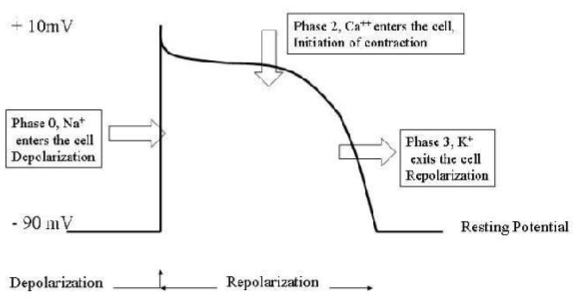
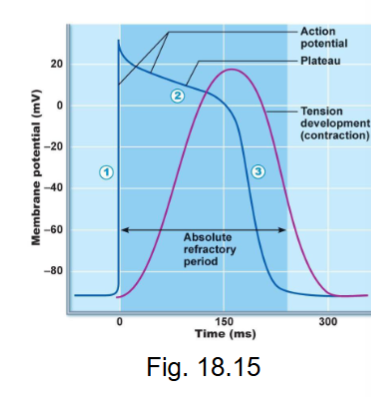
what are the phases of ventricular myocardial
depolarization
plateau
repolarization
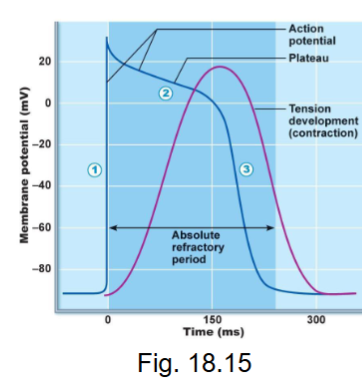
what happens during depolarization in ventricular myocardial APs?
Na+ voltage gates open (fast) = same gates as neuron, skeletal muscle
MP to +30mV
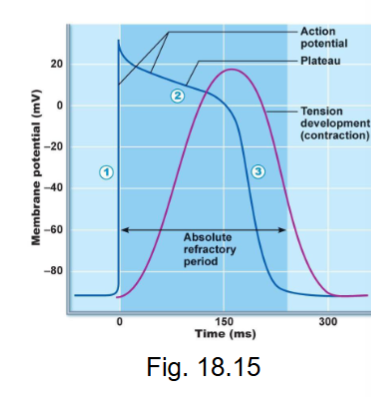
what happens during plateau in ventricular myocardial APs?
Na+ channels close + inactivate (slight drop in MP)no longer letting pos. charges in
Ca2+ slow voltage gates are open (Ca2+ influx maintains depolarization)
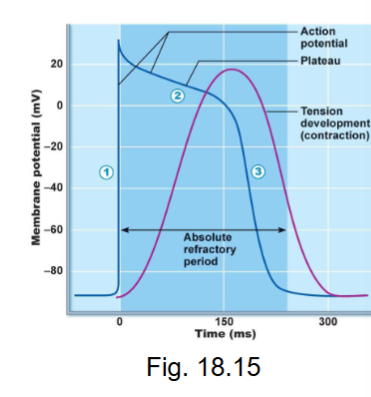
what happens during repolarization in ventricular myocardial APs?
Ca2+ channels close
K+ voltage gated channels open → increase K+ outflux → MP decrease to resting
outflux of potassium
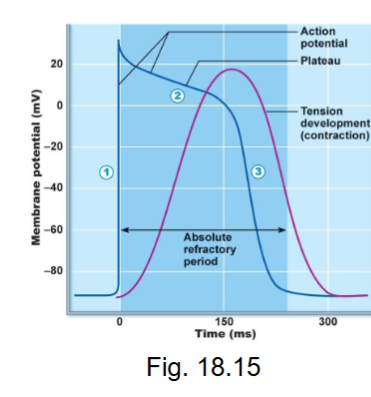
absolute refractory period of ventricular myocardium APs?
long - Na+ channels inactivated until MP is close to -70mV
what is excitation-contraction coupling in myocardial cells
how an electrical signal (AP) causes the heart muscle to contract
what are the steps to the excitation-contraction coupling in myocardial cells?
AP on sarcolemma of contractile cells triggers»>
voltage-gated Ca2+ channels open (plateau of AP) producing a small increase in cytosolic Ca2+ (from ECF). this is not enough to trigger contraction BUT…
Ca2+ binds to chemically-gated Ca2+ channels on sarcoplasmic reticulum (SR) and they open
Ca2+ is released from the SR into the cytosol producing a large increase in cytosolic Ca2+
Ca2+ binds to troponin → troponin-tropomyosin complex moves, exposing myosin binding sites on action; crossbridges form → leads to contraction
contraction
what happens during contraction phase of the excitation-contraction coupling myocardial cells?
sliding filament mechanism
begins a few msec after AP begins
duration of AP = ~250 msec and duration of twitch = ~300 msec
therefore contraction almost over when AP ends
result = NO summation therefore NO tetanus - get alternation of contraction/relaxation
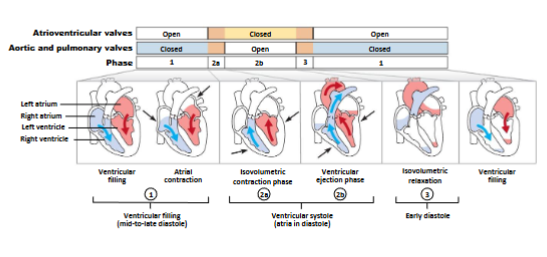
what are the components of cardiac cycle?
electrical activity (ECG)
mechanical activity
blood flow through heart
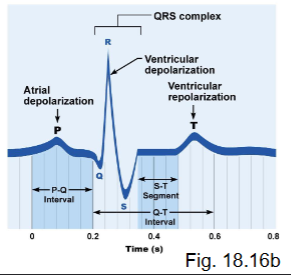
what is electrical activity (ECG)?
small currents due to depolarization/repolarization of the heart move through salty body fluids
how is potential difference measured on the body surface?
using electrode pairs: one pair = a lead
how is an ECG recording seen as?
waves
= sum of electrical activity of ALL myocardial cells (NOT an AP)
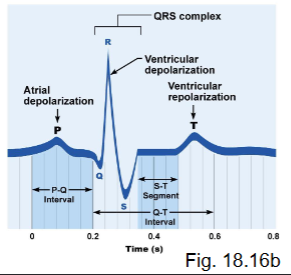
what are the ECG waves?
P wave
QRS wave
T wave
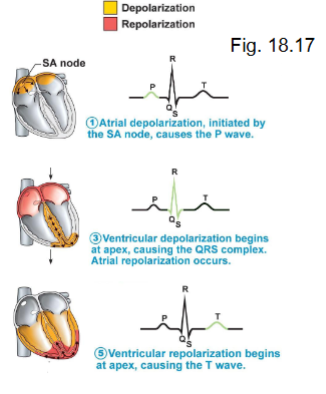
what does the P wave represent?
atrial depolarization → followed by contraction
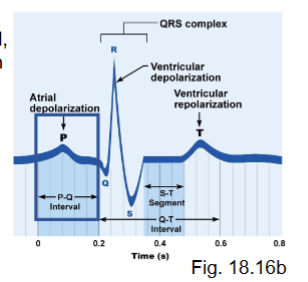
what does the QRS wave represent?
ventricular depolarization → contraction
positive ions entering (Ca2+, Na+)
atrial repolarization is also occurring (leads to relaxation of atria) - the wave created by atrial repolarization is masked by the larger ventricular electrical event (since the ventricles have a larger muscle mass compared to the atria, more cells depolarizing)
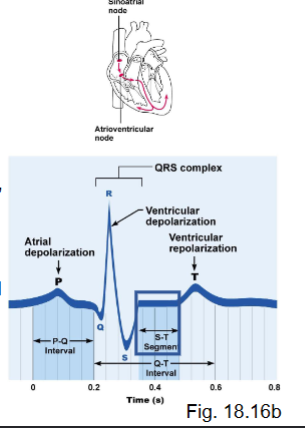
what does the T wave represent?
ventricular repolarization → followed by relaxation
outflux of K+ as it repolarizes
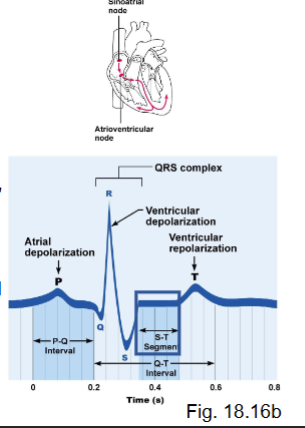
what are the ECG intervals?
P-Q
S-T
T-P
what is the P-Q interval?
atria contracted, signals passing through AV node
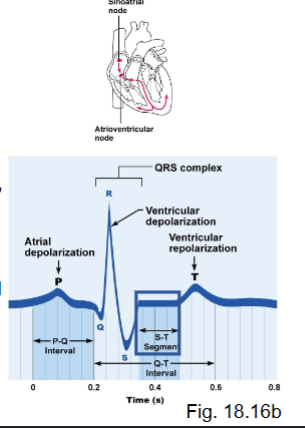
what is the S-T interval?
ventricles contracted, atria relaxed
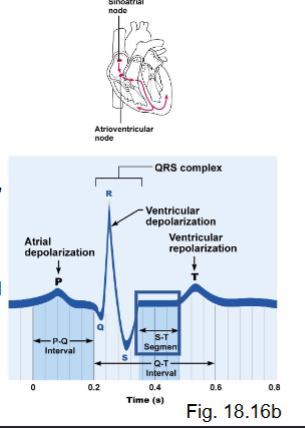
what is the T-P interval?
heart at rest (contractile muscle cells at rest)
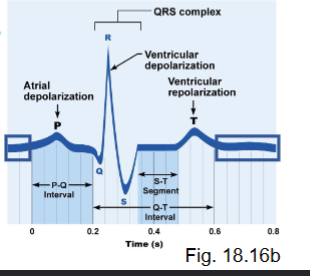
what are abnormalities of heart beat?
tachycardia
bradycardia
heart block
what is tachycardia?
resting HR more than 100bpm (less distance between waves, don’t get proper relaxation)
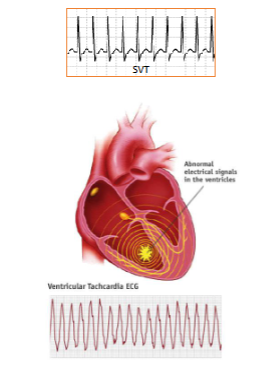
what is bradycardia?
resting HR less than 60 bpm
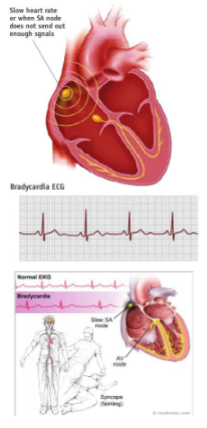
what is heart block?
when conduction through AV node slowed, get an increased P→Q interval → ventricles may not contract after each atrial contraction
not passing AP properly, still can contraction but slow (voltage gated Ca2+ are slow to close)
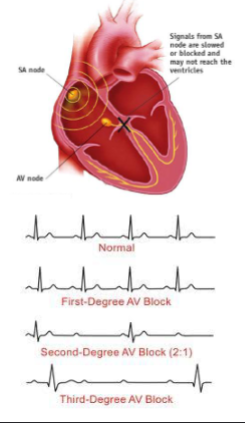
what is an example of heart block?
3rd degree heart block - no conduction through AV node - atria fire at SA node rate (~75 APs/min), ventricles at bundle/Purkinje rate (~30 APs/min)
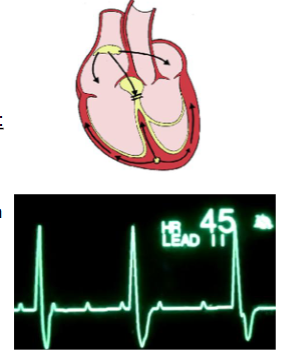
what are the two main events of mechanical activity?
systole
diastole
what is systole?
contraction, emptying (blood should be leaving)
what is diastole?
relaxation, filling (allow to refill)
what are systole and diastole initiated by?
electrical activity
what does 1 complete heart beat consist of?
diastole + systole of atria AND diastole + systole of ventricles
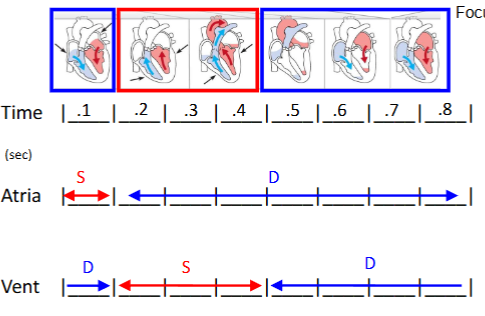
what is the timing of mechanical events?
average resting HR = 75 bpm
therefore 0.8 sec/beat = 1 cardiac cycle (60 sec/min divide 75 beats/min)
in 0.8 sec (start with atrial contraction at time 0)
atrial in systole for 0.1 sec, then diastole for 0.7 sec
ventricles enter systole after atria (0.1 sec delay at AV node) therefore the ventricles begin systole as atria begin diastole → in systole for 0.3 sec, then diastole for 0.5 sec