lecture 7-Profile test
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
Liver/Hepatic Function Test - (LFT)
designed to give information about the state of a patient's liver
Profile (test) for liver disease include:
◦ Bilirubin, ALP, AST, ALT, GGT, LD, TP,Alb., Hepatitis tests
◦ Markers increased in liver problem
reference ranges controls are based on human trends/pools to determine the high risk values
Liver
A secretory and excretory organ
Storage site for iron, glycogen, vitamins and many other substances
Makes plasma proteins (albumin, lipoproteins, coagulation proteins)
Remove toxins from the blood
Secrete bile via bile ducts and gall bladder into the small intestine which helps in digestion
Functions even if onlyy 10% viable
Bilirubin
Waste product formed in the liver and excreted in bile
◦ Produced from broken down RBC; metabolism continues in the liver
◦ Test for liver or gall bladder dysfunction
◦ Increased in patients with jaundice
◦ Increased in babies with HDN
◦ Degraded by light - protect from light and test ASAP
Total serum bilirubin level
Is the sum of the conjugated (direct) and unconjugated (indirect) bilirubin
Reference Range (Total) 2 – 21 μmol/L
Direct bilirubin
is secreted as bile into the intestine and helps with digestion
Direct Reference Range 0 – 6 μmol/L
Icteric (jaundiced) serum
contains high amount of bilirubin – serum is dark yellow to amber
indicates liver damage (like from hepatitis)
ALP (AP) - Alkaline Phosphatase
◦ Increase levels in disorders of the bone, liver (including hepatitis) or the biliary tract
◦ Reference Range 20 – 130 U/L
If this and AST elevated indicate liver issues
AST - Aspartate Aminotransferase
Previously called GOT or SGOT
◦ Enzyme present in liver, skeletal and cardiac muscle
◦ Reflects damage to the liver, and muscles, including the heart
◦ Reference Range 10 – 37 U/L
If this and ALP elevated indicate liver issues
ALT - Alanine transaminase
◦ Enzyme high in hepatocytes (liver cells)
◦ Serum ALT rises dramatically in acute liver damage
◦ More specific than ALP
◦ Reference Range 3 – 30 U/L
GGT - Gamma glutamyl transpeptidase
◦ Found in liver, kidney, prostate tissue
◦ Used to monitor recovery from hepatitis and cirrhosis
◦ Reference Range 3 – 40 U/L
LD / LDH - Lactate dehydrogenase
◦ Found in many body tissues, including the liver – not specific
◦ Elevated levels of LDH may indicate liver damage
◦ Reference Range 110 – 230 U/L
acute liver damage will cause big spike
chronic liver damage/issues will cause not as big spikes
Two major groups of serum proteins are
albumins and globulin
Albumins
make up about 60% of total serum protein
are transport protein
and maintin osmotic pressure
is synthesized in the liver
and therefore is a measure of hepatic function
help to maintain fluid balance in the body
Decreased levels/ hypoalbunminemia can be seen in
liver disease, starvation, impaired absorption
Reference range 38 - 50 g/L
Globulins
make up about 40% of serum/plasma proteins
Included are –
antibodies,
coagulation
proteins and enzymes
Measured according to specific globulin
Total Protein – TP (liver function test profile)
◦ Measure the total amount of protein,
albumin,
and globulin in the blood
◦ Low levels can suggest
a liver or kidney disorder,
malnutrition and malabsorption
◦ Increase levels may be seen with
chronic inflammation
or infections such as viral hepatitis or HIV,
and multiple myeloma
◦ Reference range 60 - 80 g/L
Albumin/Globulin ratio – A/G ratio
◦ Provide a clue as to the cause of change in protein levels
◦ Total protein and albumin are used for the measurement/calculation
A low A/G ratio may reflect
Overproduction of globulins
Underproduction of albumin
A high A/G ratio suggests
Underproduction of immunoglobulins
Bence Jones Proteins/proteinuria
◦ Found in the blood or urine
◦ Finding this protein is often suggestive of multiple myeloma
◦ The proteins are immunoglobulin light chains
◦ Found in urine due to the kidneys' decreased filtration capabilities due to renal failure
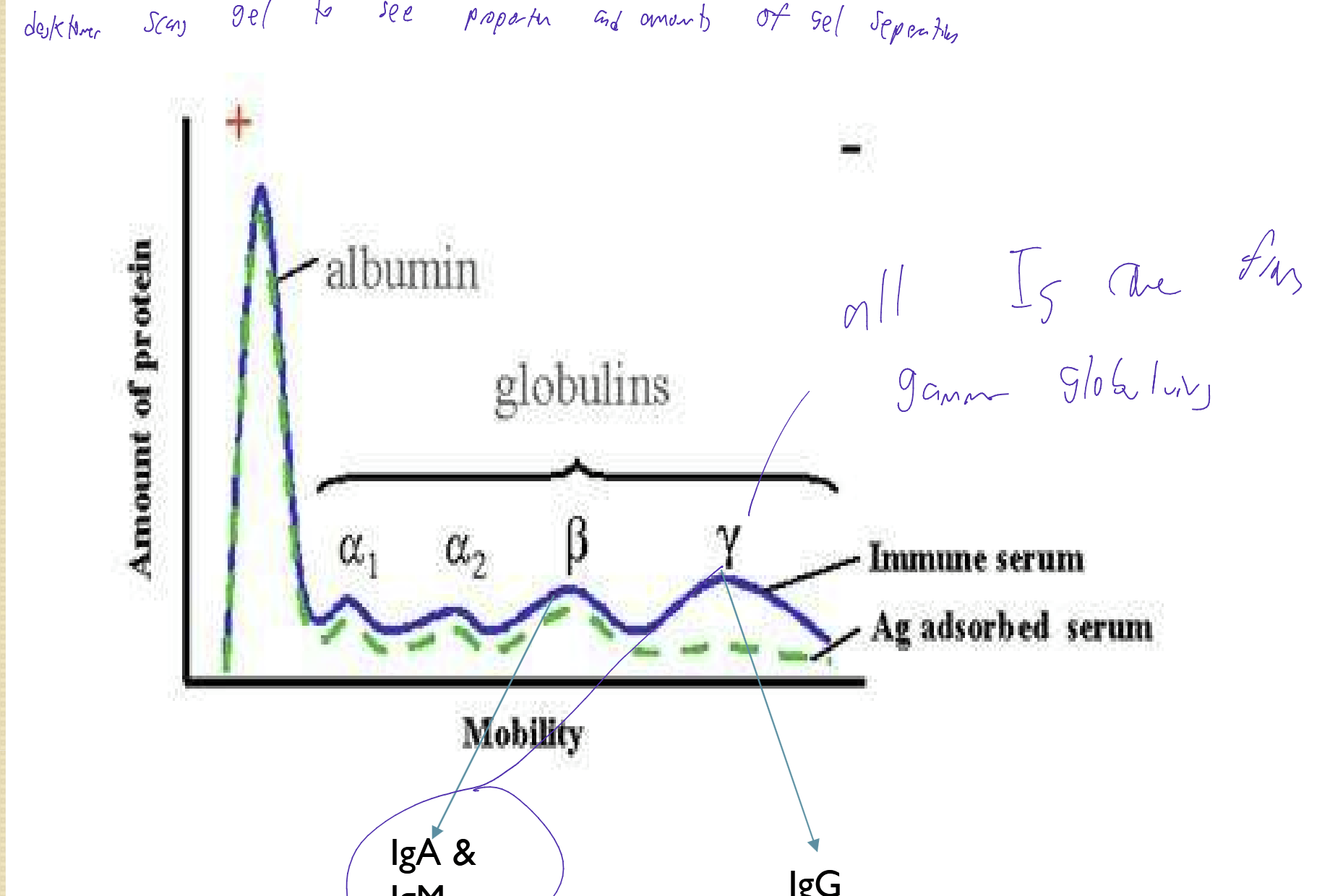
Electrophoresis
is a technique used in laboratories in order to separate macromolecules based on size and charge
Protein molecules can be separated and analyzed
Applies a negative charge, so proteins move towards a positive charge and are separated
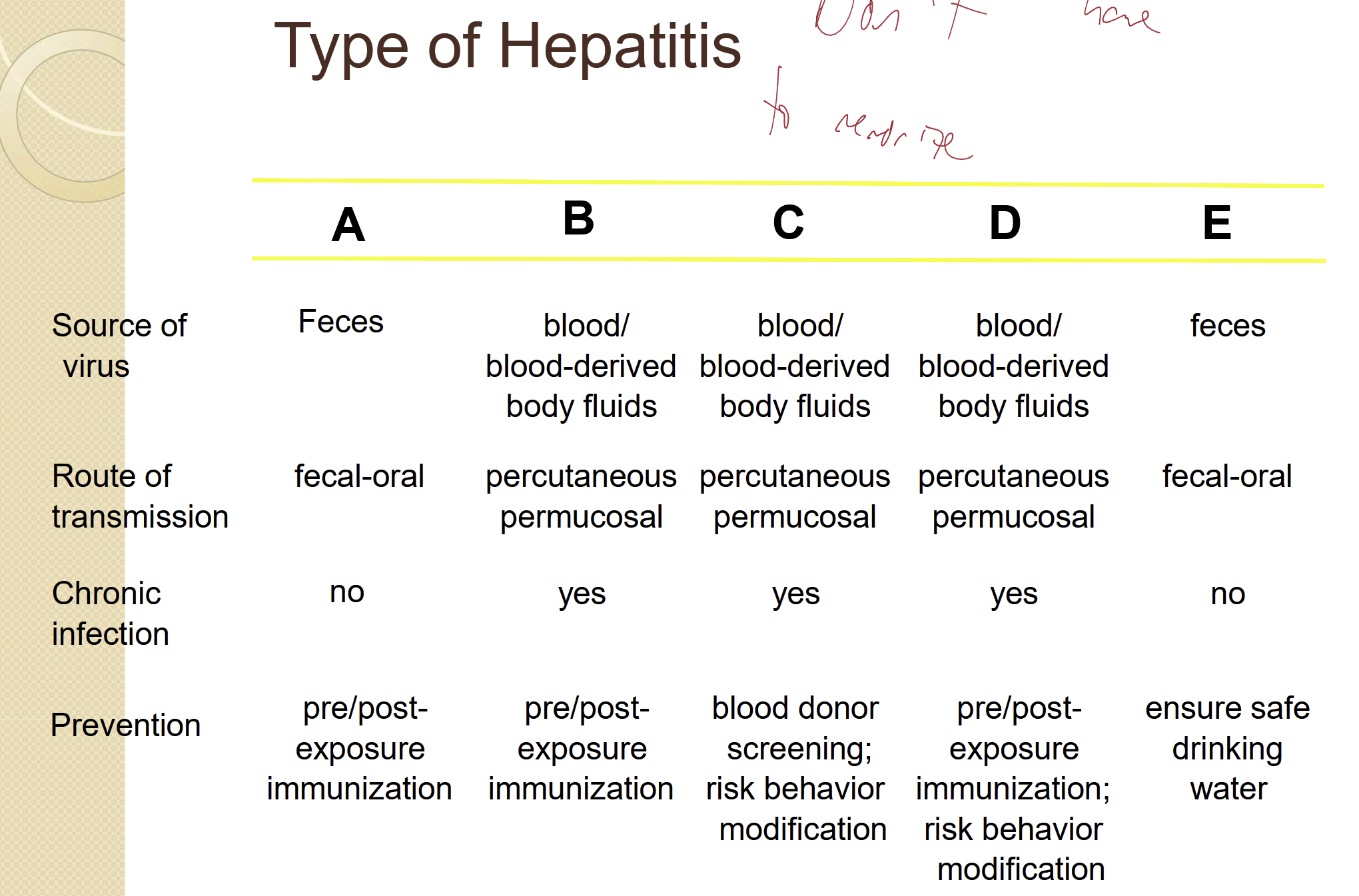
Hepatitis panel
done by PHO
done in chem department
Blood test used to find markers of hepatitis infection
Hepatitis causes inflammation of the liver
Common panel include:
◦ Hepatitis A IgM antibodies (HA Ab-IgM)
◦ Hepatitis B surface antigen (HBsAg)
◦ Hepatitis B IgM core antibody (HBcAb-IgM)
◦ Hepatitis C antibodies (HC Ab)
Reference Range – Negative
Cardiac Profile (Markers)
Substances that are released into the blood when the heart is damaged
Cardiac markers play important roles for diagnosis and therapy for myocardial infarction (MI) and ischemia
Increased in MI
Cardiac Markers Profile:
Troponin I,
CPK/CK,
CK-MB,
Myoglobin,
AST, (Cholesterol)
Specimen collection
Green Top – Heparinized blood
(Gold Top – SST)
Troponin I (cTnI)
◦ A cardiac muscle protein
◦ cTnI is a specific marker for the diagnosis of acute myocardial infarction (AMI)
◦ The most specific of all the cardiac markers
◦ cTnI is released rapidly into the blood after the onset of AMI
◦ Reference Range 0 - 0.4 ng/mL
Creatine Phosphokinase / Creatine Kinase (CPK/CK)
◦ Helps in the diagnosis of myocardial infarction (MI)
◦ Present in muscles (cardiac and skeletal) and the brain
◦ Increased after a heart attack – not specific to heart disease however (due to muscle stresss/death)
◦ Reference Range 30 - 170 U/L
Creatine kinase-MB (CK-MB)
◦ Isoenzyme of CK
◦ Highest percentage found in cardiac muscles– small % in skeletal muscles
◦ CK-MB is released in the circulation following a MI
◦ Reference Range < 6% of total (0 – 5 μ)
not spun down, TAT is usually 1 hour
Myoglobin
◦ Protein found primarily in muscle tissues – cardiac and skeletal
◦ Present in the bloodstream following muscle injury
◦ Useful with the other cardiac markers to diagnose AMI
◦ Reference Range 20 - 90 ng/ml
Lipid Profile
A group of tests ordered together to determine risk of cardiovascular disease (CVD) or stroke
◦ Caused by blockage of blood vessels or hardening of the arteries (atherosclerois)
Most commonly measured lipids are:
◦ Cholesterol/fractions and triglycerides
Fasting for 9 -12 hours before the sample is collected is required
◦ Only water is permitted
Cholesterol
is a steroid, which is a type of fat, found in the blood
produced by the body and also comes from the foods eaten (animal products)
is needed in the
membrane of cells,
organs and tissues in the body
oronary artery
disease
Too much cholesterol leads
coronary artery disease
Blood cholesterol level
is related to the foods eaten or
to genetic conditions (passed down from other generations of family members)
Cholesterol: Endogenous Sources
70% synthesized in the body or stored in the liver
Cholesterol: Exogenous Sources
30% from food (animal source as meat, eggs and dairy products)
test ordered for Cholesterol/fractionst
Total Cholesterol,
LDL,
HDL
and Triglycerides
Cholesterol (Total)
Elevated levels can increase the risk of coronary artery disease, atherosclerosis
◦ Reference Range 3.6 - 6.5 mmol/L
LDL – Low Density Lipoprotein
◦ Often called “bad cholesterol”
◦ Carries cholesterol from the liver to the blood then to organs
High levels of LDL in blood is associated with
atherosclerosis,
heart disease
and myocardial infraction
◦ Reference Range < 2.5 mmol/L
higher # higher chance of blockage
HDL – High Density Lipoprotein
◦ Often called “good cholesterol”
◦ Transport cholesterol from organs and blood to the liver to get rid of it
◦ Removes excess cholesterol from tissues (it cleans the blood)
◦ High levels linked to a reduced risk of heart and atherosclerosis disease
◦ The higher your HDL level, the better
◦ Reference Range > 1.04 mmol/L
Triglycerides
◦ Main form of lipid (fat) storage
◦ Most found in adipose/fat tissue
◦ Provide energy in the absence of carbohydrates
◦ High levels of triglycerides have been linked
to atherosclerosis,
risk of heart disease
and stroke
◦ Reference Range 0.11 - 2.15 mmol/L
Endocrine System
is a system of glands
Each gland secretes a type of hormone directly into the bloodstream to regulate body functions
Cortisol
Thyroid
Cortisol overview
produced by the adrenal glands
but is controlled by the hypothalamus and pituitary gland
the body’s main stress hormone
works with the brain to control mood, motivation and fear
Cortisol Important role
◦ Helps the body respond to stress
◦ Regulates blood pressure
◦ Keep inflammation down
◦ Increase blood sugar
◦ Controls sleep and wake patterns
essential for flight or fight response
but can be maladative
for example spikes during tests
Thyroid Profile/Function
one of the largest endocrine glands in the body which synthesize hormones
The two major thyroid hormones are
thyroxine(T4)
triiodothyronine (T3)
Thyroid hormones control how quickly the body use energy and make proteins
Profiles for Thyroid test for
◦ Free or total T4, T3 and TSH (Thyroid stimulating hormone)
◦ TSH – Hormone that regulates thyroid gland activity
– Stimulates T3 and T4 secretion
Hyperthyroidism
excessive secretion of thyroid hormones
– T4 & (T3
Graves disease
A common cause of hyperthyroidism
a chronic autoimmune disorder where antibodies cause the thyroid to overproduce hormones (hyperthyroidism), accelerating metabolism
Hypothyroidism
Decreased thyroid function/hormones – T4 & (T3)
commonly caused by hashimoto diease
Reference Range for TSH, T3 T4 vary according to age
Adult range
◦ TSH 0.35 - 5.0 μU/L
◦ T4 8.5 – 15.2 pmol/L
◦ T3 3.5 – 6.5 pmol/L
Therapeutic Drug Screening/Monitoring
To determine the presence or absence of specified drugs or their metabolites
Specimen in Biochemistry lab
– blood (serum) and/or urine
usually red top; and no anticoagulant
Could also include hair, sweat, saliva
urine can be used as well
meconium:
a newborn's first, thick, sticky, dark green-black stool, typically passed within 48 hours of birth.
help determine optimum dosage of drug/treatment
can be used for criminal case
if no metabilites of drugs in urine, cant say drug was taken
if whole drug in urine, indicates tamperin
referance range: 0
Example of drugs tested for Drug screening/monitoring
◦ Heart ailments - digoxin
◦ Antiepileptic/seizure- phenytoin (dilantin),
carbamazepine,
valproic acid,
phenobarbital
Analgesic (pain meds) & Anti-inflammatory
(drug testing/monitoring for this conditon)
- acetaminophen, tylenol, salicylate (ASA, aspirin),
Reference Range – Negative
Anti-psychotic/anti-manic
lithium carbonate
Reference Range – Negative
Respiratory ailments (eg asthma)
theophylline
Reference Range – Negative
Antibiotics
gentamicin, amikacin
Reference Range – Negative