Comprehensive Respiratory System: Anatomy, Physiology, and Gas Exchange
1/105
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
106 Terms
What is the major function of the respiratory system?
Respiration, which is gas exchange of O2 and CO2.
What are the four processes involved in respiration?
Pulmonary ventilation, external respiration, transport, and internal respiration.
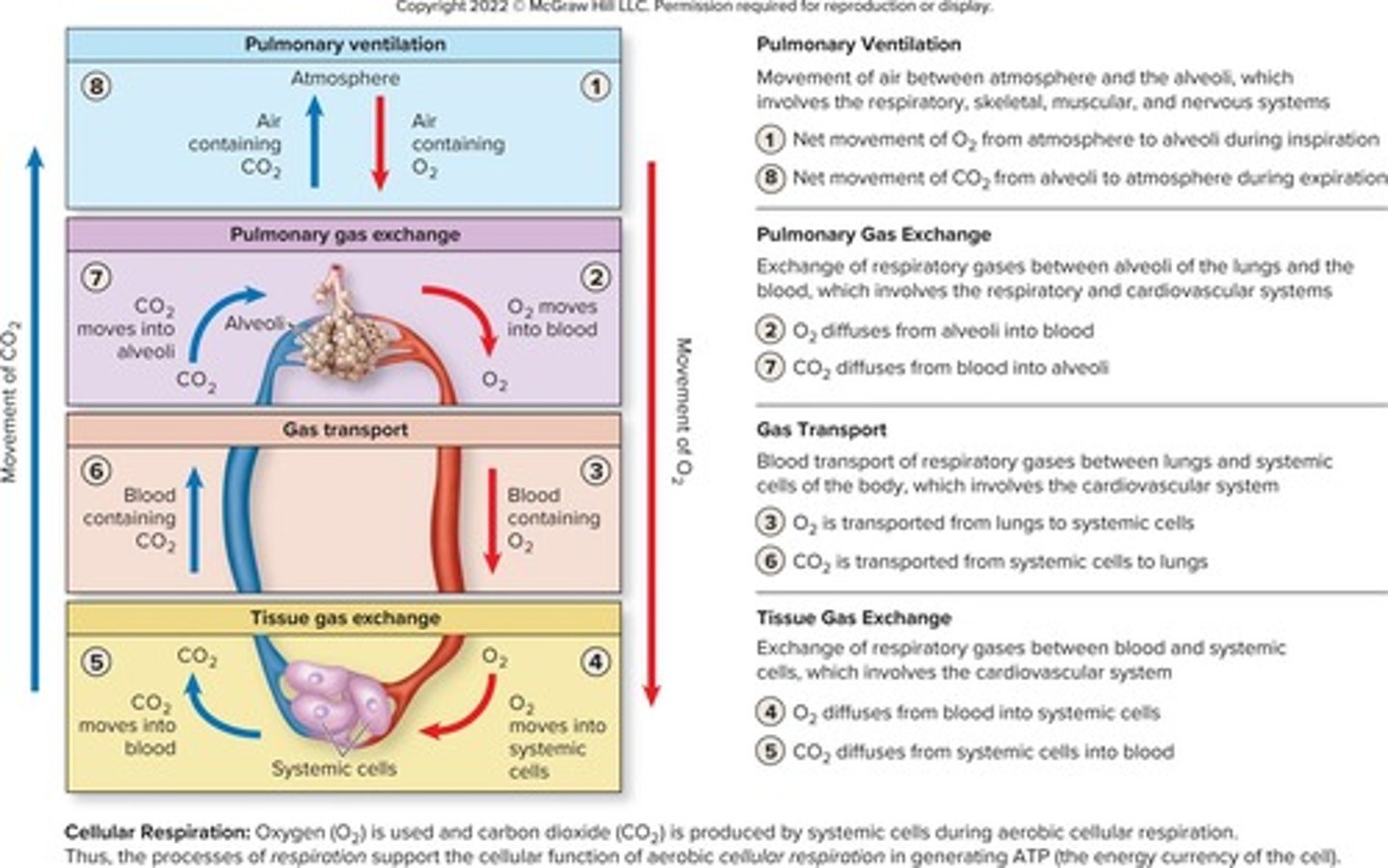
What is pulmonary ventilation?
The movement of air into and out of the lungs.
What occurs during external respiration?
O2 and CO2 exchange between the lungs and blood.
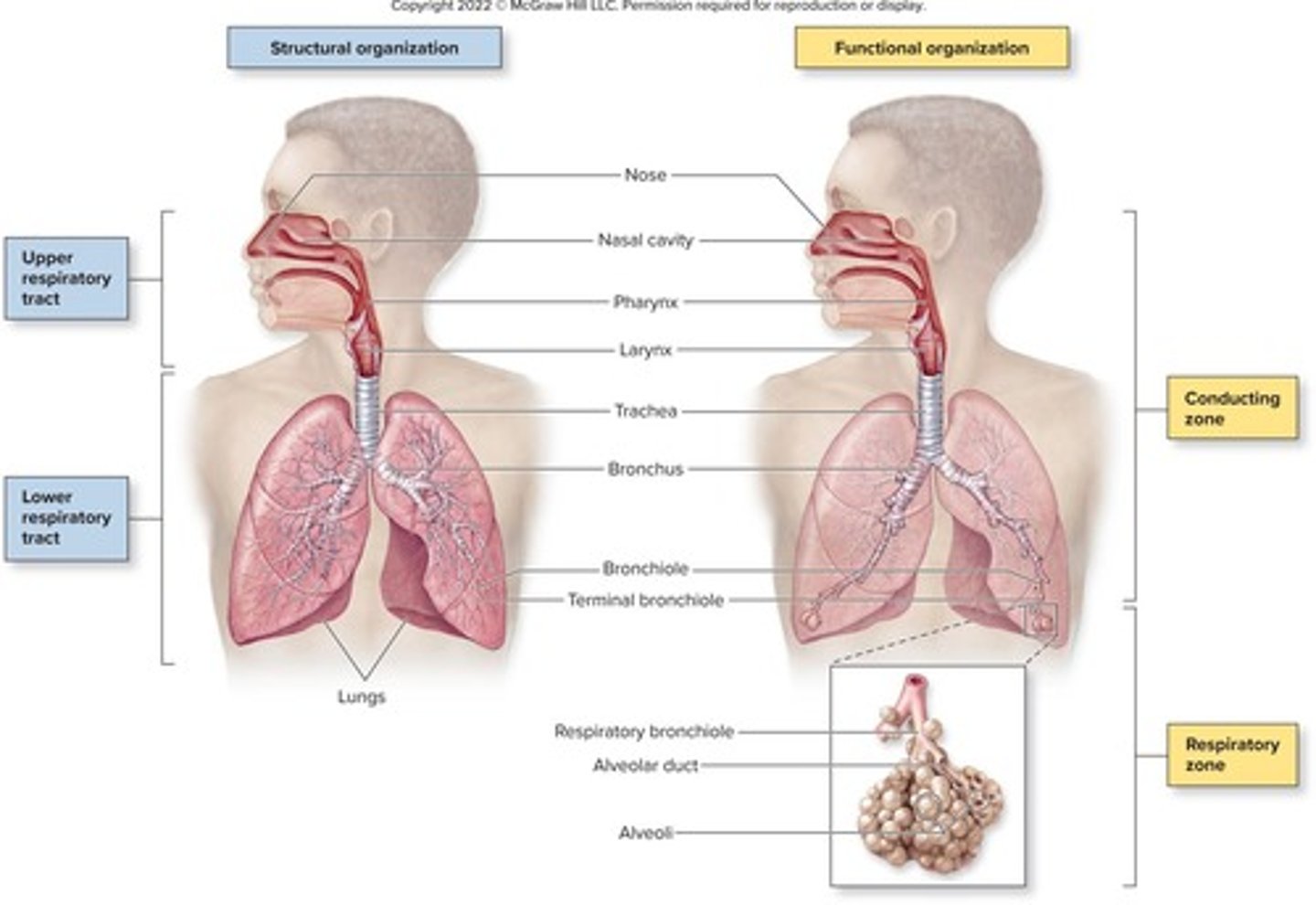
What is the role of the conducting zone in the respiratory system?
It serves as conduits to gas exchange sites, cleansing, warming, and humidifying air.
What structures are included in the conducting zone?
Nose to terminal bronchioles.
What is the respiratory zone?
The site of gas exchange, including respiratory bronchioles, alveolar ducts, and alveoli.
What are the primary functions of the nose?
Provides an airway for respiration, moistens and warms air, filters inspired air, serves as a resonating chamber for speech, and houses olfactory receptors.
What is the nasal cavity divided by?
The midline nasal septum.
What are the nasal conchae?
Three paired bony projections that increase mucosal area and enhance air turbulence.
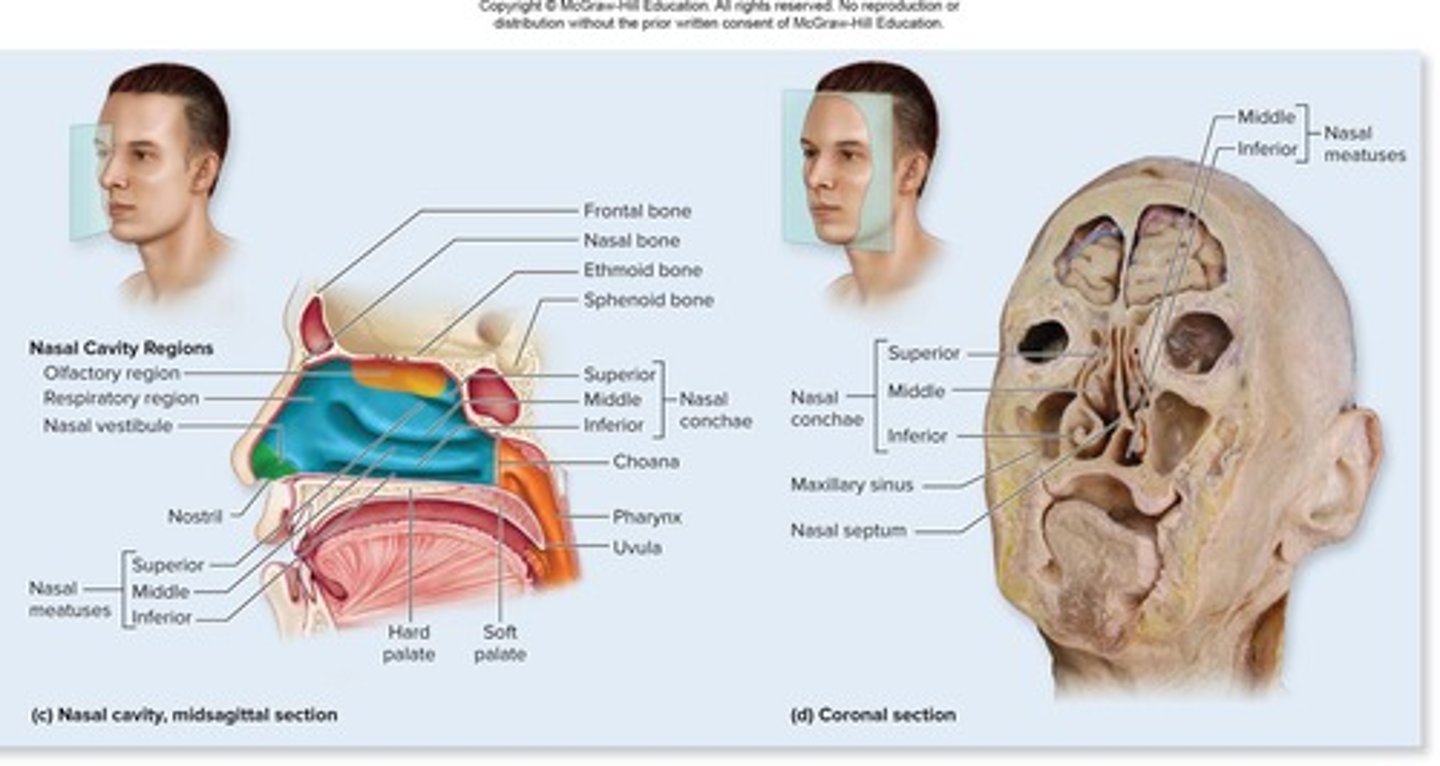
What is the function of paranasal sinuses?
They lighten the skull, secrete mucus, and help warm and moisten air.
What are the three regions of the pharynx?
Nasopharynx, oropharynx, and laryngopharynx.
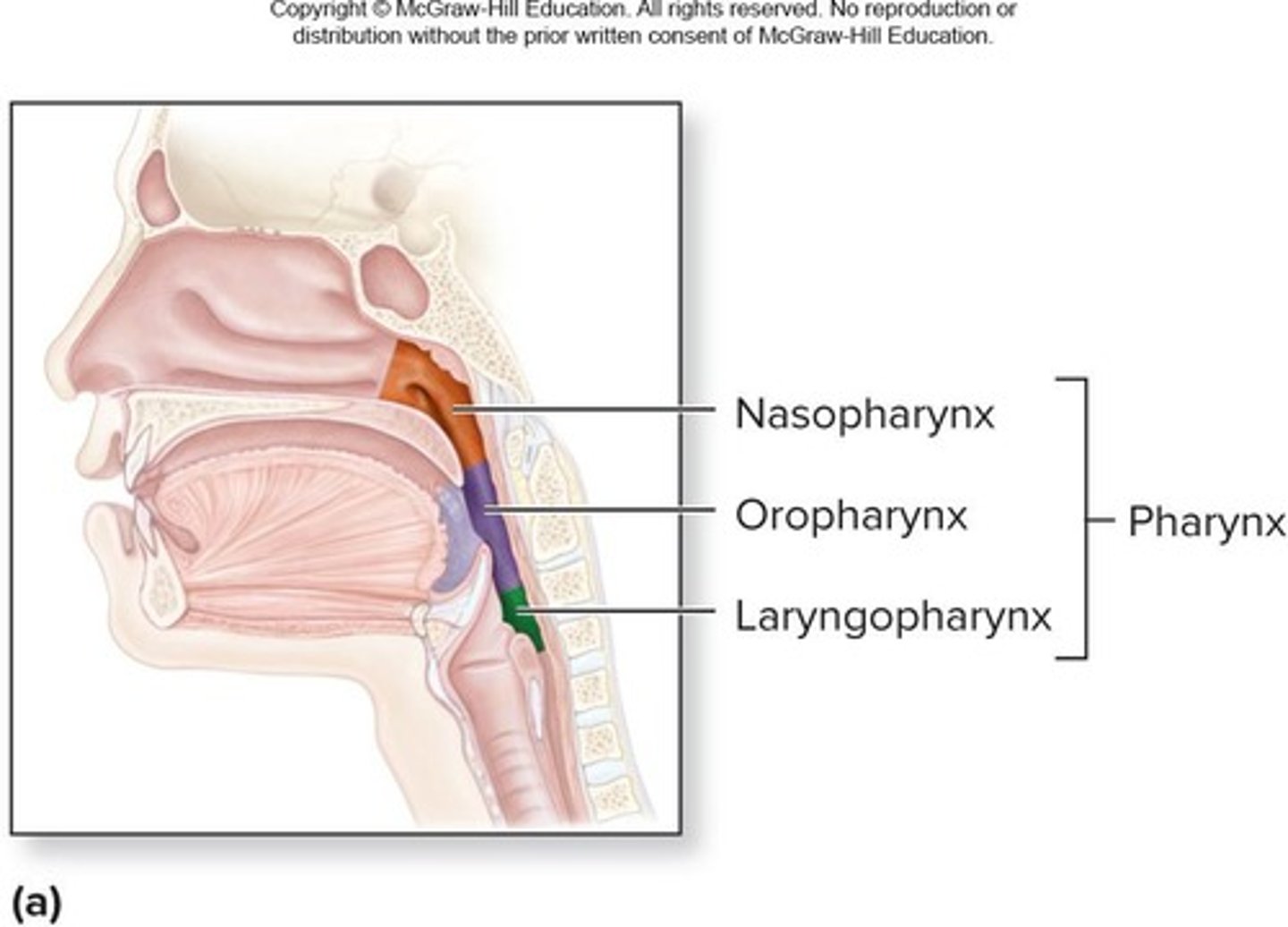
What is the primary function of the larynx?
To provide a patent airway, route air and food, and produce voice.
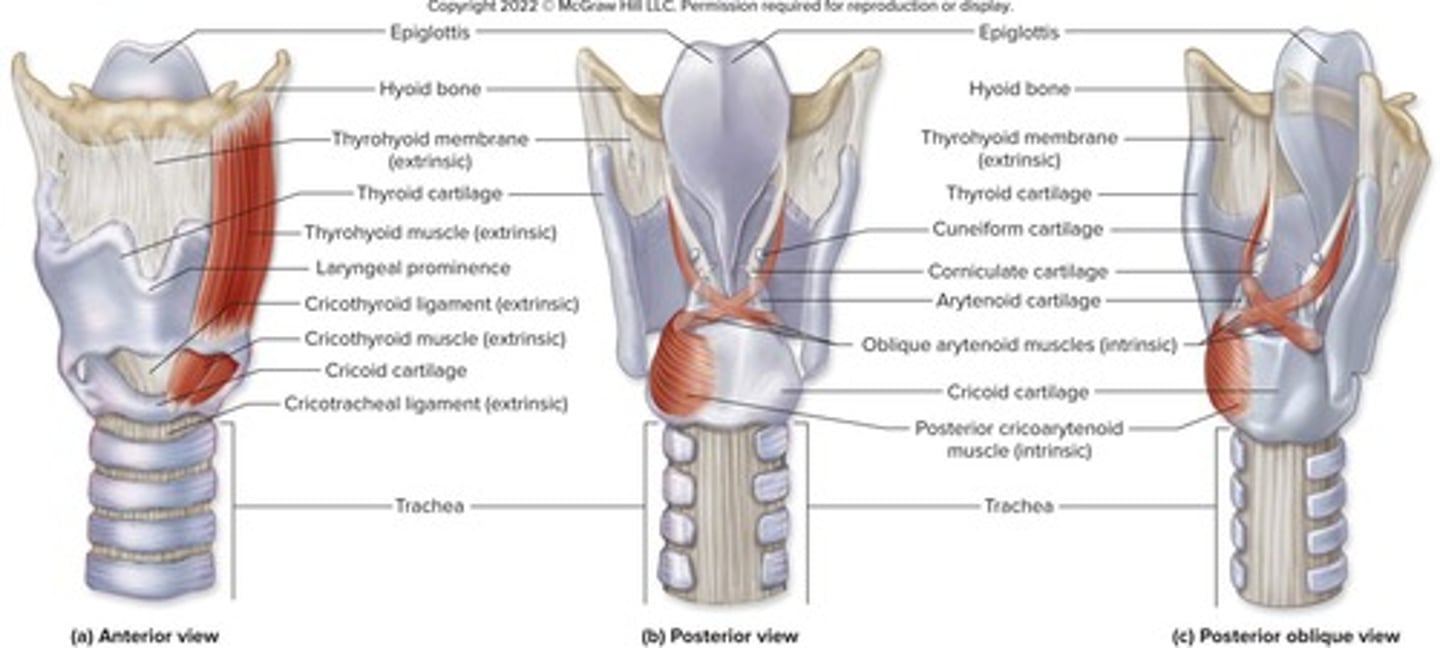
What type of cartilage primarily composes the larynx?
Hyaline cartilage, except for the epiglottis which is elastic cartilage.
What is the glottis?
The opening between the vocal folds.
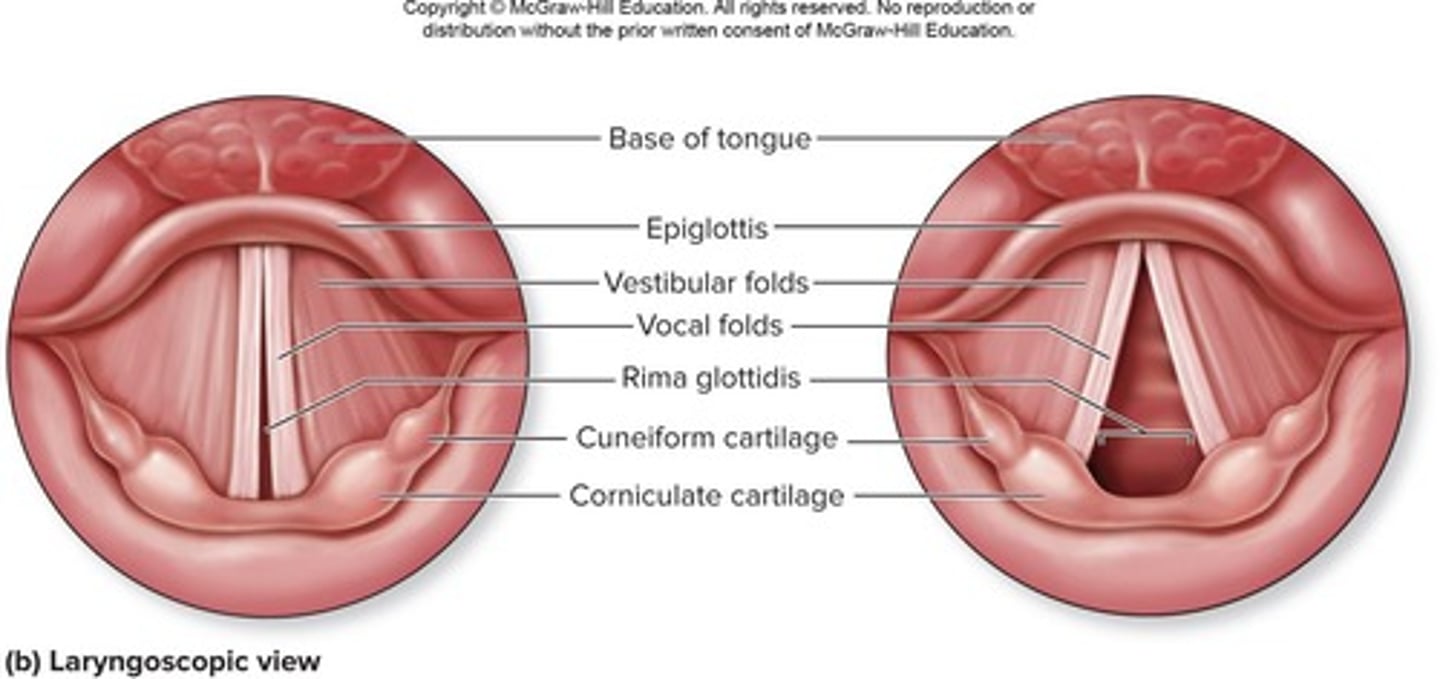
How is pitch determined in voice production?
By the length and tension of the vocal cords.
What is the trachea commonly known as?
The windpipe.
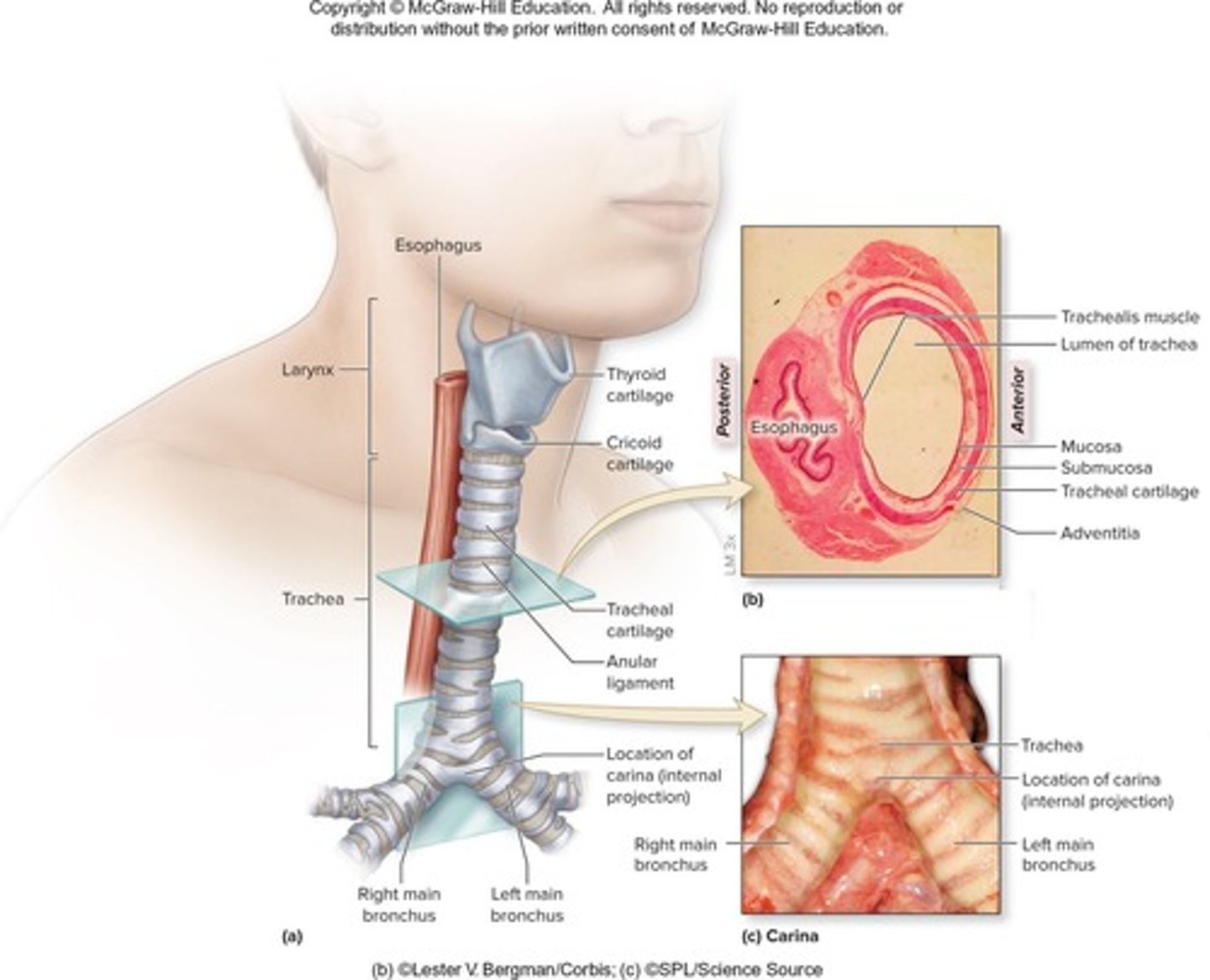
What are the three layers of the trachea wall?
Mucosa, submucosa, and adventitia.
What is the carina?
The internal ridge at the inferior end of the trachea where it splits into two main bronchi.
What is the bronchial tree?
The system of air passages that undergoes 23 orders of branching.
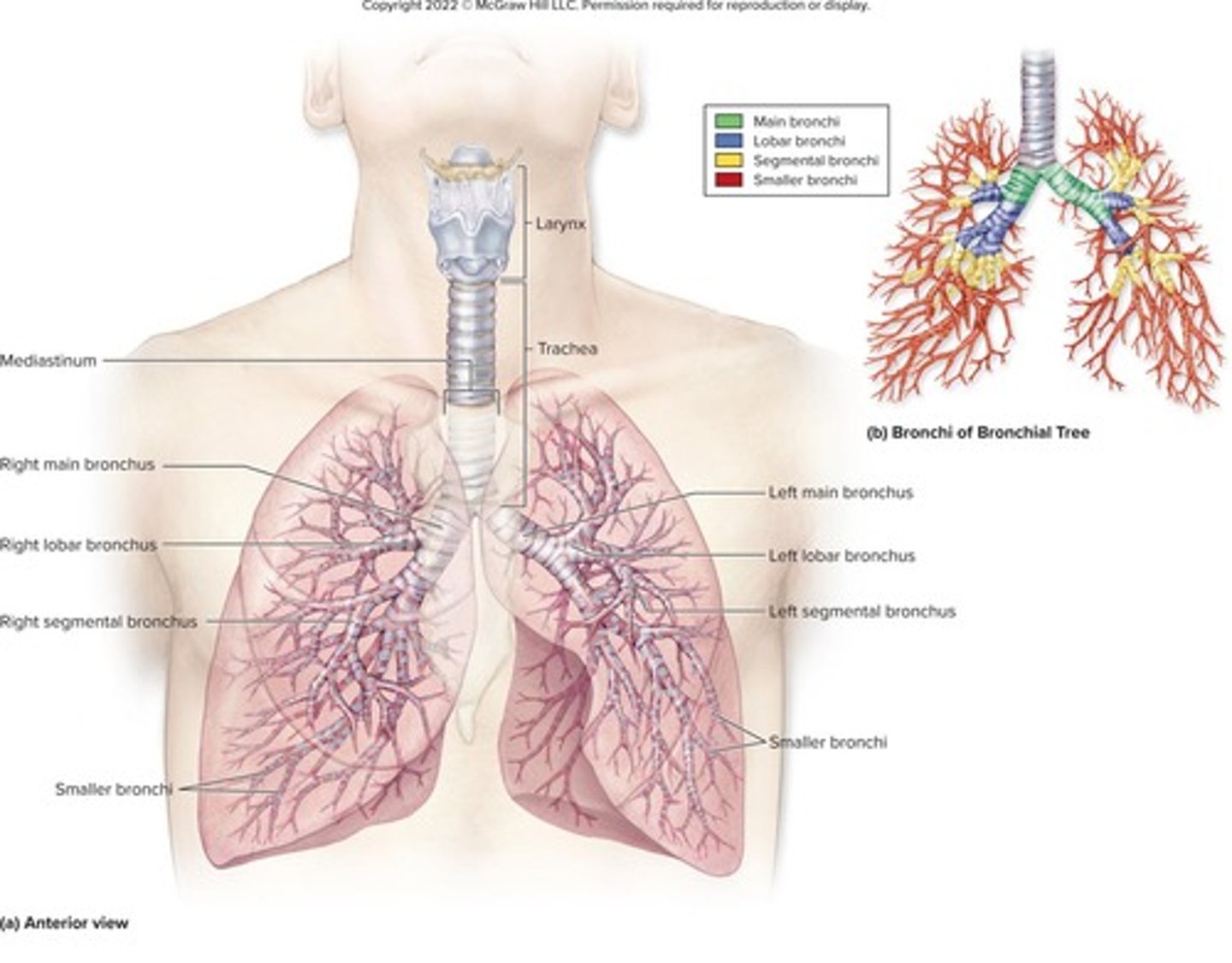
What happens to the structure of bronchi as they branch?
Cartilage rings become irregular plates, and the epithelium changes from pseudostratified columnar to cuboidal.
What are bronchioles?
Small air passages less than 1 mm in diameter that lead to respiratory bronchioles.
What is the last part of the conducting zone?
Terminal bronchioles.
What is the first part of the respiratory zone?
Respiratory bronchioles.
What is the starting point of the respiratory zone?
The respiratory zone begins at the end of the terminal bronchioles.
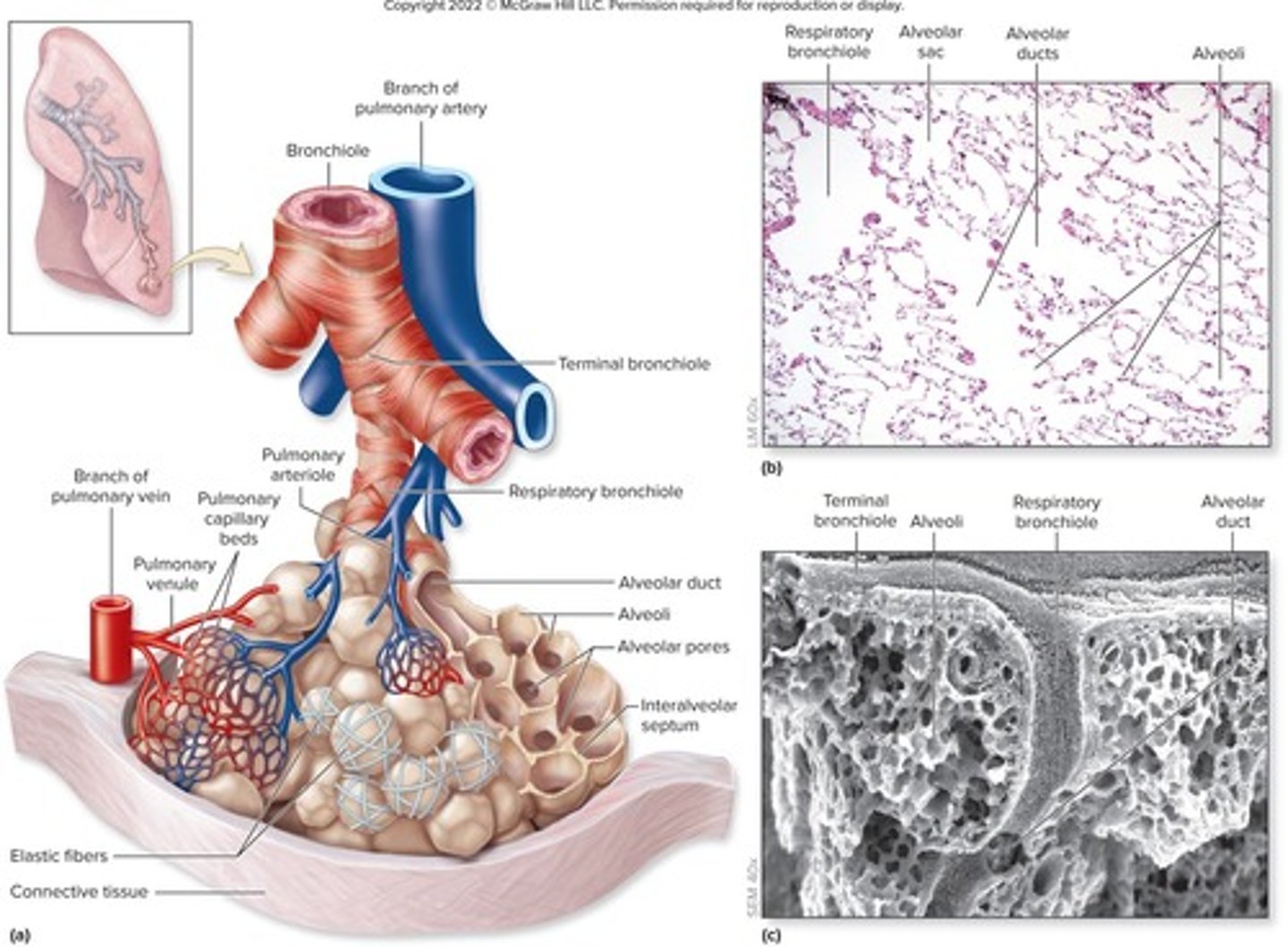
What structures make up the respiratory zone?
Respiratory bronchioles, alveolar ducts, and alveolar sacs.
How many alveoli are approximately in the lungs?
~300 million alveoli.
What is the function of alveoli?
Sites of gas exchange.
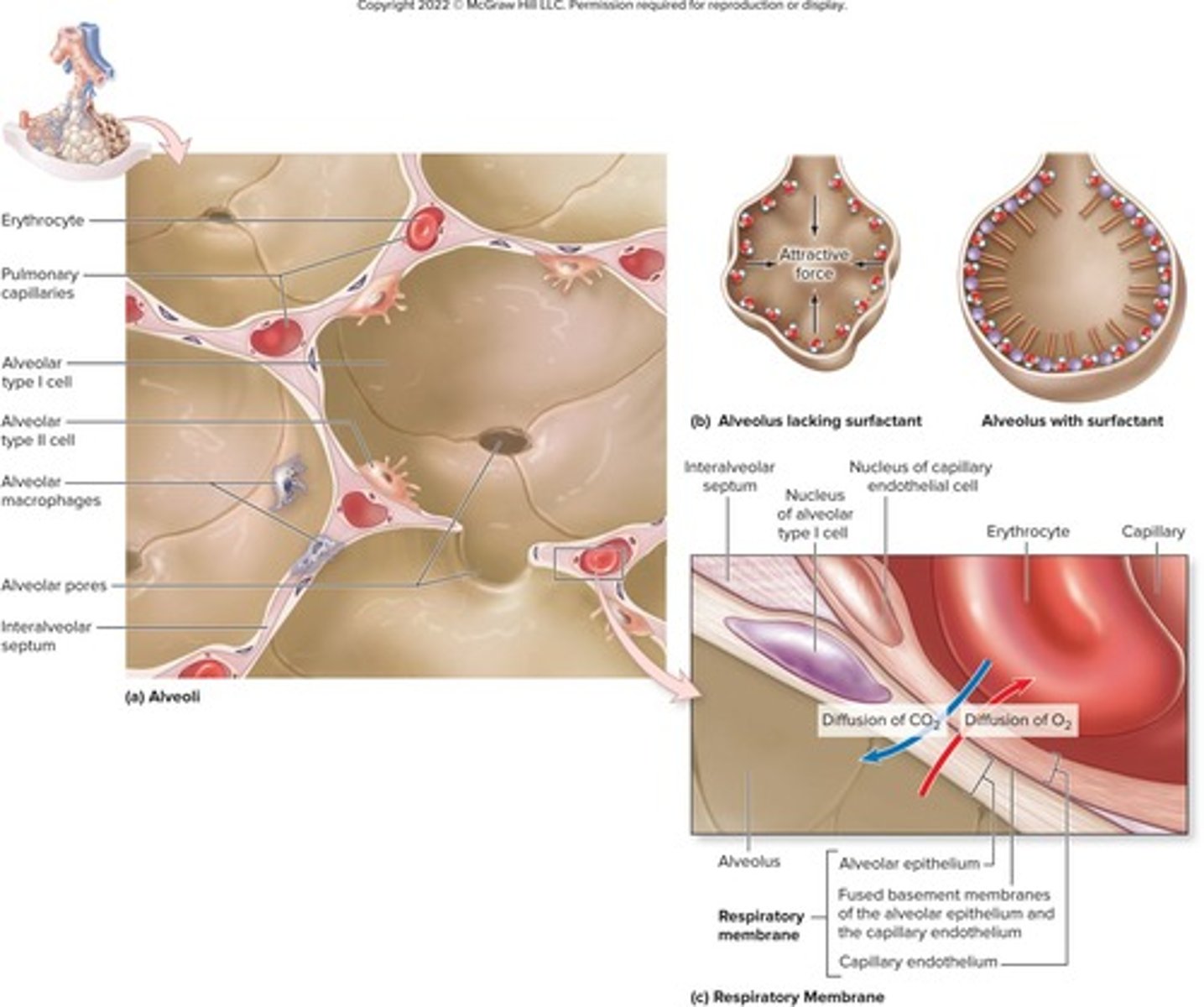
What is the respiratory membrane composed of?
Alveolar and capillary walls and their fused basement membranes.
What type of cells are found in the alveolar walls?
Type I alveolar cells (squamous epithelium) and type II alveolar cells (cuboidal cells).
What is the role of type II alveolar cells?
They secrete surfactant and antimicrobial proteins.
What is the thickness of the respiratory membrane?
~0.5 µm thick.
How does oxygen move during gas exchange in the lungs?
Oxygen diffuses from the alveolus into the capillaries.
What happens to carbon dioxide during gas exchange?
Carbon dioxide diffuses from blood to the alveolus.
What connects adjacent alveoli?
Alveolar pores.
What is the purpose of alveolar macrophages?
To keep alveolar surfaces sterile.
What is the hilum of the lungs?
The indented region on the lung's mediastinal side where vascular and bronchial attachments occur.
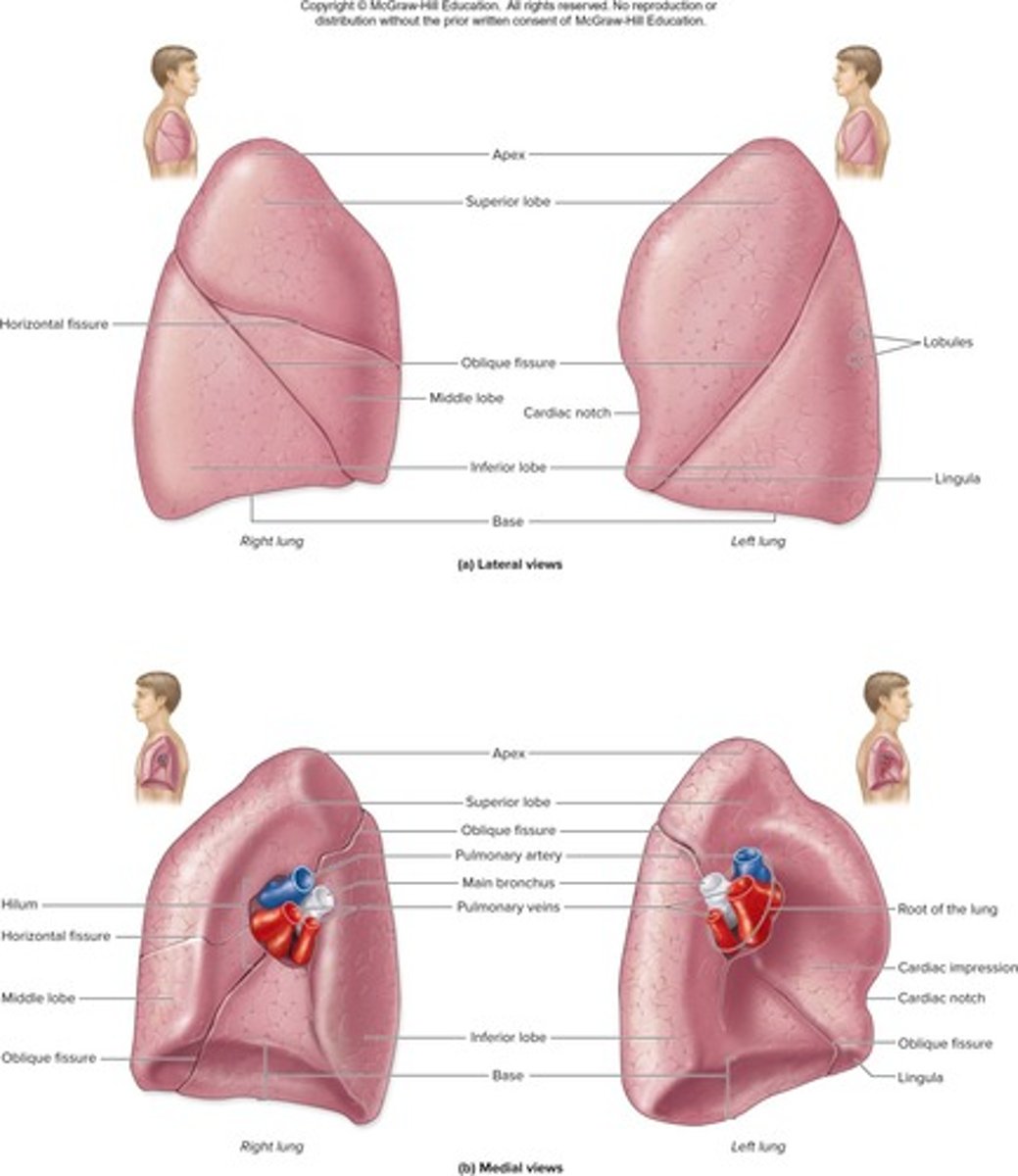
What is the apex of the lung?
The superior tip of the lung, deep to the clavicle.
How many lobes does the left lung have?
Two lobes.
What is the cardiac notch?
A concavity in the left lung for the heart.
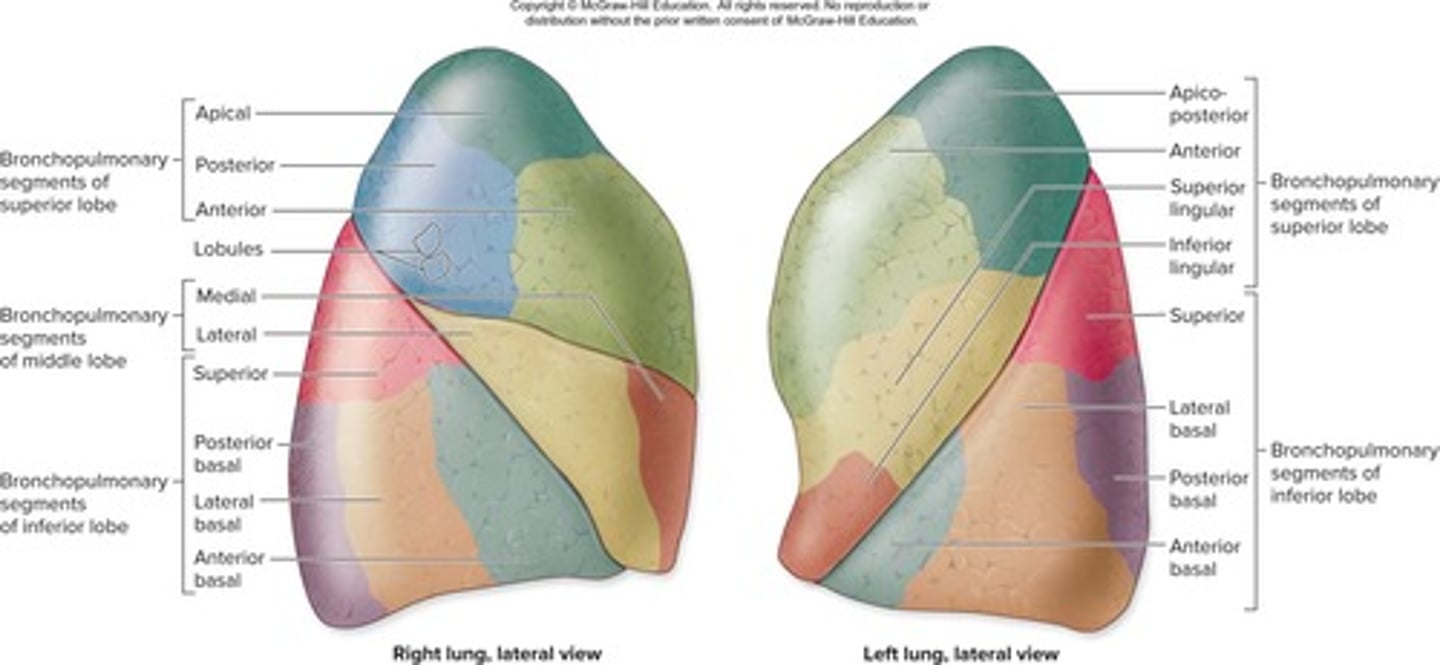
How many bronchopulmonary segments are in the right lung?
10 segments.
What is the function of bronchial arteries?
To provide oxygenated blood to lung tissue.
What is the difference between pulmonary circulation and bronchial circulation?
Pulmonary circulation is low pressure, high volume for oxygenation; bronchial circulation is high pressure, low volume for lung tissue.
What is pleura?
A thin, double-layered serosa that divides the thoracic cavity into pleural compartments.
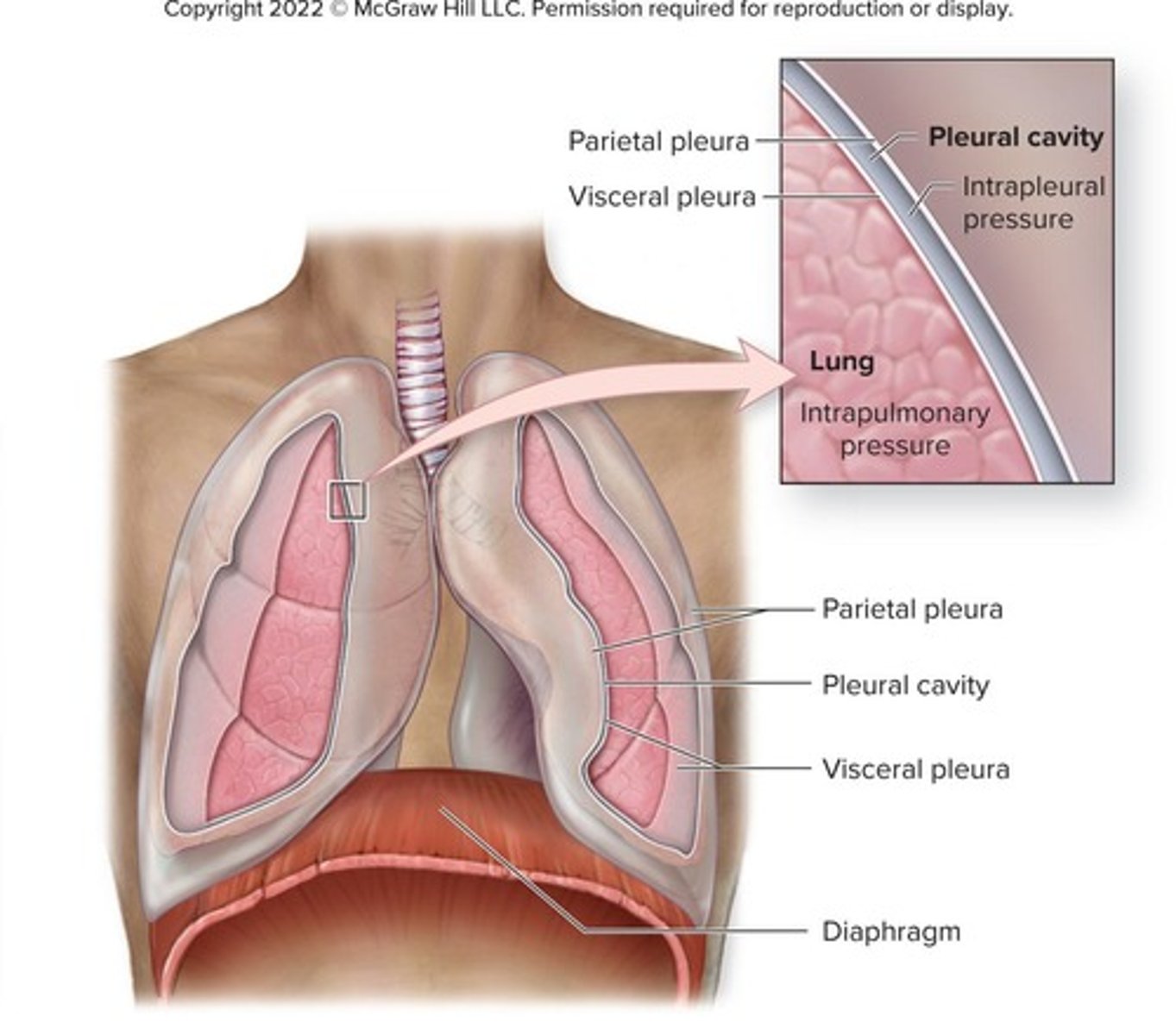
What fills the pleural cavity?
Pleural fluid, which provides lubrication and assists in lung expansion and recoil.
What are the two phases of pulmonary ventilation?
Inspiration and expiration.
What is intrapulmonary pressure?
The pressure in the alveoli that fluctuates with breathing.
What is intrapleural pressure?
The pressure in the pleural cavity that is always negative.
What happens if intrapleural pressure equals intrapulmonary pressure?
The lungs collapse.
What is Boyle's Law?
The relationship between pressure and volume of a gas, stating that pressure varies inversely with volume.
What muscles are involved in inspiration?
The diaphragm and external intercostal muscles.
What happens during quiet expiration?
It is a passive process where inspiratory muscles relax and thoracic cavity volume decreases.
What three factors hinder air passage and pulmonary ventilation?
Airway resistance, alveolar surface tension, and lung compliance.
What is the relationship between flow, pressure, and resistance in the airways?
Flow changes inversely with resistance and is directly related to the pressure gradient.
What is the primary function of the conducting zone in the respiratory system?
To progressively branch airways, increasing total cross-sectional area for airflow.
Where is the greatest resistance found in the airways?
In medium-sized bronchi.
What drives gas movement at the terminal bronchioles?
Diffusion.
What is surface tension in the context of alveoli?
It attracts liquid molecules to one another at the gas-liquid interface, resisting forces that increase surface area.
What is surfactant and its role in the alveoli?
A detergent-like lipid and protein complex produced by type II alveolar cells that reduces surface tension and prevents alveolar collapse.
What condition can arise from insufficient surfactant in premature infants?
Infant respiratory distress syndrome.
What is lung compliance?
The ease with which lungs and chest wall expand, measured by the change in lung volume with a given change in transpulmonary pressure.
What factors can diminish lung compliance?
Nonelastic scar tissue (fibrosis), reduced surfactant production, and decreased thoracic cage flexibility.
What are the four primary respiratory volumes used to assess respiratory status?
Tidal volume (TV), inspiratory reserve volume (IRV), expiratory reserve volume (ERV), and residual volume (RV).
What is the definition of anatomical dead space?
Air remaining in passageways that does not contribute to gas exchange, approximately 150 ml.
What is minute ventilation?
The total amount of gas flow into or out of the respiratory tract in one minute.
What is the normal minute ventilation at rest?
~6 L/min.
What is the alveolar ventilation rate (AVR)?
The flow of gases into and out of alveoli during a specific time.
What is external respiration?
The diffusion of gases in the lungs.
What is internal respiration?
The diffusion of gases at body tissues.
What does Dalton's Law of Partial Pressures state?
Total pressure exerted by a mixture of gases equals the sum of pressures exerted by each gas.
What is Henry's Law in relation to gas exchange?
Each gas dissolves in proportion to its partial pressure when in contact with a liquid.
What is the composition of alveolar gas compared to atmospheric air?
Alveoli contain more CO2 and water vapor than atmospheric air due to gas exchanges and humidification.
What influences the exchange of O2 and CO2 across the respiratory membrane?
Thickness and surface area of the membrane, partial pressure gradients, and gas solubilities.
What is the normal thickness of respiratory membranes?
0.5 to 1 µm thick.
What happens to gas exchange if the lungs become waterlogged?
Gas exchange becomes inadequate due to increased membrane thickness.
How does the partial pressure gradient for O2 in the lungs affect oxygen flow?
A steep gradient drives oxygen flow from alveoli to blood.
What is the role of perfusion in ventilation-perfusion coupling?
It refers to blood flow reaching alveoli, which must be matched with ventilation for efficient gas exchange.
What is the significance of changes in Po2 in alveoli?
They cause changes in the diameters of arterioles to direct blood flow where oxygen levels are high.
What is the primary transport method of oxygen in the blood?
1.5% dissolved in plasma and 98.5% bound to hemoglobin (Hb) in red blood cells.
What is oxyhemoglobin?
The combination of hemoglobin and oxygen.
What factors influence the loading and unloading of O2 from hemoglobin?
Partial pressure of O2, temperature, blood pH, PCO2, and concentration of BPG.
What is the oxygen-hemoglobin dissociation curve?
A graph that shows the relationship between hemoglobin saturation and partial pressure of oxygen, typically S-shaped.
What factors influence hemoglobin saturation with oxygen?
Increases in temperature, H+, PCO2, and BPG decrease hemoglobin's affinity for O2.
What effect does a decrease in temperature, H+, PCO2, and BPG have on hemoglobin saturation?
It increases hemoglobin's affinity for O2, shifting the O2-hemoglobin dissociation curve to the left.
What is the Bohr effect?
The weakening of the Hb-O2 bond due to increased PCO2 and H+, enhancing O2 unloading where needed most.
How is CO2 transported in the blood?
CO2 is transported in three forms: 7-10% dissolved in plasma, 20% bound to hemoglobin, and 70% as bicarbonate ions.
What happens to CO2 in systemic capillaries?
HCO3- diffuses from RBCs into plasma, and Cl- moves into RBCs to balance the charge (chloride shift).
What occurs in pulmonary capillaries regarding CO2 transport?
HCO3- moves into RBCs, binds with H+ to form carbonic acid, which splits into CO2 and water; CO2 then diffuses into alveoli.
What is the Haldane effect?
Reduced hemoglobin forms carbaminohemoglobin more easily, allowing more CO2 to be carried in blood when PO2 is low.
How does the carbonic acid-bicarbonate buffer system regulate blood pH?
It resists changes in pH by combining excess H+ with HCO3- to form H2CO3, and releasing H+ when pH drops.
What effect does slow, shallow breathing have on blood pH?
It increases CO2 in blood, leading to a drop in pH (acidosis).
What role do central and peripheral chemoreceptors play in respiration?
They sense changes in CO2, O2, and H+ levels, modifying the rate and depth of breathing accordingly.
What is hypercapnia?
An increase in blood CO2 levels that stimulates increased depth and rate of breathing.
What triggers peripheral chemoreceptors to increase ventilation?
A significant drop in arterial PO2, typically below 60 mm Hg.
How does arterial pH influence respiratory rate?
Decreased pH can stimulate increased respiratory rate, mediated by peripheral chemoreceptors.
What is the primary respiratory stimulant?
Rising CO2 levels.
How do higher brain centers influence respiration?
They modify the rate and depth of respiration through the limbic system and direct signals from the cerebral cortex.
What is the role of the ventral respiratory group (VRG)?
It is a rhythm-generating and integrative center that sets the normal respiratory rate (eupnea).
What is the function of the dorsal respiratory group (DRG)?
It integrates input from peripheral stretch and chemoreceptors and sends information to the VRG.
What is the significance of the pontine respiratory centers?
They smooth out transitions between inspiration and expiration and fine-tune breathing rhythms.