6. Chemical carcinogenesis
1/16
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
17 Terms
What is cancer?
Uncontrolled growth of cells (cell division beyond the normal limits)
Invasion (intrusion on and destruction of adjacent tissues)
Metastasis (spread to other locations in body via lymph or blood)
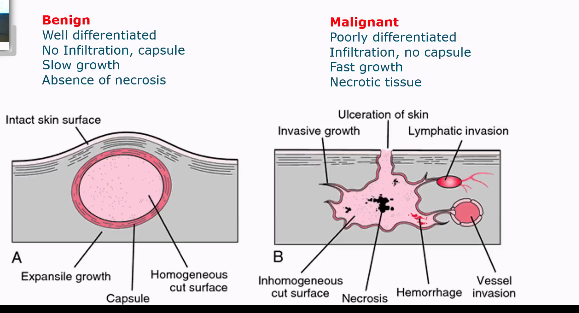
Benign vs malignant tumors
Benign
Well differentiated cells
No infiltration, capsule
Slow growth
Absence of necrosis
Malignant
Poorly differentiated cells
Infiltration, no capsule
Fast growth
Necrotic tissue
Cancer risk factors
Tobacco
Diet
Alcohol
Infection
Geophysical factors
Why is cancer a multi-step process?
Initial mutation inactivates a negative cell cycle regulator
Next mutation over-activates a positive cell cycle regulator
Third mutation inactivates a genome stability factor
Additional mutations accumulate rapidly
Cancer cells are formed
This shows that not one mutation causes cancer, accumulation of damage to a number of genes across time leads to cancer
Additionally depending on how relevant the segment of DNA is that is mutated, will also affect the chances of cancer being formed.
Which cell cycle regulators promote development of cancer when mutated?
Overactivation of positive regulators (oncogenic)
Inactivation of negative regulators
Overactivation of positive regulators
Proto-oncogenes: genes with a normal function in regulating cell division
Different effects of mutations:
“always on” protein
amplification (more protein)
“combo” unregulated
Oncogenes: transformed genes causing uncontrolled cell division
Proto-oncogenes → oncogenes
Overactivation of negative regulators
Inhibition of tumor suppressors
Tumor suppressor: a gene that normally blocks cell cycle progression (in response to DNA damage)
Active tumor suppressor gene → inactive tumor suppressor genes
Inactivation occurs through mutation
Inactive tumor suppressor genes causes no control of cell division of cells
Genotoxic vs non-genotoxic carcinogens
Genotoxic: every molecule increases cancer risk
Non-genotoxic: a threshold/safe level of exposure can be defined
PAHs
Chemical carcinogenesis
Genotoxic carcinogens
Aflatoxin B1
Chemical carcinogenesis
Pro-carcinogen is activated when it gains an epoxide group.
This makes the ultimate carcinogen very reactive and it attaches itself to the DNA
Happens on P53 gene which is a gene coding for a DNA repair.
Causes liver cancer
P53 tumor protein
Normal p53:
p53 activated binds DNA
This stops cell division, activates DNA repair enzymes and triggers apoptosis if repair is impossible.
As a result cells do not pass on damaged DNA
non-functional p53:
p53 cannot bind DNA
hence the effects mentioned above do not occur
As a result damaged DNA is passed on
Non-genotoxic chemicals
no direct binding of chemical to DNA
no direct damage
no interaction of chemical or metabolite with DNA
yet, some chemicals can cause cancer
how can non-genotoxic chemicals cause cancer?
Chemicals that:
Cause cell death and aberrant repair
Affect metabolism of chemicals
Affect cell growth
induce DNA synthesis → gene expression
Affect hormonal system
Induce production of reactive oxygen species
Dioxins
non-genotoxic chemicals
can be found in milk or eggs
activate aryl hydrocarbon receptor
results in uncontrolled cell division
Asbestos fibers
Non-genotoxic
Activates macrophages, however they cannot do this and therefore keep releasing cytokines which causes inflammation
Causes malignant mesothelioma
Classes of carcinogenicity
Group 1: carcinogenic to man; should be forbidden
Group 2A: probably carcinogenic to man; should be forbidden
Group 2B: possibly carcinogenic
Group 3: Compound cannot be classified because of lack of sufficient data
Group 4: proven to be non-carcinogenic
How is carcinogenicity data collected for risk assesment?
Epidemiology studies in humans
Preferred but absent in most ases
Can define group 1 carcinogens
Avoidable chemicals: when positive in genotoxicity studies, no testing
Non avoidable chemicals: carcinogenicity studies still needed