1/2- Spinal Cord Anatomy + Ascending Sensory Pathways
1/91
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
92 Terms
what are the 3 layers of meninges
outer → innermost D A P
dura mater
arachnoid
pia mater
T/F: the 3 meninges only surround CNS, not PNS
true
blood vessels + CSF are found between which 2 meninges
in subarachnoid space: between arachnoid + pia
how many pairs of spinal nerves
31
5 groups of spinal nerves
C T L S C
cervical
thoracic
lumbar
sacral
coccygeal
how many cervical spinal nerves
8
how many thoracic spinal nerves
12
how many lumbar spinal nerves
5
how many sacral spinal nerves
5
how many coccygeal spinal nerves
1-3
term for back of human body
dorsal
term for front of human body
ventral
term for towards the brain
rostral
term for towards the feet
caudal
spinal cord is increased in diameter in which 2 areas
cervical enlargement: C5-T1
lumbar (lumbosacral) enlargement: L3-S2
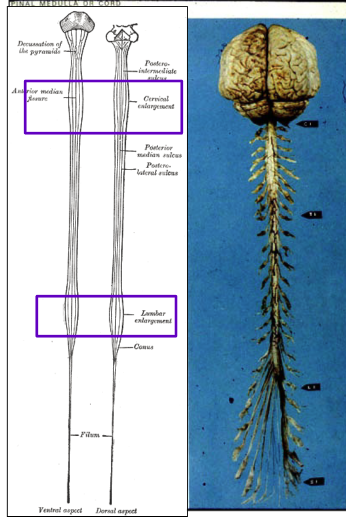
why does the spinal cord increase in diameter in those areas
to accommodate the neurons required for upper + lower extremities
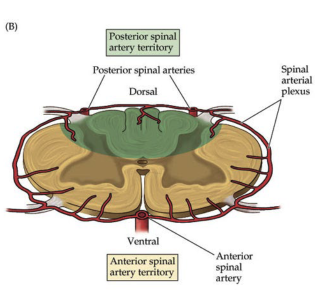
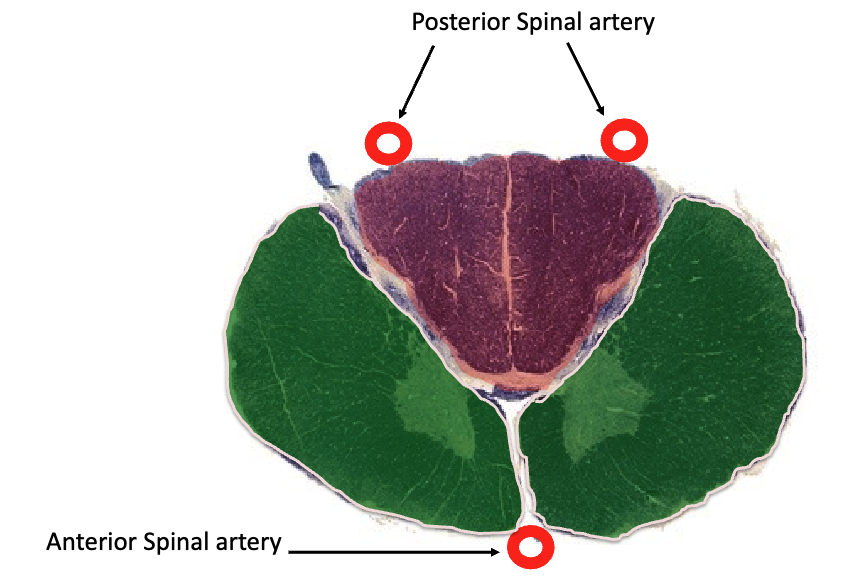
how do you differentiate between the anterior (ventral) surface vs. posterior (dorsal) surface of the spinal cord
ventral: 1 single spinal artery (supplies anterior 2/3 of cord)
dorsal: pair of spinal arteries
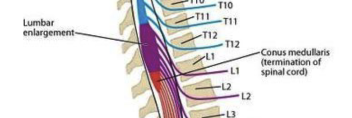
what’s the conus medullaris
termination of the spinal cord
where is the conus medullaris
between vertebrae L1/L2
what’s the cauda equina
where spinal nerves extend inferiorly from conus medullaris
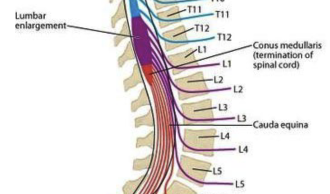
since the difference of growth between spinal cord + spinal column, length of nerve roots become
progressively longer from cervical to sacral levels
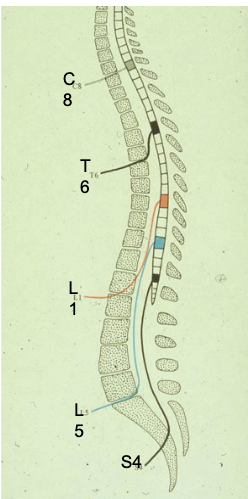
where are spinal taps performed
below L2, b/c spinal cord ends between L1/L2
spinal has _____ and _____ oragnization
segmental + longitudinal
definition of spinal cord segment
part of cord that gives rise to a pair of spinal nerves
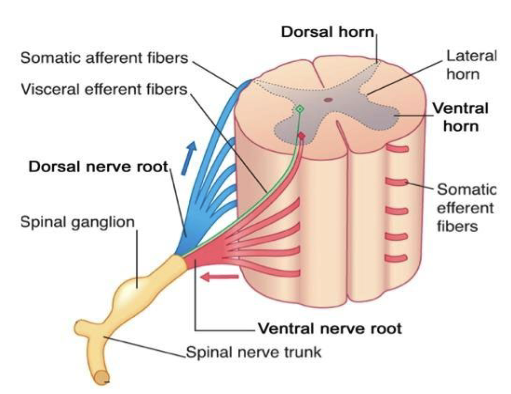
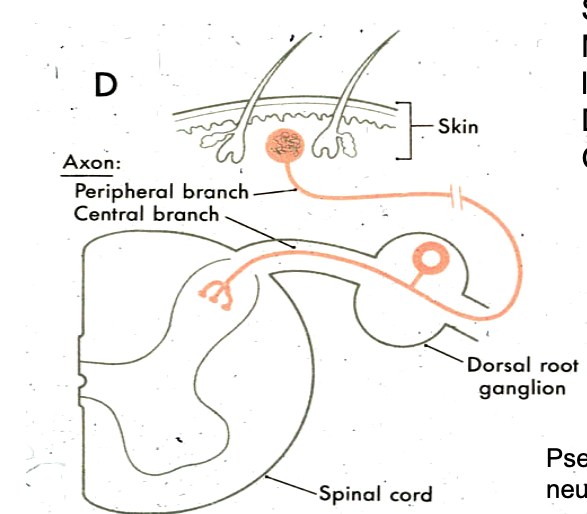
primary sensory neurons are what type of neurons (how many processes)
pseudounipolar
primary sensory neurons are located where
dorsal root ganglion
motor neurons are located where
ventral horn of spinal cord
what does DAVE stand for
Dorsal Afferent - Ventral Efferent
where are unipolar sensory neurons located
cell bodies in dorsal root ganglion
roots of unipolar sensory neurons project where
into dorsal horn of gray matter or white matter of dorsal funiculus
where are multipolar motor neurons located
cell bodies in ventral horn of gray matter
what’s a myotome
a single nerve root innervating a muscle
spinal reflexes reveal what
segmental organization of spinal cord
gray matter is divided into what 2 regions
dorsal horn
ventral horn
white matter is divided into what 4 regions
4 funiculi:
dorsal
ventral
2 lateral
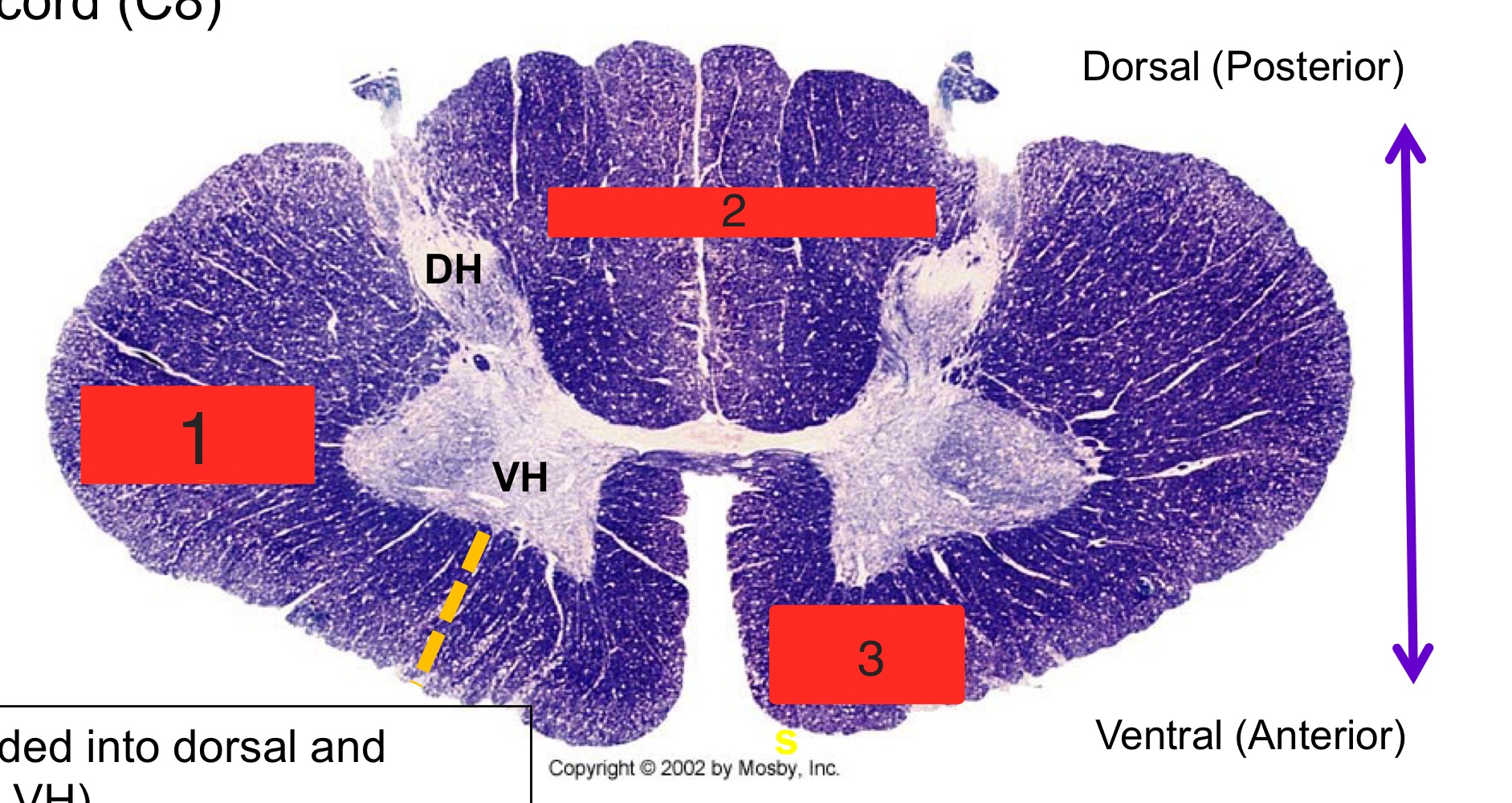
what are the numbers
lateral funiculus
dorsal funiculus
ventral funiculus
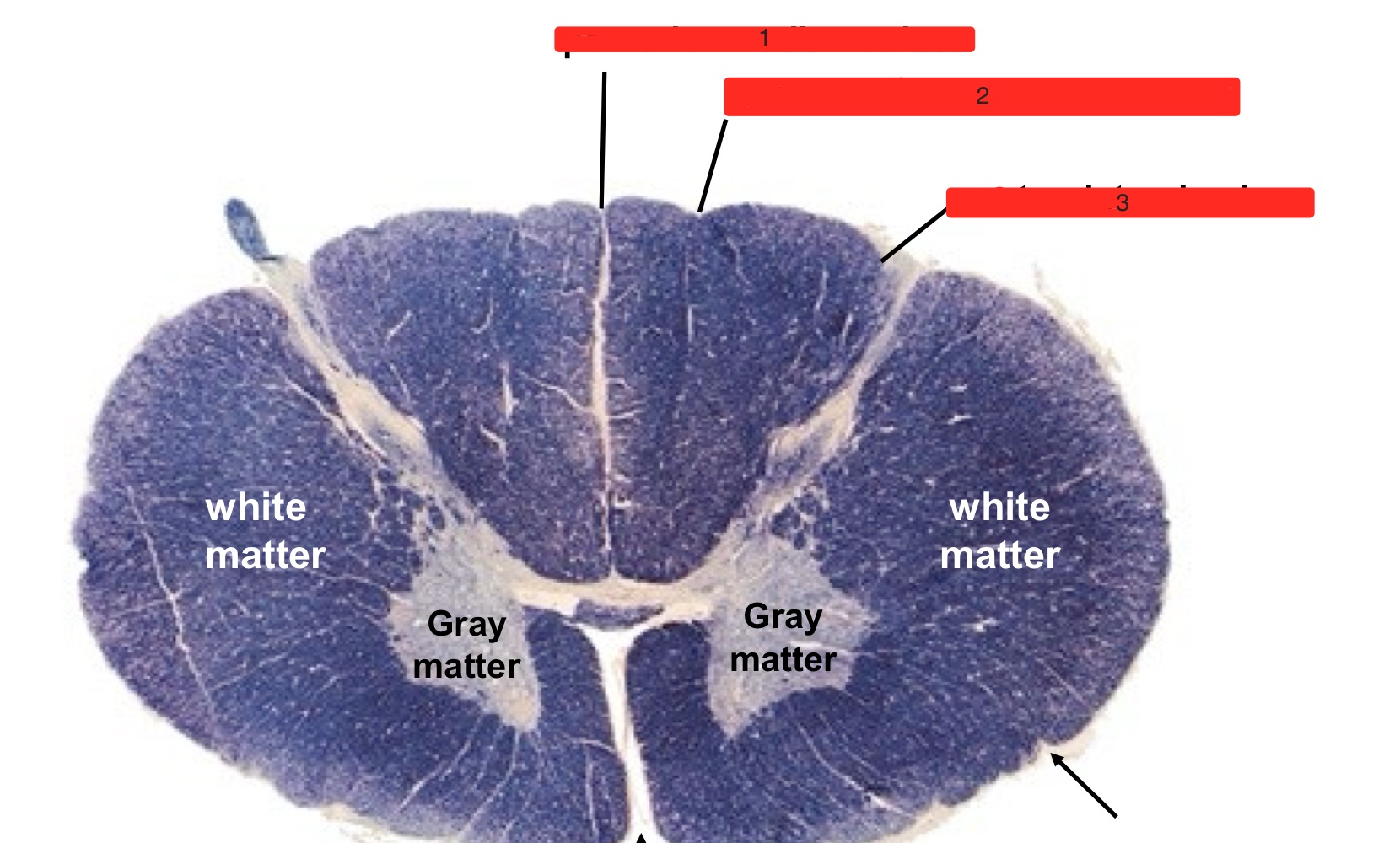
what are the numbers
posterior median sulcus
posterior intermediate sulcus
posterolateral sulcus
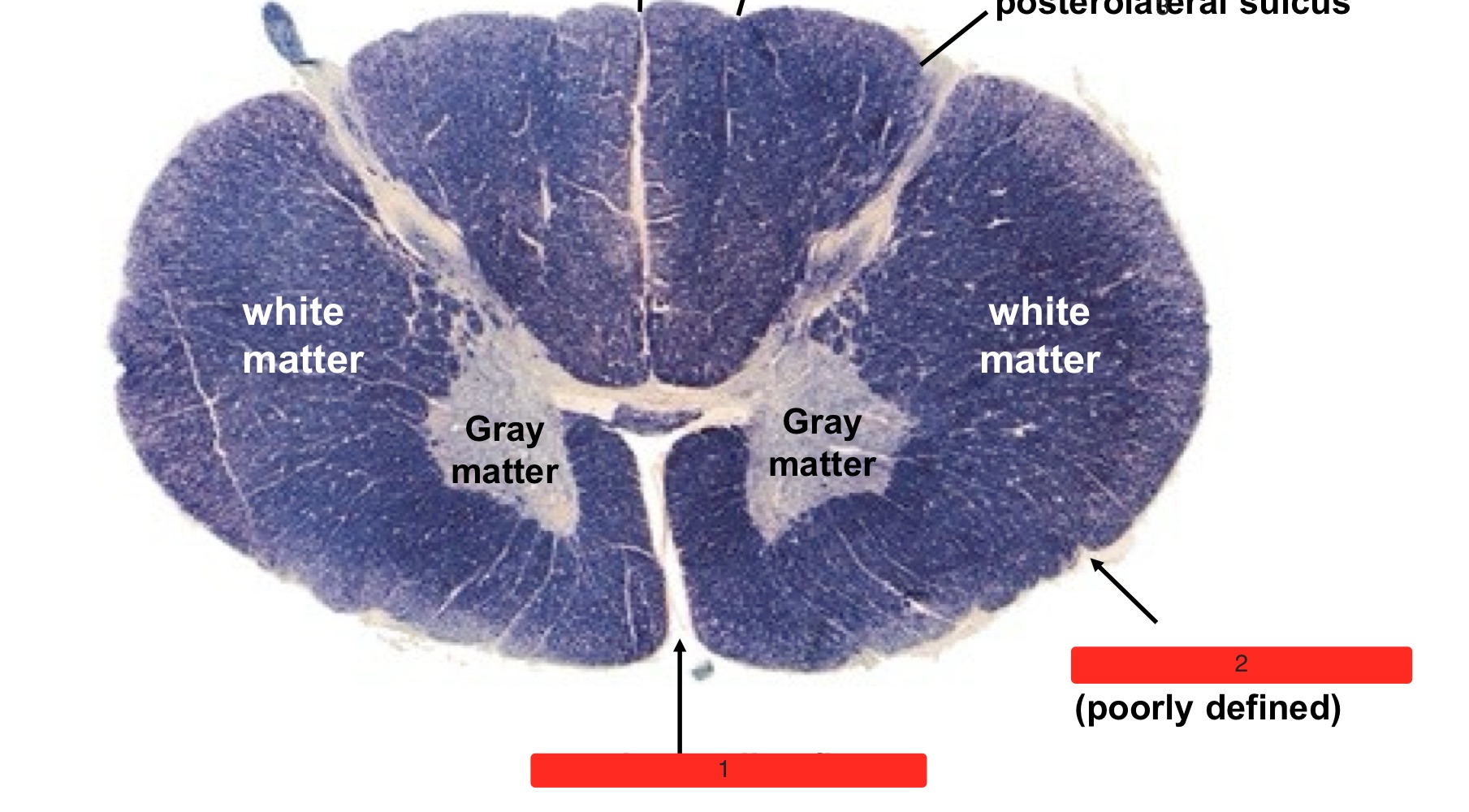
what are the numbers
anterior median fissure
anterolateral sulcus
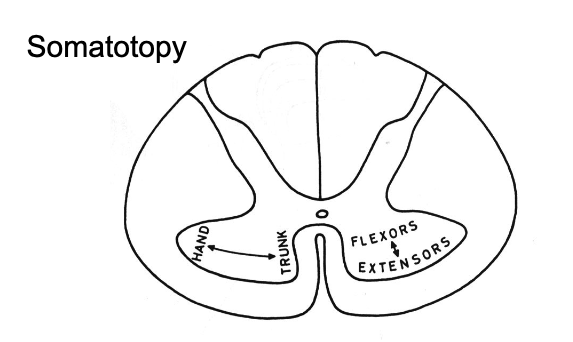
describe location of motor neuron bodies within gray matter
distal-lateral muscles are lateral in ventral horn
flexor muscles are more dorsal vs. extensor muscles are ventral
why does is there more gray matter in cervical sections than thoracic
cervical section contains brachial plexus (arm muscles) vs. thoracic contains torso nerves, which has less muscles

preganglionic sympathetic neurons originate from which vertebrae
T1-L2
preganglionic parasympathetic neurons originate from which vertebrae
S2-S4
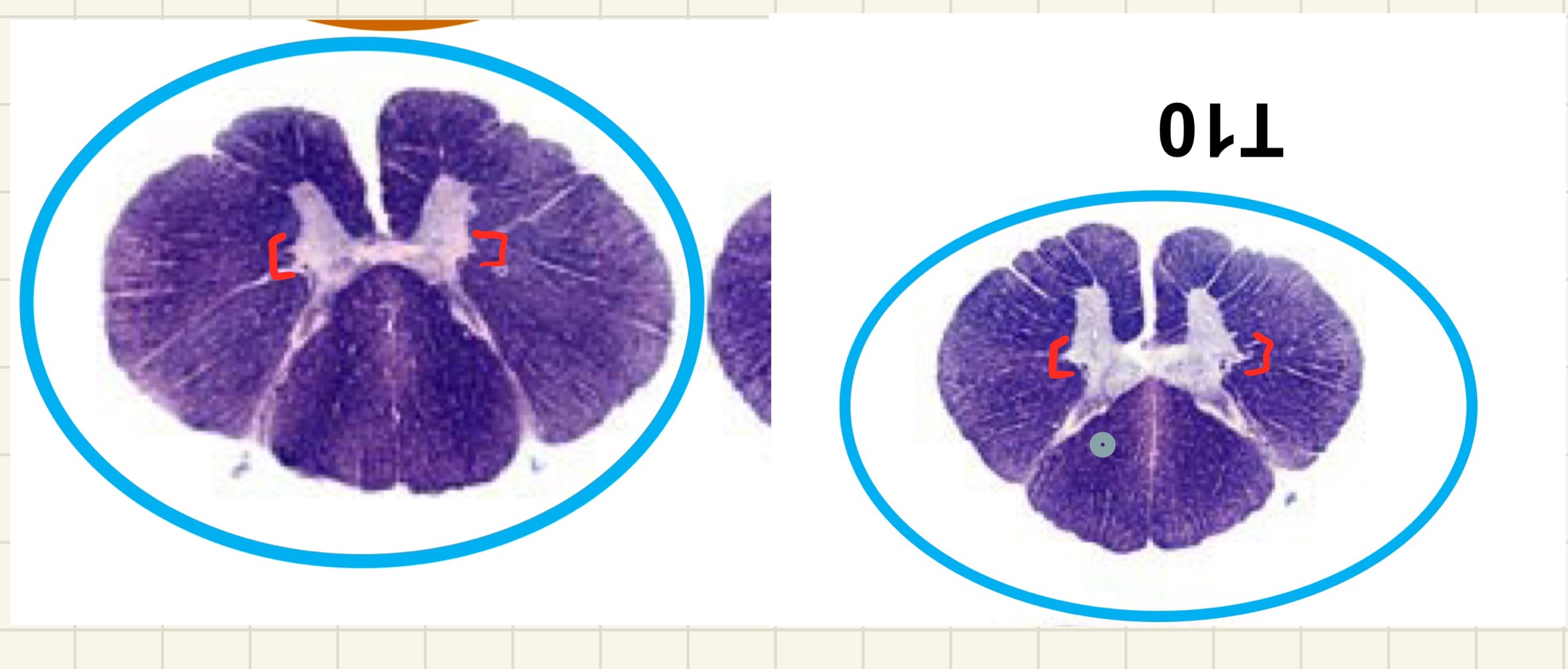
what can you find in the bracketed areas
preganglionic sympathetic neurons
motor neurons that innervate the diaphragm are found where
phrenic nucleus, C3-C5
5 functional groups of myelinated axons
long ascending fibers
long descending fibers
efferent (motor) fibers
afferent (sensory) fibers
propriospinal fibers
define long ascending fibers
sensory “bottom-up” projections from dorsal root ganglion (DRG) destined to reach the cortex, thalamus, brainstem
define long descending fibers
motor fibers “top-down” from the cortex, brainstem destined to reach motor neurons in ventral horn that project to peripheral muscles
define propriospinal fibers
3 tracts (dorsal, lateral, ventral) that ascend, descend, cross, and don’t cross that stay intrinsic to the spinal cord and interconnect different levels
4 mechanisms of spinal trauma
hyperextension: caused by extension injury
hyperflexion: caused by flexion injury
compression
rotation
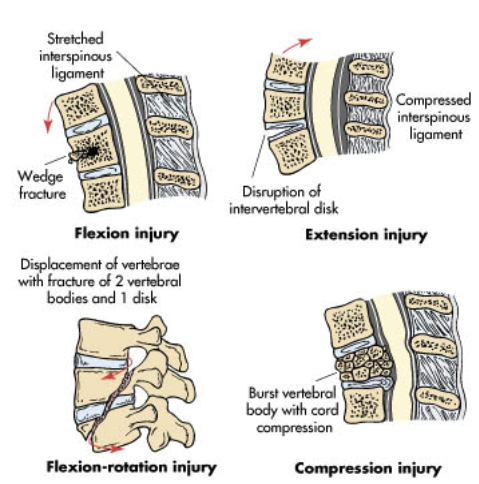
2 types of lesions
paresis: incomplete loss of muscle function
plegia/paralysis: complete loss of muscle function
3 types of plegia/paralysis
quadriplegia: C8 and above
paraplegia: below T1
hemiplegia: paralysis of ½ of body, usually brain injury
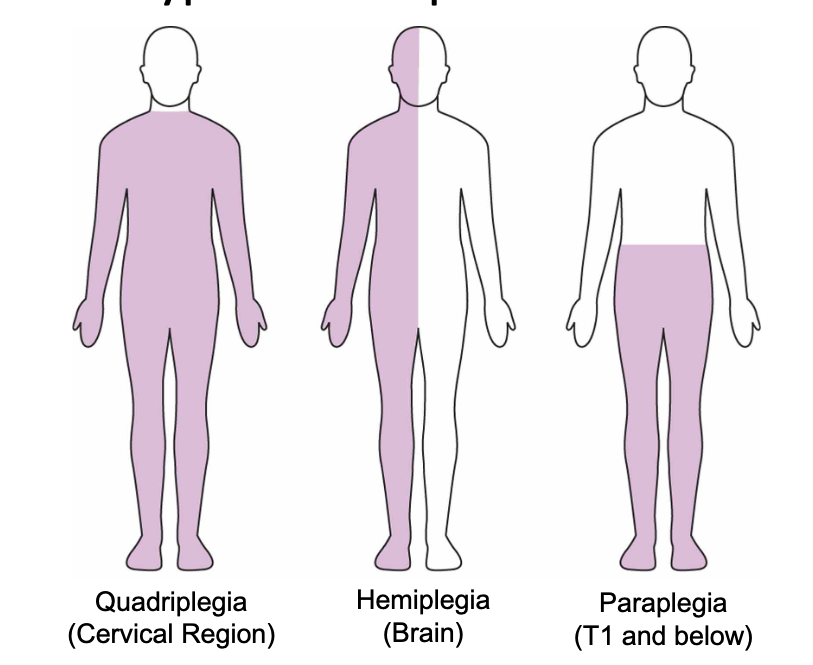
4 types of paresis
anterior cord syndrome
posterior cord syndrome
central cord syndrome
Brown-Sequard syndrome
2 important ascending pathways that are clinical testable + relays conscious sensory perception
dorsal column medial lemniscus pathway
spinothalamic pathways (anteriolateral system)
dorsal column medial lemniscus pathway relays what kind of info
position/vibration sense, discriminatory touch from the periphery to the cortex
spinothalamic pathways relay what kind of info
pain/temp + crude touch from the periphery to the cortex
important pathway that relays unconscious sensory perception
spinocerebellar pathways
2 divisions of dorsal column medial lemniscus pathway
fasciculus gracilis
fasciculus cuneatus
2 divisions of spinothalamic pathway
anterior spinothalamic tract
lateral spinothalamic tract
long tracts that bring info to/from cortex must
decussate (cross to the other side of the nervous system) during their ascent/descent
both clinically relevant ascending pathways are considered
3 neuron pathways:
1st order neuron: dorsal root ganglion (DRG)
2nd order neuron: its axons cross midline (spinal cord or brainstem)
3rd order neuron: thalamus-VPL
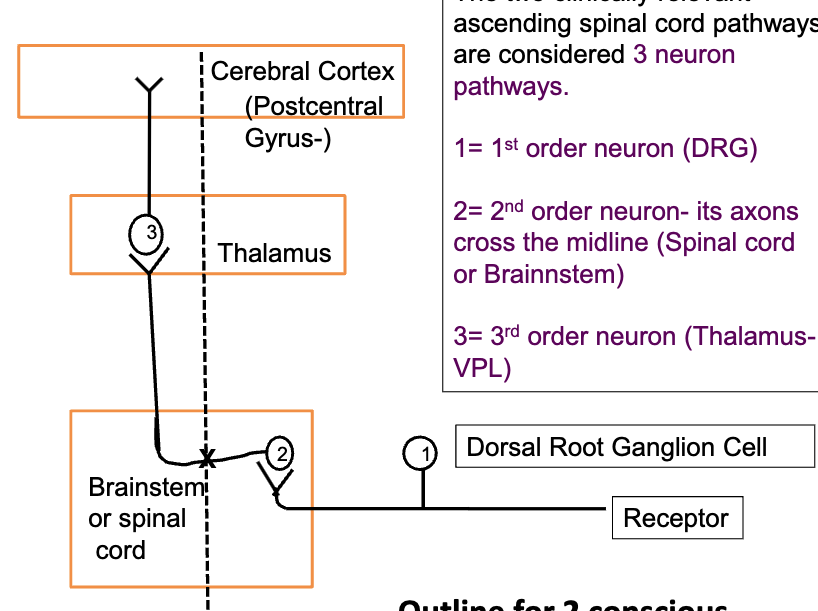
all info going to cortex must stop at thalamus except what
olfaction info, goes directly to cortex
what are the 3 modalities of the dorsal column medial lemniscus pathway
position sense
vibration sense
2-point discrimination
distinguish the origins of the 2 divisions of the dorsal column medial lemniscus pathway
fasciculus cuneatus: T5 + above
fasciculus gracilis: from T6 + below
distinguish the tracts of the 2 divisions of the dorsal column medial lemniscus pathway
fasciculus cuneatus: lateral portion of dorsal funiculus
fasciculus gracilis: medial portion of dorsal funiculus
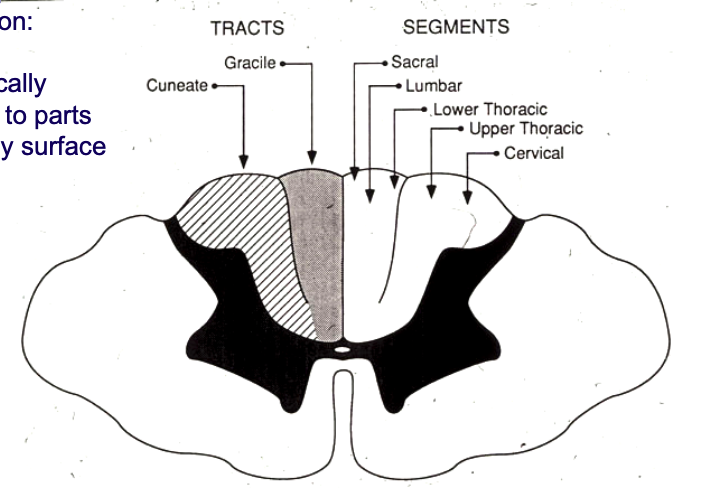
distinguish the nuclei of the 2 divisions of the dorsal column medial lemniscus pathway
within caudal medulla (lower part of brainstem)
fasciculus cuneatus: cuneate nucleus
fasciculus gracilis: gracile nucleus
T/F: pathways from both gracile + cuneate nucleus cross the midline before heading to the thalamus
true
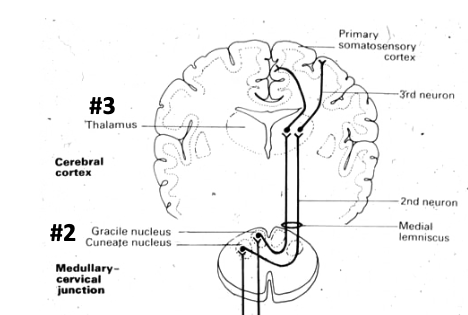
after crossing the midline, pathways from gracile + cuneate will form the
medial leminiscus
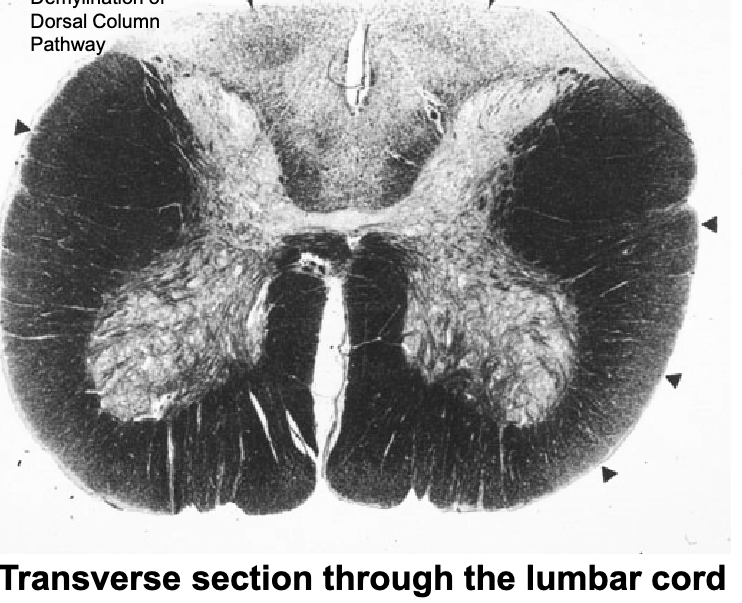
this patient has
demyelination of dorsal column pathway → loss of proprioception of lower extremities
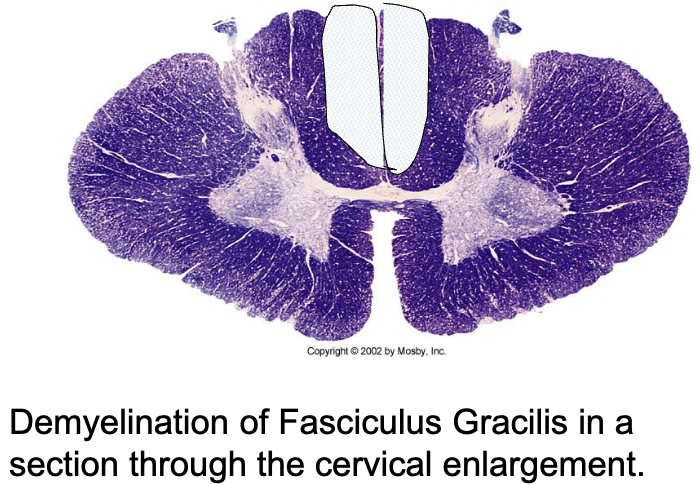
this patient has
loss of proprioception of their lower extremities
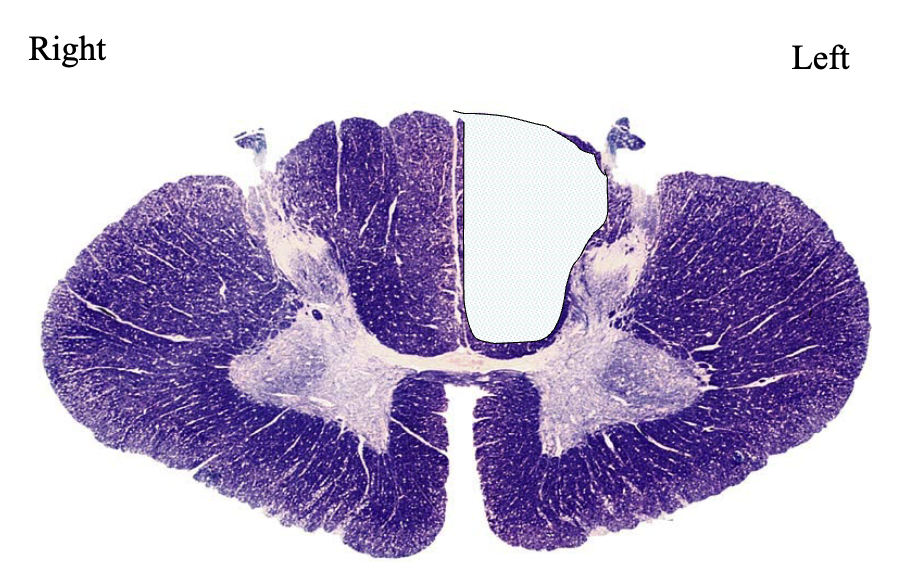
this patient has
loss of proprioception on left side
what are the 2 modalities of spinothalamic pathway
localization of pain + temp
crude touch
describe the 1st + 2nd order neurons of spinothalamic pathway
1st order: DRG
2nd order: in dorsal horn of gray matter in spinal cord
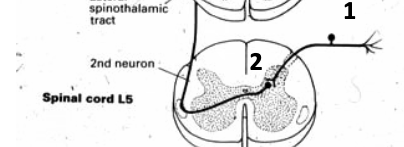
describe the pathway from 2nd → 3rd neuron of spinothalamic pathway
from 2nd, pathways crosses midline → ascends to thalamus
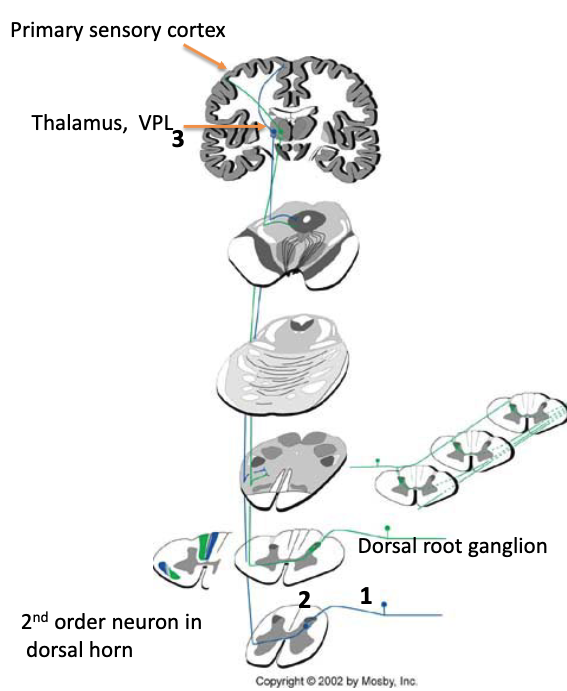
T/F: info passed through spinothalamic pathway ascends contralaterally to cortex
true
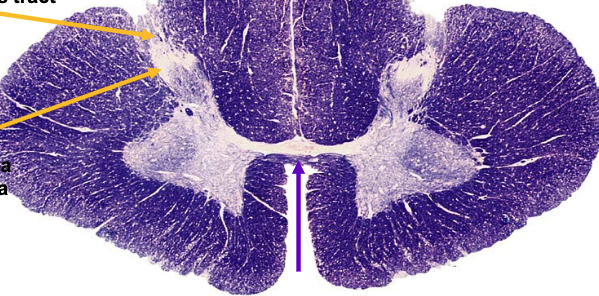
purple arrow is pointing to
ventral white commissure
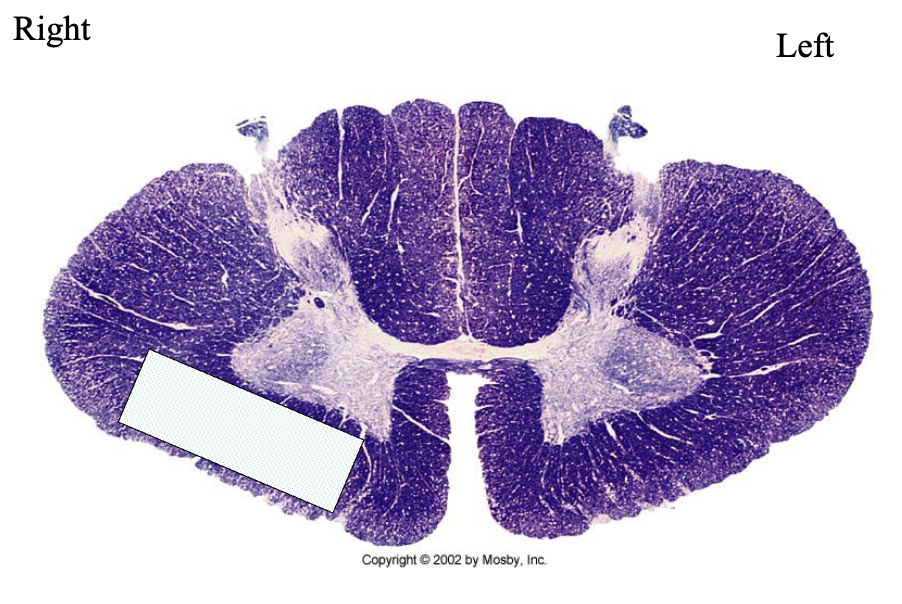
this patient has
loss of pain + temp perception on left side of body
main differences between dorsal column medial lemniscus pathway vs. spinothalamic pathway
dorsal column medial lemniscus: lesions → ipsilateral loss + has very myelinated axons
spinothalamic: lesions → contralateral loss + poorly/non-myelinated axons
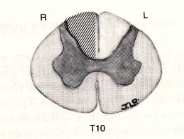
a lesion here would lead to
deficit in dorsal column medial lemniscus pathway
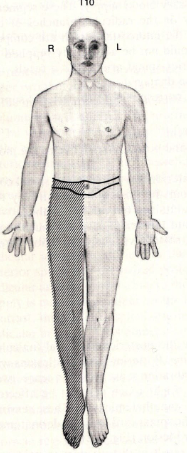
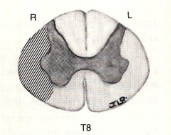
a lesion here would lead to
deficit in spinothalamic pathway
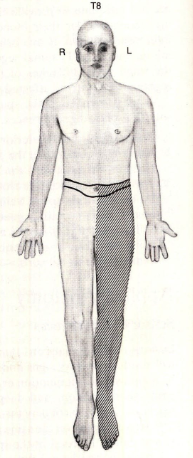
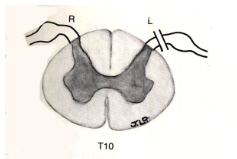
a lesion here would lead to
blocking dorsal root → suspended sensory loss at the level the lesion occurred since it does not involve the long tracts
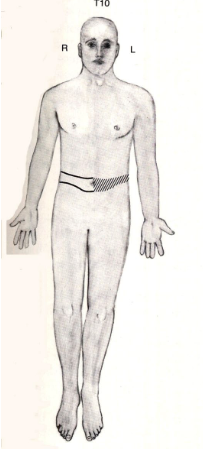
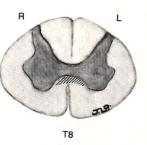
a lesion here would lead to
lesion in ventral white commissure → bilateral suspended sensory loss at the level the lesion occurred since it doesn’t involve the long tracts
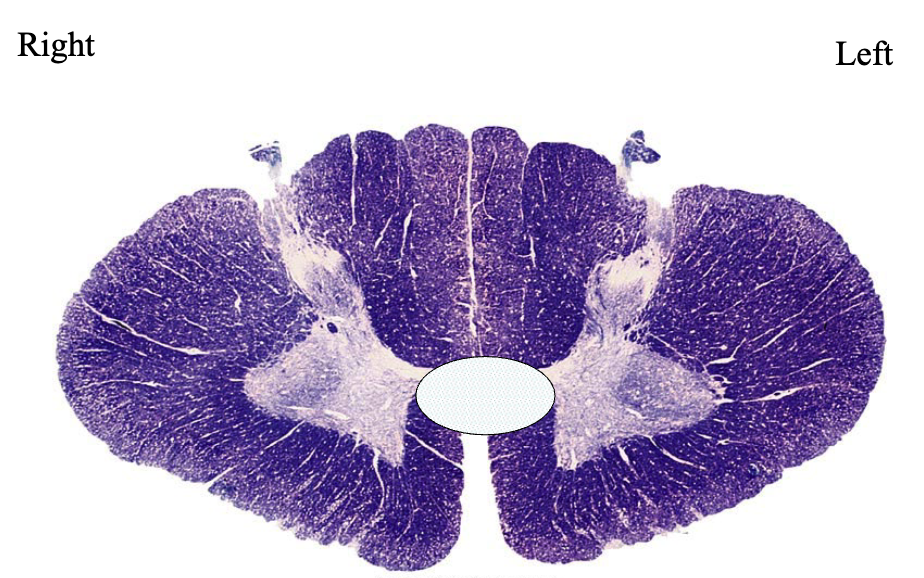
this patient has
lesion in ventral white commissure → bilateral loss of pain/temp only at level of lesion
3 pathways that go to the cerebellum
spinocerebellar pathways:
posterior (dorsal) spinocerebellar tract
anterior (ventral) spinocerebellar tract
cuneocerebellar tract
T/F: all 3 spinocerebellar pathways end ipsilaterally in cerebellum
true
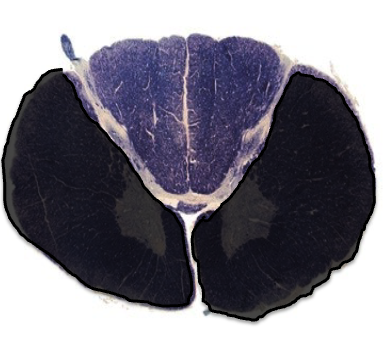
this lesion would cause which paresis syndrome
occlusion of anterior spinal artery → bilateral loss of spinothalamic pathway + motor neurons → anterior cord syndrome
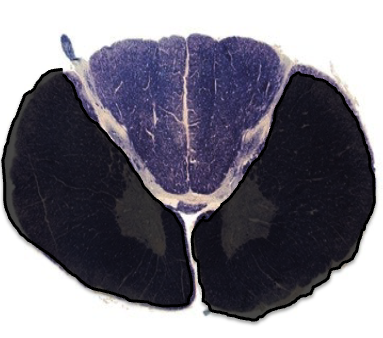
symptoms of this lesion
motor: bilateral paralysis/weakness
fine touch: normal
pain/temp: bilateral loss
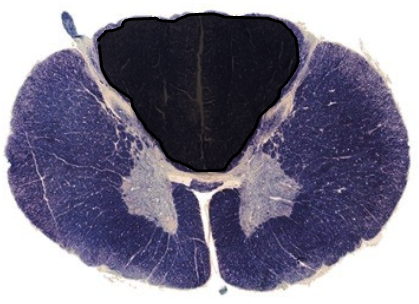
this lesion would cause which paresis syndrome
occlusion of posterior spinal artery → bilateral loss of dorsal column → posterior cord syndrome
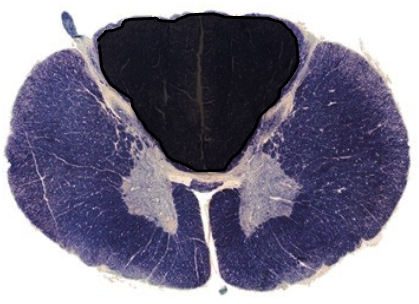
describe symptoms of this lesion
motor: normal
fine touch, vibration: bilateral loss
pain/temp: normal

this lesion would cause which paresis syndrome
damage to central area of spinal cord → bilateral loss of spinothalamic pathway → central cord syndrome

describe symptoms of this lesion
motor: progressive bilateral paralysis by direct damage on motor neurons
fine touch: normal
pain/temp: immediate bilateral loss
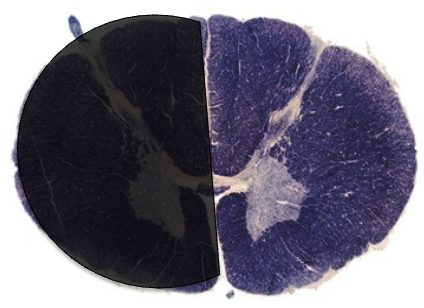
this lesion would cause which paresis syndrome
damage to ½ of spinal cord → ipsilateral loss of dorsal columnar + contralateral loss of spinothalamic → Brown-Sequard syndrome
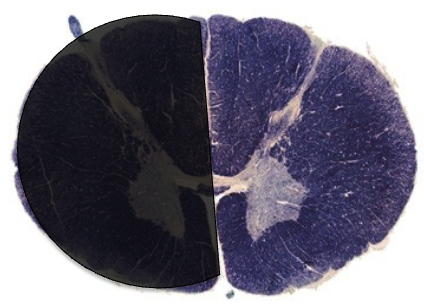
describe symptoms of this lesion
motor: ipsilesional paralysis (same side lesion)
fine touch: ipsilesional loss
pain/temp: contralesional loss