Hphys Dr. Gil Exam 4 QUIZLET. Renal System and Immune System
1/169
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
170 Terms
adaptive immunity
the ability to recognize and remember specific antigens and mount an attack on them
two components, humoral and cell-mediated immunity. Both components differ from innate immunity by the adaptive properties of recognition, specificity, and memory.
antibody
Y-shaped proteins produced by plasma B-cells. Their variable, or antigen-binding, regions are capable of physical interaction with antigens. The effectors in an immune response.
antigen
any chemical compound that triggers the adaptive immune response
antigen-presenting cell
have peptide fragments on their cell surface; the majority are from self-proteins and a few are from foreign antigens. This is essential for activation of the T-cell response to foreign antigens.
bacteria
single-celled or noncellular spherical or spiral or rod-shaped organisms lacking chlorophyll that reproduce by fission
chemotaxis
Inflammatory chemicals attract phagocytic cells to the area, which leave the blood (extravasation) and enter the damaged tissue.
complement
activation through the FC region, leading to cell lysis and attraction of other leukocytes.
cytotoxic T cell
Type of lymphocyte T cell that destroys cells infected with viruses and tumor cells by releasing lymphokines that destroy cell walls. Also called killer cell and effector cell.
bind to antigens on plasma membrane of target cells and destroys them
viruses
Pieces of genetic material surrounded by a protein coat
immune complex
combination of an antibody and antigen, can initiate a hypersensitivity reaction
innate immunity
does not require prior exposure to a foreign substance. The components of innate immunity are present before exposure and are not specific.
includes:
-External physical, chemical, and microbial barriers that prevent the entry of foreign threats and may physically remove them.
-Internal cells, proteins, and chemicals that act directly against foreign threats.
-Stereotypic responses of inflammation and fever.
Uses cytokines and Leukocytes
lymph node
junctions of lymphatic vessels located where foreign threats are most likely to enter the body. These trap foreign cells and threatening material, and activate immune cells. non encapsulated.
lymphoid tissues
tissues that contain mature and circulating lymphocytes, including tonsils, lymph nodes, spleen, appendix,
memory cell
A lymphocyte responds to an antigen upon reintroduction. They do not produce antibodies but increase the number of B-cells that express a receptor for a specific antigen.
Carry the memory of antigen exposure after the antigen has left the body
MHC class I
glycoproteins expressed on the surface of almost all nucleated cells.
MHC class II
glycoproteins expressed on the surface of macrophages, dendritic cells, and B-lymphocytes.
naïve lymphocytes
express on their surface the BcR but have never been exposed to an antigen
opsonin
any molecule (chemical or protein) that increases the phagocytosis of antigens by macrophages. This work by masking the normal negative charge on the outer surface of cells and proteins, and macrophages have surface receptors—like CR1—that bind to this
phagosome
Intracellular vesicle containing material taken up by phagocytosis.
Primary lymph organs
Where lymphocytes develop and mature (e.g., thymus, bone marrow)
secondary lymphoid organs
lymph nodes, spleen, tonsils
Neutrophils
made in bone marrow, most common, they perform phagocytosis and produce inflammatory responses.
Basophils
A circulating leukocyte that produces histamine, made in bone marrow, similar to mast cells
Eospinophils
are large long living phagocytes that defends against multi-cellular invaders, made in the bone marrow and participate in immediate hypersensitivity reactions.
Monocytes
Exit circulation and transform into macrophages, which engulf foreign invaders by phagocytosis
Lymphocytes
serve as recognition cells for specific immune responses. 2 types b cells and t cells, b cells and NK cells mature in the bone marrow, and T cells in the thymus
B cells
Initiate antibody mediated immune responses by binding specific antigens to the cells' plasma membrane receptors (immunoglobins), when activated transform into plasma cells & secrete antibodies that help T-cells
Helper T cells
secrete cytokines that help B, T, and NK cells and macrophages, they send out the signal to fight
Regulatory T cells
Act as inhibitors to other immune cells
Maintain immunological tolerance
• Block T cell-mediated immune responses at the end of the response window
NK Cells
Bind directly and non-specifically to virus and cancer-infected cells and kills them, part of antibody dependent cellular cytotoxicity ADCC
Plasma Cells
made in peripheral lymphoid organs differentiate from B cells during immune responses. they secrete antibodies
Macrophages
made in bone marrow, but are all over body, they do phagocytosis, extracellular killing via release of toxic chemicals, process and represent antigens to helper t cells, secrete inflammatory cytokines,
Dendritic cells
specialized white blood cells that patrol the body searching for antigens that produce infections, antigen presentation and phagocytosis, made in almost everywhere and microglia in the central nervous system
Mast cells
made in bone marrow and found almost everywhere they release histamines and other chemicals involved in inflammations, differentiate from bone marrow cells
Immune defenses
can be innate and nonspecific bc the identity of the target is not recognized, or adaptive bc they have a specified target.
Myeloid Cells
neutrophils, basophils, eosinophils, monocytes, dendritic cells, macrophages, mast cells
Lymphoid cells
B cells, T cells, NK cells, plasma cells
Leukocytes
circulate in blood but function mainly in the tissues
Phagocytes
eat foreign matter and destroy it internally
Cytokines
Protein messengers from certain immune cells that regulate immune responses, provide cross-talk b/w different immune system cells
Lymphatic vessels
These begin as fenestrated capillaries. Lymph is transported through progressively bigger vessels, through lymph nodes, until it reaches the vena cava. Larger ones contain one-way valves and smooth muscle
The thymus
primary gland of the lymphatic system, Flat, bi-lobed organ located in superior mediastinum above heart. Enlarges during childhood, then starts to atrophy as we enter our 20s. Each lobe is comprised of lobules held together by areolar connective tissue
cell-mediated immunity
Immunity against abnormal cells and pathogens inside living cells, produced by T cells that attack infected or abnormal body cells
antibody-mediated immunity
The production of antibodies by B cells in response to an antigen. Also called humoral immunity.
Spleen
• Filters blood, stores erythrocytes, removes defective erythrocytes/ platelets, recycles iron
• Lies between 9th and 11th rib on left side of body• Contains red pulp and white pulp
• Red pulp contains macrophages, erythrocytes, platelets, granulocytes, reticular cells, fibers
Positive selection
ensures lymphocytes are able to respond to antigen
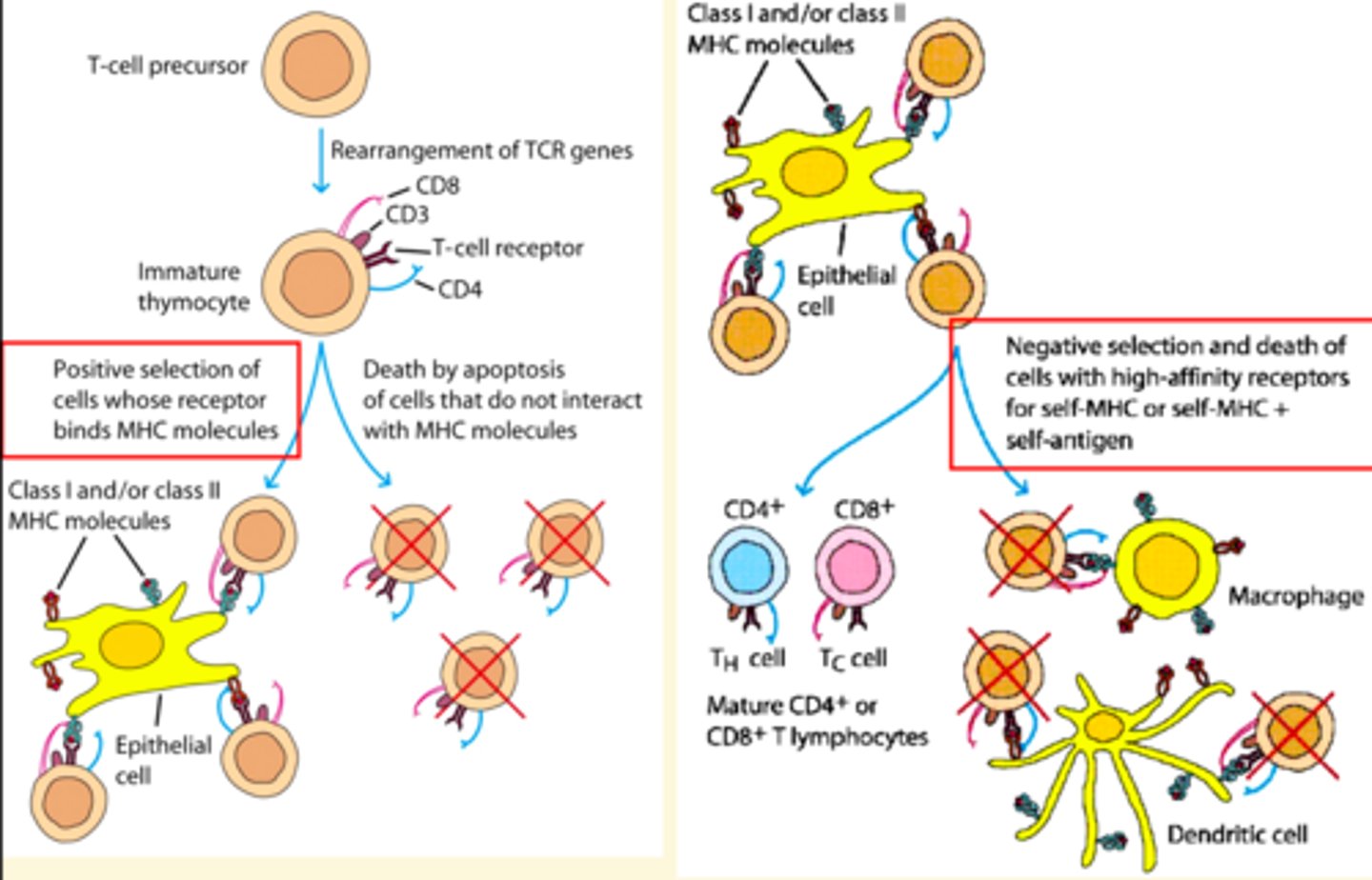
Negative Selection
removes lymphocytes that bind strongly to self antigens
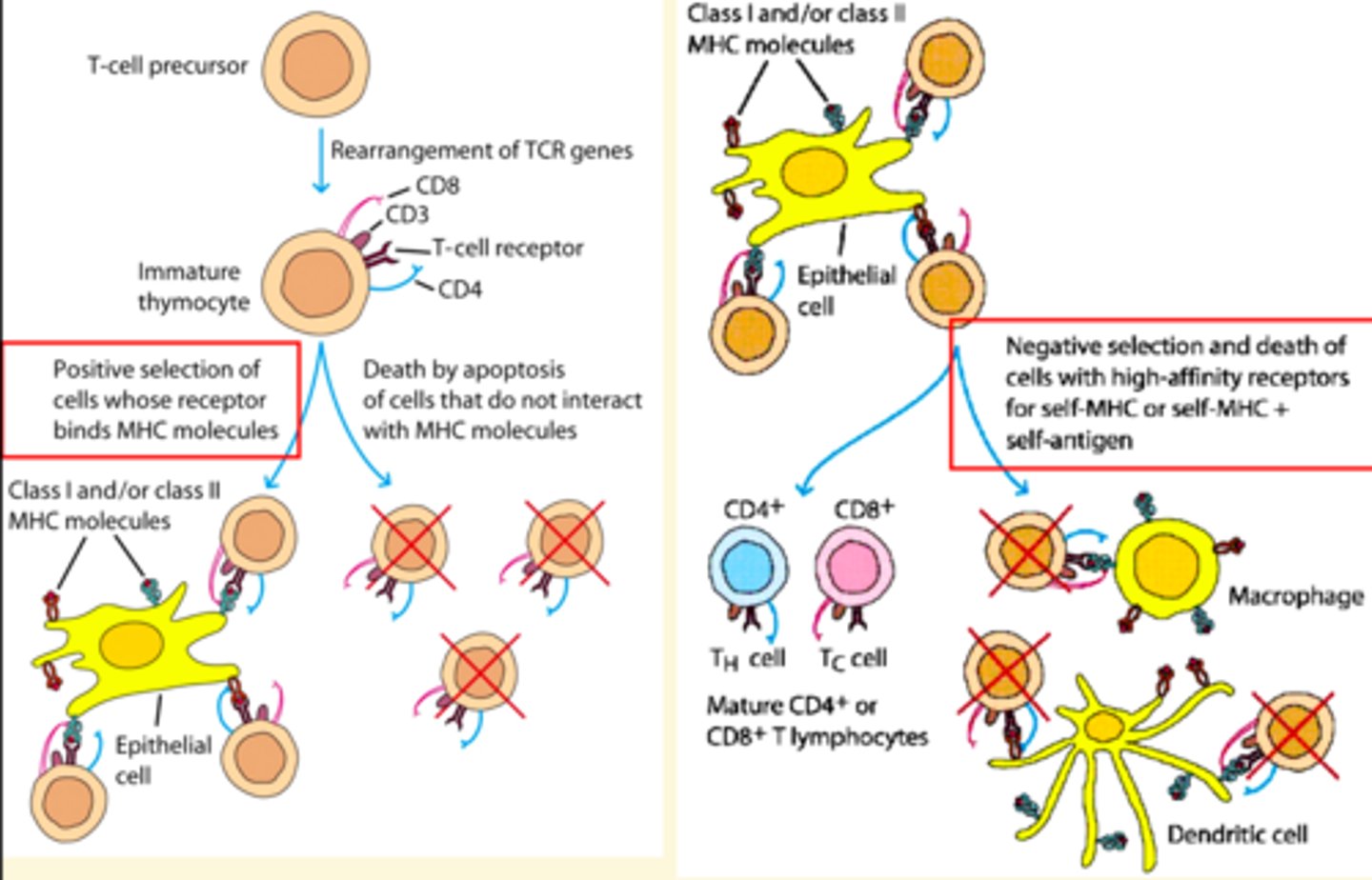
outcomes of negative selection of lymphocytes
-Receptor editing: change the lymphocyte receptor so it no longer recognizes self antigens
-Anergy: change the lymphocyte so it is no longer capable of an immune response
-Apoptosis: clonal deletion and cell death
-Ignorance: continue maturation
innante immunity
defenses against any pathogen; rapid, present at birth, includes, Histamines, neutrophils, basophils, mast cells, Eosinophils, NK cells, and macrophages
Interferons
chemical messengers from virus infected cells that trigger production of antiviral proteins in normal cells
process of macrophage phagocytosis
1) drawn to site by chemotaxis
2) physical interaction between them and foreign threat
3) produce pseudopodia that extend around foreign threat
4) pseudopodia fuse foreign threat within a vesicle forming a phagosome
5) phagosome is internalized, fuses with lysosome
6) proteases and toxic chemicals in lysosome kill foreign threat
7) parts of the foreign threat are exposed on the cell surface--antigen presentation
Adaptive immnity
Uses lymphocytes, like T cells and B cells, they use memory cells, classic completements Antigens and Antibodies, we develop this form throughout life.
Antigen
anything that can trigger an adaptive immune response. The immune system recognizes epitopes—discrete sites on macromolecules. Any molecule has the ability to act as it, but some are more potent than others. Proteins are most potent, followed by sugars
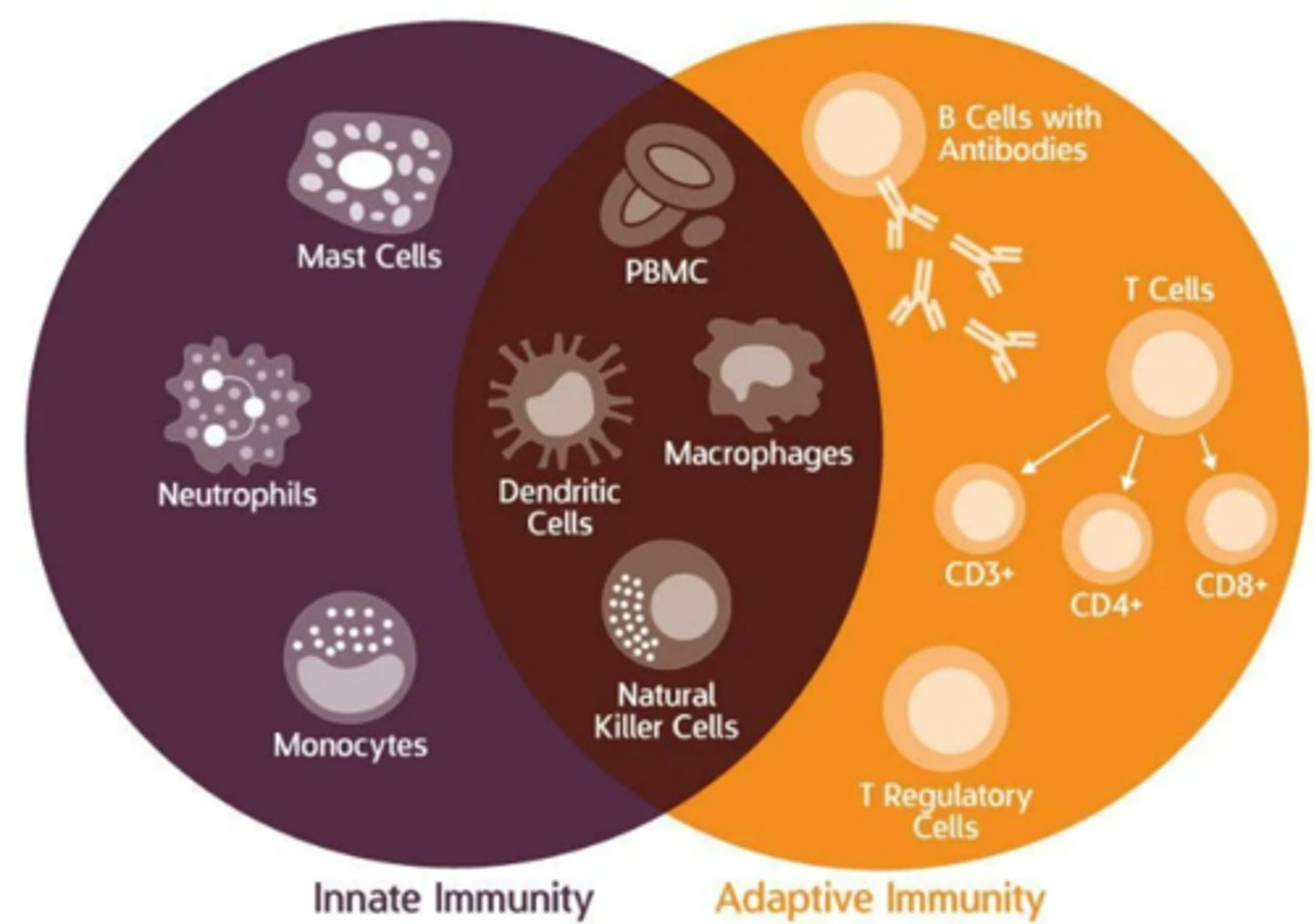
Adaptive Immune system Vs Innate Immune system
innate uses nonspecific defenses to prevent foreign matter from entering the body and attacking any foreign cell that does enter the body.
adaptive immune there is an immune response that recognizes and responds to pathogens that enter the body based on their specific properties.
Functions of antibodies in adaptive immunity
-Antigen neutralization: Covering and blocking the surface of the antigen
-Antigen agglutination: Clumping of antigens into larger complexes more readily recognized by macrophages
-Antigen precipitation: Bringing antigens out of solution, making them more easily recognized by macrophages
-Complement activation: Through Fc region; leading to cell lysis and attraction of other leukocytes
-Lymphocyte recruitment and activation
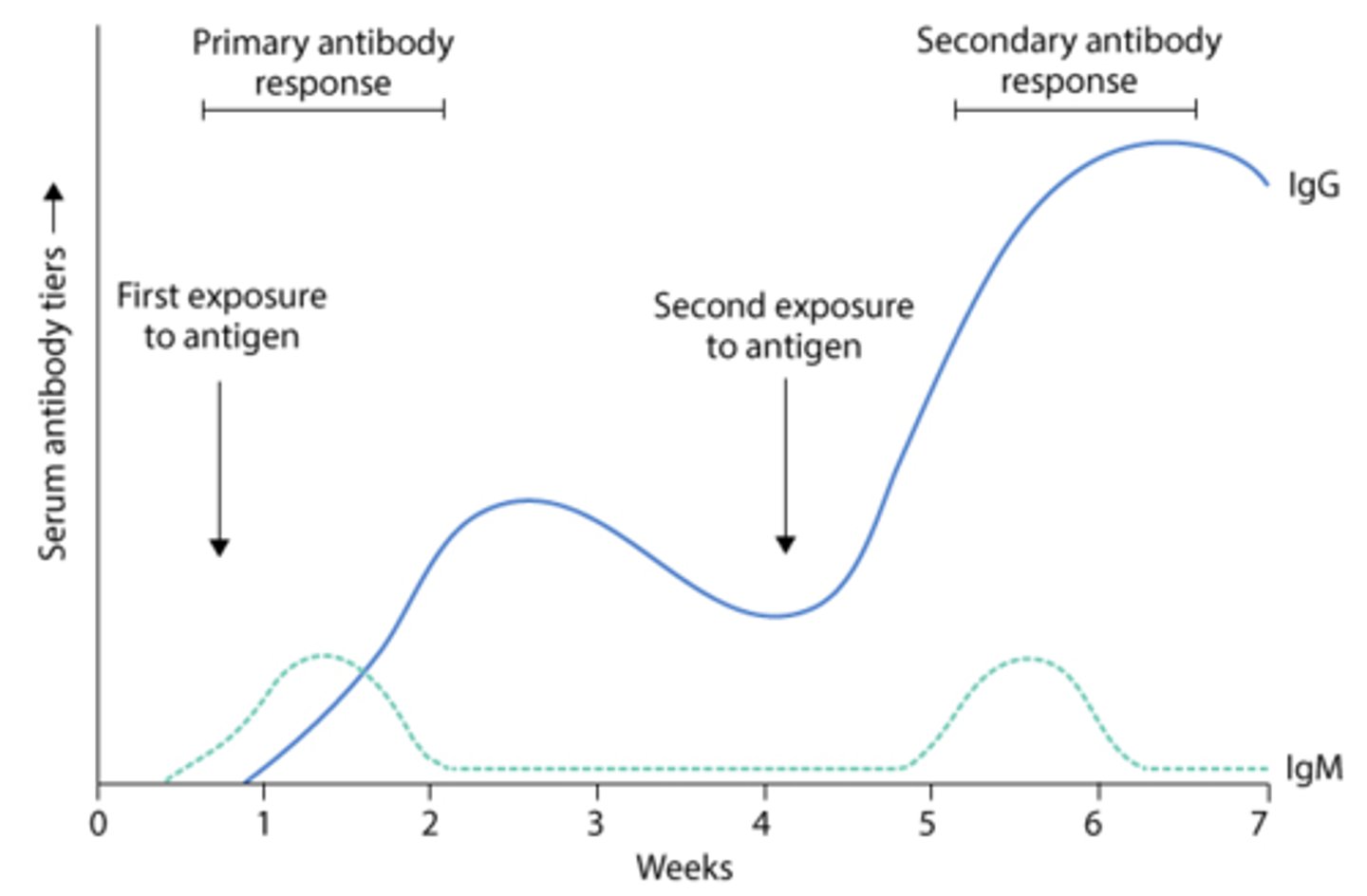
Primary versus secondary antibody responses
• Primary phase starts with IgM, while secondary phase starts with IgG
• Difference in primary and secondary response is due to presence of memory B cells in secondary response
• Antibodies are more rapidly produced in secondary response
What are the 5 types of Antibodies
IgG, IgM, IgA, IgD, IgE
IgG
crosses placenta, most abundant, activates complements and most used during 2ndary immune response
IgM
first to increase in primary immune response, work against viruses and bad blood, they're big so they stay in blood
IgA
its in the saliva and muscousa, and all the openings of body
IgD
Attached to B lymphocytes cells
Activates B lymphocytes cells
Acts like a receptor for antigens
IgE
allergic reactions and parasitic infections, works with basophiles and mast cells, for the inflammatory response,
Renal
a word used when referring to structures and processes related to the kidneys
Urination
The act of releasing urine from the body, can also be referred to as micturition, voiding, or uresis.
How the kidney and associated structures form urine
must ultrafilter the blood (filtration under pressure), reabsorb needed solutes back into the body, and secrete unwanted substances. Once urine has been formed, it flows out of the kidney into ureters, which in turn carry the urine to the urinary bladder for storage prior to release from the body. Urine leaves the body via the urethra
Ureters
Carry urine out of the kidneys to the bladder. Capable of peristalsis. Connect to the bladder at an angle that prevents backflow of urine. Further bladder filling also compresses the distal end, further preventing backflow
minor and major calyces
The collect urine produced by the kidney, which then moves into the renal pelvis. The renal pelvis is continuous with the ureter
retroperitoneal space
lateral to either side of the vertebral column, against the posterior wall of the abdominal cavity
renal hilum
The indentation on the medial side, it serves as an entryway to the hollow renal sinus. Lymphatic vessels, nerves, the renal artery, the renal vein, and the ureter enter the renal sinus by way of the renal hilum.
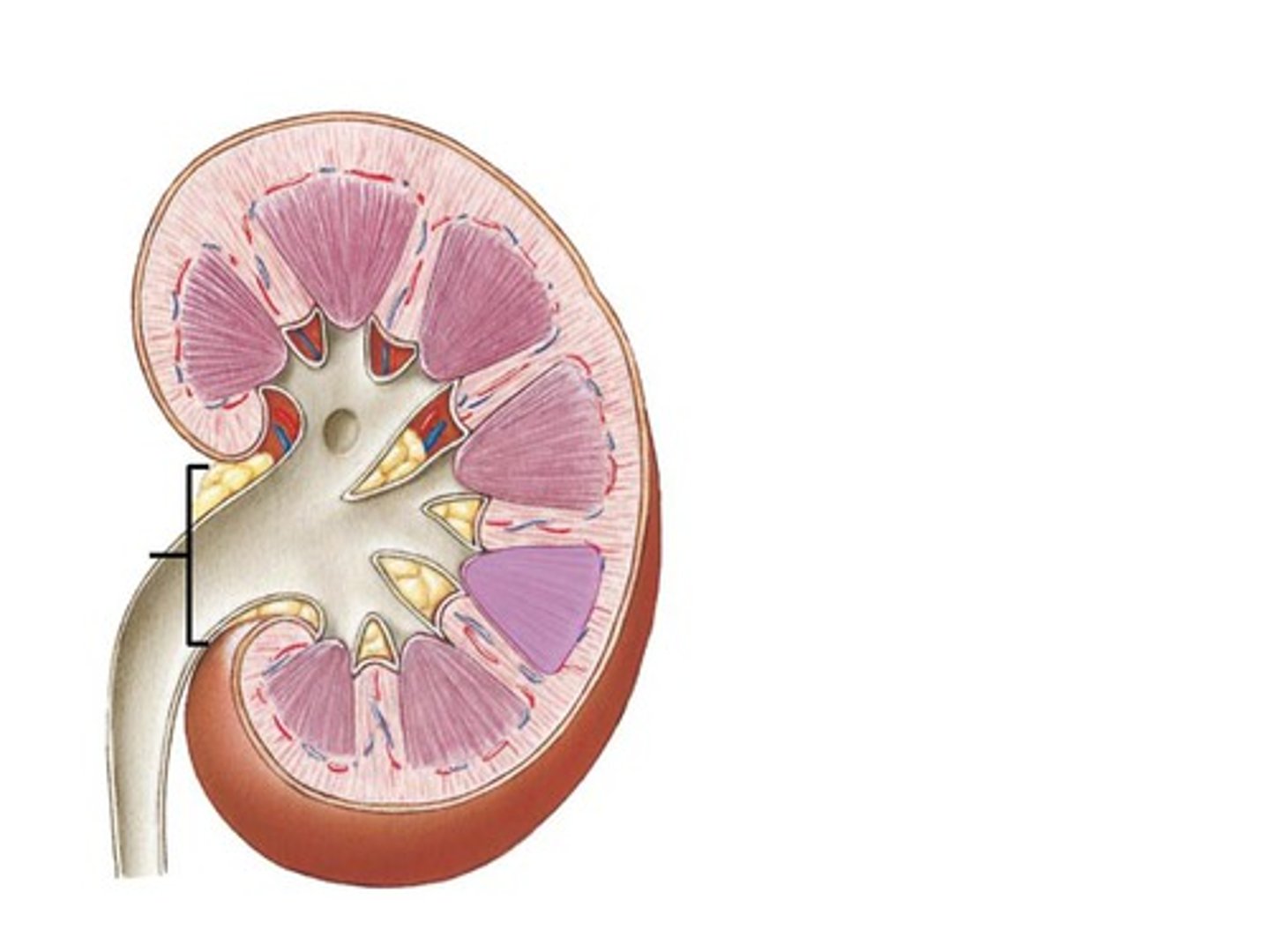
outer renal cortex
Granular tissue, form a shell around the medulla
Forms renal column—contains nephrons

inner renal medulla
tissue within renal pyramids
Nephron
onsists of two main components, a renal corpuscle and a renal tubule. A renal corpuscle, located in the cortex, is composed of a glomerulus, surrounded by a hollow glomerular capsule (or Bowman’s capsule). An afferent arteriole delivers blood to each glomerulus, which is then drained by an efferent arteriole. Filtration occurs as fluid and solutes are forced from the blood inside the glomerulus to the hollow space within the glomerular capsule.
Each nephron consists of two main components what are they?
a renal corpuscle and a renal tubule. A renal corpuscle, located in the cortex, is composed of a glomerulus, surrounded by a hollow glomerular capsule (or Bowman’s capsule).
glomerulus and bowman's capsule
An afferent arteriole delivers blood to each glomerulus, which is then drained by an efferent arteriole. Filtration occurs as fluid and solutes are forced from the blood inside the glomerulus to the hollow space within the glomerular capsule.
proximal convoluted tubule
located in the cortex, lined by simple cuboidal epithelium with microvilli. Bulk Reabsorption
• Glucose, amino acids, proteins, vitamins reabsorbed by secondary active transport, secretes acids and bases
• HCO3-, Ca2+, Mg2+, PO43-, also actively reabsorbed
• Water and other ions passively reabsorbed by osmosis
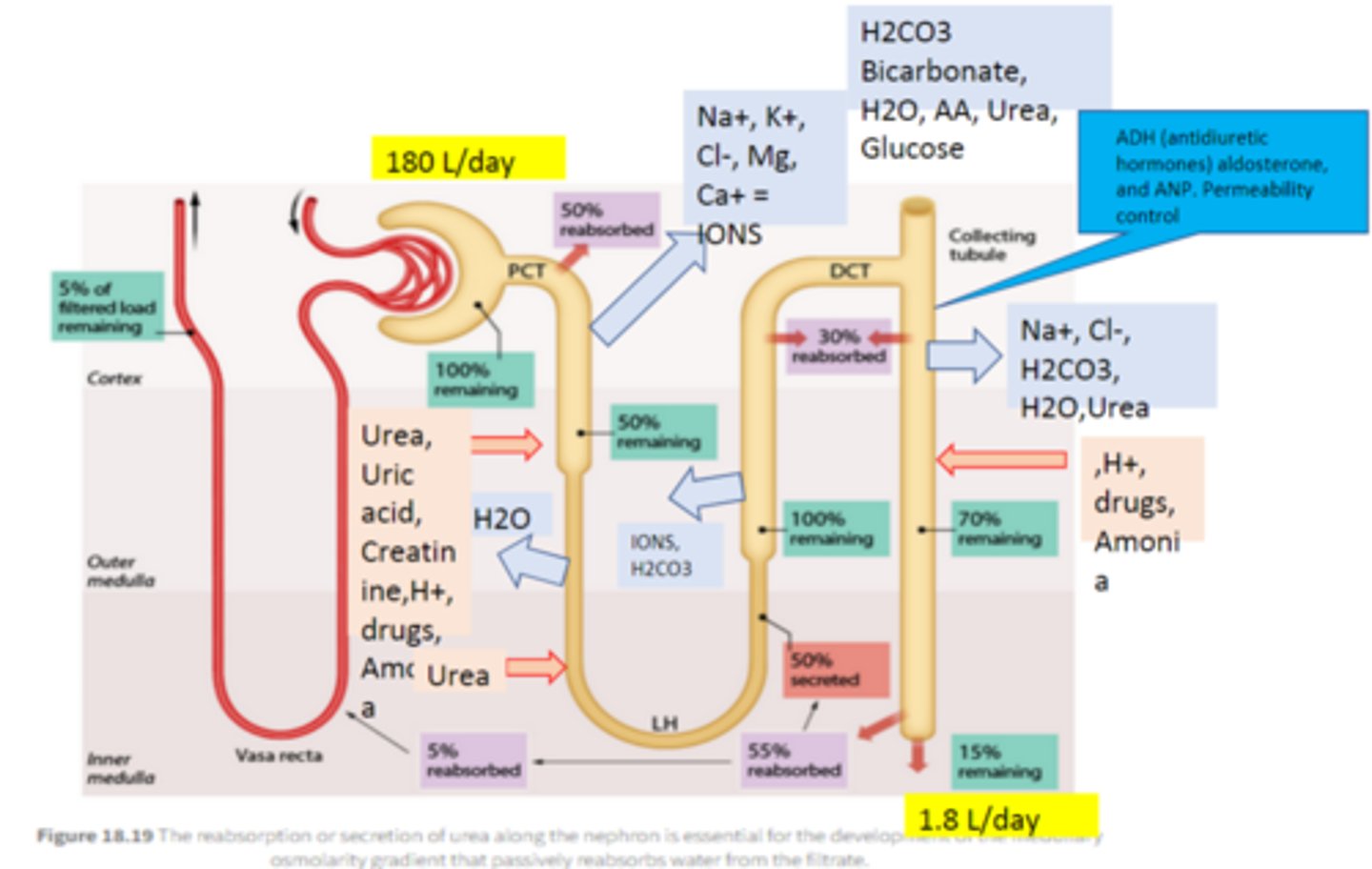
Ascending and descending loops
• Majority of remaining water, Na+, Cl- and K+ is reabsorbed
• Opposing permeability: descending loop is permeable to water(Bulk reabsorption of H2O passively), ascending loop is permeable to solutes (Bulk reabsorption of Na and Cl, actively)
thin segment of nephron loop
in the medulla, lined with simple squamous
thick segment of nephron loop
in the medulla, made of simple cuboidal
distal convoluted tubule
in the cortex, made of simple cuboidal without microvilli
Principal cells
Part of the collecting duct in the simple cuboidal epithelium, it adjusts the urine in order to maintain the body's water, Na+, and K+ balance, drain into papillary duct
Intercalated cells
cells in the collecting ducts of the kidneys that can absorb potassium if necessary, responsible for acid-base balance, drain into papillary duct
peritubular capillaries
In cortical nephrons, The network of tiny blood vessels that surrounds the proximal and distal tubules in the kidney
Vasa Recta
In juxtamedullary nephrons, its the network of tiny blood vessels that surrounds the proximal and distal tubules in the kidney
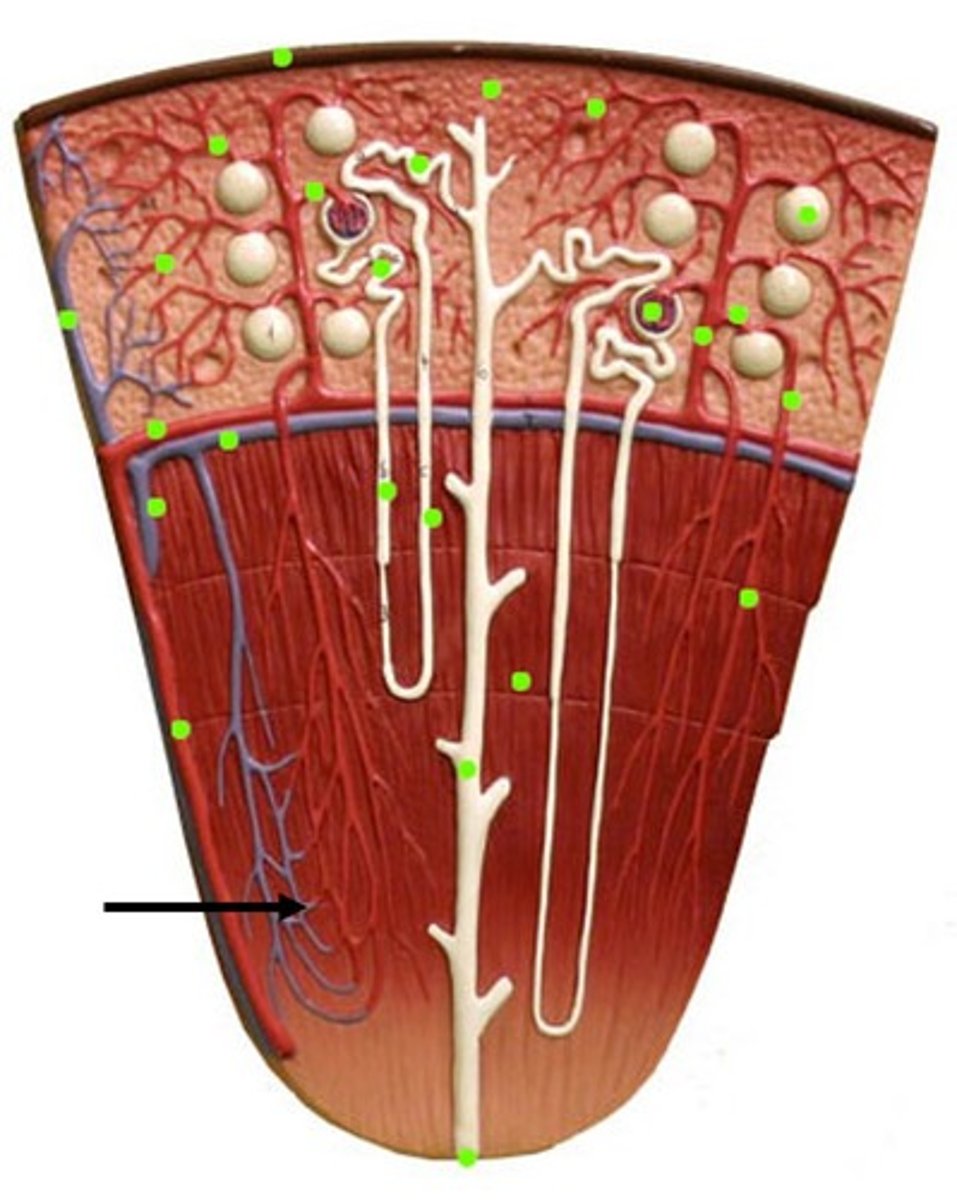
Cortical Nephron
Nephrons located almost entirely in the renal cortex. These nephrons have a reduced loop of Henle.
juxtamedullary nephrons
A small minority of nephrons, approximately 15% of the total, This type has a much longer nephron loop that extends deeper into the medulla.
juxtaglomerular apparatus (JGA)
the most distal portion of the nephron, that comes into contact with the afferent arteriole, There are two populations of specialized cells in this area for us to acknowledge.
Macula densa cells
specialized chemoreceptors, in the epithelium of the renal tubule monitor and respond to the concentrations of Na+ and Cl- in the filtrate.
granular cells, or juxtaglomerular (JG) cells
Specialized smooth muscle cells function as baroreceptors (pressure sensors) by responding to changes of blood pressure within the afferent arteriole by secretion of the protease renin
The three processes of urine formation and where they happen
first, ultrafiltration, occurs within the renal corpuscle, while the second and third, reabsorption and secretion, occur within the renal tubules and collecting ducts
Renal Lobe
consists of a renal pyramid and the surrounding cortical tissue. The end of this is called the renal papilla.
Ultrafiltration
the movement of fluid and solutes (smaller than proteins) from the blood in the glomerulus to the glomerular capsule space, driven by Starling forces—the predominant force being blood pressure in glomerular capillaries. This process is size-selective, meaning that anything smaller than ~7 nm is filtered into the nephron but is not solute-specific
reabsorption
solute-specific process during which particular solutes are brought from the tubular lumen into the interstitial space and then into the peritubular capillaries (or vasa recta)
Secretion
Solute-specific, is the movement of solutes from peritubular capillaries (or vasa recta) to the interstitial space and then into the tubular lumen.
filtration barrier
composed of fenestrated capillary endothelium, a single layer of basement membrane, and podocyte cells with foot processes—pedicels
The filtration barrier is size and charge-selective. The components of the filtrate are determined by the relative permeability of these sublayers
-freely permeable to water, all ions, and small molecules (glucose, amino acids, etc.). It is impermeable to all proteins, charged macromolecules (like heparan sulfate), and cells.
mesangial cells
outside the filtration barrier, and help to make the glomerular capsule.
Podocyte Pedicles
long cytoplasmic processes that interdigitate with those of adjacent podocytes to create filtration slits preventing the passage of any remaining macromolecules
Angioblasts
form the filtration barrier, and blood vessel precursor cells, they interact with mesangial cells and developing podocytes by releasing signals, such as when vascular endothelial growth factor (VEGF) interacts with cell surface receptors
glomerular blood hydrostatic pressure (GBHP)
Drives filtration and is the afferent arteriole blood pressure within the glomerulus
Capsular hydrostatic pressure (CHP)
As water passes through the filtration barrier it develops a fluid pressure that opposes filtration. Also opposing filtration is the osmotic pull of proteins that are not passing through the filtration membrane