NUR 315 Exam 3 - Postpartum Maternal Physiologic Adaptation
1/25
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
26 Terms
Uterus postpartum changes
Involution
Decreasing size and weight
Muscle contraction, catabolism, and regeneration
Separation of decidua
The thick layer of modified mucous membrane which lines the uterus during pregnancy and is shed with the afterbirth
Fundal height
Decrease corresponds with # days postpartum
Afterpains
Pain associated with contractions after birth
Fundal height
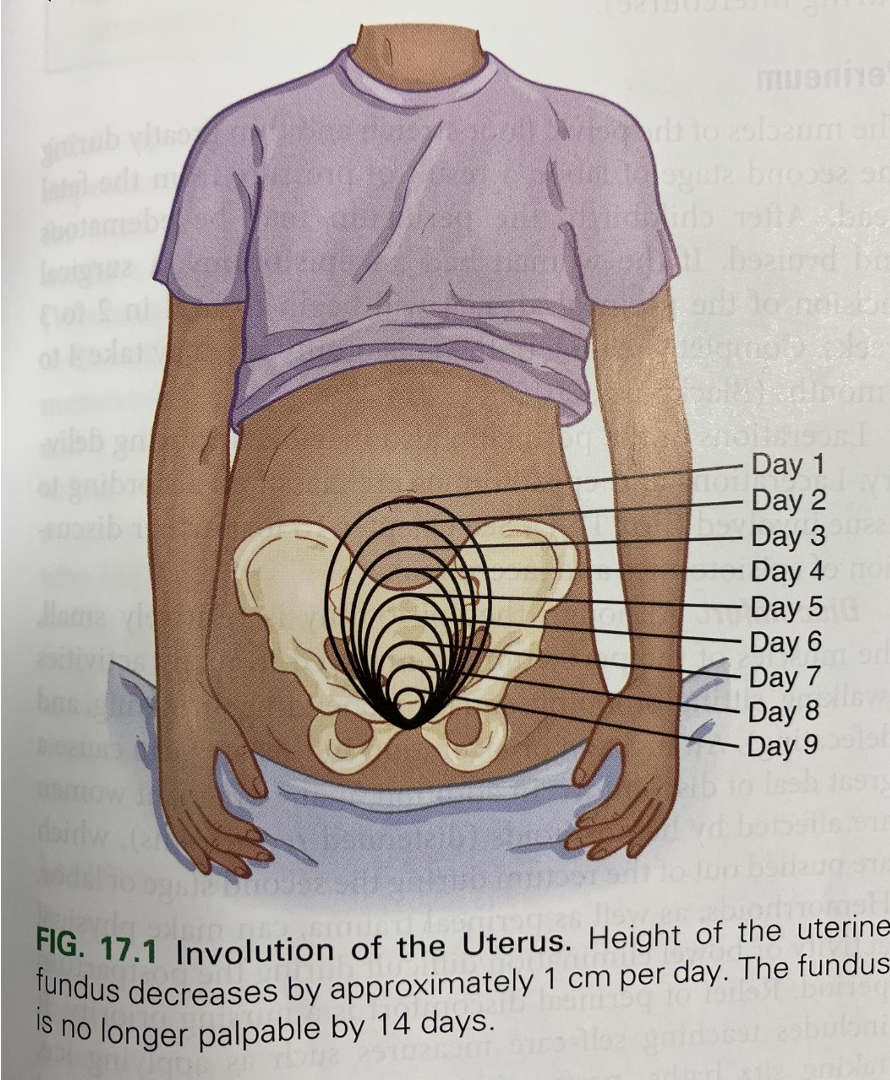
Lochia patterns
Short time frame of bleeding 7-14 days after birth (associated with sloughing at the placental attachment site)
Lochia rubra (days 1-3)
Lochia serosa (days 3-10)
Lochia alba (days 10-42)
Lochia rubra
Days 1-3
Bloody, small clots, dark red or red-brown
Lochia serosa
Days 3-10
Serosanguinous, pink or brown tinged
Lochia alba
Days 10-42
Serous, white to light yellow
Measuring lochia
Consider
Time since last pad change and any position change
Quantified blood loss (QBL)
Weigh pad with lochia
Weigh clean pad
Subtract the difference
Estimated blood loss (EBL)
Scant
Light
Moderate
Heavy
Excessive (saturated in 15 min)
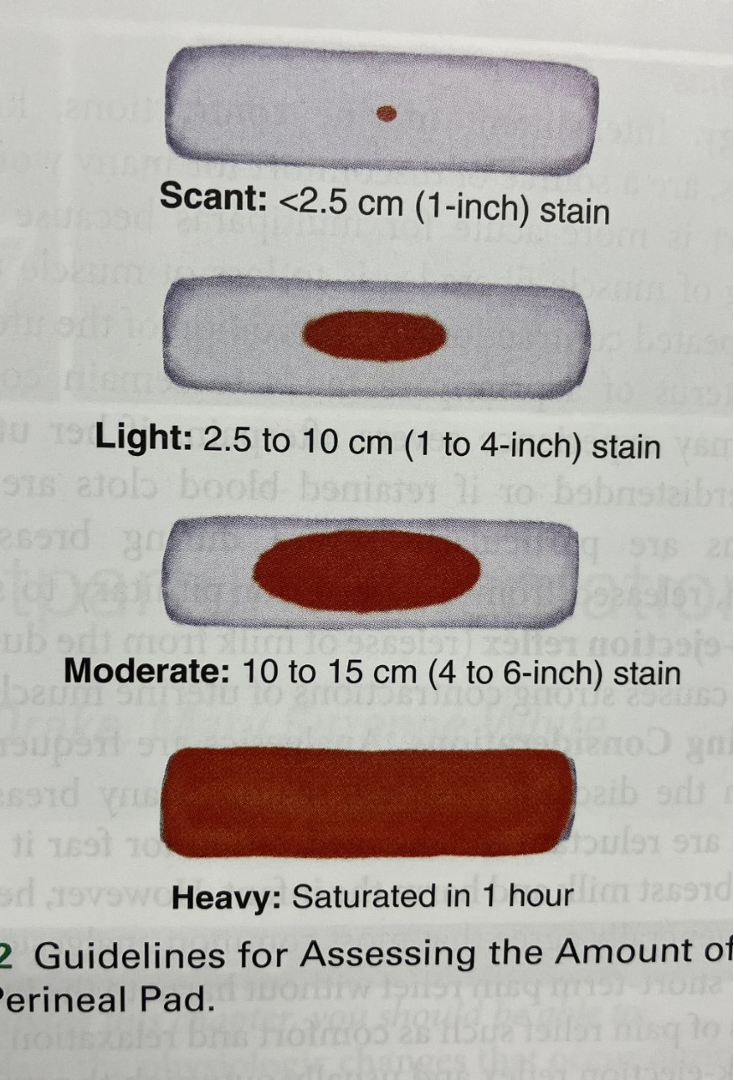
Calculating blood loss
Remember 1 gram is assumed to equal to 1 mL of blood
Assume one dry peripad = 30 grams
Assume one dry chucks pad = 100 grams
Cervix postpartum changes
Dilated, edematous, and bruised after birth
Small lacerations may be present
Returns to 1 cm by 1 week postpartum
Internal os shaped slit-like rather than round
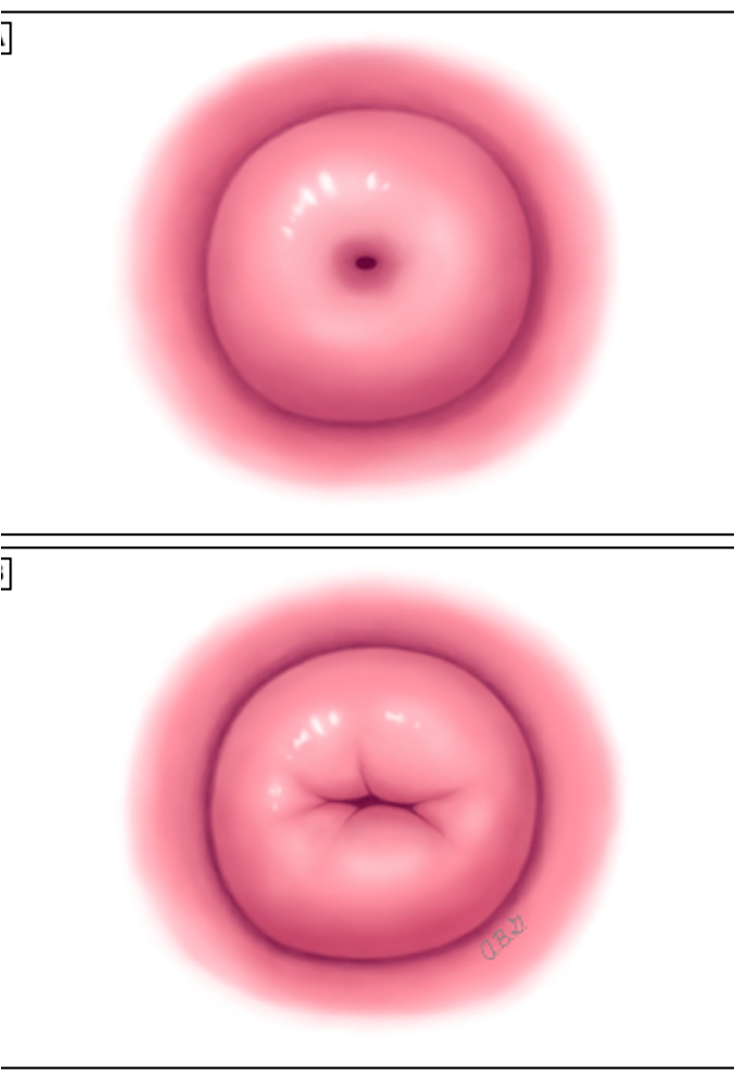
Vagina postpartum changes
Vaginal walls
Edematous with small lacerations
Tone and rugae slowly improve starting about week 3
Cervical mucus
Less production until estrogen levels re-establish
More likely to experience dyspareunia (painful intercourse)
Perineum postpartum changes
Edematous and bruised
Episiotomy begins healing about wk 2-3; complete 4-6 mo
Labor may create or worsen hemorrhoids
Pain with positional changes or bowel movements
Ovulation and mensturation postpartum changes
First few bleeds may be anovulatory
Ovulation may begin before 1st menses
Nonlactating: resumes in about 6 to 10 weeks
Lactating: resumes in 10 weeks to 6 months, but may be shorter or longer duration
Breasts postpartum changes
Placental brith triggers increase in breastmilk production
Oxytocin = breastmilk let-down
Areola darker as a visual cue to infant
Breastmilk phase 1
Colostrum
First milk following delivery
Production starts by week 16 of pregnancy
AKA liquid gold, thick, yellowish-white fluid
High in protein and IgA
Lower in carbs and fat than breastmilk
Assists in infant digestive system bacteria growth
Breastmilk phase 2
Transitional milk
Starts 2-5 days after delivery until 2 weeks
Sometimes bluish-white in color
Often associated with initial symptoms of breasts feeling warmer and fuller (AKA Engorgement)
Breastmilk phase 3
Mature milk
Starts 10-15 days after birth
Should allow infant to empty one breast before changing to other side to ensure proper mix of nutrients at each feeding.
Demand vs. supply dependent
Breast care general recommendations
If non-breastfeeding...
Wear form-fitting bra (but not super tight)
Do not express milk unless necessary for comfort
If breastfeeding...
Breastfeed, pump, or hand express q 2-3 hr approx. 15 minutes/session
No special cleansers or ointments needed, but can use lanolin for chapping
Engorgement
Feed as appropriate to empty regularly
Use cool packs; cabbage leaves; supportive bra
Consult early and often with clinical expert if questions or concerns!
Postpartum cardiovascular changes
Blood volume
Immediate loss of ~1000 mL during delivery
Rebound increase of 900–1200 mL over days due to fluid redistribution
Normal plasma volume restored by 6–8 weeks postpartum
Cardiac output
Elevated during pregnancy
Returns to baseline by ~6 weeks postpartum
Heart rate & blood pressure
Heart rate normalizes within 6 weeks
Blood pressure typically returns to pre-pregnancy levels early in the puerperium
Hormonal influence
Fluctuations in estrogen and progesterone affect vascular tone and fluid balance
Thrombosis risk
Increased coagulation factors (I, II, VII, VIII, IX, X) during pregnancy
Risk of thromboembolism heightened postpartum, especially with trauma or immobility
Cardiac output at pre-pregnancy levels within 6-12 wk via diuresis and diaphoresis
Postpartum hematologic changes
WBC
Leukocytosis up to 30,000 can be normal during labor/immediate postpartum
Temp up to 38 degree (100.4) for first 24 hr
Baseline WBC's by day 6
RBC and clotting
Vary widely depending on compensatory mechanisms, normal physiology, and blood loss during delivery
Baseline Hct and clotting factors by 4-6 wk
Postpartum gastrointestinal changes
Increased hunger d/t energy expenditure
Increased thirst
From exertion
Breastfeeding
Fluid loss
Constipation
Progesterone levels decrease gradually
Recent decreased food and fluid intake
Discomfort → ineffective bowel movements
Iron intake
Normal bowel pattern
Return by 8 to 14 days postpartum
Postpartum urinary changes
Urinary retention initially
Urethra edematous, traumatized
R/t diuresis and decreased sensation
May displace uterus from midline
Baseline kidney function within 4 weeks
Increased bladder capacity and decreased tone
Stress incontinence
Takes several weeks to months to resolve
Postpartum musculoskeletal changes
Muscles
Fatigue and aches from labor exertion
Decrease in relaxin
Ligaments and cartilage return to pre-pregnancy position
Abdominal muscles
Weaker
Softer
May separate longitudinally
Postpartum integumentary changes
Chloasma and linea nigra gradually fade and disappear
Striae gravidarum fade but do not disappear
Increased hair loss due to increased hair growth during pregnancy
Postpartum neurologic changes
Anesthetics or analgesics
Cause temporary lack of feeling in extremities or dizziness
Headaches may occur...reasons vary
Normal fluid-electrolyte changes?
Pre-eclampsia?
Stroke?
Post-dural puncture headache?
Postpartum endocrine changes
Decrease in estrogen, progesterone, and human placental lactogen
Prolactin
Supersedes and triggers more breastmilk production
Returns to pre-pregnancy level in non-breastfeeding parents
Helps regulate the menstrual cycle
Postpartum vaccines
MMR or varicella if mother's titers were non-immune prenatally
Influenza if in season and not given during pregnancy
Rhogam within 72 hours after birth for Rh- mother if baby is confirmed as Rh +