Lab Dx Exam 8 (OBGYN, Newborn Screening)
1/95
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
96 Terms
What is a pap (papanicolaou) smear?
Screening test that detects neoplastic cells in cervical/vaginal secretions
95% accurate in detecting cervical cancer
What types of cells are shed into cervical and endometrial secretions?
Cervical and endometrial cells
What is the updated method for pap smear?
Liquid-based cervical cytology (LBCC)
Specimen is placed in preservatice solution, the old method involved actually "smearing" the specimen directly on to the slide
What is the benefit to the new pap smear screening?
Blood and debris left in solution, spun down where only cells left are examined on the slide
Why are two samples taken during a pap smear?
- First is to test the cells
- If abnormal can use the second sample fror further testing
When is a pap smear contraindicated?
- During menses
- Patients with vaginal infections (can introduce infection into uterus when swabbing)
What are some interfering factors with a pap smear?
- Delay in fixinf the specimen
- Lubricants
- Douching
- Drugs (digitalis, tetracycline)
What are the guidelines for cervical cancer screening?
- <21 y/o or women who have a hysterectomy: no screening
- 21-29 y/o: cytology for cervical cancer alone (thin prep) every 3 years
- 30-65 y/o: cytology for cervical cancer every 3 years, HPV every 5, OR combo every 5
- >65 y/o: no screening recommended as long as they have had 3 prior negative consecutive pap smears and have never had any abnormalities
How do we perform a pap smear?
- Do pap smear before bimanual exam
- Use water lubrication only (if needed)
- Sample endocervix with a brush, and ectocervix with a spatula, or use broom --> include T zone
What are the different histologic reports we can get from a pap? (2)
- "Normal" - no atypical cells found
- "Abnormal"
Abnormal cervical cells are known as:
Cervical intraepithelial neoplasia (CIN)
Cervical glandular intraepithelial neoplasia (CGIN)
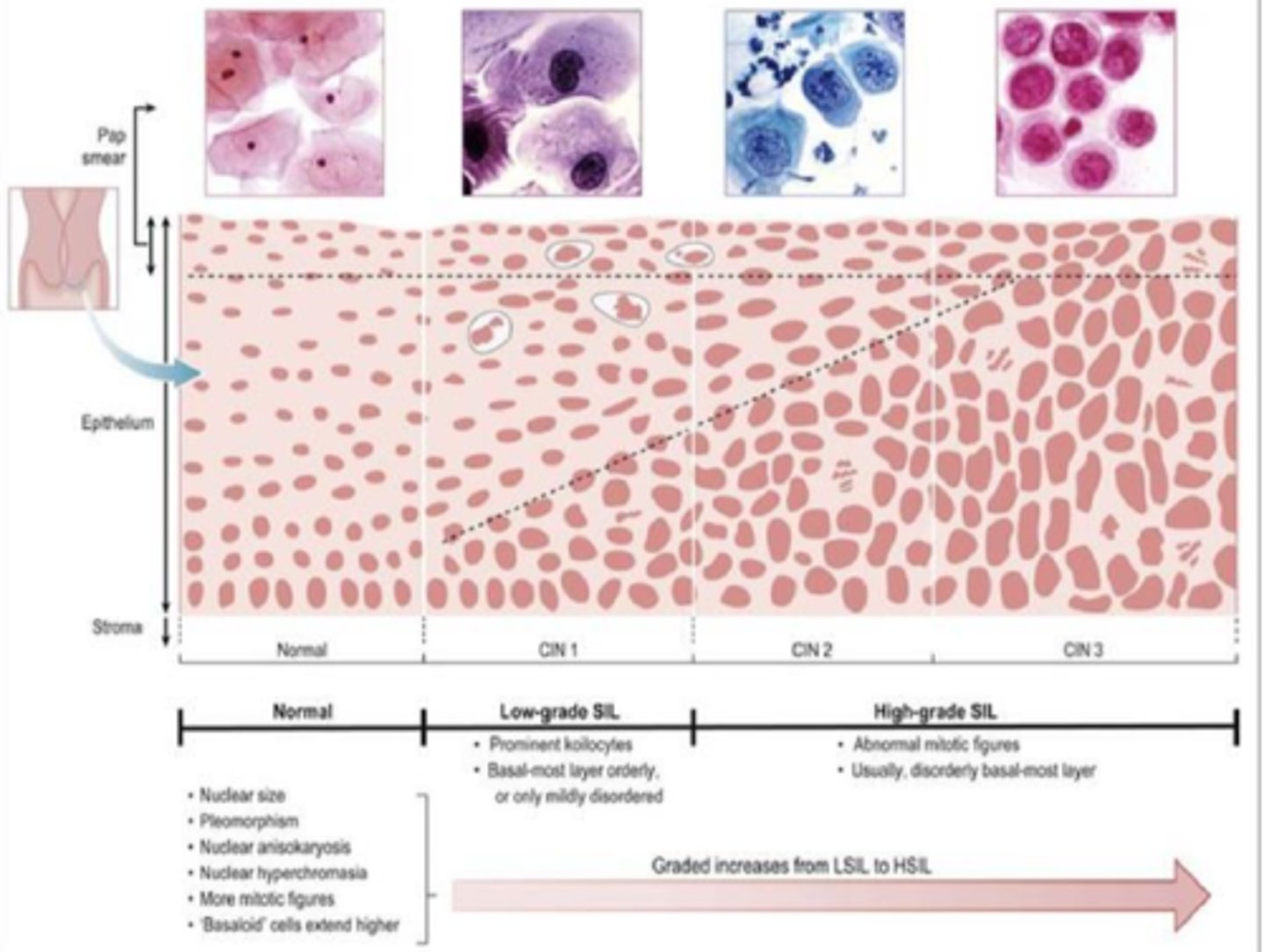
What does ASC-US stand for in an abnormal pap result?
Atypical squamous cells of undetermined significance
What does an ASC-US pap result mean?
Almost always HPV - second sample is used for testing direct HPV mRNA
If HPV testing is not able to be done repeat in 4-6 months
What does LSIL stand for in an abnormal pap result?
Low grade squamous intraepithelial lesion, involvement of inner 1/3 of the epithelium
CIN-1 or mild dysplasia
What does a LSIL pap result usually do?
Spontaneously regresses
What does HSIL stand for in an abnormal pap result?
High grade squamous intraepithelial lesion, involvement of the outer 2/3 of epithelium
CIN II and III, moderate/severe dysplasia
What does an HSIL pap result indicate?
35% with this result develop into cancer within 10 years
What are some other abnormal results of pap cytology?
- Atypical glandular cells
- Endocervical adenocarcinoma in situ
- Adenocarcinoma
What is CIN 1?
Slight changes in cells (unlikely to become cancerous, may go away on their own)
This is LSIL
What is CIN 2?
Moderate changes in cells (will become cancerous, tx and removal recommended)
This is HSIL
What is CIN 3?
More severe changes in cells
This is also HSIL
What is HPV (Human papillomavirus)?
- DNA tumor virus infecting gential areas, throat and mouth
- Spread via skin to skin contact
- Can be asymptomatic or result in gential warts
- Some are low risk, others are high risk (like 16 and 18)
- Women >30 years old: 60% high risk, while <30 likely regresses
How long does it take for actve HPV to clear?
12-18 months
Repeat DNA testing after this time, if still positive should have aggressive cancer monitoring
What is done for HPV screening?
Cervical cytology and HPV DNA screening via ELISA testing
What is important about oropharyngeal HPV?
- Leading caused of oral cancer in non-smoking patients aged 33-35
- Only 1% of patients have HPV 16 (most clear the virus naturally and sceening is not cost effective since we already do paps)
Flow chart for HPV screening
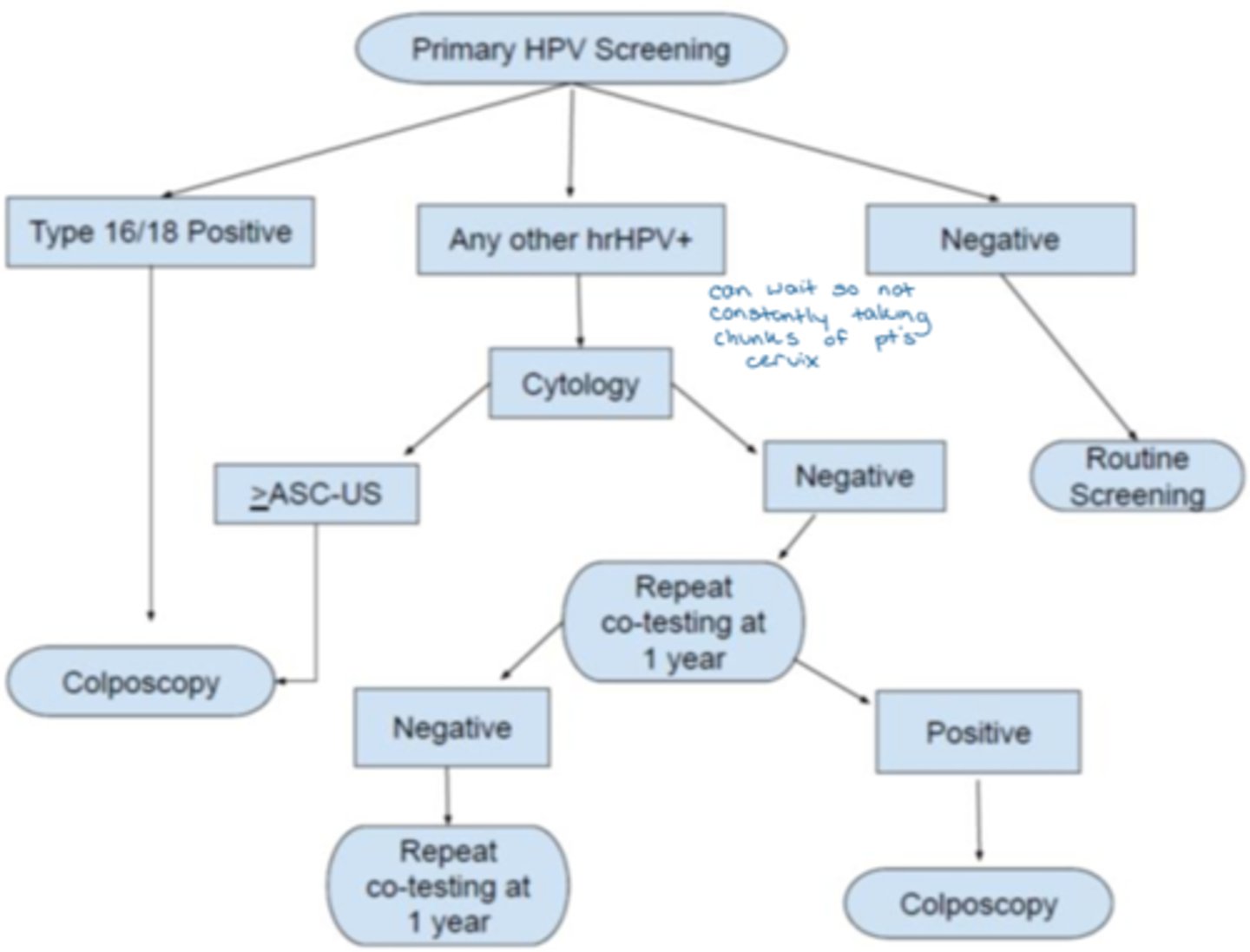
What is colposcopy?
Microscopic examination of vagina and cervix using colposcope
Looks for dysplasia, CIN, and invasive cancer
What is a "satisfaction" colposcopy?
Entire transformation visualized, biopsy is taken, and endocervical curettage taken
What is conization?
Cone shaped tissue removed, cone biopsy
When is a cone biopsy indicated?
- Pap shows HSIL and colposcopy uncertain (Transformation zone not visualized, or lesions extends beyond vision)
- Pap shows adenocarcinoma
- If endocervical curette doesn't match PAP or curette shows HSIL
Where is tissue taken from in a colposcopy?
Transformation zone (middle portion of line in cervix where columnar epithelium is being replaced by squamous epithelium)
What is endometrial testing done for?
Fertility reasons, abnormal bleeding, and endometriosis
What does endometrial testing determine?
- If ovulation has occurred
- Estrogen and progesterone levels
- Dx CA and polyps
- Evaluate abnormal bleeding
- Thickness of uterus
What are some examples of endometrial testing?
- Hysterectomy
- Endometrial biopsy
- Ultrasound
- D&C
What is a hysteroscopy?
Visualization of the uterus for polyps and tumors
Why is an endometrial biopsy done?
Histopathology for cancer
What are contraindications for endometrial biopsy? *not in slides
- Pregnancy
- Acute pelvic inflammatory disease (PID)
- Clotting disorders (coagulopathy)
- Acute cervical or vaginal infections
- Pt in whom cervix cannot be visualized
What does an ultrasound measure in regards to the endometrium?
Endometrial thickness and location (enometriosis)
What is a dilation and curettage (D&C)?
Cervical dilation and scraping of the endometrium with surgical instruments (curettage)
What is dilation and curettage (D&C) done for?
Diagnostic and therapeutic
- Heavy menses or irregular pleasing from hyperplasia
- May remove polyp
Used for menstrual irregularities (unless bx has already dx CA)
What is beta-hCG?
Beta human chorionic gonadotropin
Secreted by the placental trophoblast after the ovum is fertilized --> seen in the blood and urine during pregnancy
How should hCG increase in pregnancy?
In the first 30 days should double every 2.2 days
What can an US observe in early pregnancy?
- Intrauterine sac can be identified at 5-6 weeks
- Heart detected at 7 weeks
What is the quantitative vs. qualitative measurement of beta-hCG?
Quantitative: measures the specific amount of beta-hCG in the blood (ex: urine and serum)
Qualitative: gives a simple positive or negative result to whether beta-hCG is present and the patient is pregnant or not (ex: at home urine test)
What are the different categories for quantitative measurement of beta-hCG?
<5IU = negative
5-25IU = undetermined
>25IU = positive
What causes b-hCG levels to be increased?
- Molar pregnenacy
- Multiples
- Trophoblastic disease
What causes b-hCG levels to be decreased?
- Nonviable pregnancy
- Ectopic pregnancy
What is part of a first trimester visit for a pregnancy patient?
- Pap smear (abnormal cells/HPV)
- CBC (Baseline, signs of infxn or anemia)
- UA (Bacteremia)
- Type and Screen (Rh compatibility)
- Rubella (Seronegative = vaccinate after birth)
- Syphilis (State mandated)
- Hepatitis B (can vaccinate during pregnancy, infant recieves prior to discharge home)
- Tdap (can give vaccine betwen 27-28 weeks)
- HIV
- GC/Chlamydia
- TB - if high risk
- DM and Thyroid in select population
What is TORCH screening for?
Toxoplasmosis
Other (e.g., syphillis, varicella-zoster virus)
Rubella
Cytomegalovirus
Herpes simplex virus (HPV)
Why do we screen for TORCH diseases?
To detect infections that can harm the fetus, potentially leading to birth defects, growth delays, and brain/nervous system problems
Where is group B strep naturally colonized?
Between vagina and rectum
Why is the colonization of group B strep between the vagina and rectum harmful during birth?
Can pass to the fetus during delivery, causing complications such as meningitis, pneumonia, sepsis, and RDS
When should we culture for group B strep, and what should we do if it is positive?
Between 36-38 weeks of pregnancy
Begin IV penicillin at the start of labor (very important it is NOT before!!)
When is genetic counseling indicated?
- Advanced maternal age
- Previous child or family hx of birth defects/mental retardation
- Multiple fetal losses
- Previous baby who died in neonatal period
- Exposure to teratogenic material
- Abnormal U/S finding
- Parent who is a known carrier of genetic disorder
What are the most common chromosomal abnormalities screened for in genetic counseling?
- Sex aneuploidies (Turner, Klinefelter, Robertsonian, translocation)
- Autosomal trisomies (Downs)
What are examples of some autosomal recessive diseases?
- Sickle cell
- Cystic fibrosis
- Tay-sachs disease
- Thalassemia
If the maternal screening tests are positive, then more accurate diagnostic tests are needed such as:
- Chorionic villus sampling (CVS)
- Amniocentesis
What is an amniocentesis?
Amniotic fluid analysis
When should an amniocentesis be done?
- Advanced maternal age with suspected genetic abnormalities (14-16 weeks, the earlier than this the higher the risk)
- Fetal maturity (35 weeks)
What are some complications of amniocentesis?
- 1%: post procedure amniotic fluid leak
- 0.3%: pregnancy loss rate
- Rh isoimmunization (must give RhoGAM to Rh- mother)
What is used to evaluate fetal maturity status in an amniocentesis?
- Lecithin/splingomyclin (L/S) ratio (>2:1 = mature; Decreased = immature lungs, RDS)
- Phosphatidyloglycerol (PG) (+ = mature)
- Lamellar body count (>30,000/mL = mature)
- Surfactant activity (Foam when fluid is shaken in alcohol, bubbles = mature)
- Optical density (Denser = more mature, rapid screening test)
What is lecithin and when is it increased?
Constituent of surfactant; PG produced by mature alveloa (less accurate but if present high indication of lung maturity)
Increases at 35 weeks
What can amniocentesis detect?
- Sex of the fetus
- Genetic and chromosomal irregularities
- Rh isoimmunization (assess level of bilirubin pigmentation in fluid, indicates hemolysis)
- Hereditary metabolic disorders (i.e., CF)
- Anatomic abnormalities (AFP; high = neural tube defects, low = trisomy)
- Fetal distress (meconium staining)
- Culture and sensititvity (bacteria/virus in chorioamnionitis)
- Premature rupture of membranes (dye is injected into aminotic fluid and if it found in vaginal fluid, it indicates rupture of waters)
- Paternity testing
- Therapeutic (polyhydramnios, twin-twin transfusion testing)
What has fetal distress aminocentesis been replaced with?
Biophysical profile
What has premature rupture of the membrances amniocentesis testing been replaced with?
Nitrazine test strip
What is chorionic villus sampling (CVS)?
- Test fetal cells from villi of placenta for prenatal genetic diagnosis that can be preformed earlier than amniocentesis
- Fetal loss <1%
- Take only 3 days for results
What can amniocentesis test for that chorionic villus sampling cannot?
AFP
What are the indications for chorionic villus sampling?
- Advanced maternal age
- Frequent spontaneous abortions
- Previous fetus/infant with genetic abnormalities
- Personal genetic defect
What is fetal nuchal translucency?
Echo free area at the back of the fetal neck, visualized via U/S and used for screening only
What does increased fluid in testing of fetal nuchal transluency mean?
Genetic or chromosomal abnormalities
When is fetal nuchal translucency performed?
Between 10-14 weeks (often at time of anatomy scan)
Typically combined in 1st trimester with maternal age, b-hCG, and plasma protein A
When is alpha-fetoprotein (AFP) detected in mother's blood?
When fetus has neural tube defect or ventral wall defects
What should be ordered if AFP is elevated?
U/S to rule out possible cause for false positives (multiple gestation, fetal demise, inaccurate gestational age)
What should be ordered if AFP is elevated and US is normal?
Amniocentesis to test amniotic fluid AFP and acetylcholinesterase (AChE only present in neural tube defects)
What could low AFP indicate?
Downs syndrome
What is the triple screen for downs syndrome and what is its percent indication?
Low AFP, elevated hCG, low unconjugated estradiol (UE3)
70%
What is the quad screen for downs syndrome and what is its percent indication?
Low AFP, elevated hCG, low unconjugated estradiol (UE3), and increased inhibin A
81%
What is non-invasive prenatal testing (NIPT)/cell-free fetal DNA testing (ffDNA)?
Maternal serum is taken and can detect fetal DNA as early as 9-10 weeks gestation
What does non-invasive prenatal testing (NIPT)/cell-free fetal DNA testing (ffDNA) test for?
>99% detection of trimsomy 21 and 18 and >96% sex chromosome abnormalities, can also detect hemophilia and muscle dystrophy
What should be done if non-invasive prenatal testing (NIPT)/cell-free fetal DNA testing (ffDNA) is positive?
Chorionic villus testing or amniocentesis to rule out false positive (happens in 1% of cases)
What was mandated for newborn testing in 1964?
Phenylketonuria (PKU)
What does NJ require to be screened for newborns today?
- 61 disorders with continued growth of list expected
- All babies born in New Jersey are required to be tested for sixty-one (61) disorders within 48 hours of birth
- One heel prick provides enough blood to test for all sixty-one disorders
What is phenylketonuria (PKU)?
- Rare disorder that prevents the body from breaking down part of a protein called phenylalanine (Phe)
- If you have PKU and eat foods with Phe, the Phe will build up in your blood. If the level gets too high, it can permanently damage your nervous system and brain resulting in seizures, delayed development, psychiatric disorders
How long does it take to get results for PKU and what are the normal ranges?
- Results in 3 days
- Normal Results: Phe level less than 2 mg/dL
- Abnormal Results: RPhe level greater than 4 mg/dL
What is galactosemia?
Inherited condition that prevents the body from breaking down galactose, which is found in milk, cheese, yogurt, etc.
Whar are the signs and symptoms for galactosemia?
Vary
Jaundice, Vomiting, Diarrhea, Failure to thrive, Liver damage, Kidney problems, Cataracts, and Intellectual disability
How long do results take for galactosemia and what are the normal and abnormal results?
- Results in 24 hours
- Results either positive or negative
Normal level of erythrocyte galactose-1-phosphate is <1 mg/dL
Any detection higher than 1mg/dL will results in a positive test
What can happen with the thyroid at birth that is screened for?
Hypothyroidism
Thyroid gland may be completely absent, or it may be too small or in the wrong place. In some cases, the thyroid may be normal-sized or even large. In all types of congenital hypothyroidism, the thyroid does not make enough of certain hormones that the body needs.
What are the signs and symptoms of undiagnosed congenital hypothyroidism?
Slow growth, hypotonia, increased sleep, difficulty feeding, constipation, jaundice
What are the postive results for hypothyroidism?
Low or normal levels of T4 with high levels of TSH
What is sickle cell anemia?
Inherited disorder causing abnormal shape (sickle) of blood cells
What are the signs and symptoms of sickle cell anemia?
- Acute chest syndrome
- Anemia
- Hand-foot swelling/pain
- Infection
- Splenic episodes
- Pain
- Stroke
What are some abnormal findings for sickle cell anemia?
- Presence of Hemoglobin S = positive for trait
- Presence of abnormal shaped blood cells = positive for disease
What is thalassemia?
Mutations in the DNA of cells that make hemoglobin, cannot carry oxygen throughout your body correctly
Results in low Hgb/Hct, MCV and MCH
What is alpha thalassemia (Hydrops Fetalis)?
- 4 mutated genes
- Rare
- Stillborn, die shortly after birth
- Rarely saved with transfusion and stem cell transplant
- Hgb Barts (tetrameter of gamma globin chains that appears in the blood in the newborn period) = positive
What is beta thalassemia?
- 2 mutated genes
- Asymptomatic at birth, develop symptoms 1-2 years of life
- High levels of fetal hemoglobin (HbF) and low levels of adult hemoglobin (HbA) = positive