PSIO 201: Exam 2
1/77
Earn XP
Description and Tags
Lectures 2.1-2.9
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
78 Terms
What does the skeletal system contain?
Bone, Cartilage, Ligaments, and other connective tissues
What does bone contain?
Blood CT
Blood vessels and nerves
Lymphatic vessels
Cartilage CT
CT coverings
What are the 6 functions of the skeletal system?
1.) Support
2.) Protection
3.) Leverage (assistance in movement)
4.) Mineral homeostasis (homeostasis of Ca)
5.) Triglyceride storage (in yellow bone marrow)
6.) Hemopoiesis (red and white blood cell formation, in red marrow)
What are the 6 classification of bones?
Give examples.
1.) Long bones (humerus)
2.) Short bones (carpals)
3.) Flat bones (sternum, ribs)
4.) Irregular bones (vertebrae)
5.) Sesamoid bones (patella)
6.) Sutural (cranial bones)
*7.) Pneumatized bones (shock absorption, hollow)
What are the endosteum and periosteum important for?
Bone growth and remodeling
What is the periosteum?
Covers outer surface of bone
Continuous with tendons and CT of joints
Attached to bone matrix via perforating fibers
2 layers: Outer fibrous and Inner osteogenic layer
What is the endosteum?
Coats inner surface of bone (marrow cavity, trabeculae of spongy bone, and canals of compact bone)
Contains osteogenic cells
What is the anatomy of a short bone?
Spongy bone located inside, compact bone located outside
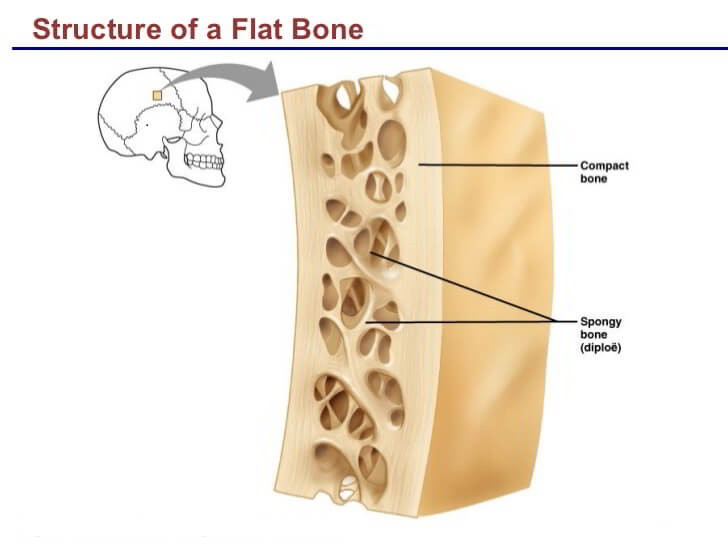
What is the anatomy of a flat bone?
Contains compact bone, spongy bone, periosteum, and endosteum
What are osteogenic cells?
Bone stem cells
Formed from mesenchyme (embryonic CT)
Differentiate into osteoblasts
Found in periosteum and endosteum
Only one daughter cells of osteogenic cells will differentiate into osteoblasts
What are osteoblasts?
Cells that build bone (bone formation)
Synthesize organic components (collagen fibers) of matrix
Initiate calcification: take calcium from blood and deposit it within matrix by exocytosis (starts process by hardening bones)
Immature bone cells
What are osteocytes?
Mature bone cells
Involved in maintenance of bone tissue
Sense bone micro damage and mechanical forces on bone, send signals needed for repair
What are osteoclasts?
Break down bone for bone resorption (remove bone in order to repair)
Release proteolytic enzymes and acids to degrade collagen and release minerals to blood
Derived from myeloid stem cells (not from osteogenic cells)
What is the Sealing Zone of osteoclasts?
Special proteins that bind osteoclasts to the bone
What is the Ruffled Border of an osteoclast?
Proton pumps that can release proteolytic enzymes and acid (allows for secretion)
Side that is in contact with bone
What is the goal of bone remodeling?
1.) To achieve strength for loading (support any stress bone encounters)
2.) Lightness for mobility (keep bone light)
Happens through strategically depositing bone where it is needed for strength, and removing bone where it is not to avoid bulk.
-Achieve skeleton’s peak strength during growth
-Maintain bone strength by removing damaged bone during adulthood
What is bone able to do?
1.) Detect location and magnitude of damage (osteocyte)
2.) Remove damage (osteoclast)
3.) Replace it with new bone (osteoblasts)
4.) Restore bone’s material composition, microarchitecture, and macro architecture
What are the organic components of Bone ECM?
1.) Ground Substance: glycosaminoglycans (GAG)
Glycoproteins (polysaccharide + protein)
GAGs are negatively charged (trap water)
Examples: Chondroitin sulfate, hyaluronic acid
2.) Collagen fibers: fibrous protein arranged in a helical form (Type I Collagen)
Very resistant to pulling forces
Provides flexibility and a framework for deposition of calcium
What are the inorganic components of Bone ECM?
1.) Water:
Attracted to ground substance
Makes up 25% of ECM
2.) Hydroxyapatite:
Forms mineral plates that fill up spaces within collagen fibers
What does collagen do for bone?
Provide flexibility
Apply proteolytic enzymes (denature protein), removes collagen from bone, and bone become brittle/ crumbly
What do minerals do for bone?
Provides firmness
Soak bone in vinegar, remove minerals from bone, bone becomes rubbery/ flexible
What is rickets?
Inorganic component deficiency
Calcium deficiency due to lack of Vitamin D (allows gut to absorb calcium from diet)
Leads to flexible bones (bowed legs)
What is scurvy?
Organic component deficiency
Problem with collagen synthesis due to Vitamin C deficiency
Leads to brittle bones that can fracture easily
What is spongy bone?
Location: Epiphyses of long bones, surrounding marrow cavities, flat, short, and irregular bones
Functions: Withstands forced from many directions, trabeculae arranged along lines of stress, lightense the skeleton, contains red marrow for hemopoiesis, irregular lattice of thin plates called trabeculae
What is compact bone?
Organization: Solid network of bone organized in concentric ring structure called osteons.
Location: External layer of all bones, diaphysis of long bones
Function: Gives long bones ability to withstand forced along longitudinal axis (can only withstand in certain direction)
Where is the bone of an infant particularly soft (bone formation incomplete)?
Fontanels (soft spots on skull)
Epiphyses of long bones (made of cartilage in infants)
Epiphyseal (growth) plates (stays as cartilage until end of puberty)
What are the bones of a fetus composed of?
Loose CT: Mesenchyme
Hyaline cartilage
What is ossification?
The replacement of connective tissue by bone
Begins during the second month of development
Continues for many years after birth
What are the two types of ossification?
Intramembranous ossification: “Within membrane”
Mesenchyme (starting tissue) to bone
Endochondral ossification: “Inside cartilage”
Mesenchyme to cartilage to bone (cartilage intermediate)
What bones are formed by intramembranous ossification?
1.) Cranial bones (frontal, parietal, occipital, temporal, sphenoid, ethmoid)
2.) Most facial bones
3.) Sternum
4.) Clavicle
All the REST are ENDOCHONDRAL OSSIFICATION
What is heterotropic bone formation?
Happens with sesamoid bones (forms within ligaments/ tendons to give more support to join)
Abnormal stresses can stimulate bone formation in areas where bone is not normally found
What are the steps of intramembranous ossification?
1.) Development of ossification center
Mesenchymal cells differentiate into osteogenic cells then osteoblasts
Osteoblasts secrete bone matrix
2.) Calcification
Osteoblasts deposit calcium into the matrix
Osteoblasts differentiate into osteocytes
3.) Formation of trabeculae (spongy bone)
4.) Development of periosteum
Remodeling of spongy bone to compact bone
What is calcification?
The deposition of calcium into matrix
Important step in ossification but NOT ossification
What are the steps of endochondral ossification?
1.) Development of cartilage model
2.) Growth of cartilage model
3.) Osteoblasts create a primary ossification center (bone replaces cartilage)
Blood vessels penetrate model and stimulate differentiation of osteogenic cells into osteoblasts
Osteoblasts form bone on the outer surface of the model
4.) Osteoclasts create a marrow cavity
Spongy bone is remodeled into compact bone
5.) Around birth, secondary ossification center form in epiphyses.
6.) Spongy replaces most of the cartilage at the epiphyses (except for the epiphyseal plate and articular cartilage)
What 2 processes happen at the epiphyseal plate?
1.) Interstitial growth of cartilage (hyaline cartilage must grow for bone to grow)
2.) Endochondral ossification
What is the interstitial growth of cartilage?
Cartilage growing from within at the epiphyseal side of the epiphyseal plate (grows at side closet to epiphysis)
What are the steps of the interstitial growth of cartilage?
1.) Mesenchymal cells differentiate into chondroblasts
2.) Chondroblasts build matrix and differentiate into chondrocytes
3.) Chondrocytes divide and spread apart (mitosis)
4.) Cartilage tissue grows from within
When does the epiphyseal plate close?
At the end of adolescence (18 for women, and 21 for men)
Epiphyseal cartilage cells stop dividing and are replaced by bone
Epiphyseal line forms
Interstitial growth cannot occur after the epiphyseal plate closes
What is appositional growth and what does it generate?
Growth in width
Periosteal osteogenic cells differentiate into osteoblasts
Periosteal osteoblasts build bone on outer surface of bone
Endosteal osteoclasts increase the diameter of the marrow cavity
Bone diameter, cortical width, and medullary cavity size increases.
Appositional growth generates new osteons.
How are osteons added to the periosteal side of the bone?
1.) Ridges in periosteum create groove for periosteal blood vessel.
2.) Periosteal ridges fuse, forming an endosteum-lined tunnel.
3.) Osteoblasts in endosteum build new concentric lamellae inward toward center of tunnel, forming new osteon.
4.) Bone grows outward as osteoblasts in periosteum build new circumferential lamallae. Osteon formation repeats as new periosteal ridges fold over blood vessels.
What is acting together in Appositional Growth?
Osteoblasts and osteoclasts woking together in medullary cavity.
Osteoclasts acting first, osteoblasts going in to build bone
What is a fracture?
A break in the continuity of bone rendering it structurally incompetent.
What are the classification of fractures?
1.) Traumatic: normal bone experiencing abnormal force (i.e car accident)
2.) Pathologic: abnormal bone experiencing normal forces (i.e. results from having a disease).
What are the steps of fracture repair?
1.) Formation of fracture hematoma (about 6 to 8 hours)
Nearby bone cells die which leads to swelling and inflammation.
Phagocytes and osteoclasts remove damaged tissue (3 to 4 weeks)
2a.) Fibrocartilage callus formation (3 weeks)
Blood vessels grow into hematoma
Mesenchymal cells in periosteum differentiate into fibroblasts, chondroblasts and osteogenic cells
Chondroblasts produce fibrocartilage; fibroblasts produce collagen
2b.) Bony callus formation (endochondral ossification; 3-4 months)
Osteogenic cells differentiate into osteoblasts
Osteoblasts produce spongy bone
3.) Bone remodeling (up to 6 to 9 months)
What are the treatments for bone fractures?
Immobilization: prevent movement using a splint, cast, or brace
Reduction: repositioning bones (followed by immobilization)
Closed reduction: the manipulation of bones without surgery
Open reduction: the surgical use of rods, plates, pins, etc. to position bones and bone fragments correctly for proper bone healing
What are the 3 factors that influence bone?
1.) Dietary
2.) Hormones
3.) Exercise
What are the minerals that influence bone?
Calcium and phosphorus
( also magnesium, fluoride, and manganese)
What are the vitamins that influence bone?
Vitamin A: stimulate activity of osteoblasts
Vitamin C: needed for collagen synthesis
Vitamin D: Stimulates calcium absorption in GI tract
Vitamin K, B12: needed for synthesis of bone proteins
Why is calcium homeostasis important?
1.) Membrane excitability: action potential relies on calcium concentration
2.) Blood clotting: need to properly clot in response to injury
3.) Intracellular activity: carry signals as a part of cascade
How is the blood calcium level regulated?
Control calcium entry into and exit from blood:
1.) Bone storage
2.) Kidney excretion: getting rid of calcium in urine (dec. of calcium of urine, inc. blood calcium level, inc. calcium of urine, dec. blood calcium level)
3.) Intestinal absorption
Which hormones influence bone and are involved in calcium homeostasis?
Calcitriol (Active form of Vitamin D)
Calcitonin
Parathyroid Hormone (PTH)
Travel through blood and have effects on different target tissues (hormones are signaling molecules with receptor molecules)
How much calcium do you need per day?
1000 mg of calcium per day
Which hormones that influence bone act on osteoclasts?
Calcitonin and Parathyroid hormones
Which hormones that influence bone act on osteoblasts?
Growth hormones and estrogen/ testosterone (sex hormones)
What does growth hormone (somatotropin) do?
Simulates cell growth and protein synthesis (collagen)
Stimulates secretion of insulin-like growth factors (IGFs) then stimulates osteoblast activity then stimulates bone formation
Example: HGH
What are the skeletal disorders associated with growth hormones?
1.) Pituitary dwarfism: children with low levels of GH results in slow epiphyseal growth (short stature)
Signals not being sent to actively grow
2.) Pituitary gigantism: hyper secretion of GH in childhood results in accelerated epiphyseal growth (tall stature)
Too much growth hormone being secreted while epiphyseal plate is still open
*Both happening before puberty
3.) Acromegaly: hyper secretion of GH after puberty results in appositional growth (thickening of bones) in the skull, hands, and feet as well as overgrowth of cartilage
Epiphyseal plates of long bones already closed
What do estrogen and testosterone do?
Both stimulate osteoblast activity (bone formation)
Levels increase at puberty
Bone growth/ growth spurts (surge in estrogen/ testosterone increase massively)
Eventually cause closure of the epiphyseal plates because osteoblast/ osteoclast activity is slightly greater than chondrocyte activity
Levels decrease with older age
What are the effects of the exercise of exercise on bone?
Bone will change in response to the stresses it encounters:
1.) Muscle pulling on bone results in joint reaction forces
2.) Impact results in ground reaction forces
Sir Isaac Newton: “For every force, there is an equal and opposite force”.
What is spongy bone like compared to compact bone?
More metabolically active: can respond to changes in mechanical loading more readily
Where are the sites of fracture mostly located and what do they all have in common?
Hip, wrist, and spine
All have high spongy bone content
What is the goal of exercise and what are its roles?
Goal: reach the fracture threshold later in life
1.) Exercise early in life- increase peak bone mass
2.) Exercise later in life- prevent bone loss
3.) Fall prevention- exercise promotes better balance and coordination
Improved strength
Improved balance and coordination
Why do astronauts need to exercise in space?
Osteoclasts act more because osteocytes are not sensing stress in microgravity (bone still needs to be remodeled)
Astronauts exercise for at least 2 hours each day in space to prevent bone and muscle loss (loose average of 1-2% of their BMD each month)
What happens when you exercise?
Force applied to bone is sensed by osteocytes then proliferation of osteocytes begins, bone formation is greater than bone resorption in response to exercise.
What is osteoporosis?
Porous bones (reduced bone mass), increase risk of fractures
The proportion of collagen and minerals is normal but there is a decrease in mass
Osteoclasts more active than osteoblasts
Silent disease: no symptoms unless a fracture occurs, cannot diagnose using blood tests
What causes reduced bone mass?
Any factor that stimulates bone resorption or inhibits bone formation (or both)
Osteoclast activity > osteoblast activity
What is osteomalacia?
Decreased mineralization of newly formed bone matrix at sites of bone remodeling as a consequence of Ca2+ deficiency (due to Vitamin D deficiency) associated with achy bone pain
What is osteogenesis imperfecta?
Congenital disorder that affects production of Type I collagen due to genetic mutation
Brittle bones that fracture easily, often in childhood or adolescence
Pain associated with fracture
What is an articulation?
A point of contact between:
1.) Bones (elbow)
2.) Bones and cartilage (epiphyseal plates)
3.) Bones and teeth
What is arthrology?
The study of joints
What is kinesiology?
the study of body motion
The more stable a joint is ….
The less mobility it affords the body
The less stable a joint is ….
The more mobility it affords the body
What are the two types of arthritis caused by synovial joints?
Osteoarthritis: degenerative
“Wear and tear” arthritis (one joint affected on one side of the body)
Rheumatoid arthritis: inflammatory
Body attacks Type 2 collagen (sees it as foreign), causes inflammation and pain on both sides
What kind of joint is the shoulder?
Diarthrosis- freely movable
Ball and socket joint
Tri-axial joint (more prone to injury)
What kind of joint is the knee?
Diarthrosis- freely movable
Hinge joint
Mono-axial joint
Medial and lateral menisci cushion the joint
How many ligaments stabilize the knee joint?
7: 2 intracapsular ligaments, 5 extracapsular ligaments
What are the 5 extracapsular ligaments?
1.) Fibular Collateral ligament: stabilizes lateral side of knee
2.) Tibial Collateral ligament: stabilizes medial capsular of ligametns
3.) Patellar ligament: stabilizes anterior side of knee
4.) Oblique Popliteal ligament: stabilize popliteal side of ligament
5.) Arcuate Popliteal ligament: stabilizes popliteal side of ligament
What are the 2 intracapsular ligaments?
1.) Anterior cruciate ligament: prevents anterior sliding of tibia on femur
2.) Posterior cruciate ligament: prevents posterior sliding on tibia and femur