GP multifocals
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
what are the designs of simultaneous GP MF lenses (2)
concentric or aspheric
concentric - mainly CD
aspheric - front or back surfaces - can be CD/CN
what are the advantages of simultaneous lenses (8)
◦Minimal gaze dependence - px can read in every POG not only when looking down
◦PPL effect - allows for intermediate vision - comfy for computer users
◦Comfort equal to single vision GP CLs
◦3-4 mm pupils or greater are more suitable
◦Early to mid-presbyopes (adds 1.00 to 2.50 D)
◦Normal stereopsis
◦No image jump - no line in the lens
Easier to fit than alternating GP CL designs
what are the disadvantages of simultaneous lenses (7)
◦Difficult to achieve high adds (>2.50 D) - depending on e value of the eye
◦Top up spectacles or modified monovision may be needed for these px therefore
◦Compromised VA with some contrast loss
◦Can be difficult to attain required centration
◦BS aspherics - majority of designs limited to this
◦spectacle blur in higher adds - can be induced
◦not available in back-surface toric designs
explain troubleshooting of a low riding position simultaneous CL (4)
Avoid steep fit - increase lens diameter
change edge design by adding a –ve carrier on high-plus CLs
Thickness control - ↓ bulk - to increase lid attachment
Avoid high WTR astigmatism (>2.50DCyl)
explain troubleshooting of a high riding position simultaneous CL (5)
Ensure fit not too flat
Avoid excessive lid attachment - optimise thickness
↓ lens diameter (TD) - if narrow palpebral aperture
Avoid WTR >2.50 D
Consider different lens design or prism ballast - to maintain centration of lens
explain troubleshooting of a laterally decenterd simultaneous CL (2)
◦Avoid moderate ATR astig (>1.50 DCyl)
◦ increase lens diameter - TD
explain what to do in the case of a px having good centration but poor distance vision (4)
◦Over-refract & give minimum extra minus
◦↓ add in dominant eye
◦Change lens in dominant eye to single vision (enhanced monovision)
◦increase zone over which add functions (concentric designs/or by width) - only if patient has large pupils (>5 mm)
explain what to do in the case of a px having good centration but poor near vision (3)
•Increase the add in dominant eye
•Over-refract &, if required add is >1.75 in total, work onto front surface of CL on non-dominant eye
•↓ zone over which add functions (concentric designs) - only if patient has small pupils (<3 mm)
what are the 2 designs of translating GP lenses (3)
long line segment - tangent streak - achieved by truncation and prism ballast

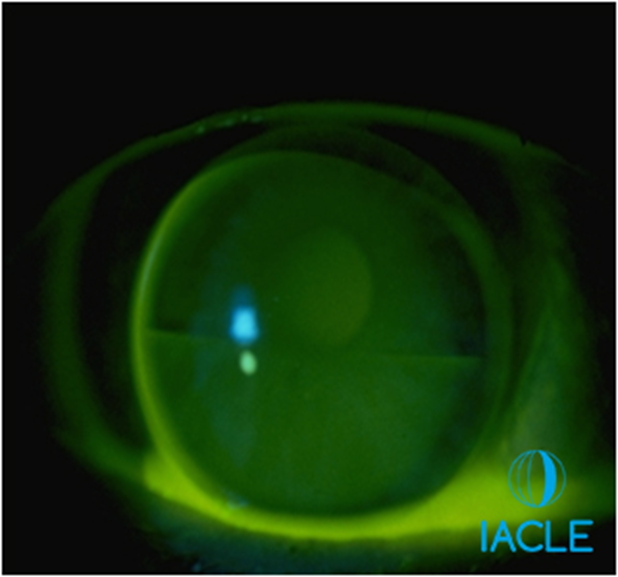
triangle shaped segment - presbylite - NO truncation, achieved by prism ballast

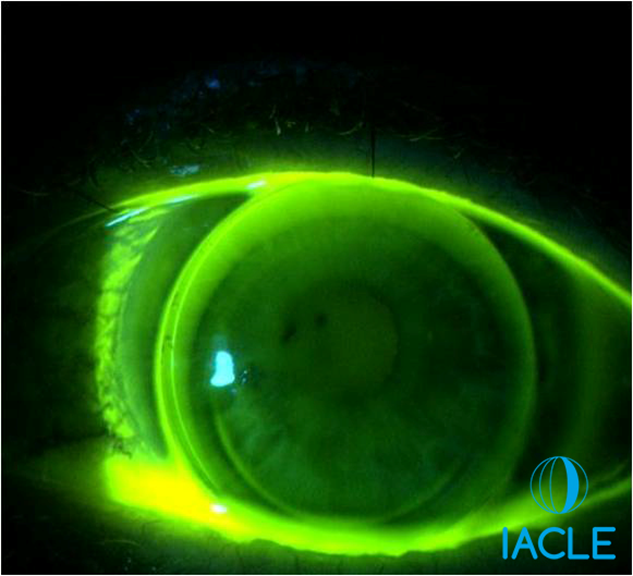
both are available with toric BS
what are the advantages of translating GP bifocal lenses (4)
◦Excellent VA distance & near - as segments specific for distance/near
◦Normal stereopsis
◦Good contrast
◦Custom CLs offer: wide parameter range / choice of materials / high adds available
what are the disadvantages of translating GP bifocal lenses (3)
◦Stabilisation necessary (prism ballast/truncated) - so reading portion is in line with where it needs to be
◦Require to be ‘very’ mobile on eye - not very comfortable
◦Bifocal (unless made into trifocal) - gaze-dependent (can’t read in every POG) and intermediate vision poor/lacking
when fitting translating GP CLs what are we looking for (5)
Inferior centration / rapid post-blink recovery - Prism Ballast / thin upper edge
Segment line - on inferior pupil margin – covering 20% max
Small pupils best to avoid flare
Minimum 2 mm translation - lower lid support - truncation where required - avoid truncation if possible due to comfort – irregular edge of lens interferes with comfort on lower lid
Keep prism as low as possible - for binocular vision and comfort – due to thickness in inferior lid margin
explain how we assess the rotation of translating GP lenses (3)
If marks rotate inwards (nasal) - if < 30 o – OK – as when we read eyes come together nasally
if ≥ 30 o – Compensate
Rotate temporal compensate - be wary of making very large compensations
how do we assess the fit of the segment on the eye (5)
via ophthalmoscopy - see red reflex - ask patient to blink
Check speed of return if < 1 sec, perfect / if > 1 sec, improve fit
improve fit by - making BC steeper / flatter – depending if too much movement/too tight - if too tight FLATTEN BC / if too much movement - STEEPEN BC - flattening is inc BC and steepening is decreasing BC
if segment Position < 1/3 mm in pupil sector - proceed to over-refraction
if segment Position > 1/3 mm in pupil sector - ↓ lens diameter
how do we decide which px are better suited to simultaneous lenses (4)
◦Patients that require near vision in the straight ahead gaze
◦Can accommodate any reading position - doing a lot of lateral reading - not always looking down
◦Early to moderate presbyopes
◦Intermediate task demands - computer work, playing a musical instrument, sewing machine etc.
how do we decide which px are better suited to translating lenses (7)
◦Read in normal position (slightly inferior)
◦Require excellent distance vision
◦Patent with higher adds
◦Larger pupils and very small pupils - translating can bi sect any pupil size whereas in simultaneous it is pupil dependent - cannot fit v. large/small - would miss out on some portion of reading addition
◦Lower lid within 1mm of the limbus - ectropion, entropion
◦Fair sized palpebral aperture
-require a sclera that is flatter than cornea - or lens would not be able to translate