Lipid Lowering Drugs
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
How are lipids transported in the body?
Lipids are transported in the blood packaged inside lipoproteins (like chylomicrons, LDL, and HDL), which carry fats and cholesterol through the bloodstream.
What is the relationship between triglycerides/proteins and density?
The higher the fat content the lower the density
The higher the protein content the higher the density
What is the least dense lipoprotein? What is the most dense lipoprotein?
Chylomicrons is the least dense because it has the most fat and HDL is the most dense because it has the highest amount of protein
Rank the order of the 6 lipoproteins in accordance to density from lowest to highest
(IDL,LDL,HDL, VLDL, CM, and free fatty acid albumin complex)
1. CM
2. VLDL
3. IDL
4. LDL
5. HDL
6. Free fatty acid albumin complex
Is cholesterol essential?
yes
What is cholesterol a precursor for?
bile acids and steroid hormones
Total cholesterol is defined as
combination of all cholesterol in the body = VLDL, LDL, HLD
Atherosclerosis is a primary cause of premature death in the US. Define atherosclerosis.
Atherosclerosis is a condition in which fatty plaques made of cholesterol build up inside artery walls, narrowing them and reducing blood flow.
How are triglycerides stored in the body? Triglycerides are hydrolyzed to generate what?
Triglycerides are stored in fat cells throughout the body and carried in the blood. Triglycerides are hydrolyzed to generate free fatty acids.
What are some causes of high triglycerides in the general population?
overweight
physical inactivity
smoking
excess alcohol intake
high carb diet
drugs like steroids, protease inhibitors, estrogen
genetic factors
What triglyceride score puts someone at high risk for metabolic syndrome?
150
A clinical diagnosis of metabolic syndrome requires more than __ of the following risk factors:
3
abdomen obesity, TGs 150+, reduced HDL, hypertension 130-85, impaired fasting glucose
When there is a prescence of a artherosclerotic lesion what cells are recuirted to the injured endothelium? What do these cells become and why?
macrophages are recruited to the site of injured endothelium and become foam cells because they will engulf lipids (making them look foamy) and eventually die and become part of the plaque
hat is the exogenous lipoprotein pathway?
It is the pathway that transports dietary lipids from the intestine to tissues and the liver.
Where are chylomicrons formed and what do they carry?
They are formed in intestinal mucosal cells and carry dietary triglycerides and cholesterol.
How do chylomicrons enter the bloodstream?
Through the intestinal lymphatic system before reaching circulation.
What are chylomicron remnants? What happens to chylomicron remnants?
Particles depleted of triglycerides but enriched in cholesterol. They are taken up by the liver via LDL receptor-related proteins and metabolized.
What is the endogenous lipoprotein pathway? Where does the endogenous pathway begin?
The endogenous pathway transports lipids made by the liver to tissues. Begins with VLDL synthesis in the ER of hepatocytes.
What happens to VLDL after it is made?
It is secreted by the liver into circulation.
What does lipoprotein lipase (LPL) do to VLDL?
It removes triglycerides, converting VLDL into IDL.
What are the two fates of IDL?
Taken up by the liver (via LDL receptor-related protein)
Converted into LDL by hepatic lipase
What is the most commonly prescribed lipid lowering drug?
statins
Statins are ineffective in patients with what defect?
familial hypercholesterolemia or homozygous for a defective LDL receptor gene
What is the mechanism of action of statins?
They competitively inhibit HMG-CoA reductase, the rate-limiting enzyme in cholesterol synthesis
What is the main effect of statins on cholesterol?
They lower LDL cholesterol.
What other lipid effects do statins have?
They decrease triglycerides and may increase HDL.
Where are statins metabolized?
In the liver, and some metabolites remain active.
How are statins excreted?
Mainly through bile and feces, with some urinary excretion.
Overall effect of statins on lipids?
↓ LDL (main effect), ↓ VLDL, ↓ triglycerides, ↑ (slight) HDL
chat explained:
🧠 Statin Story (Never forget this)
Imagine your liver is a cholesterol factory 🏭
💊 Statins shut down the factory machine → (HMG-CoA reductase is blocked) → Liver can't make cholesterol
😱 Liver panics:
"I don't have enough cholesterol!!"
🚪 So it puts out more "LDL catcher doors" (LDL receptors) → to grab cholesterol from the blood
🧹 Blood gets cleaned: → LDL gets sucked out of circulation → LDL ↓↓↓
📉 Also: → Liver sends out less VLDL (less fat leaving)
What are the two major serious adverse effects of statins?
Hepatotoxicity and myopathy/rhabdomyolysis.
What is rhabdomyolysis and why is it dangerous?
Breakdown of muscle → releases contents that can cause kidney failure.
What common (less serious) side effects can statins cause?
GI upset (nausea, diarrhea, constipation), headache, insomnia, blurred vision.
When are statins contraindicated?
pregnancy
Which generation of fibrates is not on the market?
1st generation
name 2 second generation fibrate drugs
gemfibrozil (Lopid)
fenofibrate (tricor, lofibra, triglide)
name 3 omega-3 FAs
- docosahexaenoic and elcosapentaenoic acids (LOVAZA, various OTC preparations)
- vascepa
What is the mechanism of action of fibrates?
Fibrates activate PPAR-α, which:
↑ lipoprotein lipase → breaks down triglycerides (↓ VLDL)
↓ fat production in liver
↑ fat breakdown (β-oxidation)
↑ HDL
What are the pharmacokinetics of fibrates?
Oral drugs
Fenofibrate = prodrug → converted to active form
Undergo extensive metabolism
Excreted in urine (as glucuronides)
What is the mechanism and effect of niacin (nicotinic acid)?
Niacin inhibits fat breakdown in adipose tissue, so fewer fatty acids go to the liver → ↓ VLDL production → ↓ LDL, and ↑ HDL.
What are the pharmacokinetics of niacin?
Rapid oral absorption (peaks < 1 hr)
Short half-life (rapid kidney excretion)
Requires frequent dosing unless extended-release is used
What are the main disadvantages of niacin?
Flushing and GI distress (very common)
Can worsen hyperglycemia/insulin resistance
Extended-release helps side effects, but NOT flushing
What is the mechanism of bile acid sequestrants?
They bind bile acids in the intestine and prevent reabsorption and promote excretion, so the liver uses cholesterol to make more bile acids therefore decreasing LDL.
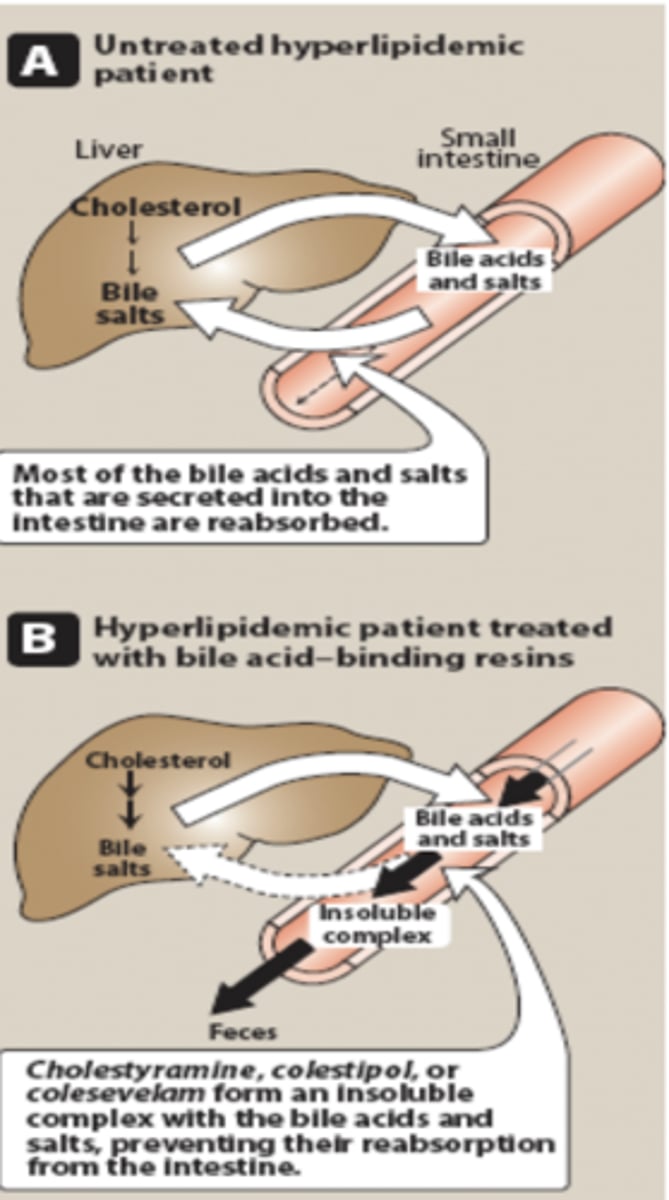
What are the effects of bile acid sequestrants on LDL and when are they ineffective?
They increase LDL receptors → increase LDL uptake → lower plasma LDL, but are ineffective in familial hypercholesterolemia (no functional LDL receptors).
What are the main side effects of bile acid sequestrants?
GI issues (constipation, bloating)
Bind other drugs → ↓ absorption
Can cause hyperchloremic acidosis
Bad taste → poor compliance
name 1 cholesterol absorption inhibitor
ezetimibe
What population of patients should not be treated with ezetimibe?
patients with moderate to severe hepatic insufficiency
What is ezetimibe commonly combined with?
simvastatin
(The combination of Statin with a bile acid-binding agent has been shown to be very useful in lowering LDL levels (there are risks though))
What do omega-3 fish oils do in lipid management?
Omega-3s (EPA, DHA) decrease triglycerides by reducing VLDL production, may increase HDL, and can be taken as diet or supplements.
Which type of lipoprotein is the largest particle of low density, and who's main function is to transport dietary lipids to tissues for use and storage?
A. LDLs
B. HDLs
C. Chylomicrons
D. IDLs
E. VLDLs
C. Chylomicrons
Which lipoprotein is considered a scavenger for cholesterol?
A. HDLs
B. LDLs
C. VLDLS
D. Chylomicrons
E. IDLs
B. LDLs
What is the function and location of lipoprotein lipase?
A. Transfer of cholesteryl esters from HDL to LDL and VLDL -
Plasma
B. Hydrolysis of triglycerides in HDL and IDL - Liver
C. Esterification of free cholesterol to cholesteryl esters -
Plasma
D. Conversion of LDL into HDL - Intestinal epithelium
E. Hydrolysis of triglyceride in chylomicrons and VLDL - capillary endothelium
E. Hydrolysis of triglyceride in chylomicrons and VLDL - capillary endothelium
What type of cells to macrophages become as they engulf
more and more cholesterol, becoming large and vacuolated?
A. Plasma Cells.
B. Neutrophils.
C. Super macrophages.
D. Foam Cells.
E. Hepatocytes
D. Foam Cells.
How do the Bile Acid-Binding Resins (Cholestyramine,
Colestipol, and Colesevelam) function?
A. By binding LDLs and removing them from circulation
B. By directly increasing HDL synthesis
C. By attacking the plaque directly
D. By binding bile acids
E. By inducing triglyceride metabolism
D. By binding bile acids
What type of individual would not benefit from the bile acid-binding resins?
A. Hemophiliacs
B. Patients suffering from gout
C. Patients genetically deficient in functional LDL receptors
D. Patients with a fever
E. Patients in renal failure
C. Patients genetically deficient in functional LDL receptors
Which drugs are competitive inhibitors of hepatic HMG CoA reductase, the rate-limiting enzyme in cholesterol biosynthesis?
A. Statins
B. Ezetimibe
C. Fibric acid derivatives
D. Bile acid-binding resins
E. Niacin
A. Statins
What drugs act as act as PPARalpha ligands ultimately resulting in increased lipases and therefore increased lipid degradation?
A. Statins
B. Ezetimibe
C. Fibric acid derivatives
D. Bile acid-binding resins
E. Niacin
C. Fibric acid derivatives
What drug class can have a side-effect of breakdown of
muscle proteins that leads to renal toxicity with symptoms that
include muscle pain and weakness and dark urine?
A. Statins
B. Ezetimibe
C. docosahexaenoic acid
D. Bile acid-binding resins
E. Fibric acid derivatives
A. Statins
Which lipid lowering drug acts by inhibiting the absorption of dietary cholesterol?
A. Colesevelam
B. Ezetimibe
C. Fenofibrate
D. Fluvastatin
E. Niacin
B. Ezetimibe
Which lipid lowering drug acts by inhibiting endogenous cholesterol synthesis?
D. Fluvastatin
The main function of chylomicrons is to do which of the following?
A. Transport endogenously synthesized lipids out of the liver
B. Transport dietary lipids from the intestine to target tissues
C. Transport cholesterol from HDL to LDL
D. Act as a receptor for triglycerides in the liver
E. Metabolize triglycerides to glycerol and fatty acids
B. Transport dietary lipids from the intestine to target tissues