Respiratory System
1/53
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
54 Terms
Conchae
Projection/Lobes
- Increased surface area
- Increased air turbulence
**Note: We want air here to be turbulent to maximize contact with mucous membrane
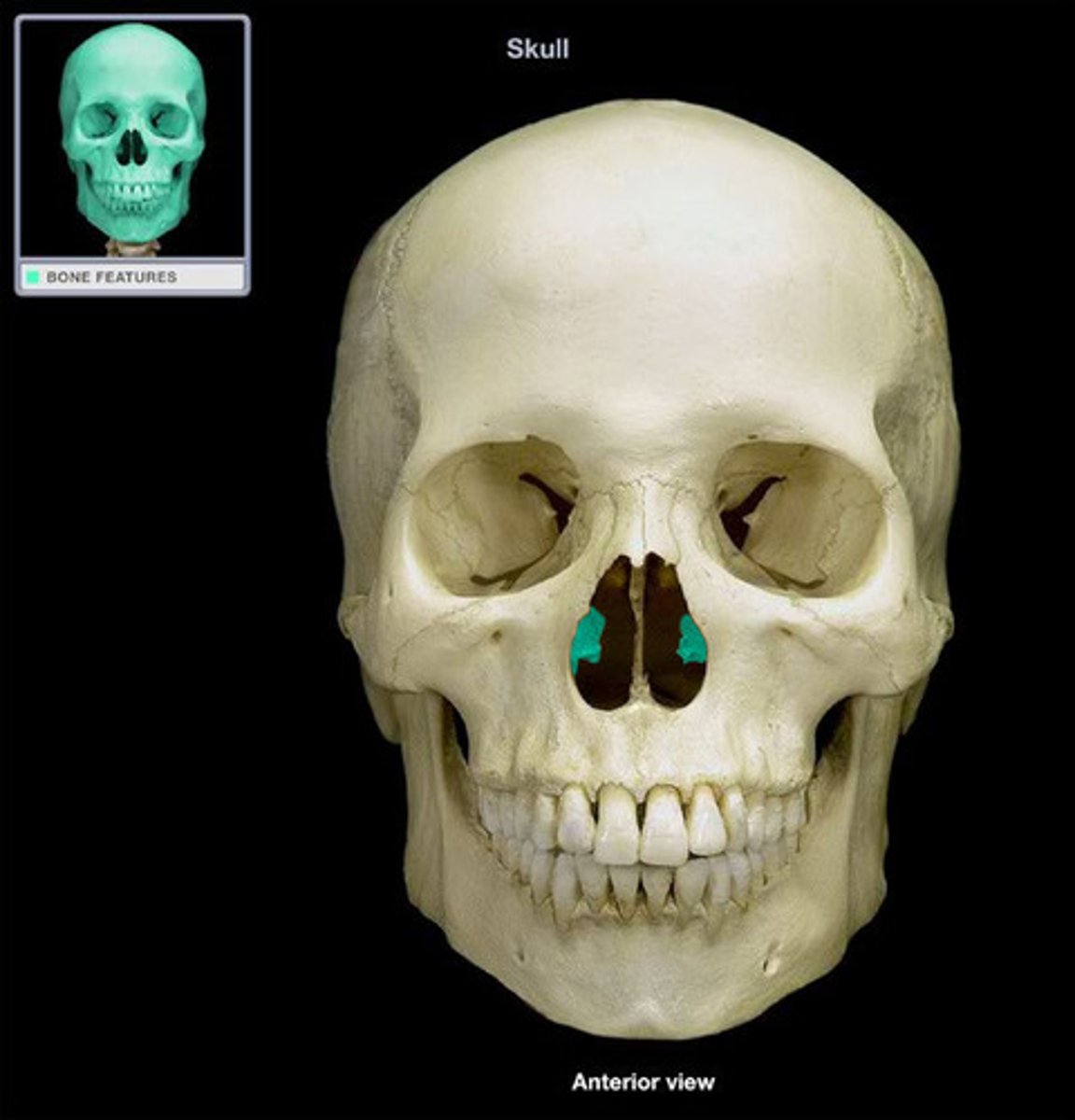
Respiratory Mucosa
Warms the inhaled air
- Superficial thin-walled veins
- Nosebleeds
Traps Foreign particles (ex. bacteria)
- Lysosome enzymes
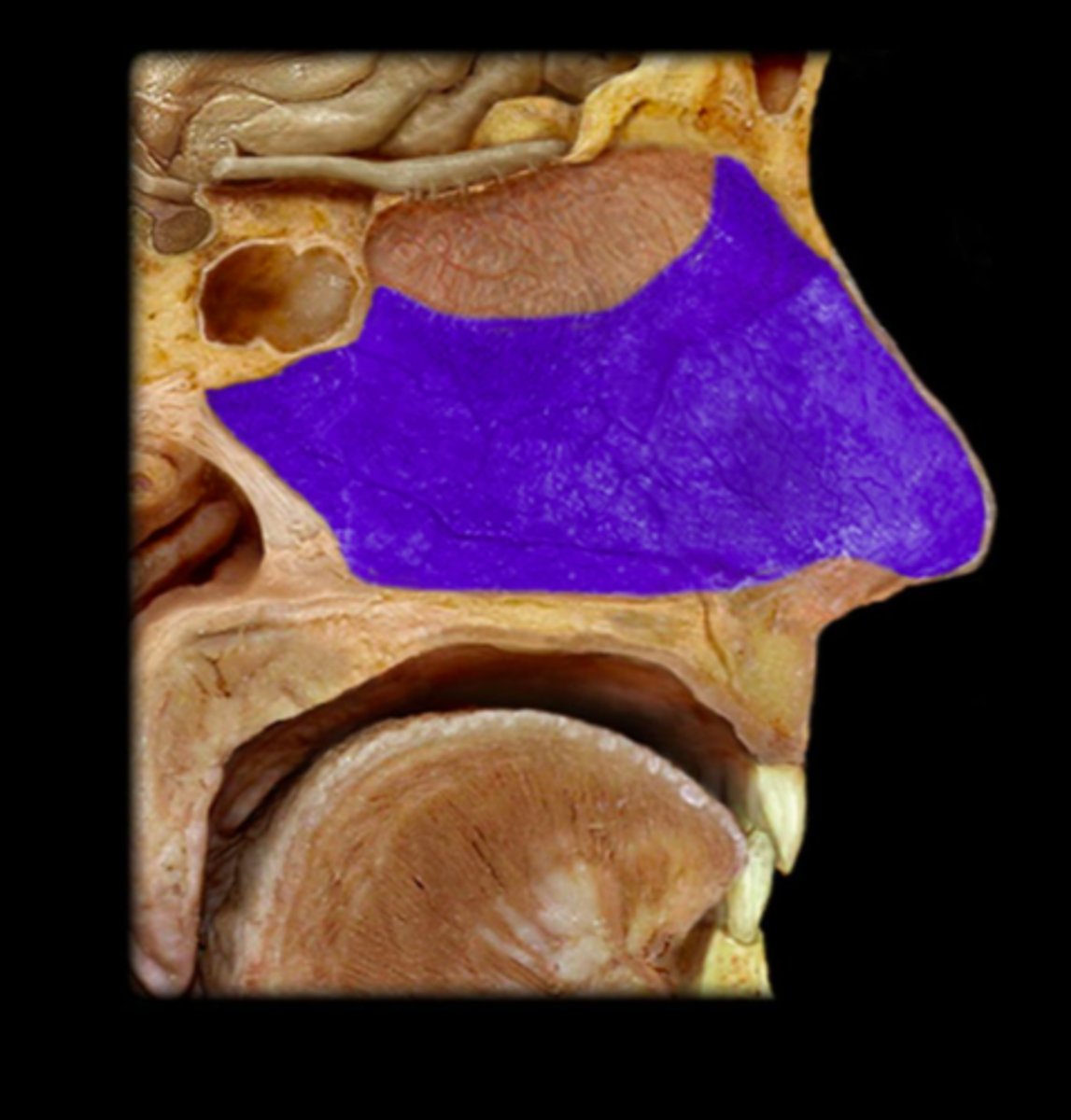
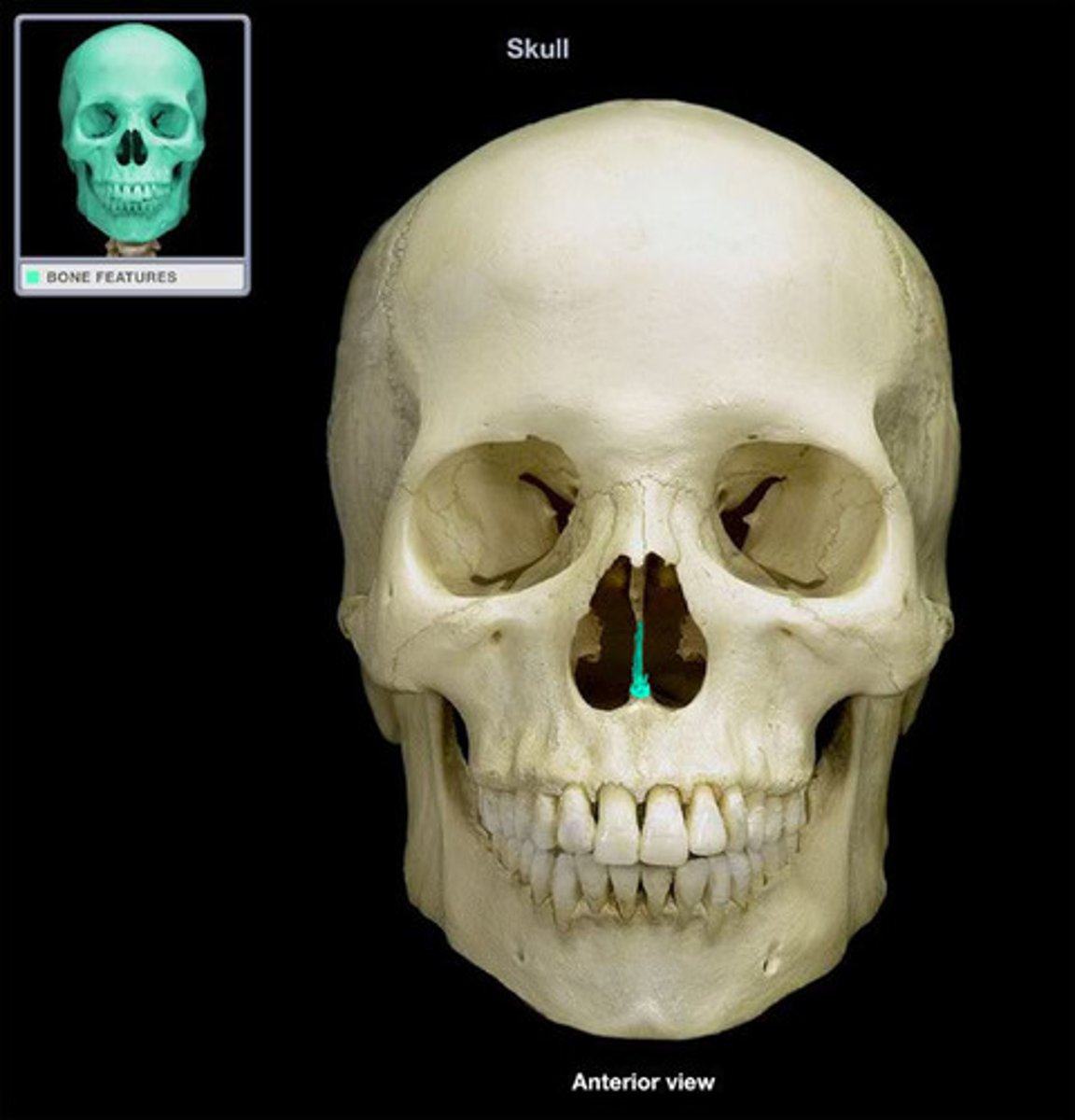
Nasal Septum
A wall of cartilage (midline) that divides the nose into two equal sections
Hard Palate
anterior "roof of the mouth" portion, supported by bone
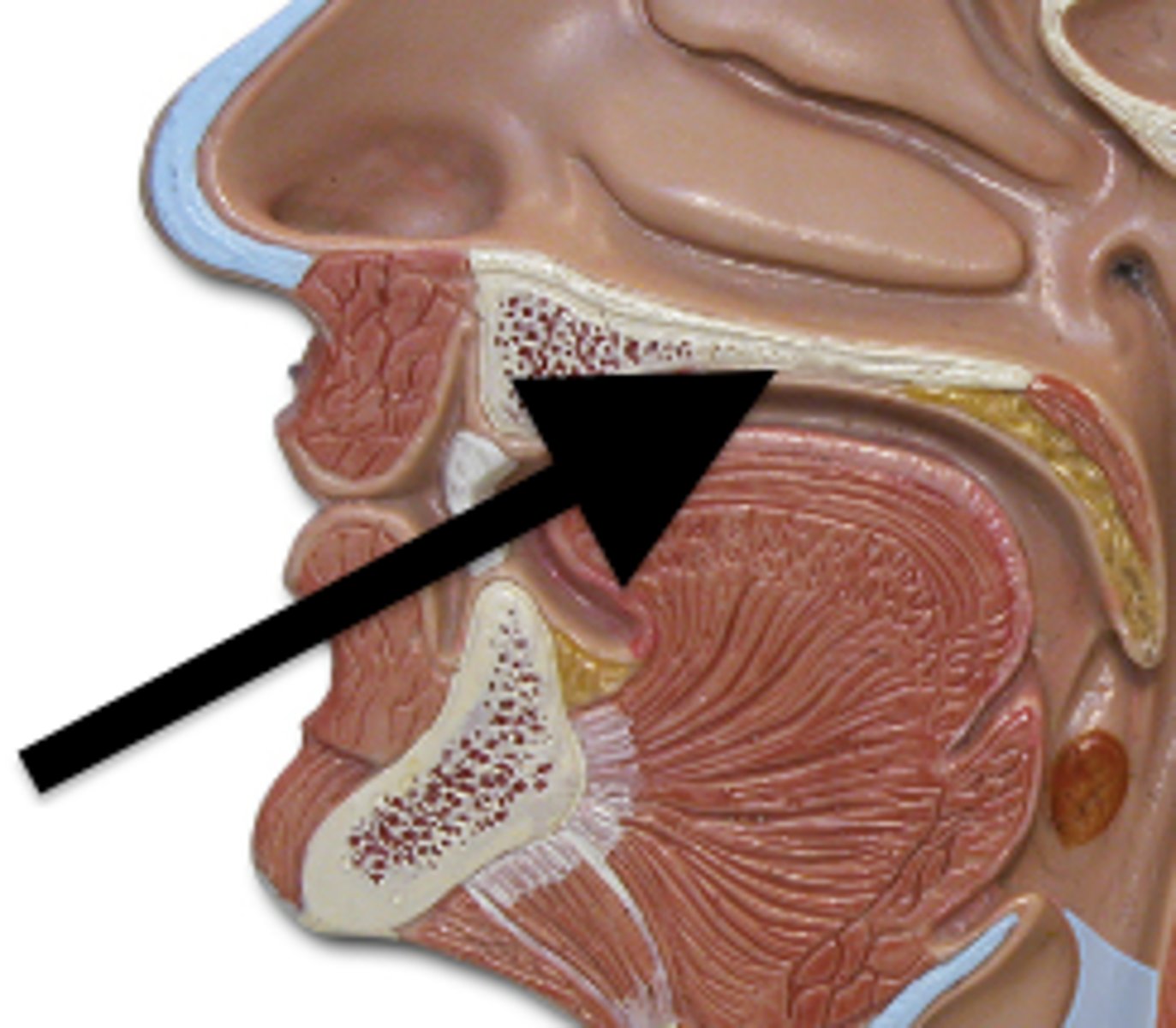
Soft Palate
posterior portion, not supported by bone
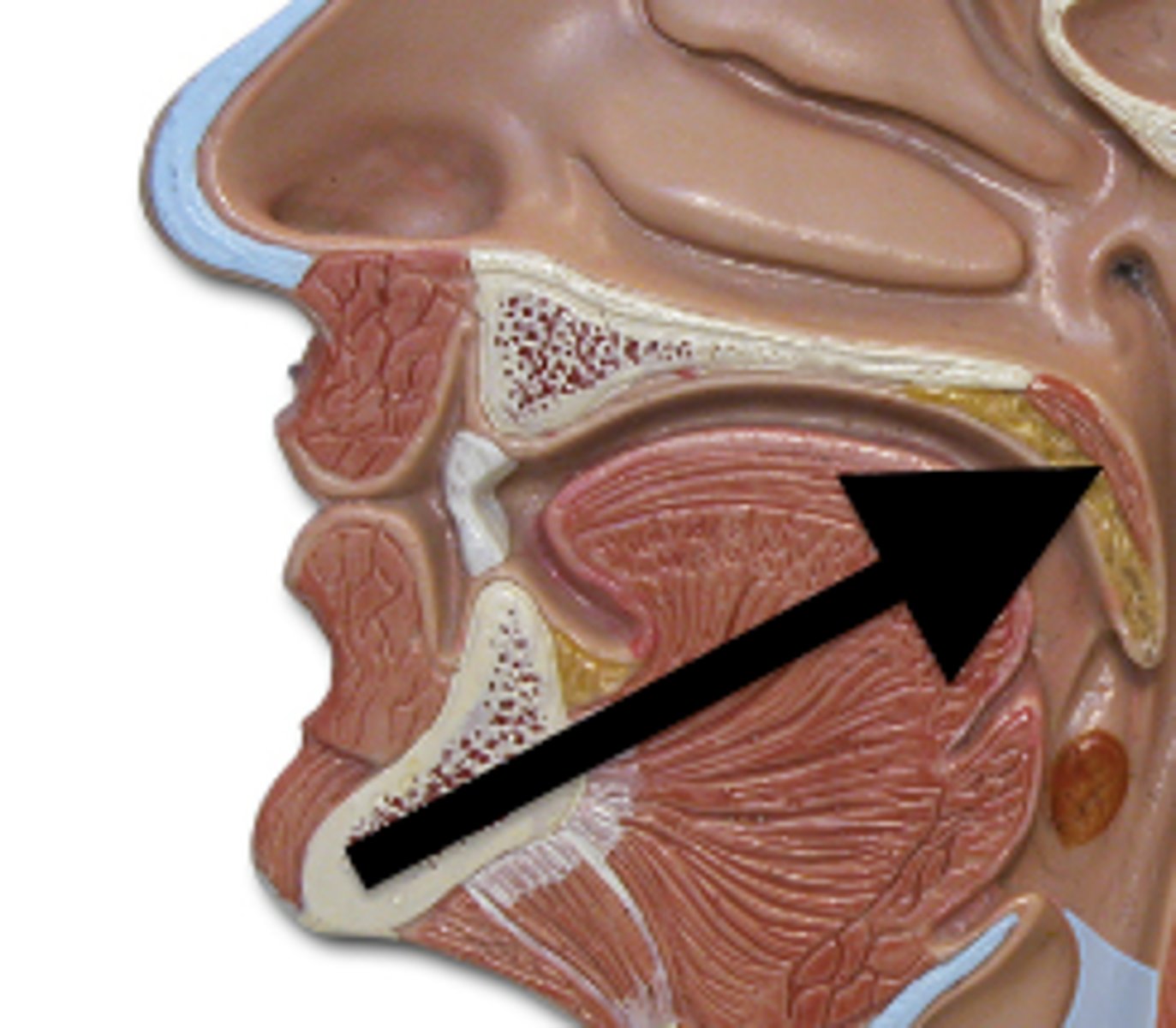
Paranasal Sinuses
Openings in bones
- produce mucus
- Resonance chambers for speech
- Frontal, Sphenoid, Ethmoid, and Macillary
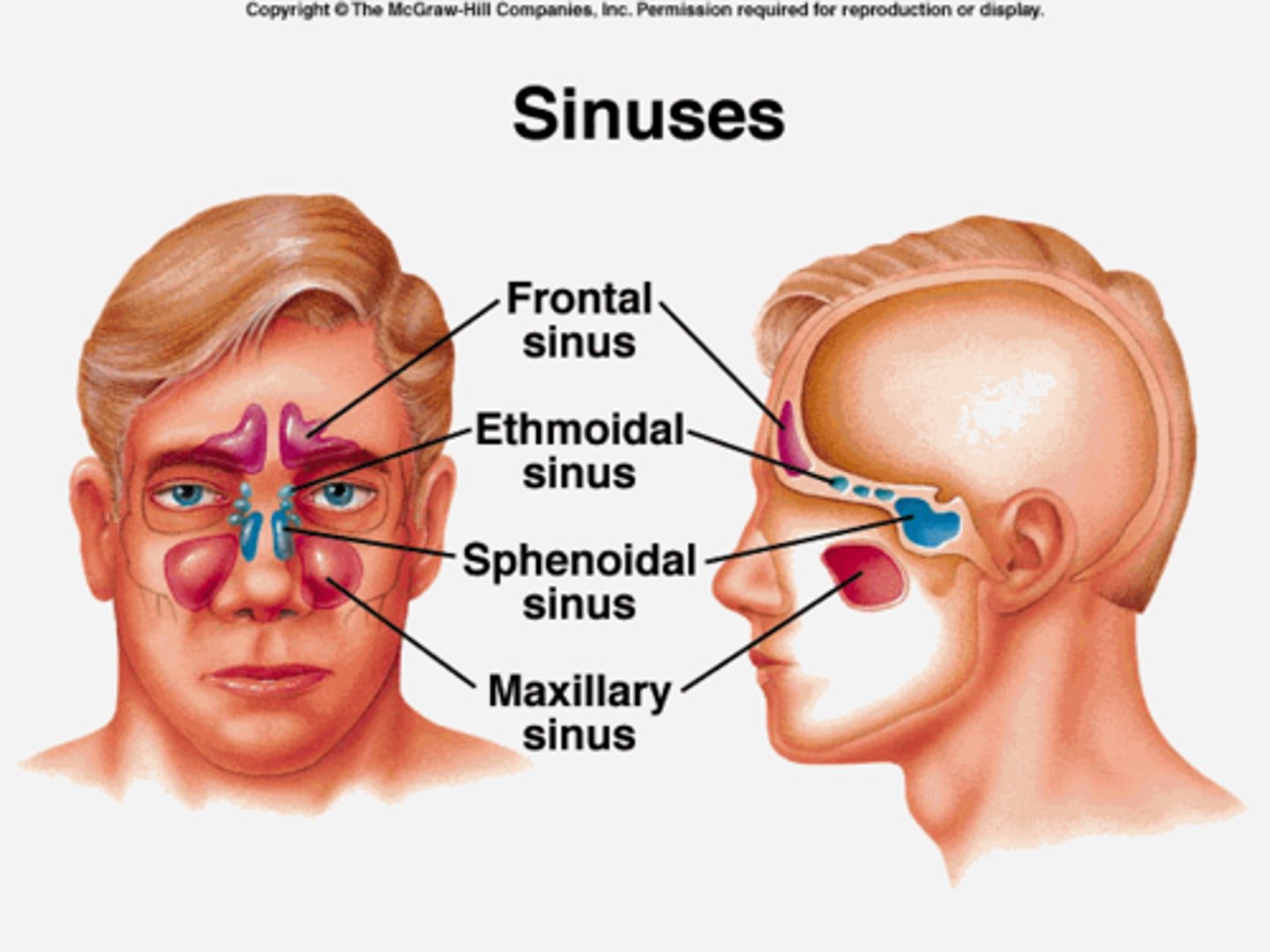
Sinuses
cavities in the skull that surround the nasal area
Function =
1. Secretes mucus
2. Humidifies and warms the air
3. Lightens the skull
4. Helps with speech
Ethmoid Sinus
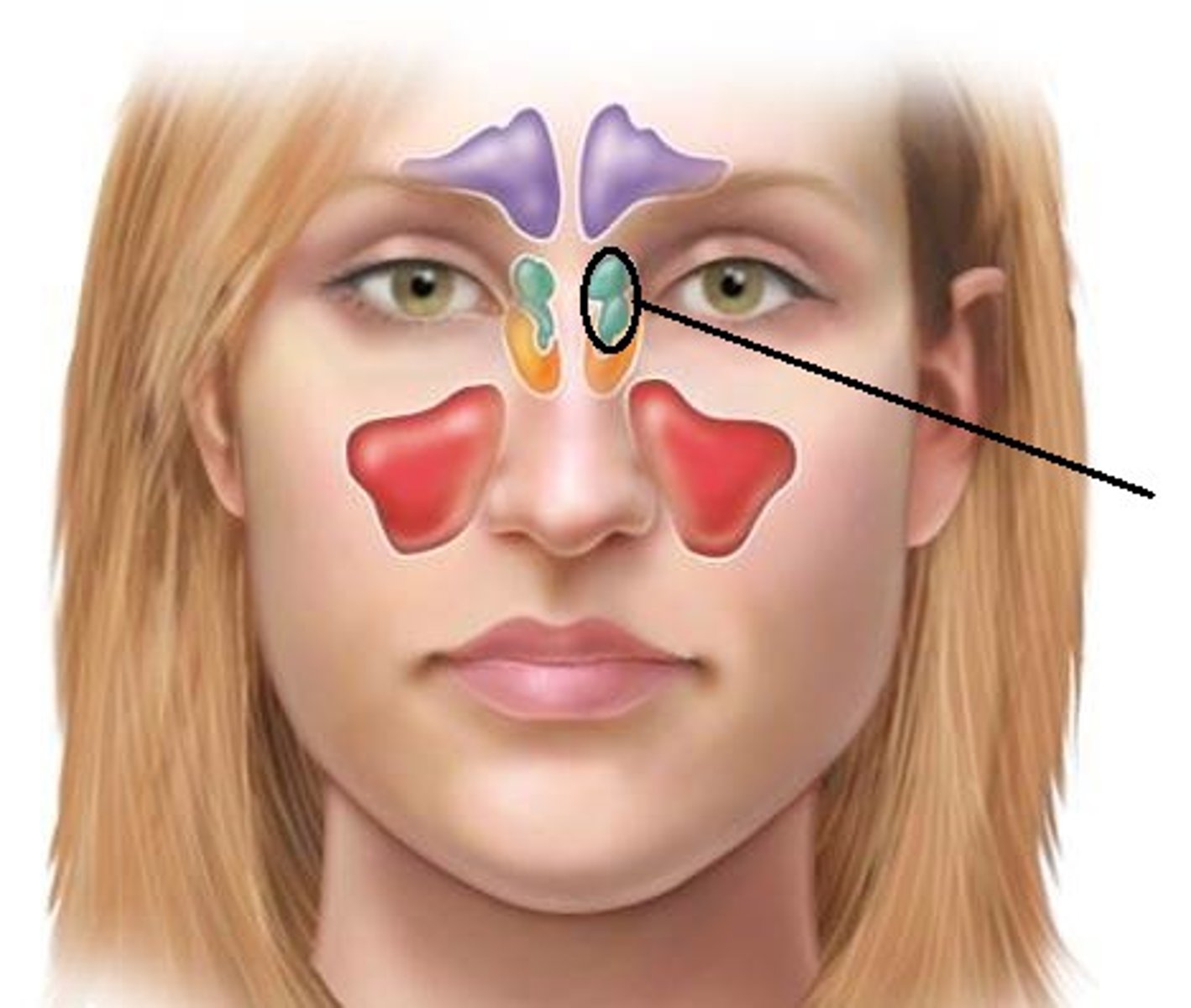
Sphenoid Sinus
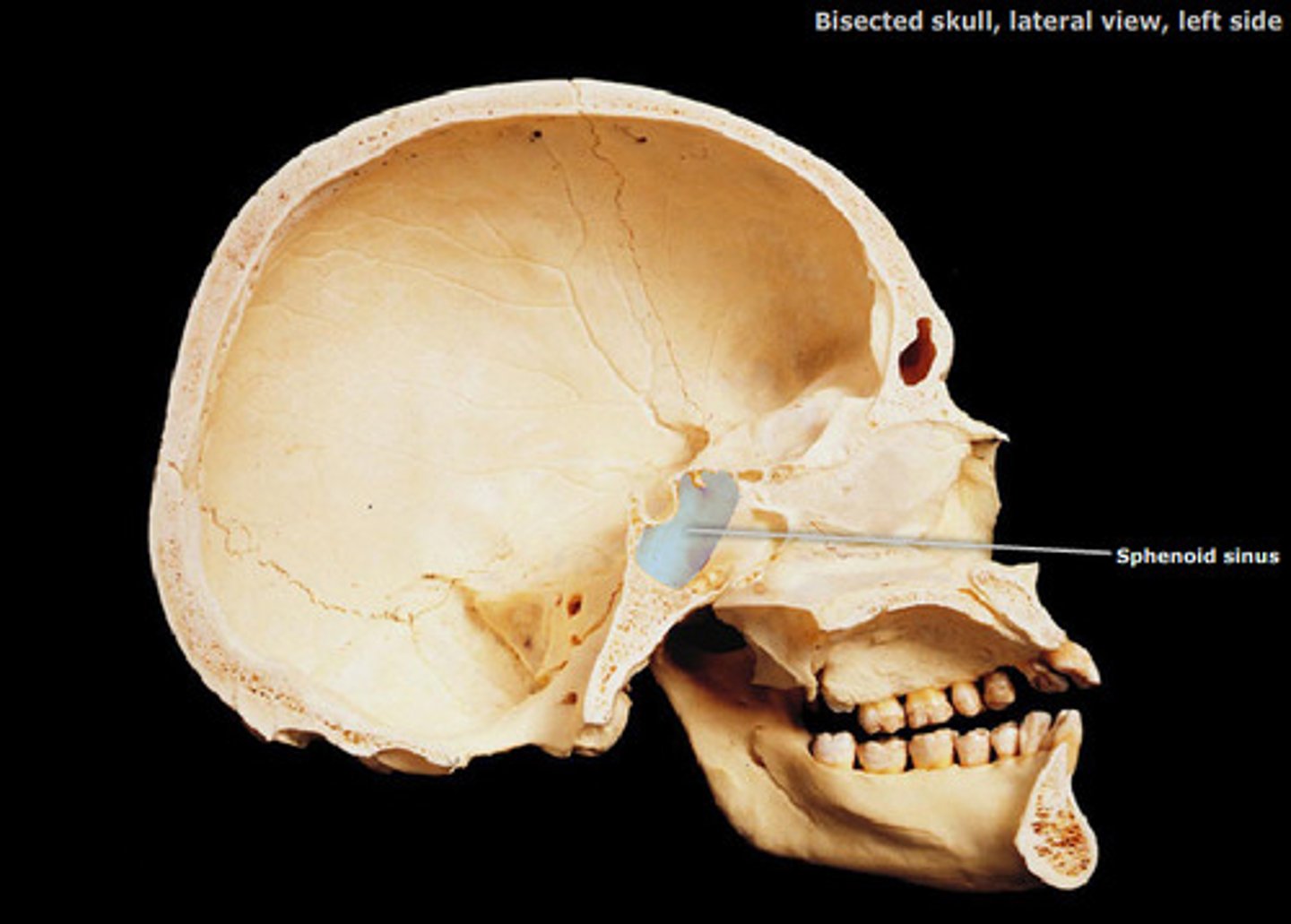
Pharynx ("Throat")
About 5 inches long -> The passageway for food and air
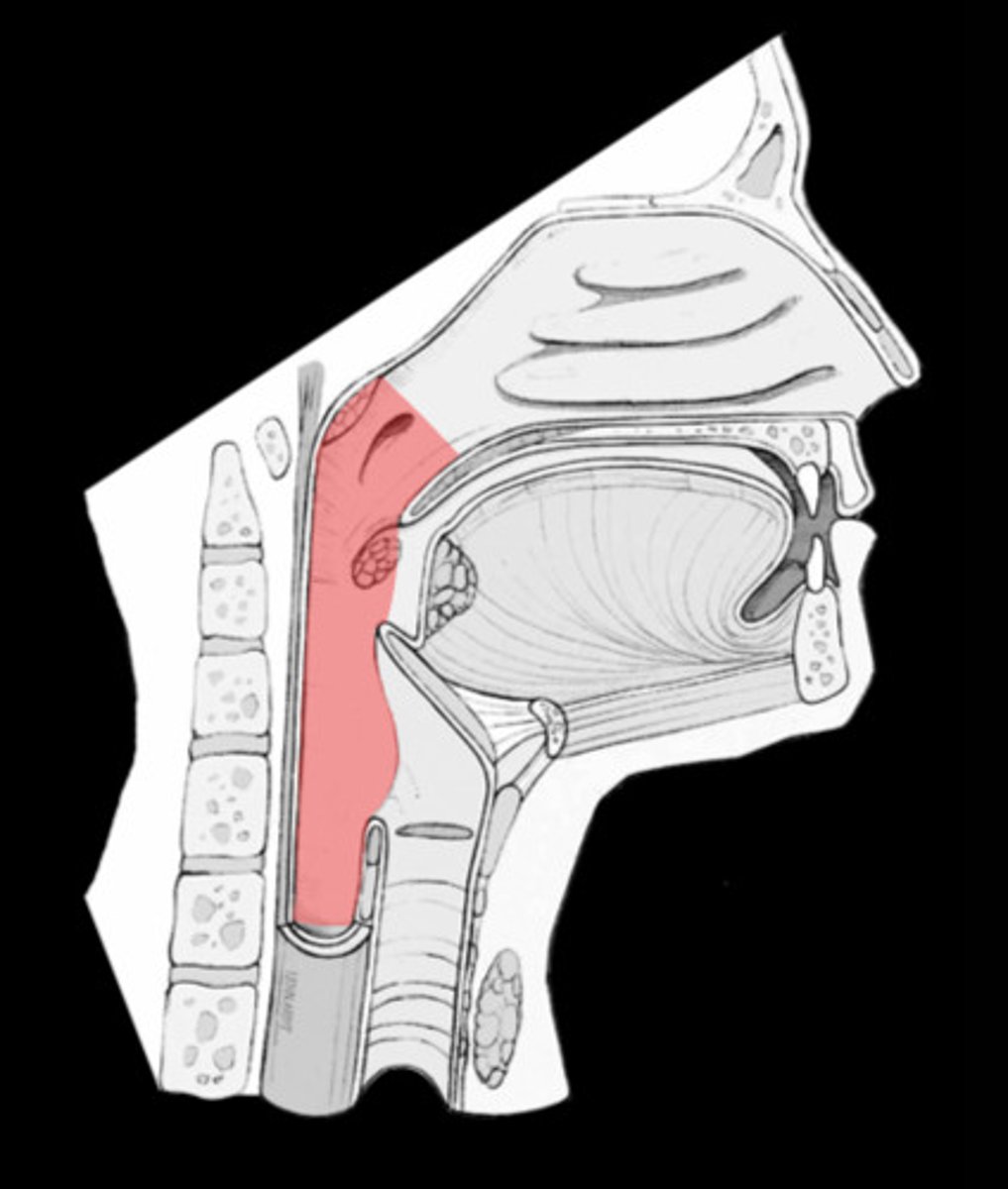
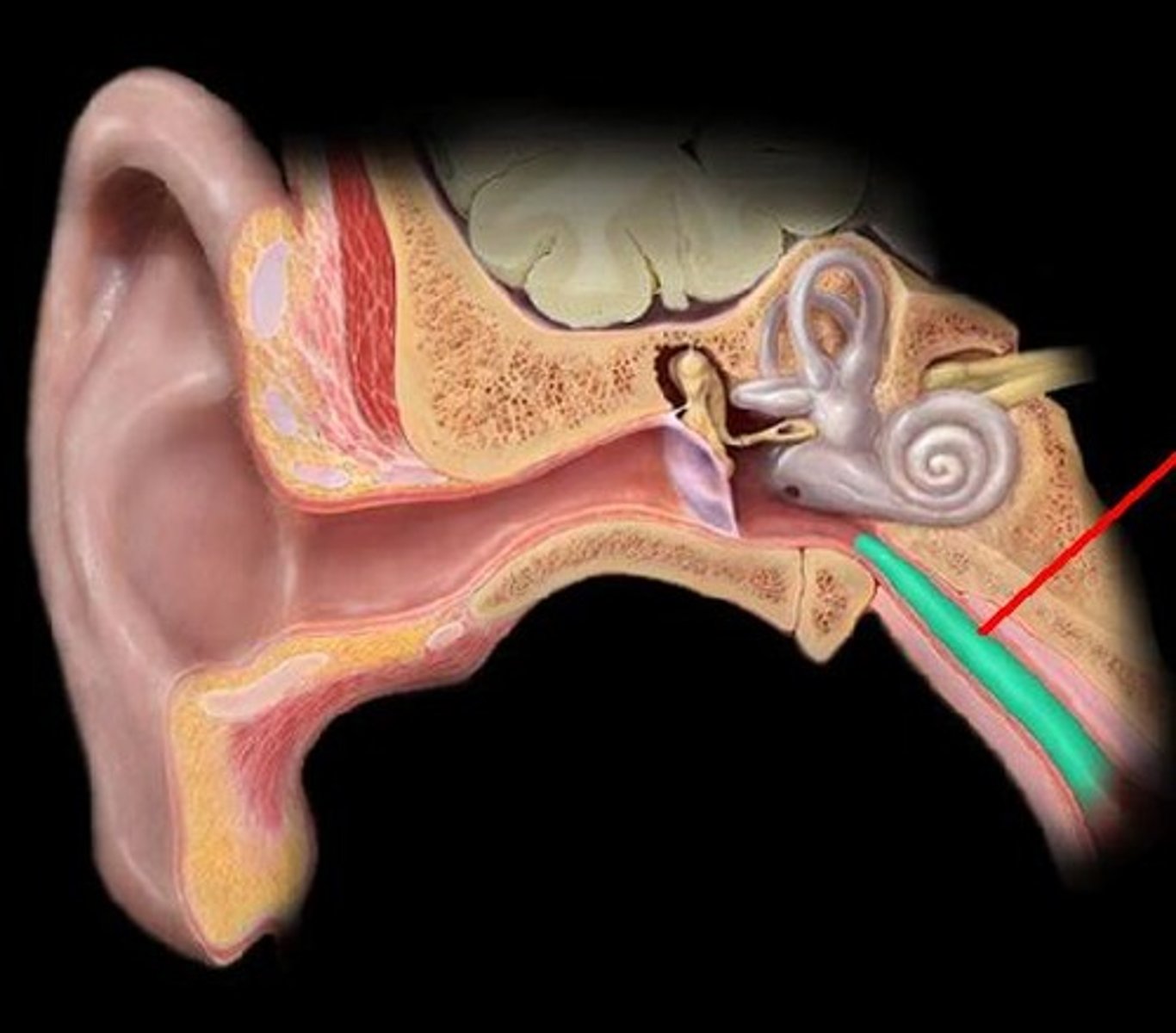
Pharyngotympanic tube
connects the middle ear to the nasopharynx
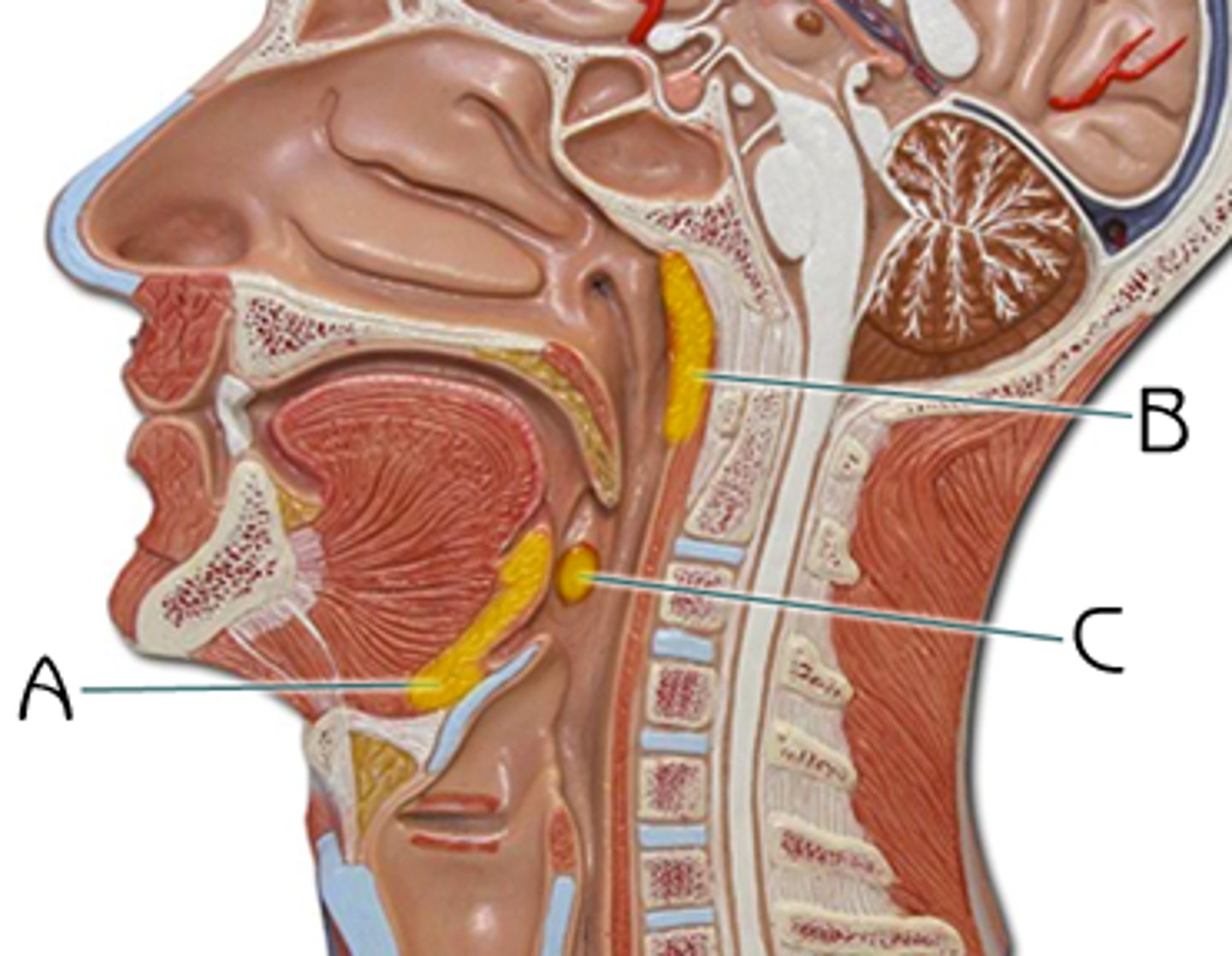
1) Pharyngeal tonsil - 1
- AKA "adenoid"
2) Palatine tonsils - 2
- AKA "tonsils"
3) Lingual tonsils - 2
Types of Tonsils
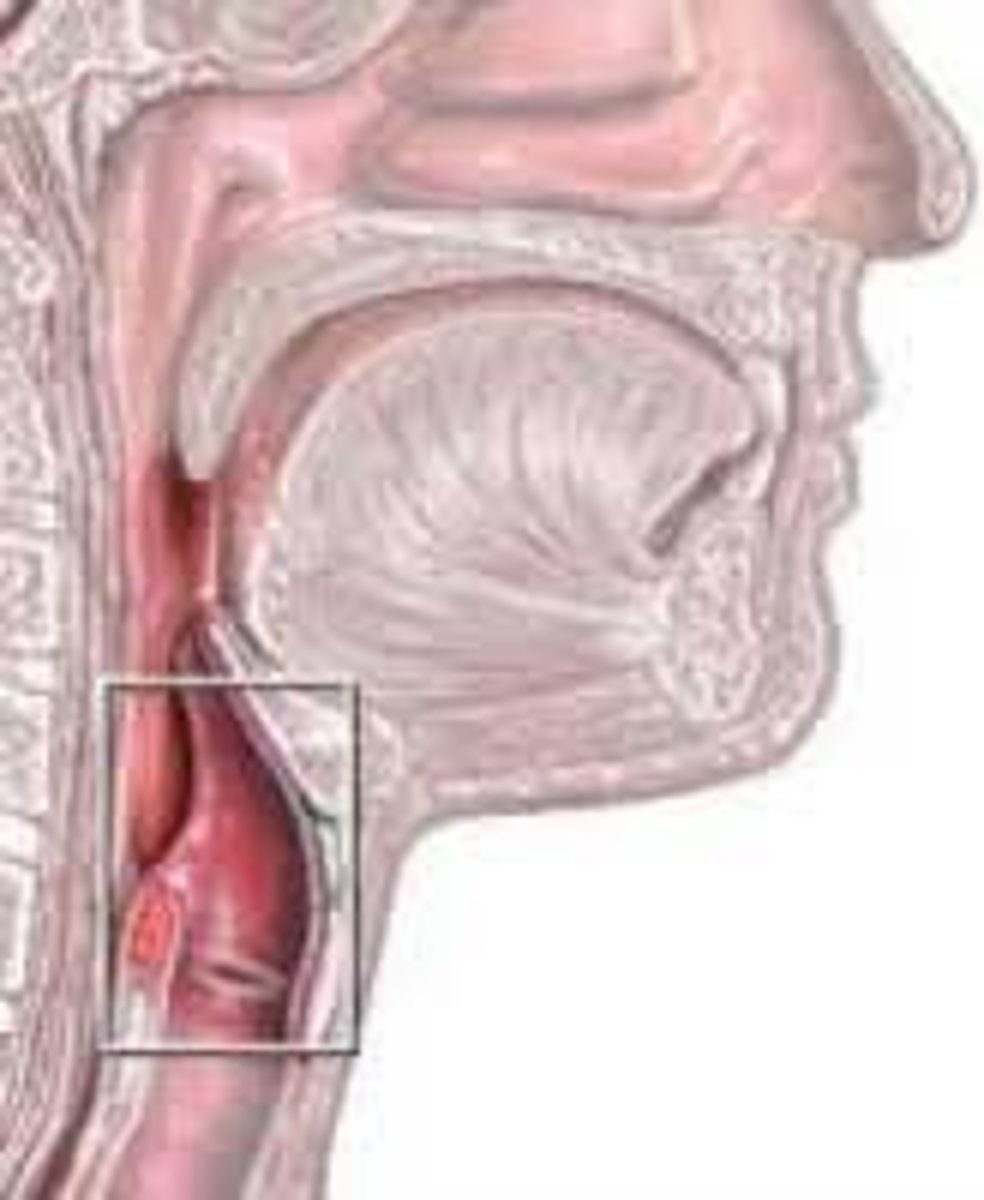
Larynx ("Voice box")
Properly routes air in/out
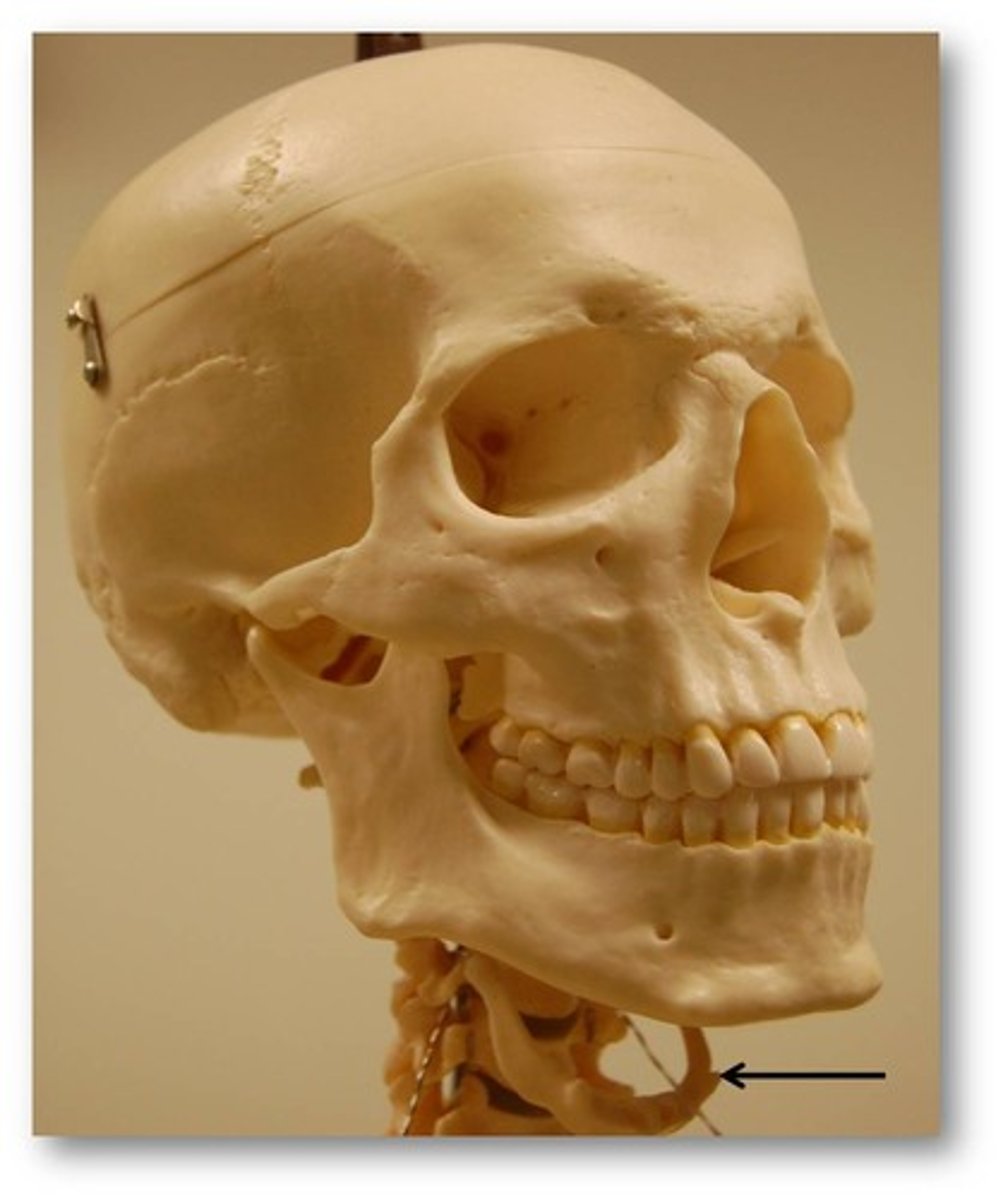
Hyoid bone
muscular control of the epiglottis + controls swallowing
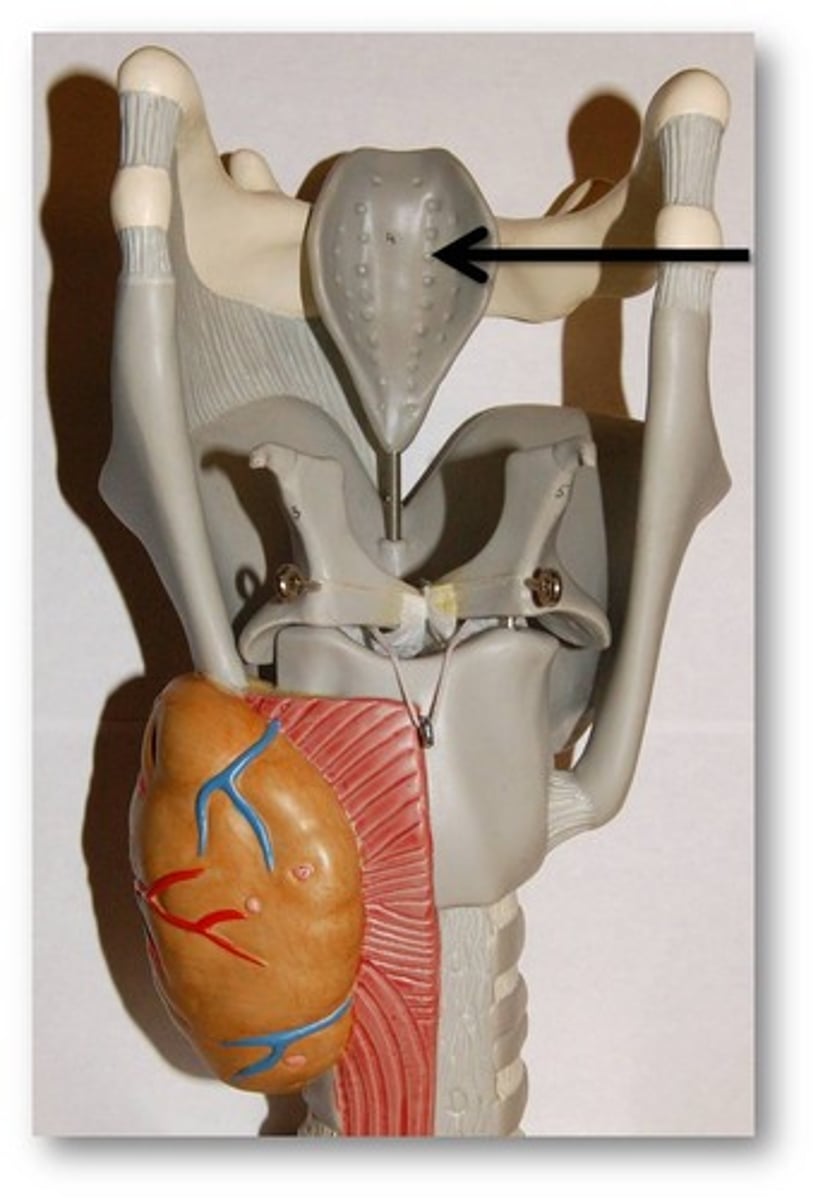
Epiglottis
spoon-shaped flap of elastic cartilage
- closes the larynx when swallowing
Hyaline cartilage
Protruding thyroid cartilage
- Produces "Adam's apple"
Glottis
Vocal Cords = mucous membrane folds in the larynx
- Vibrates with expelled air
Trachea ("windpipe")
Air passageway between the larynx to the 5th thoracic vertebra
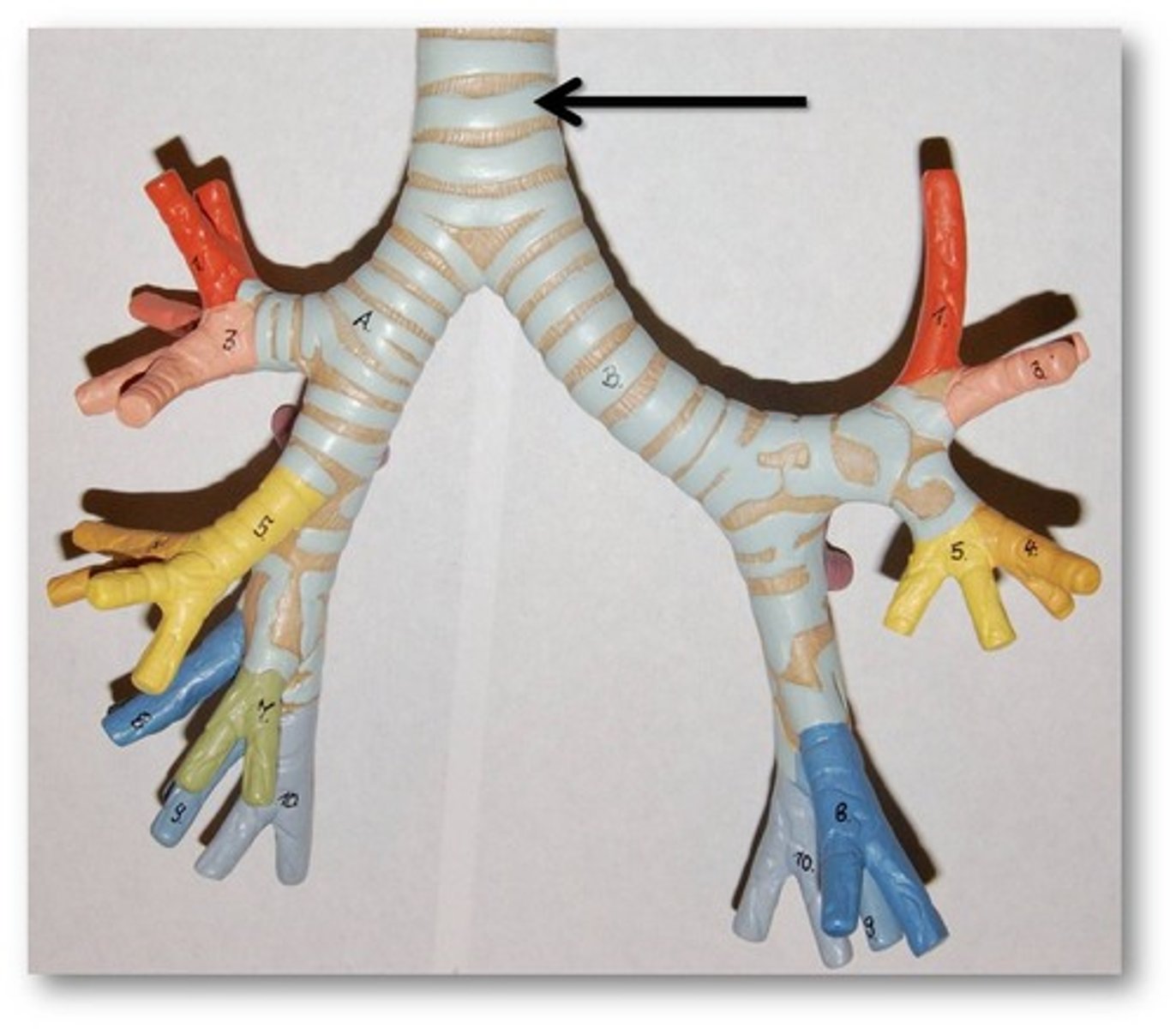
C rings
Rings of Hyaline cartilage on the trachea
- Keeps the trachea open for air flow despite pressure changes
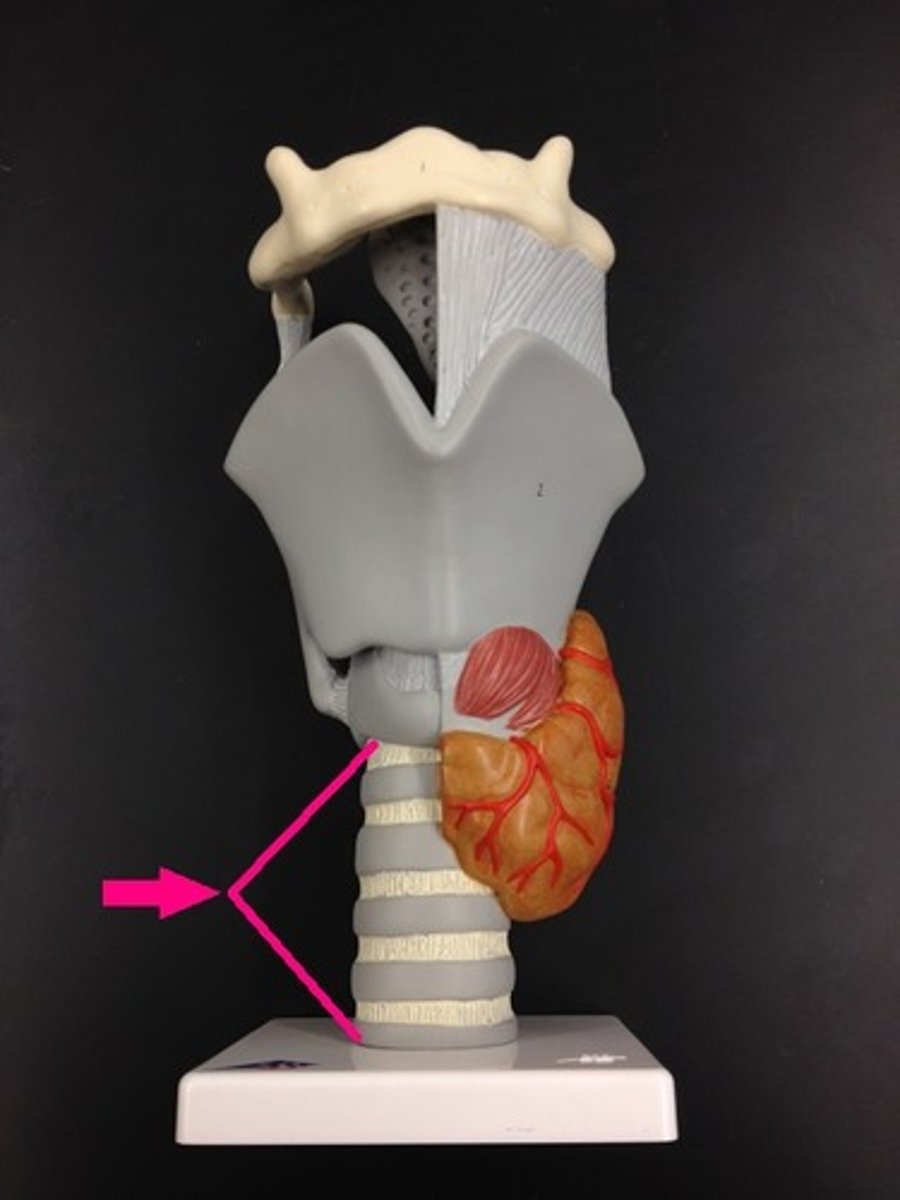
Trachealis muscle
band of smooth muscle that connects the tracheal and esophagus
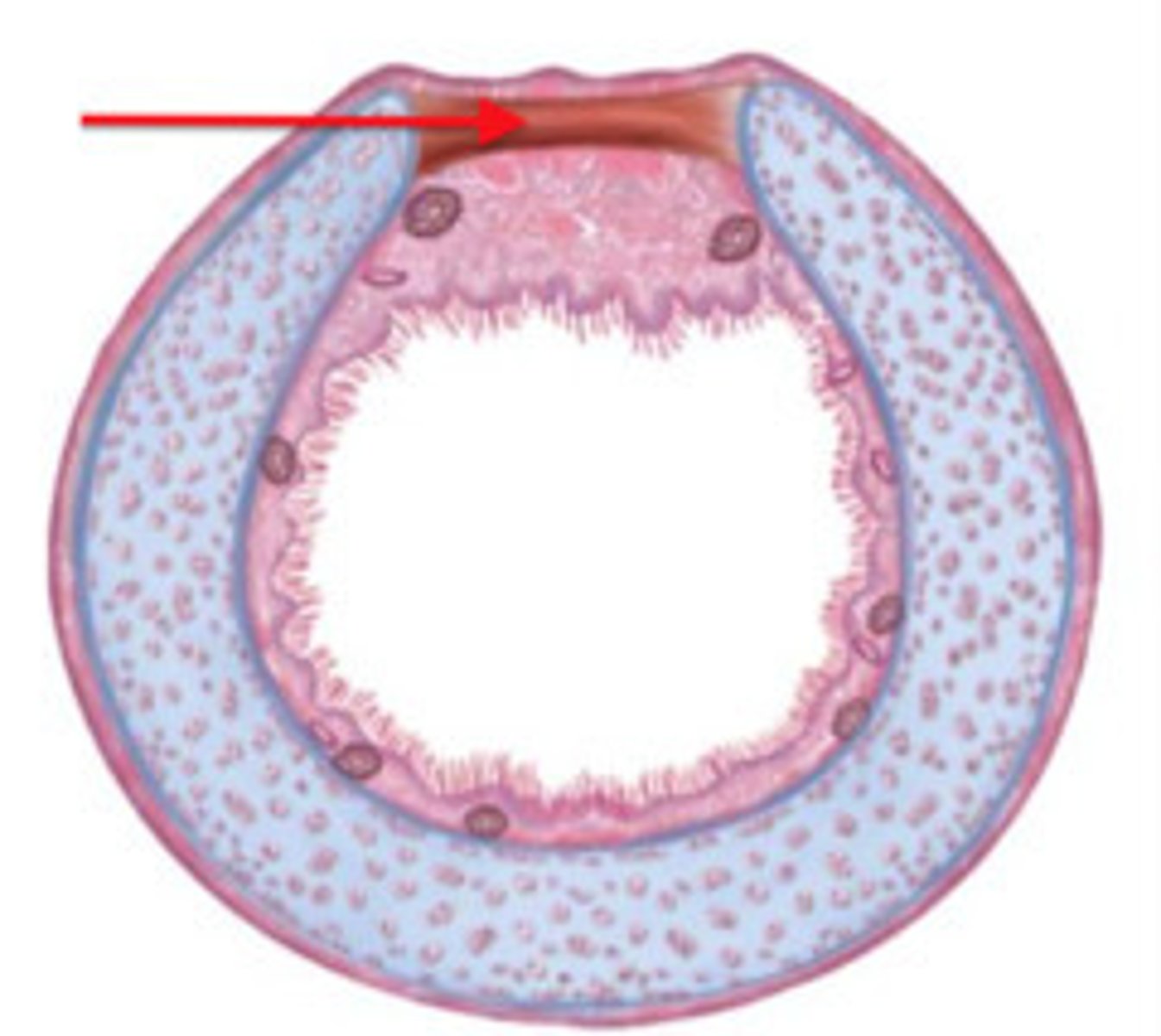
ciliated mucosa
Pushes against the flow of air and Traps Pathogens
- ciliated pseudo-stratified columnar epithelium
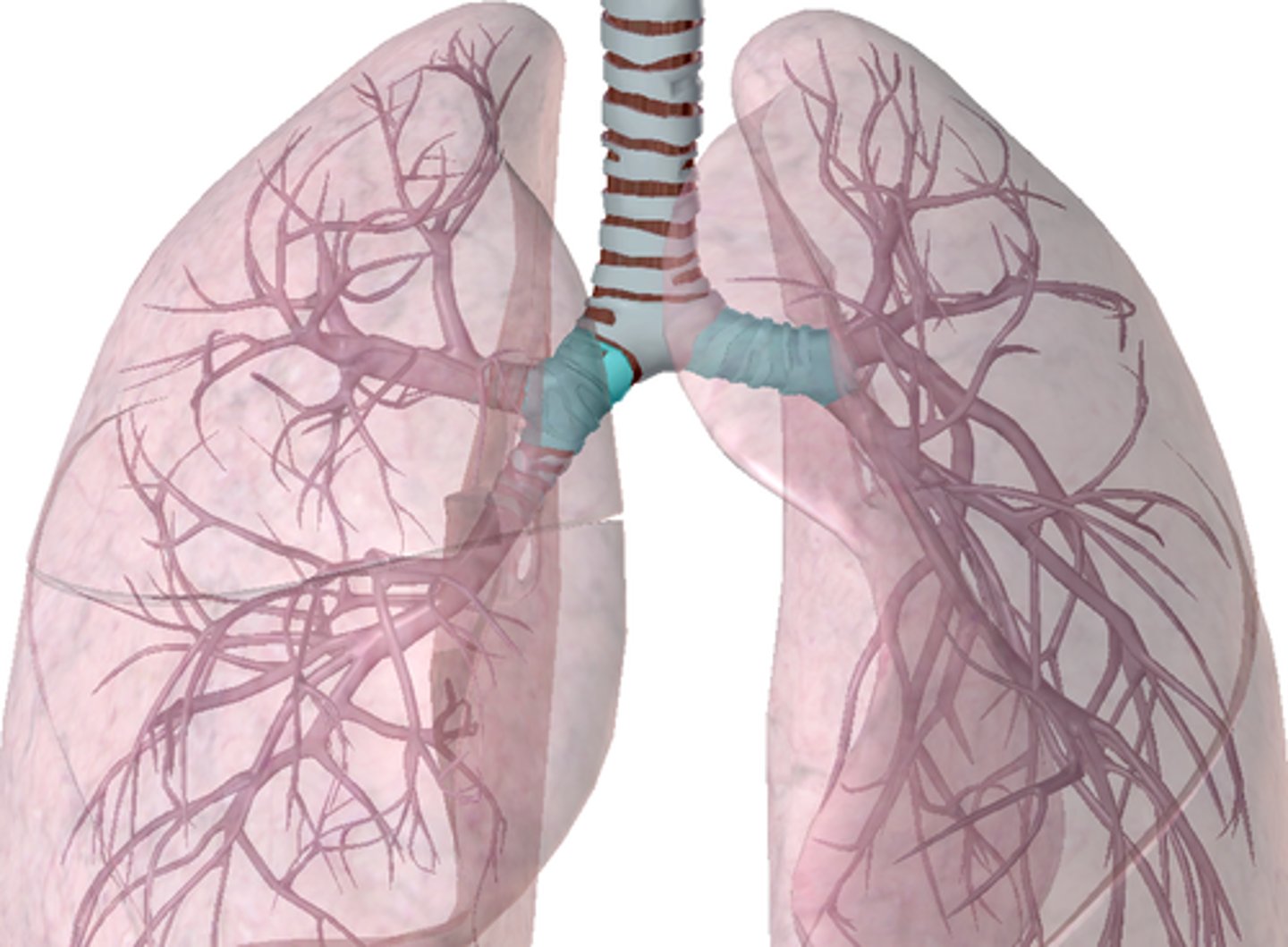
Main bronchi
Right and left main lung (primary bronchi)
- Right primary bronchus = wider, shorter, and straighter than left (left smaller to make room for heart)
- Bronchi subdivisions (bronchioles) -> Air sacs (alveoli)
Apex
Superior point of lungs near the clavicle
Base
Inferior point of lungs along the diaphram
Left lung = 2 lobes
Right lung = 3 lobes
Lobes of Right and Left lungs
**Note: Lungs surrounded by elastic connective tissue
Pleural cavity
Serous Layer
- Pleural fluid; slippery
- Pulmonary pleura and parietal pleura
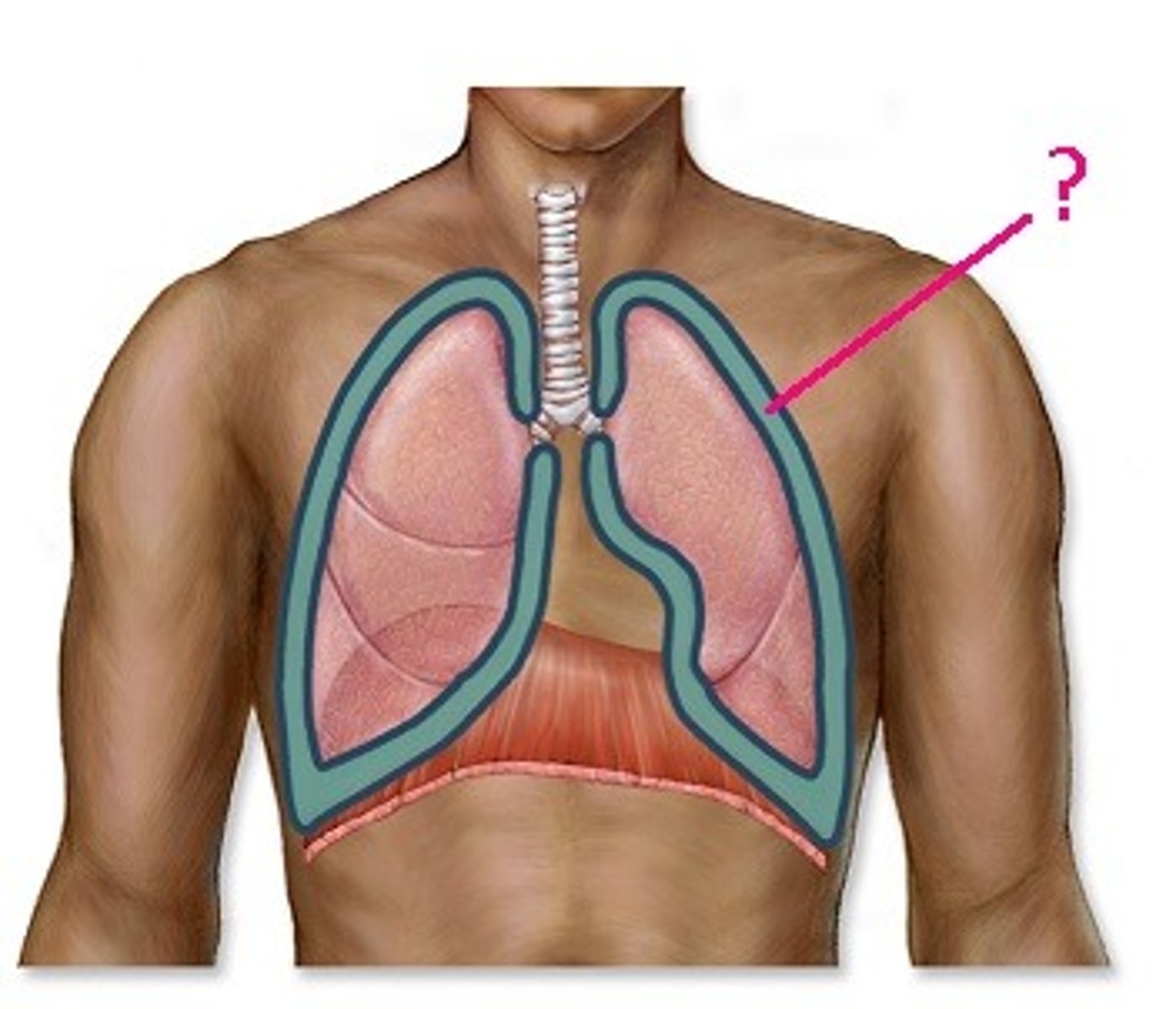
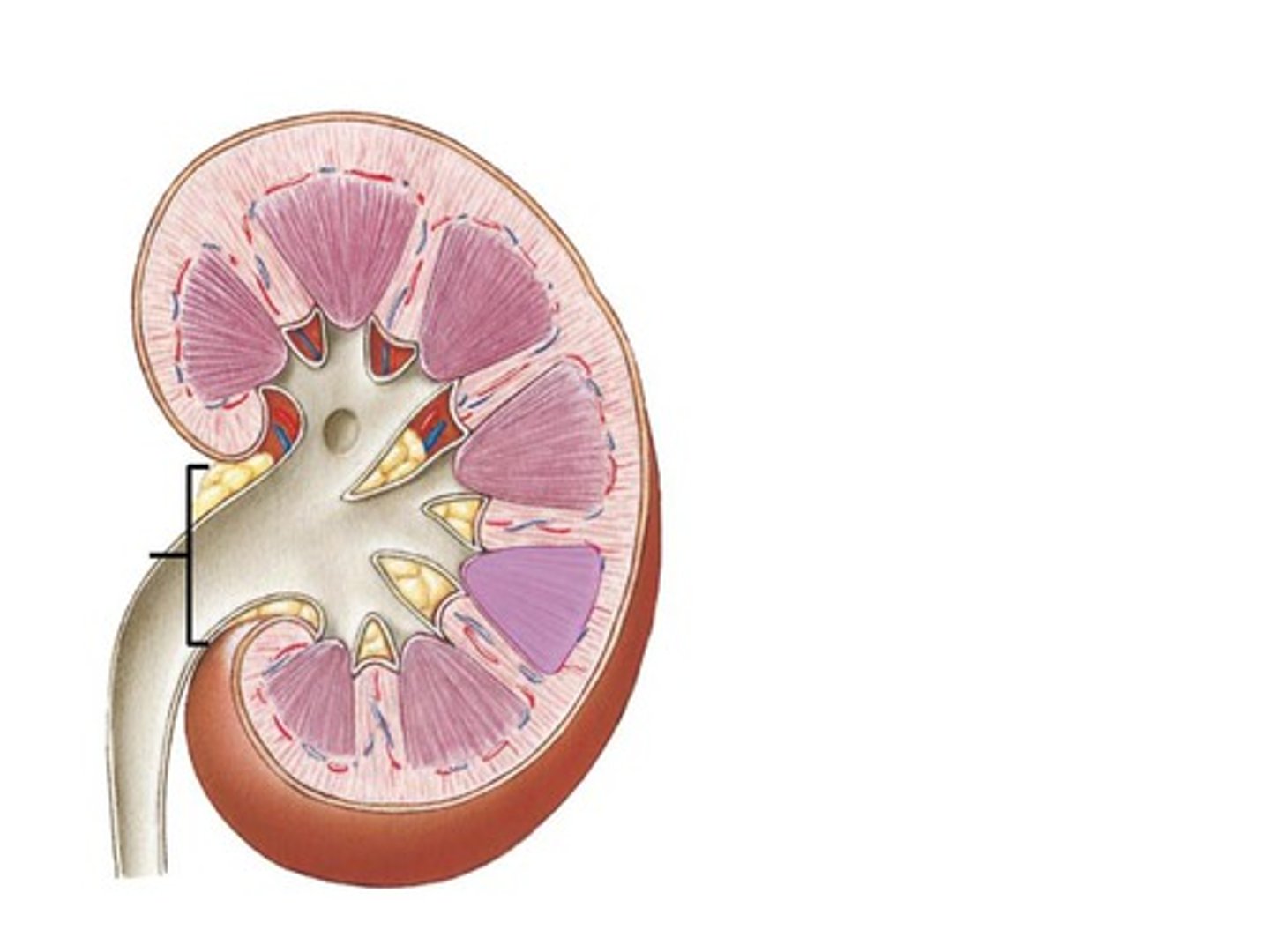
Hilum
"root" of lungs where bronchi attach
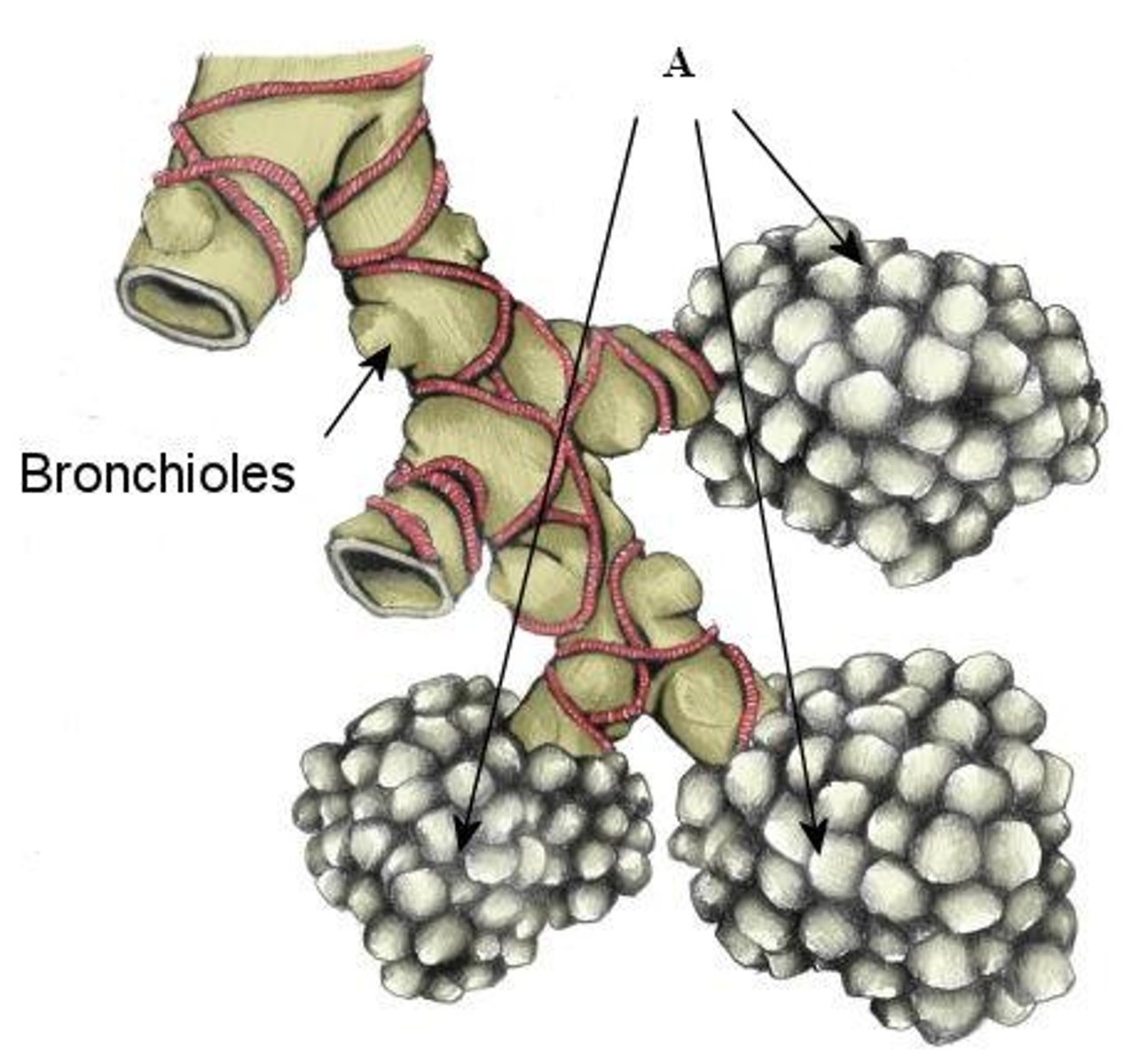
Alveoli
Air sacs where gas exchange occurs
- Makes up most of the lungs
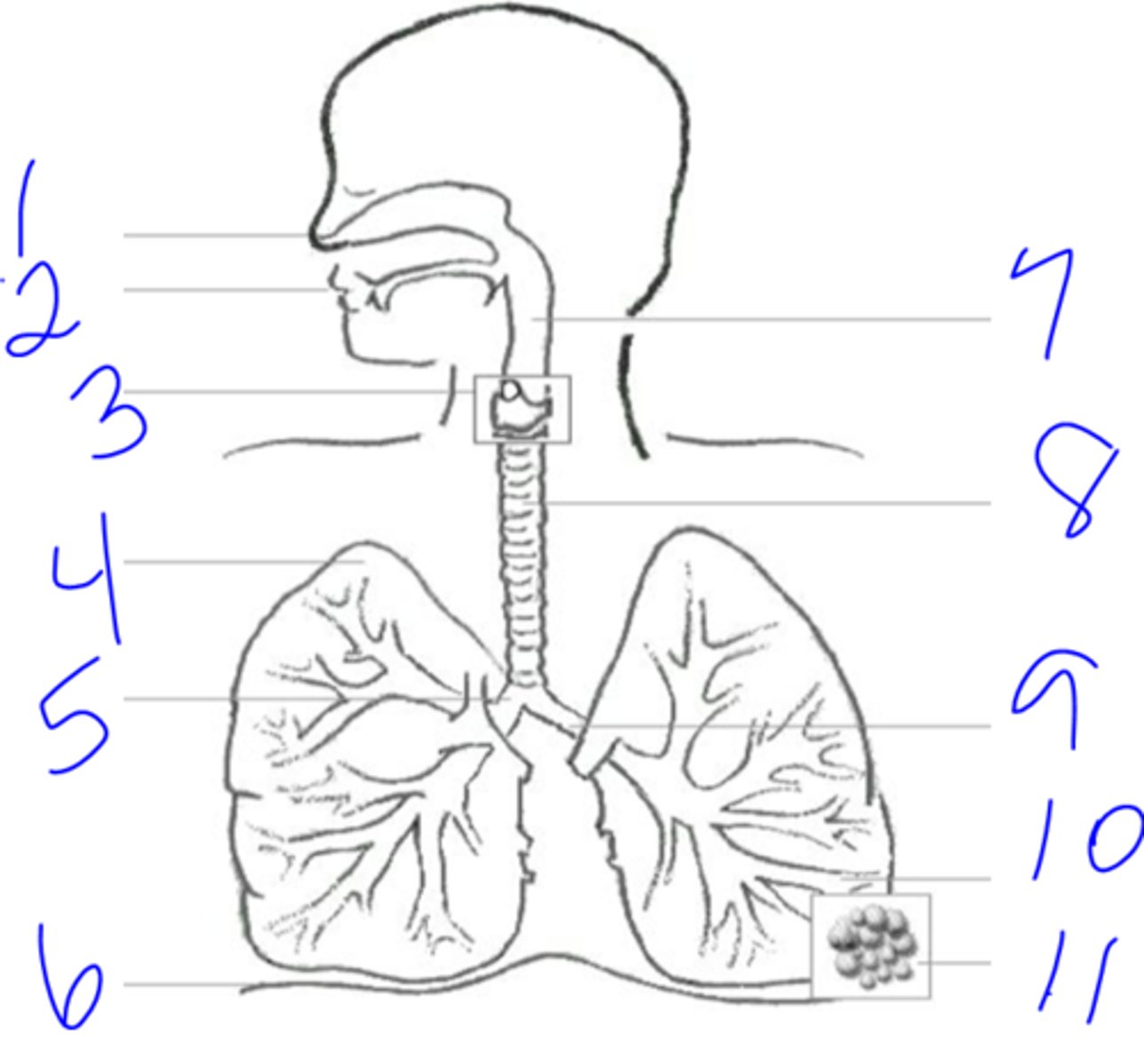
1. Oral/Nasal cavities
2. Pharynx
3. Larynx
4. Trachea
5. Bronchi
6. Bronchioles
7. Alveoli
Flow of Air
Respiratory membrane
Where gas exchange occurs between the air on the alveolar side and the blood on the capillary side
- the alveolar and capillary walls form the respiratory membrane
- "air-blood barrier"
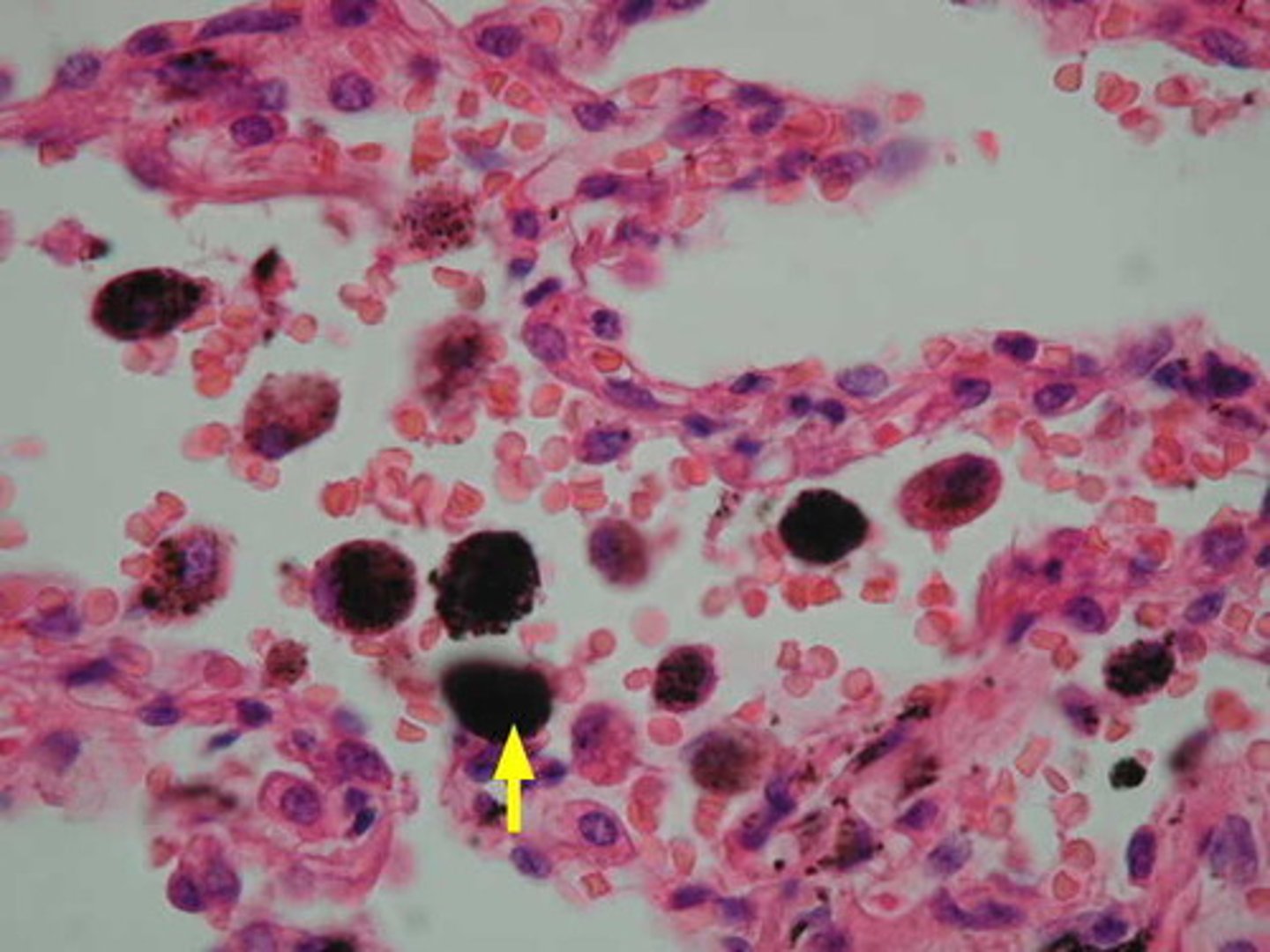
Alveolar macrophages
Clean up bacteria and other debris
- cuboidal cells that secrete surfactant
Surfactant
- Decreases water surface tension
- Without it -> water molecules stick together and alveolus collapses
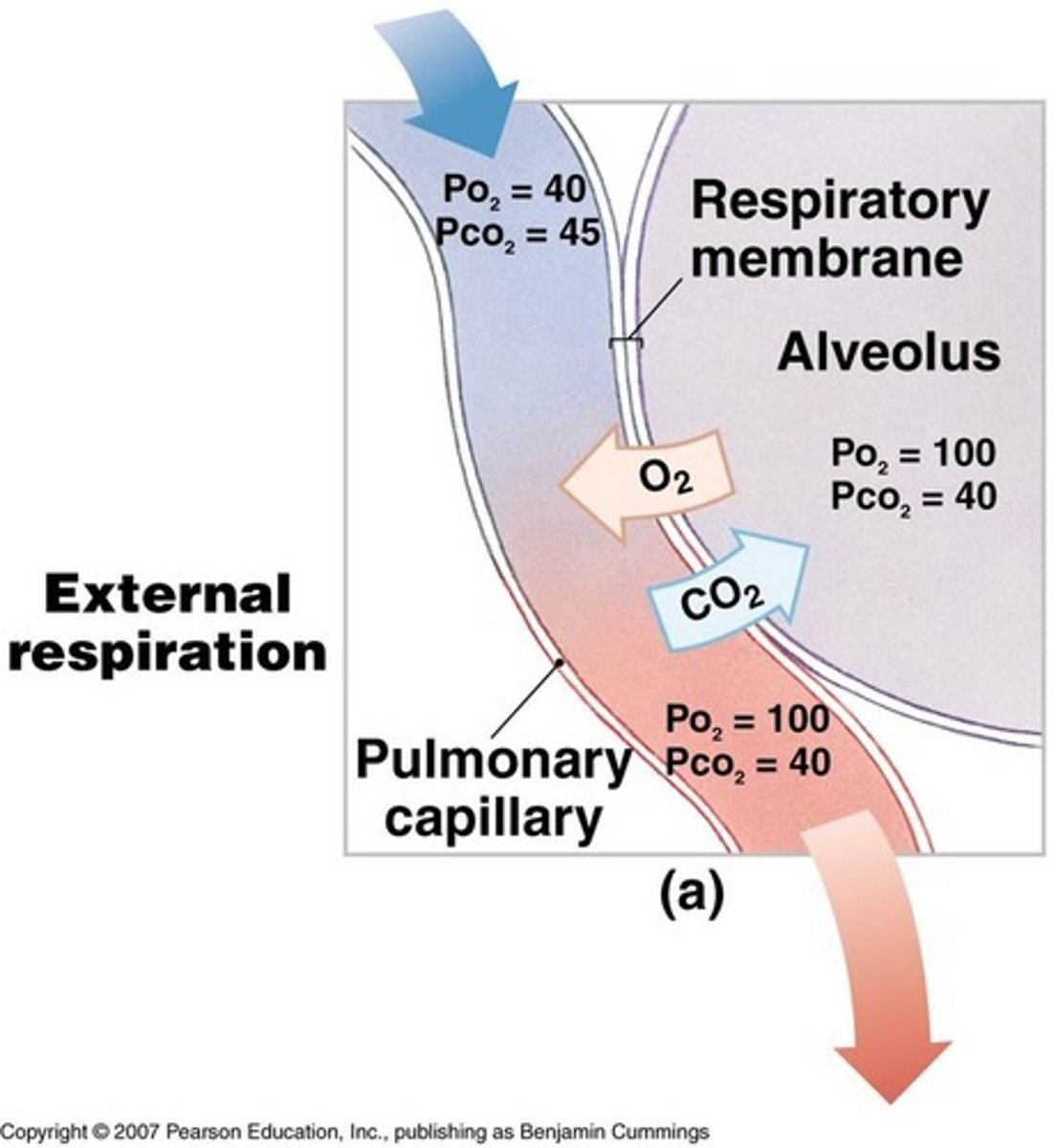
External Respiration at alveoli
- Oxygen enters blood
- Carbon dioxide exits blood
Internal respiration at the body's tissues
- Oxygen exits blood
- Carbon dioxide enters blood
External respiration
The exchange of gases between the atmosphere and the blood
- Oxyhemoglobin and bicarbonate ion
Oxyhemoglobin
hemoglobin + oxygen
- some oxygen dissolves in the plasma
Bicarbonate ion - HCO3-
Carbon dioxide transported in the plasma as this
- Some carbon dioxide transported in Red Blood Cells
- HCO3- reduced to carbon dioxide and water -> Then can be released to alveoli
Internal Respiration
- Oxyhemoglobin offloads its oxygen
- Carbon dioxide and water SYNTHESIZE to form bicarbonate ion HCO3-
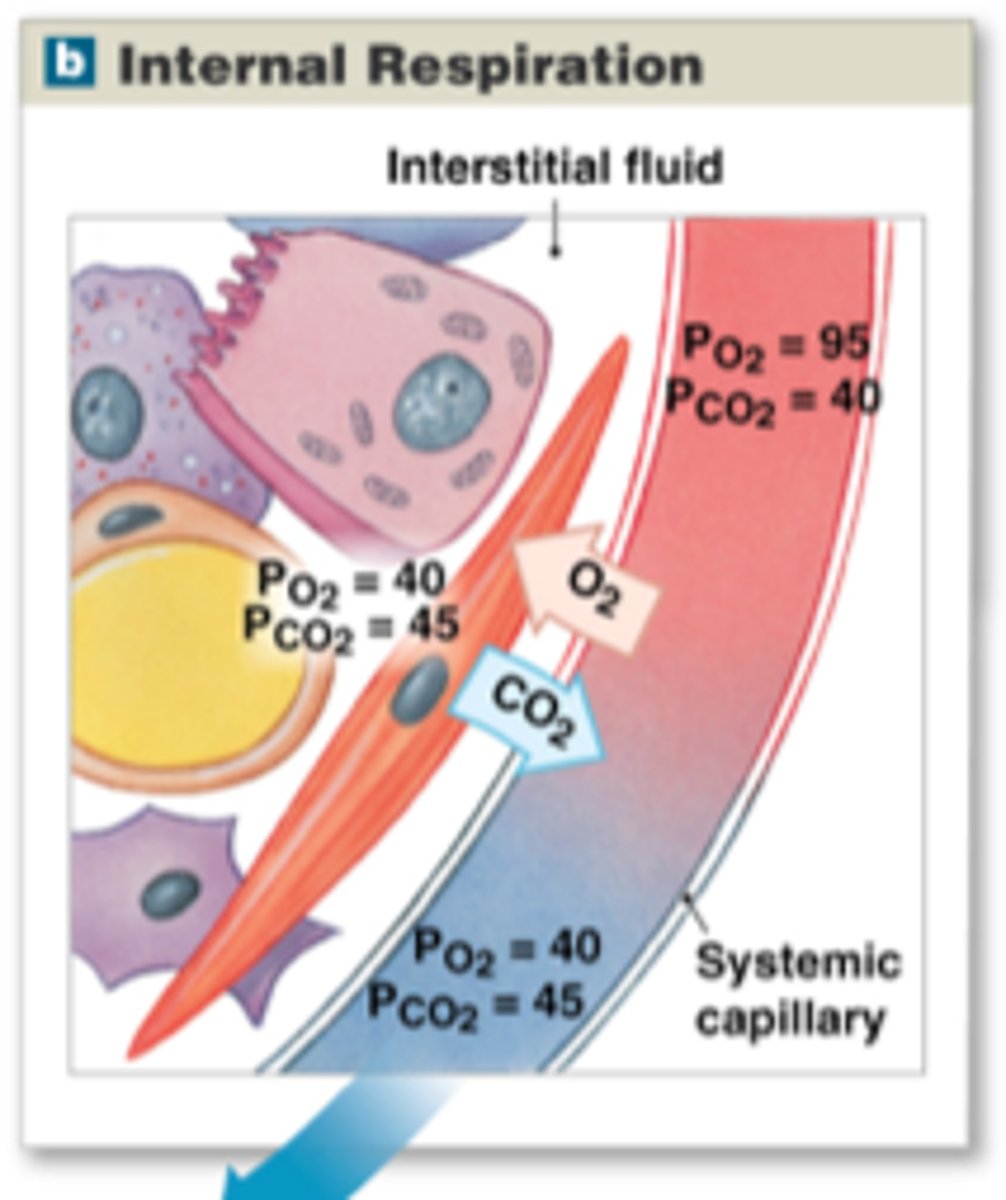
Inhalation (aka inspiration)
Air flows into the lungs
- Diaphragm contracts (flexes downwards + thoracic cavity expands)
- Intercostal muscles contract (lifts ribs and thrusts sternum forward)
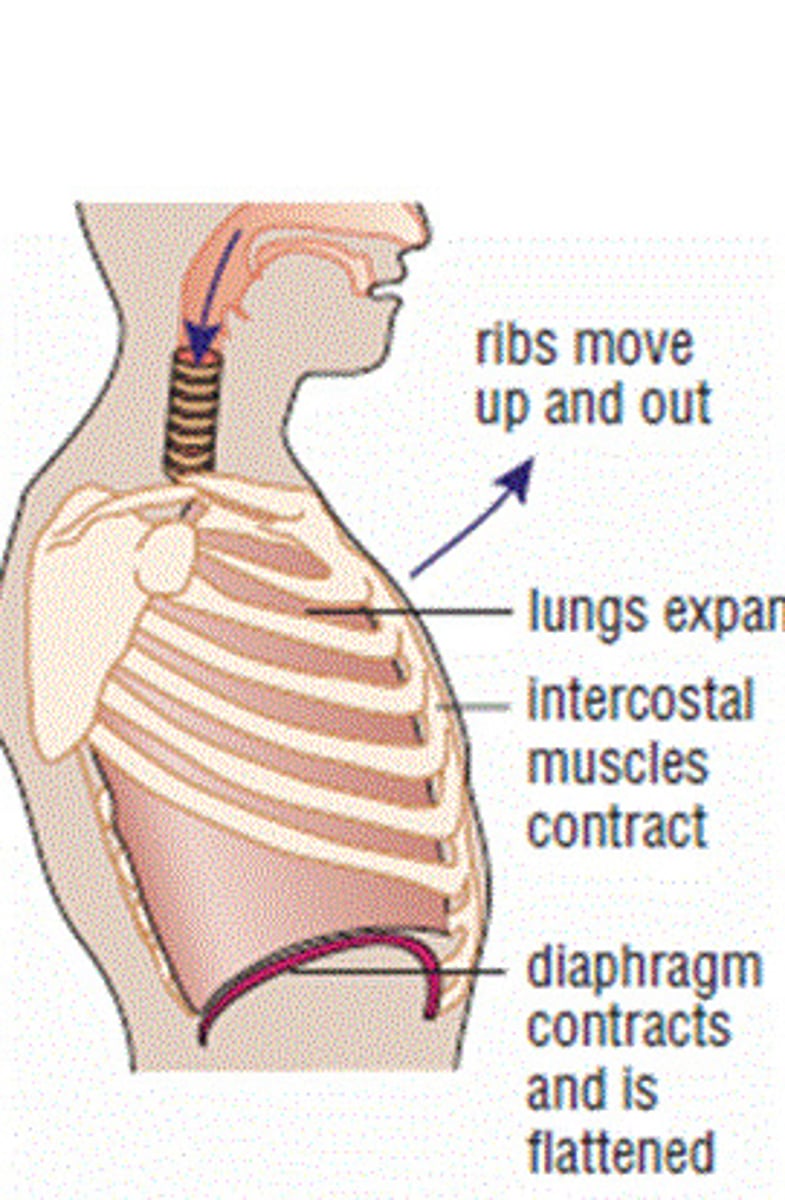
Exhalation (aka expiration)
Air flows out of the lungs
- More passive process
- Relies on elasticity
- Muscles relax
- Affected by asthma, bronchitis, and pneumonia
- May need forced exhalation
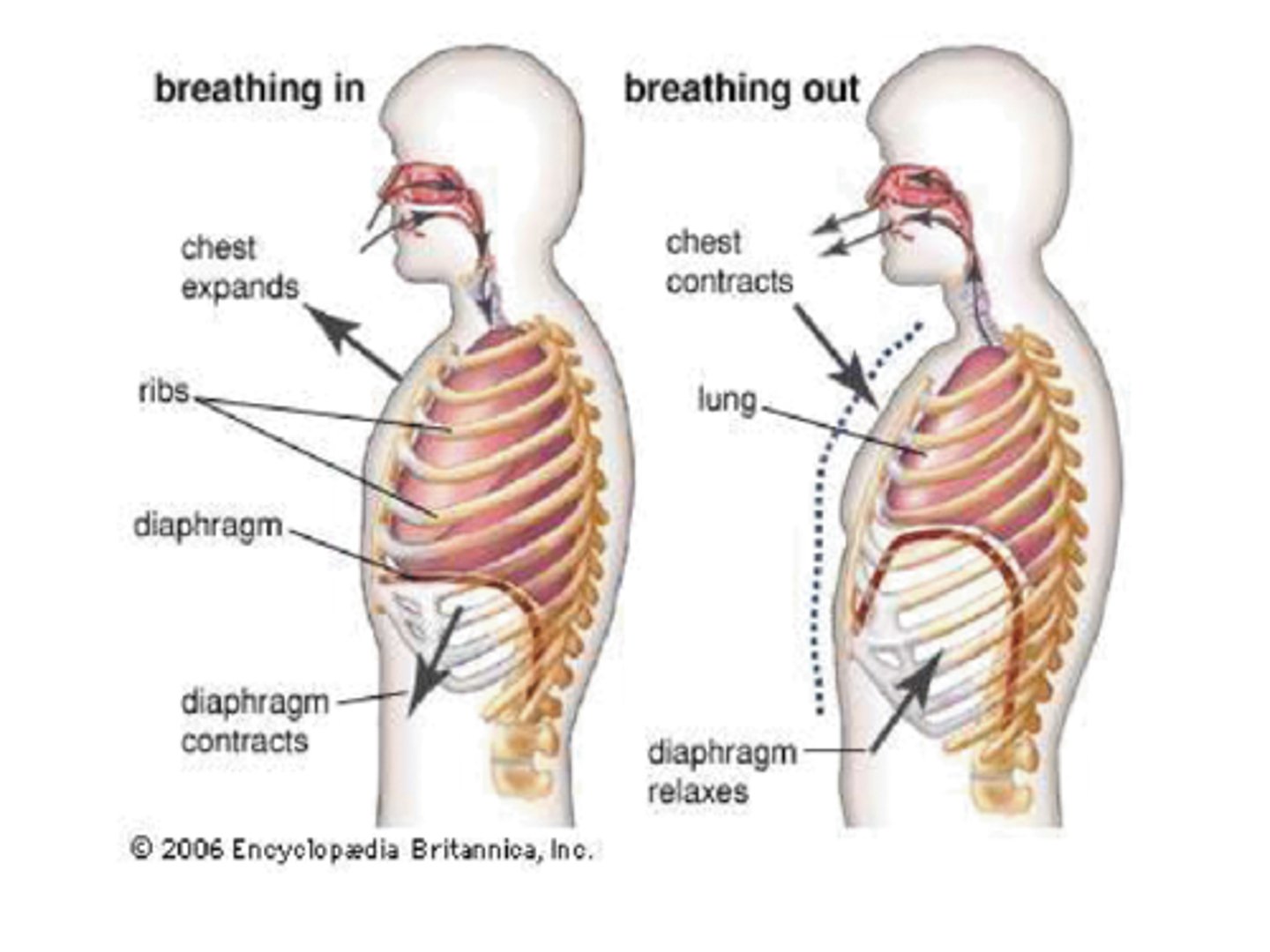
Pressure
Air flows from HIGH to LOW pressure
- Inspiration creates a partial vacuum
Intrapleural pressure
Pressure within the pleural space
- always negative pressure to keep lungs inflated
Atelectasis
lung collapse
- when air gets into the pleural space
Respiratory volumes
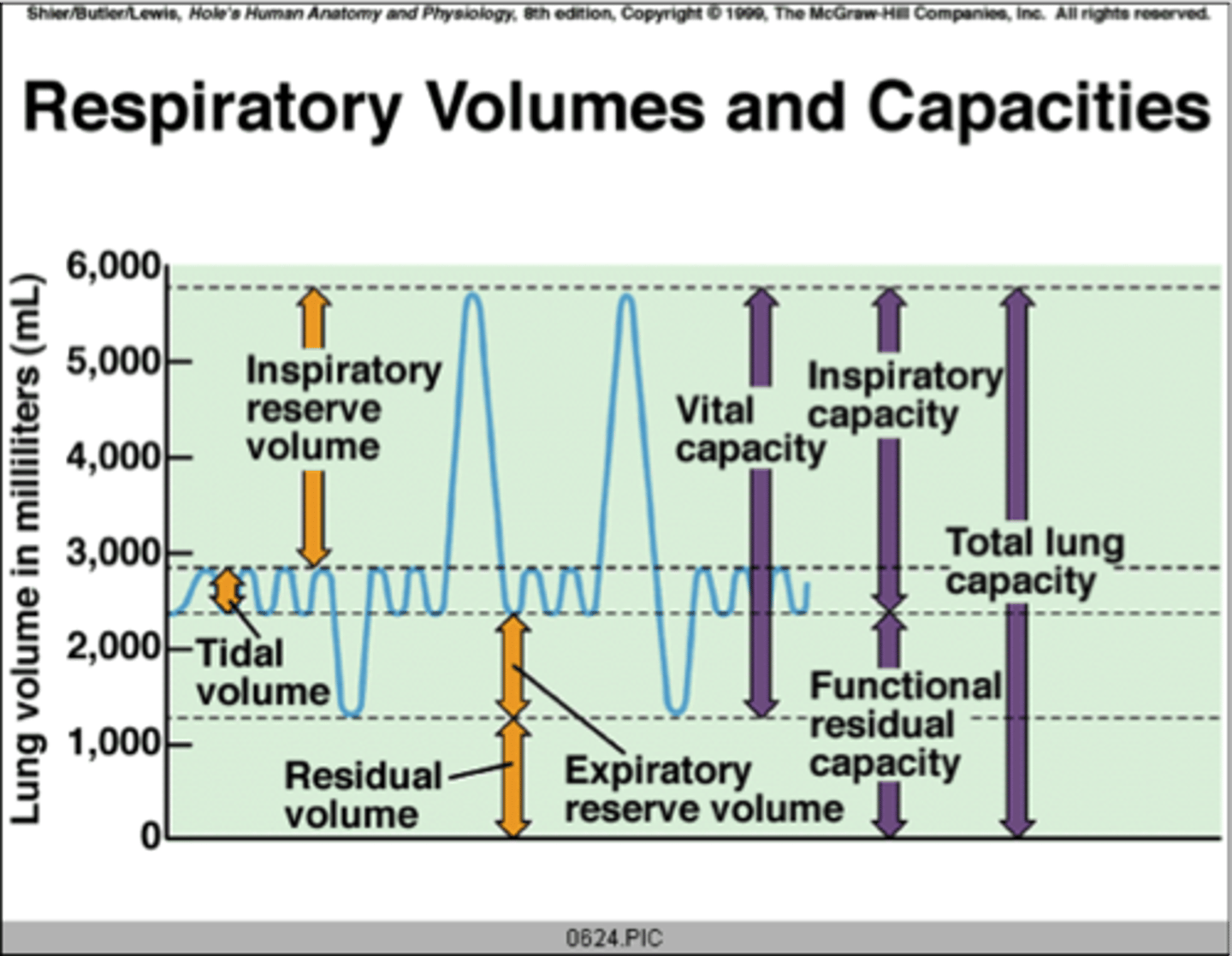
TV = Tidal volume
normal breathing
IRV = Inspiratory reserve volume
Forced inspiration
ERV = Expiratory reserve volume
forced expiration
RV = Residual volume
cannot be exhaled from the lungs
- allows for continuous gas exchange
- keeps alveoli open
VC = Vital capacity
Total exchangeable air
- TV + IRV + ERV
Characteristic of blood pH
Exercise/holding breath builds up carbon dioxide -> blood pH drops (more acidic)
- chemoreceptors sense blood pH drop
- Increases breathing to exhale carbon dioxide -> Blood pH returns to 7.4
Hyperpnea
Fast breathing
Apnea
Stopped Breathing
Normal respiration rate = eupnea
12-15 breaths per min
Medulla/Pons - controls breathing rhythm
Phrenic and intercostal nerves - trigger muscles
Cerebrospinal Fluid - senses CO2 levels and primary driver for detecting high CO2 as low pH (acidosis)
Aorta chemoreceptors - detect low O2 levels
Other body parts in respiratory system