CONGENITAL HEART DEFECTS
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
52 Terms
CONGENITAL HEART DEFECTS
1. Patent Ductus Arteriosus (PDA)
2. Atrial Septal Defect (ASD)
3. Ventricular Septal Defect (VSD)
4. Coarctation of the Aorta
5. Tetralogy of Fallot (TOF)
6. Transposition of the Great Vessels
Fetal & Postnatal Circulation
During gestation the lungs are nonfunctional, & fetal oxygenation occurs via the placenta.
• Key structures in fetal circulation include:
• FORAMEN OVALE. Is an opening between the atria that allows blood flow directly from right atrium to the left atrium.
• DUCTUS ARTERIOSUS: Is a conduit between the pulmonary artery & the aorta that shunts blood away from the pulmonary circulation
Overview of Congenital Heart Defect
• CHD are structural defects of the heart, great vessels of both that are presented from birth.
• Children w/ CHD are more likely to have associated defects: Transesophageal Fistula & chromosomal defects.
• CHD is second only to prematurity as a cause of death in the first year of life.
Etiology
• The exact cause is unknown (more than 90% of cases)
• Factors associated w/ increased incidence of CHD:
• Fetal & maternal infection (rubella)
• maternal alcoholism
• Maternal use of teratogenic drugs
• maternal age older than 40
Etiology 2
• maternal dietary deficiency
• Maternal insulin-dependent induced diabetes
• sibling w/ chd
• parent w/ chd
• A chromosomal abnormality such as Down syndrome
ACYANOTIC HEART DISEASE
1. Patent Ductus Arteriosus (PDA)
2. Atrial Septal Defect (ASD)
3. Ventricular Septal Defect (VSD)
4. Coarctation of Aorta (COA)
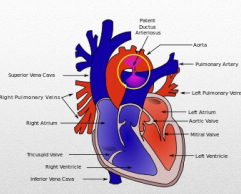
1. Patent Ductus Arteriosus (PDA)
• acyanotic
• There is failure of fetal ductus arteriosus to close completely after birth.
• After birth, ductus arteriosus must close/constrict to become only a ligament so as to reverse the blood flow to pulmonary artery.
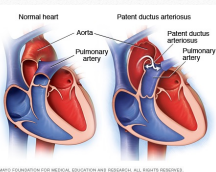
Hemodynamics PDA
Because of the opening between aorta & pulmonary artery, oxygenated blood to be delivered by aorta to the different parts of the body is diminished.
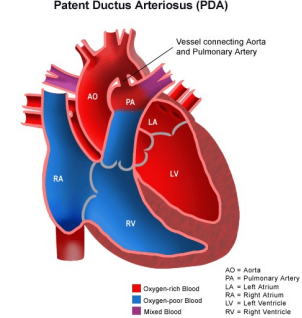

Laboratory & Diagnostic Tests PDA
• chest x ray
• ECG: usually normal but may show ventricle enlargement if the shunt is large
• echiocardiography
• Occasionally a cardiac catheterization may be necessary to assess lung blood pressures or amount of shunting through a PDA
Assessment Findings PDA
• T – achypnea
• C – ontinuous machinery murmur at the left upper sternal border
• H – epatosplenomegaly (enlargement of the liver & spleen)
• I – irritability
• P – oor feeding & weight gain
• S - sweating
Complications PDA
• Heart failure
• recurrent pneumonia
• Ineffective endocarditis
• pulmonary hypertension
• Pulmonary vascular disease
Medical Management PDA
• Diuretics – decreases excess lung fluid caused by increased blood flow
• Increased caloric concentration in infants feeding
• Indomethacin & Prostaglandin inhibitor – used to facilitate closure if PDA is noted immediately after birth
• prophylactic antibiotics
• Surgical ligation through a left thoracotomy
• closure of PDA
• In older children, a PDA can be closed in the cardiac catheterization lab with a device placed in the duct to occlude flow
Nursing Management PDA
• Assess cardiopulmonary/respiratory status.
• Monitor of patient weight, vital signs, pulse oximetry & intake/output
• raise head of bed
• Give high calorie, easy to digest foods
Atrial Septal Defect (ASD)
• Acyanotic
• Heart defect wherein atrial septal tissue does not fuse properly
• associated w/ down syndrome
Hemodynamics ASD
• Because of the opening between left and right atrium, oxygenated blood will go back to right atrium, back to right ventricle into pulmonary artery to the lungs for reoxygenation, so oxygenated blood that is supposed to be delivered into the different parts of the body is very much diminished.
Laboratory & Diagnostic Tests ASD
• ECG: reveals an enlarge right side of the heart & increased pulmonary circulation
-cardiac catherization
Assessment Findings ASD
Systolic ejection murmur maybe heard at the second intercostal space
Medical Management ASD
• Digoxin
• diuretics
• Direct closure of the defect w/ a patch or stitch (If the defect is 8mm or larger with evidence of increased pulmonary blood flow)
• fluid restriction
DIGOXIN
a medication derived from a digitalis plant that helps make the heart beat stronger and with a more regular rhythm. It is used to treat heart failure and atrial fibrillation
given for VSD and ASD
Ventricular Septal Defect (VSD)
Abnormal opening in the septum between two ventricles that allows blood to divert its flow between left & right ventricle.
• Associated w/ Down’s Syndrome, renal anomalies, prematurity & fetal alcohol syndrome
hemodynamics VSD
• Because of the opening between left & right ventricles, oxygenated blood will go back to right ventricles back to pulmonary artery into the lungs for re-oxygenation so oxygenated blood which is supposed to be delivered into different parts of the body is diminished.
Medical Management VSD
• Closure of VSD by age 6 months
• direct clsoure w/ patch or stitch
• Digoxin
• diuretics
• Prophylactic antibiotics
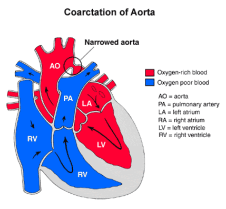
Coarctation of Aorta (COA)
• COA involves a localized narrowing of the aorta
hemodynamics COA
Because of the narrowing of aorta, the oxygenated blood which is supposed to be delivered to all part of the body is very much diminished
Laboratory & Diagnostic Tests COA
•ECG
• echocardiography
•Chest radiography may reveal an enlarge left side of the heart
Assessment Findings COA
• Weak or Absent femoral pulse – PATHOGNOMONIC SIGN
• BP higher in the upper extremities. Normally - systolic BP in lower extremities is 20-40 mmHg higher than the upper extremities because of the pull of gravity,
• Headache & epistaxis is common
• Pulse in the upper extremities will be rapid & bounding.
• Leg pain in exertion
• cold feet
• muscle spasm
• Pulse is weak, delayed or even absent
• Myocardial hypertrophy
• Weak or Absent femoral pulse –
PATHOGNOMONIC SIGN
• BP higher in the upper extremities
Normally - systolic BP in lower extremities is 20-40 mmHg higher than the upper extremities because of the pull of gravity,
Nursing Management COA
• Provide family teaching about treatment options.
• Surgical removal of stenotic area
• Grafting
• Non-surgical: BALLOON ANGIOPLASTY
• Provide preoperative & postoperative care
CYANOTIC HEART DISEASE
5. Tetralogy of Fallot (TOF)
CONGESTIVE HEART FAILURE
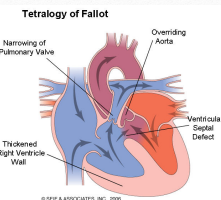
5. Tetralogy of Fallot (TOF)
• A combination of 4 cardiac defects:
• ventricle septal defect
• Right ventricular hypertrophy
• overriding of aorta
• Pulmonary artery stenosis
Hemodynamics TOF
Because of the very small pulmonary artery, unoxygenated bld cannot go to the lungs, resulting to accumulation of unoxygenated bld in the right ventricles thus building up the pressure in the right ventricles.
Because of the opening between the right & left ventricles, & increasing pressure in the right ventricles, the unoxygenated blood will go through the ventricular septal defects (right-to-left shunting) & enter the aorta because it is overriding the ventricular septal defect so that now the unoxygenated blood now is being delivered by the aorta to the different parts of the body
In an effort of right ventricle to push harder against the stenotic/small pulmonary artery so as to deliver more unoxygenated blood to the lungs, the right ventricle enlarges. There is little amount of unoxygenated blood that is able to go thru the small pulmonary artery; therefore there is also unoxygenated blood that is being oxygenated by the lungs. However, it is a very small amount, not enough to supply the whole body
Assessment Findings tof
• S – quatting to reduce shortness of breath
• C – yanotic or “blue” spell (Tet spell);
C – lubbing of digits
• A – Loud systolic murmur heard best along the left sternal border
• T – hrill at left sternal border
T – ransient cerebral ischemia
• E – vidence of growth retardation
• R – ight ventricular impulse & prominent inferior sternum
• D – ifficulty eating
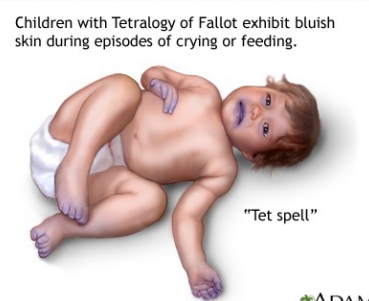
children with tetralogy of fallot have blue skin during crying or feeding
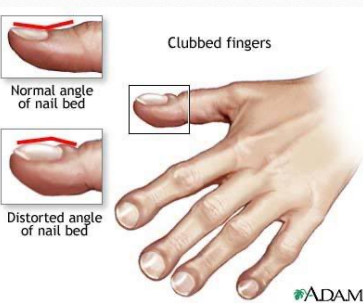
clubbed fingers, distorted angle of nail bed
Management TOF
Conservative
• adeuquate hydration
• Prevent recurrent infections
• Alleviate dyspnea by letting the child assume knee-chest position or squatting
• oxygen and morphine
• Do not allow child to cry for long periods of time
surgery TOF
palliative
corrective
Palliative:
• blalock-taussig procedure- left pulmonary artery is anastomosed to left subclavian artery.
Corrective
• open heart surgery– VSD & pulmonary stenosis are corrected, using hypothermia & heart-lung machine.
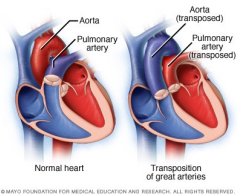
Transposition of Great Vessels (TGV)
• Rising of the aorta from the right ventricle, & pulmonary artery from the left ventricle, producing two noncommunicating circulatory system
Hemodynamics TGV
-Because the aorta is on the right side of the heart, the unoxygenated blood will now empty to the aorta & out into the general circulation
-Because pulmonary artery is now on the left side, the oxygenated blood will go back to the lungs for re-oxygenation, & cycle is repeated all over.
To sustain life, the child must have an associated defect.
Assessment Findings TGV
• C – yanosis from birth (dark, bluish skin due to deficient oxygenation of blood)
• A – gallop rhythm (heart)
• T – achycardia; T - achypnea
• C – ardiomegaly
• H – epatomegaly
• E – vidence of gallop rhythm
• D – iminished exercise tolerance; D – yspnea
• F – atigue
• M – urmurs of ASD, VSD, PDA
CONGESTIVE HEART FAILURE 4 questions
• Heart failure is severe circulatory congestion due to decreased myocardial contractility which results to heart’s inability to pump sufficient blood to meet the body’s need.
• Conditions that overwork the heart.
Causes CHF
• Existing disorder such as:
• Rheumatic fever
• kawasaki disease
• Infectious endocarditis
• Congenital Heart Defects
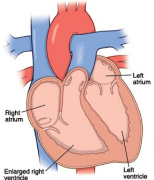
Right-sided Heart Failure CHF
• Right-sided heart failure occurs when the right ventricle is unable to pump enough blood into the pulmonic circulation.
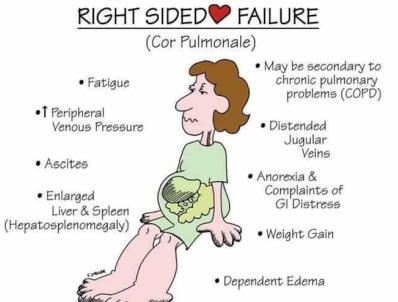
Assessment Findings RHF
• Hepatomegaly; abdominal pain
• Anorexia
•
• Diaphoresis
• Edema – late sign
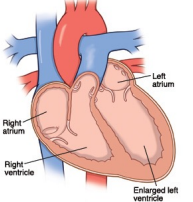
Left-sided Heart Failure
Left-sided heart failure occurs when the left ventricle is unable to pump enough blood into systemic circulation

Assessment Findings LHF
• Feeding difficulty
• pallor
• Dyspnea - because of pulmonary hypertension & edema, lung compliance is decreased.
• tACHYPNEA
Nursing Management
• Improve myocardial efficiency by giving digitalis.
• Reduce cardiac workload by reducing energy requirements
• Remove accumulated fluid
• Improve tissue oxygenation by oxygen administration
• Improve myocardial efficiency by giving digitalis.
• Not given if HR is below the minimum range of the particular age.
• Signs of digitalis toxicity:
GI (nausea, vomiting, anorexia, diarrhea);
CNS ( headache, lethargy, irritability); Cardiovascular (arrhythmias, cardiac failure)
• Reduce cardiac workload by reducing energy requirements
• Complete bed rest
• Orthopneic position
• Small frequent feedings
• Minimal handling
• Remove accumulated fluid
• Diuretics
• Low sodium diet
• Intake & output
• Weigh daily- use the same weighing scale at the same time each day