pancreatic and salivary glands
1/54
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
secretory glands of the GI tract do what
secrete mucous
secrete digestive enzymes usually produced by zymogens
secretory glands are stimulated by
direct contact stimulation by food
enteric nervous system of gut wall activation
tactile stimulation
chemical irritation
distension of gut wall
what type of glands are pancreas and major salivary glands
compound exocrine glands
lubricates and initiates breakdown of starch
what saliva does
neutralizes acid and completes intraluminal digestion of carbohydrates fats and proteins
pancreatic juice
pancreatic juice is rich in
bicarb
pancreatic exocrine digestive main enzymes and what they do
proteases digest protein
amylases digest carbs
lipases digest fat
secretory units of exocrine pancreas located where
within lobules, acinus and small intercalated duct
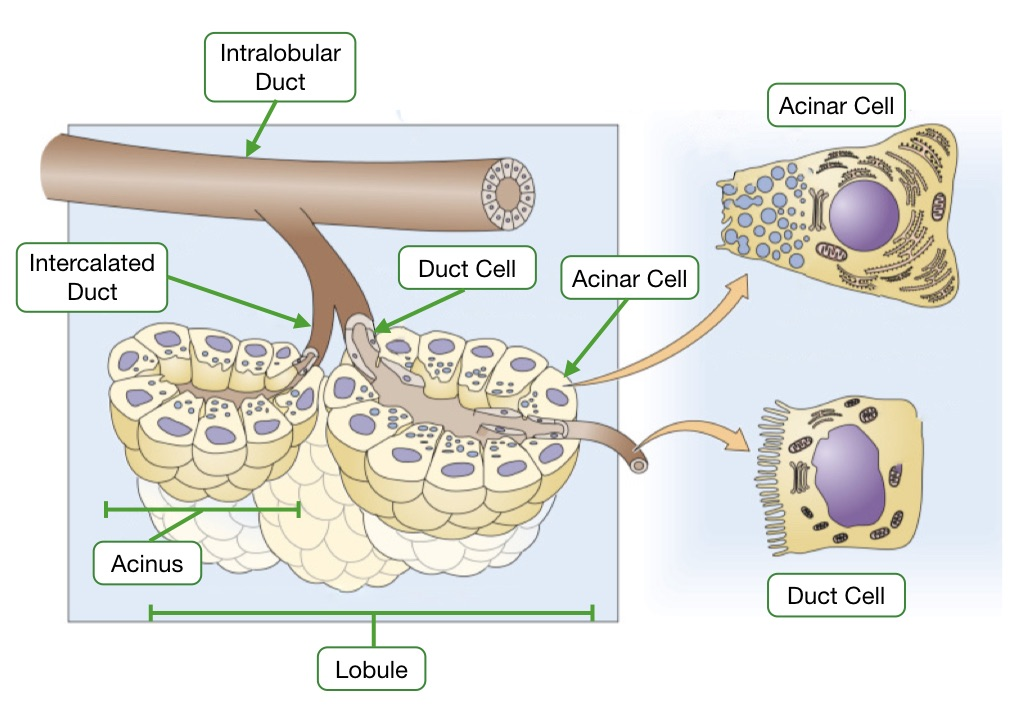
what cells synthesize and secrete proteins into lumen of pancreas
acinar cells
epithelial cells do what to secretions as they move along the duct
modify fluid and electrolyte composition
pancreatic juice is a composite of what two things
enzymes in isotonic solution from acinar cells
bicarb rich solution from pancreatic duct cells
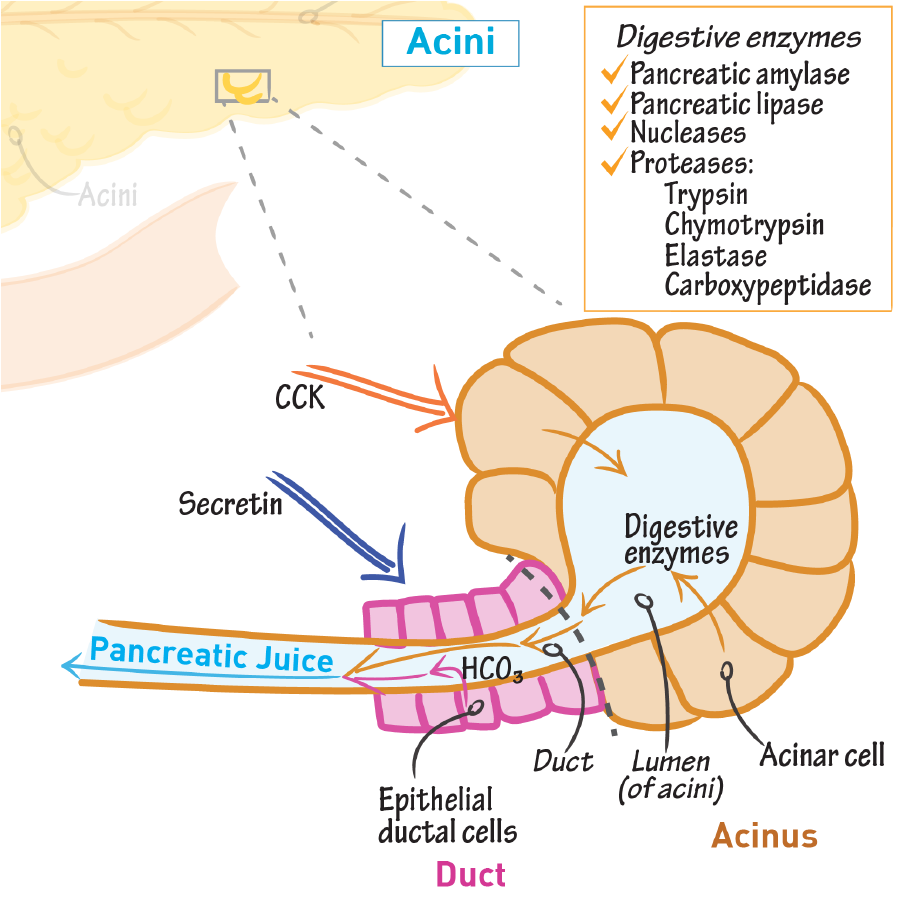
secretagogues of pancreatic acinar cells
CCK and ACh
also secretin (bicarb), vip, GRP
Both CCK and ACh stimulate the secretion of what in acinar cells
NaCl (via Cl- secretion)
NaK pump basal surface does what
creates inwardly directed Na gradient across basolateral membrane
NaKCl cotransporter on basolateral surface does what
produces net Cl- uptake which is driven by the Na gradient which is driven by the NaK pump
intracellular accumulation of Cl- due to NaK and NaKCl leads to what
electrochemical gradient driving Cl- secretion into lumen through apical membrane Cl- channels
this is stimulated by CCK and ACh
lumen becoming more negative because of Cl does what
drives Na into the lumen via the tight junctions, H2O follows
what cells secrete HCO rich fluid that alkalizes and hydrates protein rich primary secretions
pancreatic duct cells
what is responsible for recucling Cl back to the lumen
CFTR, cystic fibrosis transmembrane regulator
acinar cells made the lumen very Cl- which then the pancreatic duct cells are able to use the
Cl-/HCO3 exchanger which secretes HCO into lumen, but Cl MUST be present in the lumen for it to work
(so if there was a problem with acinar cells, or CFTR which sends the cl back, then the bicarb exchange wouldnt work)
what is the most important humoral regulator of ductal bicarb secretion
Secretin
how does secretin do its thang
activates adenyl cyclase
→ raises cAMP
→ protein kinase A
→ phosphorylates CFTR
loss of CFTR expression at plasma membrane
disrupts apical transport
decreased secretion of bicarb and water by ducts
→ thick protein ricj primary acinar secretions → block ducts and cause tissue destruction
maldigestion, fat in stool
how much pancreatic juice is produced every day
1.5 liters
during fasting, enzyme secretion does what
varies cyclically with MMC
ACh regulation of pancreatic secretion
from parasympathetic nerve endings
stimulates acinar cells to increase enzyme production and secretion
CCK regulation of pancreatic secretion
from I cells
acts on pancreatic acinar cells in fed state to increase secretion
stimulated by lipid and CCK releasing factors
secretin regulatino of pancreatic secretion
from s cells
stimulates bicarb
acts in concert with CCK ACh and others
three phases of pancreatic secretion
cephalic
gastric
intestinal
sight smell and taste of food does what
activates cephalic phase of pancreatic secretion
vagus nerve → Ach → digestive enzymes
presence of food in stomach does what
activates the gastric phase of pancreatic secretion
stomach distension → vagovagal gastropancreatic reflex → low levels of pancreatic secretion
chyme entering small intestine does what
stimulates the intestinal phase of pancreatic secretions
stim duodenal S cell by gastric acid bile acid and lipids
stim CCK release from duodenal cells by lipids
vagovagal enteropancreatic reflex, ACh stimulaiton
presence of what reduces pancreatic secretions
fat in distal end of the small intestine
peptide yy mediated most likely
what hormones may play a role in decreasing pancreatic secretions
somatostatin released from d cells
also likely glucagon from alpha cells
pancreatic secretions retained within the organ bc inflammation or obstruction
acute pacnreatitis
what is hyperstimulation pancreatitis
if acinar trypsin (protease) prematurely process to active form and retained in cell
symptoms of acute pancreatitis
severe abdominal pain, nausea and vomiting
may have fever, tachycardia, hypoxemia and hypotension
factors that cause acute pancreatitis
alcohol and gallstones
lipid metabolism disorders (hyperglyceridemia) → pancreatitis
principal salivary glands
parotid
submandibular
sublingual
tell me about the acinar cell populations of the salivary glands
two distinct populations
parotid: alpha amylase (ptylain)
sublingual/submandibular gland: mucin glycoproteins
what controls the salivary gland secretion
ANS
Ach for PNS and NE for SNS
acini secrete a primary secretion in saliva that contains what and is like what
it contains alpha amylase and or mucin
solution much like typical extracellular fluid
how is hypotonic salivar produced
salt reabsorption without water reabsorption in ducts
during max salivation, ionic reabosprtion is _____ due to ________
lower, high flow rate
sodium ions are _________ in from salivary ducts
reabsorbed (reduces concentration in saliva)
potassium ions are _________ into duct
secreted (increases concentration in saliva)
how is bicarb secreted in saliva
Cl-HCO3 exchanger (and CFTR recycles Cl to lumen)
role of saliva
prevent dehydration of oral mucosa and lubrication for chewing and swallowing food
oral hygiene
how is saliva important for oral hygiene
salivary flow washes away pathogenic bacteria
proteolytic enzymes in saliva attack bacteria
what is xerostomia
dry mouth
nervous regulation of salivary secretion
controlled mainly by the PNS
what nuclei are involved in PNS control of salivary secretion
superior and inferior salivatory nuclei in brainstem
taste stimuli activate nucleus and it acts on the glands
sympathetic can slight stimulate what
salivation
chronic progressive autoimmune disease that affects salivary secretion and eye duct secretion
sjogren syndrome
how does sjogren syndrome lead to its dry symptoms
it has antibodies that react with salivary glands that cause inflammation and net decrease in secretion function
(might involve SLC26A6, bicarb cl exchanger)
→ dry mouth and eyes
→ hard to taste, chew, swallow, speak, and have enlarged parotid gland