Maternal Newborn exam 1 guide
1/168
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
169 Terms
Where in the fallopian tubes would fertilization occur most often?
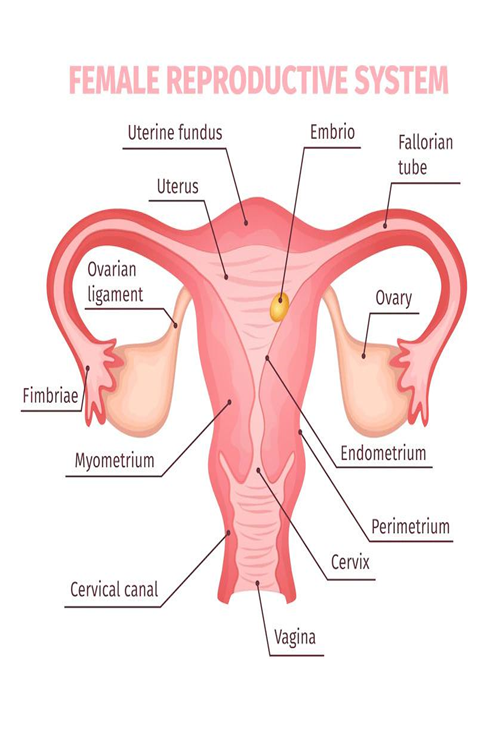
Ampulla- wide part near the fimbriae and ovary
What is the difference between the true and false pelvis?
The false pelvis supports the abdominal organs, has no role in delivery
The true pelvis is the bony passageway that the baby must pass through during birth.
What is colostrum? What cells make them?
First milk, before the regular milk comes in, liquid gold, yellow colored, antibody filled.
Acini
When is a good time to recommend a breast self exam considering menstruation?
Physiologic alterations in breast size reach minimal level 5 to 7 days after menstruation stops to avoid feeling false bumps or mass
What is menarche?
a first menstrual period, usually between 9-16, avg 28 days (21-35 days)
What does the Hypothalamic-Pituitary Cycle stimulate and release?
The hypothalamus controls the cycle by secreting GnRH (gonadotropin-releasing hormone).
GnRH stimulates the anterior pituitary gland to release two key hormones:
FSH (Follicle-Stimulating Hormone): Stimulates ovarian follicle growth.
LH (Luteinizing Hormone): Triggers ovulation and corpus luteum formation
What is the ovarian cycle?
Follicular (follicles develops, estrogen rises), U(Surge of LH causes ovulation (egg release), and luteal phase (Corpus luteum secretes progesterone to support potential
Endometrial Cycle
Menstrual Phase – Shedding of endometrium (day 1–5).
Proliferative Phase – Endometrium rebuilds under estrogen (pre-ovulation).
Secretory Phase – Endometrium thickens, becomes receptive (post-ovulation, progesterone driven).
Ischemic Phase – If no pregnancy, hormone levels drop; blood supply decreases, leading to menstruation.
What is Mittelschmerz?
mid-cycle ovulatory pain, usually presents unilaterally can be similar to appendicitis
What is a prostaglandin?
oxygenated fatty acids, but they act like hormones in the body, important to control contractions of smooth muscles in uterus, fallopian tubes,
Pitocin
a synthetic version of the hormone oxytocin, commonly used to induce or strengthen uterine contractions during labor, and to control postpartum bleeding
what can untreated STI manifest in women?
primarily chlamydia and gonorrhea can develop pelvic inflammatory disease, possibly resulting in infertility
What is Pre-Exposure Prophylaxis ?
PrEP- daily oral antiretroviral medication, used for someone at high risk for HIV exposure, effective when taken consistently
What is Post-Exposure Prophylaxis?
PEP- emergency antiretroviral after potential exposure, must be started within 72 hours, used for high risk exposures of HIV
What is chlamydia? What are some S/S?
very common STI in US, silent but harmful, S/S vaginal discharge, dysuria, intermenstrual or post coital pain, pelvic or lower abdomen pain
What can happen if you don’t treat chlamydia?
you can develop pelvic inflammatory disease, ectopic pregnancy, acute salpingitis
Ectopic inflammatory disease
When the sperm develops in the fallopian tube and can rupture the tube
what is put on babies eyes after birth, and what does it do?
Erythromycin ointment- protects newborn eyes from STIs
What does a child usually pick up if they have chlamydia?
conjunctivitis and pneumonia
What is a the treatment for non pregnant adults with chlamydia vs pregnent patients?
non pregnant- doxycycline
pregnant- azithromycin
What does Gonorrhea do to the body?
Premature rupture of membranes (amniotic fluid sac), preterm birth, it is a cervical infection that may progress to fallopian tub inflammation
What can you use to treat gonorrhea?
ceftriaxone IM, Concomitant Chlamydia Treatment (if chlamydia infection not ruled out), azithro if preg doxy if not, ABSTAIN FROM INTERCOURSE FOR 7 DAYS AFTER TREATMENT
Syphillis, what is a huge warning?
primary- 5-90 days after exposure, secondary- rash (palms/soles), lymphadenopathy, condylomata lata, systemic symptoms, latent- no symp, tertiary- organ failure
Untreated maternal syphilis can cross the placenta at any stage of pregnancy
What is the only treatment of syphilis?
penicillin G
what are some S/S of syphillis?
hepatosplenomegaly, jaundice, snuffles (copious nasal discharge), later complications hearing loss, dental abnormalities, neurologic damage
What is Pelvic Inflammatory Disease (PID)? s/s?
infection of the upper urinary tract, uterus, fallopian tubes, ovaries, surrounding pelvic structures
S/S- fever above 100.9, abnormal cervical or vaginal discharge, elevated ESR and CRP, positive test of N. Gonorrhoeae or chlamydia T. one of three lower abdominal tenderness, adnexal tenderness, cervical motion tenderness
How do you treat Pelvic Inflammatory Disease (PID)?
broad-spectrum antibiotic, infection determines line of care
What is the most common Viral STI?
HPV
Condylomata acuminata
genital warts from HPV 6 and 11
What types of HPV are responsible for the majority of cervical cancers?
HPV types 16 and 18
What are the two types of herpes simplex virus?
HSV-1 → usually transmitted nonsexually; more common in oral infections (gingivostomatitis, cold sores).
HSV-2 → usually transmitted sexually; more common in genital infections. Results in painful, recurrent genital ulcers.
What is the usual medications for Herpes Simplex Virus?
Acyclovir, with also valacyclovir, famciclovir
If the mom has active herpes lesions, what should be the priority for birth
transvaginal birth is contraindicated, contamination of the warts is the highest risk of contracting HSV
What are the types of hepatitis?
ABCDE
What is hep A?
fecal oral route, flu-like symptoms, nausea anorexia, fever, right upper quadrant pain, HAV vaccine avaibale, IVIG can provide post exposure protection.
What is Hep B?
blood and body fluid transmission(perinatal, sexual contact, IV drug use) often asymptomatic, if pregnant you should be screened
What is Hep C?
liver infection with no vaccine
What is HIV?
Severe depression of the cellular immune system associated with HIV infection characterizes AIDS
What is the CDC recommendation for treatment?
ART therapy antiretroviral therapy and AZT
Over-the-Counter (OTC) Antifungal Medications
lotrimazole (Lotrimin, Gyne-Lotrimin)
Miconazole (Monistat)
Tioconazole (Vagistat)
finish whole treatment
Trichomoniasis
Inflammation of the vagina and/or vulva Caused by Trichomonas vaginalis - an anaerobic one-celled protozoan with characteristic flagellae
NAAT test recommended: most sensitive
Speculum examination with wet mount: not as accurate
TORCH infections
all of these infections can cross the placenta can cause major concerns
Toxoplasmosis
Other infections (e.g., hepatitis, HIV)
Rubella virus
Cytomegalovirus
Herpes simplex virus (HSV)
What is Spinnbarkeit?
stretchy stringy quality of cervical mucus, promotes pregnancy
What should female patients know who use a diaphragm or cervical cap?
after 6 weeks post partum it must be refitted (also after massive weight loss)
What is a spermicide available in the US
Nonoxynol-9 (N-9) decreases sperm motility, alone or with barrier, has a 20% chance to fail
How do oral contraceptives work?
Prevent ovulation, thicken cervical mucus to block sperm, thin endometrium to reduce implantation
What oral contraceptive can be used while lactating?
Mini pill- contains no estrogen, which can effect milk supply
What are the two types of contraceptive injectable?
combined estrogen-progesterone and just progestin only
What is the most common contraceptive injection?
Depo-Provera (medroxyprogesterone acetate – DMPA) or Depo-SubQ Provera 104 (subcutaneous version)
given 12-13 weeks or about 3 months
“Depo”!
How do you use the transdermal or vaginal ring contraceptive system?
A hormonal patch or ring that releases estrogen and progestin through the skin.
Worn on the skin for 3 weeks, with one week off to allow for a withdrawal bleed
What is a implantable progestins?
nexplanon
What are some contraindications to combined oral contraceptive use?
History of thromboembolic disorders, or smoking more than 15 cigarettes a day above the age of 35, cerebrovascular disease, uncontrolled hypertension
How does a IUD work?
t shaped arms that block the cervix, can be hormonal (thicken mucus, prevent sperm movement, thins endometrium) or copper based (Copper is toxic to sperm)
What is the copper based IUD?
Paraguard copper T 380A- effective up to 10 years
When can you use emergency contraceptives?
as soon as possible but can be effective up to 5 days or 120 hours after intercourse
What is the prescription emergency contraceptive?
Ulipristal acetate, effective up to 5 days
What is the most effective emergency contraception?
Copper ParaGard IUD, must be placed within 5 days of intercourse, but it is the most effective form of emergency contraception
What are the permanent sterilization procedures for female patients?
Tubal occlusion- electrocoagulation and /or ligation (tying) considered a permanent methods, can try to reverse with mixed results
What are the permanent sterilization procedures for men?
vasectomy- surgical interruption of a mans vas deferens, can be reserved with mixed results
What is LAM?
Lactational Amenorrhea Method (LAM): Breastfeeding as Contraception
Needs to meet three criteria
1) Infant : Baby is younger than 6 months
2) Exclusive Breastfeeding: Baby receives only breast milk
Frequent feeding (day and night)
Minimal supplementation
3) No Return of Menses: Mother has not resumed menstruation
Before what week of pregnancy can an intentional abortion occur?
20 weeks of gestation
What is and when can you do a medical abortion?
12 weeks (first trimester) Methotrexate and misoprostol
Mifepristone and misoprostol
Most common first-trimester abortion?
Aspiration- 1st trimester (vacuum or suction curettage) in clinic setting
What kind of abortion is done past the first trimester?
Second trimester abortions are usually dilation and evacuation. can be done at any point up to 20 weeks of gestation, usually 13-16 weeks
Capacitation
Physiologic change that prepares sperm for fertilization
Removes protective coating on sperm head
Releases enzymes that allow sperm to penetrate the ovum
what is Oogenesis (Female)?
Produces egg cells (ova).
Occurs in the ovaries.
Results in one functional ovum and three smaller non-functional cells (polar bodies) from a single germ cell.
What are the two protective lays of the ovum?
Zona Pellucida
-Thick inner acellular layer
-Protects the ovum and regulates sperm entry
Corona Radiata
-Outer layer of elongated cells
-Surrounds and nourishes the ovum
What is another name for the outer third layer of the fallopian tube?
Ampulla
What happens on day 3 of fertilzation to implantation timeline?
A solid ball of 16 cells develop
What happens during the blastocyst stage?
hollow structures form like the embryoblast- embryo, and Trophoblast → placenta
What happens on the implantation stage
The blastocyst attaches to the uterine lining (endometrium), which becomes the decidua, chorionic villia form as finger like projections to form fetal placenta
what is a Decidua
It is the endometrium or uterine lining after implantation
What is the Ovum period?
moment of conception to day 14
What is the embryonic period?
day 15 to 8 weeks after conception, most critical time for development of the organ system and main external features, very susceptible to teratogen
What is the fetal period?
9 weeks until the end of pregnancy
What are the three layers of the embryonic disk?
ectoderm- upper layer- floor of amniotic cavity, mesoderm- middle, endoderm, lower layer- roof
Umbilical cord information to know
“AVA” two arteries one vein, also has wharton’s jelly which surrounds vessels to prevent compression, rare for any vessel malformation
What are the two membranes that protect the developing fetus?
Chorion- placenta formation, amnion- forms the amniotic sac and directly surrounds the fetus
Oligohydramnios?
too little amniotic fluid, can be linked to kidney problems in baby, less than 300 mL
Polyhydramnios
too much amniotic fluid, usually indicative of congenital GI problems, more than 2 L of fluid
What does amniotic fluid do? (7 things)
maintains fetal temp, physically protects, allows fetal movement and musculoskeletal development, fluid and electrolyte balance, repository for fetal waste, antibacterial properties, and allows sound transmission
What is Human Placental Lactogen (hPL)?
Alters maternal metabolism to provide glucose for the fetus
What is a general viability age range for the fetus to turn to a baby?
20 weeks and hopefully above 350, 400, or 500 g depending on state
Vernix caseosa?
white cheesy coating
Pulmonary surfactants?
Helps line interior of alveoli and makes lungs more pliable and able to breathe, usually peaked at 32
L/S ratio
tests for lung maturity using amniotic fluid samples.
Lecithin-Sphingomyelin
What do we need to give babies vitamin K?
Coagulation factors are not synthesized in the fetal liver, they need Vitamin K to be able to clot
How and what does the neurologic system develop with the embryo and fetus?
Originates from ectoderm
Fetal senses: taste by 16 weeks, sound response by 24 weeks, sight by 26 weeks
What is lanugo?
very fine hairs on the baby
24 week pregnant and after i dropped some books my baby jolted, why?
they are able to hear sound by 24 weeks
Dizygotic
Multiple mature ova resulting in two zygotes
Monozygotic
one ova that divides, same sex and often identical
What is the best birth control to offer a woman who is a smoker, over 35, and has migraines with auras?
progestin only BC, no combined or estrogen patch
How long is the first trimester? What is going on in it?
0 – 13 weeks, 6 days
organ development, hCG rising, Nausea and vomiting occurs commonly, uterus is still a pelvic organ
how long is the second trimester? What's going on?
14 weeks, 0 days – 27 weeks, 6 days
fetal growth, quickens around 16-20 weeks and feels comfortable, sometimes around 12 weeks the uterus rises into the abdominal cavity and dextrorotation (right rotation)
How long is the third trimester? Whats going on?
28 weeks, 0 days – 40 weeks, 6 days
rapid growth, rising discomfort on back and SOB due to weight of fetus, preparation of birth
Where should the fundal height for a 12-14 week pregnant woman
uterus palpable above symphysis pubis
Where should the fundal height for a 20-22 week pregnancy?
level of the umbilicus
What happens to the fundal height during the 38-40 week period?
lightning or decent of the fetus into the pelvis
What is a Uterine Soufflé?
Soft, blowing sound
Heard with a stethoscope
Caused by increased blood flow in uterine vessels
Not synchronous with fetal heart rate