MMCP 2 - Ischemic Heart Disease and Cardiac Arrhythmias (Dr. Stephens)
1/192
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
193 Terms
- A 56 yo male presents to your office for a NPE
- Pt reports that they have not seen a dentist in the past couple of year but have no acute complaints
- You obtain the following history:
- C.C.: "I haven't seen a dentist and need a check up"
- HPI: Pt reports that due to "life getting in the way" he has not seen a dentist for the last 2 years. He reports that he has not experienced any significant pain or other concerns since his last visit. Overall, he is not concerned with his dental health and is hoping to get "back on track"
- PMH: Hypertension, Hyperlipidemia
- PSH: Denies
- Family Hx: Mom- Myocardial infarction (@ age 55) Dad- Myocardial infarction (@age 60)
- Social Hx: "Occasional" EtOH, 1 pack/day cigarette smoker, denies recreational drugs
- Medications: Atorvastatin, Lisinopril
- Allergies: NKDA
- ROS: Pt reports weight gain over the last 5 years (Current BMI: 39)
What should we be thinking about?
Atherosclerosis

What are two other names for Atorvastatin and what is its drug class?
- Lipitor, Statin
- HMG-CoA reductase inhibitor (used for cholesterol)
when you talk about things that lead to acute fatal cardiac events (cardiac arrest, etc.) _________ is going to comprise the majority of or is going to be present at least in the majority of those cases.
coronary artery disease
What drug class is Lisinopril?
ACE inhibitor
What condition?
- Inflammatory disorder affecting the lining of arteries, development of plaque in the walls of arteries leads to narrowing of vessel lumen.
- Narrowing of vessel lumen decreases the capacity for blood flow and oxygen delivery
- In coronary arteries this can lead to limitation of oxygen supply to the myocardium
atherosclerosis
in atherosclerosis, narrowing of vessel lumen decreases the capacity for ______ and _________
blood flow; oxygen delivery
atherosclerosis in coronary arteries can lead to limitation of oxygen supply to the ________
myocardium
What is the leading cause of death in the US?
Cardiovascular disease
What comprises the majority of cardiac arrests?
Coronary Artery Disease
A dental practice with 2000 patients will statistically have at least ______ with IHD
100
what are some modifiable risk factors for atherosclerosis?
a. hypertension
b. cigarette smoking
c. physical inactivity
d. obesity, insulin resistance, diabetes metillus
e. diet rich in simple sugars and starches
f. hyperlipidemia
g. mental stress depression
i. infection and systemic inflammation
what are some non-modifiable risk factors for atherosclerosis?
a. family history of cardiovascular disease
b. old age
c. male gender
d. genetic hyperlipidemia
What plays a key role in all stages of atherosclerotic disease?
inflammation
What is a physiological cause of endothelial damage (that can in turn cause atherosclerosis)?
disturbances in blood flow at bifurcations of vessels
What are some pathological causes of endothelial damage (that can in turn cause atherosclerosis)? (6)
- Hyperlipidemia
- Oxidative stress
- Glycation end products in diabetes
- Irritants in tobacco smoke
- Immune complexes and infection
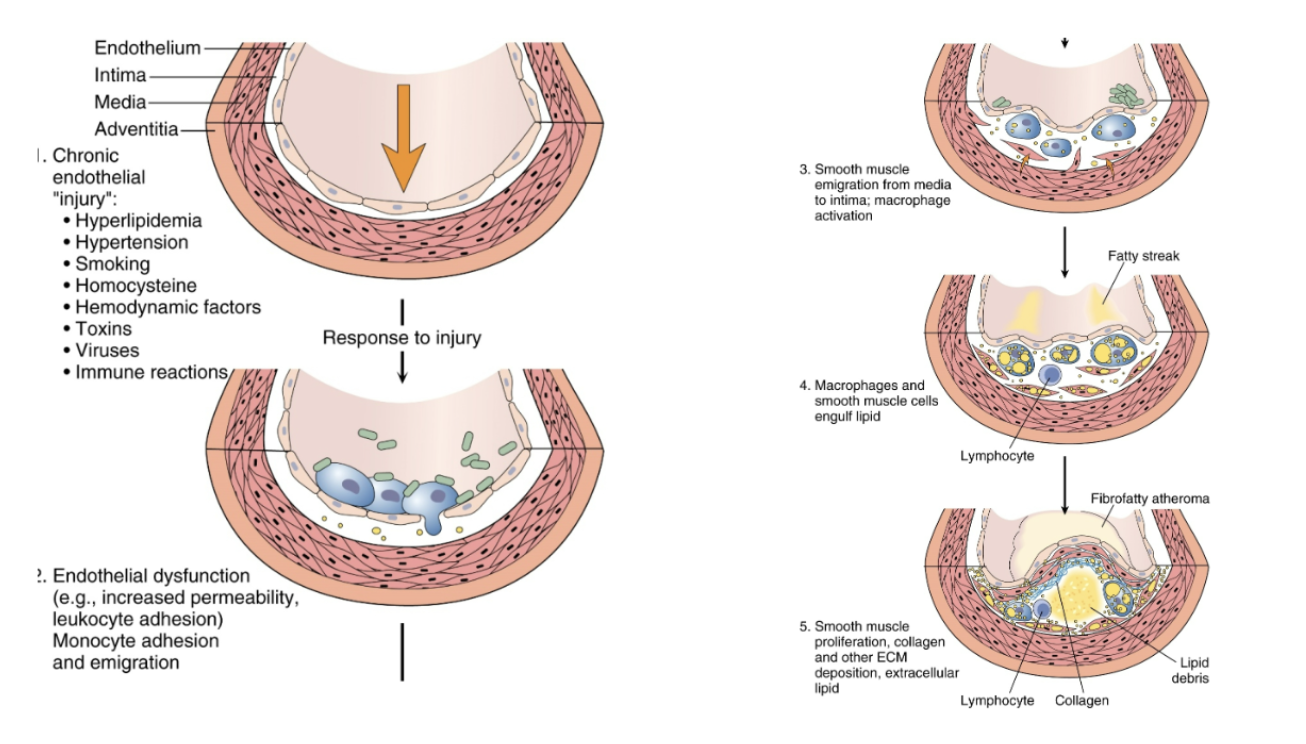
In atherosclerosis, there is endothelial damage. How does this endothelial damage then lead to the development of atherosclerosis?
Monocyte adherence to site of injury:
- Promoted by pathologic factors (not seen in healthy endothelium)
- Monocytes migrate to vessel intima and become macrophages
- Macrophages engulf lipids --> Foam cells --> Fatty streak
- Inflammatory response to foam cells --> proliferation of smooth muscle and collagen --> fibrous cap
- Further inflammatory response --> thinning of fibrous cap and rupture
What factor initiates the earliest step in atherosclerosis?
Endothelial dysfunction/damage
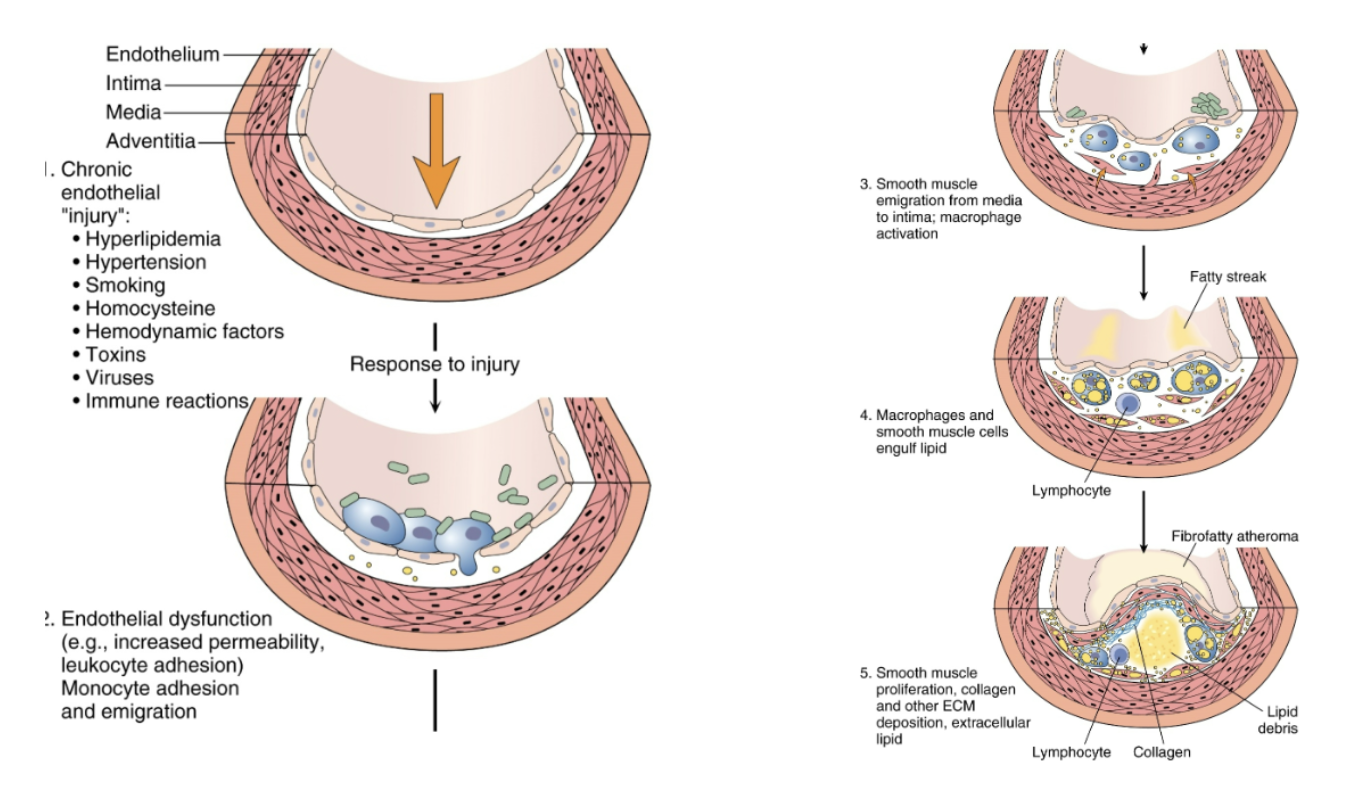
Once a fatty streak is formed, inflammatory cells respond and proliferate smooth muscle and collagen, what is formed from this?
fibrous cap
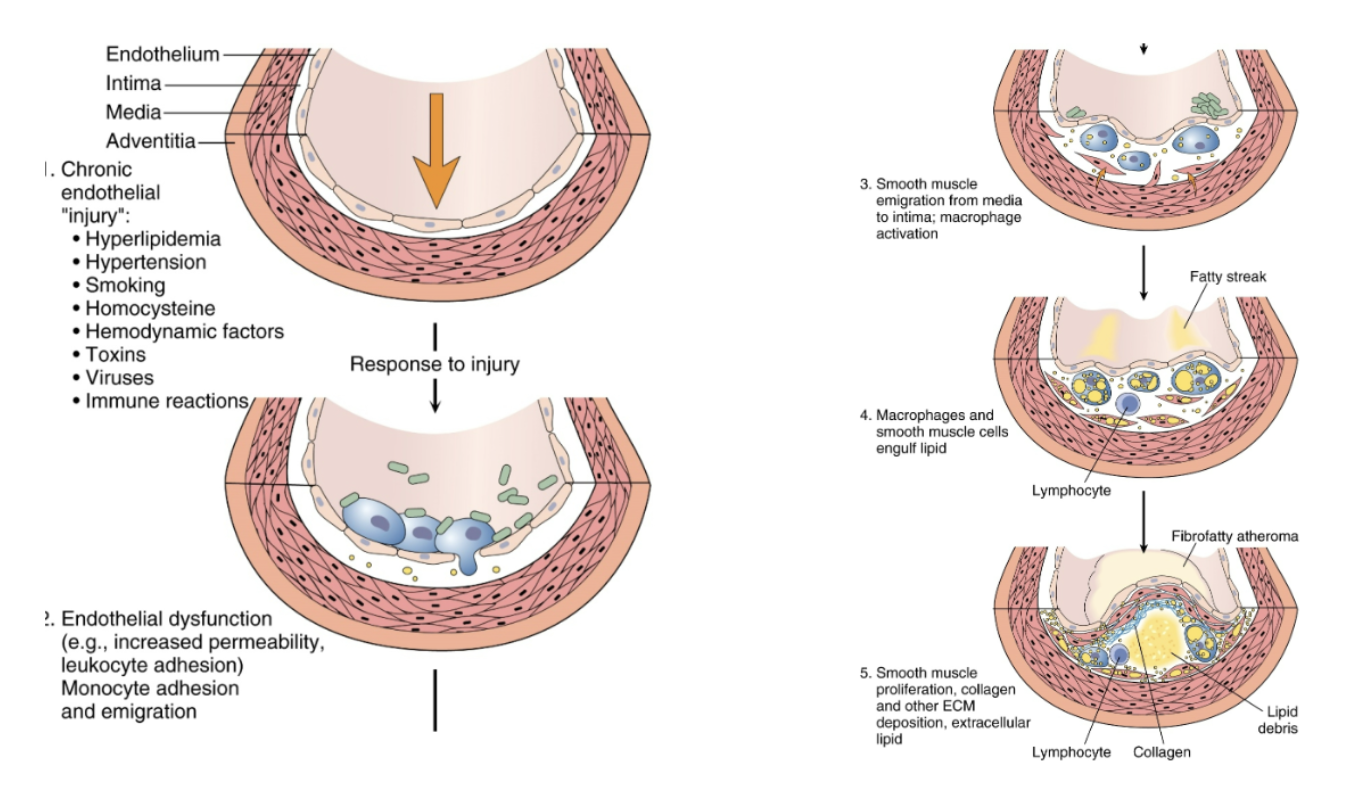
If there is further inflammatory response to a fibrous cap, leading to a thinning of the fibrous cap, what can happen?
fibrous cap rupture (leads to thrombus formation or embolism)
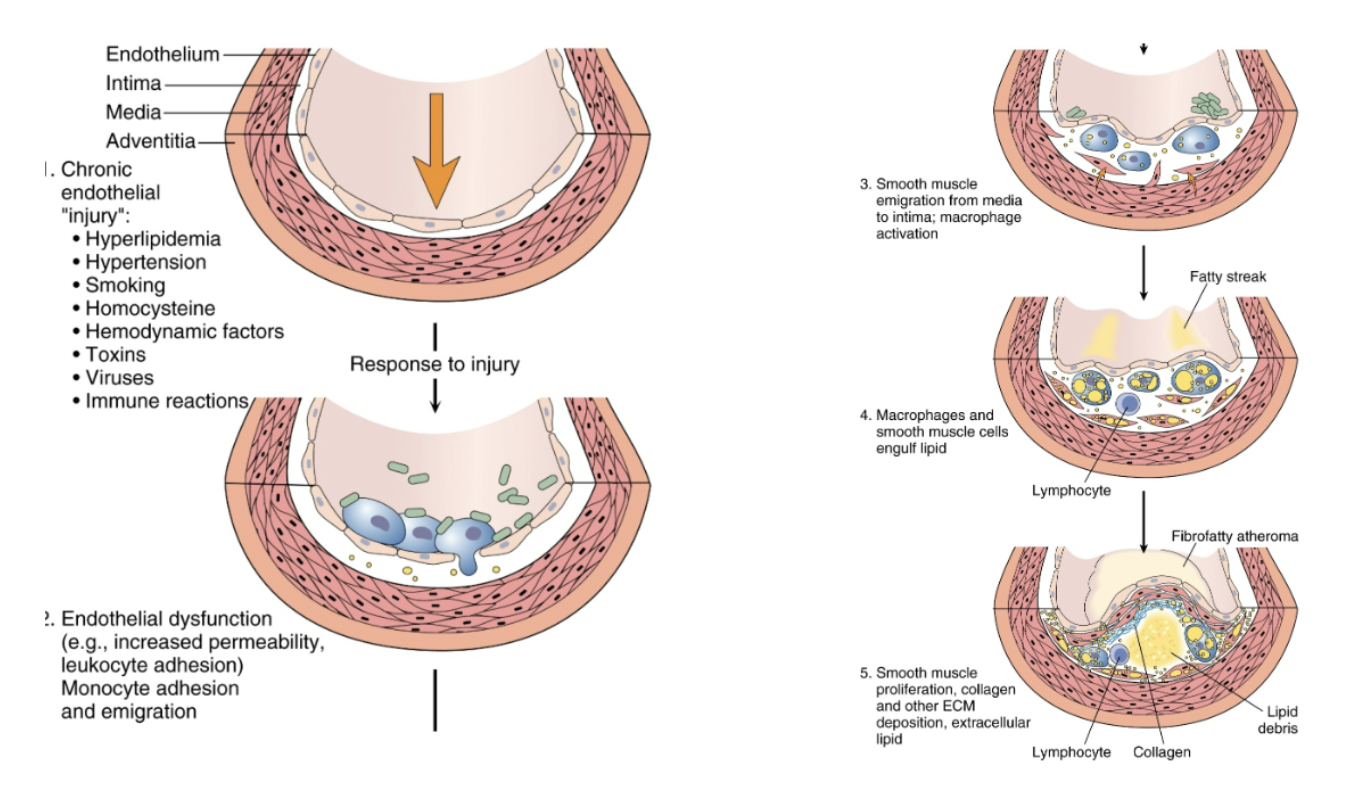
If the fibrous cap in atherosclerosis ruptures, what happens?
thrombus formation
Thrombus formation is a result of circulating blood coming into contact with what?
tissue factor (TF)
There may be a limitation in oxygen supply due to the coronary artery reaching ____% stenosis due to plaque growth
75%
Most symptomatic ischemia is due to disruption or fracture of what?
plaque
Weakening of the fibrous cap occurs due to what?
various inflammatory products
t/f: most symptomatic ischemia is due to the disruption of, or the fracture of the plaque, not necessarily that it just grows so large that it occludes the vessel.
true
What four sites are most commonly affected by atherosclerotic plaques?
- Brain
- Aorta
- Peripheral arteries
- Heart
In which site does atherosclerotic plaque lead to vascular dementia?
Brain
What is the most common site of atherosclerotic plaques in the heart?
proximal left anterior descending artery
If a patient with atherosclerosis has an intact plaque, flow limitation occurs and this is known as what type of angina?
stable angina
if a patient with atherosclerosis has a ruptured plaque, what type of angina is this?
acute or unstable clinical picture (unstable angina, MI, sudden death)
Pt Case:
What is the patient taking each med for?
CC: haven't seen a dentist and need a check-up
HPI: has not seen dentist for 2 years, no significant pain or concerns
PMH: hypertension, hyperlipidemia
PSH: denies
Family Hx: mother- MI at age 55, father- MI at age 60
Social Hx: occasional alcohol, 1 pack of cigarettes per day
Meds: atorvastatin, lisinopril
BMI: 39
Atorvastatin-cholesterol (HMG CoA reductase inhibitor)
Lisinopril - hypertension (ACE inhibitor)
Pt Case:
CC: haven't seen a dentist and need a check-up
HPI: has not seen dentist for 2 years, no significant pain or concerns
PMH: hypertension, hyperlipidemia
PSH: denies
Family Hx: mother- MI at age 55, father- MI at age 60
Social Hx: occasional alcohol, 1 pack of cigarettes per day
Meds: atorvastatin, lisinopril
BMI: 39
What are some pertinent findings?
- MI in both parents
- Tobacco use
- BMI
Pt Case:
CC: haven't seen a dentist and need a check-up
HPI: has not seen dentist for 2 years, no significant pain or concerns
PMH: hypertension, hyperlipidemia
PSH: denies
Family Hx: mother- MI at age 55, father- MI at age 60
Social Hx: occasional alcohol, 1 pack of cigarettes per day
Meds: atorvastatin, lisinopril
BMI: 39
What are some treatment considerations?
- Call cardiologist/medical consultation
- Talk about smoking cessation strategies
- Ask about respiratory, hypertension, or any chest pain
Pt Case:
68-year-old female for yearly recall
HPI: no pain, no dental symptoms
PMH: hypertension, diabetes type 2, chest pain on exertion
PSH: bilateral knee replacements 5 years ago
Social Hx: 1-2 glasses of wine per night
Meds: Nitroglycerin 0.4mg sublingual PRN chest pain, atenolol 25 mg PO
Q day, Metformin 500 mg PO Q12hr
Allergies: Penicillin
ROS: Per HPI
What should we be thinking?
Stable angina
Pt Case:
68-year-old female for yearly recall
HPI: no pain, no dental symptoms
PMH: hypertension, diabetes type 2, chest pain on exertion
PSH: bilateral knee replacements 5 years ago
Social Hx: 1-2 glasses of wine per night
Meds: Nitroglycerin 0.4mg sublingual PRN chest pain, atenolol 25 mg PO
Q day, Metformin 500 mg PO Q12hr
Allergies: Penicillin
ROS: Per HPI
What are some treatment considerations?
- Anesthesia (epi)
- If symptoms present with increased heart rate
- Bleeding control
What condition?
- Sensation of aching, heavy, squeezing pressure, or tightness in the midchest region that may radiate into the shoulder, left or right arm, neck, or lower jaw
Angina Pectoris
can angina pectoris occur without chest pain?
rarely but yes
how is angina pectoris classified?
stable or unstable
how is the feeling of angina pectoris often described?
- "Crushing substernal chest pain"
A patient presents with Angina Pectoris. How long would their symptoms last?
5-15 min
how is angina pectoris relieved?
nitroglycerin administration
What condition?
- Uncommon variant that occurs at rest due to vasospasm, not atherosclerotic disease
Prinzmetal angina (common in women)
what demographic groups are most likely to have myocardial infarctions present atypically?
elderlies and women (more likely to see things like tingling in the fingers or toes, pain in the back, numbness, etc.)
if a patient does respond, if their chest pain does respond to nitroglycerin, then it probably is ______
angina (not an myocardial infarction since MI is irreversible necrosis of heart muscle)
what is the difference between angina and myocardial infarction?
angina (stable or unstable) = reversible ischemia to the heart (heart is not getting enough blood flow or oxygen to supply the demand of the heart,)
myocardial infarction = irreversible necrosis of cardiac muscle
t/f: if a pt responds to nitroglycerin and their chest pain goes away, it is a good sign to continue with treatment and send patient home.
FALSE. patient must go to hospital every single time to rule out definitively that they do not have an MI
What drug class is Atenolol?
beta blocker
Metformin is used in what conditions?
type 2 diabetes
In a patient with stable angina, is the atherosclerotic plaque in tact or ruptured?
in tact
(stable angina is caused by myocardial ischemia, because the plaque is causing stenosis of the vessel)
Stable angina is most often precipitated by what?
exertion
(because when under exertion, oxygen demand for heart will increase but oxygen supply is limited by decreased lumen size)
What has better prognosis, stable or unstable angina?
stable (relatively good prognosis)
what causes stable angina?
myocardial ischemia
stable angina is differentiated from unstable angina based on…?
predictability of symptoms
ID type of angina:
- Reproducing, unchanging, consistent overtime
- Most often precipitated by exertion
- May be associated with eating or stress
- Relatively good prognosis
stable
stable angina may be associated with what factors?
eating or stress
Unstable Angina and Myocardial Infarction are both considered to be part of what syndrome?
Acute coronary syndrome
In unstable angina, there is a physical disruption or fracture of a vulnerable atherosclerotic plaque. What happens when arterial blood is exposed to the lipid core of the plaque?
contact between blood, tissue factor, and collagen leads to platelet aggregation/adhesion -> coagulation cascade -> clot/thrombus formation

Clot/thrombus formation with rapid expansion of the lesion leading to compromise or complete blockage of blood flow to myocardium occurs in what type of angina?
unstable angina

What conditions can precipitate or worsen stable angina and should be identified and treated?
- Anemia
- Obesity
- Hyperthyroidism
- Sleep apnea
What are some interventions to help manage patients with stable angina?
- Behavior modification/lifestyle intervention (weight loss, exercise)
- Pharmacologic management (nitrates, beta-blockers, calcium channel blockers, antiplatelet agents)
- Revascularization (percutanous transluminal coronary angioplasty with stenting, coronary artery bypass grafting)

What are some pharmacological management considerations we should make for patients with stable angina pectoris?
- Nitrates
- Beta blockers
- CCBs
- Antiplatelets agents
How does nitroglycerin work to manage angina symptoms?
Primary pharmacological agent = Vasodilator (Decreased cardiac preload and after load --> decreases oxygen demand)

How is nitroglycerin usually administered?
- Sublingual tablet (also comes in spray, ointments, transdermal patches)

T/F: Nitroglycerin can treat angina
False (reduces symptoms, does not alter underlying CAD)

with nitroglycerin, the patient's blood pressure should be at least ___/___ if you're gonna give it.
90/60
what are 2 absolute contraindications to using nitroglycerin?
cannot give patients who have taken Viagra or Cialis in the last 48 hours (will lead to profound hypotension that can be life threatening)
How do beta blockers work to treat angina?
Decrease heart rate and contractility --> Decreased oxygen demand

how do calcium channel blockers work to treat angina?
Decrease intracellular calcium --> vasodilation and decreased contractility and HR

how do ACE inhibitors and ARBs work to treat angina?
antihypertensive effects

Why are antiplatelet medications (like aspirin) used as a tx for unstable angina?
Regular use of aspirin decreases occurrence of fatal and non fatal MI in patients with unstable angina

All of the following are examples of what drug class?
- Verapamil
- Diltiazem
- Amlodipine
- Nifedipine
Calcium channel blockers
After a patient has a stent placed or an acute MI, what drugs are commonly used?
anti platelets (like aspirin, clopidogrel, etc)

What type of medications are:
- Aspirin
- Clopidogrel (Plavix)
- Ticagrelor (Brilinta)
antiplatelet medications

______ may be used instead of or in combination with aspirin. It is especially common in patients after stent placement or acute MI
Clopidogrel (Plavix)

If a patient has a D0150 appointment with you on the 3rd floor and then you send them to the 8th floor for a consult, will the 8th floor accept your medical history?
No, everyone has to take their own history
A 67 year old male is referred from the emergency clinic to the oral surgery clinic at a dental school for extraction of #3 and #19 due to decay and infection. Pt history per emergency clinic note:
C.C.: My teeth hurt
HPI: Pt presents with pain and infection at #3 and #19. He states that he was referred by an outside dentist for extraction
PMH: Pt reports that he has no conditions that would affect his dental treatment
Meds: Pt takes two medications that he does not remember the name of
Allergies: NKDA
Exam: Swelling & redness at #3 and #19
Pt consented for extraction of #3 and #19 with LA
- Anesthetized with 8 carpules of 2% lidocaine with epi 1:100K
- Pt was very anxious during appt
- After final injection of LA pt reported substernal chest pain, diaphoresis, and markedly increased anxiety
- Procedure was stopped and pt reported similar symptoms to heart attack a few years ago
What was the critical error?
Terrible history --> ALWAYS need to take your own history
t/f: Medical history is critical to the ability to both provide safe routine care and to respond to medical emergencies
true
All of the following are true EXCEPT:
A) It is our responsibility to educate our patients on why it is important to fully understand their medical history
B) At TUSDM each clinic is an individual treatment site
C) Always take your own history
D) You can provide safe care without medical history
D) You can provide safe care without medical history
Why is myocardial infarction irreversible?
Significant coronary ischemia --> myocardial necrosis/ infarction
Myocardial Infarction is _________ to ruptured plaque/ thrombus
Secondary
T/F: Both stable and unstable angina are reversible
true (no death of cells)
Ventricular fibrillation (and pulseless V-tach) is an arrythmia that can result from ___________. Life threatening event leading to cardiac arrest
Myocardial Infarction
describe the continuum of atherosclerotic diseases
angina → myocardial infarction → cardiac arrest rhythms → cardiac arrest
what 2 things help distinguish myocardial infarction from angina?
duration of symptom (MI usually lasts > 15 min w increased severity)
response to nitroglycerin or rest (MI does NOT respond)
Patient presents with crushing substernal chest pain with radiation to shoulder, arm, neck, mandible and teeth. They tell you that their symptoms have been present for about 25 minutes. Will the administration of nitroglycerin help?
No, this is a myocardial infarction which does not respond to nitroglycerin
>15 min
women experiencing myocardial infarction present less often with chest pain. what other symptoms are more common in women?
fatigue, dyspnea, GERD (nonspecific)
what are some additional symptoms of myocardial infarction beside chest pain?
- - Cough
- - Shortness of breath
- - Diaphoresis
- - Dizziness
- - Syncope
- - Fatigue
- - Palpitations
Why doesn't MI respond to nitroglycerin?
Because in MI an emboli has gotten lodged in a vessel. If you use a vasodilator it will only move farther down
Why does angina respond to nitroglycerin?
This is a plaque based process and so if their symptoms are happening becuase the vessel is narrower (stenosis) then by using a vasodilator you will allow blood to pass the area and therefore relieve symptoms temporarily
what is myocardial infarction diagnosis primarily based on?
serum cardiac enzymes and EKG + Symptoms

diagnositic cardiac enzymes of MI include…?
- - Troponins (most specific and sensitive)
- - Creatinine Kinase
- - Myoglobin
which cardiac enzyme is most specific and sensitive AND is a product of cardiac sarcomere breakdown?
how long after MI onset can it be first detected?
troponin; 2 hours
Approximately what proportion of patients with confirmed acute myocardial infarction present without chest pain (silent MIs)?
1/3
What ECG findings meets diagnostic criteria for acute myocardial infarction?
- New or preseumed new significant ST segment T-wave changes or new left bundle branch block
- Development of pathological Q waves on ECG
STEMI stands for __________
ST elevation myocardial infarction
(complete blockage of flow and profound ischemia)
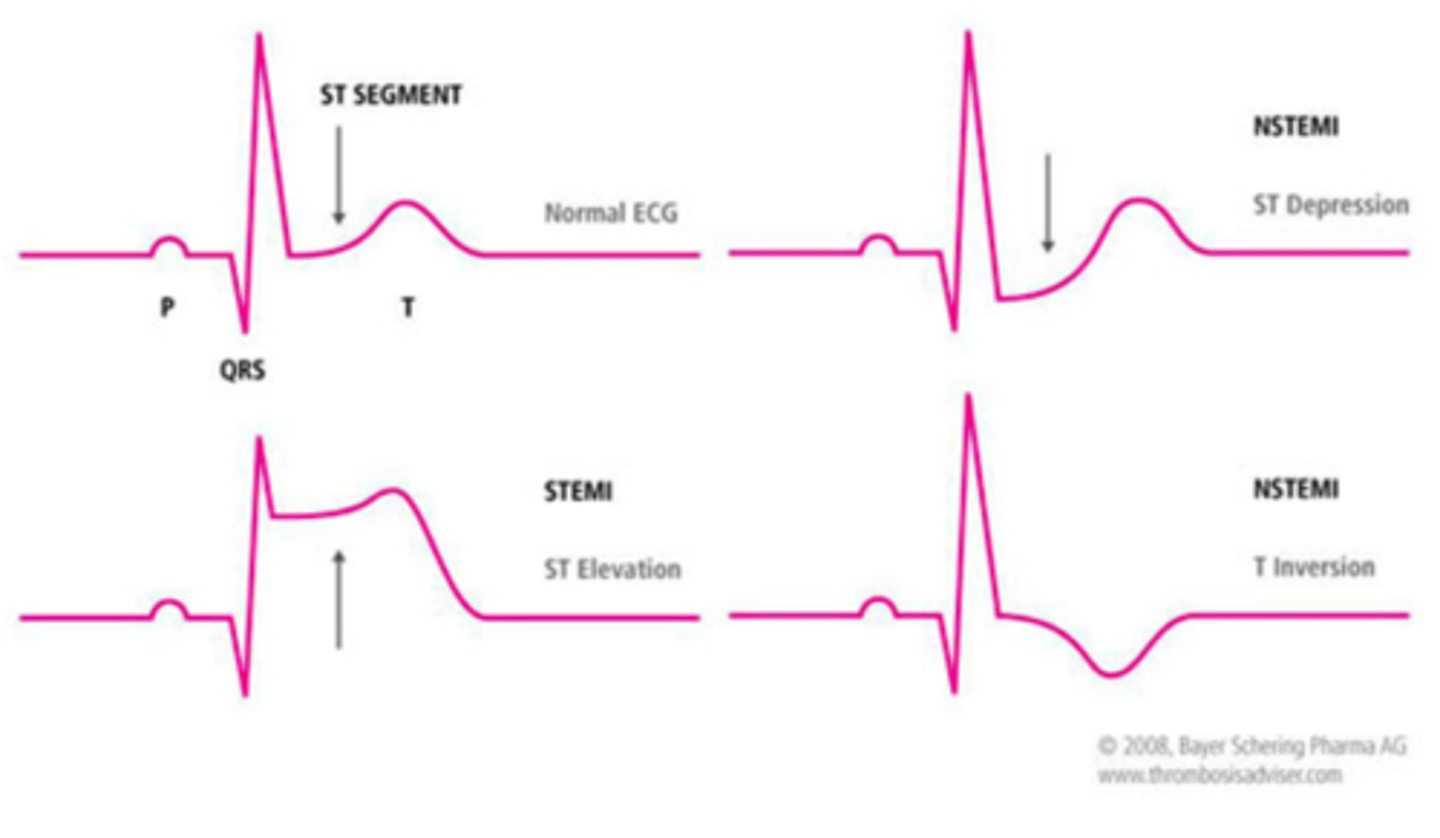
NSTEMI stands for __________
non-ST elevation myocardial infarction
(partial blockage of flow)
Which is worse: a STEMI or NSTEMI?
STEMI
What are your immediate actions if your patient is in your chair and suffering from MI? (3)
- Activate EMS/BLS protocol
- Administer oxygen, aspirin, nitroglycerin if indicated
- AED if necessary
For what type of MI would you use early fibrinolytic therapy (<3hrs) like streptokinase?
STEMI
What are some methods of revascularizatoin that may be used when treating a MI (3)
- Percutaneous coronary angioplasty
- Stents (bare metal vs drug eluting stents)
- Coronary artery bypass grafting (CABG)
