Lecture 26
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
Proximal tubule
§ Most of the solute and water reabsorption
Proximal tubule also carries out secretion
Loop of Henle
Descending limb
§ Ascending limb
§ Distal tubule
Reabsorption completed for most solutes
Collecting duct
Drains multiple nephrons
Carries urine to renal pelvis
Describe the lumen or differences in epithelium of the proximal tubule
microvila on proximal side
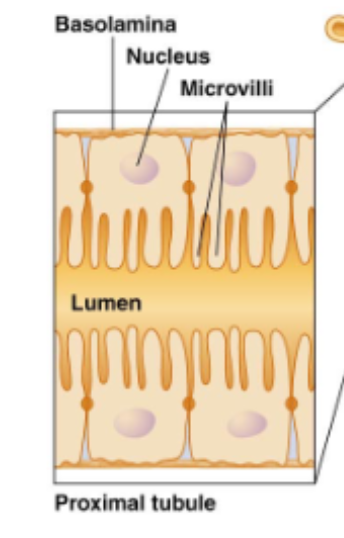
Describe the lumen or differences in epithelium of the descending limb
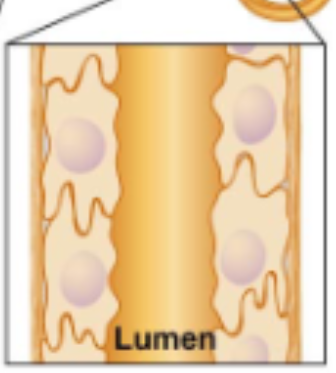
Describe the lumen or differences in epithelium of the ascending limb
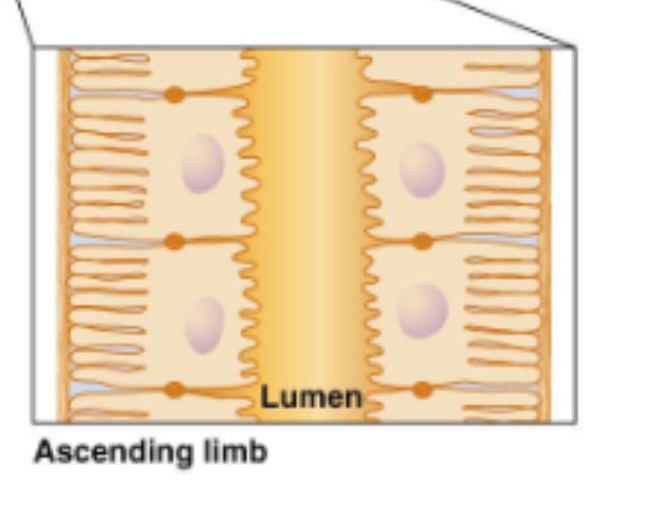
Describe the lumen or differences in epithelium of the collecting duct
One side no villa one side villa
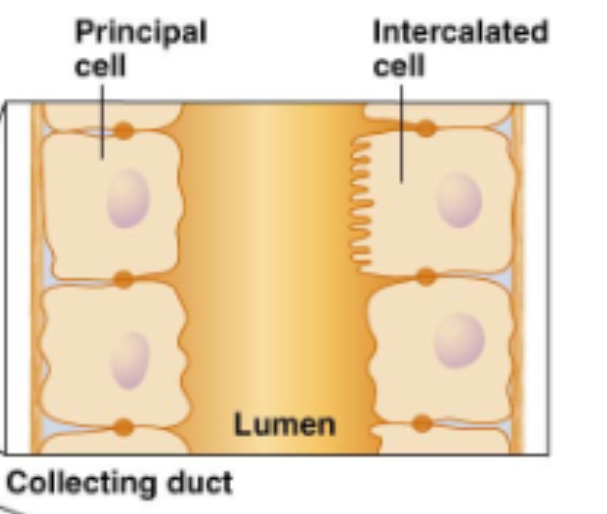
what are the 4 processes of urine production
filtration, reabsorption, secretion, excretion
Filtration
§ Filtrate of blood formed at glomerulus
§ Reabsorption
§ Specific molecules in the filtrate
removed
Most water and salt in primary urine reabsorbed
using transport proteins and energy
Each zone of the nephron has transporters for
specific solutes
§ Secretion
§ Specific molecules added to the filtrate
§ Excretion
§ Urine is excreted from the body
What is Primary Urine
Initial filtrate filtered in Bowman’s capsule that is
isosmotic to blood
formed during reabsorption
Rate of reabsorption is limited by
number of transporters
renal Threshold is
Concentration of a specific solute that will overwhelm
reabsorptive capacity
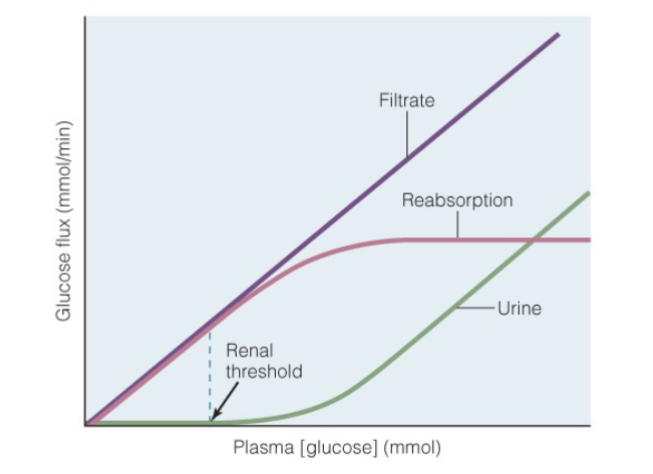
What happens during reabsorption in proximal tubule
Many solutes reabsorbed by Na+ cotransport
Water follows by osmosis
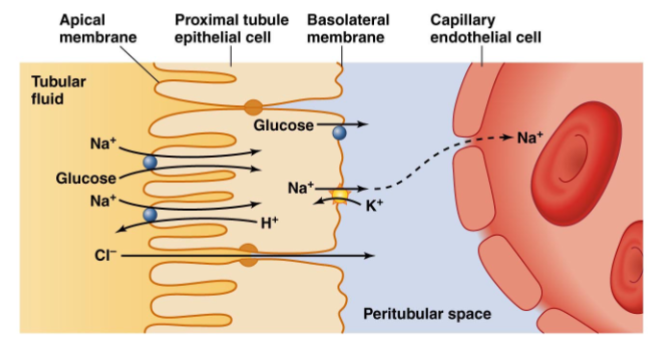
How is glucose reabsorbed
secondary active transport
Reabsorbed molecules taken up by the blood
The secretion process involves
Molecules removed from blood and transported into the filtrate
Molecules secreted include K+, NH4+, H+, pharmaceuticals, and water-soluble vitamins
Requires transport proteins and energy
Ion and Water Transport in the Loop of Henle
Descending limb is permeable to water
Ascending limb is impermeable to water
Reabsorbed ions accumulate in interstitial fluid
What happens because Descending limb is permeable to water
Water is reabsorbed
§ Volume of primary urine decreases
§ Primary urine becomes more concentrated
What happens because Ascending limb is impermeable to water
Ions are reabsorbed
Primary urine becomes dilute
What happens as Reabsorbed ions accumulate in interstitial fluid
An osmotic gradient created in the medulla
The loop of henle is a….
Concurrent multiplier
Transport in the Distal Tubule
Distal tubule can reabsorb salts and water
Distal tubule can secrete potassium
Transport function of distal tubule affected by hormones
Parathormone increases Ca2+ reabsorption
Aldosteron increases K+ secretion
Process of Excretion
After urine is produced, it leaves kidney and enters urinary bladder via ureters
Urine temporarily stored in bladder
Urine leaves bladder via urethra
Sphincters of smooth muscle control flow of urine out
of bladder
Opening and closing of sphincters controlled by a
spinal cord reflex arc (micturition reflex) and can be
influenced by voluntary controls
Urine concentration is dependent on
Osmotic concentration of final urine depends on permeability (aquaporins) of the collecting duct,
Regulated by vasopressin (AVP)
Water concentration in impermeable parts
Water not reabsorbed from collecting duct
Dilute urine (formed in ascending limb) excreted
Water concentration in permeable parts
Water reabsorbed from collecting duct
Concentrated urine (formed in collecting duct) excreted
How is urinary function regulated
Hormones and Dietary factors
What hormones regulate urinary function
Steroid hormones
For example, aldosterone
Slow response
Peptide hormones
For example, vasopressin
Rapid response
What dietary factors regulate urinary function
Diuretics
Stimulate excretion of water
Antidiurectis
Reduce excretion of water
Regulators of GFR
Hormones
Vasopressin (antidiuretic hormone, ADH)
Renin-Angiotensin-Aldosterone (RAA)
pathway
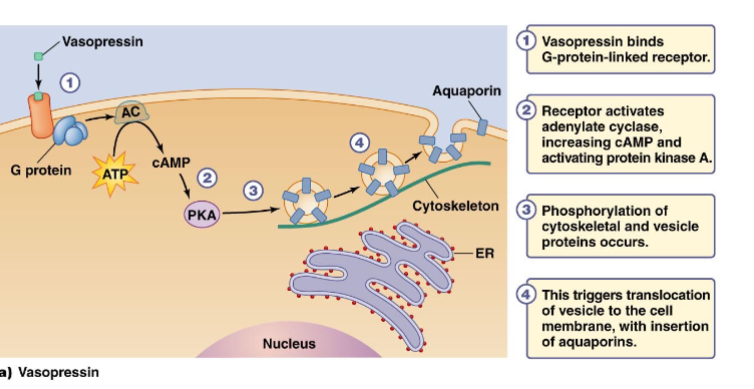
What does vasopressin do
Increase cell permeability
Describe Vasopressin Process
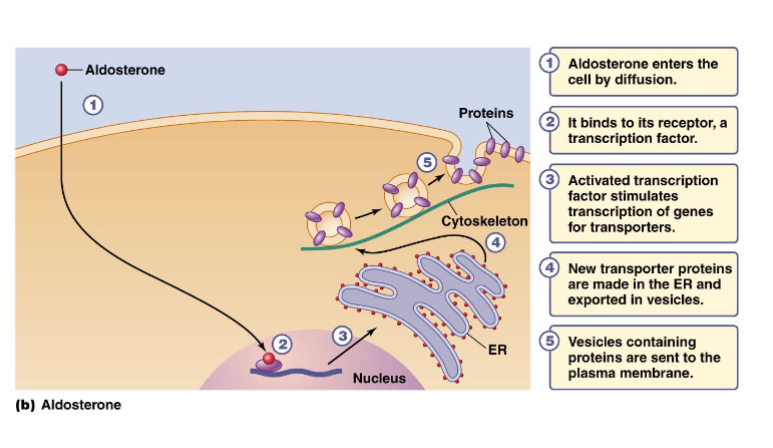
What does aldosterone do
Stimulates Na+ Reabsorption
Process of aldosterone
Juxtaglomerular cells
secrete enzyme renin
3 ways renin is secreted
Baroreceptors in juxtaglomerular cells release renin in response to low blood pressure
Sympathetic neurons in cardiovascular control center of medulla oblongata trigger renin secretion in response to low BP
Macula densa cells in distal tubule respond to decreases in flow by releasing a paracrine signal that induces juxtaglomerular cells to release renin
When is renin secreted
When blood pressure or GFR lower than normal
What does Renin do
converts angiotensinogen to angiotensin I
Angiotensin converting enzyme (ACE) on epithelia of blood vessels converts angiotensin I to angiotensin II
Angiotensinogen an inactive protein in plasma
What does Angiotensin II do
Causes synthesis and release of aldosterone from adrenal cortex
Steroid hormone
Targets cells in distal tubule and collecting duct
Stimulates Na+ and water reabsorption from urine
Enhances K+ excretion
Also stimulated by increases in circulating K
How does Renin-Angiotensin-Aldosterone Pathway control blood pressure
Angiotensin II a vasoconstrictor Raises blood pressure by increasing resistance
Aldosterone increases Na+ (and water) retention
Raises blood pressure by increasing blood volume
Visualize the feedback loop of AAP
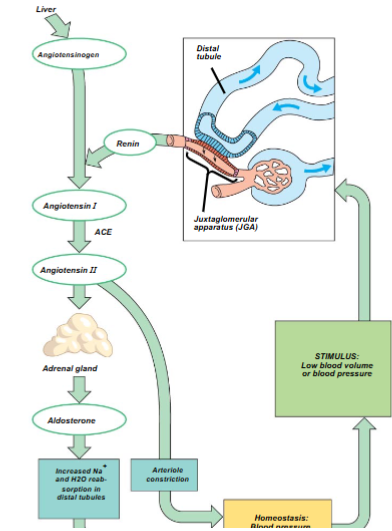
What do ACE Inhibitors do
↓ Angiotensin II
Vasodilation (blood vessels relax)
↓ Aldosterone → ↓ water retention