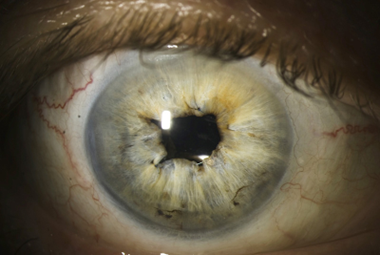
pupil assessment
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
define what the pupil is and what it is controlled by (3)
•Pupil is an opening in the centre of the iris, controlled by the sphincter and dilator muscles - reciprocal relationship between the 2 to ensure pupils are working correctly.
•The sphincter contracts causing constriction of the pupil (miosis).
•The radial dilator muscle contracts causing dilation of the pupil (mydriasis)
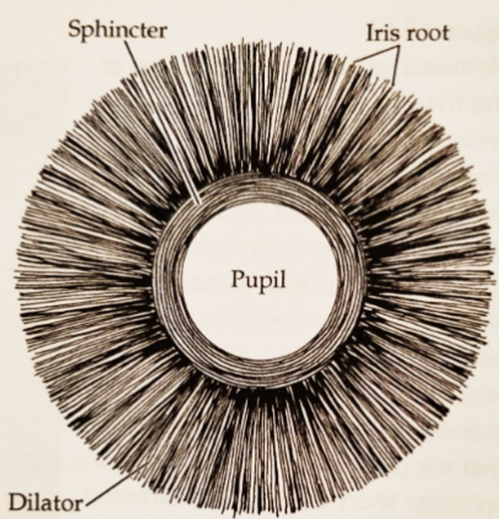
what are the 3 main pupillary reflexes (automatic actions not active)
the light/dark reflex
the near reflex
the psychosensory reflex
explain the light/dark reflex (1)
pupils constrict in response to bright light - and dilate in the dark (to allow more light in to be able to see better in the dark)
explain the near reflex (1)
accommodation and / or convergence is linked with pupil constriction
explain the psychosensory reflex (4)
pupil size is influenced by emotional state - can signal to other people about our state of mind
this can over-ride the other reflexes like the light reflex
Pleasant emotions = pupil dilation (arousal, fear, shock etc…) remember fight or flight?
Unpleasant emotions = pupil constriction (anger, boredom etc…)
what are the pupillary functions (4) and explain each one
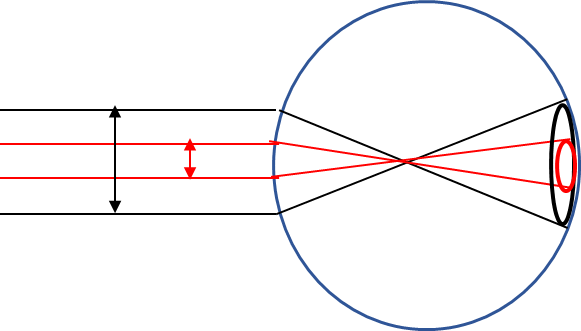
To control depth of focus – pupil constriction leads to greater depth of focus - helps with accommodation slightly (still need rx but it helps)
Signalling – pleasant emotional states, or shocking stimuli result in pupil dilation (fight or flight)
Controlling how much light enters the eye – this has a protective effect (reducing UV), but also aids night vision by minimising the amount of light adaptation that occurs (therefore speeding up dark adaptation) - not good for driving however as take in more bright lights from cars (has its advantages)
Minimising aberrations from the peripheral cornea/lens - think of a pinhole you see more accurately as only central rays pass where the light is bent more accurately as opposed to the periphery - results in a sharper image
define depth of focus
the distance along the optical axis over which the image is in focus, without having to adjust the focus of the lens (i.e. accommodate)
describe and explain the Stiles-Crawford Effect (5)
Apparent brightness varies from the centre of the pupil to the edge
Light appears brightest when entering through the centre of the pupil - as opposed to the edge
This is due to cones in the retina being directed towards the centre of the pupil
Leads to a lower photoreceptor response from orthogonal rays (rays that hit the cones at a sideways angle) - so cones respond less strongly and light looks dimmer
So large pupils don’t limit our acuity vastly - even though larger pupils let in more peripheral light - this effect comes into play - so the brain gets mostly the good quality central light - large pupils don’t blur our vision as much as we would expect
what are the dilator and sphincter muscles innervated by
dilator muscle - controlled/innervated by the sympathetic system
sphincter muscle - controlled/innervated by the parasympathetic system
what are the dilator and sphincter muscles an example of and explain
antagonist pair - they work in opposition
the amount the sphincter muscle contracts - need equal relaxation of the dilator muscle and VV
explain what the pupillary light reflex consists of - what pathways (4)
When light is shone into the eye (under normal circumstances) - the pupils will constrict
since constriction requires the sphincter muscle to contract - it involves the parasympathetic pathway
the light reflex consists of an Afferent pathway (Away from the eye), and an Efferent pathway (towards the eye)
The efferent pathway is the parasympathetic pathway in this case.
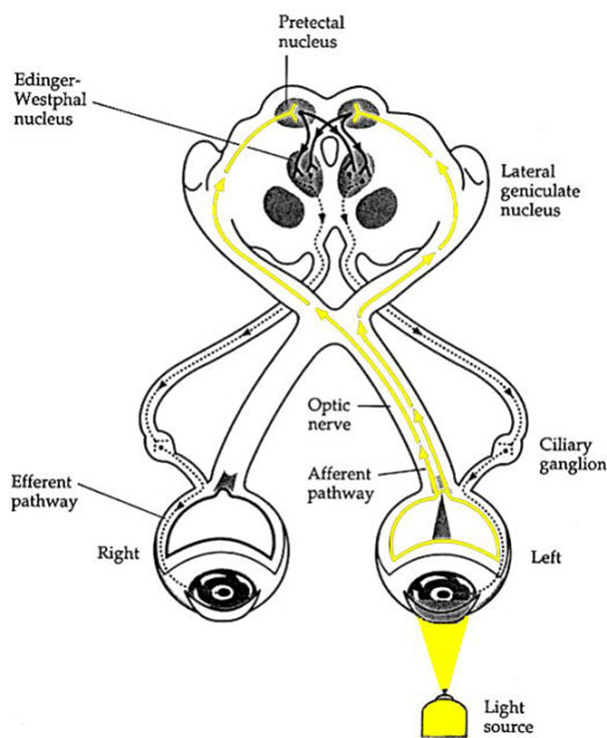
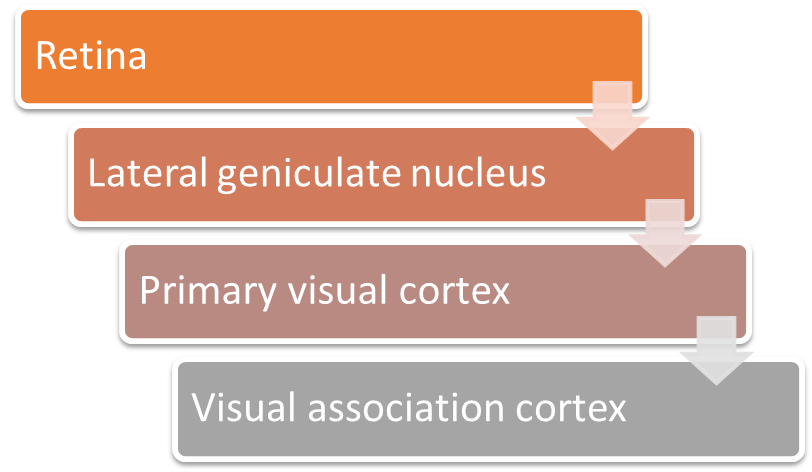
explain pathway of light through the afferent pathway (5) light reflex
•Light enters the eye and stimulates the retina
•Light signal is transmitted down the optic nerve
•At the optic chiasm (point in the brain where the optic nerves from both eyes meet and partially cross over) fibres from the nasal retina cross to the opposite (contralateral) side. Temporal fibres stay on the same (ipsilateral) side
•Fibres project to the pretectal nuclei in the midbrain
•The pretectal nuclei project fibres to both the ipsilateral and contralateral Edinger Westphal nuclei
explain the efferent pathway (4)
–signal to constrict the pupil originates in the Edinger Westphal nucleus in the midbrain
–Travels along the 3rd cranial nerve (latterly the inferior division) - if issues here - will cause issues in the eye (accommodation, ability to move the eye, lids are all affected) - considering the muscles that the 3rd cranial nerve innervates
–Synapses at the ciliary ganglion
–Short ciliary nerves then innervate the iris sphincter - then causing constriction
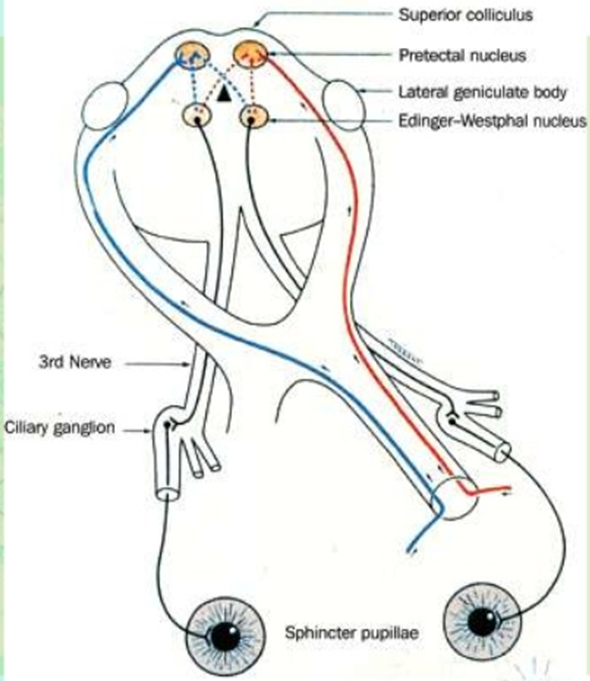
explain what the consensual response is (3)
fibres from both eyes synapse onto both pretectal nuclei
and these in turn innervate both Edinger Westphal nuclei (one on each side of the brain)
light entering one eye causes equal constriction of both pupils - call this consensual response
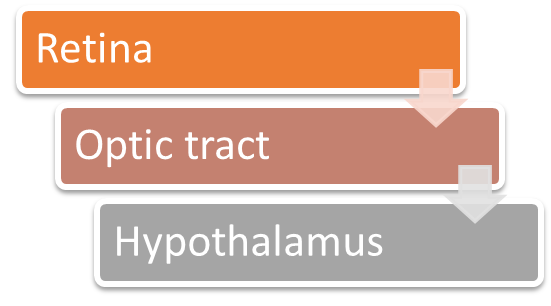
explain the afferent pathway of the pupillary dark reflex
the retina signalling an absence of light to the hypothalamus in the brain

explain the efferent pathway of the sympathetic pathway (5)
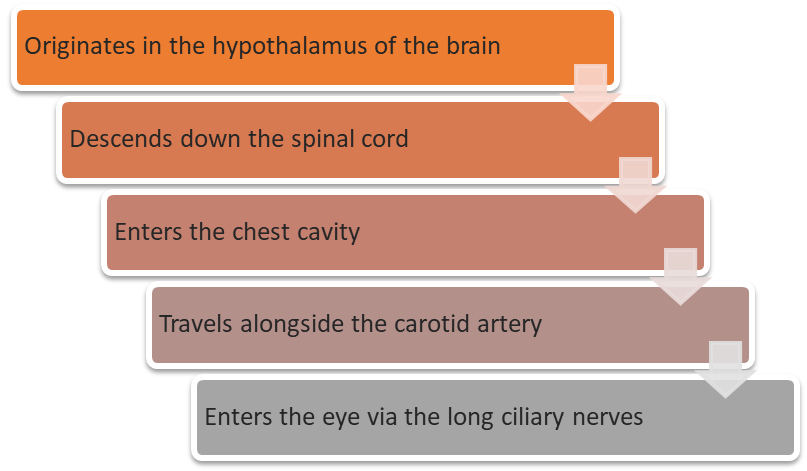
much longer pathway for dilation than there is for constriction
what do problems arising from the sympathetic pathway cause and give an example (5)
causes a miotic pupil (constricted pupil)
because the parasympathetic nerves (which control constriction) are unopposed/working normally
dilator muscle is no longer working due to problems in the sympathetic pathway - so no dilation
important note: the pupil is not actively constricting more than normal — it’s just unable to dilate, so the natural parasympathetic tone keeps it small
example - Horner’s syndrome
define anisocoria
difference in size between 2 pupils
if less than 1mm okay - if more can be said to be pathological
why might diseases arising in the spinal cord, chest and neck manifest with a purely ocular sign - like Horner’s syndrome (3)
Because the sympathetic pathway to the eye physically passes through the chest and neck
If a tumour or aneurysm presses on that pathway/the pathway is damaged anywhere along that route, the eye loses sympathetic input, causing:
➤ Miosis ➤ Ptosis ➤ Anhidrosis (reduced sweating on one side of the face)
this set of signs is Horner’s syndrome, even though the original disease is far from the eye
what does pupil size result from (3)
results from a constant balance between sympathetic (dilation) and parasympathetic (constriction) innervation
both systems are always active to some degree
if both systems are balanced = normal mid size pupil / if one is increased more than the other will result in either a dilated OR constricted pupil
define the near response
This response is part of a triad of responses that occur when a near object is fixated upon:
1.Pupillary constriction
2.Accommodation
3.Convergence
when does this response occur
occurs automatically when an out of focus, near object is viewed
(so the stimulus is a blurred retinal image), and is equal in both eyes.
why does the near response occur - purpose
occurs to maximize resolution acuity - rather than to allow a greater lag of accommodation (through increased depth of focus)
allows us to clearly focus on close objects
explain the near response - afferent pathway (4)
explain the near response - efferent pathway
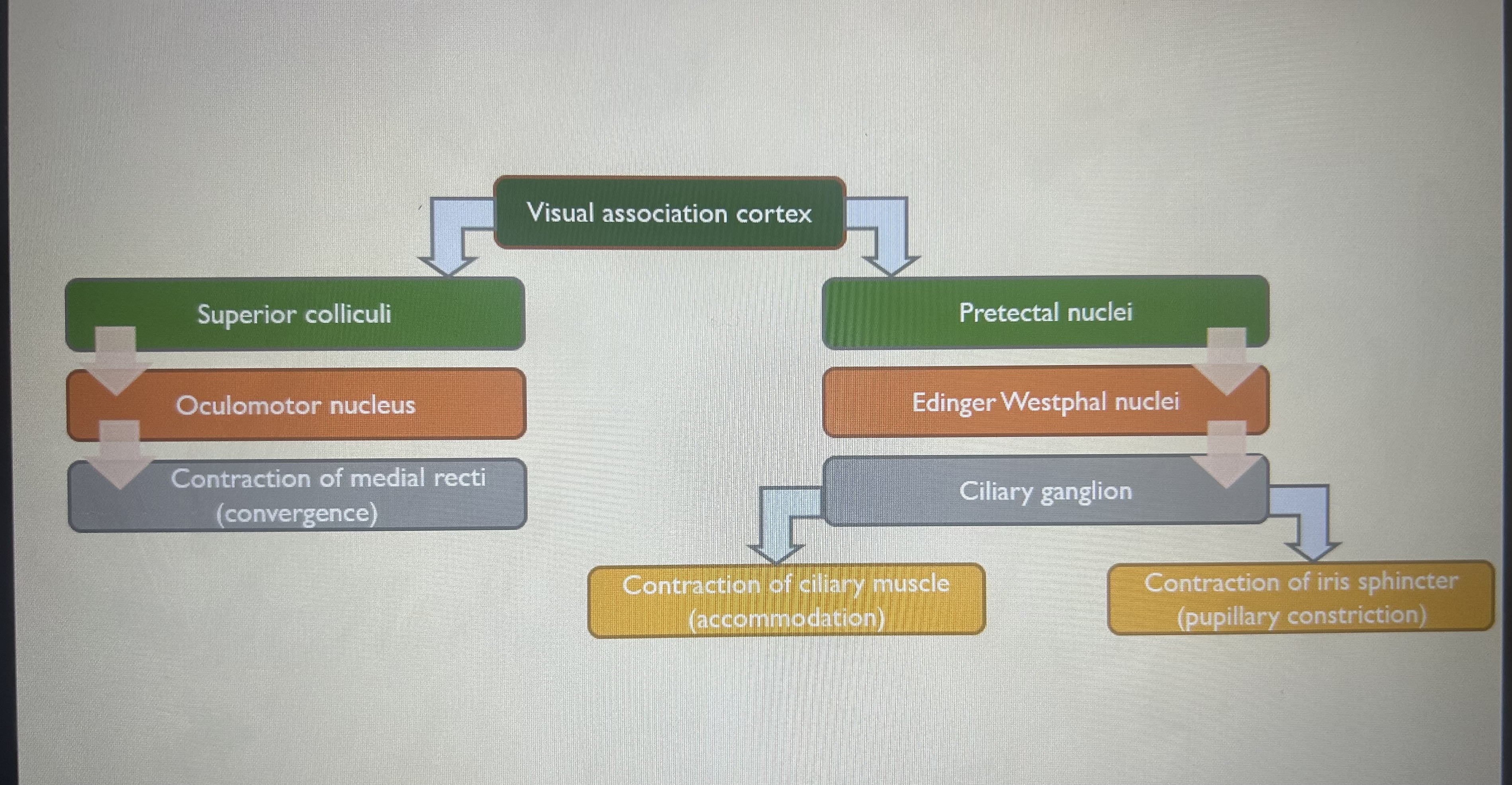
what 3 things need to be considered when observing/examining a px’s pupils
–Size - In human adults pupil size tends to vary in diameter from 2-8mm - also varies with age and room illumination - record what lighting conditions you measured the size in
–Shape – should be round
–Equality – do both pupils look equal? - esocoria
what 4 responses do we look out for when performing the pen torch assessment - (performed without the px’s gls on)
–Direct response – does the pupil constrict when light is shone directly into the eye? If the pupil constricts you would say this is the direct response for the px’s LE/RE - then repeat for other eye - grade response from 0-4 - will get more used to with time
–Consensual response – does the fellow pupil constrict when light is shone into the eye? - shining light in one eye (LE) and looking at the OTHER eye (RE) - the other eye should also constrict - this is the consensual response for the px’s LE - repeat with RE
–Near response – do the pupils constrict when moving from a distance to near target? - not using a pen torch for this obvs
–Relative afferent pupillary defect (a.k.a. swinging flashlight) test - is there a relative difference in pupil constriction?
explain what heterochromia is (4)
Difference in the colour of the two irides
Usually congenital
If acquired, can be associated with:
–Cataract
–Glaucoma
–Iridocyclitis - inflammation of the iris and the ciliary body - is a type of anterior uveitis
–Iris melanoma - malignant tumour of the iris
if a px has always had this - all good / if not further investigation needed
why would the direct response be more difficult to observe in px’s
as we age pupil gets smaller
more difficult to actually see the constriction of the pupils
what is relative afferent pupillary defect (RAPD) and how is it presented under different lighting conditions (5)
tests specifically for any problems in the afferent pathway of the pupillary light response
generally highlights if there is a unilateral or asymmetrical defect in the optic nerve or retina, which causes a relative difference in the pupil response
the affected eye will dilate when light is shone into it, because signals cannot reach the brain - ONLY works when doing swinging flashlight test
however, under normal lighting conditions both pupils will appear equal (due to the consensual response from the non-affected eye which is still intact)
also known as “Marcus-Gunn pupil”

what can cause RAPD (4)
Can be caused by:
advanced glaucoma
retinal detachment
central retinal artery occlusion
ischaemic optic neuropathy and etc…
explain the method of the swinging flashlight test (4)
1.Shine the light into the right eye – look for pupil constriction
2.Rapidly swing the light across to the left eye – the pupil should remain constricted (not tooooo quickly)
3.Repeat several times
If there is a RAPD - the affected pupil will dilate when the light is ‘swung’ in front of the affected eye (because the direct response can’t occur – the pathway is interrupted)
how do we examine pupils when testing for the near response (4)
Ask the patient to look at a distant target
and then rapidly swap to looking at a near target (such as the budgie stick, or tip of your pen)
Look for both pupils to constrict when moving from distance to near
NB: : If the direct and consensual responses are both normal, it is not always necessary to perform the near test. This is because there are no pupil abnormalities which would cause an abnormal near response but a normal direct/consensual response.

give the method for the full process of examining the pupils to check for all responses (7)
Look at the size, equality and shape of eye before doing pen torch/swinging light test
Shine light into the right eye – look at the right eye (direct)
Shine light into the right eye – look at the left eye (consensual)
Shine light into the left eye – look at the left eye (direct)
Shine light into the left eye – look at the right eye (consensual)
Swing light rapidly from one eye to the other, looking to see if the direct response is maintained at all times (RAPD)
Check the near response, if needed (after a recovery period)
look at video on brightspace !!!
how do we record pupil observations (4)
using tick box grid
Eye | D(irect) | C(onsensual) | N(ormal) |
Right | ✓ | ✓ | ✓ |
Left | ✓ | ✓ | ✓ |
number scale - usually from 0 to 4 (where 0 is no reaction, and 4 is a brisk, normal reaction)
PERRLA – Pupils Equally Round and Reactive to Light and Accommodation
Generally, we would write “no RAPD” and “No Anisocoria” next to all of the above (if appropriate)
state the different pupil abnormalities to know (4:3)
physiological anisocoria
Horner’s syndrome
Adie’s pupil
3rd Nerve Palsy
anomalies of the iris - cause an unusual appearance of the pupil - however indicate a problem with the iris:
trauma to iris from cataract surgery
iris coloboma
persistent pupillary membrane
what is physiological anisocoria
•one pupil is naturally slightly larger than the other
describe the features of physiological anisocoria (6)
•The difference in size will remain consistent under bright, normal and dim illumination
•Normally the size difference is <1mm
•Normal reaction to light observed
•It is present in about 15 – 20% of the population (but may be very subtle)
•It is present at birth
•There are no visual side effects
describe what Horner’s syndrome is (4)
•Affected pupil is miotic (and more noticeable in dim illumination)
•Indicates a problem along the sympathetic pathway
•There might also be a ptosis
•Normal reaction to light (as the parasympathetic pathway is intact – which controls constriction)
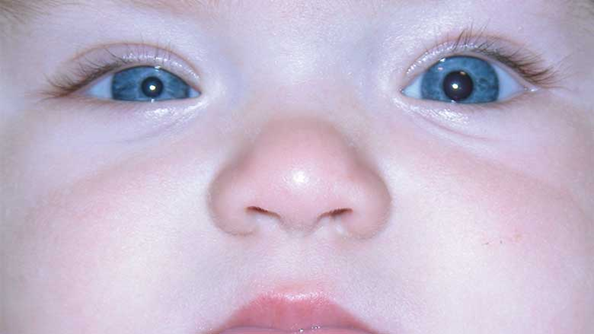
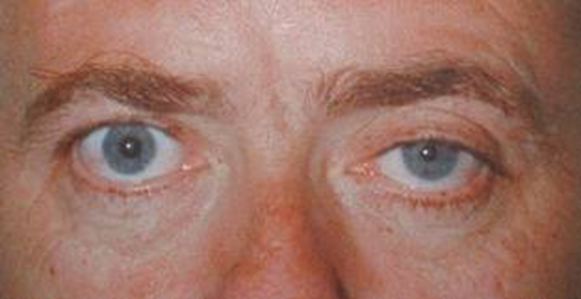
what is the differential diagnosis of horner’s syndrome (3)
physiological anisocoria - this causes one pupil to be smaller than the other just like with Horner’s syndrome
however Horner’s syndrome is a pathological miosis whereas PA is a normal variation
must always consider PA as a diagnosis before diagnosing something more serious like Horner’s syndrome
how do we check if a px has Horner’s syndrome (2)
Can be checked at the hospital through the instillation of a drop that blocks the sympathetic pathway (e.g. 10% cocaine)
this will cause both pupils to dilate in physiological anisocoria (but there would be no dilation of the affected eye in Horner’s syndrome) - determines what the diagnosis is therefore
what can Horner’s syndrome indicate
Can indicate a life-threatening condition (e.g. stroke, lung tumour, spinal cord tumour, carotid artery dissection)
explain what Adie’s pupil is (3)
Affected pupil appears dilated/larger, and is slow to react in response to light
Responds normally to near objects (light-near dissociation) – but can be slow to re-dilate at distance
Rare neurological disorder – often cause unknown (idiopathic), and may indicate selective degeneration of nerves supplying parasympathetic pupil pathway (e.g. ciliary ganglion)
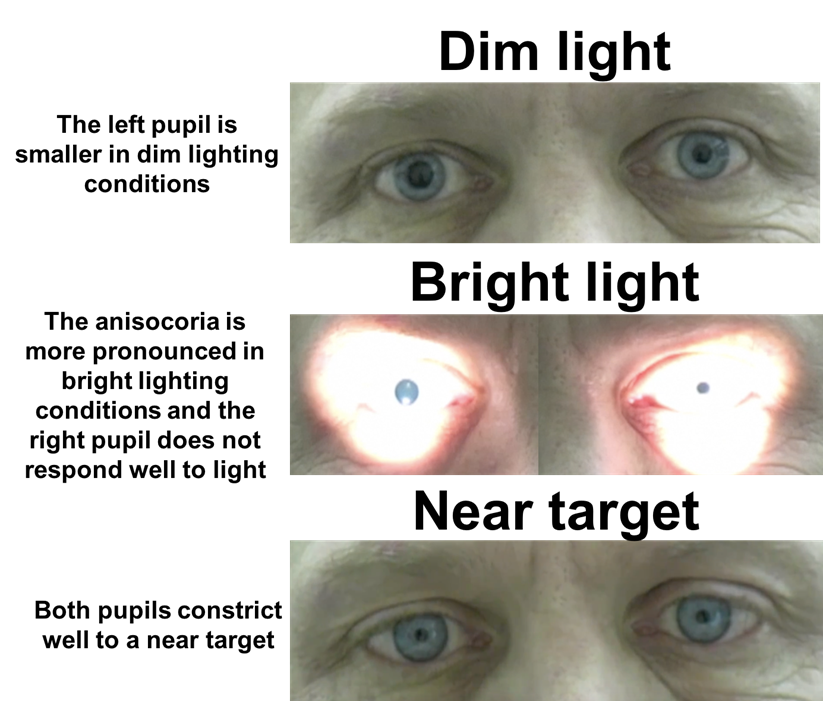
describe the features of Adie’s pupil (8)
•Usually non-progressive
-usually unilateral
•May also be called “Tonic pupil” or “Holmes-Adie pupil”
•Patients might complain of sensitivity to light
•More common in females
-average age of onset around 30 years
•No treatment required
•May become a small, miosed pupil over time (“little old Adie”)
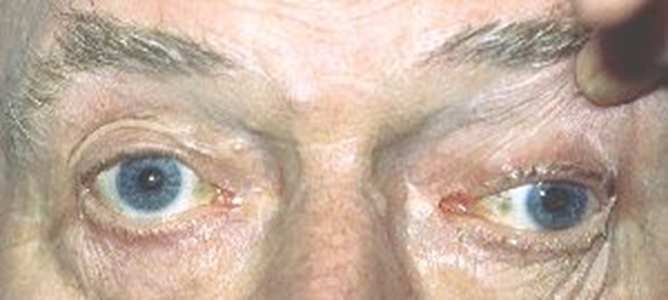
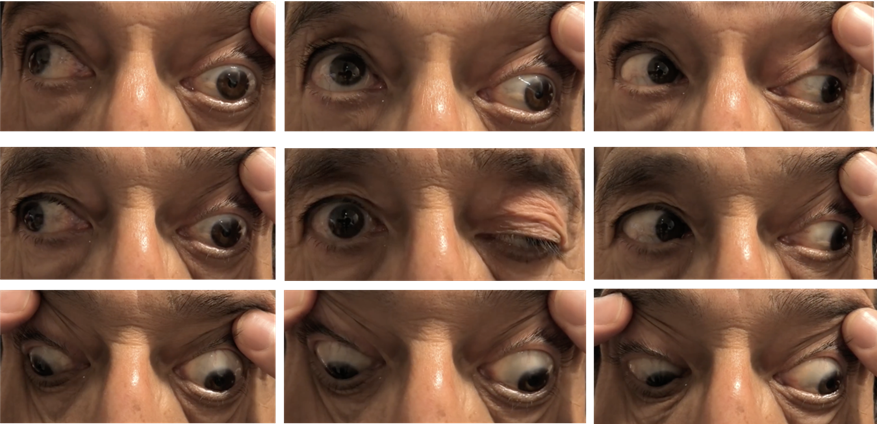
explain 3rd Nerve Palsy (4)
•Presents with pupil dilation, ptosis, and a “down and out” appearance of the affected eye - unable to centre itself
•Pupil involvement not always present
•Patient likely to complain of diplopia (if acquired)
•May be due to ischaemia of the cranial nerve (nerve not receiving enough blood supply which causes it to malfunction), aneurysm or tumour
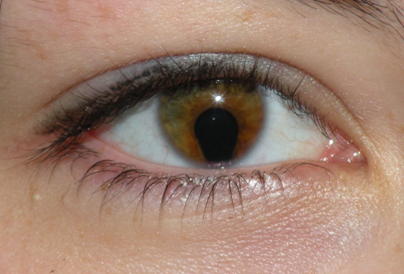
explain iris coloboma (3)
congenital abnormality
the iris doesn’t form properly
It can also affect the retina and optic nerve
explain persistent pupillary membrane (2)
remnants of the membrane that supplied blood to the lens during development - congenital (formed when lens under development)
very rare
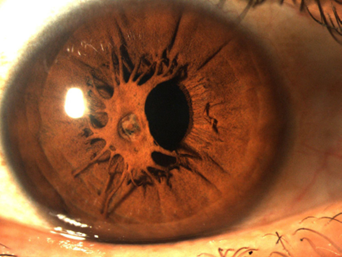
trauma to iris from cataract surgery
clips are used to hold the pupil open (if it doesn’t dilate well)