BIOL204 Spring 2025 Exam 2
1/419
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
420 Terms
The heart is located in the...
mediastanum
3 multiple choice options
Atrium
thin-walled upper chambers that receive blood returning to the heart through veins
1 multiple choice option
Ventricle
thick, muscular lower chambers that pump blood out of the heart through arteries
1 multiple choice option
(Atria/Ventricles) receive blood in the heart
atria
1 multiple choice option
Atria/Ventricles pump blood away from the heart
ventricles
1 multiple choice option
Blood returns to the heart via (veins/arteries)
veins
1 multiple choice option
Blood is pumped out of the heart via (veins/arteries)
arteries
1 multiple choice option
What is the purpose of hear valves?
to allow one-way flow of blood
Semilunar Valves
prevent backflow of blood into the ventricles when they are relaxing
1 multiple choice option
Atrioventricular Valves
prevent backflow of blood into the atria when the ventricles are contracting
1 multiple choice option
Semilunar valves include...
pulmonary and aortic valves
3 multiple choice options
Atrioventricular valves include...
tricuspid and mitral valves
3 multiple choice options
The mitral valve is also called the...
biscuspid valve
3 multiple choice options
Pulmonary Valve
valve positioned between the right ventricle and the pulmonary artery
3 multiple choice options
Aortic Valve
valve positioned between the left ventricle and aorta
3 multiple choice options
Tricuspid Valve
valve positioned between the right atrium and right ventricle
3 multiple choice options
Mitral Valve
valve positioned between the left atrium and left ventricle
3 multiple choice options
Cardiac Skeleton
a layer of connective tissue that stabilizes the positions of the four valves and prevents overdilation
Chordae Tendineae
thin bands of fibrous tissue that attach to the valves in the heart and prevent them from being pushed into the atria during systole
Papillary Muscles
enlarged muscles within the ventricular wall that are attached to chordae tendineae
Which valves have chordae tendineae?
the atrioventricular valves
1 multiple choice option
Pericardium
a sac-like membrane surrounding the heart
What are the two parts of the pericardium?
fibrous and serous pericardium
Fibrous Pericardium
tough, white fibrous connective tissue that is the outer layer of the pericardium
Serous Pericardium
thinner portion of the pericardium that is split into the parietal and visceral layers
Parietal Layer of Serous Pericardium
adheres to surface of fibrous pericardium
Visceral Layer of Serous Pericardium
outer layer of the heart
The visceral layer of the serous pericardium is also called the...
epicardium
2 multiple choice options
Heart Wall
epicardium, myocardium, endocardium
Coronary blood vessels travel through which layer of the heart wall?
epicardium
2 multiple choice options
Myocardium
Thick middle muscle layer of the heart
Endocardium
inner lining of the heart
Pericardial Cavity
contains pericardial fluid that reduces friction
Cardiomyocytes
heart muscle cells
Cardiomyocytes are...
branched
1 multiple choice option
Cardiomyocytes are...
striated
1 multiple choice option
Intercalated Discs
specialized adhesive junctions that connect adjacent cardiac muscle cells
Desmosomes
Anchoring junctions that prevent cells from being pulled apart
Gap Junction
protein channels that connect the cytoplasm of neighboring cells, allowing passage of materials between cardiac cells
Cardiomyocytes are dependent on _____ metabolism
aerobic
1 multiple choice option
Cardiac Action Potential
repeated cycle of depolarization and repolarization
Phase 0 of Cardiac AP
rapid depolarization due to rapid sodium influx
3 multiple choice options
Phase 1 of Cardiac AP
transient potassium channels open, and potassium efflux begins to return the membrane potential to normal
3 multiple choice options
Phase 2 of Cardiac AP
influx of calcium ions balances the potassium efflux, creating the plateau phase
3 multiple choice options
Cardiac Plateau Phase
lengthens cardiac action potentials; ensures ventricles have enough time to squeeze all blood out with each beat
Phase 3 of Cardiac AP
calcium channels close and rectifier potassium channels remain open, allowing the membrane potential to return to normal
3 multiple choice options
Phase 4 of Cardiac AP
potassium rectifier channels maintain the resting membrane potential
3 multiple choice options
Absolute Refractory Period
the minimum length of time after an action potential during which another action potential cannot begin
1 multiple choice option
Relative Refractory Period
the period of time following an action potential, when it is possible, but difficult, for another action potential to fire
1 multiple choice option
Fibrillation
a state of rapid and disorganized contraction
Cardiac Cycle
the sequence of events that occur during one complete heartbeat
The cardiac cycle consists of two phases called...
diastole and systole
Systole
contraction; blood leaves the chamber
Diastole
relaxation; chamber refills
(Atria/Ventricles) fill with blood first
atria
1 multiple choice option
What is the first step of the cardiac cycle?
atrioventricular valves open and ventricles fill passively
3 multiple choice options
What is the second step of the cardiac cycle?
atrial systole and ventricular diastole
3 multiple choice options
What is the third step of the cardiac cycle?
first phase of ventricular systole; atrioventricular valves close, but not enough pressure for semilunar valves to open
3 multiple choice options
What is the fourth step of the cardiac cycle?
second phase of ventricular systole; semilunar valves open, pushing blood into pulmonary and systemic circuits
3 multiple choice options
What is the fifth step of the cardiac cycle?
ventricular diastole; semilunar valves close and ventricles relax
3 multiple choice options
What is the sixth step of the cardiac cycle?
all valves are closed, and blood passively fills the atria
3 multiple choice options
Isovolumetric Contraction
the initial phase of ventricular contraction where the muscle fibers contract but the valves remain closed, resulting in no change in ventricular volume; builds tension, preparing to eject blood
3 multiple choice options
Isovolumetric Relaxation
the ventricles relax, but the valves remain closed, resulting in no change in ventricular volume
3 multiple choice options
Ventricular Ejection
the phase of ventricular contraction where the aortic and pulmonary valves open, allowing blood to be ejected from the ventricles into the aorta and pulmonary artery
3 multiple choice options
End-Diastolic Volume
the amount of blood in the ventricle at the end of diastole
3 multiple choice options
What causes the sound associated with heartbeat?
the turbulence of blood hitting a closed valve or rapidly filling a chamber
S1 Sound
"lub;" AV valves closing
3 multiple choice options
S2 Sound
"dub;" semilunar valves closing
3 multiple choice options
S3 Sound
very faint ventricular filling sound
3 multiple choice options
S4 Sound
normally inaudible "atrial gallop"
3 multiple choice options
Valve Regurgitation
leaking of blood through a closed valve
Valve Stenosis
when valves become narrower than normal, impeding the flow of blood
Pacemaker Cells
heart cells that regularly produce spontaneous electrical impulses
3 multiple choice options
Purkinje Fibers
fibers in the ventricles that transmit impulses to the right and left ventricles, causing them to contract
3 multiple choice options
What type of muscle cell is found in the walls of blood vessels?
smooth
2 multiple choice options
What type of cells line the inner surface of the heart and blood vessels?
endothelial
3 multiple choice options
Fibroblasts
cells that produce and maintain the extracellular matrix
3 multiple choice options
Cardiomyocytes
cardiac muscle cells responsible for contracting and pumping blood
3 multiple choice options
Auto-Rhythmicity
cardiac muscle's ability to contract at its own pace independent of neural or hormonal stimulation
Conducting Cells
nerve-like conduction pathways through the myocardium
The Sinoatrial Node
sets the rate of the heartbeat due to having the fastest rate of depolarization
3 multiple choice options
The sinoatrial node is also called the...
pacemaker
What is the first step of the electrical conduction for a heart contraction?
the sinoatrial node generates an electrical impulse which spreads through the atria
3 multiple choice options
What is the second step of the electrical conduction for a heart contraction?
the impulse reaches Bachmann's bundle, helping to spread it to the left atrium
3 multiple choice options
What is the third step of the electrical conduction for a heart contraction?
the impulse reaches the atrioventricular node, delaying the impulse
3 multiple choice options
What is the fourth step of the electrical conduction for a heart contraction?
the delayed impulse travels through the bundle of His
3 multiple choice options
What is the fifth step of the electrical conduction for a heart contraction?
the impulse travels through the Purkinje fibers to the ventricles, causing them to contract
3 multiple choice options
Bachmann's Bundle
the structure that relays the electrical impulse from the SA node to the left atrium in a normal heart
3 multiple choice options
Bundle of His
a bundle of modified muscle that transmits the cardiac impulse from the atrioventricular node to the ventricles
3 multiple choice options
Atrioventricular Node
a node of specialized heart muscle located in the septal wall of the right atrium
3 multiple choice options
What is the difference between the action potential in the atria and ventricles vs the pacemaker?
the pacemaker action potential has pacemaker potential, responsible for the spontaneous repetitive depolarization
Electrocardiogram
records the sum of all electrical potentials generated by all of the cells of the heart at any given time
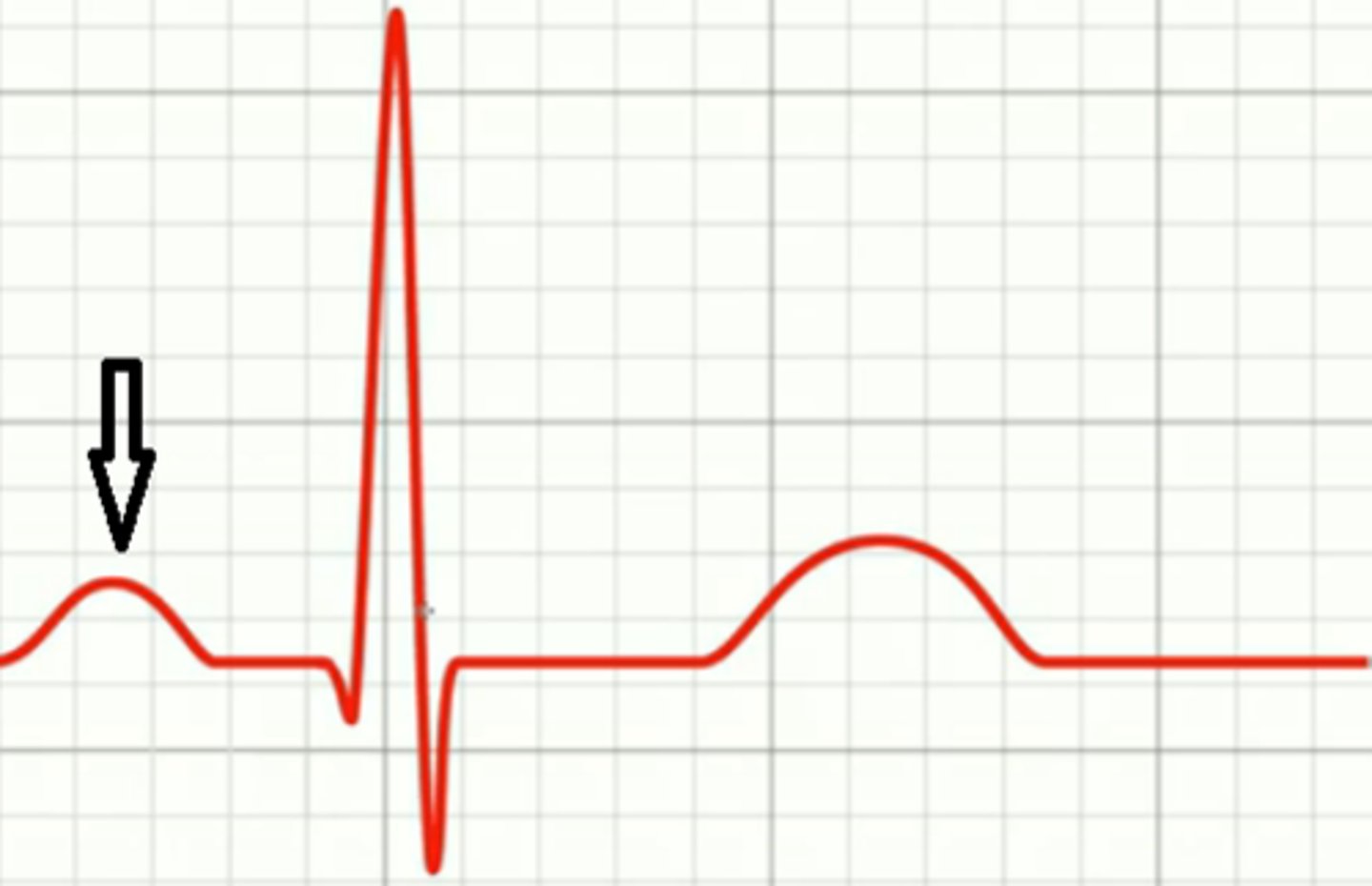
P Wave
atrial depolarization
Label the P Wave
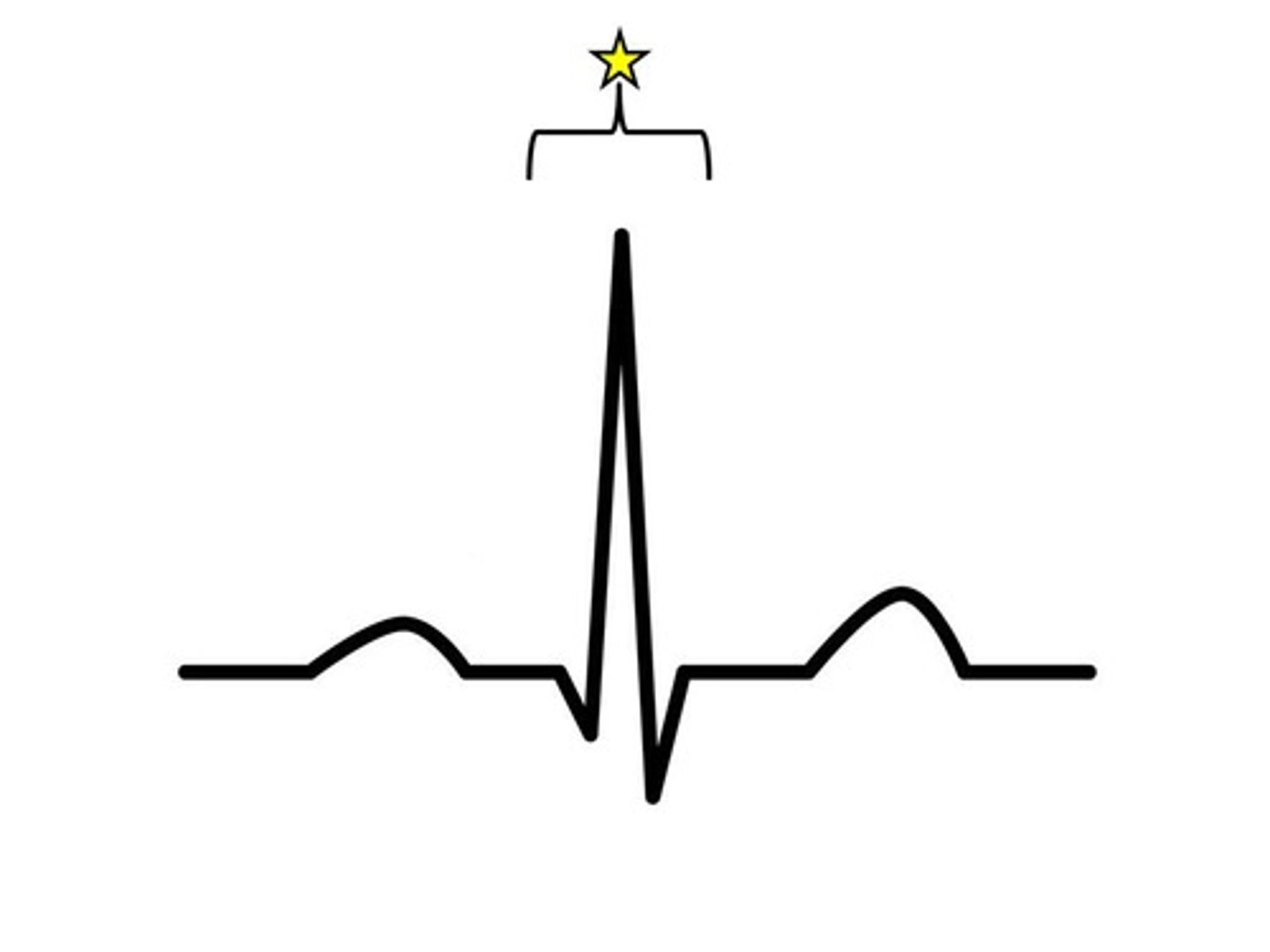
QRS Complex
ventricular depolarization
Label the QRS Complex
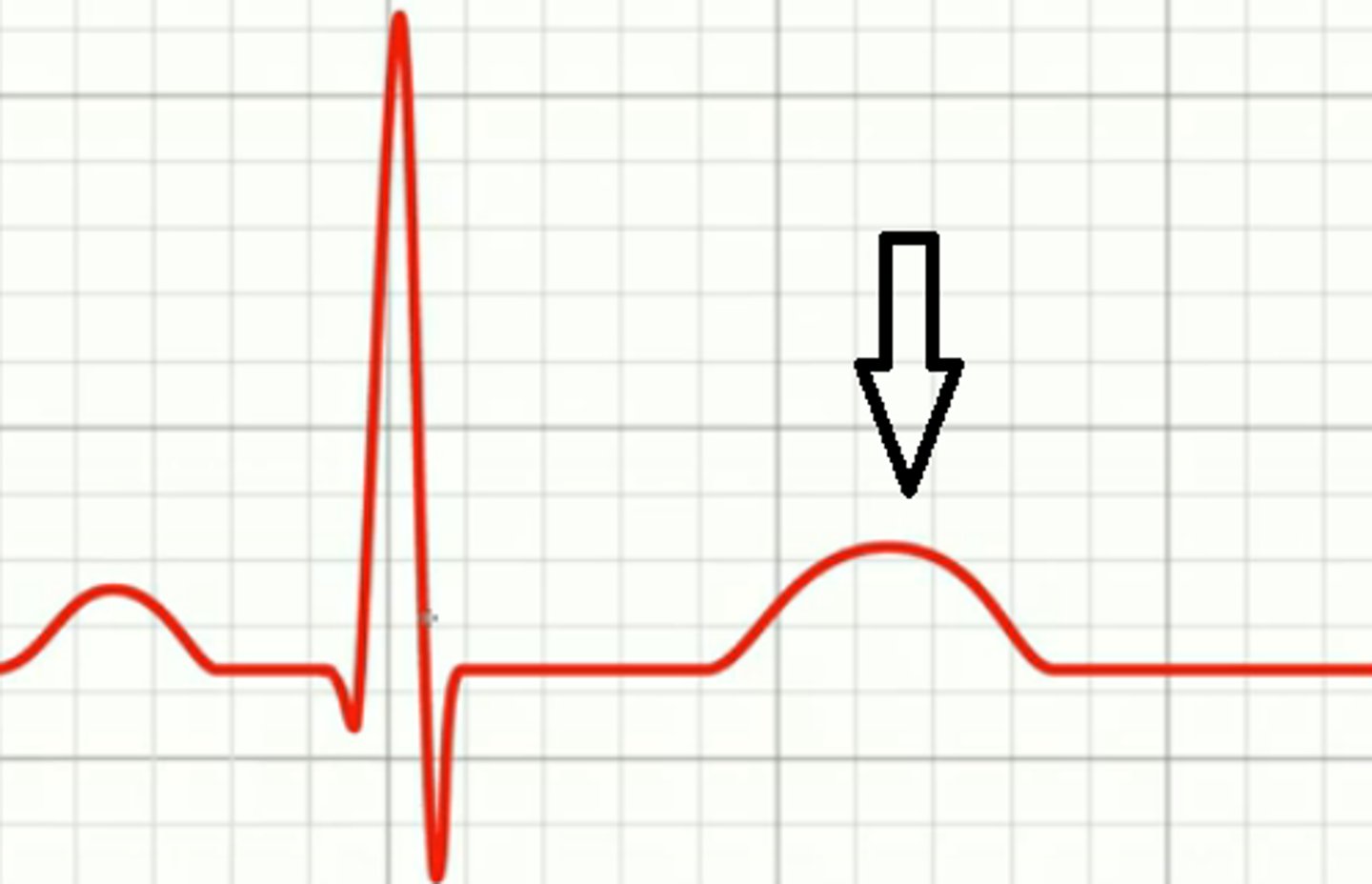
T Wave
ventricular repolarization
Label the T Wave
Heart Rate
calculated from R wave to R wave; beats per minute
2 multiple choice options
What is a normal resting heart rate?
60-100 bpm
3 multiple choice options