Microbiology Lecture Exam 3
1/141
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
142 Terms
holobiont
A human plus all of its normal microbiota (its microbiome)
infection
A condition in which pathogenic microorganisms penetrate host defenses, enter the tissues, & multiply
pathologic state
Cumulative effects of infection damage, disruption of tissues & organs, results in disease
disease
Any deviation from health, factors that cause disease: Infections, Diet, Genetics, Aging
infectious disease
Disruption of tissues or organs caused by microbes or their products
endogenous infection
Caused by biota already in the body. Normal biota is introduced to a site that was previously sterile. Immunocompromised state allows overgrowth of normal flora.
Describe why people don’t get sick all the time, even though their bodies are covered in microbes.
The immune system, genetics, and microbiome work together to detect, neutralize, and tolerate pathogens efficiently.
Human Microbiome Project
Since 2007, a worldwide research effort has been underway to utilize “big data” tools to analyze the variability of human microbiomes (location, health status, etc.) This research topic is in its infancy.
The makeup of the intestinal biota can influence many facets of one’s health.
Identify the benefits of the normal biota (the microbes that naturally live in and on the body).
Influence the development of organs, prevent the overgrowth of harmful microorganisms
Describe how the human microbiome begins to form, especially during early life.
Microbes are acquired during birth, feeding method (breastfeeding vs. formula) affects microbial makeup, microbial exposure begins in the womb.
pathogen
A microbe whose relationship with its host is parasitic, results in infection & disease
true pathogen
Capable of causing disease in healthy persons with normal immune systems
opportunistic pathogen
Cause disease when: The host’s defenses are compromised, when they become established in a part of the body that is not natural to them
virulence factor
Any characteristic or structure of the microbe that contributes to toxin production or induction of an injurious host response
Explain what biosafety levels (BSLs) are and give an example of safety precautions used at each level.
The Centers for Disease Control and Prevention (CDC) categorized pathogens as a way of protecting people who work with them in research and clinical settings.
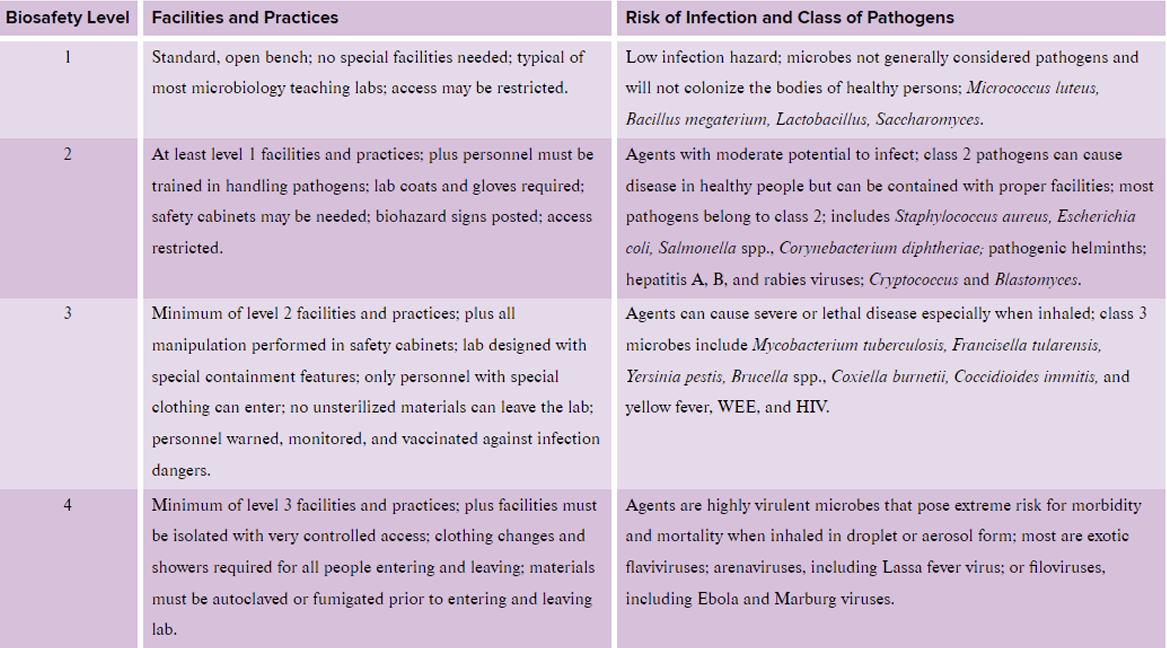
Understand how both the host and the pathogen influence the outcome of an infection.
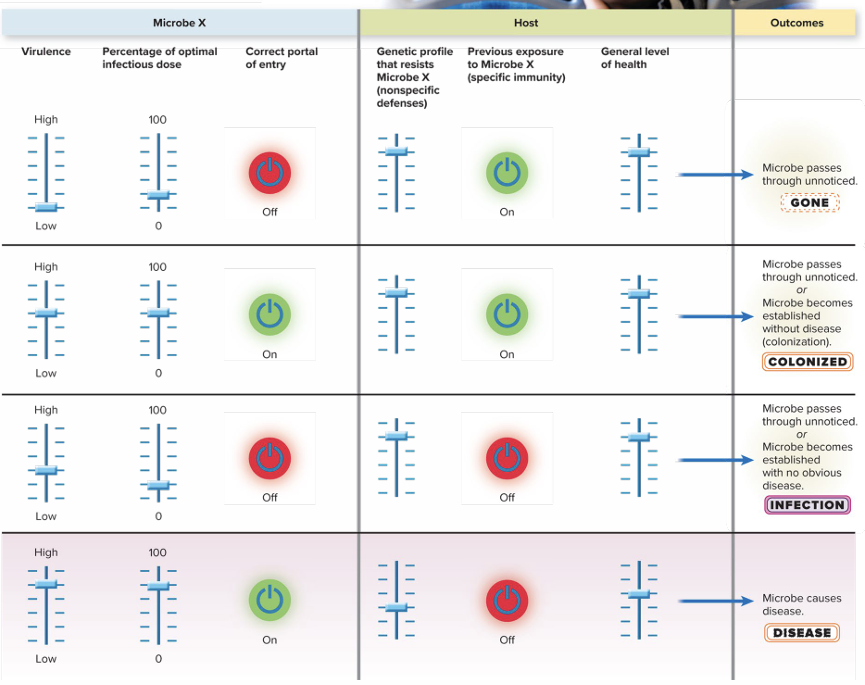
Define infectious dose (ID) and use graphs to interpret values like ID₅₀, ID₇₀, and ID₉₀.
A minimum number of microbes required for an infection to proceed. Determined experimentally for many microbes. Microbes with a smaller infectious dose have greater virulence.
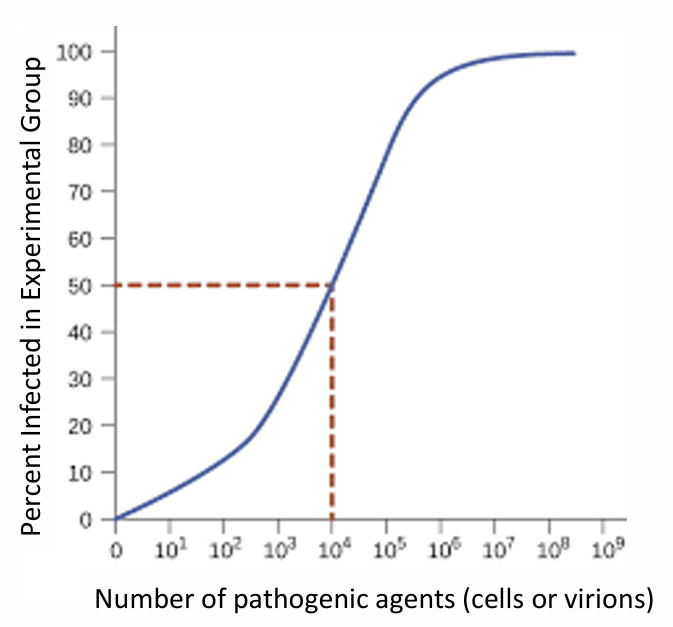
Apply your understanding of infectious dose to explain what information is needed to determine LD₅₀ (lethal dose 50).
LD₅₀ is the dose of a pathogen or toxin that kills 50% of an exposed population.
1. A precisely measured range of doses
2. A defined, standardized host population
3. Outcome data: mortality at each dose
Describe common portals of entry for pathogens
Skin
GI Tract
Respiratory Tract
Urogenital Tract
Endogenous Tract
explain the difference between endogenous and exogenous infections
Exogenous: originating from outside the body: the environment, another person, or animal.
Endogenous: already existing on or in the body: Normal biota or a previously silent infection.
Entry
A characteristic route taken by a microbe to initiate infection. Usually through skin or mucous membranes. Some pathogens that enter through the wrong portal will not be infectious.
Attachment
A particular pathogen is limited to only those cells & organisms to which it can bind. Once attached, a pathogen can invade body compartments.
Bacterial, fungal, & protozoal pathogens attach most often using fimbriae (pili), surface proteins, & adhesive slimes or capsules. Viruses attach via specialized spikes, or glycoproteins.
Invading bacterium can attach & communicate with other bacteria through quorum sensing. Chemical communication between nearby bacteria critical to establishment of infection. Changes microbial behavior, & blocking this communication has been shown to change infection dynamics.
Survival
Phagocytes: White blood cells that engulf & destroy pathogens
Antiphagocytic factors: Virulence factors used by pathogens. Circumvent some part of the phagocytic process. Leukocidins that kill phagocytes. Slime layers to make it difficult for the phagocyte to attach. Intracellular growth to avoid detection.
Damage
1. Secreting enzymes and toxins that directly damage host cells
2. By causing an overreaction by the body’s defenses
3. By altering the host cell genome or transcription
Exit
Respiratory and Salivary Portals, Skin Scales, Fecal Exit, Urogenital Tract, Removal of Blood or Bleeding
latency
A dormant state of an infectious agent. During this state, a microbe can periodically become active & produce a recurrent disease. Example: Herpes simplex (cold sores or genital herpes) or herpes zoster (chickenpox/shingles)
sequelae
Long-term or permanent damage to organs & tissues. Example: Long COVID
Incubation
The time from initial contact with the infectious agent to the appearance of first symptoms (hours to years). Average is 2-30 days.
Prodromal period
When the earliest notable symptoms of infection appear. Fatigue, headache, malaise, upset stomach. Some diseases have very specific prodromal symptoms, other diseases have imperceptible symptoms.
Height of Infection/Period of Invasion
Infectious agent multiplies at high levels, exhibits its greatest virulence, & becomes well established in its target tissue. Fever, cough, rashes, diarrhea, jaundice, muscle spasms, pain, etc.
Convalescent Period
Patient responds to infection & symptoms decline. Danger period for patients not taking full course of antibiotics.
reservoir and
Primary habitat in the natural world from which a pathogen originates. Human, animal, or plant carriers.
source of infection
Distinct from a reservoir. Individual or object from which an infection is acquired.
Name and describe the five types of carriers.
An individual who inconspicuously shelters a pathogen & can spread it to others without knowing. Asymptomatic carriers, Incubating carriers, Convalescent carriers, Chronic carriers, Passive carriers.

Compare biological and mechanical vectors of disease transmission.
Vectors can be placed in one of two categories (mechanical or biological). Defecate around the bite wound (flea). Injected infected saliva into the blood (mosquito). Regurgitate blood into wound (tsetse fly).

Zoonosis
An infection indigenous to animals but also transmissible to humans
communicable disease
Occurs when an infected host can transmit the infectious agent to another host & establish infection in that host
contagious
The agent is highly communicable, especially through direct contact
noncommunicable disease
Does not arise through transmission of the infectious agent from host to host
vertical transmission
Transmission from parent to offspring via ovum, sperm, placenta, or milk
horizontal transmission
Disease is spread through a population from one infected individual to another. We divide these diseases into direct or indirect.
State Koch’s Postulates and explain why they do not apply to all diseases. Give two examples to support your explanation.
A series of proofs that established classic criteria for etiologic studies. Reliable for many infectious diseases, but not all. Leprosy caused by M. leprae is not readily grown in the lab. Diseases with no suitable animal model. Many viruses have very narrow host ranges. We are further in understanding polymicrobial infections that we were originally.
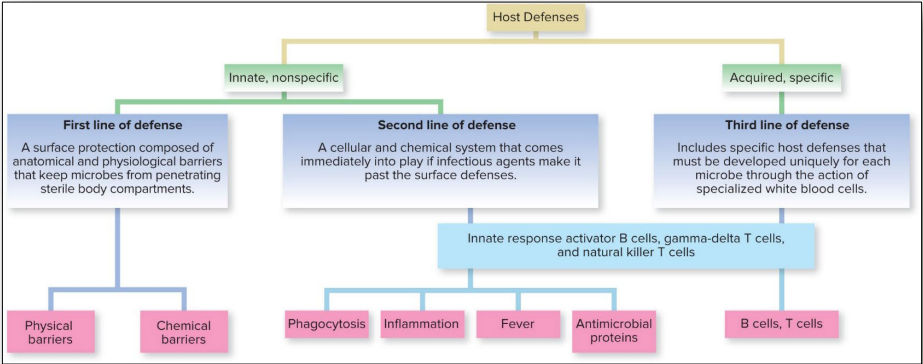
innate immunity
Non-specific, it does not require “training” and treats all invaders similarly.
First line of defense = Nonspecific barriers that block invasion at portals of entry
Second line of defense = Nonspecific system of cells and fluids
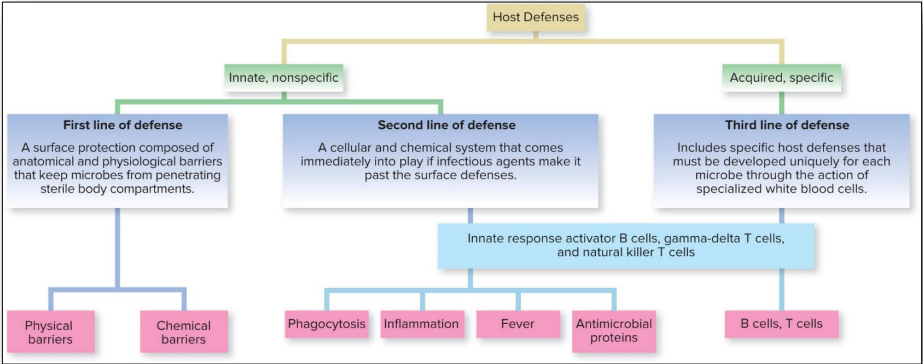
adaptive immunity
Adaptive immunity is specific and slower to activate (taking days to weeks).
Third line of defense = Specific memory response mediated by lymphocytes
Explain the three major jobs of the immune system and how it avoids damaging the body’s own tissues.
1. surveillance of the body
2. recognition of foreign material
3. destruction of entities deemed to be foreign.
On top of these, the immune system needs to not attack self
Understand how the body distinguishes self from nonself using surface markers.
White blood cells move throughout the body, searching for potential pathogens. Trained to recognize self, or body cells, & nonself, bacterial cells or other invading pathogens.
Markers: Molecules on the surfaces of cells, Composed of proteins and/or sugars, Evaluated by cells of the immune system
PRR (Pattern Recognition Receptor)
essential components of the innate immune system that detect pathogens and initiate immune responses by recognizing specific molecular patterns
PAMP (Pathogen-Associated Molecular Pattern)
conserved molecular structures found in pathogens that are recognized by the immune system, playing a crucial role in initiating innate immune responses.
antigen
A chemical/molecule/protein that can trigger an adaptive immune response. These receptors are used by white blood cells of adaptive immune system to recognize very specific microbes (example: E. coli strain 0157:H7).
Understand why the innate immune system is considered nonspecific in its response.
it provides a general defense against a wide range of pathogens without targeting specific one
Know the difference between blood plasma and serum.
Blood cells suspended in plasma. Side note: Plasma & serum are not the same; serum is what remains after blood clots & does not contain any clotting factors.
Classify key immune system locations as:
Connective fluid (e.g., blood, lymph)
Primary lymphoid organs (where immune cells are made and mature)
Secondary lymphoid organs (where immune responses are activated)
secondary lymphoid organs
In secondary lymphoid organs, the immune response is activated. Lymph Nodes: Sites of Activation From Lymph Fluid. Spleen: Sites of Activation From Blood. Associated Lymphoid Tissues: Sites of Activation From Mucosal Membranes or Skin.
primary lymphoid organs
These organs are critical sites where white blood cells develop and mature into active cells. Two sites: Bone marrow (All blood cells original in bone marrow). Thymus (A particular type of white blood cell, the T cell, finishes development here but begins development in bone marrow).
leukocyte (white blood cell)
essential immune cells that protect the body from infections, foreign invaders, and disease
lymphocyte (B cells, T cells, etc.)
A type of white blood cell that play a critical role in the immune system. They are responsible for recognizing and responding to pathogens, such as bacteria and viruses.
agranulocyte vs. granulocyte
Agranulocytes are white blood cells without cytoplasmic granules, mainly involved in adaptive immunity, while granulocytes contain granules and primarily mediate rapid innate immune responses.
Identify the stem cell that gives rise to all blood cells and platelets.
Hematopoietic stem cells (HSCs)
Know which agranulocytes (monocytes, macrophages, dendritic cells) can present antigens to T cells.
Dendritic cells
Understand the distinct roles of T cells and B cells in the adaptive immune response.
T cells are your body’s coordinators and direct attackers. B cells are your antibody factories.
Describe the roles of each granulocyte type (e.g., neutrophils, eosinophils, basophils, mast cells).
neutrophils: Rapidly phagocytose and destroy bacteria and fungi.
eosinophils: Combat parasitic worms (helminths) and modulate allergic responses.
basophils: Amplify allergic and inflammatory responses in the bloodstream.
mast cells: Initiate local allergic responses and coordinate inflammation.
Explain the functions of red blood cells and platelets.
RBC: transports O2 and CO2
platelets: cell‑fragment responders that prevent blood loss after vessel injury
Define the role of cytokines as chemical messengers in immune system communication.
Cytokines are small, secreted proteins that allow immune cells to send signals, coordinate responses, and shape the intensity and type of immune reaction.
Define the first line of defense in the immune system and provide at least three examples of physical or chemical barriers that help prevent infection.
First line defenses are made up of anatomical structures and physiological features of the body.
Physical Structures - Skin & mucosal membranes
Secretions - Sebum, tears, wax, mucus, saliva, sweat
Removal - Defecation, urination, skin shedding
Enzymes – Lysozyme
Microbiome
List the three main phagocyte types and where each is commonly found in the body.
neutrophils (bloodstream), monocytes (blood), & macrophages (tissues)
Describe the steps of phagocytosis, including how immune cells recognize targets using PAMPs and PRRs.
1. Chemotaxis by PRR & PAMP recognition, Peptidoglycan, LPS, dsRNA. (recognize their targets using pattern recognition receptors)
2. Adhesion of bacteria
3. Engulfment into phagocytic vacuole
4. Phagosome
5. Phagolysosome formation, Hydrolytic enzymes & low pH
6. Killing and destruction of microbes (usually within 30 min)
7. Release of residual debris
Explain how antibodies enhance phagocytosis through opsonization.
Opsonization is the process by which antibodies “tag” pathogens, making them dramatically easier for phagocytes to recognize, bind, and ingest.
Describe the stages of inflammation, using key terms such as exudate, edema, diapedesis, and chemotaxis.
To mobilize & attract immune components to the site of injury. To set in motion mechanisms to repair tissue damage & localize & clear away harmful substances. Destroy microbes & block their further invasion.
Exudate: blood-borne components that escape into extracellular space
Edema: local swelling & firmness due to accumulation of exudate into the tissues
Chemotaxis: Movement of white blood cells from the bloodstream into the tissues, Occurs because white blood cells are actively motile & able to change shape, Receptors on endothelial cells capture WBCs & participate in their transport.
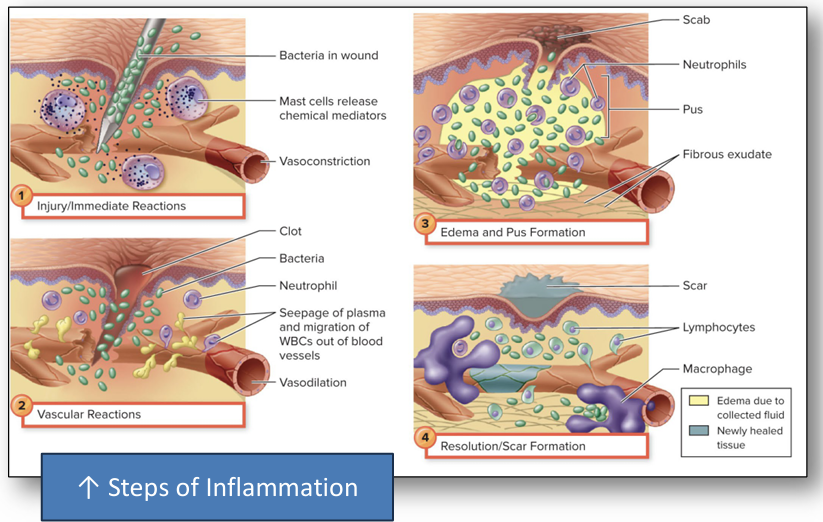
List the four classic signs of inflammation
Rubor: redness caused by increased circulation & vasodilation in injured tissues
Tumor: swelling from increased fluid escaping from tissues
Dolor: pain caused by the stimulation of nerve endings
Calor: heat from the increased flow of blood
explain three benefits of edema and chemotaxis
Influx of fluid dilutes toxic substances, Fibrin clot can trap microbes & prevent further spread, Neutrophils actively phagocytose & destroy bacteria, dead tissue, & particulate matter. Pus: whitish mass of cells, liquefied cellular debris, & bacteria.
Know the normal oral body temperature for healthy adults and how it may change with age
Normal body temperature ranges from 97.5°F to 98.9°F (36.4°C to 37.2°C)
Ranges of fever → Depend on age & site tested
Define exogenous and endogenous pyrogens, and how they influence body temperature.
Exogenous: originating outside the body, Products of infectious agents such as viruses, bacteria, protozoans, & fungi. Endotoxin. Blood, blood products, vaccines, injectable solutions.
Endogenous: originating inside the body, Released by monocytes, neutrophils, & macrophages during the process of phagocytosis, Interleukin-1 (IL-1) & tumor necrosis factor (TNF)
Explain the benefits of a mild fever in supporting immune function.
Inhibits multiplication of temperature-sensitive microorganisms
Impedes the nutrition of bacteria by reducing the availability of iron
Increases metabolism & stimulates immune reactions & naturally protective physiological processes
Know how many proteins make up the complement system, and how its three activation pathways are triggered.
Consists of over 30 blood proteins, work together to destroy bacteria & viruses.
Classical complement pathway: Begins when antibody binds to microbial cells
Lectin pathway: Activated by mannans
Alternative pathway: Activated by bacterial or fungal cell wall, viruses, or parasite surfaces
Describe what happens when the complement system is activated and how it contributes to microbial destruction.
Sequential physiological response. First substance in a chemical series activates the next substance, which activates the next, & so on until the desired end product is reached.
Define antimicrobial peptides and explain how they kill or inhibit microbes as part of innate defense.
Antimicrobial peptides (AMPs) also act to kill microbes by inserting themselves into bacterial membranes. These types of peptides are secreted into mucosal membrane secretions, tears, and even on the skin.
Identify the major cell types involved in adaptive immunity and describe six key traits that distinguish it from innate immunity.
• Specificity • Diversity • Inducibility • Clonality • Tolerance • Memory
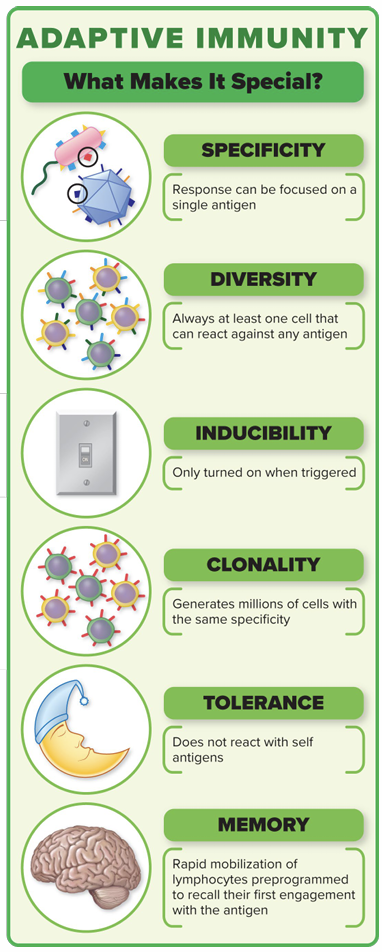
Define an antigen and differentiate it from pathogen-associated molecular patterns (PAMPs) recognized by the innate immune system.
Antigens are unique identifiers that adaptive immunity learns to recognize with precision.
PAMPs are generic microbial patterns that innate immunity uses to detect infection quickly.
List and explain the four chronological stages of a specific adaptive immune response.
I. Lymphocyte development & differentiation
II. Presentation of antigens
III. The challenge of B & T lymphocytes by antigens
IV. Lymphocyte responses, B-lymphocyte response, Production & activities of antibodies, T-lymphocyte response, Cell-mediated immunity
Describe where B cells and T cells mature and trace their migration to secondary lymphoid organs after maturation.
Bone Marrow and Thymus, travel through blood to lymph nodes, spleen, and MALT
Explain the functions of MHC Class I and MHC Class II receptors, and identify which cell types express each class.
Class I MHC: Genes Markers appear on all nucleated cells (aka no RBCs). Display unique characteristics of self. Allow for recognition of self & the regulation of immune reactions. Each human inherits a particular combination of class I MHC genes.
Class II MHC: Genes Code for immune regulatory markers found on macrophages, dendritic cells, & B cells. Involved in presenting antigens to T cells during cooperative immune reactions.
Describe the difference between MHC Class I and Class II antigen presentation pathways and the types of T cells they activate.
MHC Class I: endogenous antigens, activate CD8⁺ cytotoxic T cells
MHC Class II: exogenous antigens, activate CD4⁺ helper T cells
Define antigen-presenting cells (APCs) and explain their role in activating T cells.
Ingest the antigen, Migrate to the nearest lymphoid organ, Process & present antigen to T-lymphocytes
Explain how lymphocyte receptors (BCRs and TCRs) recognize antigens and the differences in how B and T cells are activated.
B cells have B-cell receptors (BRCs) that recognize unique antigens. These BCRs are a form of membrane-bound antibody. T cells have T-cell receptors (TCRs) that bind antigens, but only when those antigens are processed & presented in MHC molecules on the surface of antigen-presenting cells, like dendritic cells.
Describe the process of clonal selection and clonal expansion, including the formation and function of memory cells.
Creates a clone of cells, Genetically identical cells, which all recognize the same original antigen, Some of these cells become memory cells which remain behind & help us fight the antigen better next time.
Summarize the role of memory cells in secondary immune responses and their importance in protection upon re-exposure.
Memory cells turn the adaptive immune system into a learning system—one that improves with experience and protects you more effectively each time you encounter the same threat.
plasma cells
These plasma cells still bind the same antigen as the original mother cell that found the antigen. Plasma cells release antibodies into the tissue & blood.
helper T cells (CD4)
activate macrophages, assist B-cell processes, & help activate cytotoxic T cells
regulatory T cells
control the T-cell response
cytotoxic T cells (CD8)
lead to the destruction of infected host cells & other “foreign” cells
Summarize how B cells and T cells develop, including genetic recombination that gives rise to their unique receptors.
Maturation for T cells occurs in the thymus, where formation of the T-cell receptor (TCR) & its coreceptors is accomplished.
Maturation for B cells occurs in the bone marrow, where formation of the B-cell receptor (BCR) & its coreceptors is accomplished. The formation of B cell receptors (BCRs) is through extensive DNA rearrangements of more than 500 gene segments Theoretical number of possible variations varies from 1014 to 1018 different antigen specificities.
Describe the structure of B-cell receptors.
The BCR is an immunoglobulin molecule composed of. Two heavy (H) chains. Two light (L) chains. One light chain is bonded to one heavy chain. The two heavy chains are bonded to each other with disulfide bonds. Creates a symmetrical, Y-shaped arrangement.
Antigen-binding sites: Pockets at the ends of the forks formed by the light & heavy chains. Can be highly variable in shape to fit a wide range of antigens.
Variable (V) regions: Found in antigen binding sites. Amino acid position is highly varied from one clone of B lymphocytes to another as the result of genetic reassortment.
Constant regions: Amino acid content does not vary greatly
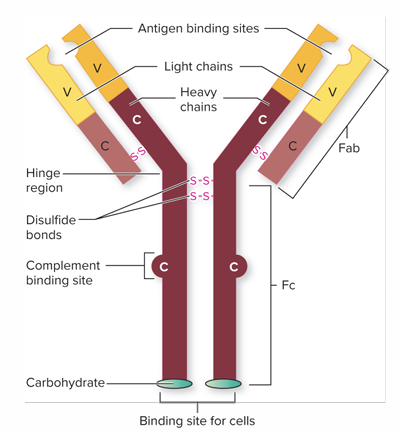
Describe the structure of T-cell receptors.
Like the B cell receptor, Formed by genetic modification. Has variable & constant regions. Inserted into the membrane. Has antigen binding site formed from two parallel polypeptide chains. Unlike the immunoglobulins, Relatively small, Never secreted. T cells need coreceptors known as CD4 or CD8 to recognize the MHC that allows them to find antigen. CD4 on helper T (TH) cells. CD8 on cytotoxic T (TC) cells.
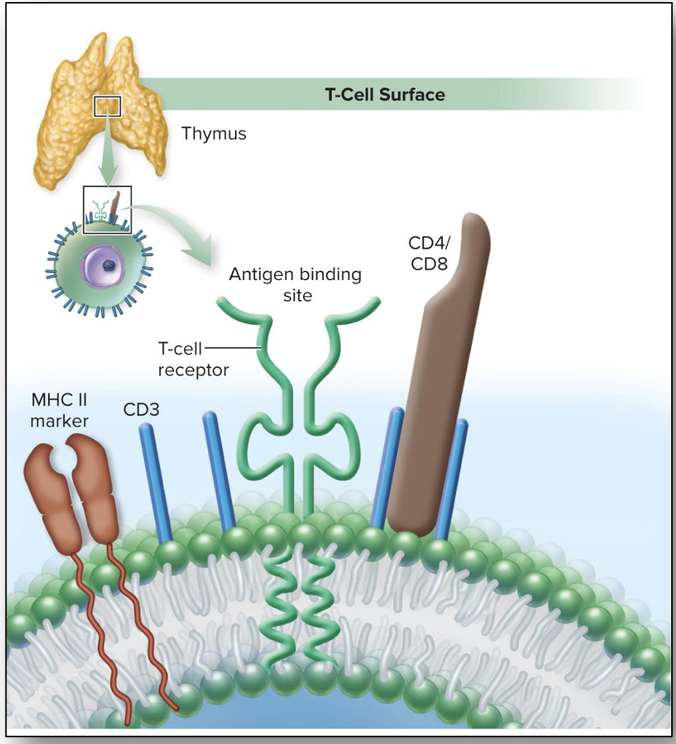
Know which CD markers are found on helper (CD4+) and cytotoxic (CD8+) T cells, and what MHC class each recognizes.
CD4 on helper T (TH) cells MHC Class II
CD8 on cytotoxic T (TC) cells MHC Class I
Understand that BCRs are membrane-bound antibodies.
A B‑cell receptor (BCR) is essentially a membrane‑anchored form of an antibody. Before a B cell is activated and begins secreting antibodies, the antibody molecule exists in this surface‑bound form.
Outline the process of clonal selection and expansion.
Clonal selection, aka expansion, happens after exposure to antigen. Lymphocytes that recognize their cognate antigen proliferate massively, all bearing the same antigen specificity. Reactions to antigens depend on the chance creation of lymphocytes specific to it. This also can lead to self-reactive lymphocytes. Immune tolerance removes these harmful clones using clonal deletion.
Define antigen and epitope, and give examples of molecules that can act as antigens.
A substance that provokes an immune response in specific lymphocytes. To be perceived as an antigen or immunogen, a substance must meet certain requirements in foreignness, shape, size, & accessibility.
Epitope: A portion of the antigen molecule recognized & responded to by a lymphocyte. The primary signal that a molecule is foreign.
Define hapten and how it differs from a full antigen.
Consist only of a determinant group. Too small by themselves to elicit an immune response. If linked to a carrier group, the combined molecule develops immunogenicity.
alloantigens
“Allo” meaning other. Proteins & other molecules of one person that are antigenic to another. Cell surface markers that occur in some members of the same species but not in others. The basis for an individual’s blood group & major histocompatibility profile. Responsible for incompatibilities that occur in blood transfusion or organ grafting.
superantigens
Usually bacterial toxins Potent stimuli for T cells. Activate T cells at a rate 100 times greater than ordinary antigens. Can result in an overwhelming release of cytokines & cell death, as well as clotting issues, autoimmunity,& immunodeficiency. Toxic shock syndrome & certain autoimmune diseases are associated with these antigens.