Digestive System Pennix (copy)
1/130
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
131 Terms
Digestive Processes
ingestion, movement, digestion (breakdown of food via mechanical/chemical processes), absorption (into cardiovascular/lymphatic systems), defecation
Chemical digestion
catabolic reactions that break down carbs, lipids, and proteins into smaller molecules
Mechanical Digestion
Purpose: Increase the surface area of ingested foods to be physically prepared for digestion by enzymes
Includes:
chewing,
mixing food with saliva by the tongue
churning food in the stomach,
segmentation within the small intestine
Segmentation = mixing food with digestive juices, making absorption faster by repeatedly moving different parts of food mass over intestinal wall
GI Tract Organs
mouth, pharynx, esophagus, stomach, S/L intestine, liver, pancreas, gallbladder, rectum, anus
GI tract structure
tube running down the ventral cavity from the mouth to the anus
GI Tract accessory structure/function
teeth, tongue, salivary glands, liver, gallbladder, and pancreas that produce/store secretions that aid in chemical breakdown of food
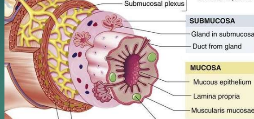
Mucosa
inner lining of GI tract
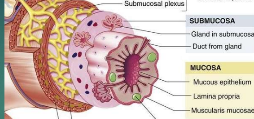
Mucosa Epithelium (Part of Mucosa)
stratified in mouth/esophagus and simple throughout the rest of the GI tract
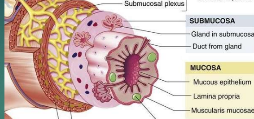
Mucosa lamina propria
loose CT that connects the epithelial layer to the muscularis mucosae and provides space for blood and lymphatic vessels
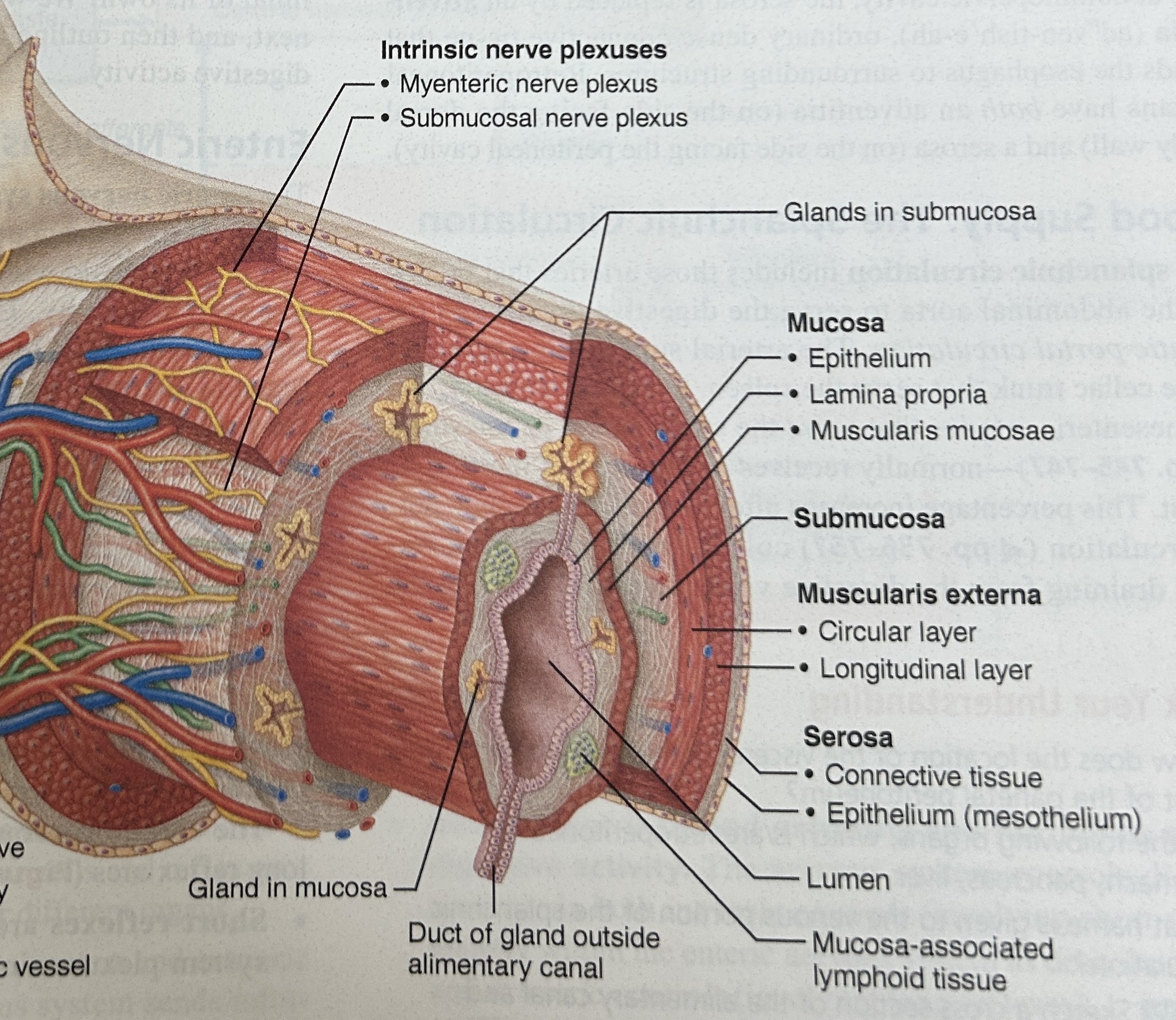
Muscularis mucosa
smooth muscle that puts folds into the intestine to increase the surface area of the intestine
-contains longitudinal layer and circular layer
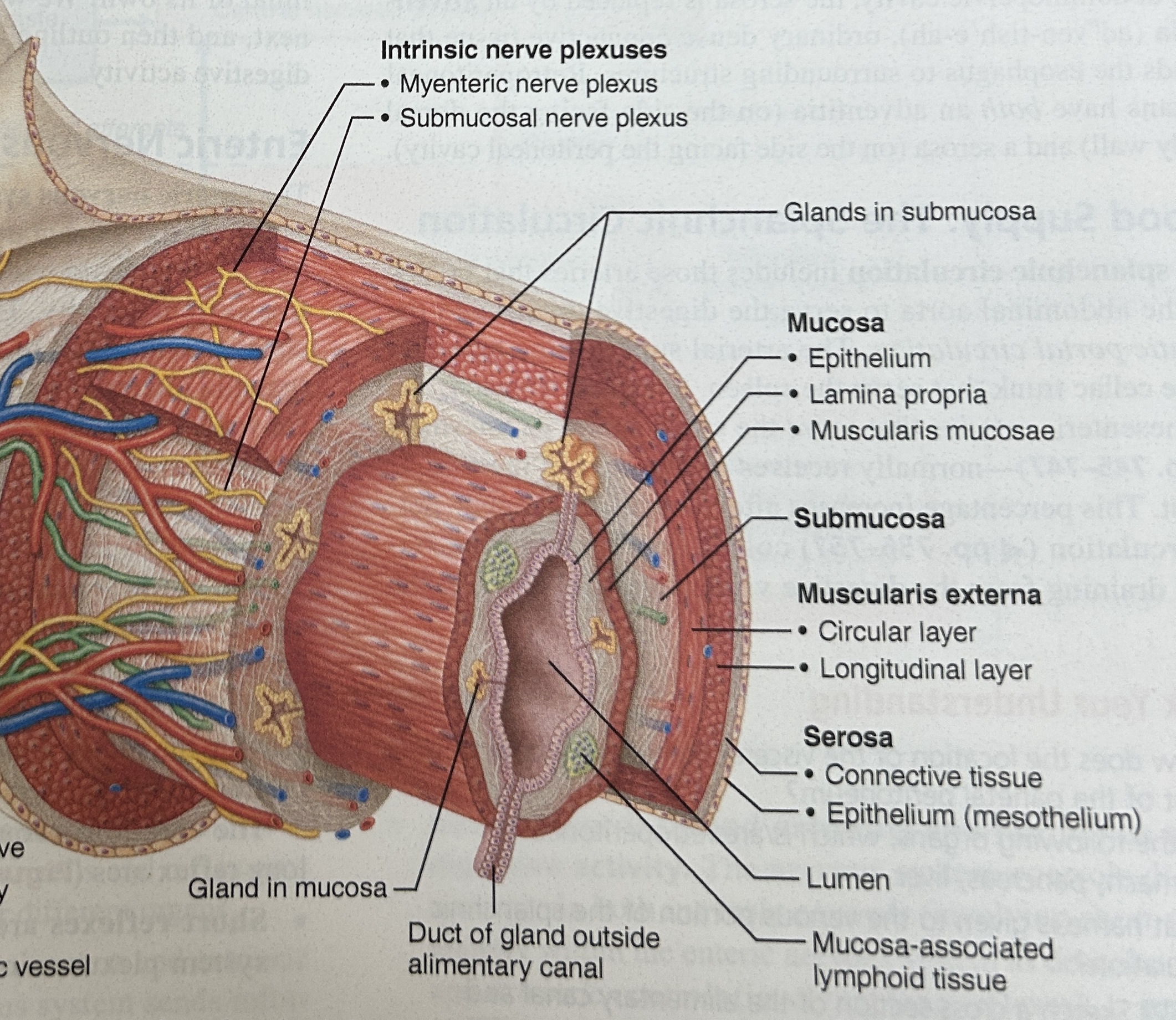
Submucosa(middle)
dense CT that binds the mucosa(inner) to the muscularis(layer before serosa).
Highly vascular and contains an autonomic nerve supply to the muscularis mucosa
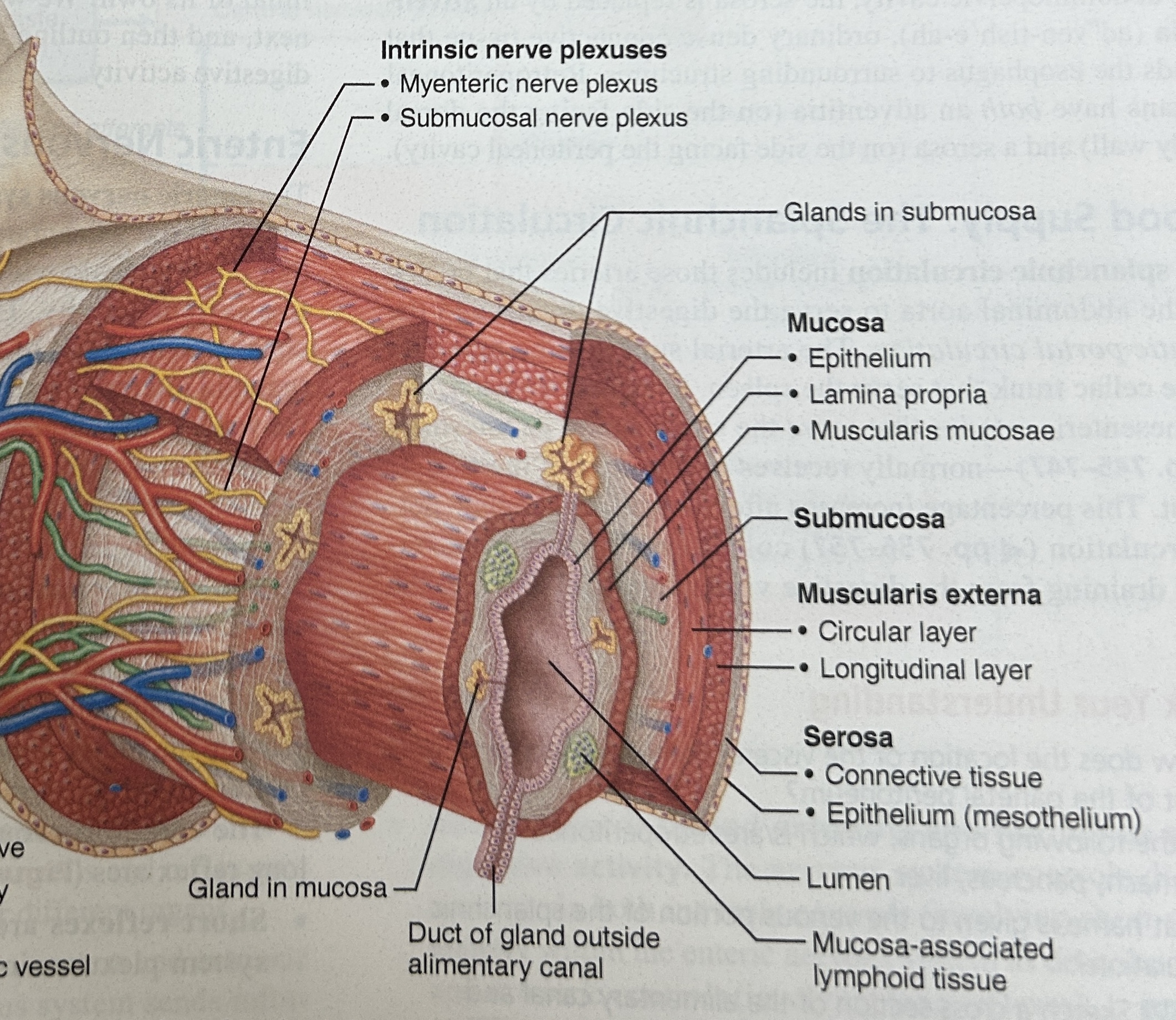
Muscularis
-in the mouth, pharynx, and upper esophagus,
-some skeletal muscle -voluntary swallowing,
-helps to fix food and move it through the GI tract
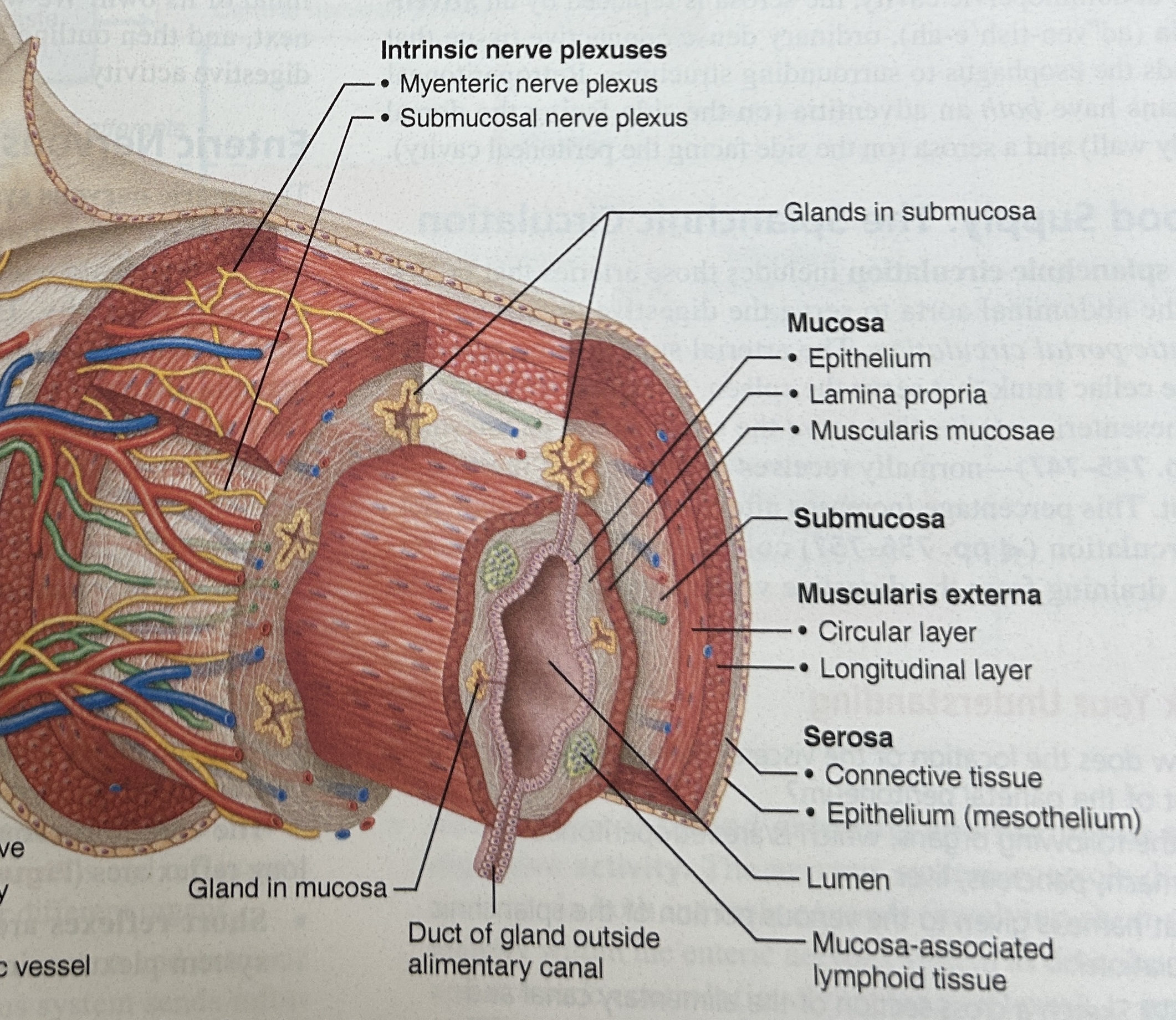
Serosa (visceral peritoneum)
outermost layer of GI tract, the part you see
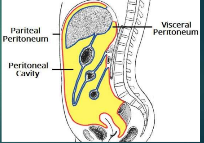
Parietal peritoneum
lines the wall of the abdominal cavity
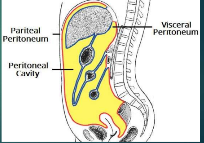
Visceral peritoneum
covers organs
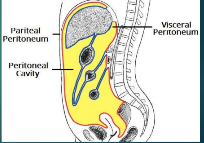
peritoneal cavity
open space between visceral peritoneum and parietal peritoneum
uvula
tissue protrudes past end of soft palate (hang down in back)
Medial Septum
divides tongue symmetrically lateral halves and tongue attached to hyoid bone inferiorly
tongue
composed of skeletal muscle covered by mucous membranes
lingual frenulum
attaches tongue to the floor of the mouth
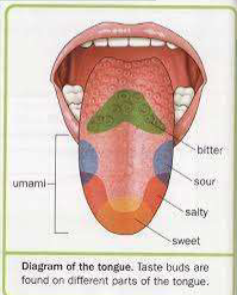
Papillae
bumps on tongue
filiform papillae- roughen tongue surface to help manipulate food
fungiform papillae- scattered and vascular TASTE BUD
vallate papillae - V shape row back of tongue TASTE BUD
foliate papillae- lateral aspects TASTE BUD
Salivary glands
lubricates and produces salivary amylase
Salivary amylase
enzyme, hydrolyse dietary starch into disaccharides and trisaccharides that are converted into glucose by other enzymes to supply the body with energy
Teeth order
Deciduous - 6 mo
Permanent= 32 total
6- 1 set molars
12- 2 set molars
18- 3 set molars or wisdom teeth
mastification
chewing
bolus
food reduced to a soft flexible mass
Voluntary process of deglutition
bolus forced to back of mouth cavity by the tongue
Pharyngeal process of deglutition involuntary
bolus stimulates nerves in orpharynx
impulses cause the soft palate to move up and seal off the nasopharynx
Esophageal process of deglutition
bolus pushed down esophagus by peristalsis
Peristalsis
-function of the muscularis (part of the mucosa layers) that is controlled by the medulla
- circular and longitudinal layers of the muscularis contract, forcing food down
-involuntary muscle movements
esophagus
collapsed tube behind trachea
stomach
j-shaped and inferior to diaphragm
Cardiac Sphincter
sphincter between esophagus and start of stomach
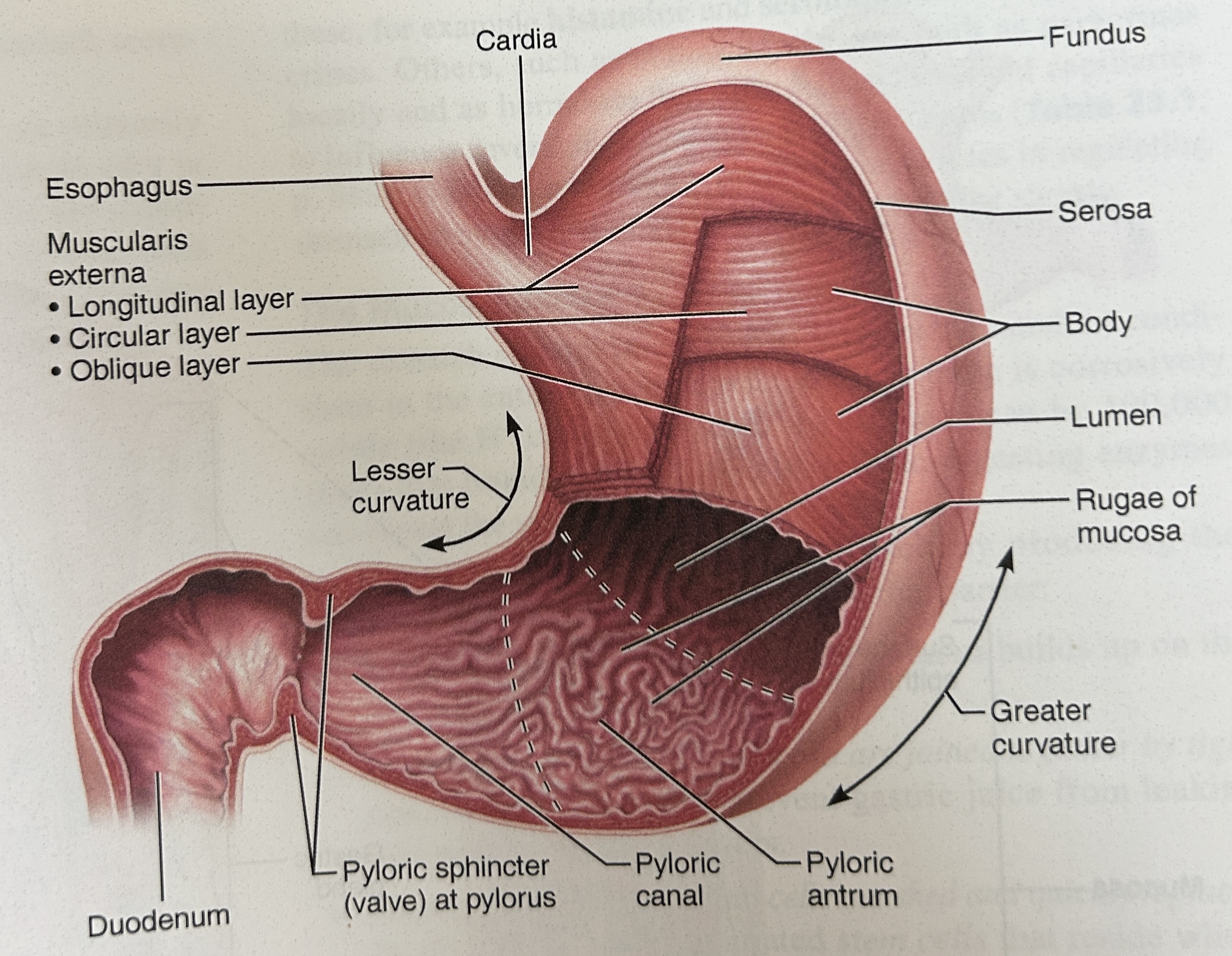
cardia (part of stomach)
closet to esophagus
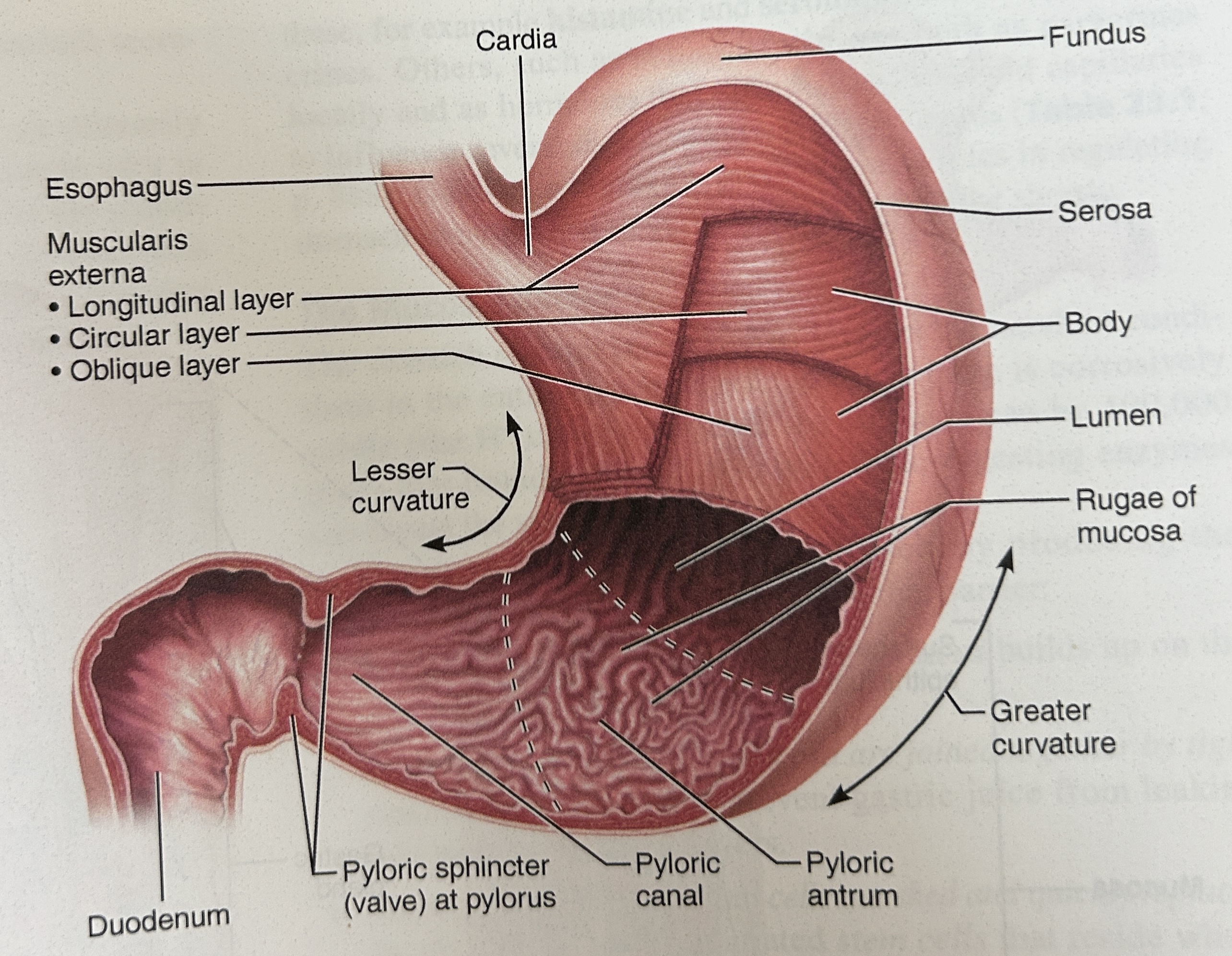
Fundus part of stomach
rounded portion above cardiac and space for extra food
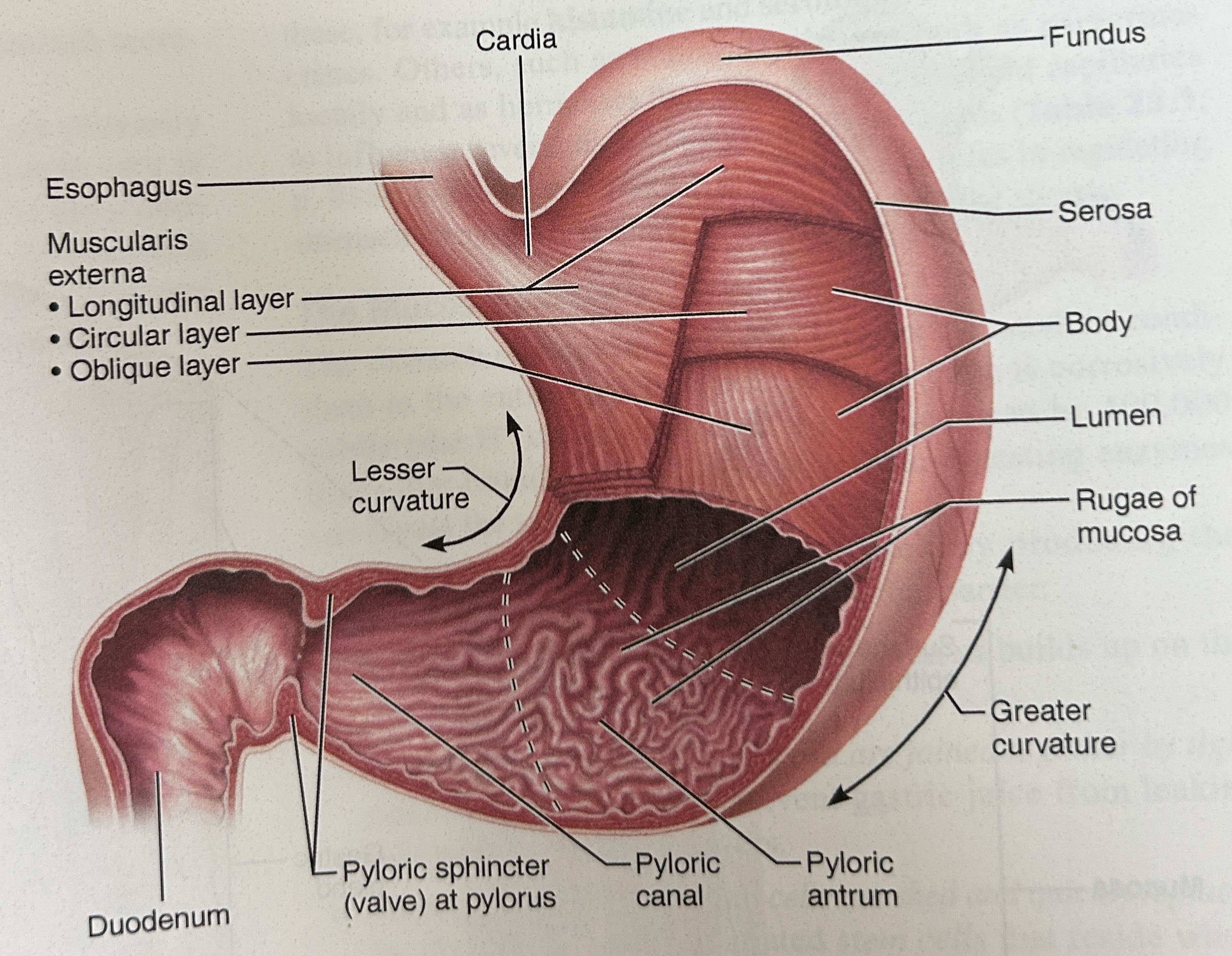
body of stomach
central portion and most of stomach
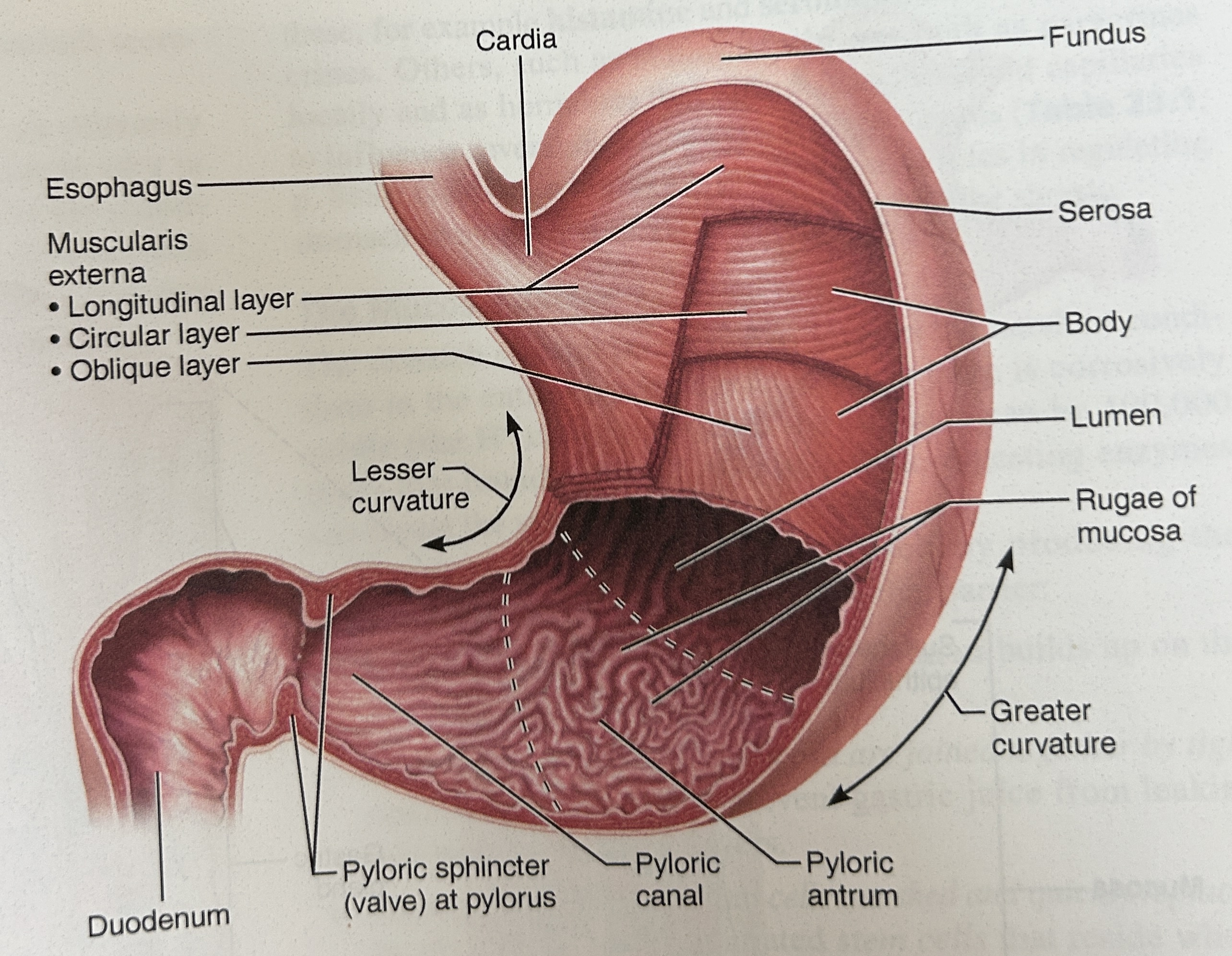
pylorus
narrow, inferior region prior to sm int
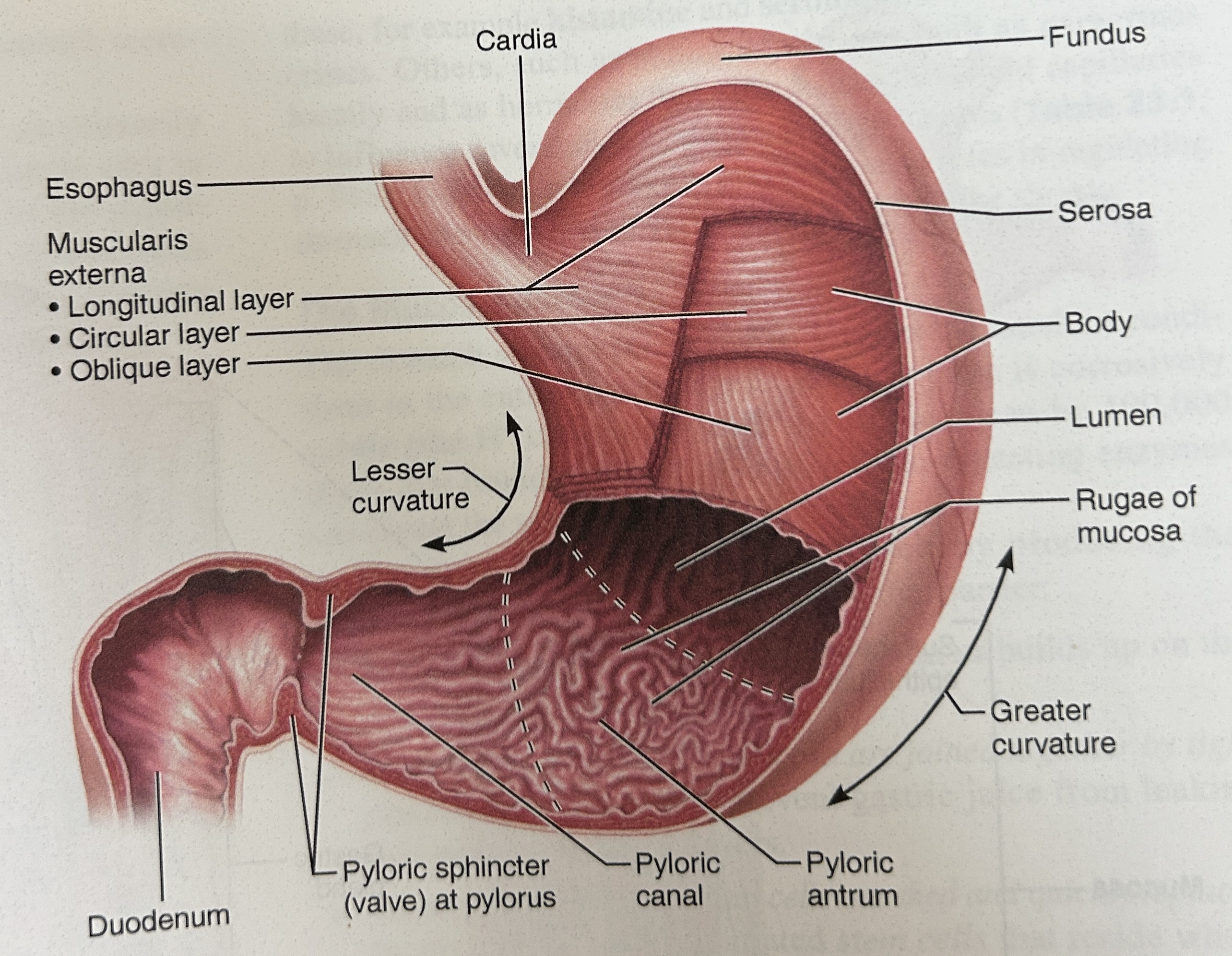
pyloric sphincter
Connection spot between duodenum (small intestine) and stomach
Function: controls stomach emptying
rugae
large folds of an empty stomach
chief cells
secrete pepsin, enzyme to chemically digest proteins
parietal cells
Secretes hydrochloric acid and intrinsic factor helps absorption of B12
Hydrochloric acid = super acidic stomach necessary for activation of protein-digesting enzyme, pepsin
enteroendocrine cells (gastric juice)
produce gastrin that regulates stomach secretion and motiliy, stims hcl and pepsin production
closes cardiac sphincter(opening) and relaxes pyloric sphincter (last)
Digestion in stomach
peristalsis movement begin and passes over stomach every 15-25 seconds
Gastric juices reduce bolus to a thin liquid=chyme
excess food stored in the fundus
mixing waves force chyme toward the pyloric sphincter
sphincter only allows a portion of chyme to pass
Chemical Digestion in Stomach (amino acids)
Pepsin breaks peptide bonds that hold amino acids together
only works in an acidic environment (ph of 2)
Alkaline mucous
lines stomach and prevents breakdown of stomach walls
Cephalic phase
before food enters the stomach,
sight, smell, taste, or thought of food = stimulation of the production of gastric juices
gastric phase
Food enters the stomach
Distention of the stomach that activates stretch receptors and initiates short/long reflexes travels to the medulla
Partially digested proteins and caffeine stimulate the secretion of stomach gastrin
Stomach gastrin increases the production of gastric juice, increases the coordinated contractions of the GI tract, and relaxes pyloric (bet. duodenum/stomach) and ileocecal spincters
intestinal phase
Overall effect=inhibition of gastric secretions
Stimulation caused by digested food entering duodenum of small intestine causing mucosal cells to release enteric gastric hormone that encourages gastric glands to continue to secrete UNTIL OVERRIDDEN BY INHIBITORS
Inhibition begins when distension of the duodenum or the presence of acidic, fatty, or hypertonic chyme
secretin (hormonal inhibitor)
stims pancreatic secretion
gastric juice inhibitors
secretin, cholecystokinin, GIP
cholecystokinin (hormonal inhibitor)
induces contraction of gallbladder that releases bile
GIP (Gastric inhibiting peptide)
stims release of insulin
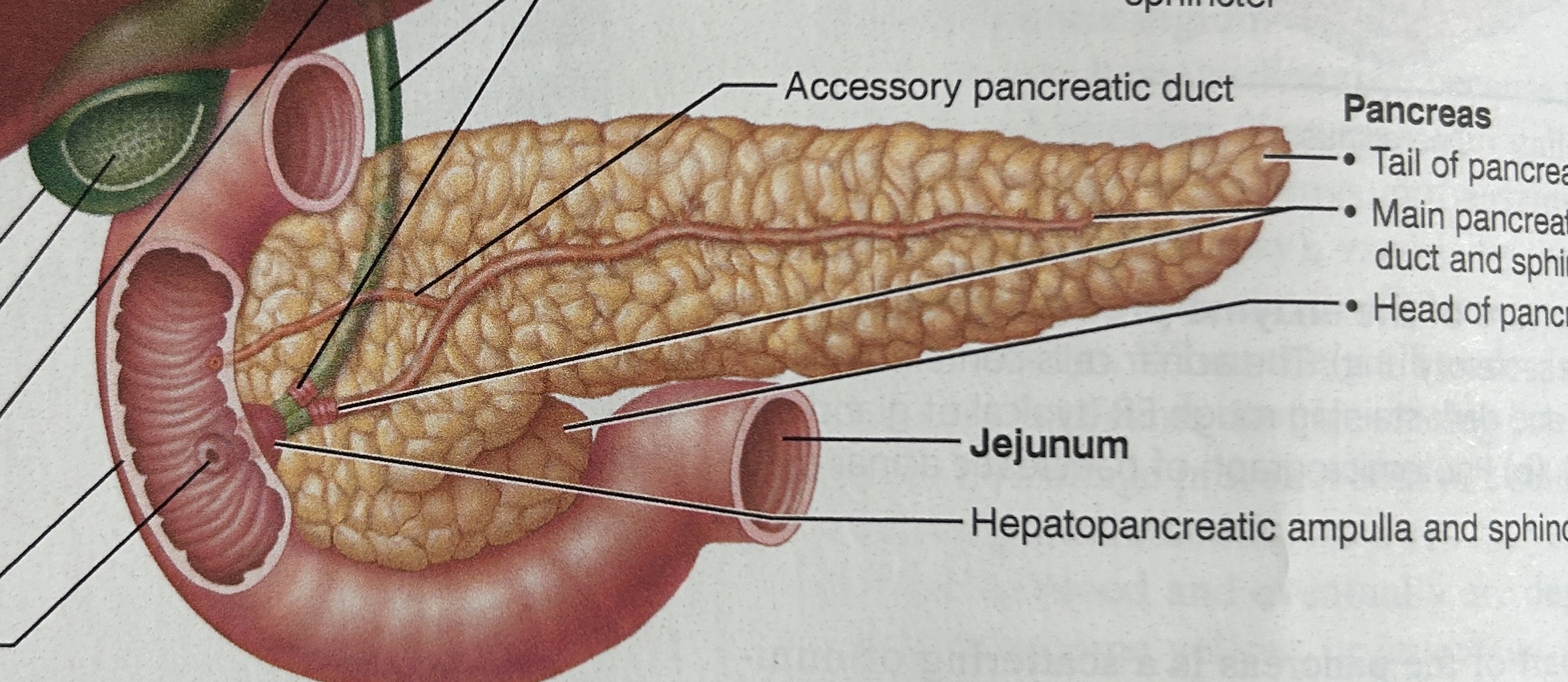
pancreas structure
oblong gland connected by two ducts to the duodenum
posterior (under) greater curvature of stomach
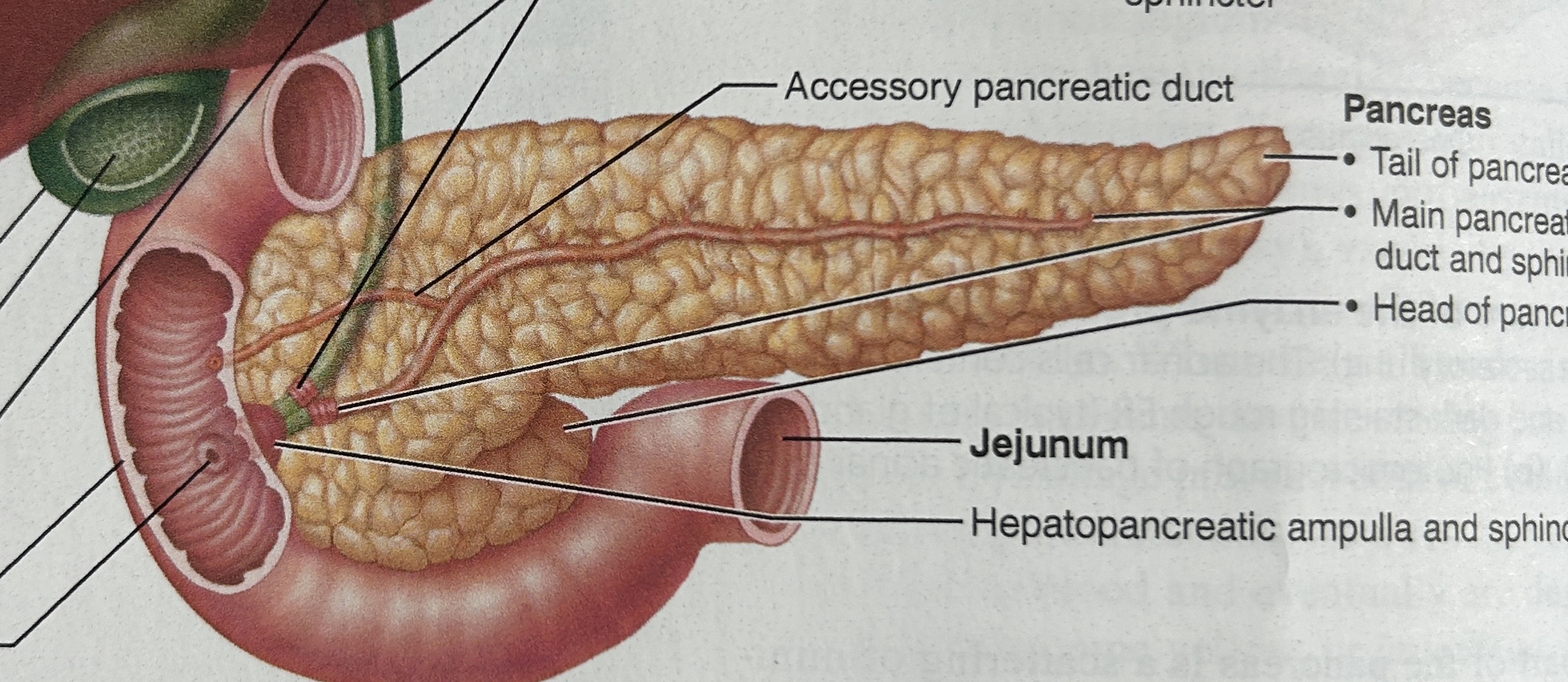
pancreatic duct
above ampulla
function: carrying pancreatic juice from the pancreas
unites with the bile duct from the gallbladder at the wall of the duodenum to fuse and form the hepatopancreatic ampulla
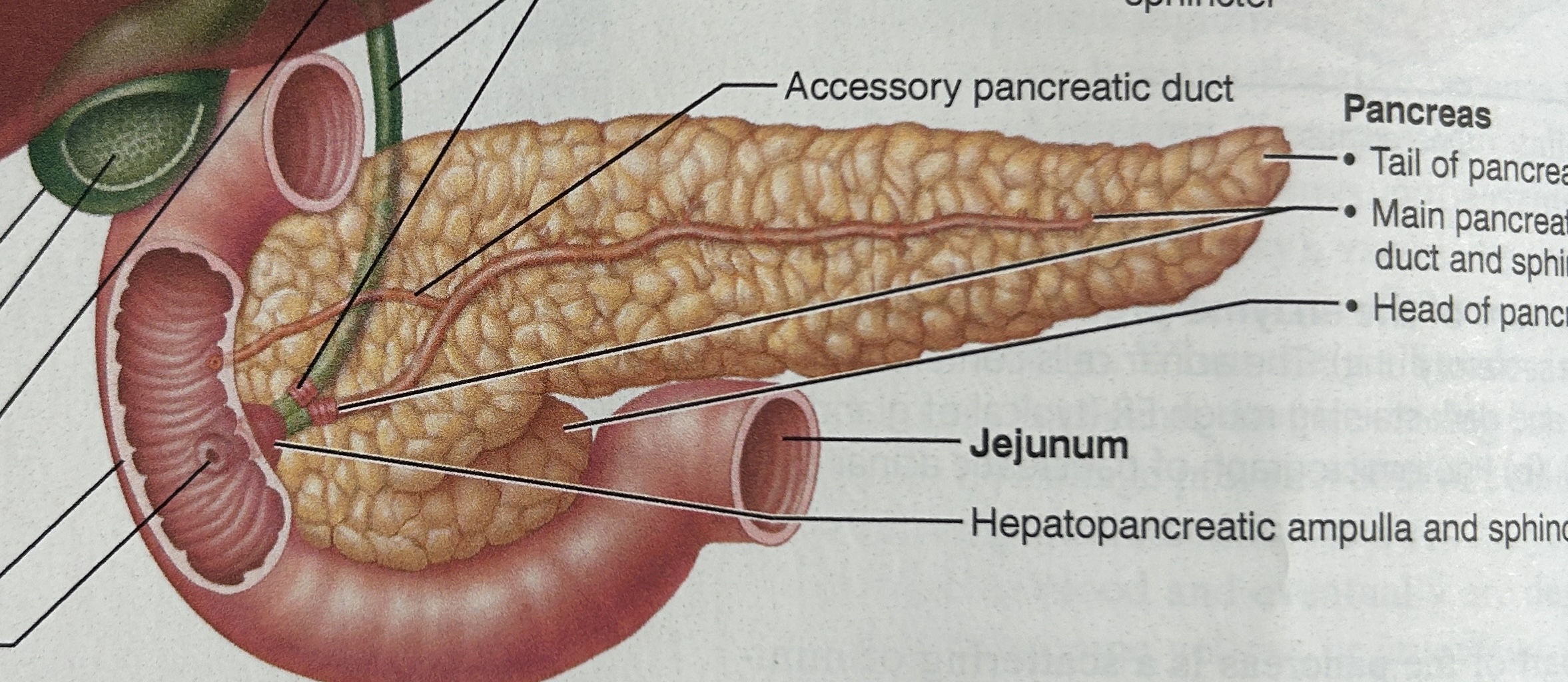
hepatopancreatic ampulla
empties pancreatic juice and bile into the small intestine below pylorus
pancreatic histology
Glandular epithelial cells include:
Islets of Langerhans = endocrine portion that secretes hormones like insulin (only 1%)
remaining 99% acini = exocrine glands that secrete digestive enzymes called pancreatic juice
pancreatic juice
slightly basic, enzymes for all foods, especially for lipids, secretion triggered by chyme entering duodenum
liver
4 lobes (largest=right lobe, left lobe(smaller seperated by fissure, caudate, and quadrate lobe) 1.4 kg in average adult
Function: producing bile for export to duodenum
lobules
functional unit of liver that are made of hepatocytes(liver cells) each surrounding a vein
At the corner of each bile is a portal triad that has:
hepatic artery for blood to the liver
hepatic portal vein carrying nutrient blood to digestive system
a bile duct
Lobules cells secrete:
bile
Kupffer’s cells
bile
yellow, brown, olive-green liquid with a pH of 7.6
mostly water with bile salts = emulsifiers that break down large fat
Kupffer’s cells-
destroy old RBC and WBC, bacteria, and toxins
Carbohydrate metabolism (Liver Physiology)
maintains normal blood glucose levels
Fat metabolism (Liver Physiology)
synthesises and digests cholesterol and stores fats
Protein Metabolism (Liver Physiology)
removal of nitrates
conversion of NH3 to urea
synthesizes plasma proteins
synthesis of anticoagulants and fibrenogen (blood coagulent)
conversion of amino acids
loss of this functiion = death
Liver Physiology steps 5 and 6
excretion and synthesis of bile salts
Removal of drugs and hormones (Liver Physiology)
detoxify penicillin, ampicillin, and excrete or alter into bile, estrogen, or aldosterene
Storage (Liver Physiology)
stores glycogen and vitamins A, B , D, E, K, iron, copper
Steps 8 and 9 (Liver Physiology)
Phagocytosis (kupffer’s cells) and activation of vitamin d
gallbladder structure
pear shaped sac, located in the fossa of the liver attach to right lobe
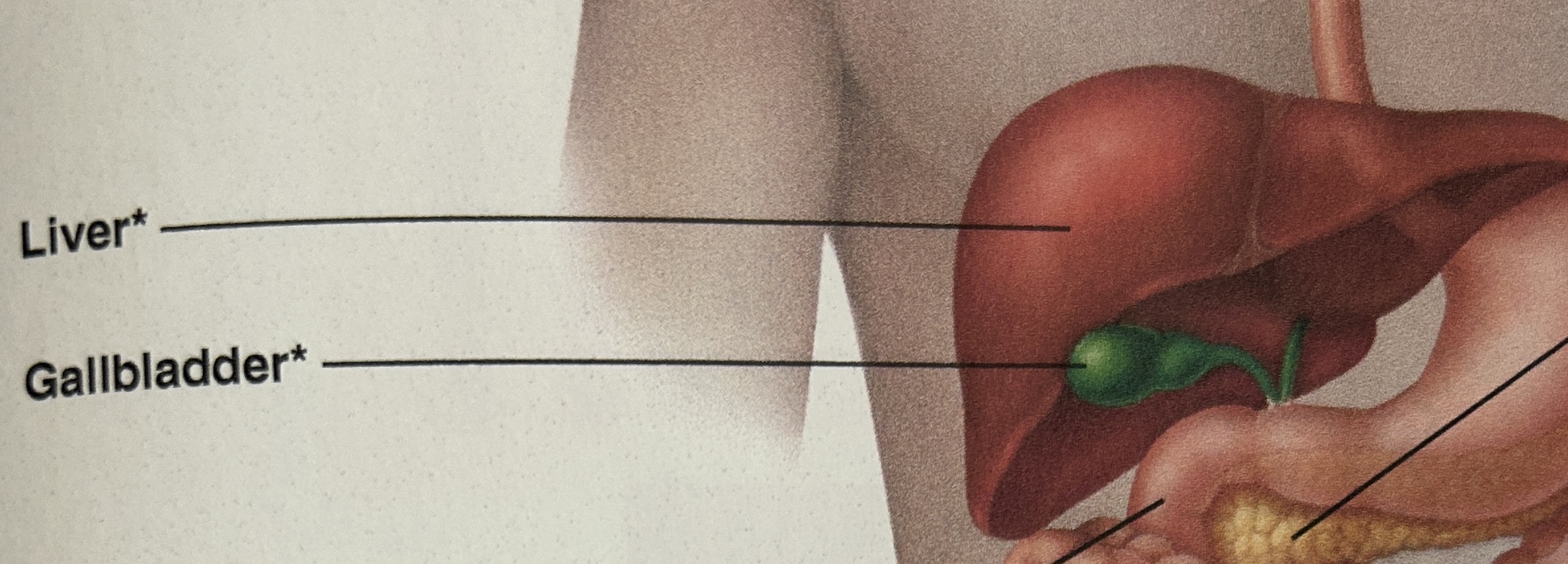
gallbladder physiology
Hormonal stimulation causes the smooth muscle to contract and squeeze contents into the cystic duct and common bile duct
stores and concentrates bile until small intestine needs
small intestine empty=closed hepatopancreatic ampulla = bile flows back to gallbladder
small intestine
6-7 m long, absorption and most digestion occurs here
mesentery (outer covering)
extends to the digestive organs from the body wall (tip is attached to the posterior abdominal wall)
supplies small intestine with blood supply and nerves
hold organs in place (binds small intestine to wall)
store fat
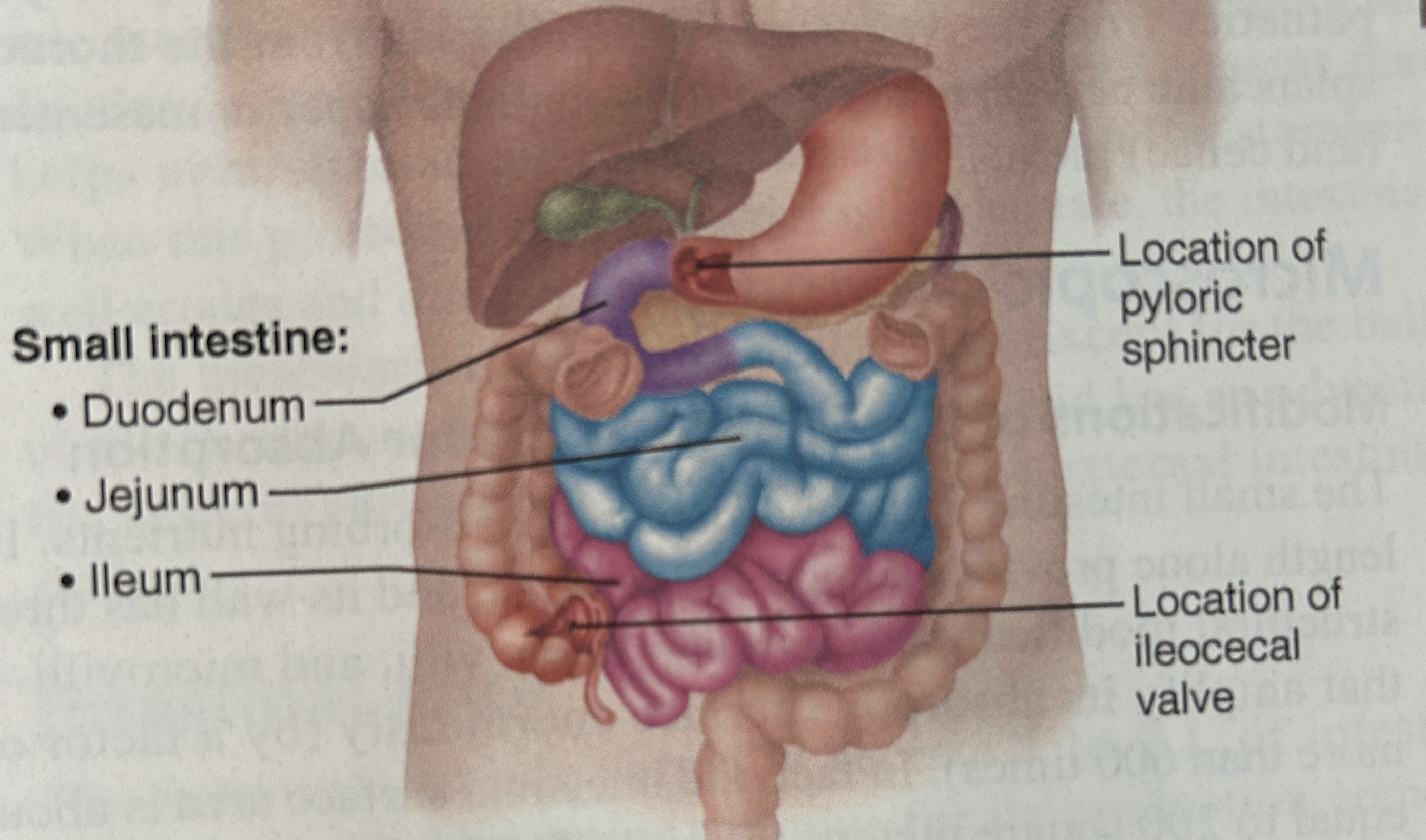
duodenum
1st 12 fingers width from pyloric sphincter
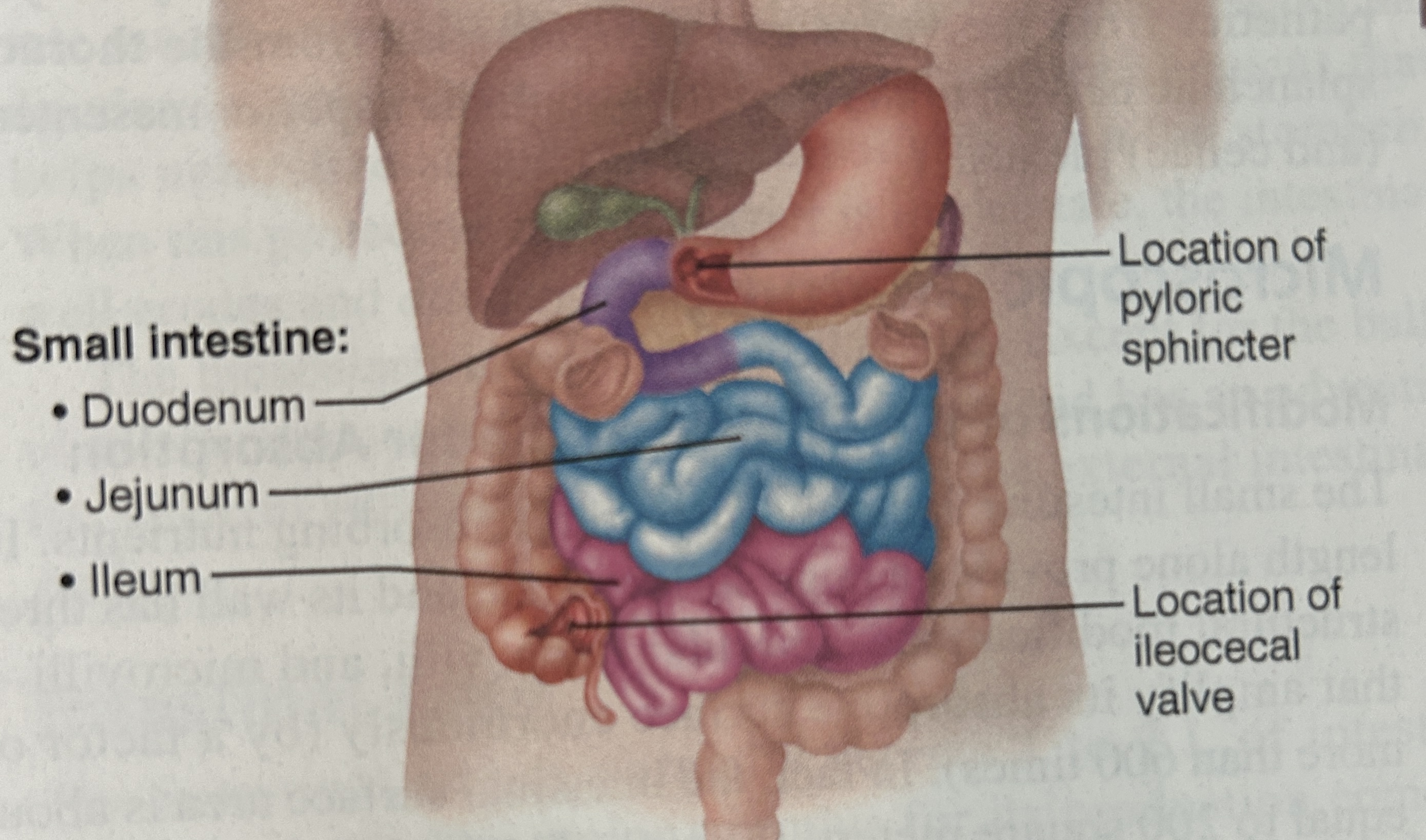
jejunum (squiggly part)
portion is empty at death
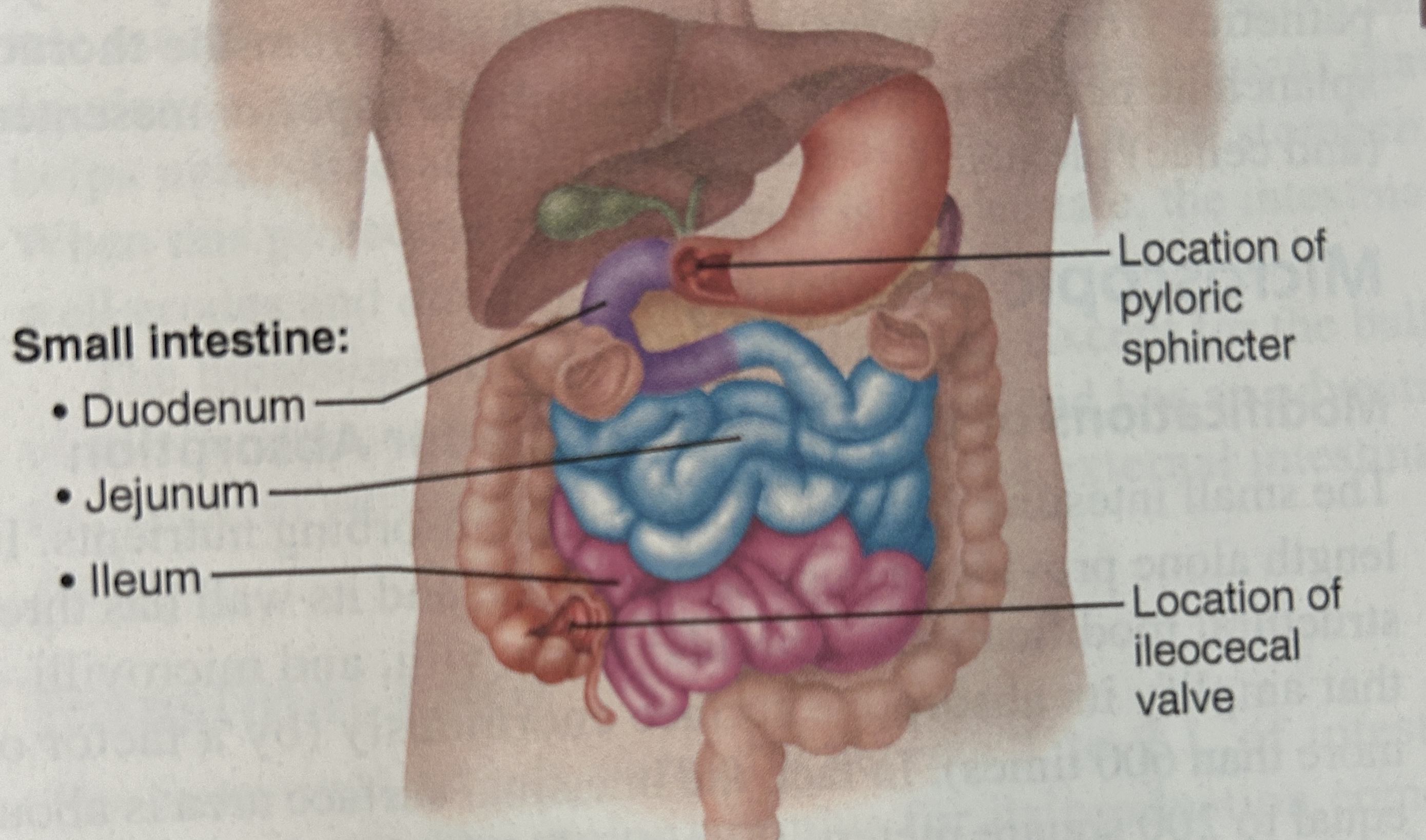
ileum
longest part, joints the large intestine at ileocecal sphincter
Histology of Small intestine
large surface area= better absorption
intestinal glands = secrete juices
duodenal gland
secrete alkaline mucous (that neutralizes acidic chyme)
length of small intestine allows?
times for chyme to pass through
villi
increase surface area for absorption
in core of each villi is a capillary bed and a lymphatic capillary called a lacteal
Digested food is absorbed into capillary blood and lacteal
contain: arteriole and venule also
circular folds
permanent ridges, causes chyme to spiral which enhances absorption by increasing the contact with vili
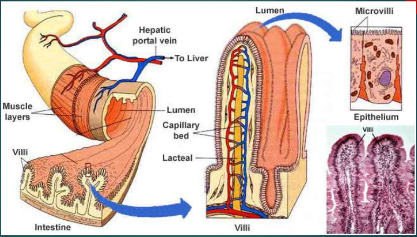
Microvilli
absorptive cells that form brush border that complete digestion of carbohydrates and proteins in small intestine
segmentation
localized contractions and doesn’t move chyme
Chemical
pancreatic juice, bile, intestinal juice complete breakdown of carbohydrates, proteins, and lipids
Absorption in small intestine
diffusion(high to low without energy/carrier)
lipid soluble molecules
short fatty chains
facilitated diffusion(high to low w carrier)
monosaccharides(carbohydrate)
Osmosis (low to high water)
Active transport (low to high w ATP)
amino acids
most carbohydrates
irons/electrolytes
Fats/lipid absorption
bile salts dissolve and form bubbles called micelles
micelles= come in contact with epithelial cells they allow contents to diffuse out into small intestine
lipoproteins
when lipids hitch rides with protein transporters
HDL (high density lipids)
removes cholesterol from arteriole walls to take to the liver
LDL (low density lipoproteins)
transport cholesterol to tissues for hormone production and causes buildup in arteries
water
absorbed by osmosis except for 1 liter
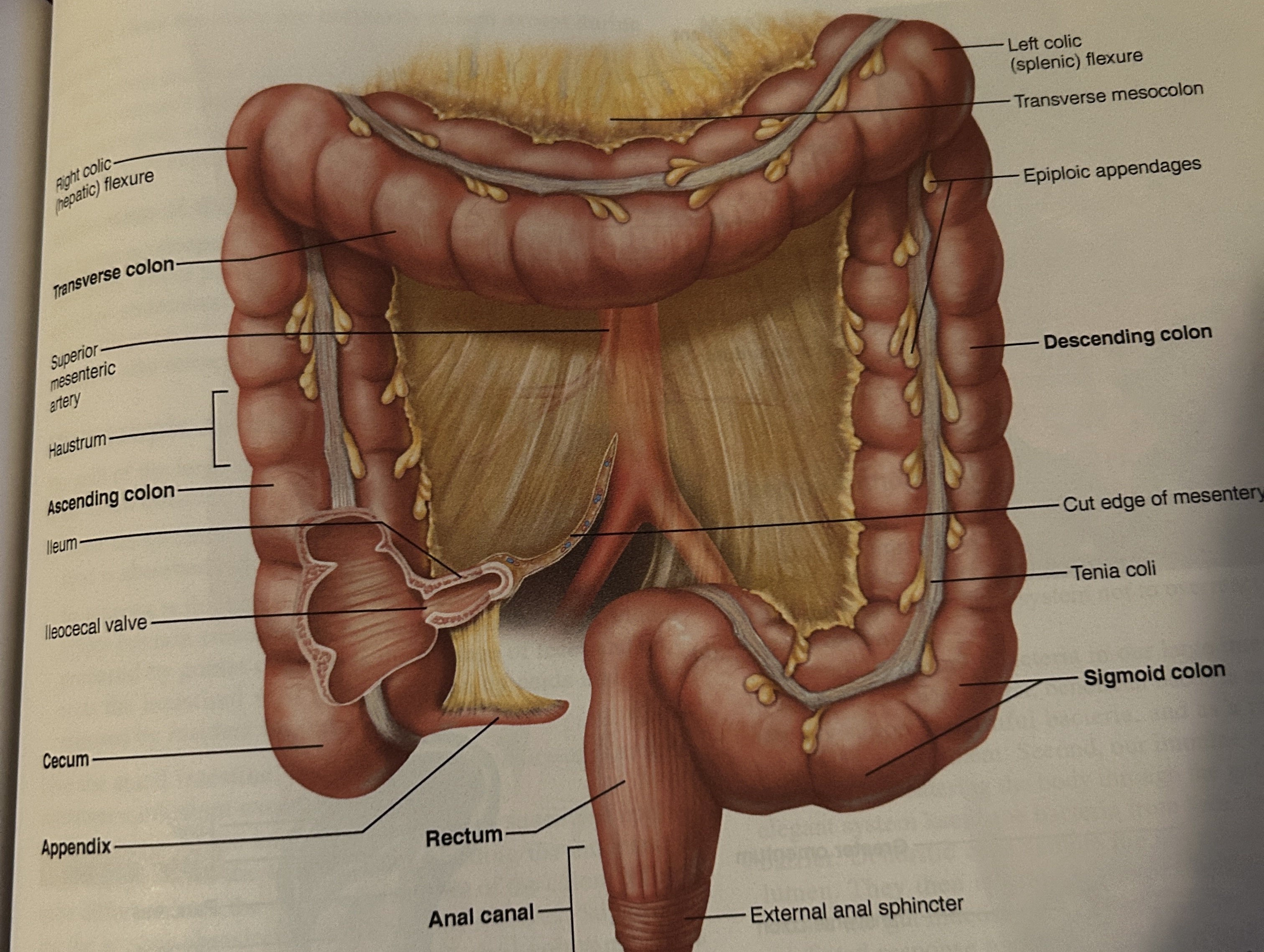
large intestine
completes absorption mostly water and forms/expels feces
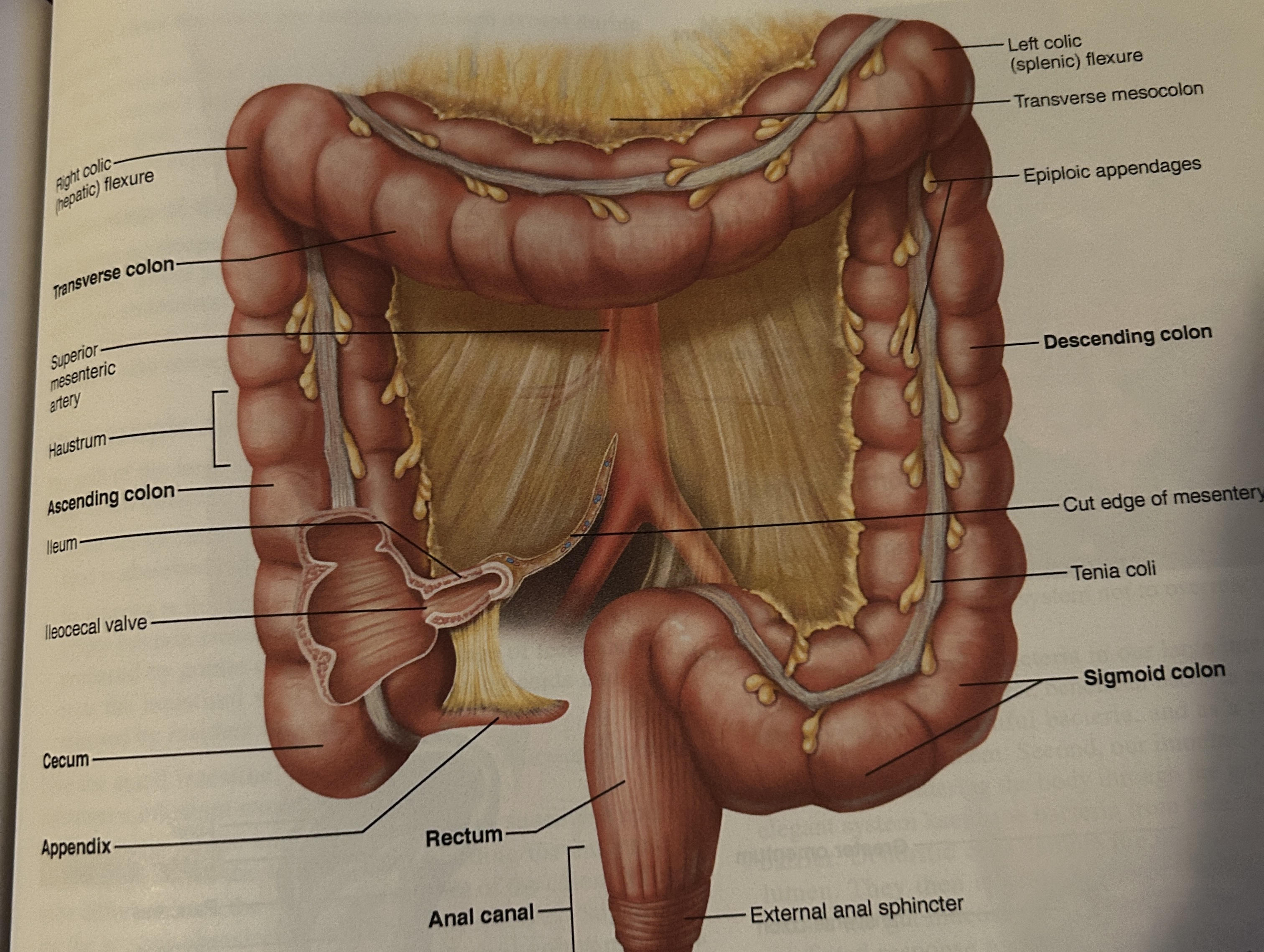
cecum structure
portion below ileocecal valve
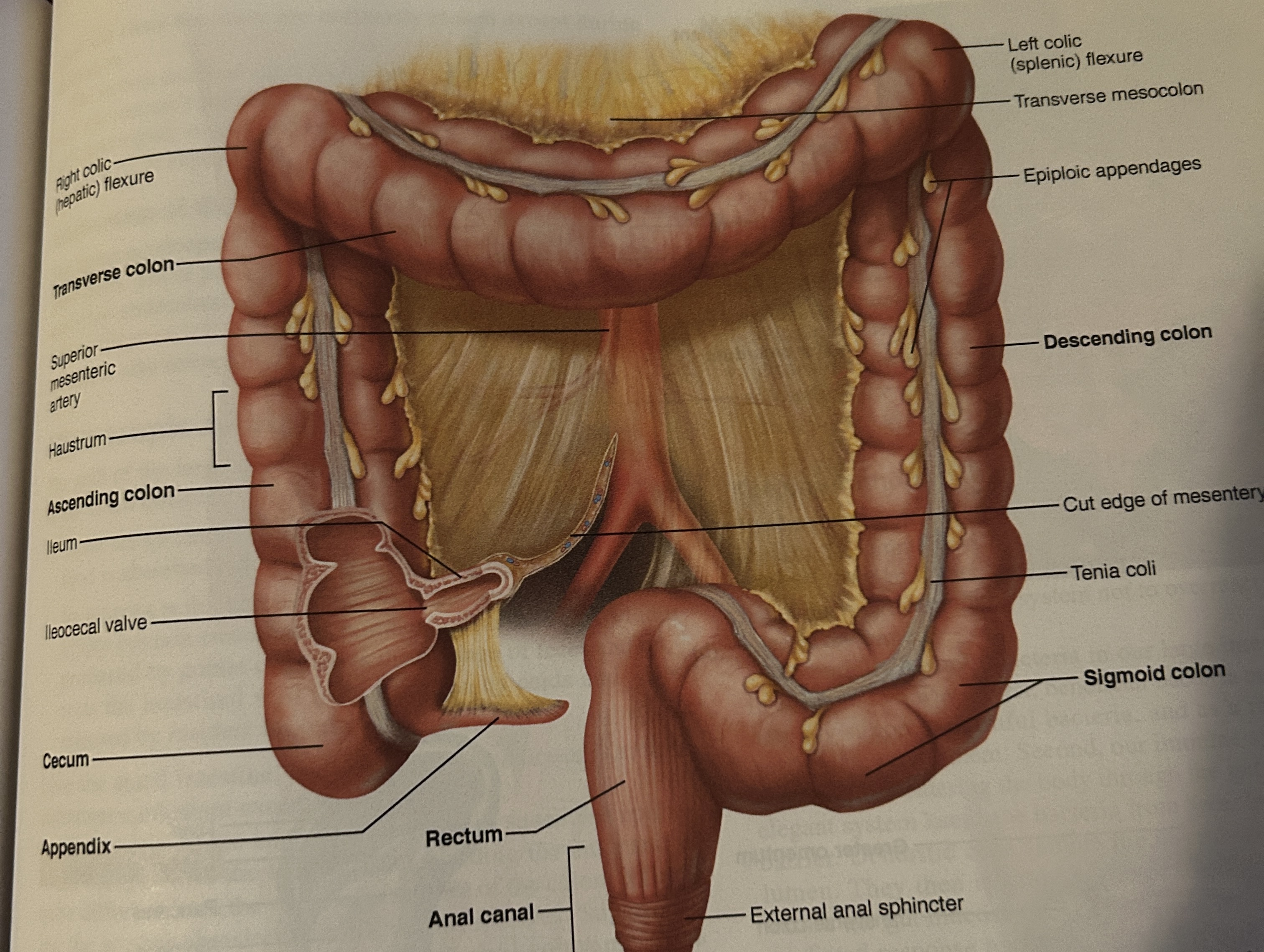
Where is the appendix located at?
attached to the pouch of cecum
colon
absorbs water, electrolytes, vitamins and solidifying waste into stool
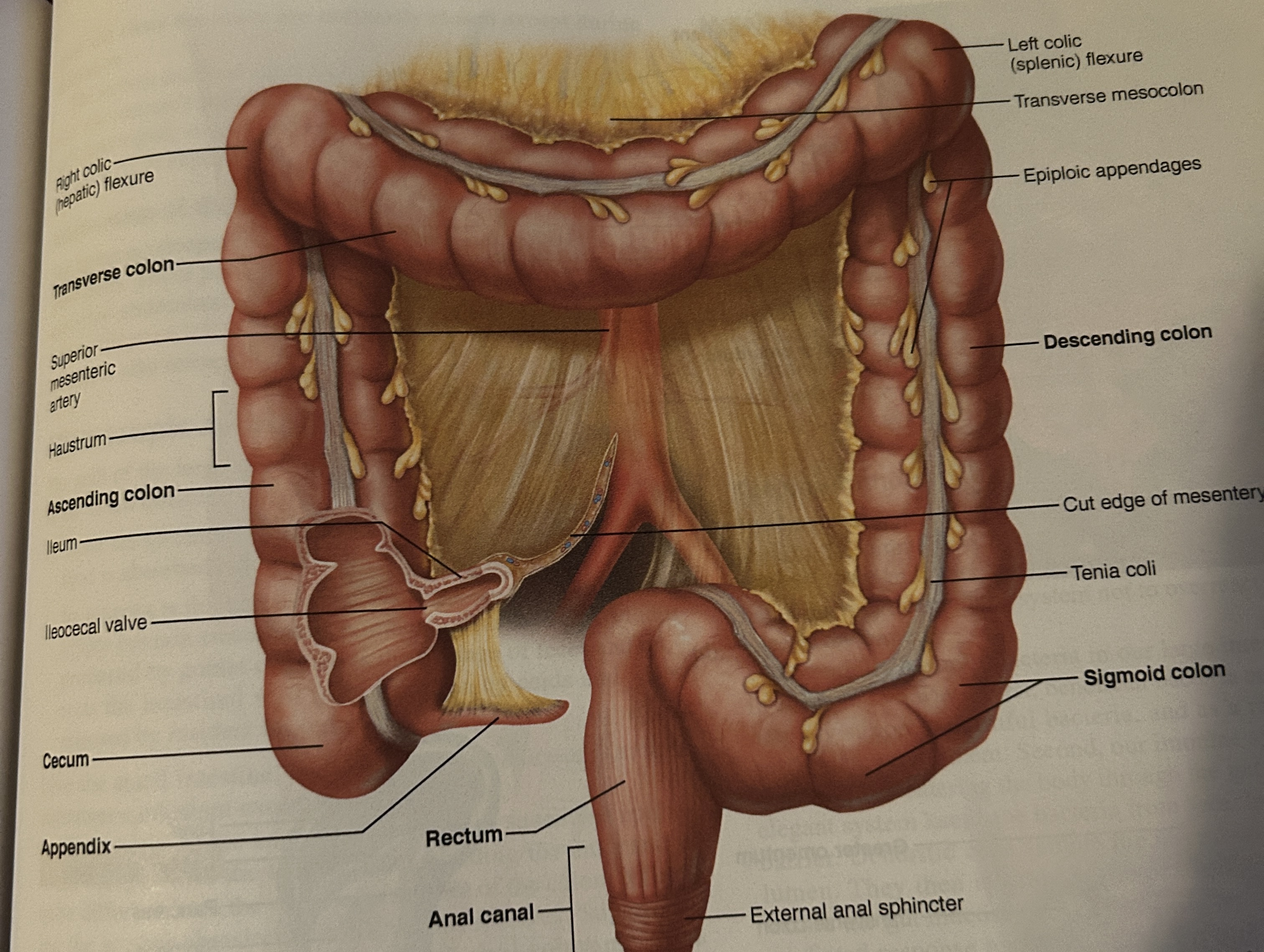
ascending colon
up
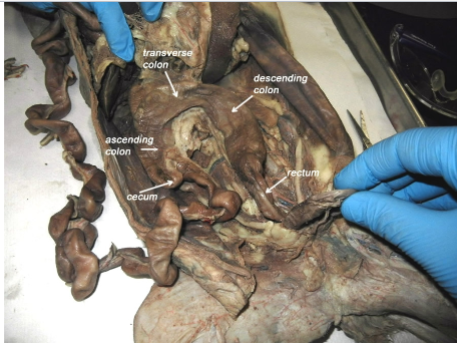
descending colon
down
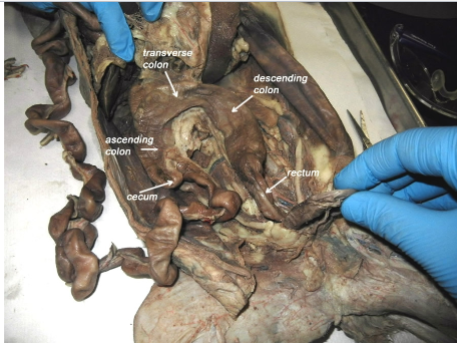
transverse
across
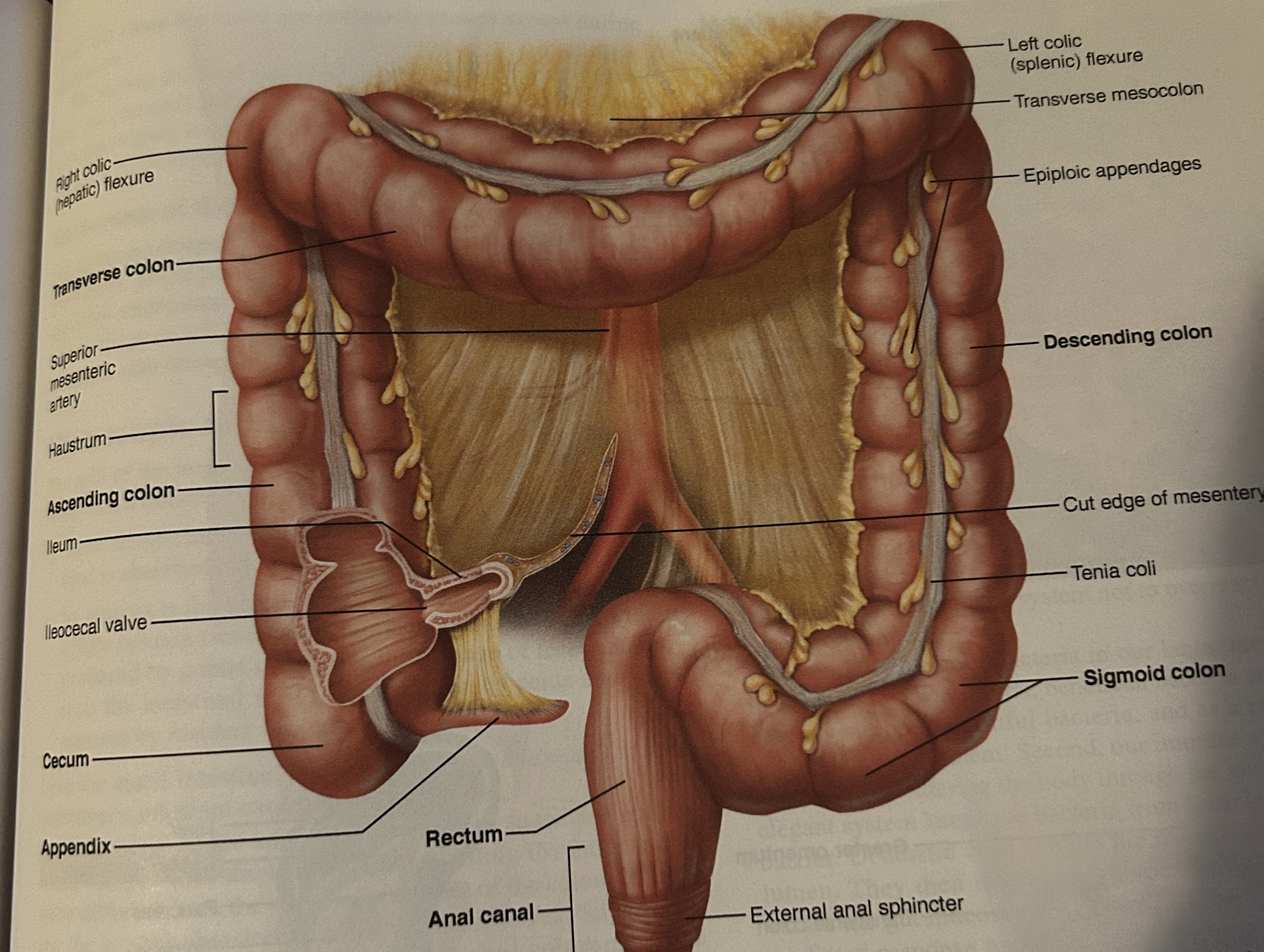
sigmoid colon
angles toward the midline of the body (s-shaped)
pepsin
breaks down dietary proteins into smaller peptides and amino acids in the stomach
rectum
last 20cm of the GI tract
anal canal
last 204cm of rectum