A&P 2: TopHat Lab 16
1/47
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
Kidney
Primary excretory organ of the body; filters the blood; keeps useful molecules and ions; gets rid of toxins, and metabolic wastes; regulates the volume of the blood by excreting or retaining water; regulates blood pressure by adjusting blood volume; regulates the pH of the blood by excreting excess H+ ions, which contribute to blood acidity; involved in the production of red blood cells, and the synthesis of vitamin D; approximately 11-12 cm long, 5-7 cm wide, and 3 cm thick; located in the lumbar region on either side of the spine, and lay against the body wall; embedded in fat, and lay beneath the parietal peritoneum; connected to the dorsal aorta by the renal arteries, and to the posterior vena cava by the renal veins
Urethra
Exits the urinary bladder and carries the urine to the outside
Renal cortex
Superficial layer of the kidney; shaded dark brown due to the dense system of blood vessels that aid in the filtering of blood in the kidney
Renal medulla
Inner layer of the kidney that contains the renal pyramids
Renal pyramid
Series of darker, conical regions found in the renal medulla; majority of nephron tubules occur in these regions
Renal columns
Inward extensions of the renal cortex into the renal medulla; separate the renal pyramids and help distinguish the different lobes of the kidney
Renal papillae
Tips at the base of the renal pyramids that project into a minor calyx; drain urine from the pyramids into the minor calyxes.
Minor calyx
Cup-shaped cavity at the base of the renal papilla; drains urine from the renal papillae into the major calyxes
Major calyx
Cavity formed by the convergence of several minor calyces; drains urine from the minor calyxes into the renal pelvis
Renal pelvis
Funnel-shaped cavity formed by the convergence of the major calyxes; collects urine from the major calyxes and joins the ureter
Ureter
Tube that conducts urine from the renal pelvis and kidney to the urinary bladder for storage
Renal capsule
Connective tissue covering the external surface of the kidney
Renal artery
Vessel which carries oxygenated blood from the aorta to the kidney to be filtered
Renal vein
Vessel that carries un-oxygenated and filtered blood from the kidney to the inferior vena cava
Leukocytes in Urine
Urine is normally sterile. Therefore, the presence of white blood cells in the urine suggests a urinary tract infection
Nitrite in Urine
Formed when bacteria in the urine change nitrate to nitrite; presence of this compound indicates a probable urinary tract infection
pH of Urine
Measure of the acidity or alkalinity of the urine; factors such as drugs, diet, time of day, and health affect the pH of urine. Normal pH of urine is 6.0, but can range from 4.5 to 8.0.
Protein in Urine
Large molecules not normally found in the urine, or only in small amounts; presence may be caused by severe emotional stress, strenuous exercise, fever or chronic causes may include diabetes, malaria, heart disease, high blood pressure, sickle cell anemia, or even pregnancy
Glucose in Urine
Usually reabsorbed by the kidney and is not found in urine; high glucose levels in urine can indicate diabetes, kidney damage, or stress
Ketone in Urine
Produced when fat is metabolized for energy; may indicate a low carbohydrate diet, starvation, or ketoacidosis.
Ketoacidosis
Life-threatening chemical imbalance that occurs in people with diabetes; caused when cells do not get enough glucose to meet energetic demands and begin breaking down fat for energy
Bilirubin in Urine
Not normally found in urine; formed from the breakdown of red blood cells; may indicate liver damage, or blockage of the flow of bile from the gallbladder
Urobilinogen in Urine
Usually only present in small amounts; forms from the breakdown of bilirubin; eliminated from the body through the bile, and goes into the digestive tract; may indicate liver damage or blockage of the flow of bile from the gallbladder
Blood
Normally not filtered by the kidney because they are too large to pass through the glomerulus; indicates damage to the kidney caused by inflammation, kidney stones, kidney disease, or blunt trauma. Menstruating females often show a positive result of this test, although the cells are not coming from the urinary system.
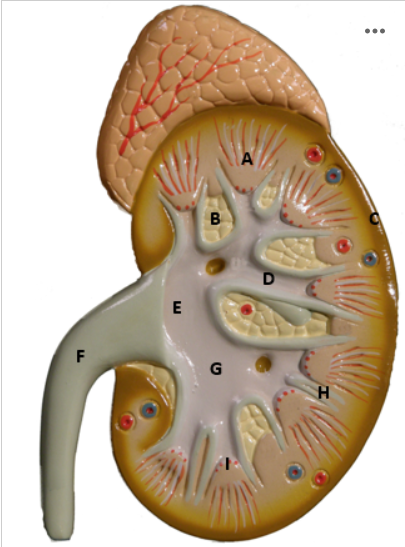
Identify A
Renal Pyramid - picture
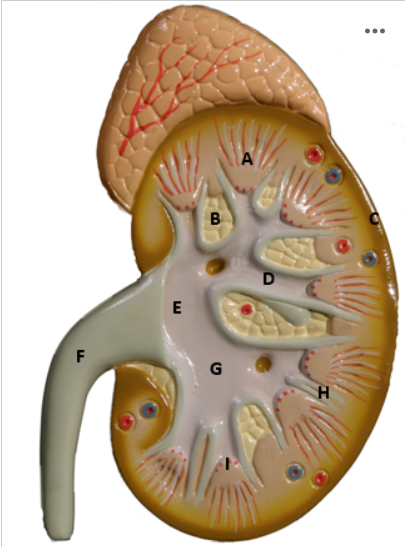
Identify B
Renal Column - picture
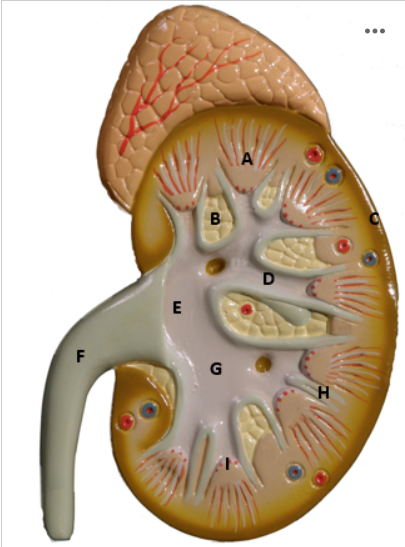
Identify C
Renal cortex - picture
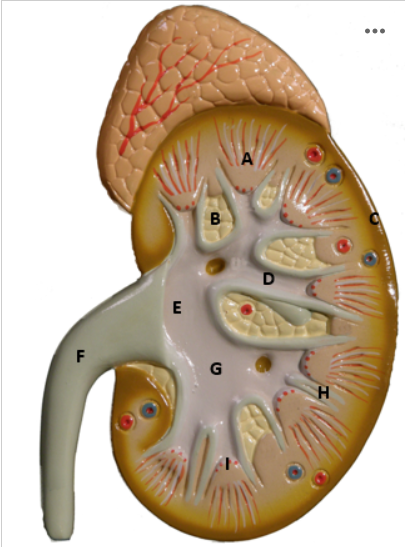
Identify D
Minor Calyx - picture
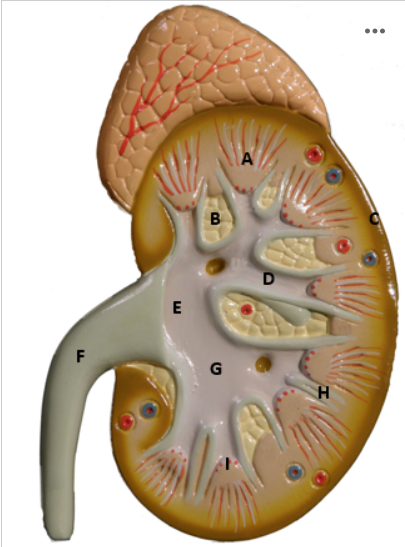
Identify E
Renal Pelvis - picture
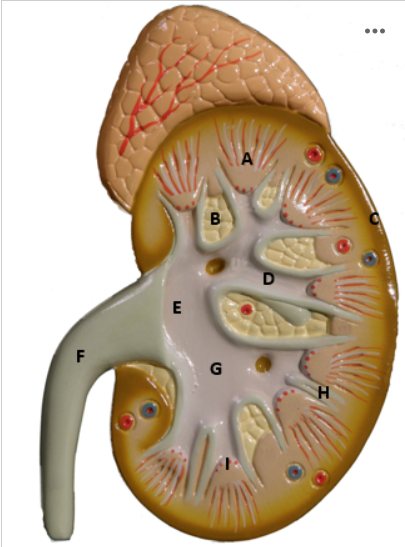
Identify F
Ureter - picture
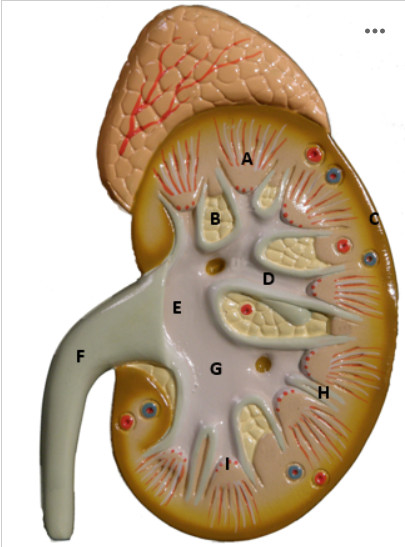
Identify G
Major Calyx - picture
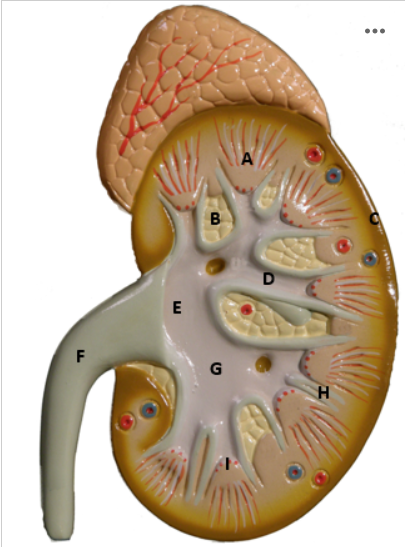
Identify I
Renal Papilla - picture
Cells in Urine
Epithelial cells result from a sloughing off of the lining of the urinary tract into the filtrate; presence of blood cells in the urine may indicate inflammation of the urinary tract or a urinary disease
Casts in Urine
Hardened proteins and cells that can form plugs in the shape of the distal convoluted renal tubule, or collecting duct; flushed from the tubules by the urine; form in very acidic urine, when proteins are present, and/or when the urine is very concentrated
Crystals in Urine
Form when minerals crystallize in the urine, due to either highly acidic or basic urine pH; normally, people have a few of these in their urine; may indicate kidney stones, or a metabolic problem
Centrifuge
Device that uses rapid rotation to generate high centrifugal force, separating substances of different densities
Method used for obtaining the sediments from the urine and making wet mount
Fill a centrifuge tube to the appropriate level indicated by the instructor.
Place the centrifuge tube in the centrifuge according to the instructions of your instructor.
Close the lid of the centrifuge.
Spin the urine at a speed of 15000 rpm for five minutes.
Obtain a clean microscope slide and coverslip. Put a drop of methylene blue stain on the center of the slide.
Pipette a drop of urine sediment onto the stain, in the center of the microscope slide.
Place the cover slip on the slide.
Examine the sediment under low and high magnification and look for the solid components
Squamous Epithelial Cells in Urine
Flat nucleated cells that shed from the lining of the urethra; have a large, non-uniform appearance
Transitional Epithelial Cells in Urine
Rough cuboidal cells that shed from the lining of the ureters, urinary bladder, and renal pelvis of the kidneys
Erythrocytes in Urine
RBCs found in urine; presence may indicate some kind of kidney damage
Leukocytes in Urine
Nucleated WBCs; presence may indicate a urinary tract infection
Erythrocyte Cast in Urine
A precipitate of RBCs in the shape of a tubule or duct
Leukocyte Cast in Urine
A precipitate of WBCs in the shape of a tubule or duct
Granular Cast in Urine
A precipitate of cells that remained in the duct but degenerated into a granular cast
Hyaline Casts in Urine
A cast composed of RBCs, WBCs, and oval fat droplets
Calcium Oxalate Crystals in Urine
Greenish crystals usually in the shape of an octahedron (polygon with 8 sides)
Uric Acid Crystals in Urine
Yellow to reddish-brown crystals, highly variable in shape
Calcium Phosphate Crystals in Urine
Have various forms, including six to eight sided prisms appearring in single or rosette shapes