Emma Holliday - Psychiatry
1/278
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
279 Terms
Schizophrenia:
Time duration and Brain histological findings
Chronic mental disorder with periods of psychosis, disturbed behavior and thought,
and decline in functioning that lasts > 6 months.
Associated with increase dopaminergic
activity, decrease dendritic branching.
Schizophrenia:
Symptoms needed for diagnosis
2 or more of the following
(first 4 in this list are "positive symptoms"):
~Delusions
~Hallucinations—often auditory
~Disorganized speech (loose associations)
~Disorganized or catatonic behavior
"Negative symptoms"—flat affect, social withdrawal, lack of motivation, lack of speech or thought
Most common type of schizophrenia
Paranoid type
Most treatable type of schizophrenia
Paranoid type
Prevalence in society of schizophrenia
1%
Schizophrenia:
~Risk of MZ twin
~Risk of sibling
twin = 50%
sibling = 10%
Positive symptoms for schizophrenia
Increased dopamine in the mesolimbic tract
Negative symptoms for schizophrenia
Decreased dopamine in the mesocortical tract
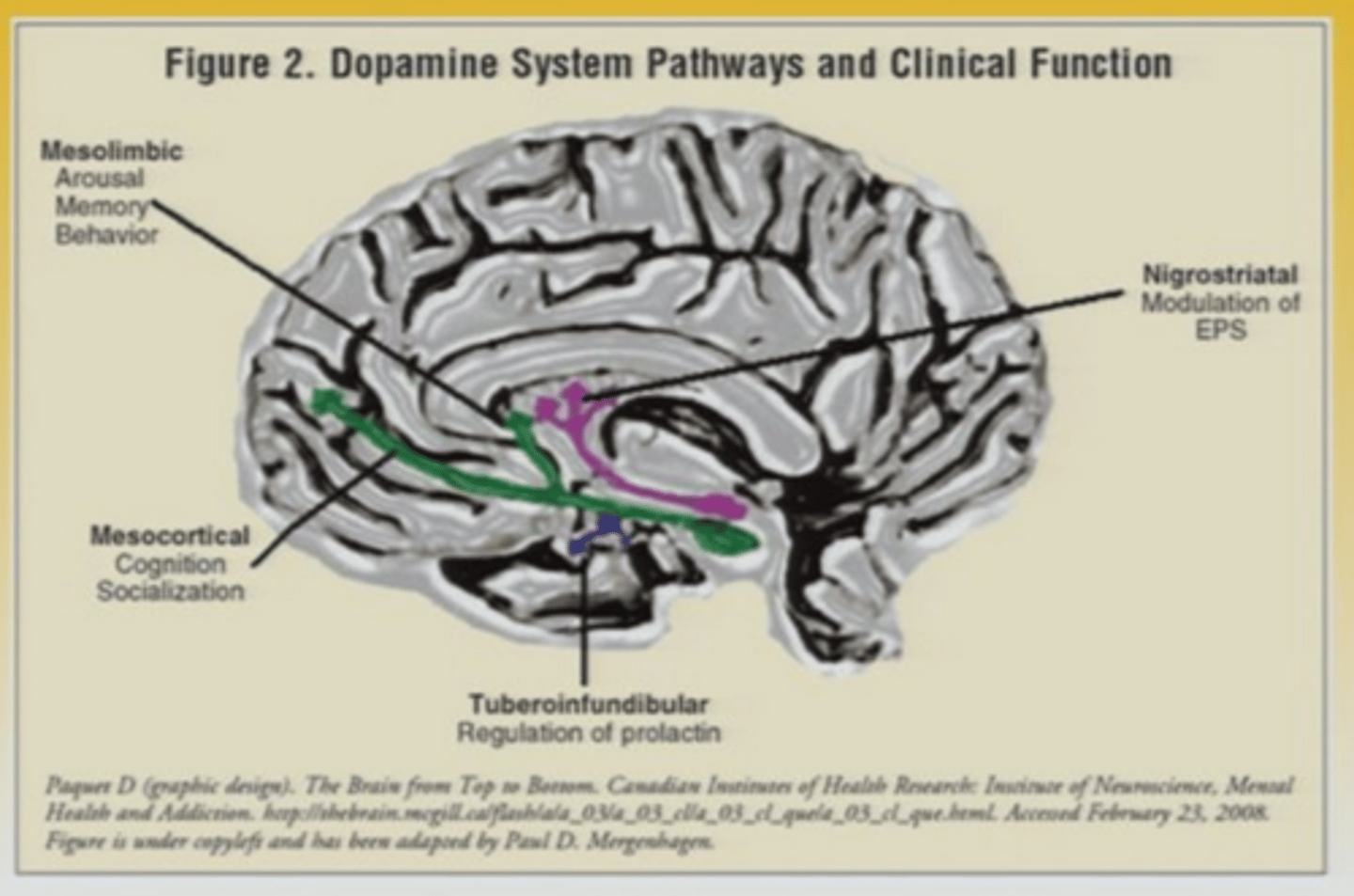
Dopamine systems of the brain
which one controls the: EPS
which one regulates prolactin
Diagnosis: Delusions hallucination and flattened affect for 3 weeks
Brief psychotic disorder ( > 1 WEEK AND <1 MONTH)
Diagnosis: Delusions hallucination and flattened affect for > 1 month and < 6 month
Schizopreniform disorder
Typical antipsychotics help what kinds of symptoms in schizophrenia
Positive symptoms, but no effect on the progression
Difference between schizoaffective disorder and depression with psychotic features?
What was present first without the other, i.e. schizoaffective thave had psychosis without any depressive symptoms
Diagnosis: MDD for 3 years and reports hearing voices telling him he is worthless and to kill himself
MDD with Psychotic Features; delusions are typically mood congruent
Treatment for MDD with Psychotic Features?
Atypical antipsychotic + SSRI or ECT (especially in pregnant patients)
Diagnosis: Persecutory delusions for past 3 years (diagnosed with schizophrenia), 6 months ago he started having sadness, guilt, insomnia, ↓ concentration, SI
Schizoaffective Disorder; delusions/hallucinations for > 2 weeks in absence of mood symptoms
Treatment for Schizoaffective Disorder?
Atypical antipsychotics
+ SSRI if depression
+ Li if manic
A man is convinced Miley Cyrus is in love with him, but is otherwise functional
Delusional Disorder, erotomanic type. Non-bizzare
Treatment for Delusional Disorder?
Therapeutic relationship + meds
Treatment: Acute agitation OR psychosis
IM haloperidol
--Quick onset of action
--D2 dopamine angtagonist
Haloperidol: Effects on nigrostriatal pathway and tubularinfundibulum?
Nigrostrial = causes EPS
Tubularinfundubulum = Hyperprolactinemia
Low potency antipsychotics:
Chlorpromazine and Thioridazine
--Less EPS, more anti-Ach
--Non-neurologic side effects (anticholinergic, antihistamine, and α1-blockade effects).
Side effects of Chlorpromazine?
Corneal deposits
Side effects of Thioridazine?
Retinal deposits
Side effects of haloperidol?
--NMS
--Tardive dyskinesia
Symptoms of Neuroleptic malignant syndrome (NMS)?
Rigidity, myoglobinuria, autonomic instability,
hyperpyrexia
Treatment for NMS?
Dantrolene, D2 agonists (e.g., bromocriptine)
Stop offending med, cooling blankets, and Dantroline Na or Bromocriptine
Neuroleptic syndrome:
FEVER
Fever
Encephalopathy
Vitals unstable
Enzymes elevated
Rigidity of muscles
High potency Antipsychotics:
Trifluoperazine, Fluphenazine, Haloperidol
—neurologic side effects (EPS symptoms)
Treatment of psychotic patient with a history of medication non-adherence?
Give injection/decanoate - Fluphenazine or Haldol every 2-4 weeks
Side effect: Purple grey metallic rash over sun-exposed areas and jaundice?
Chlorpromazine
Side effect: Prolonged QTc and pigmentary retinopathy?
Thioridazine --> can lead to torsades
Diagnosis: Medicated, psychotic patient wakes up with eyes "stuck" looking up or head "stuck" turned to the side
Acute Dystonia
<12 hours of beginning medication
Treatment for Acute Dystonia?
Benztropine or diphenhydramine
Diagnosis: Medicated, psychotic patient reports feeling like they "always have to move"
Akathesia
30 - 90 days of beginning medication
Treatment for Akathesia?
Propranolol (1st line) or benzodiapene
Diagnosis: Coarse resting tremor, masked facies, unsteady gait, bradykinesia
Parkinsonism
>6 months of beginning medication
Treatment of Parkinsonism side effects?
Treatment: Benztropine, diphenhydramine, amantidine or bromocriptine
NOT L-dopa!
Diagnosis: After 10 years on fluphenazine, tongue movements and grimacing
Tardive Dyskinesia
> Many years after starting antipsychotic
Treatment of Tardive Dyskinesia?
Stop antipsychotic and switching to and atypical or clozapine
Diagnosis: Within hours of a haloperidol injections, ↑CPK, T = 103F, rigidity, autonomic instability, and delirium
Neuroleptic Malignant Syndrome
Other causes: metoclopramide, compazine and droperidol
Antipsychotic medication: Weight neutral but prolongs the QTc?
Ziprazodone
Antipsychotic medication: Weight neutral but increases akathesia?
Aripiprazole
Antipsychotic medication: Atypical agent with highest risk for EPS and ↑prolactin?
Risperidone, also in depo form
Antipsychotic medication: Most associated with weight gain, BUT most common side effect is sedation?
Olazepine
Antipsychotic medication: Causes orthostasis and cataracts?
Quetiapine
--Alpha blocking properties
Antipsychotic medication: Good for treatment-refractory schizophrenia?
Clozapine
Most common side effects of Clozapine?
Sedation, weight gain, ↑blood sugar and lipids
Most dangerous side effects of Clozapine?
Agranulocytosis
Decreased seizure threshold
What do you monitor with Clozapine?
CBC --> ANC every week for 6 months and every 2 weeks for next 6 months
Stop Clozapine if WBCs < 3000 or ANC < 1500
What the most important and first question to ask the depressed patient?
Suicidal ideation, most likely to kill the patient
Risk factors for suicidal ideation?
#1 - Prior attempt
>45 years old, white male, serious illness, detailed plan, no support, use of ETOH and drugs
Polysomnogram for a depressed person?
Early REM latency and more frequent REM
Increased hormone in depressed patient?
Coritsol
Dexamethsone supression test would be abnormal
Medications that might cause depression?
IFN, beta-blockers, α-methyldopa, L-dopa, OCPs, ETOH, cocaine/amphetamine withdrawal, opiates
Medical diseases that might cause depression?
HIV, Lyme, Hypothyroidism, Porphyria, Uremia, Cushings Dz, Liver disease, Huntington's, MS, Lupus, L-MCA stroke
First line drug for treatment of depression?
SSRIs = Fluoxetine, paroxetine, sertraline, citalopram
Other conditions treated with SSRIs?
OCD, bulemia, anxiety, or premature ejaculation
Side effects of SSRIs
GI distress, sexual dysfunction (anorgasmia and decreased libido)
Fewer than TCAs
SSRI toxicity
Serotonin syndrome with any drug that increases 5-HT
(e.g., MAO inhibitors, SNRIs, TCAs
Symptoms of Serotonin syndrome?
Hyperthermia, confusion, myoclonus,
cardiovascular collapse, flushing, diarrhea,
seizures
Treatment of Serotonin syndrome?
Cyproheptadine (5-HT2 receptor antagonist)
SSRI with most drug-drug interactions?
Paroxetine
SSRI that can be discontinued without a taper?
Fluoxetine
SSRI with fewest drug-drug interactions?
Citalopram
Suddenly stopping SSRI and experiences HA, N/V/D dizziness and fatigue
5-HT discontinuation syndrome; more common with sertraline and fluvoxam
Diagnosis: Myoclonic jerks, tachycardia, hypertension, hyperreflexia, n/v/d
5-HT syndrome, particularly if the patient is taking both SSRI + MAOI
Patient experiences loss of erection/ejaculation on SSRI?
Switch to buproprione (dopamine and norepinephrine antagonist)
Contraindications of buproprione?
Due to increased rick of seizures:
Alcoholics
Epileptics
Bulimics
Drug: Erections lasting longer then 3 hours?
Trazodone
Drug: Anti-depressant for old, skinny, sad ladies?
Mirtazepine - Sedating, increases appetite
Drug: Anti-depressent NOT for hypertensives?
Venalfaxine
Drug: Anti-depressent NOT for patients taking St John's Wart?
Venalfaxine
Diagnosis: Pounding head, flushing, nausea, myoclonus after eating cheese, drinking red wine, taking decongestant or merperidine?
Hypertensive crisis with MAOI
Treatment for Hypertensive crisis with MAOI?
5mg IV phentolamine
Pediatric patient ingested unidentified pills. He now has dry mouth, tachycardia, vomiting, urinary retention, and seizures. EKG demonstrates widened QRS and prolonged QT intervals. What medication did the child ingest?
Tricyclic antidepressants
Most common cause of death in a kid who ingested TCAs?
Arrhythmia --> torsades, v-fib, and death
What is the treatment for tricyclic antidepressant overdose?
Sodium bicarbonate
--Helps metabolic acidosis
--Cardio protective
Patient who is eating and sleeping more, gaining weight, and has leaden paralysis in the morning.
Atypical depression
--Hypersensitive to rejection, affecting social functioning
Treatment for Atypical depression
MAOI
Diagnosis: One month following the death of her child, a mother feels guilty, can't sleep, concentrate, eat, or enjoy her interests?
Uncomplicated Bereavement
--No suicidal ideation (other than thoughts of wanting to be with loved one)
--No psychosis (other than hearing/seeing loved one)
Treatment for Uncomplicated Bereavement?
Rarely; treat with antidepressants for symptoms
Diagnosis: Four months following the death of her chihuahua, a woman still feels guilty, can't sleep, concentrate, eat, or enjoy her interests?
Adjustment Disorder
Symptoms present within 3 months of stressor and are out of proportion to inciting event
--Can't persist longer than 6 months
What is Adjustment disorder?
Emotional symptoms (i.e. anxiety, depression) causing impairment following an identifiable psychosocial stressor (e.g., divorce, illness) and lasting < 6 months
(> 6 months in presence of chronic stressor)
Treatment for adjustment disorder?
Psychotherapy
Prevalence of Bipolar disorder in the population?
1%
Prevalence of Bipolar disorder in MZ twin?
90%
Diagnosis: 75 year old man with first manic phase of lifetime?
Medical cause
--Right frontal hemisphere stoke
What is Generalized anxiety disorder?
Pattern of uncontrollable anxiety for at least 6 months that is unrelated to a specific person, situation, or event. --Associated with sleep disturbance, fatigue, GI disturbance, and difficulty concentrating
Treatment for GAD?
SSRIs, SNRIs, buspirone, cognitive behavioral therapy
How many symptoms and for how long do you need to have in order to diagnose schizophrenia?
Bizarre delusions or hearing voices = 1 month
Otherwise = 2 or more symptoms for 6 months
Incidence of mania in the population?
1%
Risk for diagnosis of mania in a MZ twin?
80-90%
Diagnosis: Symptoms of manic depression in 75 year old patient for the 1st time in that patient's lifetime?
Medical cause
--Right frontal hemisphere stroke
What medication need to be avoided in a patient with manic depression
SSRI and TCA can trigger mania
Medications to start in a manic depressive patient? For maintenance?
Haloperidol or clonazepam for acute agitation/delusion (if you cant interview them)
Maintenance: Lithium or valproic acid or carbamazepine
Diagnosis: Manic patient takes Advil and develops n/v/d, coarse tremor, ataxia, confusion, and slurred speech?
LIthium toxicity
Precipatated by NSAIDs
Preferred pain medications for patients on Li: aspirin or sulindac
EKG findings in Lithium toxicity?
--T wave flattening or inversion
--U inversions
Treatment For Lithium toxicity?
Depends on serum Li levels:
<4: Fluid resuscitiation
>4: Emergent dialysis
Side effects of Lithium?
Weight gain, acne, GI irritation, and cramps