Final- Clinical testing for microbes
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
Extrinsic factors, ocular surface disease, corneal epithelial abnormalities, & systemic conditions
What are some risk facors for bacterial keratitis?
microbial analysis
Clinical features of bacterial keratitis are not always enough to make a diagnosis, so ___________ can be employed to aid treatment
Culture & sensitivity test (cytology is non-specific)
If you are trying to determine a specific type of organism, what tests must be done?
empirically; treated based on observations, not culutres
>50% of microbial keratitis are treated how?
1. Central (edge within 3 mm of center), large (>= 2 mm in diameter), AC
cells (1+),
2. Infiltrates that extend to middle-deep corneal stroma. Appearance of stromal melting,
3. Unresponsive to broad-spectrum antibiotics,
4. Atypical cases that resemble fungal or amoebic keratitis,
5. Past Hx of corneal surgery,
6. Multiple infiltrates.
What are the factors taken into consideration when doing smears and cultures?
50-60%
Cultures only yield positive results in _______% of cases
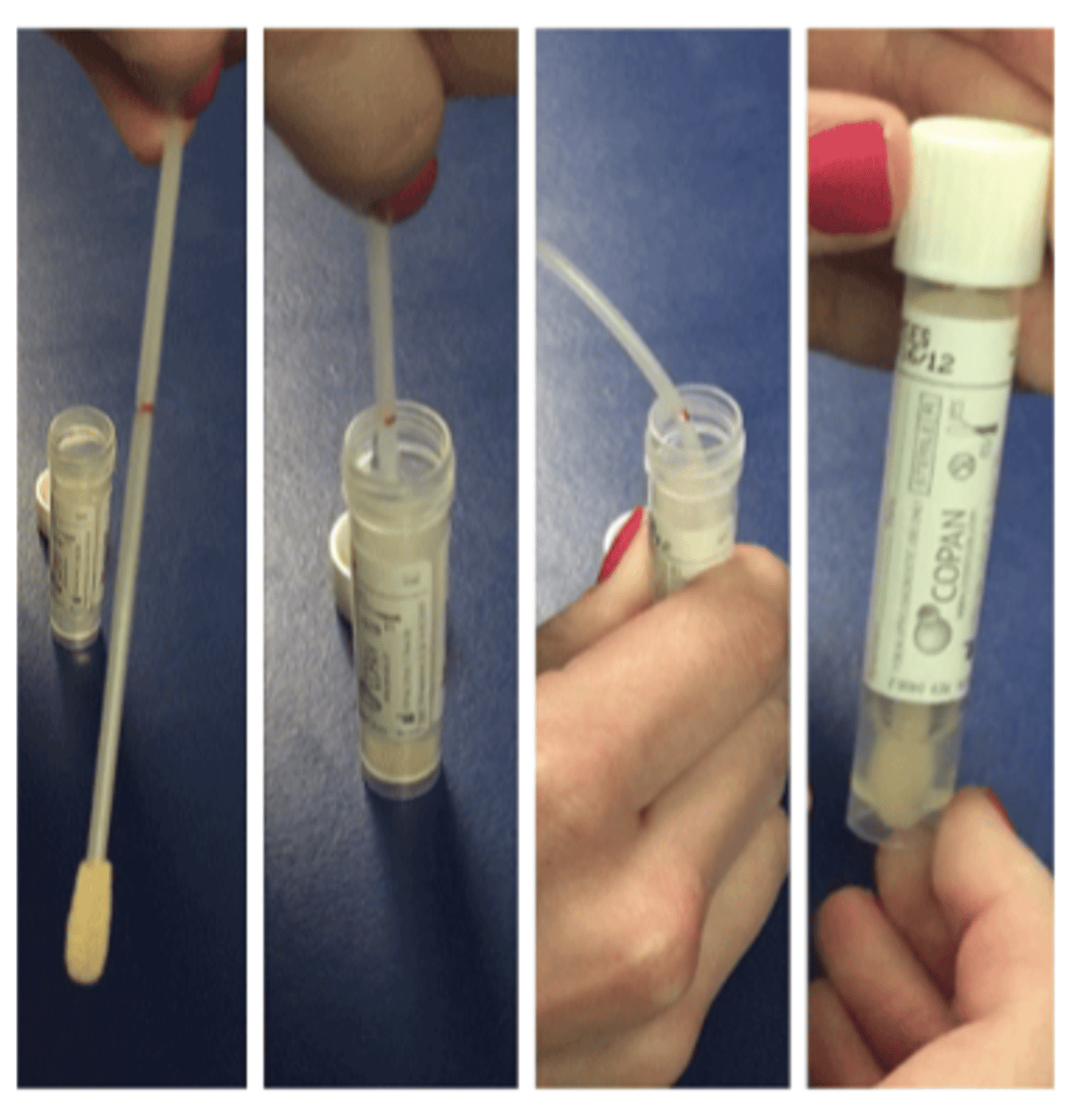
A sterile spatula, spud, or swab can be used to scrape an ulcer to collect a small amount of microorganism (anesthetic applied, collect from edge and base of ulcer, directly transfer sample to collection device).
We can also use cotton applicator, dacron swab, calcium alginate swab, cytobrush, kimura spatula, scalpel, impression.
What are some sample collecting methods?
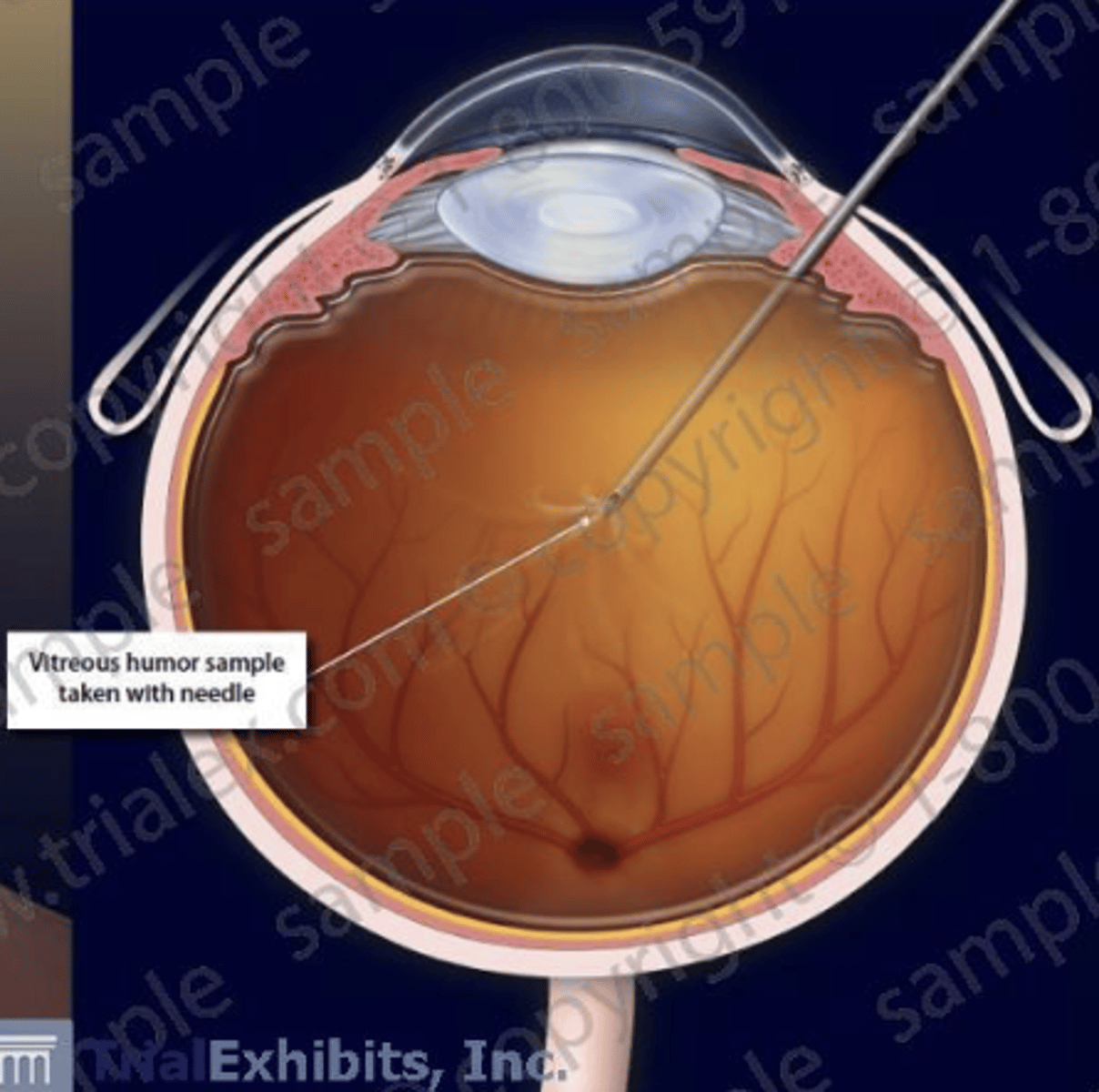
Aqueous/vitreous taps
What should be done if there's suspected microbial endophthalmitis (infection/inflammation inside eyeball)
Collection of superficial cells of conj in order to study under a microscope
1. Anesthetize eye,
2. Choose area to sample and apply filter paper,
3. Remove filter paper,
4. Repeat steps 2-3,
5. Air dry filter paper,
6. Fix and stain filter paper
How would you carry out impression cytology?
If treatment response is poor, if repeated cultures are negative, or if infiltrate is deep
When would we need to resort to a corneal biopsy?
1. Direct observation (slit lamp),
2. Microscopic observations (smears, confocal microscopy),
3. Culturing (plates, broths),
4. Diagnostic machines (PCR, ELISA, Adenoplus)
What are some analysis methods?
Distinguish between bacteria, fungi, and parasites
What is the purpose of a smear?
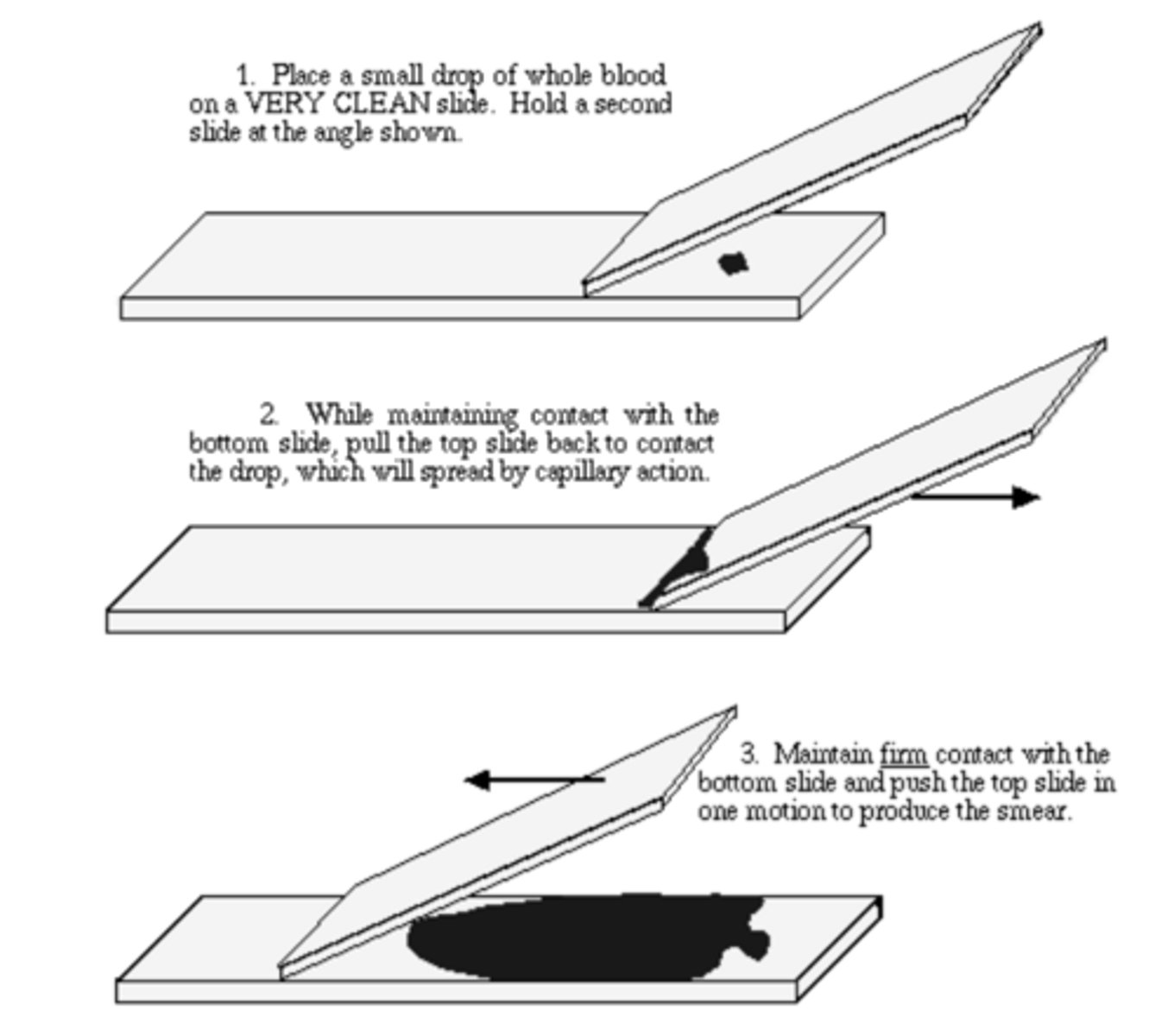
1. Place a small drop of blood on a clean slide,
2. Hold a second slide at an angle & while maintaining contact w the bottom slide, pull the top slide back to contact the drop,
3. Maintain firm contact with the bottom slide & push the top slide in one motion to produce smear.
How can you prepare a smear?
1. Gram stain= Bacteria, yeast, fungi, microsporidia.
2. Giemsa stain= Fungi, Acanthamoeba, microsporidia,
3. Acid-fast stain= Mycobacterium, nocardia,
4. Periodic acids-schiff= Fungi, acanthamoeba,
5. Potassium hydroxide= Fungus
What types of stains are used for different analyses?
Purple= Gram-positive (thick peptidoglycan wall)
Pink= Gram- negative (thin peptidoglycan wall)
After doing a gram stain you will observe either a purple or pink sample. What do each of these results mean?
When visualizing a "hazy" cornea under a slit lamp (it can offer up to 500x mag in comparison to slit lamp which offers around 40x mag).
What would be indicative that confocal microscopy might be beneficial?
Acanthamoeba & fungal keratitis (sensitivity of 88.3% & specificity of 91.1%)
What diagnoses would be beneficial to do confocal microscopy on?
No!
Would it be beneficial to do confocal microscopy on bacterial keratitis?
1. Slides should be available in clinic,
2. Collected samples need to be transported to lab,
3. Cultures incubated 1-2 weeks (growth seen in 2 days).
Describe the process of culturing
True
T/F: Viruses and parasites are not generally cultured
Agar plates= 60 days in refrigerator, broths= 1 year at room temp
What is the shelf life of agar plates and broths?
For aerobic & facultative anaerobic bacteria: p. aeruginosa, s. aureus, s. epidermidis, & s. pneumoniae
When would we use blood agar plates to culture?
For aerobic & facultative anaerobic bacteria: h. influenzae & n. gonorrhea
When would we use chocolate agar plates to culture?
For aerobic & facultative anaerobic bacteria
When would we use thioglycolate broth to culture?
On fungi
When would we use sabouraud dextrose agar to culture?
With non-nutrient agar
How would we culture E. coli (e.g. acanthamoeba- always know confocal microsc is prefered)?
1. Sample is collected and placed in a sample medium (medium is stable at RT for up to 18 months).
2. Sample is viable for 48 hours and preserved for PCR for up to 6 month.
3. Sample can be split into 10 different samples for analysis.
Describe the "one touch" culture method
Provides comparable results
What is the benefit to the one touch method over a traditional plating method?
Positive cultures are typically subjected to a panel of biochemical tests that allow for definitive identification of the organism!
What is susceptibility testing?
Disc diffusion method for bacteria= We typically use paper discs saturated in the anti-microbial factor & lie them on agar with the bacteria to see the effects
What is the most common susceptibility test?
Determine the minimum lethal concentration
What is the broth dilution procedure's main use?
When growth is confluent (>= 10 colonies) or if organism is seen in a smear
When would bacterial and fungal cultures be considered significant?
1. Susceptible= Orgnism is sensitive to normal dose of medication,
2. Intermediate= Organism is sensitive to high dosage of medication,
3. Resistant= Organism won't respond to antimicrobial med.
What are the possible susceptibility results that can be obtained from testing?
Analysis of serum samples;
1. IgM- tests for a new antigen that usually peaks a few weeks after exposure and disappears by 6 weeks.
2. IgG- tests for past exposure to a pathogen.
What is ELISA- Enzyme-Linked Immunosorbant Assays?
CBT
An enzymatic method for amplifying nucleic acids:
1. Collect tissue,
2. Oligonucleotide DNA primer sequences specific for the pathogens, Taq polymerase, and DNA building blocks.
3. Amplify with thermal cycling machine and visualized on gel or sequence.
**Allows us to look at DNA and compare to other agents to identify
What is a PCR- Polymerase Chain Reaction?
less than 24 hours; Great for slow growing/hard to identify organisms
How long does PCR take? What is the best use for PCR?
RPS Adeno Detector can detect adenovirus (through hexon proteins); 90%= true positive rate, 96%= true negative result.
What is the epidemic keratoconjunctivitis diagnosis?