The Reproductive System
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
95 Terms
zygote
is formed when sperm and egg fuse
is first cell of new individual and all body cells arise from it
homologous structures
male and female reproductive structures share a common origin during development
example: male testes and female ovaries, or male penis and female clitoris
primary sex organs (gonads)
testes (male) and ovaries (female) produce two products:
gametes
sex hormones
gametes
sperm (male) and ova (female
formed by cell division called meiosis
sex hormones (steroid hormoes)
testosterone (males) and estrogens/progesterone (females)
vital in development and function of reproductive organs and other organs/tissues, sexual behaviours, sexual drives
accessory reproductive organs
ducts, glands, and external genitalia
hypothalamic-pituitary-gonadal (HPG) axis
production of gametes and sex hormones is regulated by sequence of hormonal events involving hypothalamus, anterior pituitary gland, and gonads
involves interacting hormones: GnRH, FSH, LH, testosterone, and inhibin
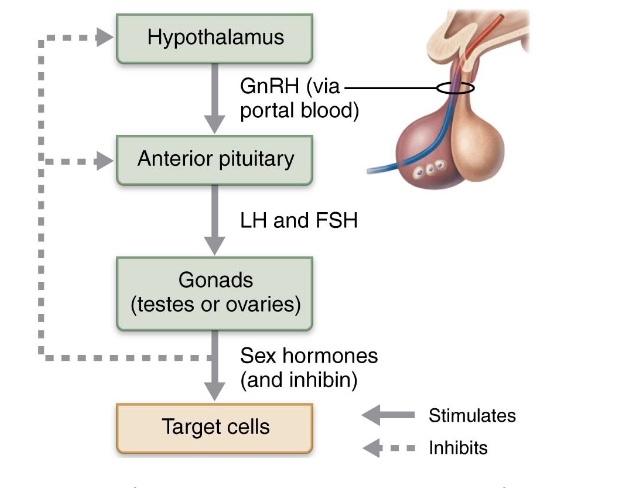
gonadotropin-releasing hormone (GnRH)
released from hypothalamus reaches anterior pituitary cells via hypophyseal portal system
follicle-stimulating hormone (FSH) and luteinizing hormone (LH)
gonadotrophin released from anterior pituitary
inhibin
released from gonads of both male and female
exerts negative feedback on FSH release from anterior pituitary
puberty
period of life when reproductive organs grow to adult size and become functional; earliest time that reproduction is possible
activation of the HPG axis at puberty
before puberty small amounts of sex hormones stop the hypothalamus from releasing GnRH
as puberty begins the hypothalamus becomes less sensitive to this “stop signal” and it starts released GnRH in pulse
soon the GnRH tells the anterior pituitary to release FSH and LH; these tell the gonads (ovaries/tested) to make more sex hormones
over time, the body needs higher hormone levels to stop GnRH and hormone release increased until the adult hormone cycle is reach
meiosis
unique kind of nuclear division that occurs only in gonads
same process for males and females
sexual production cannot take place without this
it reduces the number of chromosomes in gametes by half so zygote does not end up with twice as many chromosomes
sister chromatids
cells DNA is replicated during interphase
each chromosome has two sister chromatids that are identical and joined together by centromere
DNA coils and condenses, making chromosomes visible when viewed through light microscope
homologous pairs of chromosomes
one member of each pair is from father (paternal chromosome) and other is from mother (material chromosome)
look alike and carry same genes that code for same traits
testes
sperm-producing male gonads that lie within the scrotum
accessory sex glands: seminal glands, prostate, and bulbo-urethral glands
two tunics of testes
tunica vaginalis
tunica albuginea
tunica vaginalis
outer layer derived from peritoneum
tunica albuginea
inner layer forms fibrous capsule
seminiferous tubules
site of sperm production
conversion of sperm
seminiferous tubules → straight tubule → rete testis → efferent ductules → epididymis
accessory ducts carry sperm from testes to body exterior:
epididymis
ductus deferens
ejaculatory ducts
urethra
epididymis
sperm mature in epididymis
head contains efferent ductules that empty into highly coiled duct of epididymis
ductus deferens
~ 45 cm long
passes through inguinal canal to pelvic cavity
expands to form ampulla
joins duct of seminal vesicle to form ejaculatory duct
vasectomy
cutting and ligating ductus deferens; nearly 100% effective form of brith control
seminal glands (seminal vesicles)
on posterior bladder surface
contains smooth muscle that contracts during ejaculation
produces viscous alkaline seminal fluid
duct of seminal gland joins ductus deferens to form ejaculatory duct
prostate
encircles urethra inferior to bladder
size of peach pit
consists of smooth muscle that contracts during ejaculation
secretes milky, slightly acid fluid
bulbo-urethral glands
pea-sized glands inferior to prostate
produce thick, clear mucus during sexual arousal
spermatogenesis
process of forming new male gametes
occurs in seminiferous tubules
begins at puberty, around 14 years of age
adult males make ~ 90 million sperm daily
sustentocytes (sertoli cells)
large columner cells act as supporting cells and play role in sperm formation
spermatogenic cells
cells that are surrounded by sustentocytes and give rise to sperm
myoid cells
smooth muscle-like cells surrounding seminiferous tubule that contract to squeeze sperm and testicular fluid though tubules
interstitial endocrine cells
produce androgens and some estrogen
three steps of spermatogenesis
mitosis of spermatogonia (stem cell) forms two spermatocytes
meiosis: spermatocytes form secondary spermatocytes, which form spermatids
spermiogenesis: spermatids become sperm
regions of sperm
head: genetic region that includes nucleus and helmetlike acrosome containing hydrolytic enzymes that enable sperm to penetrate egg
midpiece: metabolic region containing mitochondria that produce ATP to move tail
tail: locomotor region that includes flagellum
role of sustentocytes
large supporting cells (also called sertoli cells) extend from basal lamina to tubule lumen and surround developing spermatogonium
contain light junctions that divide tubule into two compartments
→ basal compartment
→ adluminal compartment
provide nutrients and signals to dividing cells
secrete testicular fluid
produce 2 mediators to regulate spermatogenesis:
androgen-binding protein (ABP)
inhibin
basal comparment
compartment in sustentocytes
basal lamina to tight junctions; spermatogonia and primary spermatocytes located here
adluminal compartment
compartment in sustentocytes
internal to tight junctions; area where meiotically active cells and tubule lumen are located
testicular fluid
rich in androgens and metabolic acid
androgen-binding protein (ABP)
keeps testosterone levels high to spermatogenesis
inhibin
inhibits spermatogenesis by inhibiting FSH release by anterior pituitary
sequence of regulatory events
hypothalamus releases gonadotropin-releasing hormone (GnRH)
GnRH binds to anterior pituitary gonadotropic cells, causing them to release follicle-stimulating hormone (FSH) and luteinizing hormone (LH)
FSH stimulates spermatogenesis indirectly by stimulating sustentocytes to release androgen-binding protein (ABP)
male secondary sex characteristics
features induced in non reproductive organs by male sex hormones (testosterone)
appearance of pubic, axillary, and facial hair
enhanced growth of hair on chest on or other areas
larynx enlargements causing deepening of voice
skim thickens and becomes oily
bones grow, increase in density
skeletal muscles increase in size and mass
boosts basal metabolic rate
basis of sex drive (libido) in males
ovaries: female gonads
produce gametes (ova)
secrete female sex hormones estrogen and progesterone
paired structures flank the uterus, are almond shaped and about twice as large
internal genitalia
located in pelvic cavity, include ovaries and duct system (uterine tubes, uterus, and vagina)
external genitalia
external sex organs
tunica albuginea
surrounds each ovary and it is fibrous
ovarian follicles
tiny saclike structures embedded in cortex
contain immature egg (oocyte) encased by one or more layers of very different cells
female tube system includes:
uterine tubes
uterus
vagina
uterine tubes
receive ovulated oocyte and are usual sit of fertilization
each tube ~10cm (4in) long and extends from area of ovary to surperior refion of uterus
regions of uterine tube
infundibulum
ampulla
isthmus
infundibulum
funnel-shaped opening into the peritoneal cavity
contains ciliated projections called fimbriae that drape over ovary
ampulla
forms half of uterine tube length
is site where fertilization usually occurs
isthmus
narrow medial third that empties into superolateral region of uterus
ectopic pregannay
oocyte is fertilized in peritoneal cavity or distal uterne tube and begins developing there
normally abort naturally with substantial bleeding
the uterus
hollow, thick-walled muscular organ
function is to receive, retain, and nourish fertilized ovum
uterine wall
three layers:
perimetrium
myometrium
endometrium
perimetrium
layer of uterine wall
outermost serous layer (visceral peritoneum)
myometrium
layer of uterine wall
bulky middle layer consisting of interlacing layer of smooth muscle
contracts rhythmically during child birth
endometrium
layer of uterine wall
mucosal lining
simple columnar epithelium on top of a thick lamina propria
fertilized egg burrows into endometrium and resides thee during development
oogenesis
production of female gametes
process of oogenesis
begins in fetal period
oogonia (diploid stem cells) divide by mitosis to produce:
primary oocytes that undergo meiosis I to produce:
secondary oocytes that undergo meiosis II to produce:
ova
ovarian follicle
functional unit of ovary that encloses a single oocyte surrounded by:
pre-granulosa cells if single layer of cells present
granulosa cells if more than one layer present
primordial follicle
single layer of squamous epithelium pre-granulosa cells surrounding primary oocyte
primary follicles
have a single layer of cuboidal pre-granulosa cells surrounding primary oocyte
secondary follicles
have multiple layers of granulosa cells surrounding primary oocyte
vesicular (antral) follicle
have a fluid-filled cavity called an antrum
before ovulation primary oocyte inside vesicular follicle resumes meiosis and becomes secondary oocyte
atresia
apoptosis (programmed cell death) of oocytes and surrounding cells
99.9% of all follicles are never recruited
ovulation
each month after puberty, a select few primary oocytes are activated
→ caused by high hormonal levels, especially FSH
→ one from this group is “selected” each month to become dominant follicle
first polar body
smaller cell that us almost lacking cytoplasm
secondary oocyte
large cell with almost all of mother cell cytoplasm and organelles
ovum
large cell with enough cytoplasm to nourish fertilized egg for 6-7 day journey to uterus
second polar body
small cell lacking cytoplasm degenerates and dies
ovarian cycle
monthly series of events associated with maturation of egg
two consecutive phases, with ovulation occurring midcycle between phases
follicular phase
period of vesicular follicle growth (days 1-14)
luteal phase
period of corpus luteum activity (days 14-28)
corpus luteum
remaining granulosa cells and internal thecal cells enlarge to form this
secretes progesterone and some estrogen
hormonal interaction during ovarian cycle
GnRH stimulates FSH and LH secretion
FSH and LH stimulates follicles to grow, mature, and secrete sex hormones
negative feedback inhibits gonadotropin release
positive feedback stimulates gonadotropin release
LH surge triggers ovulation and formation of the corpus luteum
→ LH tranforms ruptured follicle into corpus luteum
negative feedback inhibits LH and FSH release
uterine (menstrual cycle)
cyclic series of changes in endometrium that occur in response to fluctuating ovarian hormone levels
three phases
days 0-4: menstrual cycle
days 5-14: proliferative (preovulatory) phase
days 15-28: secretory (postovulatory) phase
days 0-4: menstrual phase
ovarian hormones at lowest levels
gonadotropin levels are beginning to rise
stratum functionalis detaches from uterine wall and is shed
by day 5 growing ovarian follicles start to produce more estrogen
days 5-14: proliferative (preovulatory) phase
rising estrogen levels prompt generation of new stratum functionalis layer
estrogen also increases synthesis of progesterone receptors in endometrium
ovulation occurs day 14
days 15-28: secretory (postovulatory) phase
phase that is most consistent in duration
endometrium prepares for embryo to implant
rising proestrogen levels prompt functional alyer to become secretory mucosa and endometrial glands to enlarge and secrete nutrients
conceptus
developing offpsring
pregnancy
state of carrying a developing conceptus
gestation period
time from last menstrual cycle until birth
embryo
conceptus from fertilization through week 8
fetus
conceptus from week 9 through birth
cleavage
occurs while zygote moves toward uterus
rapid mitotic divisions of zygote occurs
first cleavage occurs ~36 hours and produces two daughter cells called blastomeres, which continue to divide
after 72 hours, cluster of cells contains 16 or more cells and is referred to as morula
blastocyst formation
around day 4 or 5, embryo, which consists of ~ 100 cells is now reffered to as a blastocyst, reached uterus
composed of:
→ trophoblast cells
→ embryoblast
trophoblast cell
display immunosuppresive factors
participate in placenta formation
embryoblast
cluster of 20-30 rounded cells
becomes embryonic discs, which will form embryo and three or four extraembryonic membranes
fourth extraembryonic membrane (chorin) is formed by trophoblast
implantation
begin 6-7 days after ovulation
trophoblast cells adhere to site with proper receptors and chemical signals
inflammatory-like response occurs in endometrium
cytotrophoblast
inner layer od cells
syncytiophoblast
cells in outer layer lose plasma membranes, becoming multinclear mass