Hygiene test two
1/213
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
214 Terms
What is Diabetes Mellitus?
A group of disorders characterized by hyperglycemia due to defective insulin secretion, action, or both.
What percentage of the U.S. population is affected by diabetes?
Over 37 million adults and children, which is 11.3% of the population.
What is prediabetes?
A condition that precedes type 2 diabetes, affecting ~38% of U.S. adults, also known as impaired glucose tolerance (IGT) or impaired fasting glucose (IFG).
What are the major clinical types of diabetes?
Type 1 diabetes, Type 2 diabetes, Gestational diabetes, and other specific types.
What characterizes Type 1 diabetes mellitus?
Total lack of insulin due to destruction of beta cells in the pancreas, usually presenting during childhood or adolescence.
What is the prevalence of Type 2 diabetes mellitus?
It accounts for 90 to 95% of the diabetic population and is often preventable.
What are common risk factors for Type 2 diabetes?
Obesity, age, sedentary lifestyle, history of gestational diabetes, hypertension, and dyslipidemia.
What is gestational diabetes mellitus?
Diabetes that occurs during pregnancy, affecting about 7% of the population.
What is hyperglycemia?
A rise in blood glucose concentration where glucose cannot be used or stored, leading to glucosuria.

What are the cardinal signs of diabetes?
Polydipsia (excessive thirst), Polyuria (excessive urination), Polyphagia (excessive food intake), unexplained weight loss, weakness, and blurred vision.

What complications can arise from diabetes?
Retinopathy, kidney disease, periodontal disease, cardiovascular diseases, neuropathy, and increased risk of amputations.
What is the importance of daily blood glucose testing?
It provides a snapshot of glucose levels to help manage diabetes effectively.
What is the target A1c level for diabetes management?
Less than 7%.
What types of insulin are used in diabetes management?
Rapid-acting, short-acting, intermediate-acting, and long-acting insulin.
What is the onset time for rapid-acting insulin?
5 minutes.
What is the duration of long-acting insulin?
24 hours.
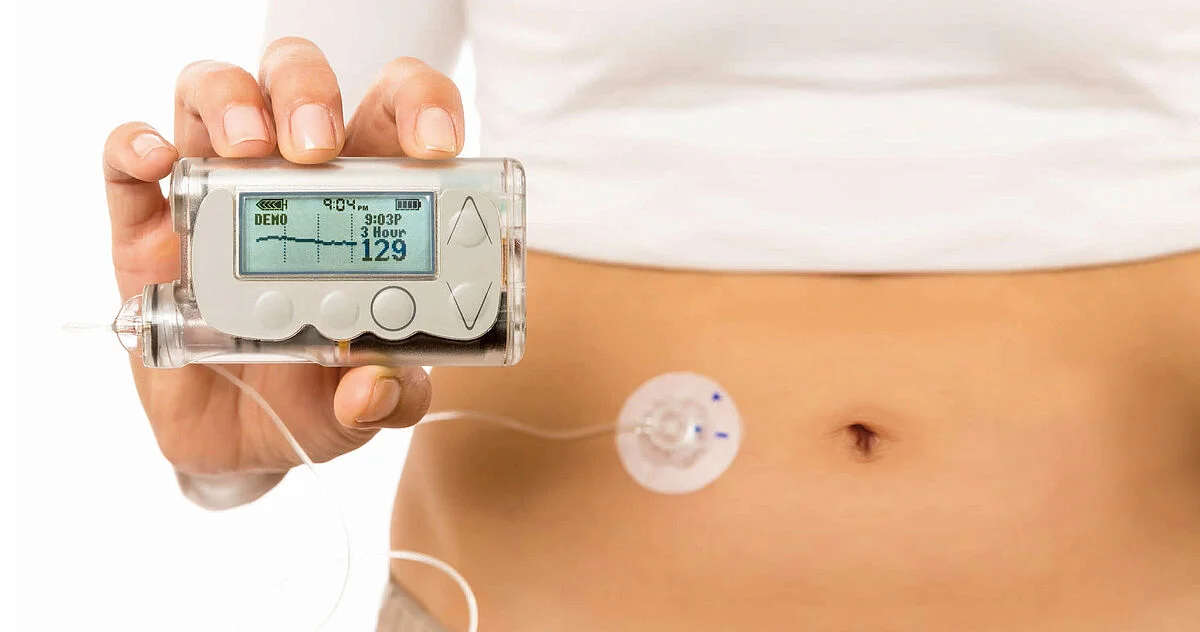
What is an insulin pump?
A device that delivers insulin through a sensor inserted subcutaneously, using wireless technology.
What is diabetic ketoacidosis?
A serious condition that can occur when blood glucose levels rise above 400 mg/dL, leading to metabolic complications.
What is the relationship between diabetes and periodontal disease?
Diabetes increases the risk of periodontal disease, and periodontal therapy can help reduce A1c levels.
What is the impact of defective carbohydrate metabolism in diabetes?
It leads to energy starvation, causing the body to use fats and proteins for energy, resulting in the production of keto acids.
What is the risk of developing Type 2 diabetes for women with a history of gestational diabetes?
They have a 50% chance of developing Type 2 diabetes later in life.
What is the role of the pancreas in diabetes?
The pancreas produces insulin, which regulates blood glucose levels.
What are the symptoms of diabetic ketoacidosis?
Symptoms include excessive thirst, frequent urination, nausea, abdominal pain, and confusion.
What is the significance of glucosuria in diabetes?
Glucosuria occurs when blood glucose levels exceed 150 mg/dL, leading to increased urine volume and dehydration.
What is the preferred initial oral hypoglycemic agent?
Metformin (Glucophage)
What are the primary actions of Metformin?
Decreases glucose production by the liver, decreases intestinal glucose absorption, and increases insulin action.
What is a significant side effect of Sulfonylureas?
Hypoglycemia and weight gain.
What is the normal blood glucose range for patients?
80 to 130 mg/dL.
What A1c level is considered well-controlled for diabetes?
A1c <7%.
What is the most common precipitating factor for severe ketoacidosis?
Infection.
How does stress affect blood glucose levels in diabetics?
It contributes to hyperglycemia by causing the release of epinephrine, which releases glycogen from the liver.
What should be done if a diabetic patient has a blood glucose level <70 mg/dL?
Provide carbohydrates and recheck blood glucose.
What are some oral complications associated with diabetes?
Xerostomia, increased caries, rapidly progressive pocketing, gingival bleeding, and opportunistic infections.
What A1c level is associated with greater periodontal inflammation?
A1c >8%.
What is the recommended timing for dental appointments for diabetics?
Appointments should be brief and preferably scheduled 2 hours after breakfast.
What is the 15/15 rule for treating hypoglycemia?
Administer 15g of simple carbohydrates, then recheck blood glucose in 15 minutes.
What are the symptoms of hypoglycemia?
Shakiness, anxiety, palpitations, increased sweating, hunger, pale skin, confusion, and dizziness.
What should be done if a diabetic patient is unconscious and unable to consume oral carbohydrates?
Call EMS and administer an IM injection of glucagon.
What is diabetic microangiopathy?
A condition that causes blindness and kidney disease in diabetics.
What is the risk of infection in relation to blood glucose levels?
The risk of infection increases when blood glucose is between 200 to 230 mg/dL.
What is the primary cause of Hyperglycemic Ketoacidotic Coma?
Absolute lack of insulin.
What are common symptoms of Diabetic Ketoacidosis (DKA)?
Thirst, polyuria, fatigue, weight loss, tachycardia, hypotension, ketotic breath, and impaired consciousness.

What percentage of the diabetic population is affected by Type 2 diabetes?
90 to 95%.
What are some risk factors for developing Type 2 diabetes?
Obesity, age, inactivity, history of gestational diabetes, and dyslipidemia.
What should be documented in the dental care of diabetic patients?
All data collected, treatment planned and provided, and recommendations relevant to patient care.
What is the impact of nonsurgical periodontal therapy on diabetic control?
It has been shown to improve diabetic control in type 2 diabetics.
What should be done if a diabetic patient has a blood glucose level >200 mg/dL?
Refer the patient for further evaluation.
What are the most common respiratory diseases?
Asthma and COPD
What is asthma?
A chronic inflammatory respiratory disease characterized by increased responsiveness of the bronchial airways.
How is asthma classified?
Intermittent and Persistent (mild, moderate, or severe).
What are specific antigens that can trigger asthma?
Pollen, molds, foods, flavorings, and dust mites.
What are some chemical irritants that can exacerbate asthma?
Smoke, tobacco, and scents.
What are non-allergenic triggers for asthma?
Respiratory infections, pollutants, exercise, cold air, and emotional stress.
What are the clinical manifestations of asthma?
Wheezing, dyspnea, coughing, chest tightness, and increased difficulty in breathing.
What is status asthmaticus?
A severe asthma attack that does not respond to adequate doses of bronchodilators and can be deadly.
What should be assessed in patients with asthma?
Frequency, conditions, time of onset, and type of asthmatic attacks.
What management strategies should be employed for asthma?
Type of medication and identification of precipitating factors.
What is a recommendation for patients using inhalers?
Rinse mouth with water after inhaler use to prevent medication-induced xerostomia.
What is the recommended daily intake of xylitol for asthmatic patients?
6 to 10 grams per day.
What precautions should be taken during dental hygiene care for asthmatic patients?
Use HVE and pre-rinse to reduce contaminated aerosols; evaluate for malocclusion.
What is a common dental concern for children with asthma?
Increased risk of caries and gingivitis due to medication-induced xerostomia.
What should be avoided when using local anesthesia in asthmatic patients?
Epinephrine, unless it is preservative-free due to sensitivity to sulfites.
What type of analgesia is indicated for asthmatic patients?
Nitrous oxide analgesia.
What medications are commonly used to manage asthma?
Anti-inflammatories, bronchodilators, and corticosteroids.
What is a significant risk for asthmatic patients during dental appointments?
Decreased lung function, especially when laying supine or experiencing anxiety.
What is a common dental trait among asthmatic children?
Many are mouth breathers, which can correlate with dental malocclusions.
What is the importance of creating a stress-free environment for asthmatic patients?
To minimize anxiety and potential asthma exacerbations during dental care.
What is COPD?
Chronic Obstructive Pulmonary Disease, a preventable disease characterized by persistent respiratory symptoms and airflow limitation.
What are the primary causes of COPD?
Chronic bronchitis and emphysema, often related to tobacco smoking and pollution.
What is emphysema?
A condition involving overinflation of the lungs and irreversible destruction of alveoli, leading to respiratory dysfunction.
What is chronic bronchitis?
Inflammation of the bronchial tubes, characterized by a cough producing large amounts of sputum for at least 3 months over 2 consecutive years.
What are the signs and symptoms of chronic bronchitis?
Cough with sputum, dyspnea, prolonged expiration, wheezing, and increased severity of respiratory infections.
What is the significance of alpha-1 antitrypsin in COPD?
It protects the lungs from elastase, an enzyme that can destroy elastic tissue; low levels can lead to emphysema.
What are the implications of COPD for dental hygiene care?
Short appointments, tobacco cessation, and avoiding aerosol-producing devices are recommended.
What is tuberculosis (TB)?
An airborne communicable disease primarily affecting the lungs, caused by Mycobacterium tuberculosis.
What are the common symptoms of active TB?
Chronic cough, fever, night sweats, weight loss, and malaise.
What is the treatment for active TB?
Hospitalization with multiple drugs for at least 18 months.
What is pneumonia?
Inflammation of the gas-exchanging units of the lungs, caused by bacteria, viruses, or aspiration of chemicals.
What are the risk factors for community-acquired pneumonia (CAP)?
COPD, alcohol abuse, cystic fibrosis, and seasonal factors.
What is obstructive sleep apnea (OSA)?
A disorder involving the partial or complete collapse of the upper airway during sleep, leading to breathing cessation.
What are the oral manifestations of OSA?
Retrognathic profile, bruxism, enlarged tongue, and edematous gingival tissue.
What is cystic fibrosis?
An autosomal recessive genetic disorder affecting salt and water movement in epithelial cells, leading to thickened secretions.
What are the implications of cystic fibrosis for dental hygiene care?
Medical consultation, short appointments, and avoiding aerosol-producing devices.
What are the two major diseases contributing to COPD?
Emphysema and chronic bronchitis.
What is the role of antibiotics in COPD management?
They can improve airflow, relieve symptoms, and enhance quality of life but do not cure COPD.
What is the significance of spirometry in COPD?
It is used to classify COPD into four levels from mild to very severe based on pulmonary function.
What is the common treatment for obstructive sleep apnea?
Continuous positive airway pressure (CPAP) therapy.
What are the signs of advanced emphysema?
Severe dyspnea, cyanosis, respiratory failure, and a barrel-chest appearance.
What is the relationship between smoking and COPD?
Tobacco smoking is a direct cause of COPD, with a strong correlation to disease severity.
What is the typical cough associated with chronic bronchitis called?
Smoker's cough.
What is the primary cause of aspiration pneumonia?
Aspirating oral microorganisms from food, drink, vomit, or saliva.
What are the common bacteria causing community-acquired pneumonia?
Streptococcus pneumoniae is the most common.
What are the symptoms of mild active TB?
Low-grade fever, listlessness, loss of appetite, malaise, and occasional cough.
What is the main goal of COPD management?
To assess and monitor disease, reduce risk factors, and manage stable COPD and exacerbations.
What is the significance of a sweat test in cystic fibrosis?
It helps diagnose the disease by measuring salt levels in sweat.
What are the common treatments for cystic fibrosis?
Antibiotics, bronchodilators, anti-inflammatories, and percussion therapy.

What is the leading cause of death worldwide?
Cardiovascular Disease (CVD)
What is the path of blood flow starting from the vena cava?
Vena cava → right atrium → tricuspid valve → right ventricle → pulmonary valve → pulmonary artery → lungs → pulmonary vein → left atrium → mitral valve → left ventricle → aortic valve → aorta
What are the nonmodifiable risk factors for CVD?
Genetics, age, race, gender, history of anorexia or bulimia
At what age does the risk of CVD increase for both genders?
Over 35 years