Animal Phys Lab Practical 1
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
The first machine invented to measure physiological events
Kymograph
Inventor of the Kymograph
Carl Ludwig
Electronic machines used to produce a permanent record of a physiological event
Recording oscillographs
The functioning unit of the recording oscillograph.
Recording channel
3 components of a Recording Channel
A sensing device
A processor
A recorder/reproducer
Picks up information from the experimental set up. Components are the Electrode and Transducer
The Sensing Device
A device used to detect electrical events (e.g. EKG, EEG, “pin,” “sleeve”)
Electrode
Transforms a non-electrical signal into an electrical signal that the computer can understand.
Transducer
Takes the electrical signal from the Transducer. Components are the Coupler and the Amplifier
Processor
Alters the electrical signal so it can be recognized by the rest of the recording channel
Coupler
This amplifies (boosts) the signal received proportionally so it can be measured
Amplifier
Device for making a permanent recording of a physiological event (the computer, printer etc.)
Reproducer/Recorder
Matches the signal from the sensing device with the processor (like setting a scale to 0)
Balancing
Standardizes the recording channel; lets us quantify our results (like setting the increments on the scale)
Calibrating
Devices for administering a controlled electrical signal to an excitable tissue to elicit a response.
Stimulators
The lowest stimulus that will elicit a physiological response
Threshold stimulus
Stimulator Variables
Intensity
Frequency
Duration
The strength of a stimulus measured in volts.
Intensity
The number of impulses administered per second measured in Hertz
Frequency
The length of time each impulse lasts (Milliseconds) (NOT the total length of time impulses are administered to a subject.)
Duration
A motor neuron and all the muscle fibers it innervates- the functional unit of muscle contraction
Motor Unit
Three parts of the Motor Unit
Neuron
Neuromuscular Junction (NMJ)
Muscle Fibers
The basic unit of skeletal muscle
Muscle Cell
Plasma membrane surrounding a muscle fiber
Sarcolemma
__ extend the entire length of a fiber but are arranged in compartments called sarcomeres.
Myofilaments
Parts of a Sarcomere
Actin
Tropomyosin and Troponin
Myosin
Primary component of the thin myofilament.
Actin
Prevents actin and myosin from binding together
Tropomyosin and Troponin
Primary component of the thick myofilament.
Myosin
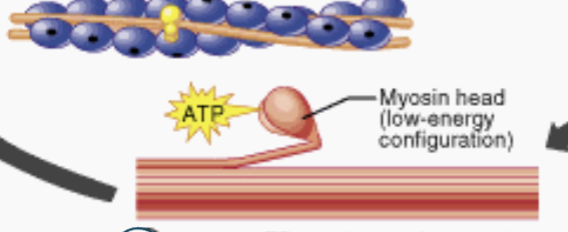
First Step of the Sliding Filament Theory
New ATP attaches to the myosin head; the cross bridge detaches
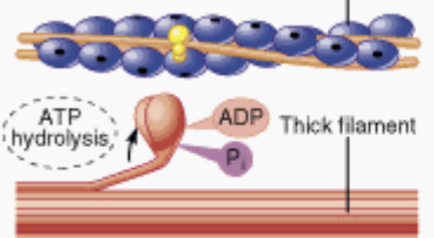
Second Step of the Sliding Filament Theory
ATP is split into ADP and Pi; cocking of the myosin head occurs
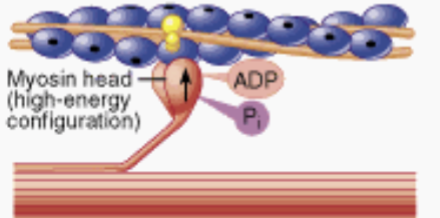
Third Step of the Sliding Filament Theory
Myosin cross bridge attaches to the actin myofilament
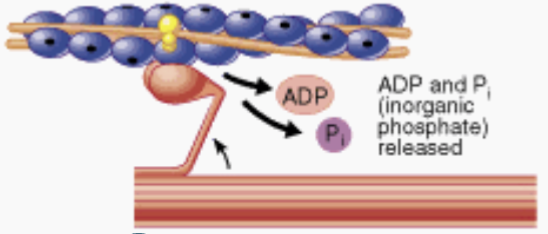
Fourth Step of the Sliding Filament Theory
“Power stroke” (working stroke) happens- the myosin head pivots and bends as it pulls on the actin filament, sliding it towards the M line. ADP and Pi are released
Neuron
In order for the muscle fiber to contract, a stimulus must be delivered from a neuron.
Neuromuscular Junction (NJM)
When the action potential reaches the end of the neuron, voltage-gated Ca2+ channels open and calcium rushes into the neuron
Influx of ___ causes vesicles filled with Actetylcholine to fuse with the neural membrane.
Ca2+
___ is released into the neuromuscular junction where it binds to chemically gated Na+ Channels on the sarcolemma of the muscle fiber. This causes an action potential on the sarcolemma
Acetylcholine (Ach)
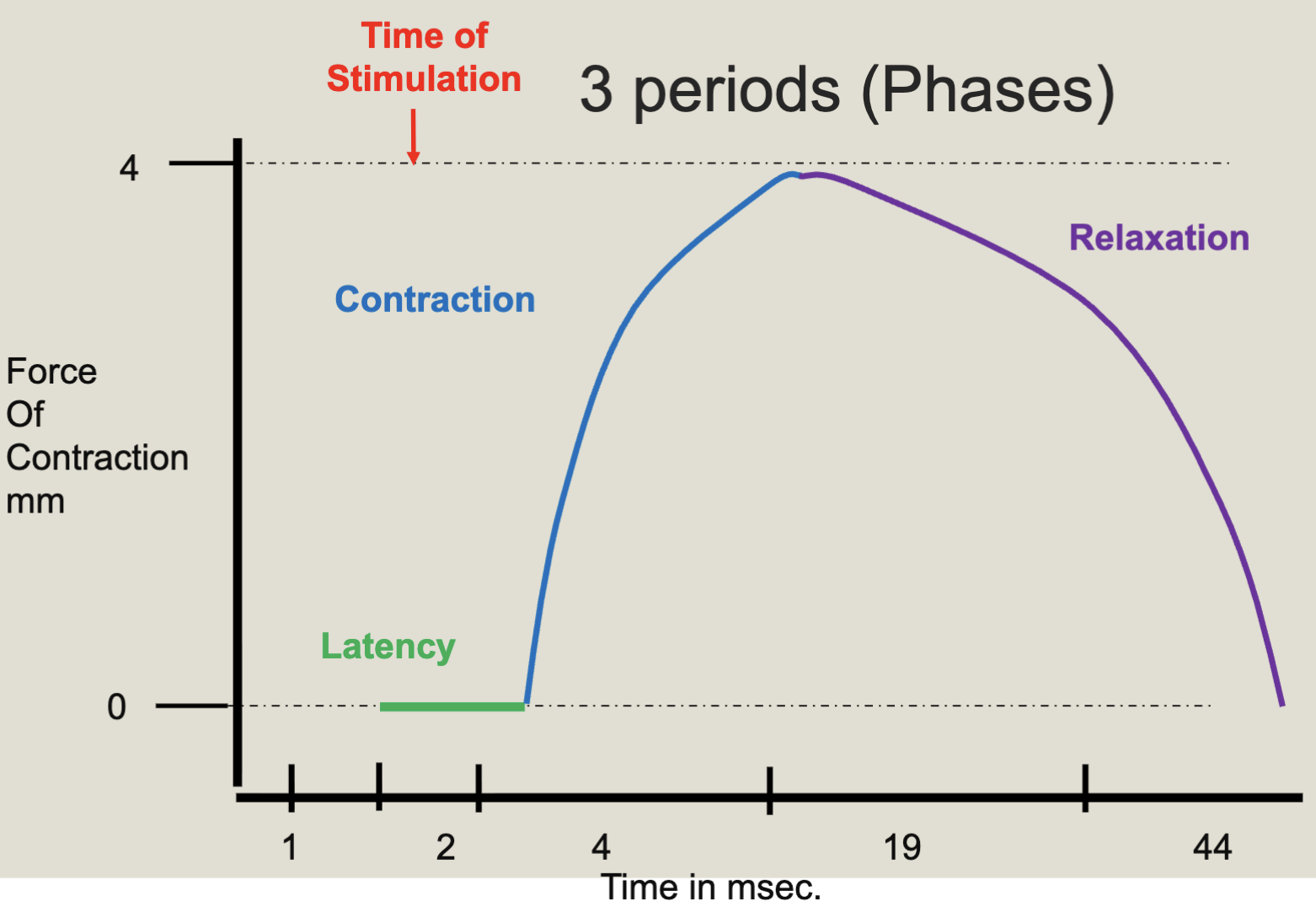
3 Periods of a Normal Form Curve (Muscle cell Twitch)
Latency
Contraction
Relaxation
Three Enzymes in Muscle Contraction
Acetylcholinesterase (AchE)
Myosin ATPase
Sarcoendoplasmic Reticulum Calcium ATPase (SERCA) pump / Calcium Pump
This enzyme breaks down Acetylcholine in the NMJ
Acetylcholinesterase (AChE)
What effect will decreased AChE function have on muscle contraction?
Increase in ACh contact with Nicotinic receptors; increase in stimulation of Ca2+ release; increase in the length of contraction
An ATPase that converts chemical energy into directed movement and can be viewed as a molecular motor; cleaves ATP at the myosin heads.
Myosin ATPase
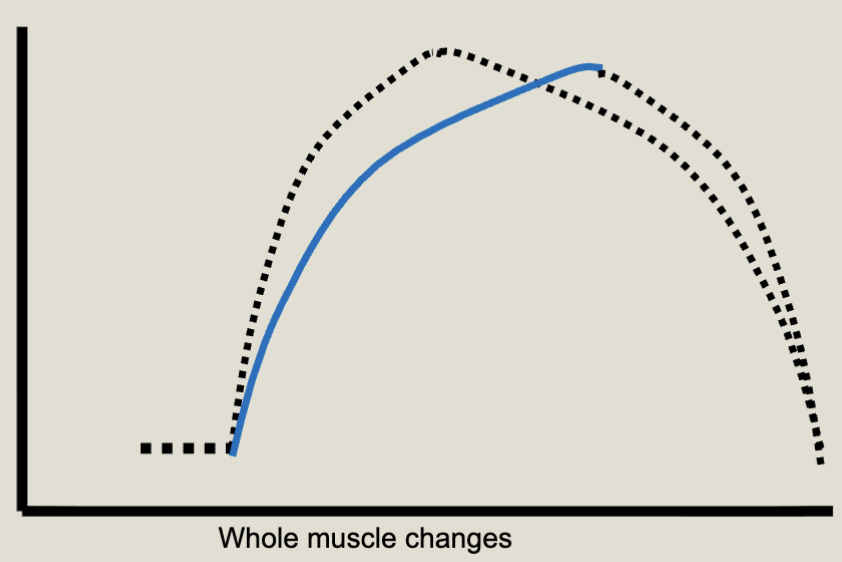
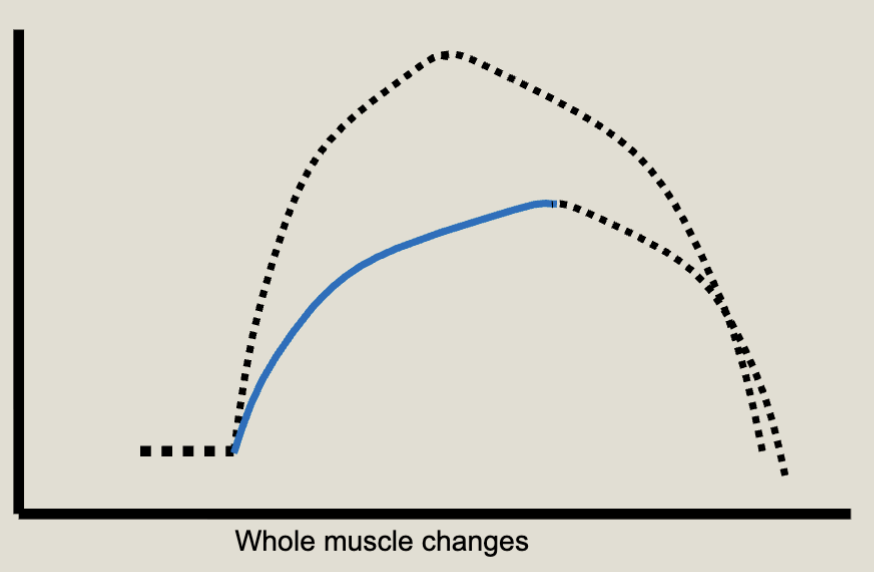
What effects will we see from decreased function of Myosin ATPase?
Decrease in ratcheting; decrease in force; increase in contraction time
Acts to transport calcium ions from the cytosol back to the sarcoplasmic reticulum following muscle contraction; cleaves the ATP that runs the calcium pump on the SR.
SERCA/ Calcium Pump
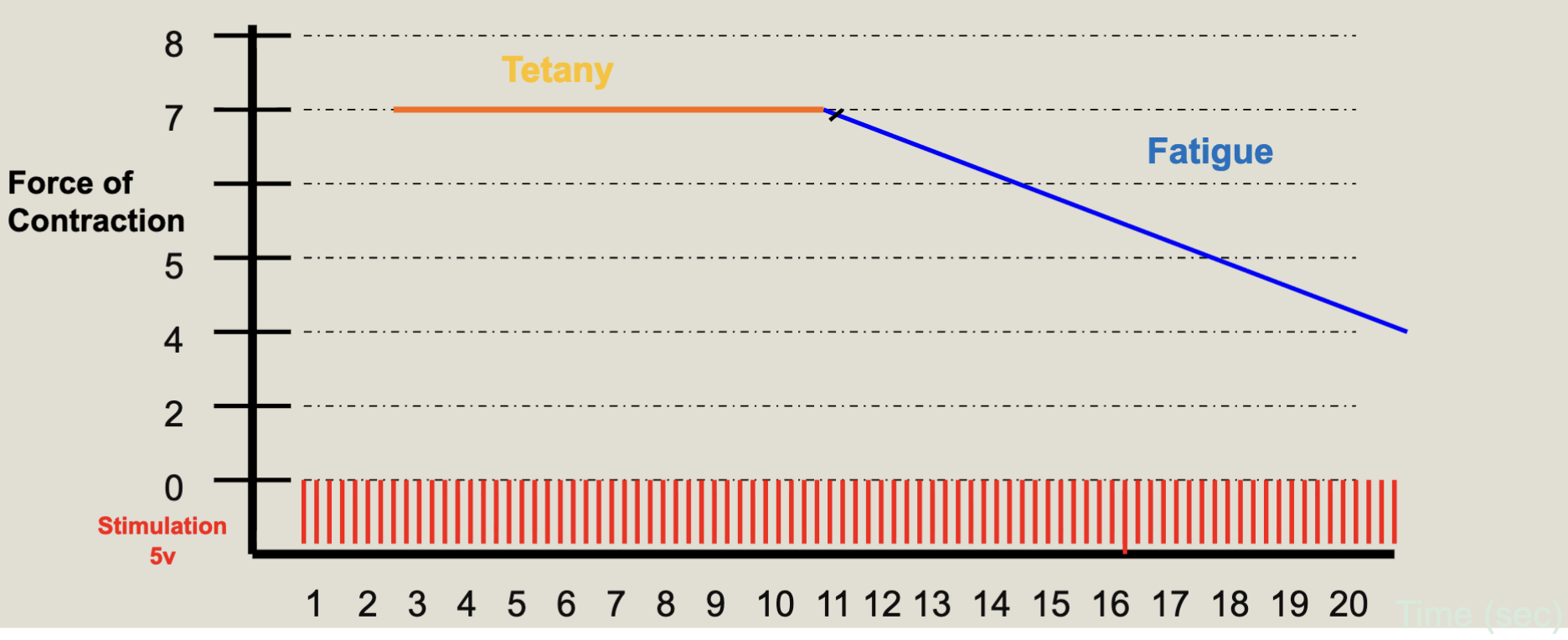
The affects of Fatigue are:
Depleted ATP
Decrease in ratcheting
Decrease in contractile force
What effect will we see from decreased function of SERCA/ Calcium Pump?
Increased time of Ca2+ in the sarcoplasm; increase in ratcheting; increase in contraction; increase in relaxation time prolonging Ca2+ residence in the sarcomere; decrease in sequester rate of Ca2+, also prolonging Ca2+ residence in the sarcomere
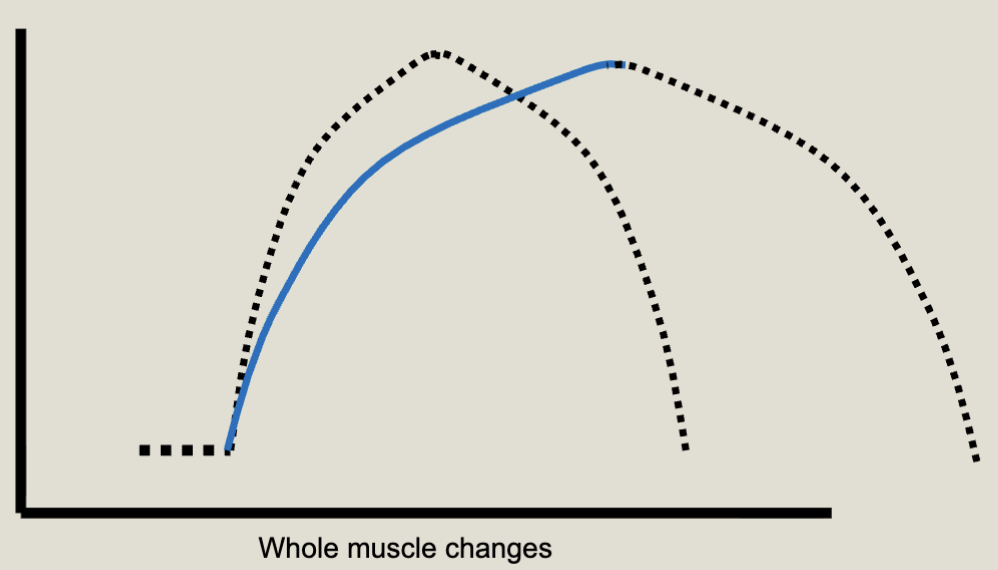
The effect of Smooth Muscle not having T-tubules:
The wave of depolarization is slow, with long-lasting contractions and slow relaxation
___ allows Na+ to diffuse at a slow but continuous rate, causing a slow wave of depolarization
“Leaky” Na+ channels
The smooth muscle cell membrane is more __ to ions _ and _ , allowing them to leak across the membrane and into the muscle cells.
permeable; Na+, Ca2+
Allows smooth muscle to contract, even without generating a typical action potential
Slow Wave Depolarization
When action potentials for contraction originate within the muscle, the muscle is called __
Myogenic
Smooth Muscle is modified by__
neural input
Smooth Muscle is double innervated by both the ___ and the ___
Sympathetic NS; Parasympathetic NS
In the Isolated System of the Autonomic control of smooth muscle, an isolated system includes the complete __
Short Postganglionic fiber of the Parasympathetic pathway
Parasympathetic innervation occurs via the __
Vagus Nerve
Sympathetic innervation occurs via the __
Coeliac Ganglion
Type of receptors in the Parasympathetic Pathway:
Cholinergic receptors (Nicotinic and Muscarinic)
Type of receptors in the Sympathetic Pathway:
Adrenergic Receptors (Alpha and Beta)
Neurotransmitter of the Parasympathetic Pathway that modifies the Smooth Muscle
Acetylcholine (Ach)
Neurotransmitters of the Sympathetic Pathway that modifies the Smooth Muscle
Catecholamines of Norepinephrine (NE) and Epinephrine (Epi)
Epinephrine is a __ neurotransmitter
adrenergic
Epinephrine works in the Sympathetic pathway and only bind to the __ and __ on the gut.
Alpha 2; Beta 2
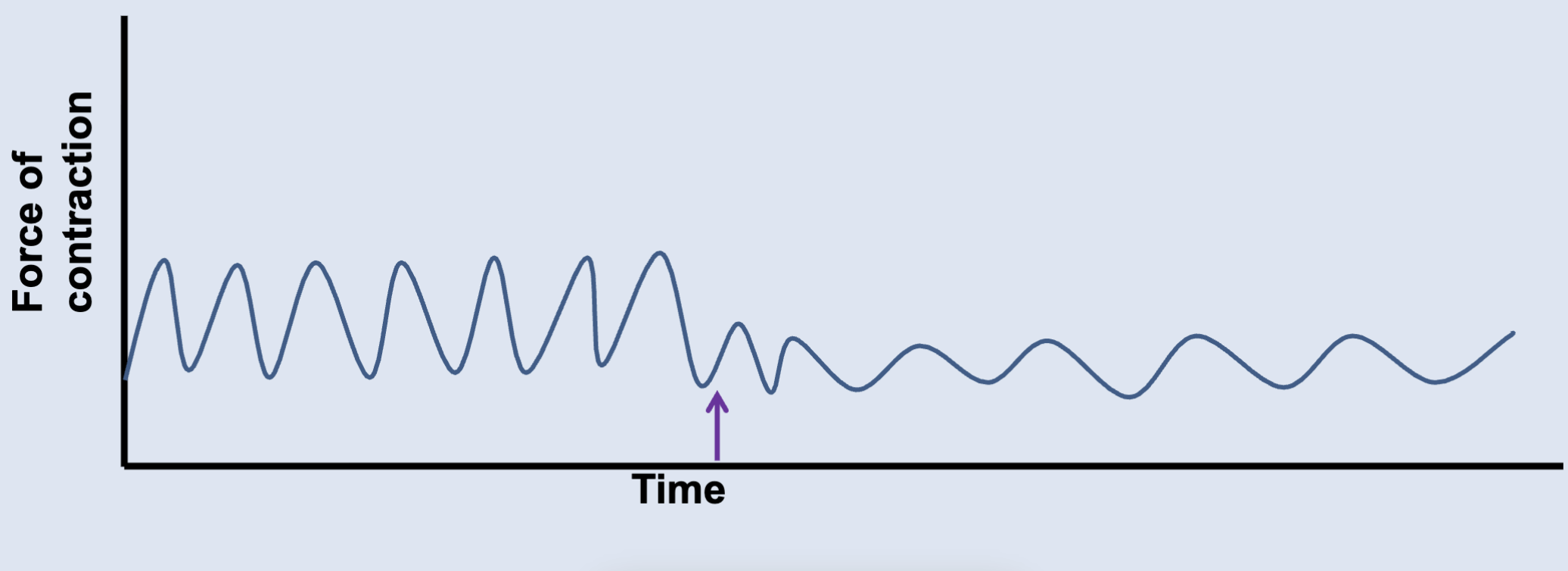
___ opens K+ channels and hyperpolarizes the membrane; inhibits smooth muscle contraction.
Epinephrine
__ binds to __ receptors on the postganglionic parasympathetic nerve and muscarinic receptors on the sarcolemma.
Acetylcholine; N2
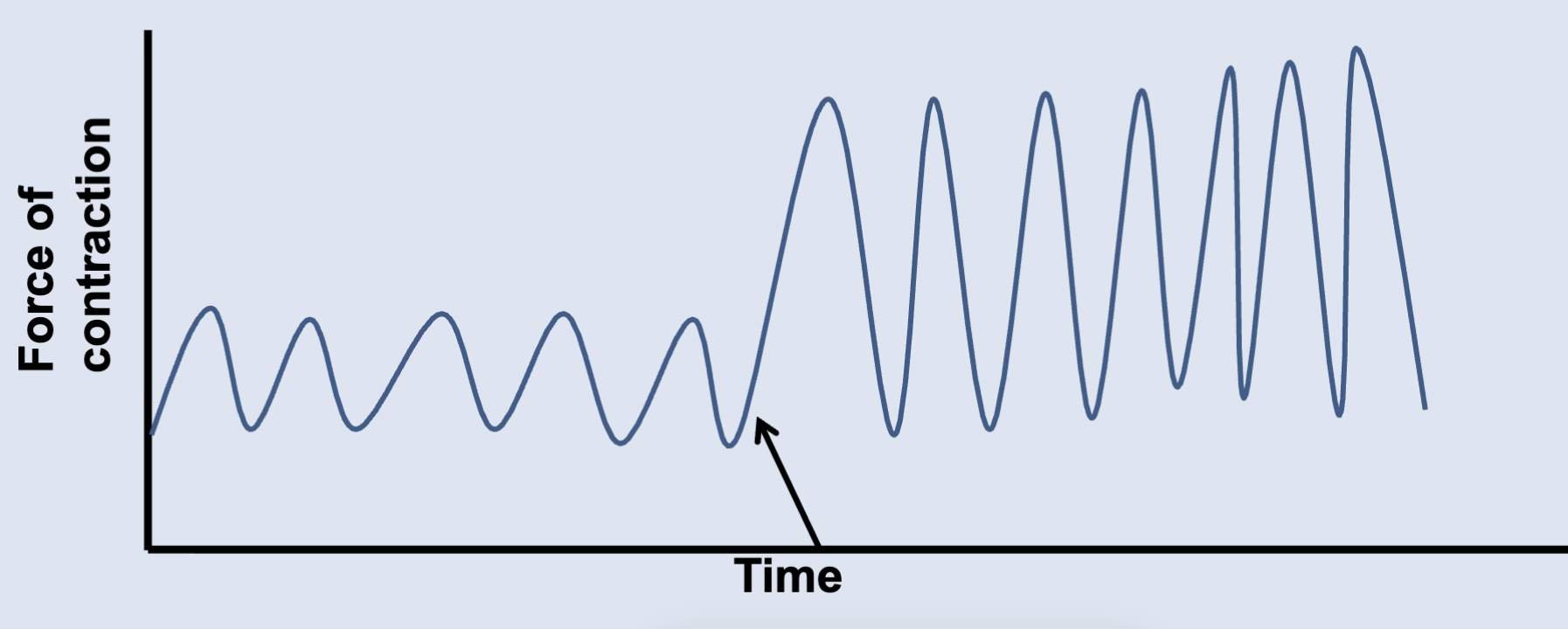
__ opens Na+ channels, depolarizes the membrane and causes an increase in contraction strength, frequency OR a smooth tonic contraction
Acetylcholine (Ach)
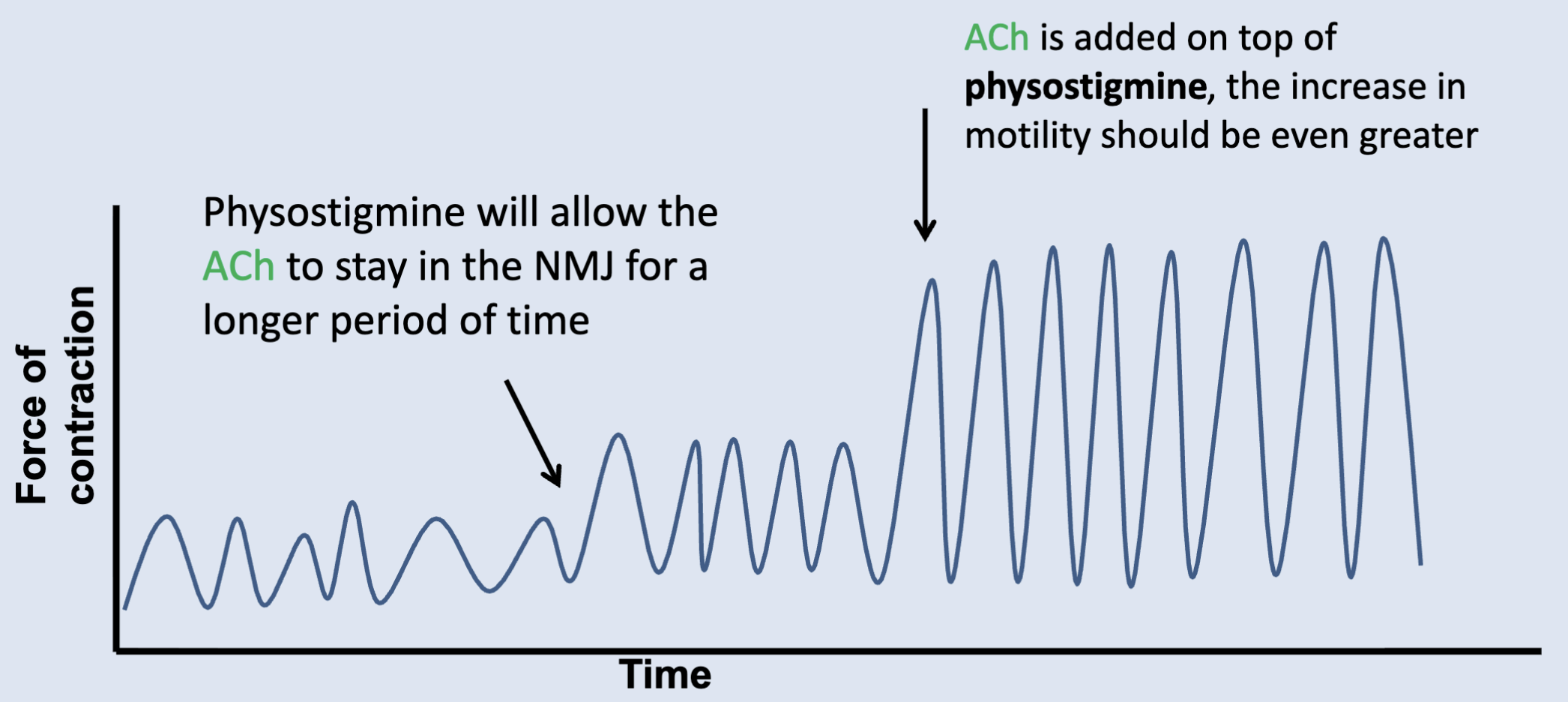
An anticholinesterase (potentiator of ACh) that prevents the breakdown of ACh by ACh-esterase (cholinesteras)
Physostigmine
Cause of Physostigmine on smooth muscle contraction
Contractions should increase in strength, frequency, or both because the myenteric plexus is spontaneously active.
Atropine is a __ blocker, meaning __ can no longer bind and motility decreases
muscarinic; Acetylcholine
Which component of the motor unit does lidocaine directly affect?
The lipid bilayer- makes it rigid/ less flexible and less able to generate action potential
Which component of the motor unit does d-tc directly affect?
Nicotinic (N2) receptor- blocks receptor and prevents Ach from binding and the transmission of the action potential.
The opening of what ion channels cause action potentials?
Sodium (Na+) channels
What causes a contraction when the nerve is pinched?
Mechanical disruption to the membrane allows Na+ to enter the cell, causing depolarization of the membrane and generation of an Action Potential
Where do you add lidocaine?
Sciatic Nerve
Name the nerve and muscle we are using in today’s lab.
Gastrocnemius muscle and Sciatic nerve
If temperature is decreased, what happens to the relaxation phase of a normal form curve?
Decreased temperatures slows down enzyme function, resulting in longer relaxation phase; the process of relaxation and contraction are negatively affected
Motor-unit summation is achieved by increasing the ___ of the stimulus.
Strength (intensity)
T or F: During the absolute refractory period of the nerve, a second stimulus produces a greater response than the first stimulus.
False
Smooth muscles sarcomere are arranged__
Non-linearly
What does smooth muscle not have that other types do?
T-tubules
What is the result of no T-tubules in smooth muscle?
Slow wave depolarization that produces long-lasting contractions with slow relaxation
The cell membrane smooth muscle cells are more permeable to __
Na+ and Ca2+ ions
What allows Na+ to diffuse at a slow, continuous rate, causing a slow wave of depolarization?
Leaky Na+ channels
What does it mean for the sooth muscle to be myogenic?
Action Potentials originate within the muscle and nervous system innervation is not necessary for contraction
What does it mean for something to be double innervated?
It is controlled by both the Sympathetic and Parasympathetic NS
What type of receptors are located in the Parasympathetic NS?
Cholinergic (Nicotinic, Muscarinic receptors)