lecture 19: aging and geriatric psychiatry
1/46
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
47 Terms
dressing, bathing, toileting, transfer, continence, eating
name the activities of daily living
early onset neurocognitive disorders
loss of IIADL usually precedes
instrumental activities of daily living (IADLs)
the activities of daily living needed for independent living
§Widely used and therefore can track cognition over time and between clinicians
§5-10 minutes
pros oof MMSE
§False positives: those with little education
§False negatives: those with high premorbid intellectual functioning
§Psychologically stressful--makes people angry!
cons of MMSE
clock drawing test
quick screening test of executiive function/visual-spatial
-does NOT test memory, less stressful, less culture based
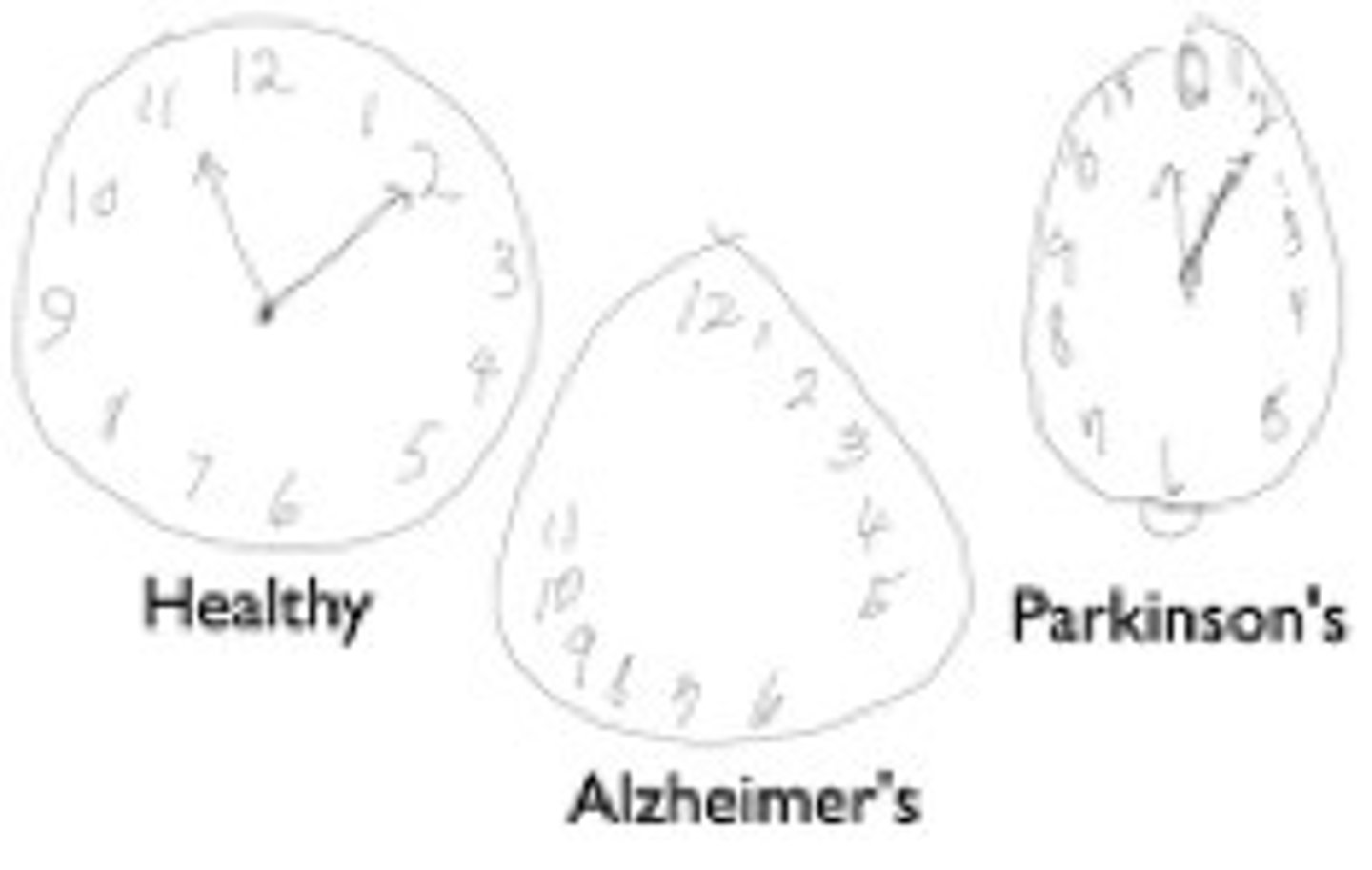
§"Draw a large circle on the (blank) page"
§"Draw in the numbers inside the circle as if a clock face 1-12
§"Draw in the hands to show 10 past 11"
instructions to conducting clock drawing test
-1 point for up to 8 correctly placed numbers
-1 point for each correctly placed hands of clock
TOTAL 10
scoring the clock drawing test
the MOCA (montreal cognitive assessment)
Screens for mild cognitive decline. 30-point questionnaire. > or = 26 considered normal
SLUMS test
screening test for cognitive impairment

mini cognitive assessment instrument
-Ask patient to repeat 3 words
-Then ask to draw a clock
-Repeat 3 words
-Clock abnormal: impaired
-Recall 1-2: Normal
-Recall 0: Impaired
-begin medical work up to assess for reversible causes of the decline
-assess the tiimeframe
-ask for collateral (baseline)
next step in work up if screen positive for cognitive impairment
§1. on-going dialogue with preparation for safety measures
§2. involve the family/caregivers
§3. include the patient (if possible) in the decision to drive with increasing restrictions
§4. know the state laws on mandatory reporting requirements (SC status is voluntary requirements for physicians to report to DMV)
§5. assess all domains of cognition
§6. may refer to OT assessment for driving assessment for safety assurance and
how do you assess driving saftey in geriatrics
-physical, financial exploitation, neglect/self-neglect, emotionall
name some of the symptoms of elder abuse
person age 18 or older who has a physical or mental condition which substantially impairs the person from adequately providing for his or her own care or protection.
how does the law define a vulnerable adult
A. A disturbance in attention (reduced ability to direct, focus, sustain, and shift attention) and awareness (reduced orientation to the environment)
B. The disturbance develops over a short time (usually hours to days), represents a change from baseline, and tends to fluctuate in severity in the course of a day.
C. May also involve additional disturbances in cognition with disorientation, memory issues, and or perceptual disturbances such as hallucinations (visual).
diagnostic criteria of delirium aka encephalopathy
§THE DIAGNOSIS OF DELIRIUM IS CLINICAL AND NO LABORATORY ABNORMALITY CAN DIAGNOSE DELIRIUM
how do you diagnose delirium
-decreased Ach
-increased cortisol and beta endorphins
-increased serotonin
-decreased GABA
-increased dopamine---> decreased release of Ach
hormonal and NT factors contributing to delirium
decreased GABA
pathophys of benzos and alchol withdrawal causing delirium
hypoactive delirium
what kind of delirium is associated with hepatic encephalopathy?
Self-extubation may cause a _____ pressure alarm.
in hyperactive delirium, pt is at risk of
aspiration, PE, decubitus ulcers
in hypoactive delirium, pt is at risk of
confusion assessment method
1) acute onset and fluctuating course
2) inattention
3) disorganized thinking
4) altered level of consciousness
+ test requires presence of 1 AND2 plus either 3 or 4
delirium
a medical syndrome with psychiatric symptoms
treatment should be done in the medical wards and may even require the ICU depending on the etiology/frailty/life-threatening state.
I WATCH DEATH
infection, withdrawal, acute causes, toxins, CNS pathology, hypoxia, deficiencies, endocrine, vascular shohck, heavy metals
mnemonic of the causes of delirium
major neurocognitive disorder
dementia is aka
depression
ex: Elderly patients who are chronically depressed may stop taking in fluids and adequate nutrition which can lead to infections/compromise and ultimately delirium possibly.
___________ may be a precursor to the development of dementia or may present with dementia symptoms in the elderly.
anxiety due to general medical condition
why is geriatric anxiety often so prevalent?
benzodiazepines, sedative hypnotics
-instead offer cognitive behhavior therapy
do NOT use these meds to treat insomnia in the elderly
buspirone
-med useful for GAD among elderly patients
-it is not psychoactive, mood altering or eurphorigenic
DM,COPD, HYPOTENSION/BRADYCARDIA
beta blockers may be used to treat anxiety in elderly unless they have
-less time in deep/slow wave sleep
-REM density increased
-more frequent awakenings
-higher incidence of sleep related breathing disorder
changes in sleep associated with aging
melatonin
1st line med for sleep in geriatrics
women in their 70s
most common age of onset of psycotic symptoms in elderly
§Persecutory-"Sheriff is killing me"
§Somatic-"there are bugs in my skin"
§Grandiose-"I have 400 million dollars"
most common types of delusions seen in elderly
dementia/neurocognitive disorder
most common cause of psychotic symptoms in elderly
the geriatric depression scale
most commonly used and validated screening tool for diagnosis of deprpession in geriatric patients
-depression in the elderly is often unrecognized
-reduces elderly person's ability to rehabilitate
-increases risk of suicide
how is depression different in the elderly compared to other age groups
memory problems, confusion, social withdrawal, loss of appetite
symptoms of depression in the older adult
-yes
-however, high risk of drug interaction
§In general, a minimum of a 8 weeks trial of an antidepressant at a therapeutic dose should be attempted. If effective, this acute dose should be continued for several months or more, then consideration for reduction to a maintenance dose can be determined based on clinical grounds.
should you use antidepressants in the elderly?
SSRI
first line drugs for treating depression in the elderly
drug interactions, their use has some risk for Hyponatremia, Gastrointestinal Bleeding, Syndrome of Inappropriate Antidiuretic Hormone (SIADH), Bradycardia, and falls
risk of SSRI use in the elderly
§ECT is well tolerated in the elderly with risks being a function of medical/surgical comorbidity
§ECT is a effective and rapid treatment for Depression in the elderly
§A course of ECT treatment can be stopped once therapeutic outcomes have been reached
is ECT appropriate to treat depression in teh elderly?
stimulant use in the elderly
§Used to improve mood in apathetic elderly
§Effectiveness has not been fully established with mostly anecdotal reports on such therapy, but if used generally start at low doses given in the morning
§Abuse and addiction in elderly in carefully selected cases for such treatment are rare
transcranial magnetic stimulation
§Non-invasive procedure that uses magnetic fields to stimulate dopamine modulation of neurons in the brain which in some individuals is thought to improve symptoms of Depression
§May be tried when other treatments for Depression have not been effective. Results of efficacy have been modest
§An outpatient procedure which typically requires five treatments per week with each session lasting about 37 minutes for a four to six week period (20-30 treatments)
vagal nerve stimulation
§Adjunctive treatment for treatment-resistant depression
§A device (pulse generator) is implanted in chest with a wire threaded to the left vagus nerve. Electrical signals are carried by vagus nerve to brain every few minutes
§Controversial treatment, but endorsed by American Psychiatric Association and FDA approved
§Depression first, followed by neurocognitive disorder
§Relatively abrupt onset: a matter of weeks
§Patient shows a lack of effort: "I don't know"
§Clears with antidepressant treatment
clinical signs of dementia syndrome of depression (pseudodementia)