2.3 Chemical messengers
1/129
Earn XP
Description and Tags
2.3 Chemical messengers
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
130 Terms
What is a chemical messenger
is a substance that can transmit information within an organ or between organs.
It requires specialized cells to release them and specific molecules to stop them.
Which types of chemical messengers do we have?
Neurotransmitters
Neuromodulators
Hormones
Pheromones
Neurotransmitters
They are manufactured by neurons and their function is to transmit information through the synaptic cleft and nerve impulses.
Chemical substances, created by the body, that transmit information signals from a neuron across synapses.
Some drugs can be very similar to neurotransmitters in part of their chemical structure, allowing them to act through the receptors for these neurotransmitters.
Neuromodulators
Chemical substances released by neurons that can modify the effects of neurotransmitters.
Neuromodulators do not produce postsynaptic potentials; instead they modulate the activity of a large number of neurons.
E.g. Endorphin
Hormones
Chemical messengers of the body and are part of the endocrine system.
They are produced by the endocrine glands, transported through the bloodstream to tissues and organs, and control most of our body's major systems.
Pheromones
Chemical substances produced by other animals that affect reproductive physiology & behavior.
Criteria which define a substance as a neurotransmitter
It is synthesized and present inside the presynaptic neuron.
The substance must be released in response to presynaptic depolarization (Ca+ dependent).
It is released in sufficient quantity to exert a defined action on the postsynaptic neuron.
Specific receptors for the substance must be present on the cell.
When administered from the outside (as a drug) it exactly mimics the action of the endogenous release transmitter.
There is a specific mechanism to remove it from its site of action (the synaptic cleft).
Types of neurotransmitters:
There are a number of neurotransmitters but acetylcoline (ACh) and noradrenaline (epinephrine) are the main types.
The synapses releasing the acetylcholine
known as the cholinergic synapses
Synapses releasing the noradrenaline
Known as the adrenergic synapses
Sequence of event typical cholinergic synapses
an arriving action potential depolarizes the presynaptic membrane.
the calcium (Ca2+) ion channels open and the calcium ions enter the cytoplasm of synaptic knob.
the calcium ions cause synaptic vesicles to fuse with the presynaptic membrane and release their content (ACh) into synaptic cleft through exocytosis.
Neurotransmitter groups
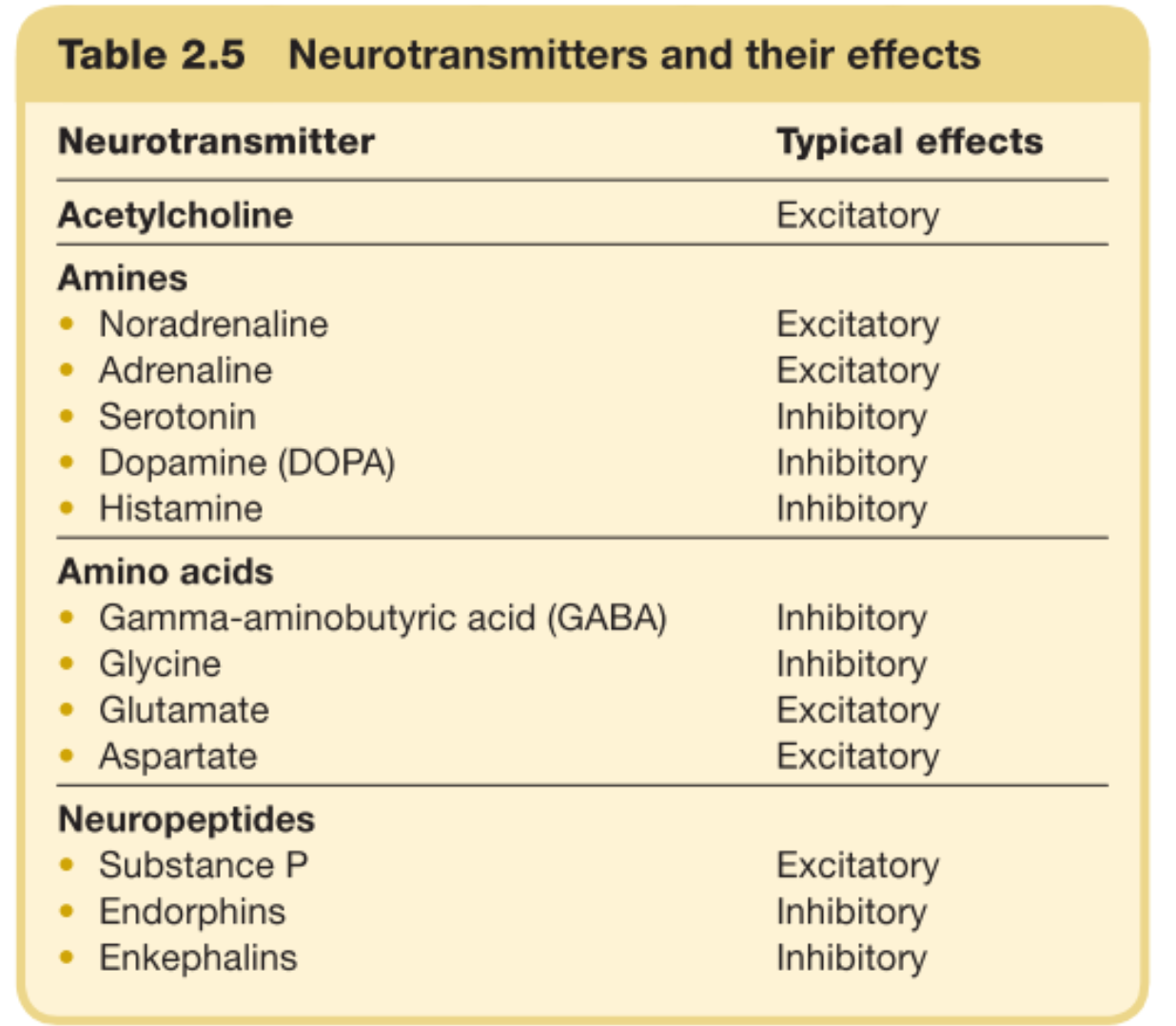
Neurotransmitter: ACETYLCHOLINE
Excitatory effect
Receptor: Cholinergic (muscarinic and nicotinic)
Functions: Parasympathetic response, skeletal muscle, memory
Synthesis of ACETYLCHOLINE
Choline and Acetyl coenzyme A: Acetylcholine
First neurotransmitter discovered.
Main neurotransmitter secreted by efferent axons from the central nervous system to the peripheral nervous system.
Important role in learning and memory.
ALL MUSCLE MOVEMENT IS CARRIED OUT BY THE RELEASE OF ACETYLCHOLINE
Storage of ACETYLCHOLINE
In presynaptic terminals
Vesamicol: a drug that causes a depletion of acetylcholine in vesicles.
Reuptake of ACETYLCHOLINE
Choline transporter, key in the reuptake function.
Hemicholine: Inhibits the choline transporter.
Role of acetylcholinesterase
ACh is degraded by the enzyme acetylcholinesterase (AChE)
Present in the postsynaptic membrane.
Receptors of ACETYLCHOLINE
Muscarinic Receptors (metabotropic)
Nicotinic Receptors (ionotropic)
Effects of ACETYLCHOLINE
located in the dorsolateral pons has a role in REM sleep
located in the basal forebrain are involved in activating the cerebral cortex, facilitating perceptual learning.
located in the medial septum control the electrical rhythms of the hippocampus and modulate its functions of formation of memories.
Parasympathetic Nervous System release the neurotransmitter:
Both pre- and post-axons release ACETYLCHOLINE.
Sympathetic Nervous System release the neurotransmitters:
• Preganglionic axons → Ach
• Postganglionic axons → NA
Neurotransmitter: EPIEPHRINE
Receptor: Alfa & Beta adrenergic
Functions: Sympathetic response
Neurotransmitter: NOREPINEPHRINE
Excitatory effect
Receptor: Alfa & Beta adrenergic
Functions: Sympathetic response, arousal, attention, mood
Adrenergic receptors
Sensitive to adrenaline as well as noradrenaline.
Receptors B1 + B2 =
They increase the neuron's response to its excitatory synapses.
Receptor A1 =
Postsynaptic slow depolarisation - Excites the neuron, making it more likely to fire.
Receptor A2 =
Slow hyperpolarisation - Inhibits the neuron, making it less likely to fire.
Pre- (autoreceptors) and postsynaptic - regulate the release of noradrenaline and act as a feedback mechanism.
Medications and Drugs Affecting Noradrenaline:
Reserpine
Clonidine
Propranolol
MDMA (Ecstasy) and Cocaine
Selective NA Reuptake Inhibitors (SNRIs)
Reserpine
storage inhibitor that prevents the vesicles from storing noradrenaline.
Clonidine
autoreceptor agonist that inhibits noradrenaline synthesis and release.
often used to treat opioid withdrawal
Propranolol
A beta-receptor antagonist, which blocks the action of noradrenaline (and adrenaline).
Used in treatment for anxiety disorders.
MDMA (Ecstasy) and Cocaine
These drugs inhibit the reuptake of noradrenaline, along with serotonin and dopamine.
Cause a rush of euphoria by increasing the levels of noradrenaline
Selective NA Reuptake Inhibitors (SNRIs)
Reboxetine, a medication that inhibits the reuptake of noradrenaline, increasing its levels in the brain.
used for depression, especially in cases where fatigue, apathy, and cognitive impairment are present due to low noradrenaline.
NOREPINEPHRINE/ Noradrenaline pathways
From locus coeruleus to different parts of the encephalon.
The signals are sent to amygadala, thalamus, hypothalamus, hippocampus and cortex.
Noradrenaline and Mood Disorders
Both noradrenaline (NA) and serotonin (5HT) are involved in mood disorders like depression, anxiety, and bipolar disorder.
Low levels of NA are associated with fatigue, apathy, and cognitive disorders, contributing to conditions like depression.
Adrenaline/Epinephrine
Molecule that carries information or message between the organs and the body (body periphery).
Prepares the body as a fight or flight system.
Works more like a hormone rather than neurotransmitter
Noradrenaline/Norepinephrine
• It acts with similar functions to Adrenaline but rather as a neurotransmitter
• Its identification was carried out by Von Euler in 1946.
• Increases the state of vigilance (alertness, arousal, activation).
• It prepares us to face events
• Food and hunger control
• Sexual behavior
• Learning, memory and attention
Neurotransmitter: DOPAMINE
Inhibitory effect
Receptors: DA1, DA2, DA3, DA4, DA5 (five types of receptors)
Functions: reward & reinforcement, motivation, extra-pyramidal motor control
DOPAMINE produce
It can produce EPSP or IPSP depending on the postsynaptic receptor.
DOPAMINE involved in
Movement
Attention
Learning
Reinforcing effects of drugs - triggers dopamine release in the nucleus accumbens
Disorder related to DOPAMINE alteration
Parkinson´s Disease
Symptoms:
Tremors
Stiffness of the limbs
Alterations in balance
Difficulty in initiating movements.
Causes of Parkinson´s Disease:
Degeneration of the Nigrostriatal System = degeneration of dopaminergic neurons in the substantia nigra which connects to caudate nucleus (brain region involved in controlling movement)
Dopamine Loss = loss of these neurons leads to the characteristic motor symptoms of Parkinson's disease.
Treatment for Parkinson´s Disease:
L-DOPA = precursor to dopamine
Deep Brain Stimulation (DBS) = implanting a device that sends electrical impulses to specific areas of the brain
Receptors of DOPAMINE
Indirect transduction (G Protein)
D1 and D5 (act through G protein)
D2, D3 and D4 (acting through G-proteins)
D2 and D3 (autoreceptors)
Degradation enzymes of DOPAMINE
MAO and COMT(catechol-O-methyltransferase)
Inhibitors
MAO: clorgiline, selegiline, tranylcypromine and phenelzine)
COMT: tropolone, tolcapone and entacapone)
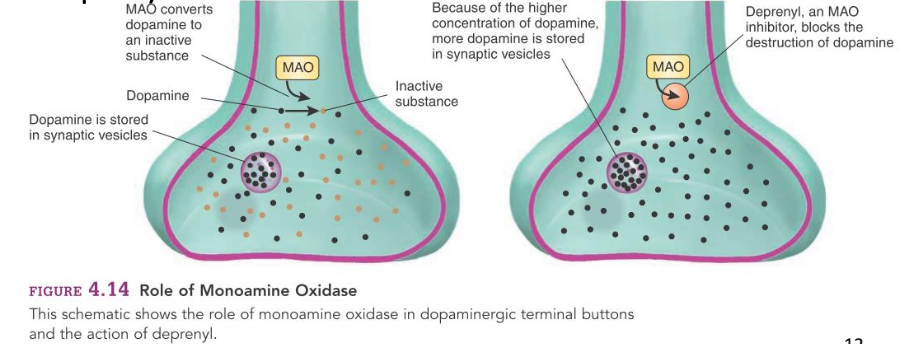
Metabolite after inactivation related to DOPAMINE
Homovallinic acid (HVA)
Dopamine and social media
Social media and new technologies can activate the dopamine system by giving instant rewards (likes, notifications, etc.).
This can make these platforms addictive, as they provide constant stimulation and feedback, leading to frequent dopamine surges.
Some people might develop dopamine-driven addictive behaviors as they seek the rewarding sensations from using social media, often at the cost of other important activities.
DOPAMINERGIC NEURONS
The brain contains several systems of dopaminergic neurons.
The most important originate in the midbrain: in the substantia nigra and in the ventral tegmental area
Dopaminergic neuronic pathways
Mesocortical pathway
Mesolimbic pathway
Nigrostriatal pathway
Tuberoinfundibular pathway
Mesocortical pathway
Essential cognitive pathway, connecting the ventral tegmental area (VTA) with the cerebral cortex, particularly at the frontal level.
Mesolimbic pathway
Connects the VTA with the limbic system.
Associated with reward mechanisms and sustained attention.
Nigrostriatal pathway
Pathway from substantia nigra to basal ganglia.
Influences movement control.
Tuberoinfundibular pathway
Pathway from the arcuate nucleus of the mediobasal hypothalamus to the median eminence.
Regulates prolactin secretion.
Hypothalamus-Pituitary Axis.
Dopamine functions
Movement, attention, learning, and the reinforcing effects of drugs that people tend to abuse.
Dopamine and catecholamine
Dopamine constitutes about 80% of the catecholamine content in the brain.
Functions of Dopamine inside the PNS
In blood vessels it inhibits norepinephrine release and acts as a vasodilator.
in the kidneys it increases sodium excretion and urine output.
in the pancreas, it reduces insulin production.
in the digestive system, it reduces gastrointestinal motility and protects intestinal mucosa
in the immune system, it reduces the activity of lymphocytes
Stimulus Perception of dopamine
When a rewarding stimulus (e.g., food, a social connection, or a pleasurable activity) is encountered, sensory information is processed by the brain.
Dopamine Release
The VentralTegmentalArea releases dopamine, a neurotransmitter associated with pleasure and reward, into the nucleus accumbens and other connected regions.
Feedback Loop in dopamine
The nucleus accumbens signals the prefrontal cortex, leading to conscious awareness of the reward and motivation to repeat the behavior.
The hippocampus and amygdala encode contextual and emotional aspects of the rewarding experience
Behavior Reinforcement
Dopamine surges reinforce behaviours, making individuals more likely to repeat actions that lead to similar pleasurable outcomes.
Neurotransmitter: SEROTONIN
Inhibitory effect
Receptors: 5HT1, 5HT2 — 5HT7 (seven types of receptors).
Functions: Digestion, sleep, anxiety, mood, appetite, social behvaiour
Where is SEROTONIN Produced?
Serotonin is produced by neurons in the Raphe nuclei (a group of cells in the brainstem)
Tryptophan
amino acid found in food that is a precursor to serotonin.
Serotonin (5-HT) is a neurotransmitter that helps regulate many behaviors and emotions.
Functions of SEROTONIN
Ingestion: Helps control appetite and eating behavior.
Dreaming: Involved in regulating sleep, especially during dreams (REM sleep).
Mood: Affects mood, and low levels are linked to depression.
Pain Regulation: Helps reduce pain perception in the body.
Termination of the Stress Response: Helps stop the body's reaction to stress once it's no longer needed.
Key role in mental disorders
Degradation of SEROTONIN
Serotonin is broken down in the body by an enzyme called monoamine oxidase (MAO).
MAO works both inside the cell (intracellular) and outside the cell (extracellular) to break down serotonin, reducing its levels in the synapse.
First Antidepressants Discovered
Monoamine Oxidase Inhibitors (MAOIs)
They work by inhibiting MAO, preventing the breakdown of neurotransmitters like serotonin
Reuptake of SEROTONIN
After serotonin is released into the synapse, it is typically reabsorbed (reuptake) by the presynaptic neuron via active transport pumps, specifically the serotonin transporter (SERT).
Antidepressants and 5HT
Reuptake inhibitors (like SSRIs) block the reabsorption of serotonin, making more serotonin available in the synapse. This action increases serotonin levels and helps improve mood and alleviate depression symptoms.
antidepressants interact
Interact with one or more receptors related to monoaminergic receptors.
Block the reuptake of monoamines
Block alpha-2 receptors
Block monoamine oxidase (MAO) enzyme
Which cortex is affected during depression?
Ventromedial prefrontal cortex
Receptors SEROTONIN
Receptors (at least 9 types identified)
- 5-HT1A, 5-HT1B, 5-HT1C, 5-HT1D, 5-HT1E
- 5-HT2A, 5-HT2B, 5-HT2C
- 5-HT3
- 5-HT4
- 5-HT5A, 5-HT5B
- 5-HT6
- 5-HT7
SEROTONIN Mood Regulation
Serotonin is commonly associated with mood stabilization.
It helps regulate mood, happiness, and well-being.
Low levels of serotonin are linked to depression and anxiety.
SEROTONIN
SEROTONIN
SEROTONIN Appetite and Digestion
In the gastrointestinal tract, serotonin influences appetite, satiety, & digestion.
About 90% of the body's serotonin is found here.
It helps control gut motility, aiding in processes like peristalsis and the secretion of digestive enzymes.
SEROTONIN Sleep Regulation
Serotonin plays a crucial role in the sleep-wake cycle.
It is converted into melatonin in the pineal gland, which helps regulate sleep patterns.
Serotonin levels also influence the quality of sleep.
SEROTONIN Cognitive Functions
Serotonin impacts learning, memory, and cognition.
It affects how we process information, make decisions, and learn from experiences.
SEROTONIN Nausea and Vomiting
Serotonin receptors in the gut and the brainstem's chemoreceptor trigger zone can trigger nausea and vomiting, especially in response to toxins or chemotherapy drugs.
SEROTONIN Blood Clotting
can promote vasoconstriction & platelet aggregation, aiding in blood clotting.
It's released by platelets to facilitate wound healing.
SEROTONIN Pain Perception
Serotonin can modulate pain perception.
It's involved in the descending pain pathways that inhibit pain signals, contributing to pain relief.
SEROTONIN Sexual Function
Serotonin affects sexual behavior and libido.
High levels of serotonin can decrease sexual desire & can cause sexual dysfunction, which is one reason why some antidepressants that increase serotonin might lead to side effects like reduced libido.
SEROTONIN Bone Health
Recent research suggests serotonin might have roles in bone metabolism, influencing bone density and structure, although the exact mechanisms can be complex and involve both central and peripheral serotonin pathways.
SEROTONIN Stress Response
It plays a role in how the body responds to stress, interacting with the hypothalamic-pituitary-adrenal (HPA) axis to modulate stress hormone release.
SEROTONIN Social Behavior
Serotonin is implicated in social behavior, aggression, and even decision-making in social contexts.
It can modulate prosocial behaviours like cooperation and empathy.
SEROTONIN Temperature Regulation
Serotonin helps regulate body temperature, influencing thermoregulatory responses.
Neurotransmitter: GLUTAMATE
Receptors: NMDA, AMPA, Kainate
Functions: Main excitatory transmitter (CNS)
GLUTAMATE
Most important or principal excitatory neurotransmitter in the brain and spinal cord.
Responsible for 75% of neurotransmissions.
Synthesis of GLUTAMATE
by the transmission of α-ketoglutaric acid.
Receptors of GLUTAMATE
Kainate receptor
NMDA Receptor
AMPA Receiver
Roles of GLUTAMATE
Vital role in learning and memory
Learning and Long-Term Potentiation (LTP)
Excitotoxicity
Chinese Food Syndrome
Monosodium glutamate (MSG), often found in Chinese food, can cause neurological symptoms in sensitive individuals.
Why can Chinese Food Syndrome occur?
When we eat a lot of food with GLUTAMATE
because GLUTAMATE is the most excitatory mechanism
Excitotoxicity
Occurs when there is an excess of glutamate in the brain, which can lead to neuronal death.
This happens due to high calcium levels inside the neuron, leading to the formation of free radicals that can damage and kill neurons
Learning and Long-Term Potentiation (LTP)
Glutamate is involved in learning through the mechanism LPT
NMDA receptors (a type of glutamate receptor) are critical for synaptic changes that underlie learning = biological basis of learning
Chinese Food Syndrome sympotoms:
Vertigo
Tachycardia (rapid heart rate)
Nausea and vomiting
Temporary paralysis
GLUTAMATE action through receptors
Acts through several types of receptors, including ionotropic receptors which directly affect ion channels, and metabotropic glutamate receptors (mGluRs) which influence intracellular signaling pathways.
Why is the balance between glutamate and inhibitory neurotransmitters like GABA vital?
Glutamate is excibitory, while GABA is inhibitory.
The balance between them is vital for maintaining normal brain function.
Dysregulation in glutamate
Can lead to various neurological and psychiatric conditions, which is why glutamate modulators are explored for therapeutic purposes in disorders ranging from schizophrenia to depression.
Neurotransmitter: GABA
Receptors: GABAA & GABAB
Functions: Main inhibitory transmitter (brain)
Functions of GLUTAMATE
Neuronal Excitation
Learning and Memory
Brain Development
Sensory Information Processing
Motor Control
Neurotransmitter Release
Pain Sensation
Cognitive Functions
Mood Regulation
Neurotoxicity
Synaptic Plasticity
Addiction and Reward
Motor Control of GLUTAMATE
Involved in motor control in the spinal cord
Neurotransmitter Release of GLUTAMATE
Glutamate can influence the release of other neurotransmitters, both excitatory and inhibitory, by acting on presynaptic receptors to either enhance or inhibit neurotransmitter release.
Pain Sensation of GLUTAMATE
Glutamate is a key player in the transmission of nociceptive (pain) signals.
It's involved in both acute pain signaling and in the central sensitization that contributes to chronic pain conditions.
Cognitive Functions of GLUTAMATE
Beyond learning and memory, glutamate influences other cognitive functions such as attention, decision-making, and executive functions through its actions in various cortical areas.
Mood Regulation of GLUTAMATE
Although primarily known for its excitatory role, imbalances in glutamate signaling can contribute to mood disorders.
For instance, excessive glutamate activity has been implicated in conditions like depression and anxiety.