Fecal Analysis
1/80
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
81 Terms
Too little water intake causes ______, while too much water intake causes ______.
constipation, diarrhea
Diarrhea can be defined as an increase in ... of bowel movements.
volume, liquidity, frequency
In the Bristol Stool Scale, diarrhea is defined as types ______.
5-7
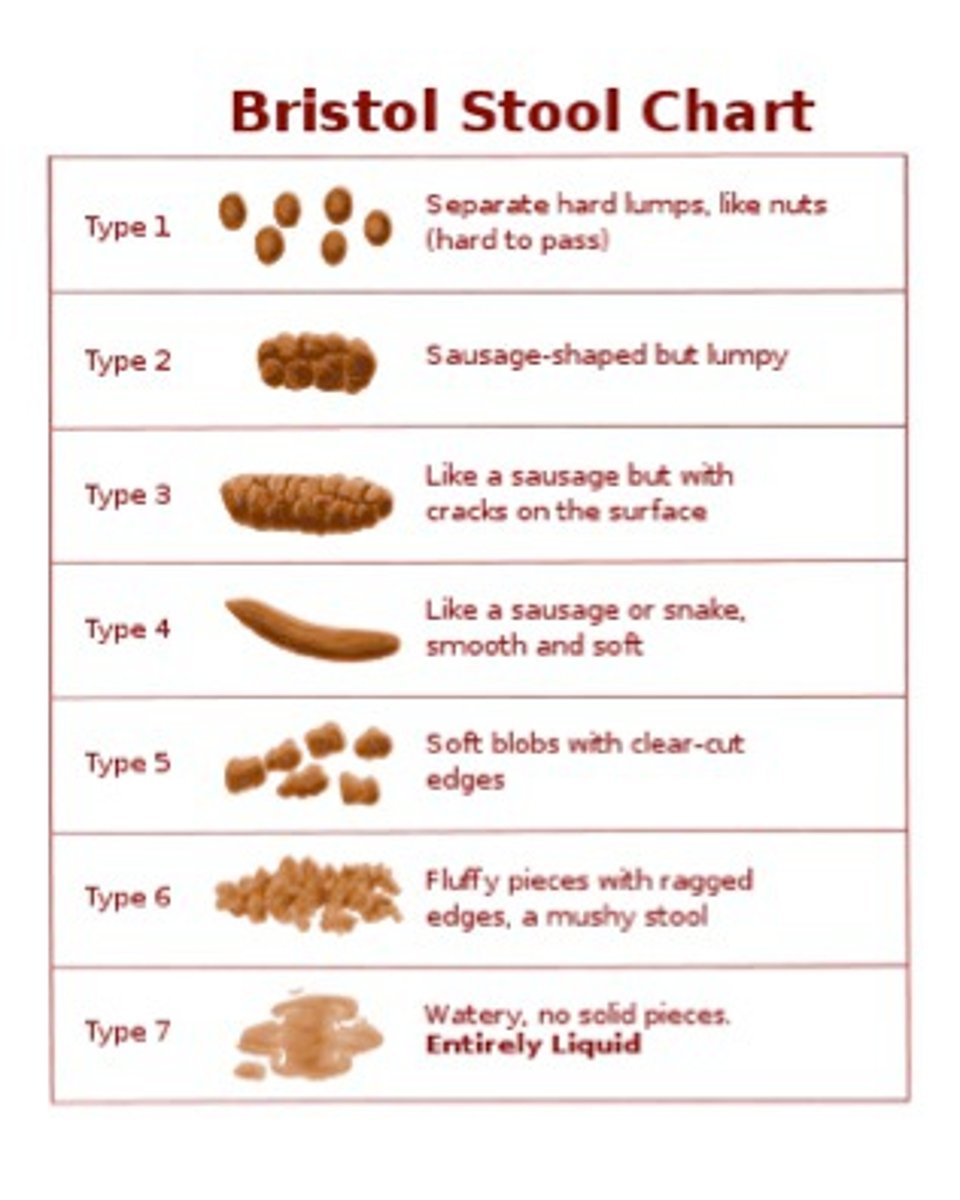
Watery diarrhea contains no ...
- WBCs
- Lactoferrin
- Calprotectin
- Blood
- Increased fat
Watery diarrhea is associated with what three types of disorders?
- Functional
- Secretory
- Osmotic
Fatty diarrhea can be due to ______ or ______ of nutrients.
malabsorption, maldigestion
Inflammatory diarrhea has the presence of any of the following ...
- WBCs
- Lactoferrin
- Calprotectin
- Blood
Functional disorders causing watery diarrhea will show improvement at ______ and with ______.
night, fasting
Functional disorders have intestinal ______, causing watery diarrhea.
hypermotility
What are the functional disorders causing watery diarrhea?
- Intestinal distention
- IBS
- RGE
- Fiber, castor oil, emotions, nerves, hormones
Stimulation of intestinal motility by intestinal distention causes a shorter ______ time and therefore buildup of water.
reabsorption
IBS S/Sx
- Muscle sensitivity
- Cramping
- Bloating
- Flatus
- Diarrhea
- Constipation
RGE, rapid gastric emptying causes the ______ to fill up too quickly.
small intestine
Secretory disorders can cause watery diarrhea via ...
- Increased solute secretion
- Reduced water absorption
- High stool volumes
Secretory disorders causing watery diarrhea have persistent S/Sx at ______ and during ______.
night, fasting
What are some enterotoxin-producing organisms which stimulate intestinal secretions?
- Staphylococcus
- E. coli
- Norwalk
- Vibrio
- Salmonella
- Shigella
What are some secretory disorders that cause watery diarrhea?
- Neoplasms
- Crohn's disease
- Gastrectomy, cholecystectomy
- Bile acid malabsorption
Osmotic disorders cause there to be increased amounts of ______ in the intestinal lumen, and therefore an increase in water within the colon.
osmotically active solutes
What are some osmotic disorders causing watery diarrhea?
- Increased retention of water and electrolytes
- Carbohydrate malabsorption (lactose, fructose)
- Laxatives
- Antacids
- Excess sugar alcohols
- Celiac disease
Fatty diarrhea due to malabsorption can be caused by ...
- Loss of surface area
- Impaired circulation
- Impaired lymphatic drainage
- Mucosal infiltration
- genetic mutations
- Impaired motility
- Gastric bypass
Fatty diarrhea due to maldigestion can be caused by ...
- Loss of regulated gastric emptying
- Insufficient pancreatic exocrine function
- Liver or biliary tract disease
Steatorrhea is an increase in stool fat over ______ grams/day.
7
What are the S/Sx of malabsorption or maldigestion?
- Weight loss/failure to thrive
- Edema
- Anemia
- Peripheral neuropathy
- Easy bruising
- Rickets, pathological fractures
- Mental changes
- Impaired night vision
Steatorrhea due to maldigestion can be due to a lack of ______ or an increase in ______.
pancreatic enzymes, neutral fats (not broken down)
Steatorrhea due to malabsorption disorder is caused by an increase in ______.
total fat (fatty acids and salts)
Normal fecal fat level
<100 globules
Bacterial Overgrowth Syndrome is increased bacteria or yeast in the ______.
small intestine
Bacterial Overgrowth Syndrome causes ______.
malabsorption
What are some other causes of malabsorption?
- Parasites
- Viral infections
Inflammatory diarrhea looks ______.
bloody/purulent
Causes of inflammatory diarrhea
- Colorectal cancer
- IBS
- Invasive bacterial or parasitic infection
- C. diff
- Radiation colitis
Stool specimens cannot touch the ______ during collection due to contamination.
toilet bowl/water
The hypochlorites in cleaners often found in the toilet bowls cause a false positive ______ result.
occult blood
Normal stool is brown due to the oxidation of ______ to ______.
stercobilinogen, urobilin
Acholic stools appear ...
Pale, gray, clay-colored, pale yellow/white
Acholic stool is caused by ______ or ______.
post hepatic obstruction, barium
Melena is ______ stools, indicative of large amounts of ______ in the feces.
black, blood
What are some other causes of black stool?
- Charcoal tablets
- Iron therapy
- Pepto-Bismol
Green stool can be caused by ...
- Vegetables
- Biliverdin (antibiotic therapy)
- Food dyes
Red stool indicates ...
- Lower GI bleed (hemorrhoids)
- Beets
- Food dyes
Frothy stool indicates ______.
steatorrhea
Ribbon-like stool indicates ______.
intestinal constriction
Greasy or spongy stool can be caused by ...
- Increased gas
- Steatorrhea
- Constipation
Mucus in the stool is caused by ...
- Constipation
- Malignancy
- Colitis, diverticulitis
- Bacterial or parasitic infection
Normally, there are no ______ in the stool.
leukocytes
Increased neutrophils in the stool is caused by ...
- Ulcerative colitis
- Bacillary dysentery
- Infection
- Abscesses, fistulas
Wet preps of stool use ______ stain, while fixed stool is stained with ______ stain.
methylene blue, Gram/Wright
Undigested striated muscle fibers in the stool indicate ______.
pancreatic insufficiency (CF)
Fecal blood indications
- Colorectal cancer
- Esophageal varices
- Ulcers
- Hemorrhoids
- Drugs (aspirin, iron supplements)
Fecal occult blood relies on ______, which is the least sensitive to reduce false positives.
Guaiac
What are some causes of false positives for occult blood testing?
- Improper collection
- Menstruation
- Hemorrhoidal bleeding
- Myoglobin and hemoglobin in meats and fish
- Peroxidases from intestinal bacteria
- Drugs
- Hypochlorite
What are some causes of false negatives for occult blood testing?
- Ascorbic acid (antioxidants, reducers)
- Outdated or bad reagents
For a quantitative fecal fat test, over 7g of fat in 24 hours suggests ______.
malabsorption
______ stain is used to count the number of fat globules in stool.
Sudan III/IV
Normal fat amounts in stool
- <60 neutral fat globules
- <100 fatty acid fat globules
A fat retention coefficient is used for children who cannot ingest ______g/day of fat.
100
APT is used to detect ______ in feces.
fetal hemoglobin
APT is important in differentiating ______ blood vs ______ blood in feces.
fetal, maternal
For the APT test, a ______ color is positive for fetal blood.
pink
Kleihauer Betke quantitatively measures ______ in maternal blood.
HgF
Fecal carbohydrate tests
- pH
- Clinitest
- Oral tolerance tests to specific sugars
Fermentation of carbs causes fecal pH to drop from 7-7.5 (adult) to ______.
5-6
Clinitest detects ______.
reducing sugars
Clinitest values
Normal = <0.25g/dL
Abnormal = 0.25-0.5g/dL
Carbohydrate intolerance = >0.5g/dL
What are some fecal carbohydrate problems?
- Lactase deficiency
- Celiac disease
- Tropical sprue
- Oral neomycin, kanamycin
- Lactose intolerance
- Xylose
What are the fecal enzymes detected to diagnose decreased pancreas function and CF?
- Trypsin and chymotrypsin
- Elastase-1
Trypsin is degraded in the ______, and therefore not a great diagnostic marker.
distal small bowel
Stool chymotrypsin levels of ______U/g suggest advanced chronic pancreatitis.
<3
Elastase-1 levels of ______mcg/g stool indicate severe insufficiency.
<100
Elastase-1 levels of ______mcg/g stool is normal.
>200
Serum trypsin levels for pancreatic function
<20ng/mL = Chronic pancreatitis (advanced)
>150ng/mL = Pancreatic inflammation
Fecal osmotic gap equation
Osmotic gap = 290 - [2(fecal Na + fecal K)]
Osmotic gap levels
Normal = <125 mOsm/kg
Osmotic diarrhea >100 mOsm/kg
Secretory diarrhea <50mOsm/kg
Chronic diarrhea causes
- IBS
- IBD
- Celiac
What are some S/Sx that raise alarms and warrant further stool tests?
- Anemia
- Unintentional weight loss
- Persistent blood in stool
Functional IBS S/Sx
- Abdominal pain
- Constipation or diarrhea
- Occurs at least 1 day/week over the past 3 months
- Watery diarrhea while awake, often after meals
- Defecation relieves pain
- Worsened with stress or eating
Functional diarrhea (not IBS) S/Sx
- Diarrhea for >25% of stools
- No abdominal pain or bloating
IBD S/Sx
- Blood and pus in stool
- Fever
- Weight loss
- Fatigue
- Skin and joint symptoms
- Family history
- Anal fissures
- Rectal ulcerations
______ test is used to screen for fecal leukocyte activity related to IBD.
Fecal calprotectin
A positive fecal calprotectin result causes a follow up ______ to be done.
colonoscopy
Celiac disease S/Sx
- Malabsorption of gluten/wheat in small intestine
- Chronic diarrhea
- Fatigue
- IDA
- Weight loss