NAP Lab - Practical 2
1/148
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
149 Terms
tract
a bundle of axons traveling together in the CNS
nerve
a bundle of axons traveling together in the PNS
nucleus
a cluster of neuron cell bodies in the cns
ganglion
a cluster of neuron cell bodies in the PNS
gray matter =
cell bodies, glia, etc.
white matter =
myelinated axons
nerve fiber
myelinated or unmyelinated axon
fascicle/fasciculus
a bundle of nerve fibers/axons
endoneurium
CT layer that surrounds a single nerve fiber
perineurium
CT layer that surrounds a fascicle
epineurium
CT layer that surrounds an entire nerve trunk
Olfactory nerve
CN1
Sensory
Sense of smell
disorder caused by damage to olfactory nerve
Anosmia (inability to smell)
Optic nerve
CNII
Sensory
Sense of vision, pupillary light reflex
disorder(s) caused by damage to optic nerve
Ipsilateral blindness
Loss of pupillary light reflex
Color blindness
Oculomotor nerve
CNIII
Motor
Moves eyes up/down/medially, elevates upper eyelid, constricts pupil, adjusts eye lens
disorder(s) caused by damage to oculomotor nerve
Ptosis (drooping eyelid)
Diplopia (double vision)
Trochlear nerve
CN IV
Motor
Moves eye medially and down
disorder(s) caused by damage to trochlear nerve
Diplopia
Difficulty reading
Visual problems during descension
Trigeminal nerve
CNV
Mixed
Blink reflex and sensation from face (sensory)
Chewing (motor)
disorder(s) caused by damage to trigeminal nerve
Trigeminal neuralgia (severe sharp pain in one or more branches of TGN)
Abducens nerve
CNVI
Motor
Moves eye laterally
disorder(s) caused by damage to abducens nerve
diplopia (double vision)
facial nerve
CNVII
Mixed
Blink reflex, facial expression, salivation and tear production (motor/glands)
Sense of taste (sensory)
disorder(s) caused by damage to facial nerve
Bell’s palsy (paralysis or paresis of ipsilateral muscles of facial expression)
vestibulocochlear nerve
CNVIII
Sensory
Sensation of head position and movement (vestibular branch), sense of hearing (cochlear branch)
disorder(s) caused by damage to vestibulocochlear nerve
Conductive deafness (transmission of vibrations prevented in outer or middle ear)
Sensorineural deafness (damage of receptor cells or cochlear nerve)
Glossopharyngeal nerve
CN IX
Mixed
Sense of taste, sensory limb of gag reflex, swallowing, salivation
which gland is responsible for salivation and which nerve controls it
parotid gland; glossopharyngeal nerve
disorder(s) caused by damage to glossopharyngeal nerve
Interruption of gag reflex and swallowing reflex
Decreased salivation
Vagus nerve
CNX
Mixed
Motor limb of gag reflex, swallowing, speech production, regulating visceral organs
disorder(s) caused by damage to vagus nerve
Interruption of gag and swallowing reflex
Difficulty swallowing
Poor digestion
spinal accessory nerve
CN XI
Motor
Elevates shoulders, turns head
disorder(s) caused by damage to spinal accessory nerve
Paralysis of ipsilateral sternocleidomastoid and trapezius
hypoglossal nerve
CNXII
Motor
Moves tongue
disorder(s) caused by damage to hypoglossal nerve
Difficulty speaking and swallowing
Atrophy of ipsilateral tongue
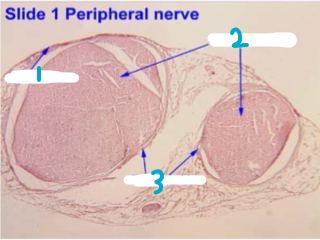
Label this chart
1 - epineurium
2 - nerve fascicles
3 - perineurium
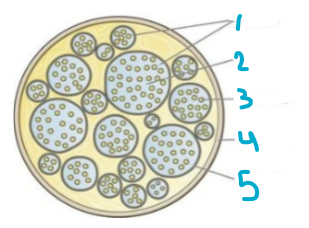
Label this chart
1 - Fasciculi
2 - Endoneurium
3 - Nerve fiber
4 - Epineurium
5 - Perineurium
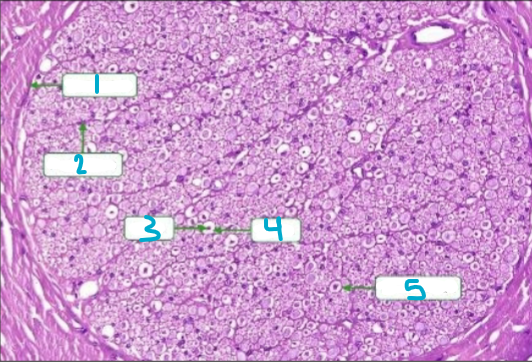
Label this chart
1 - Epineurium
2 - Perineurium
3 - Axon
4 - Myelin
5 - Endoneurium
How can you test olfactory nerve
Smelling something (ex: vanilla extract)
How can you test vestibulocochlear nerve
Trying to locate your phone by hiding it and having someone call you while it’s on vibrate, by seeing if you get dizzy on a swivel chair, or by using the Weber’s or Rinne’s tests
Weber’s test
Tests CN VIII
Tuning fork on top of your head and see if the sound is equal in both ears
Rinne’s test
Tuning fork on jaw and seeing if air conduction is louder or if bone conduction is louder (air conduction should be louder if nerve function is normal)
How to test optic nerve
Snellen chart or colorblind quiz
How can you test hypoglossal nerve
Stick your tongue out and see if it deviates to the side. If it does, your nerve is damaged
How to test trigeminal nerve
Eat something and see if you have difficulties chewing, drink something and see if you have trouble swallowing, or brush a cotton ball on your face and see if you can feel it on your face
How can you test glossopharyngeal nerve
Drink water and see if you have swallowing difficulties
How can you test spinal accessory nerve
Turn your head and shrug your shoulders and see if you have difficulties
How can you test oculomotor nerve
Follow a pen with your eyes or cross your eyes to look at the tip of your nose
what does the somatosensory system consist of
sensory receptors, sensory neural pathways, parts of brain involved in sensory perception
types of somatosensations
touch, pain, temperature, proprioception
stages of somatosensation
Activation of sensory receptors
Receptor responds to stimuli by conversion of a sensory signal to an electrical signal (action potential)
The electrical signal is carried to the brain and processed in specialized regions of brain for that sensation
types of somatosensory receptors
mechanoreceptors, chemoreceptors, thermoreceptors, nociceptors
mechanoreceptors
respond to mechanical deformities/forces
touch, pressure, vibration, stretch, hearing
chemoreceptors
respond to chemical changes in the cellular environment including cell death
taste, smell, blood composition
thermoreceptors
respond to changes in temp
nociceptors
respond to painful stimuli
responds when something may cause harm to tissues
What speeds up transmission of info to the cerebral cortex
Myelination, large diameters, and fewer synapses along the pathway
receptive field
size of an area of skin innervated by a single sensory neuron
tend to be smaller distally and larger proximally
why are fingertips, for example, more sensitive than backs?
higher receptor density and smaller receptive fields
what are the three types of somatosensory pathways that bring sensory info to the brain
conscious relay pathways (DC/ML: discriminative touch/conscious proprioception; ALS: discriminative pain and temperature), divergent pathways (single sensory signal can take different neural pathways w/ different responses), and unconscious relay pathways (proprioception from muscle spindles, tendon tension/stretch, position info)
DC/ML pathway
1st ON (psuedounipolar) enters the spinal cord, ascends ipsilaterally until reaching the medulla, where it synapses with second order neuron in the gracilis (midline; carries sensations from lower body) or cuneatus (lateral; upper body) nucleus.
2nd ON (interneuron) axon crosses the midline of medulla and ascends until synapsing with ventral posterolateral nucleus of the thalamus.
3rd ON axon ascends from the thalamus thru internal capsule to cerebral cortex
where is the somatosensory cortex
in the postcentral gyrus of the anterior parietal lobe
Anterolateral/spinothalamic pathway
1st ON (pseudounipolar) synapses with 2nd ON right after entering spinal cord. 2nd ON (interneuron) axon crosses the midline of the spinal cord, ascends contralaterally and synapses with the VPL of thalamus. 3rd ON axon ascends from thalamus through internal capsule to cerebral somatosensory cortex
precentral gyrus processes what
motor info
somatosensory homonculus
shows how much of the somatosensory cortex is devoted to a specific part of the body
electrodiagnostic studies
sensory nerve function can be examined by recording its electrical activity using either SEPs or nerve conduction studies
Somatosensory Evoked potentials (SEPs)
a type of electrodiagnostic study that evaluates peripheral nerves and CNS pathways and measures speed of impulses from sensory neuron to brain
Nerve conduction studies (NSCs)
A type of electrodiagnostic study to evaluate the function of a peripheral nerve; can determine damage to a nerve; measures how fast an electrical impulse moves along the nerve.
3 measurements are compared to normative values for the strength and speed of a nerve signal
what are the 3 measurements for the strength and speed of a nerve signal used in NSCs? describe them
distal latency (time required for depolarization to reach distal recording site—msec), amplitude (strength of a signal in uV; indicates the number of axons conducting), and conduction velocity (m/s)
gryi
rounded elevations/ridges on the surface of cerebrum
sulci
grooves/depressions on the surface of the cerebrum
fissures
deep groove/sulcus that divides an organ into lobes or parts
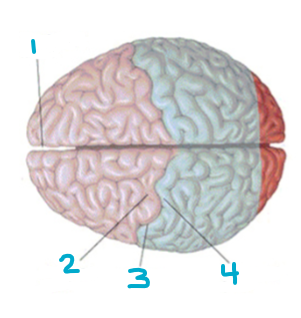
Label this
1 - longitudinal fissure
2 - precentral gyrus
3 - sulcus
4 - postcentral gyrus
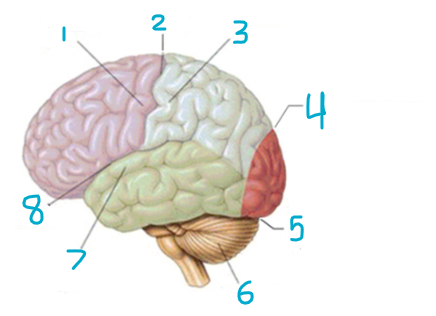
Label this
1 - precentral gyrus
2 - central sulcus
3 - postcentral gyrus
4 - parieto-occipital sulcus
5 - transverse cerebral fissure
6 - cerebellum
7 - superior temporal gyrus
8 - lateral fissure
ataxia
Improper reporting of somatosensory info; interruption of proprioceptive information
Feedback issues cause lack of muscle control and inability to coordinate volutnary movements
Balance problems, trouble walking, slurring words
Sensory ataxia (proprioception problem; only a problem when eyes are shut) or cerebellar ataxia (gait problems, lack of coordinated movements)
primary hyperalgesia
Increased or excessive response to painful stimulus above normal pain
Often caused by nerve damage
secondary hyperalgesia
painful stimulus spreads to other parts of your body beyond where the pain stimulus originates
allodynia
Pain caused by a stimulus that does not normally cause pain
paresthesia
Sensations of tingling, burning, itching, or numbness, mostly in arms or legs
Not typically painful
Can be temporary or chronic
Analgesia
Inability to feel pain; interruption of the pain pathways
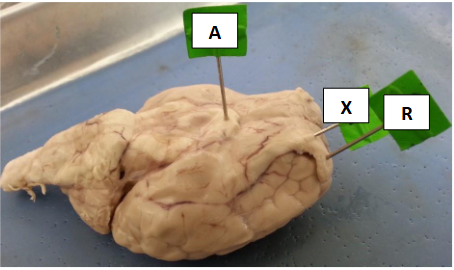
Label this
A - optic chiasm
X - olfactory nerve
R - olfactory bulb
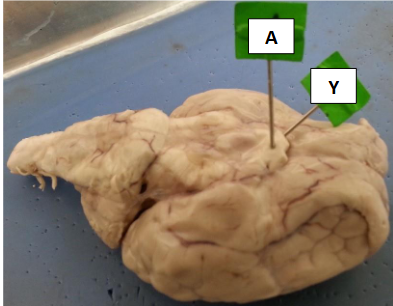
Label this
A - optic
Y - optic nerve

Label this
C - trigeminal nerve
D - medulla
P - spinal accessory
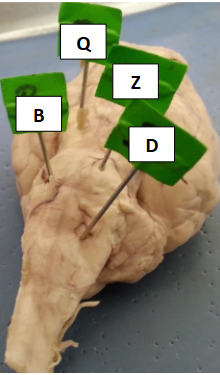
Label this
Q - oculomotor nerve
B - abducens
Z - pons
D - medulla
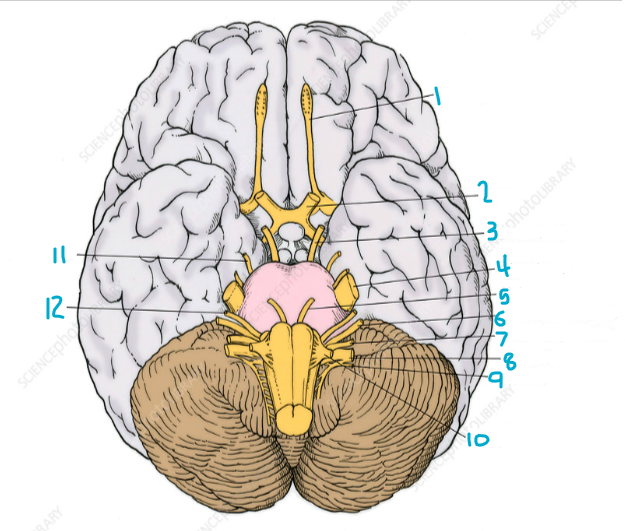
Label this
1 - Olfactory tract
2 - Optic nerve
3 - Oculomotor
4 - Trigeminal
5 - Abducens
6 - Vestibulocochlear
7 - Glossopharyngeal
8 - Vagus
9 - Accessory
10 - Hypoglossal
11 - Trochlear
12 - Facial
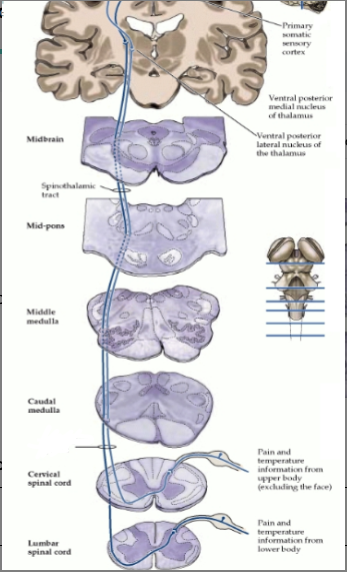
What is this a picture of
Anterolateral system/Discriminative Pain and Temperature pathway
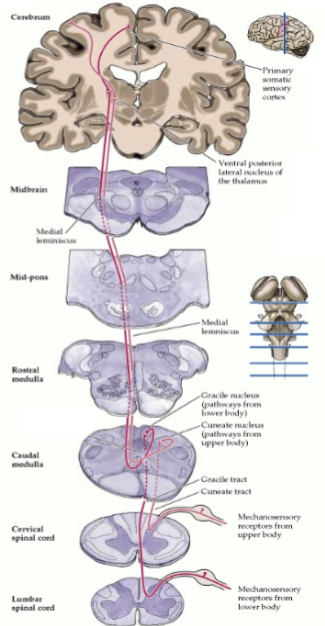
What is this a picture of?
DC/ML pathway (Discriminative touch and conscious proprioception)
which cranial nerves are found on the lateral pons
trigeminal
which cranial nerves are associated with the ability to shrug your shoulders
spinal accessory
which cranial nerves help you wrinkle your forehead and raise your eyebrows
facial
which cranial nerves are associated with the gag reflex
glossopharyngeal and vagus
which cranial nerves are found medially at the junction of the pons and medulla
abducens
which cranial nerves are the largest
trigeminal
which cranial nerves extend on the underside of the frontal lobe to synapse in the temporal lobe
olfactory
which cranial nerves send signals from the inner ear
vestibulocochlear
which cranial nerve has a branch receiving sensations from the maxilla (upper lip)
trigeminal
which cranial nerve innervates the sternocleidomastoid muscle and allows turning your head from side to side
spinal accessory
which cranial nerves are associated with eye movements
oculomotor, trochlear, abducens
which 2 cranial nerves are responsible for taste sensations
glossopharyngeal (posterior 1/3) and facial (anterior 2/3)