CHA 101 Final Exam
1/216
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
217 Terms
What does the posterior triangle of the cervical region do?
it transmits nerves and vessels from the neck to the upper limb, and consists of 2 sub triangles:
1) occipital triangle
2) supraclavicular triangle
What does the anterior triangle of the cervical region do?
- it is associated the with following structures:
esophagus, pharynx, larynx, trachea, thyroid gland, and parathyroid gland
- And it consists of 4 sub triangles: musclar, carotid, digastric, submental
What are the borders of the posterior triangle?
1) sternocleidomastoid
2) Trapezius
3) Middle 1/3 of the clavicle
What are the contents of the Posterior Triangle?
1. CN XI
2. Cervical Plexus
3. Omohyoid Muscle
4. External Jugular Vein
5. Subclavian vessels
6. Brachial Plexus
7. Phrenic Nerve
What lies in between the infra hyoid muscles?
1. laryngeal prominence
2. cricoid cartilage
3. cricothyroid membrane
the thyroid gland is deep to which muscles
sternohyoid and sternothyroid
What does the parathyroid do?
regulates Calcium and increases calcium reabsorption to increase serum calcium
What does the carotid sinus do?
at base of internal carotid artery. it detects stretch in walls due to an increase in pressure
-CN IX
What does the carotid body do?
contains chemoreceptors that detect changes in O2, CO2 and arterial pH
-CN IX
Choanae
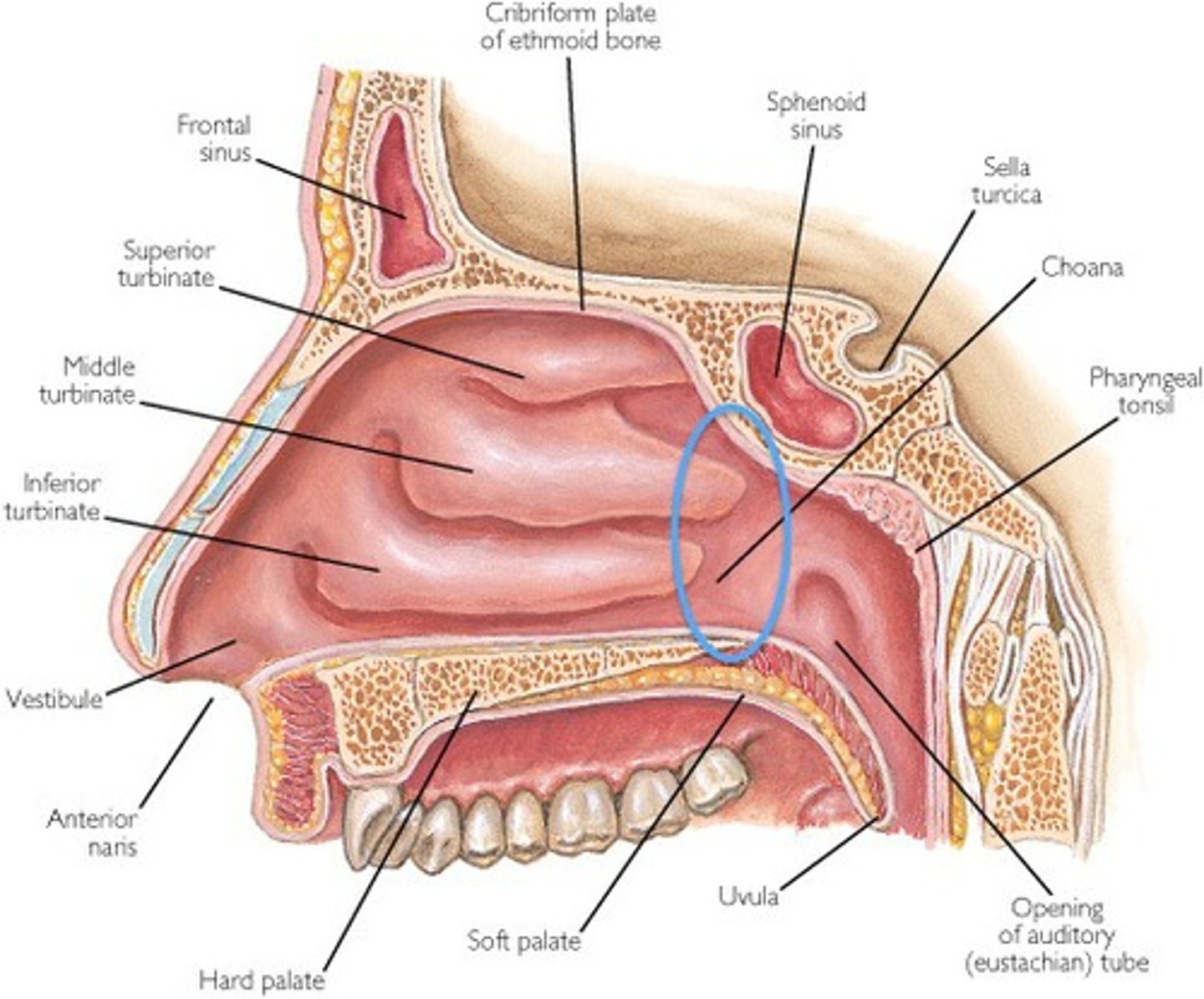
Adenoids
enlarged pharyngeal tonsils
If food gets caught in the piriform recess, what structures can get damaged?
superior and inferior laryngeal vessels, internal and recurrent laryngeal nerves!!!
The muscular layer of the pharyngeal walls is composed of 6 voluntary muscles involves in speaking and swallowing:
- 3 pharyngeal constrictors:
a) superior
b) middle
c) inferior
- 3 Pharyngeal elevators
a) palatopharyngeus
b) salpingopharyngeus
c) stylopharyngeus
Superior Pharyngeal Constrictor
originates from the pterygomandibular raphe, mandible and lateral pterygoid plate
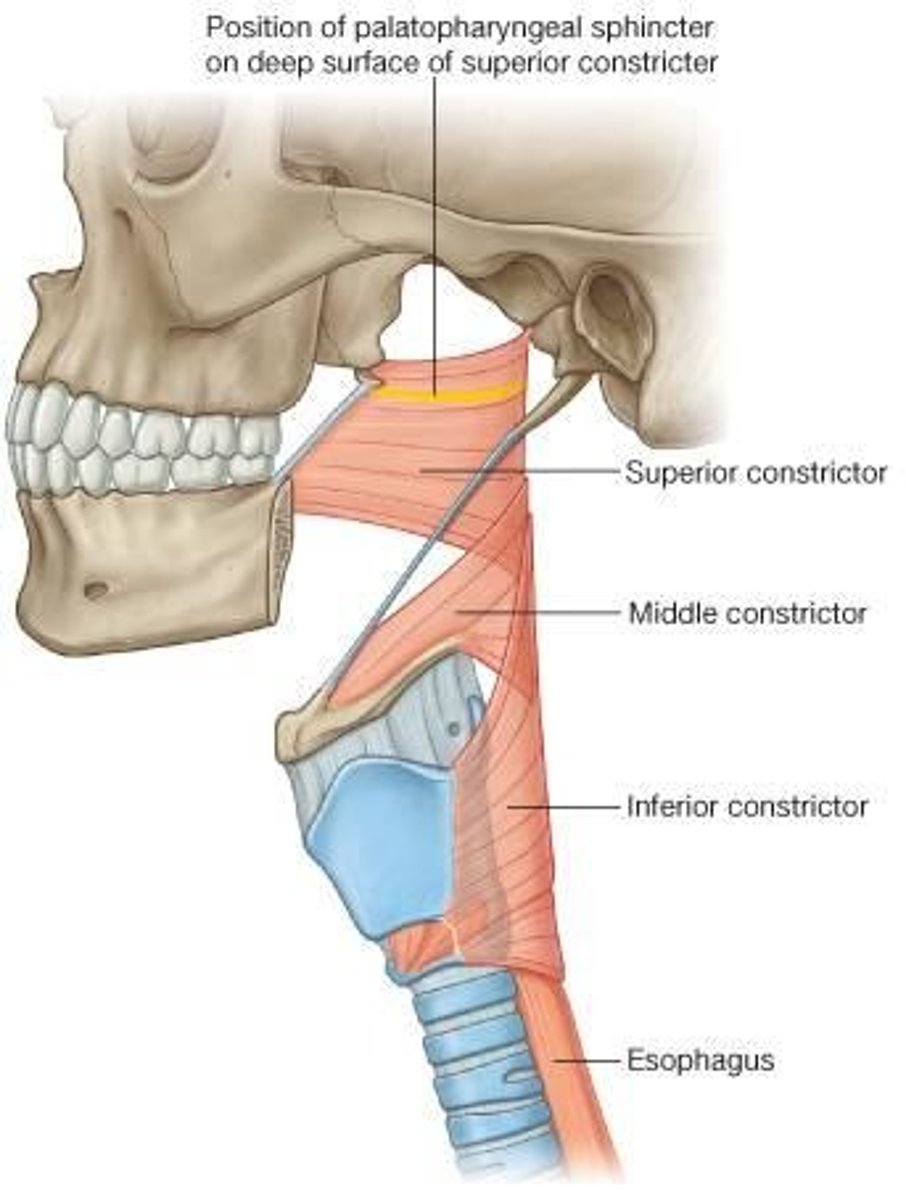
Middle Pharyngeal Constrictor
originates from hyoid bone
the stylopharyngeus muscle separates the middle and superior pharyngeal constrictor
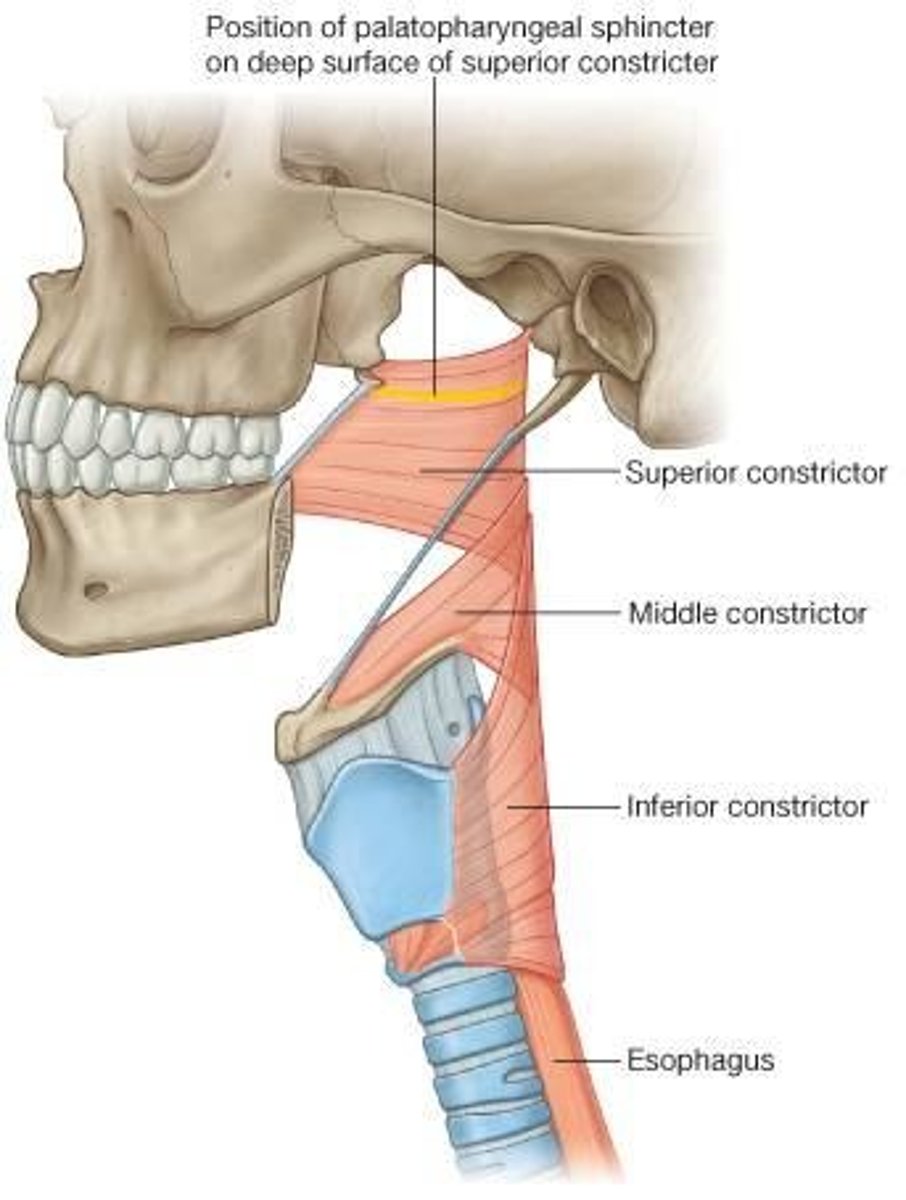
Inferior Pharyngeal Constrictor
originates from the thyroid and cricoid cartilages
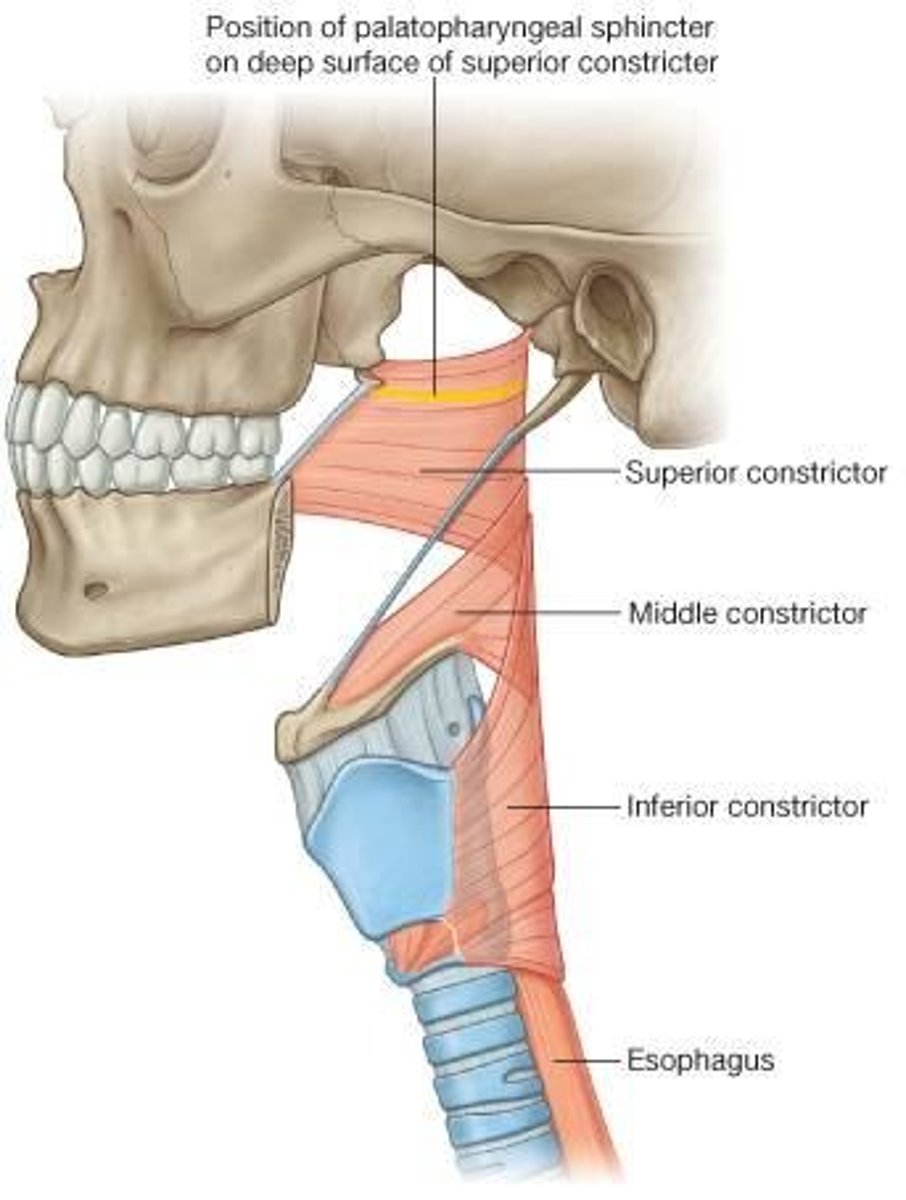
Palatopharyngeus
originated from the hard palate and inserts into the side of the pharynx and the thyroid cartilage. Function = elevates the pharynx and larynx for swallowing and speaking
- innervated by VAGUS NERVE
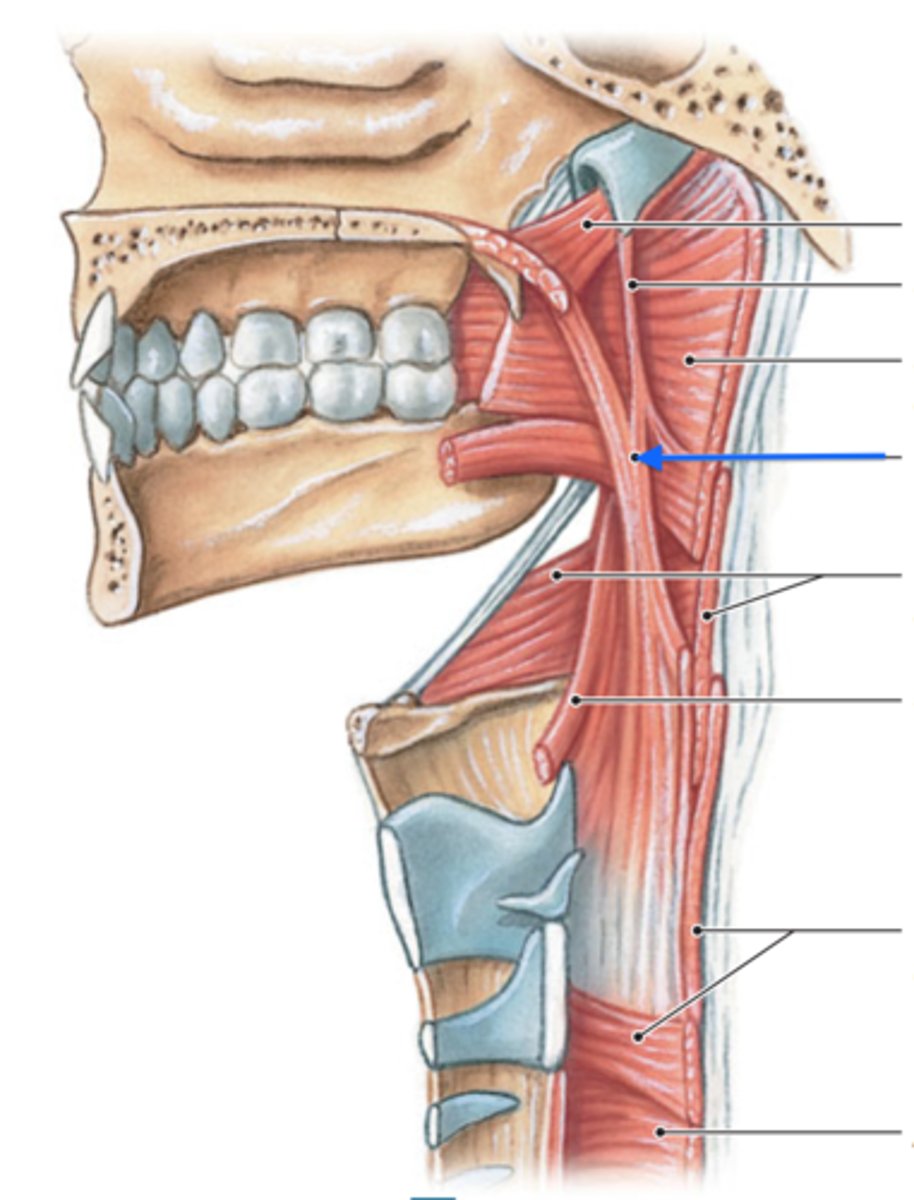
Salpingopharyngeus
- originates from the pharyngotympanic tube and terminates by blending with the palatopharyngeus muscle
- Function = elevates the pharynx and larynx for swallowing and speaking
- innervated by VAGUS NERVE
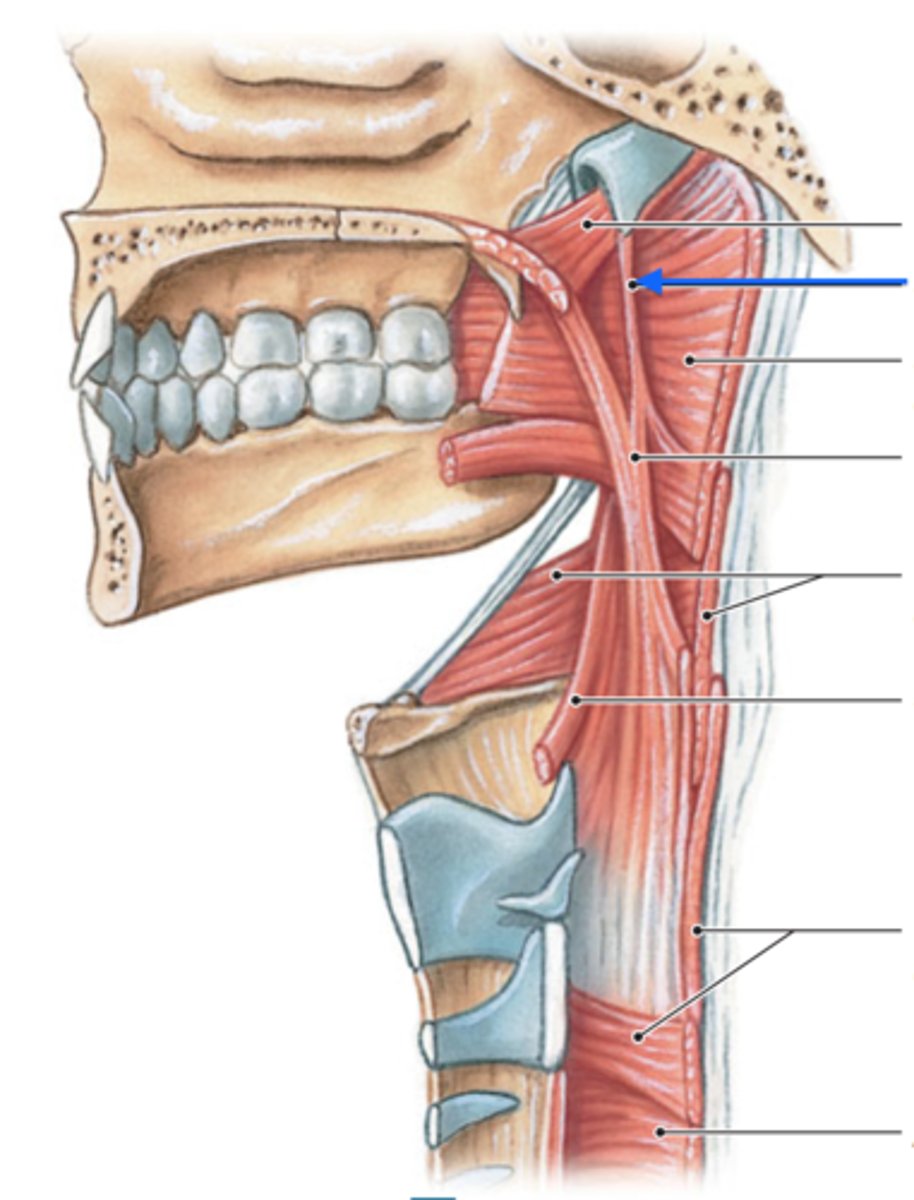
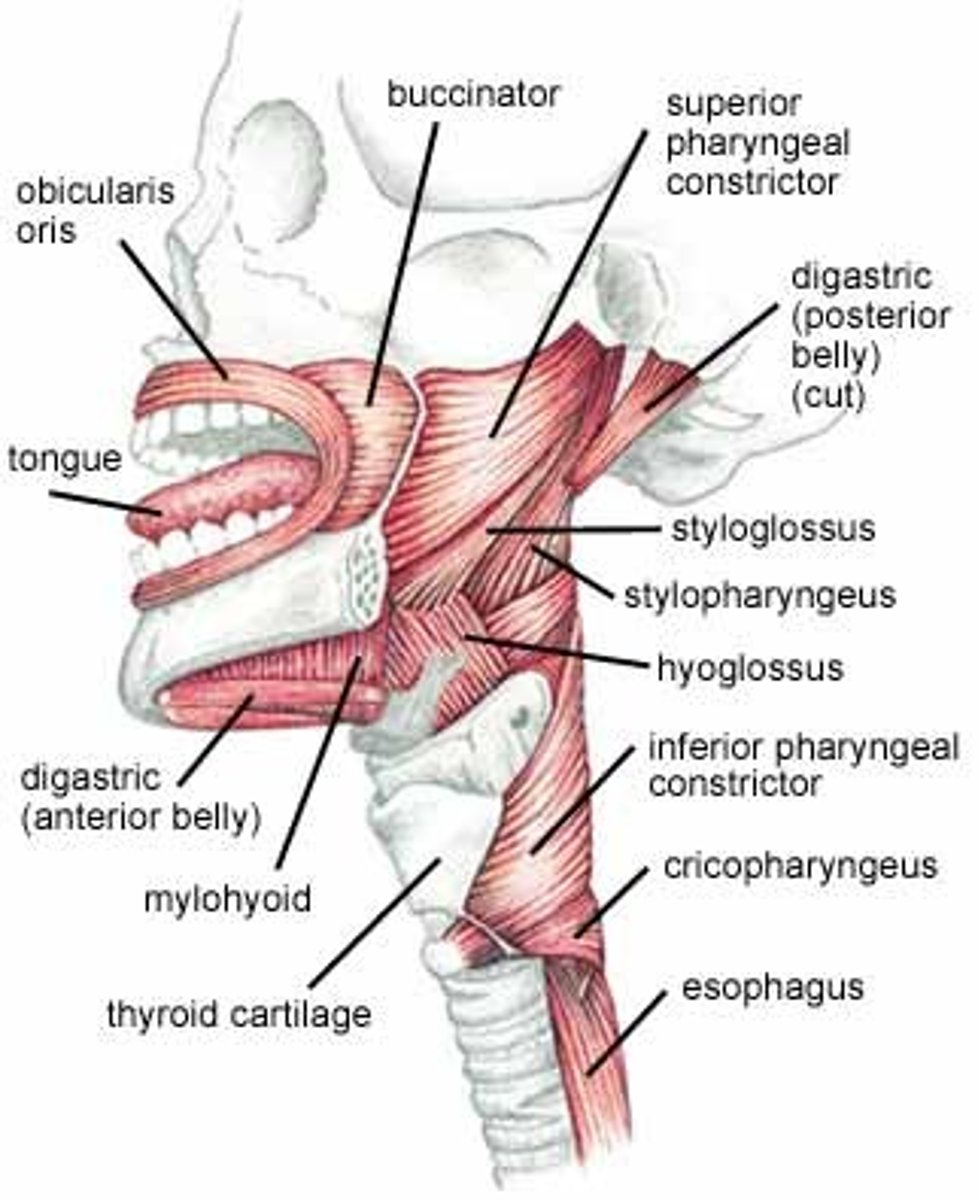
Stylopharyngeus
- originates from the styloid process of the temporal bone and inserts onto the pharynx and thyroid cartilage. it shortens and widens the pharynx during swallowing and speaking
- innervated by CN IX
What enters the gap above the superior constrictor?
1. Pharyngotympanic tube
2. levator veli palatini muscle
What enters the gap above the middle constrictor?
1. stylopharyngeus muscle
2. glossopharyngeal nerve
What enters the gap above the inferior constrictor?
internal laryngeal nerve
What enters the gap below the inferior constrictor?
The recurrent laryngeal nerve
the retropharyngeal Space contains
loose connective tissue separates the buccopharyngeal fascia of the pharynx wall from the pre vertebral fascia that covers the vertebrae and associated muscles.
- this facilitates the mobility of the pharynx necessary for its function; predisposed to abscess formation following pharyngeal infections
Innervation of the pharynx
1. Motor - CN X except the stylopharyngeus which is innervated by CN IX
2. Sensory - nasopharynx by CN V2, oropharynx and hypopharynx by CN IX*
these intermingle to form the pharyngeal plexus
Voluntary Stage of Swallowing
food is chewed and formed into a bolus. contractions of the palatoglossus muscles then squeeze the bolus backwards through the oropharyngeal isthmus into the oropharynx
Involuntary Stage of Swallowing
- nasopharynx separated from the oropharynx by tensor veli palatini muscles
(tensing) or levator veli palatini muscle (raising) on the soft palate, and when the upper fibers of the superior constrictor pull the posterior wall forward.
- Palatopharyngeal arches are pulled into oppostion
- the larynx and laryngopharynx are elevated toward the epiglottis and the laryngeal opening is narrowed.
- the bolus moves around the epiglottis and the laryngeal opening to the lower part of the pharynx by gravity and successive contractions the superior, middle, and inferior pharyngeal constrictor muscles
- the cricopharyngeal sphincter relaxes and the bolus enters the esophagus.
- peristaltic contractions push the bolus into the stomach
Bell's Palsy
damage to CN VII within the facial canal of the temporal one; causes weakness or paralysis of the muscles of facial expression on the ipsilateral side
Parotid Gland
1. secretes serous fluid containing alpha-amylase, lysozyme, IgA
2. inflammation causes mumps
3. branches of facial nerve emerge from the gland
4. the duct crosses the master muscle, and pierces the buccinator muscle, and empties into the oral cavity
Masseter Muscle
Origin: zygomatic arch
Insertion: mandible, lateral surface of the angle and lower ramus
Innervation: CN V3
Action: elevates the mandible, and allows forceful closure of the mouth, muscle of mastication
Blood Supply of the face:
mainly from branches of the facial artery and superficial temporal branches of the external carotid artery
Primary Functions of the Larynx
1. as a sphincter at the air inlet passage
2. maintain the potency of the airway
3. In voice production
--> posteriorly to the bodies of the vertebrae C3-C6 and lateral to the carotid sheath
thyrohyoid membrane
suspends larynx from hyoid bone, pierced by superior laryngeal artery and vein, and the internal laryngeal nerve
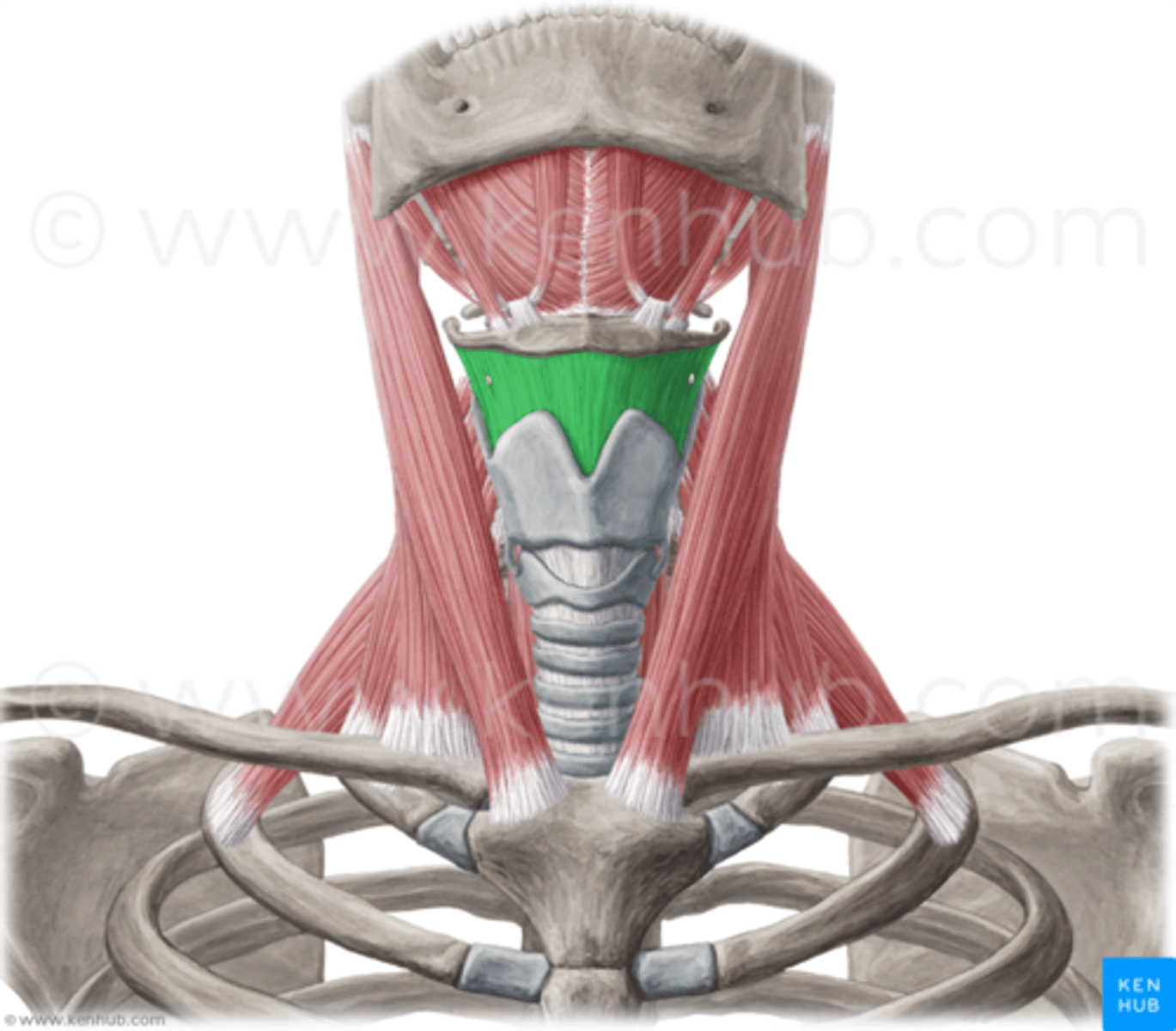
What is the laryngeal inlet bounded by
in front by the epiglottis, laterally by the aryepiglottic folds, and posteriorly by the mucosa between the arytenoids (the oblique arytenoid muscle)
The laryngeal Cavity
1. vestibule - from inlet to vestibular folds
2. ventricles - between the vestibular and vocal folds
3. infraglottic cavity - from vocal ligaments to the lower border of the cricoid cartilage
The vocal folds
vibrate to produce sound. their free margins are anterior to posterior. the laryngeal muscles adjust the tension and degree of approx. of the focal folds.
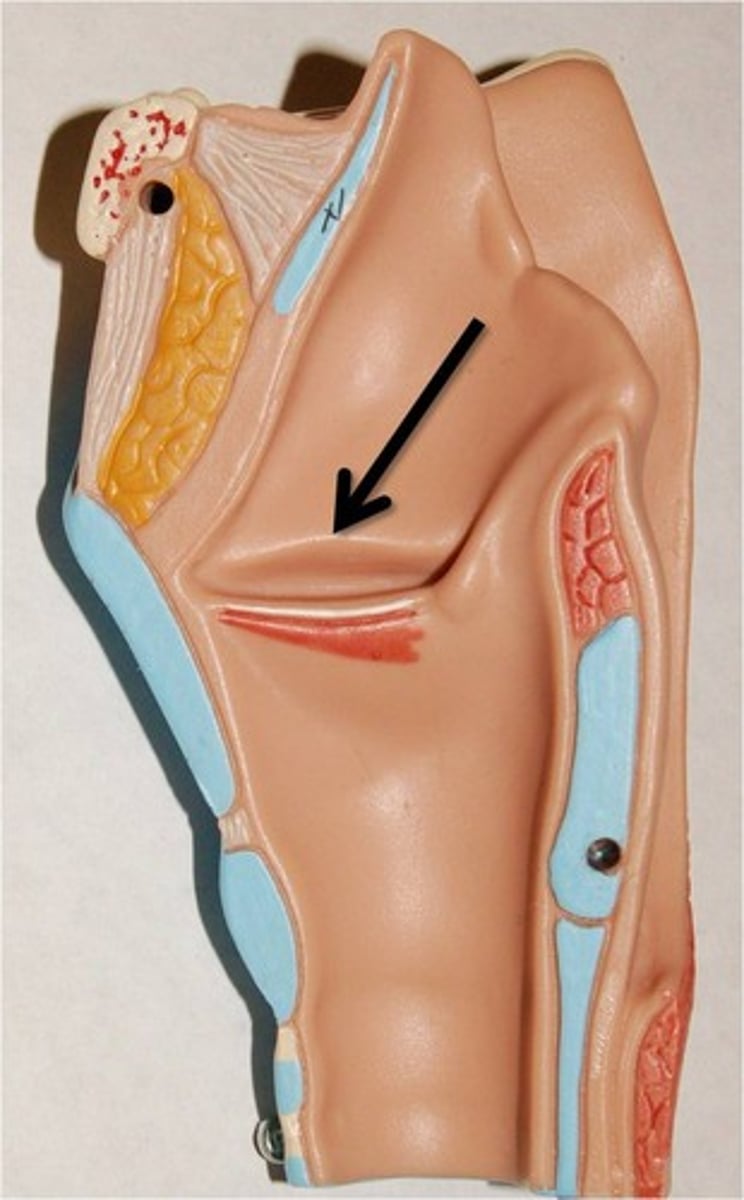
the rima glottidis is
the opening between the vocal folds
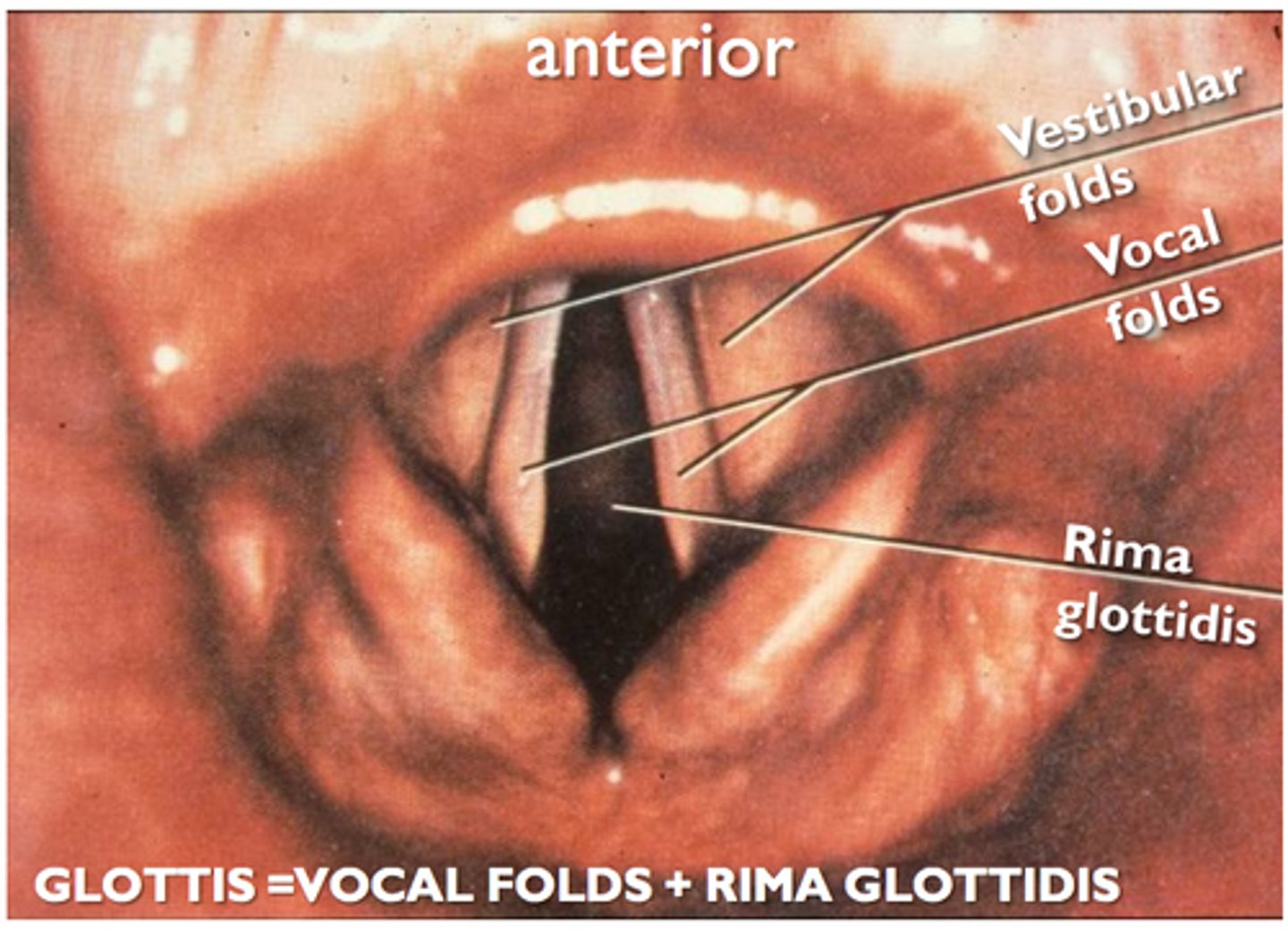
the glottis is
the rims glottides and the vocal folds
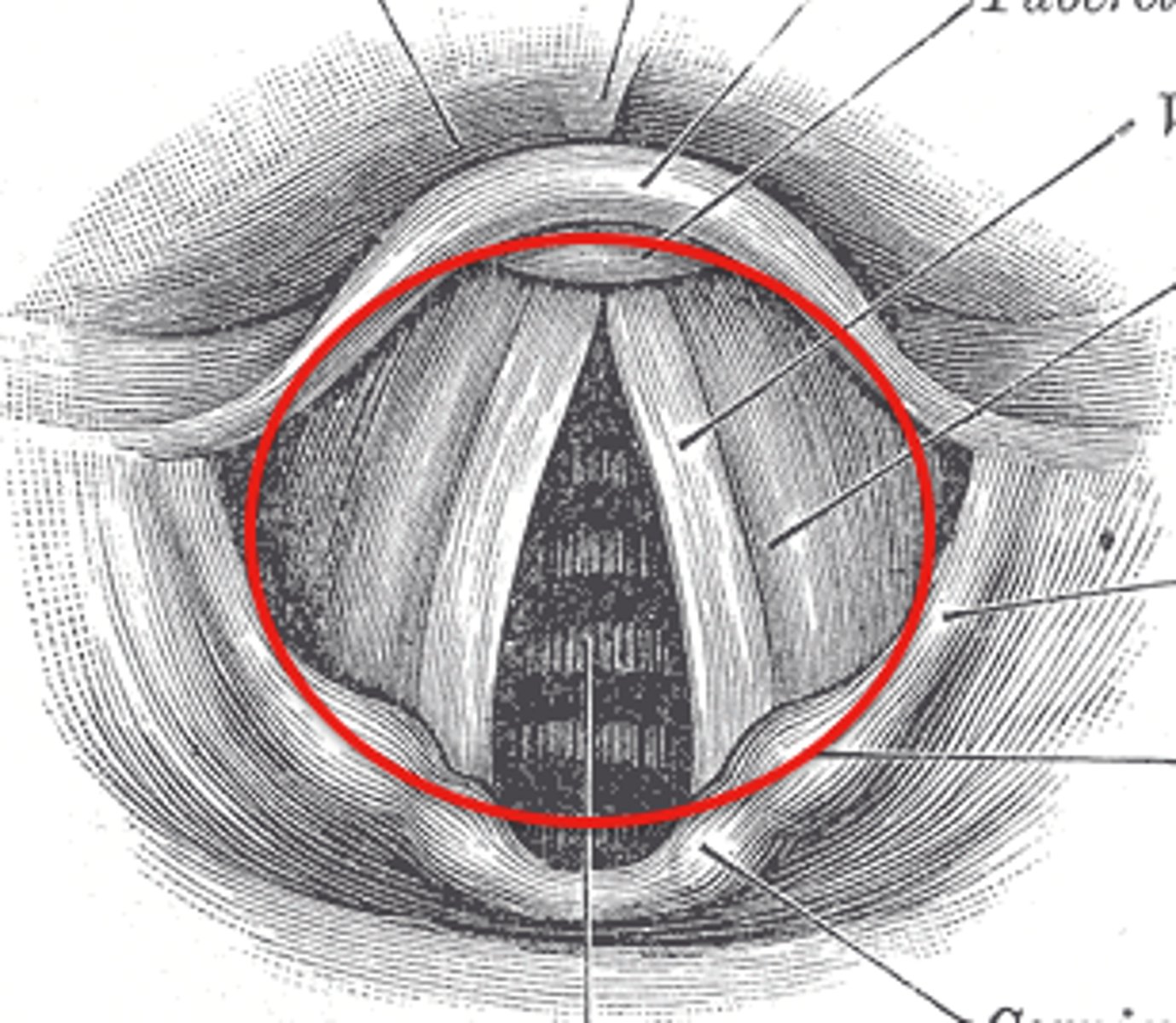
the vestibular folds
provide protection to the glottis and the infraglottic cavity
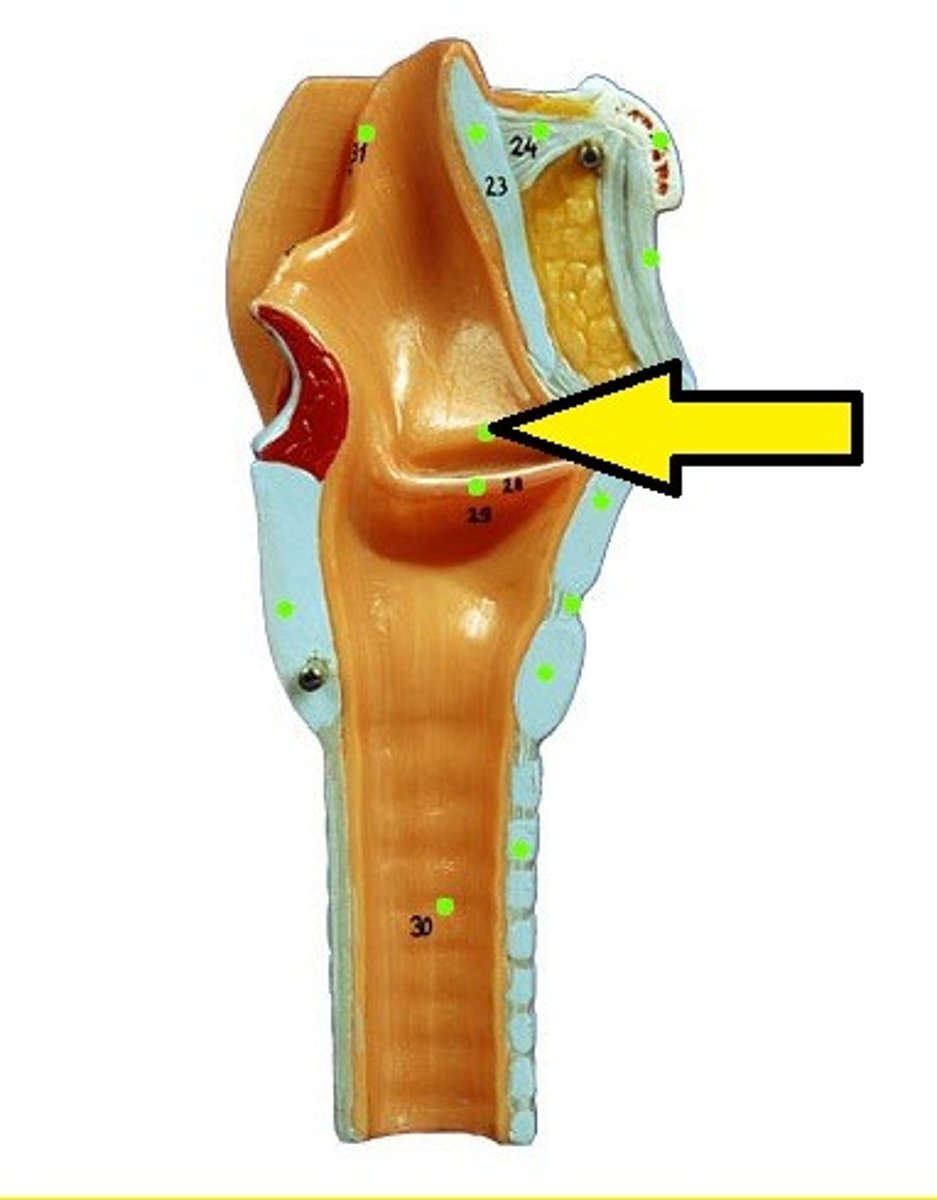
Oblique Arytenoid
Origin: muscular process of arytenoid
Insertion: apex of opposite arytenoid, then continues into aryepiglottic folds as the aryepiglottic muscles
Innervation: Recurrent laryngeal nerve
Action: adducts arytenoid cartilages to close the posterior part of the rima glottidis
laryngeal sphincter
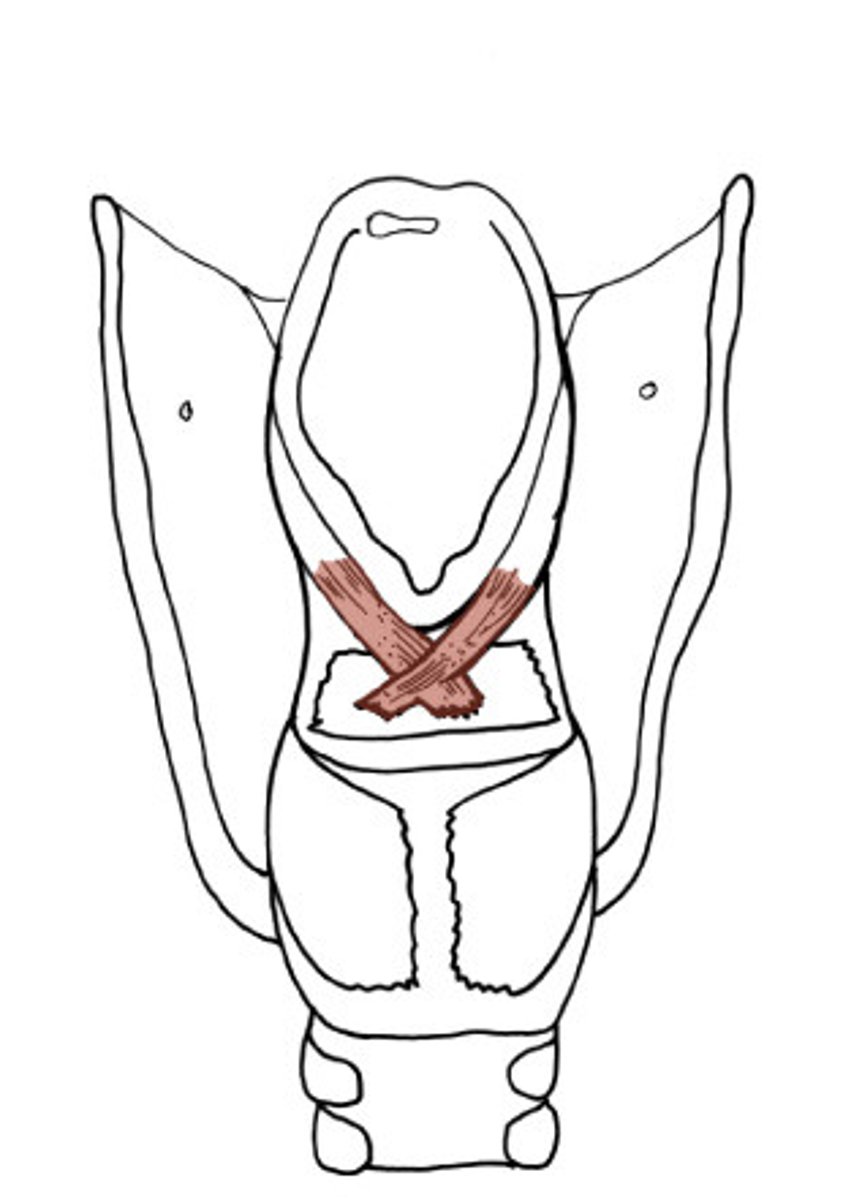
Transverse Arytenoid
Origin: back and medial surface of arytenoid
Insertion: back and medial side opposite of arytenoid
Innervation: Recurrent laryngeal nerve
Action: adducts arytenoid cartilages to close the posterior part of the rim glottidis
laryngeal sphincter
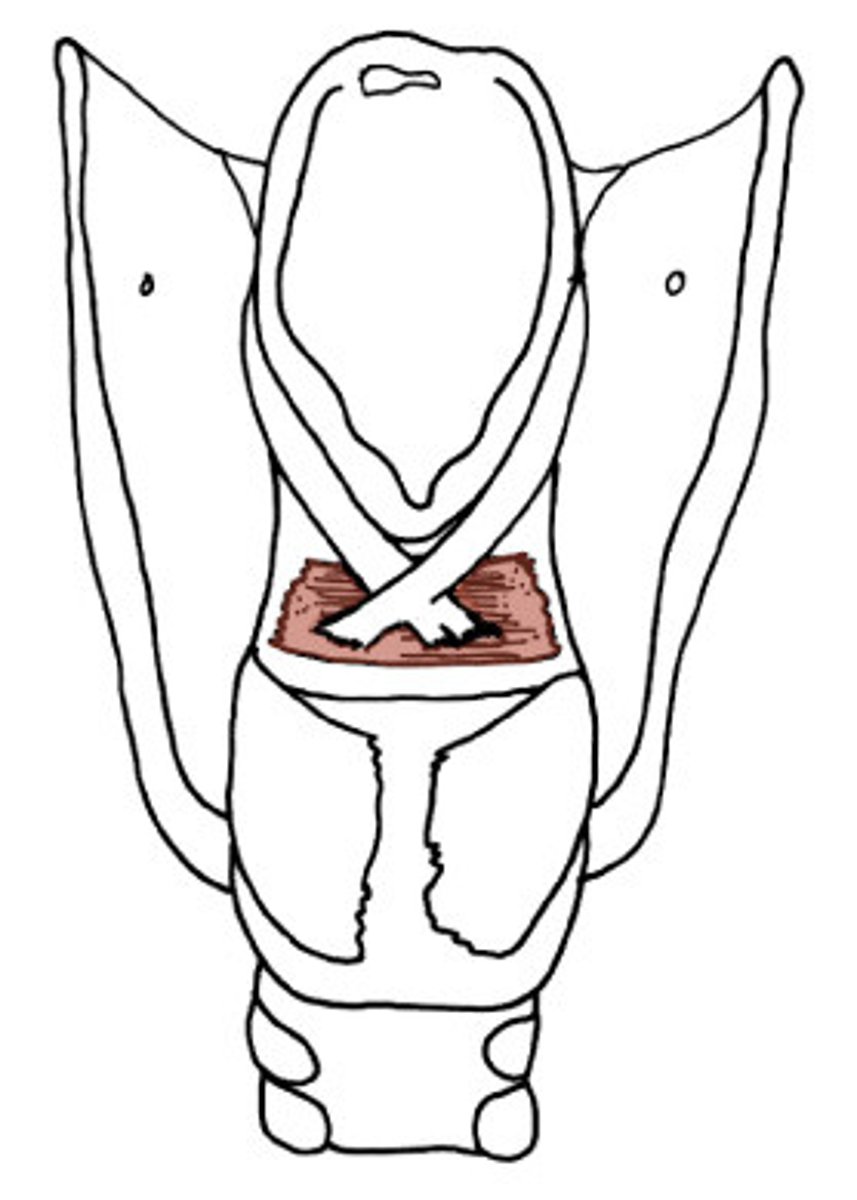
Lateral Cricoarytenoid
origin: lateral part of cricoid arch
insertion: back to muscular process of arytenoids
action: adducts vocal folds
innervation recurrent laryngeal
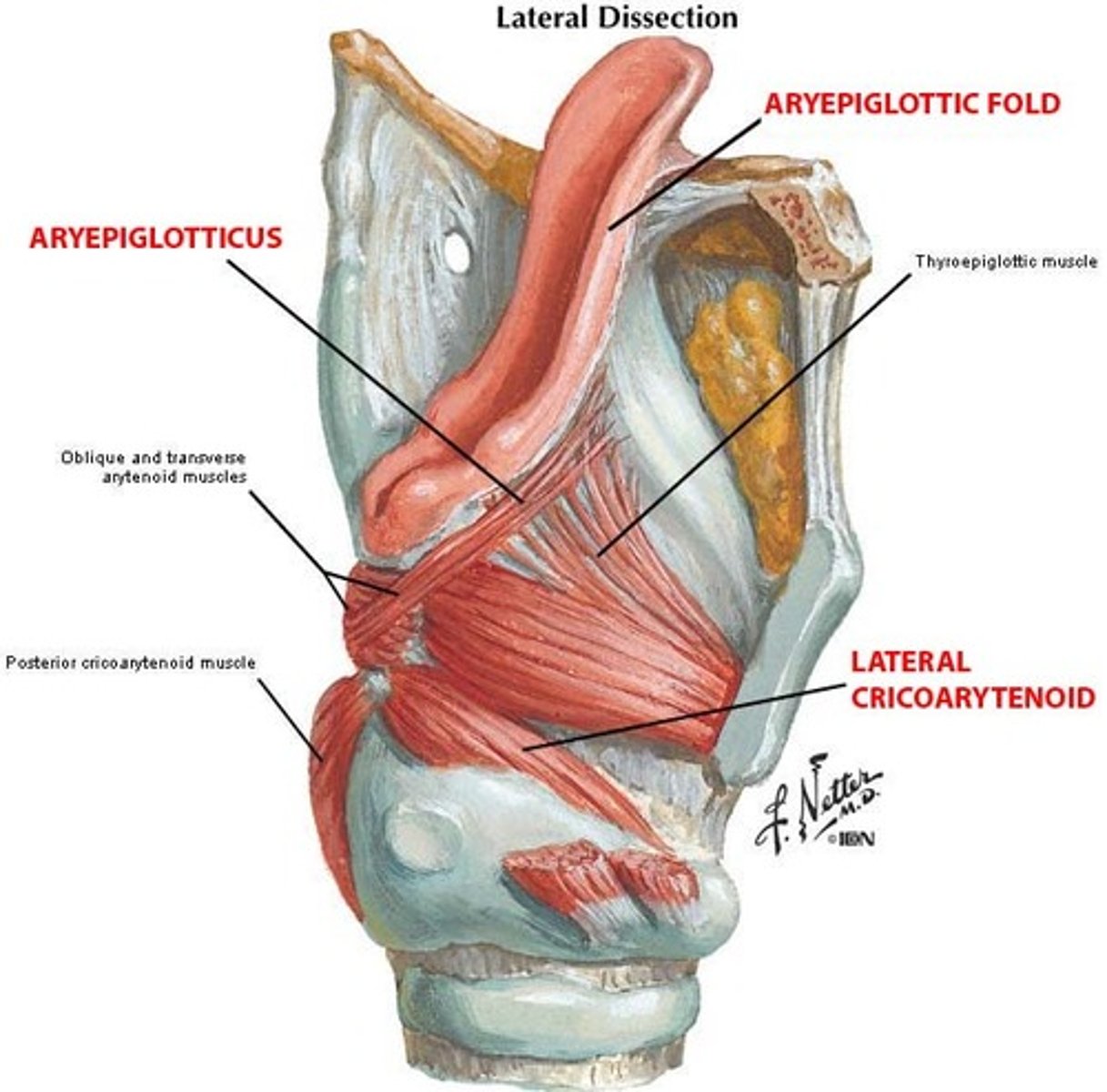
Posterior Cricoarytenoid
origin: back of cricoid lamina
insertion: laterally, to the muscular process of the arytenoid
action: ABDUCTS vocal fold and arytenoid cartilage
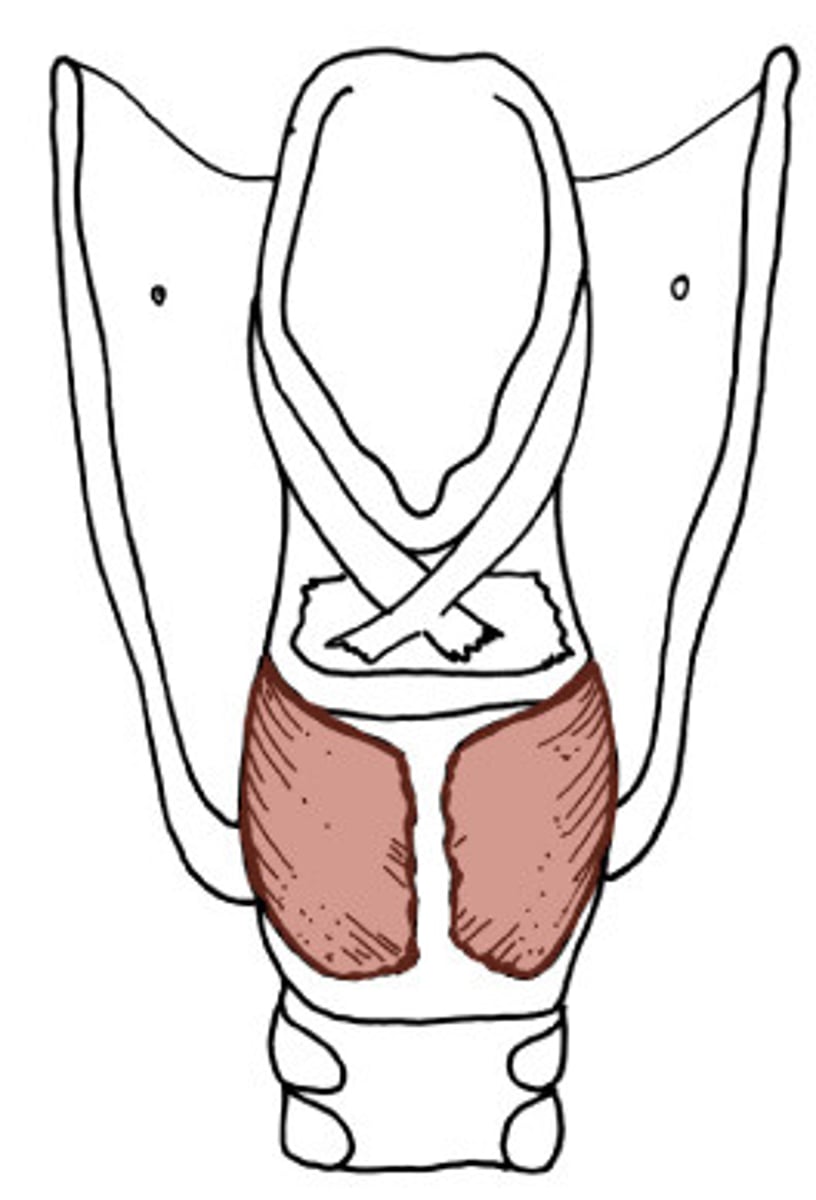
Cricothyroid
origin: side of cricoid arch
insertion: back to lamina and inferior horn of thyroid cartilage
action: pulls thyroid cartilage forward and tilts cricoid lamina posteriorly, stretching the vocal ligament to raise the pitch of the voice
INNERVATED by: external laryngeal nerve
Thyroarytenoid
origin: side of cricoid arch
insertion: anterior surface and vocal process of arytenoid
action: stiffens the vocal ligament via isometric contraction. Fibers parallel to the vocal ligament are known as vocals muscle, which makes minute adjustments in tension during speech
INNERVATION of the Larynx
1. Motor: all intrinsic muscles (oblique arytenoid, transverse arytenoid, lateral cricoarytenoid, posterior cricoarytenoid, and thyroarytenoid) except cricothyroid are innervated by the recurrent laryngeal nerve. The cricothyroid is innervated by the EXTERNAL LARYNGEAL NERVE
1. Sensory: the mucosa from the vocal folds upward is by the internal laryngeal nerve and the mucosa below the vocal folds is innervated by the recurrent laryngeal nerve.
Blood Supply of the Larynx
1. Superior laryngeal artery - from the superior thyroid artery
2. Inferior laryngeal artery - from the inferior thyroid artery
Functions of the Larynx
1. Swallowing
2. Coughing, sneezing
3. Micturition, defection, parturition
4. voice production
Swallowing
larynx is elevated by the supra hyoid muscles and the other elevators. The inlet is narrowed by the oblique arytenoid and aryepiglottic muscles. food passes laterally down the piriform recesses into the esophagus
Coughing and Sneezing
the rims glottides is closed by the sphincters after a deep breath. The expiratory muscles are contracted to increase intrathoracic pressure, then the rim glottides is opened rapidly.
Micturition, Defecation, parturition
the rims glottidis is closed after a deep breath. due to air trapped in lungs, the diaphragm cannot move upwards when the abdominal muscles are contracted, so pressure is transmitted to the pelvis and abdomen
Voice Production
vocal ligaments adducted. Expired air vibrates the vocal ligaments with a frequency depending on length and tension. the quality of the voice depends on resonation by the pharynx, mouth, and paranasal sinuses. for high tones, the entire larynx is elevated; for low tones, it is depressed.
External Fibrous Layer of Eye
a supporting layer, consisting of sclera posteriorly and cornea anteriorly. The cornea is avascular but innervated with sensory nerves from CN V1.
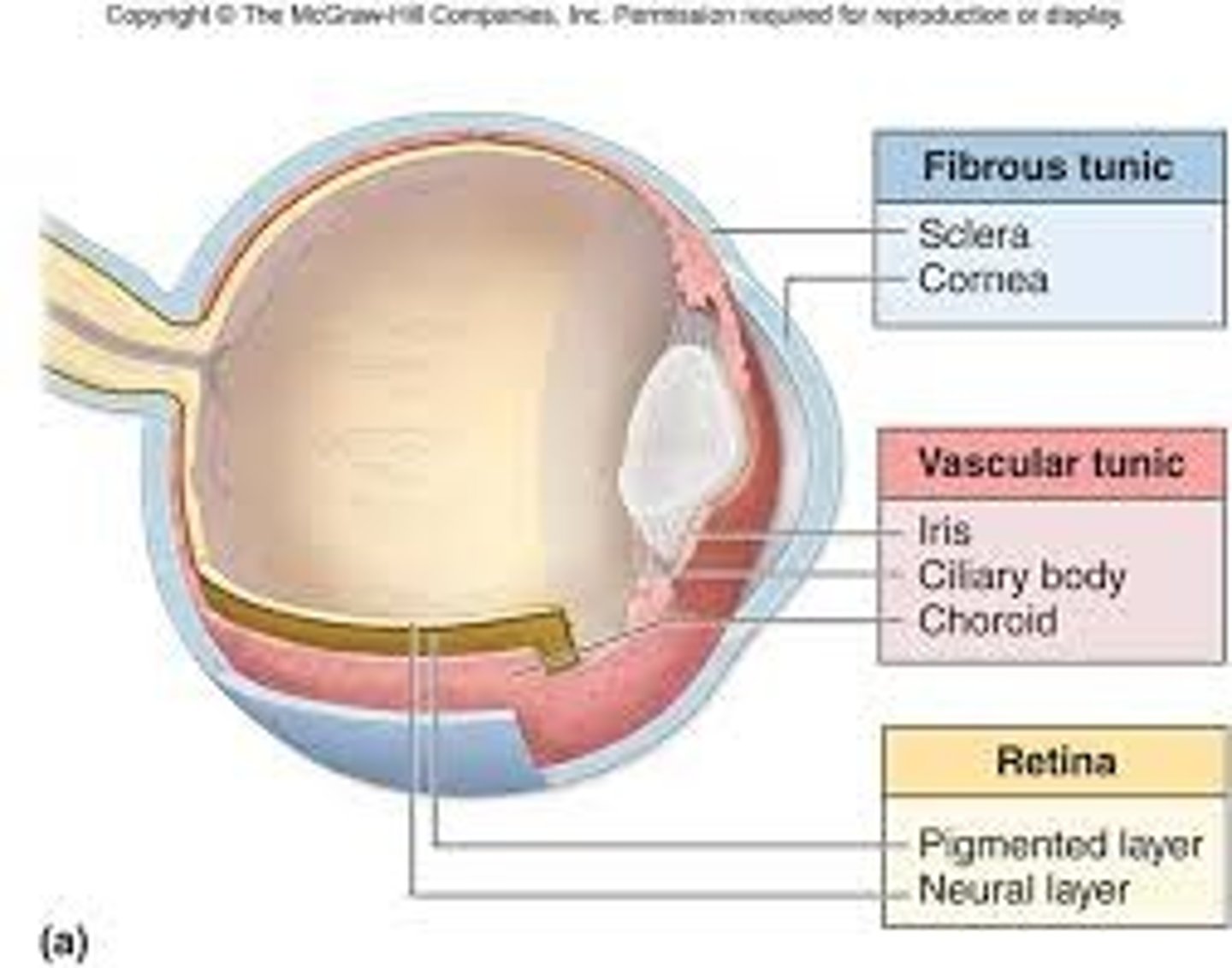
Middle Vascular Layer
from posterior to anterior, consists of choroid, ciliary body, and iris
Choroid
Ciliary Bodybetween sclera and retina; highly vascularized to supply retina
Ciliary Body
- divides the posterior and anterior compartments. Structure that encircles the eye opening posterior to the iris
- secretes aqueous humor into posterior chamber of the eye.
- connects the iris, suspensory ligaments, and ora serrata and includes muscles that draws it closer to the lens
- innervated by parasympathetic fibers of CN III

How does the ciliary body increase its focus on nearby objects?
since the lens is suspended from the ciliary body by suspensory ligaments, this action relaxes the suspensory ligaments, allowing the natural elasticity of the lens to become more convex, allowing an increase in focusing ability for near objects
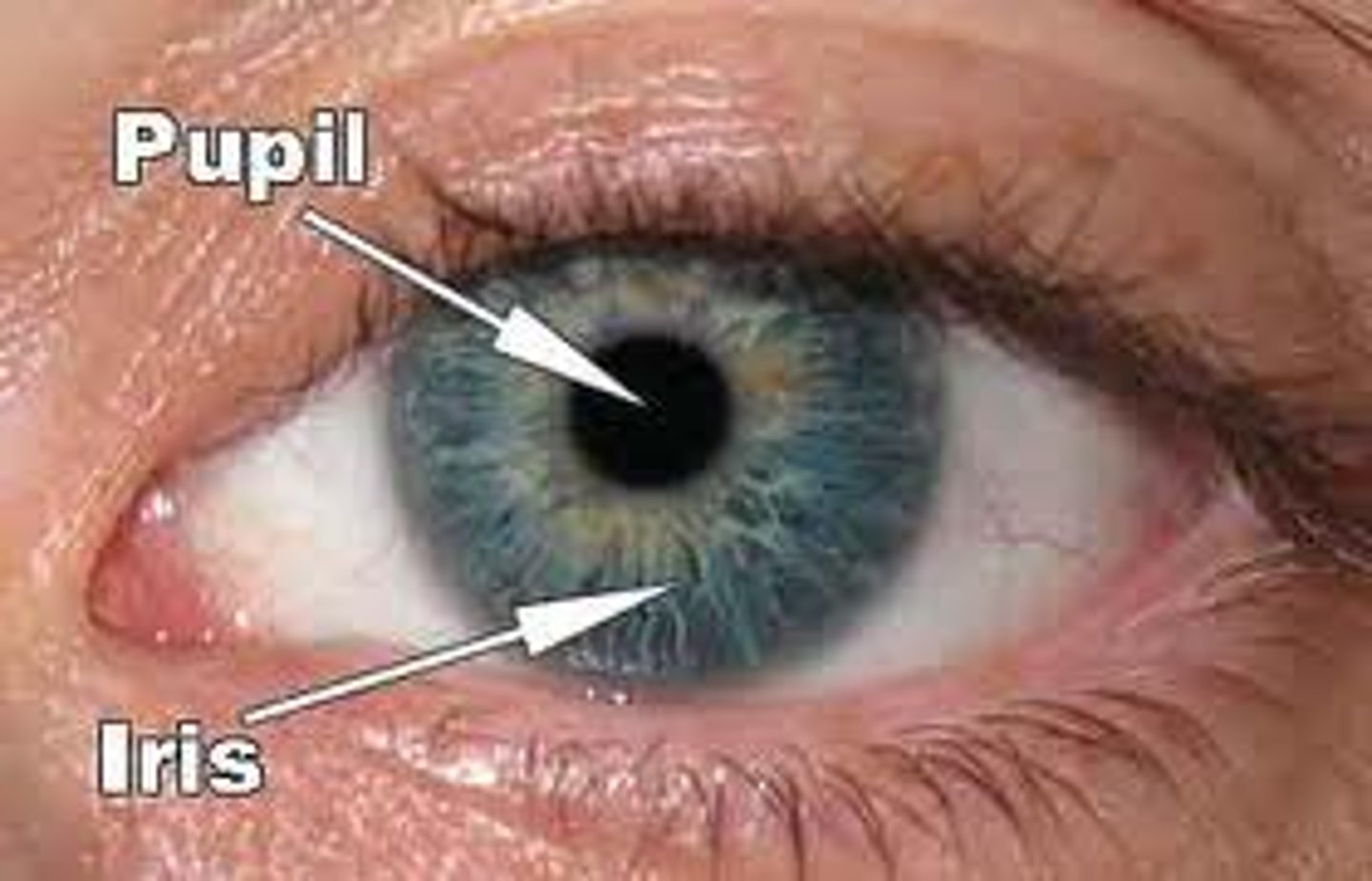
Iris
pigmented diaphragm that regulates the size of the pupil to control the amount of light entering the eye
- the dilator pupillae dilates the pupil and is innervated by sympathetic nerve fibers from the superior cervical ganglion.
- the sphincter pupillae constricts the pupil and are unnerved by parasympathetic fibers of CN III
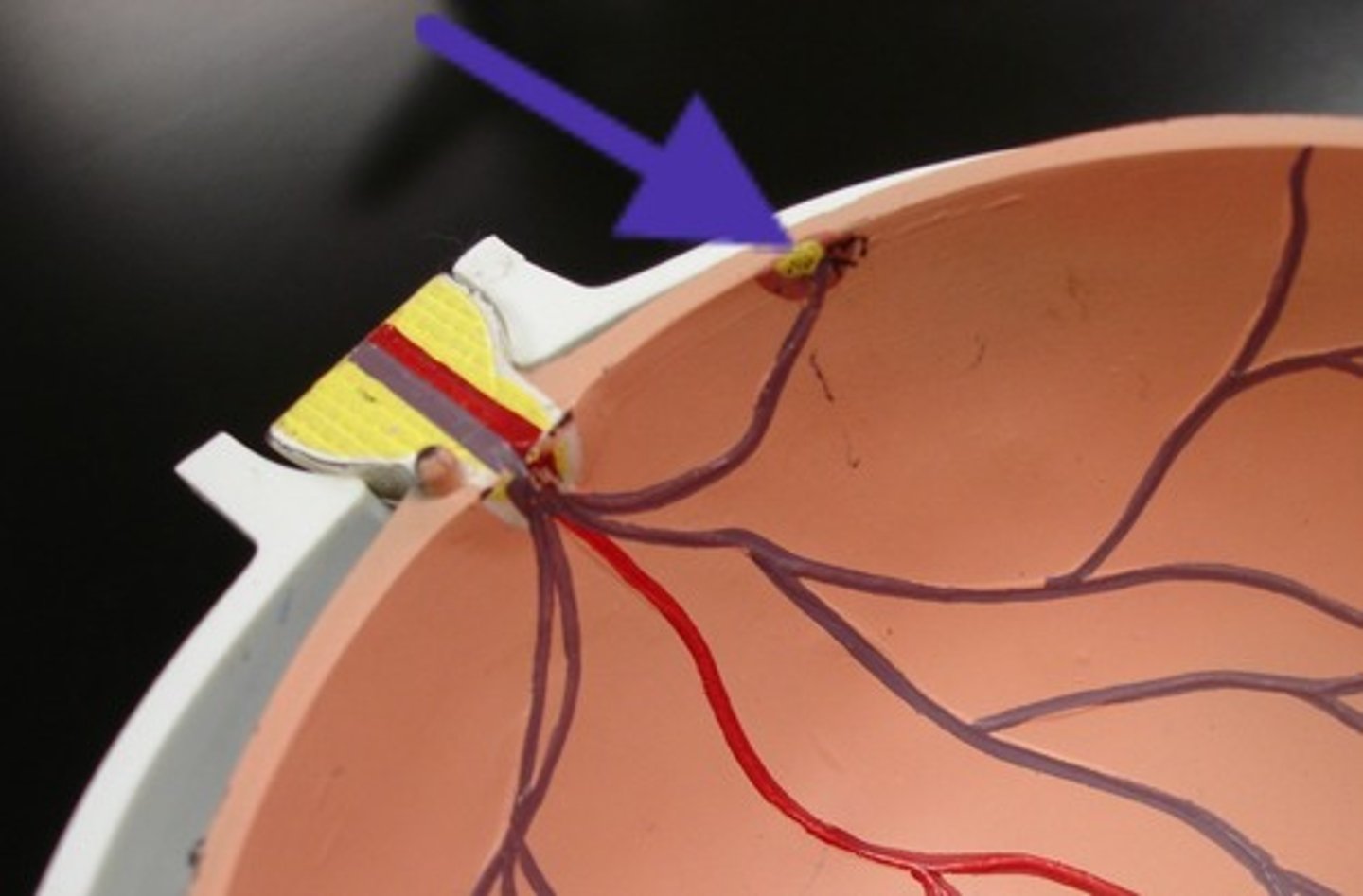
Optic Disc
a circular region medial to the posterior pole of the retina, where the optic nerve leaves the eyeball
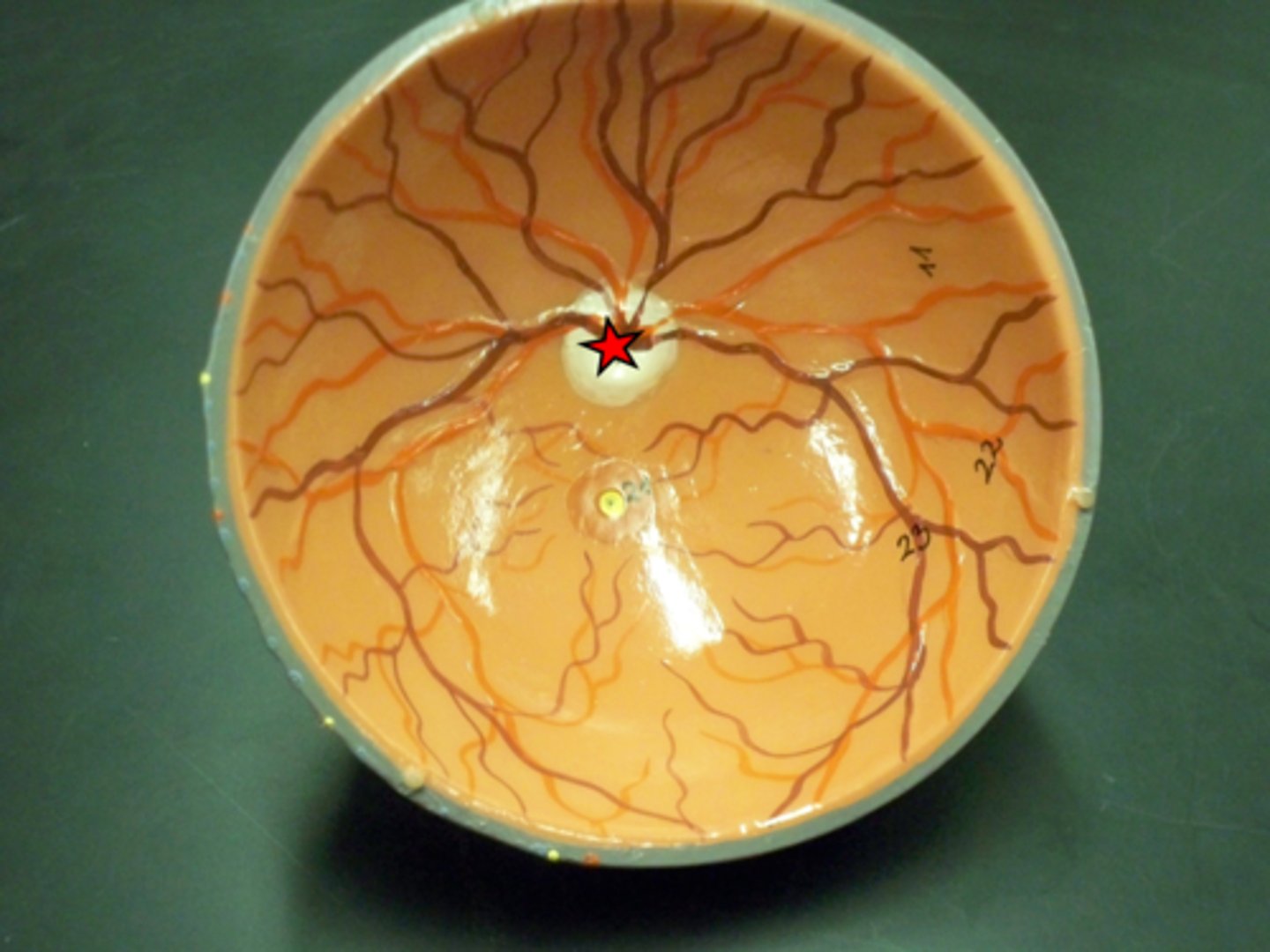
Macula Lutea
just lateral to optic disc; the small yellowish area of the retina near the optic disk that provides central vision
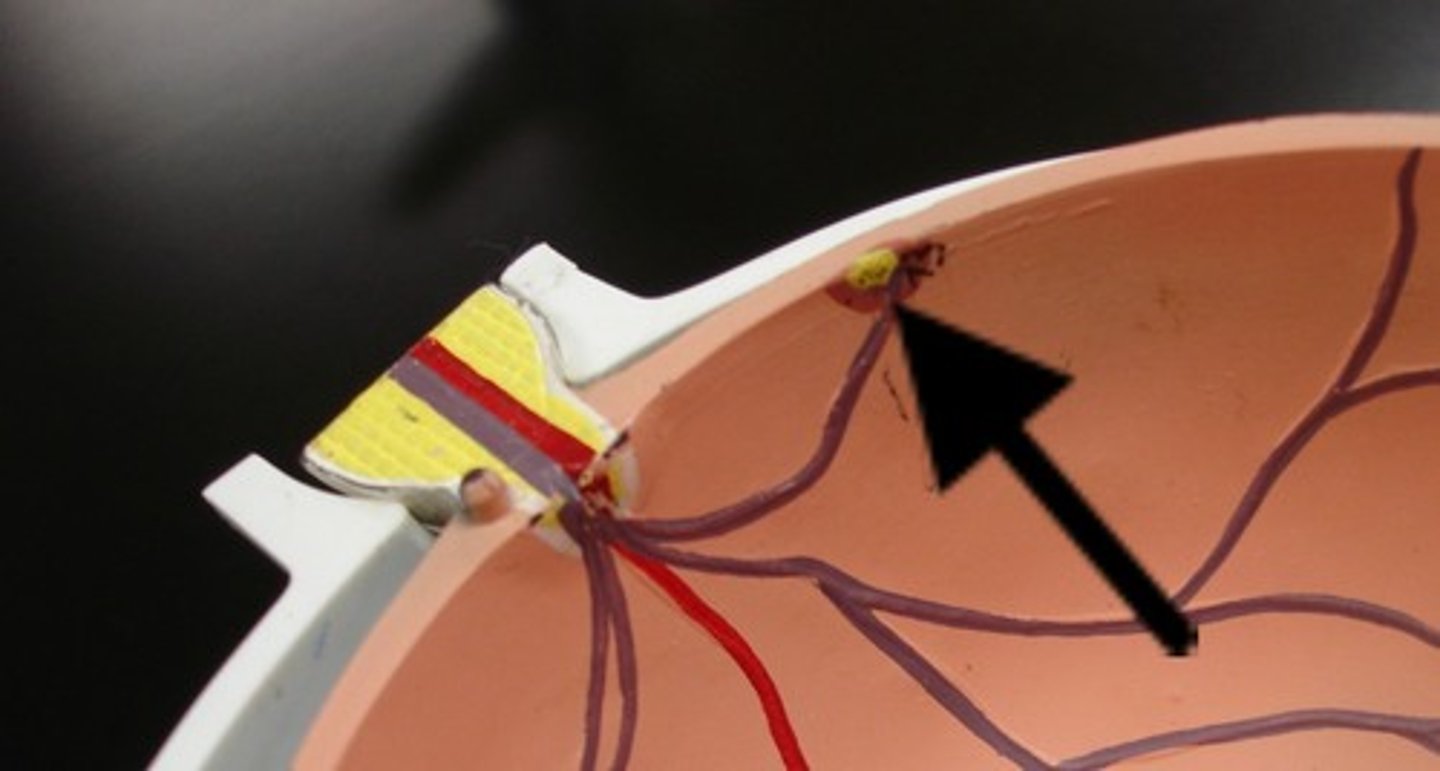
Fovea Centralis
central depressed part of macula lute; the area of highest visual acuity
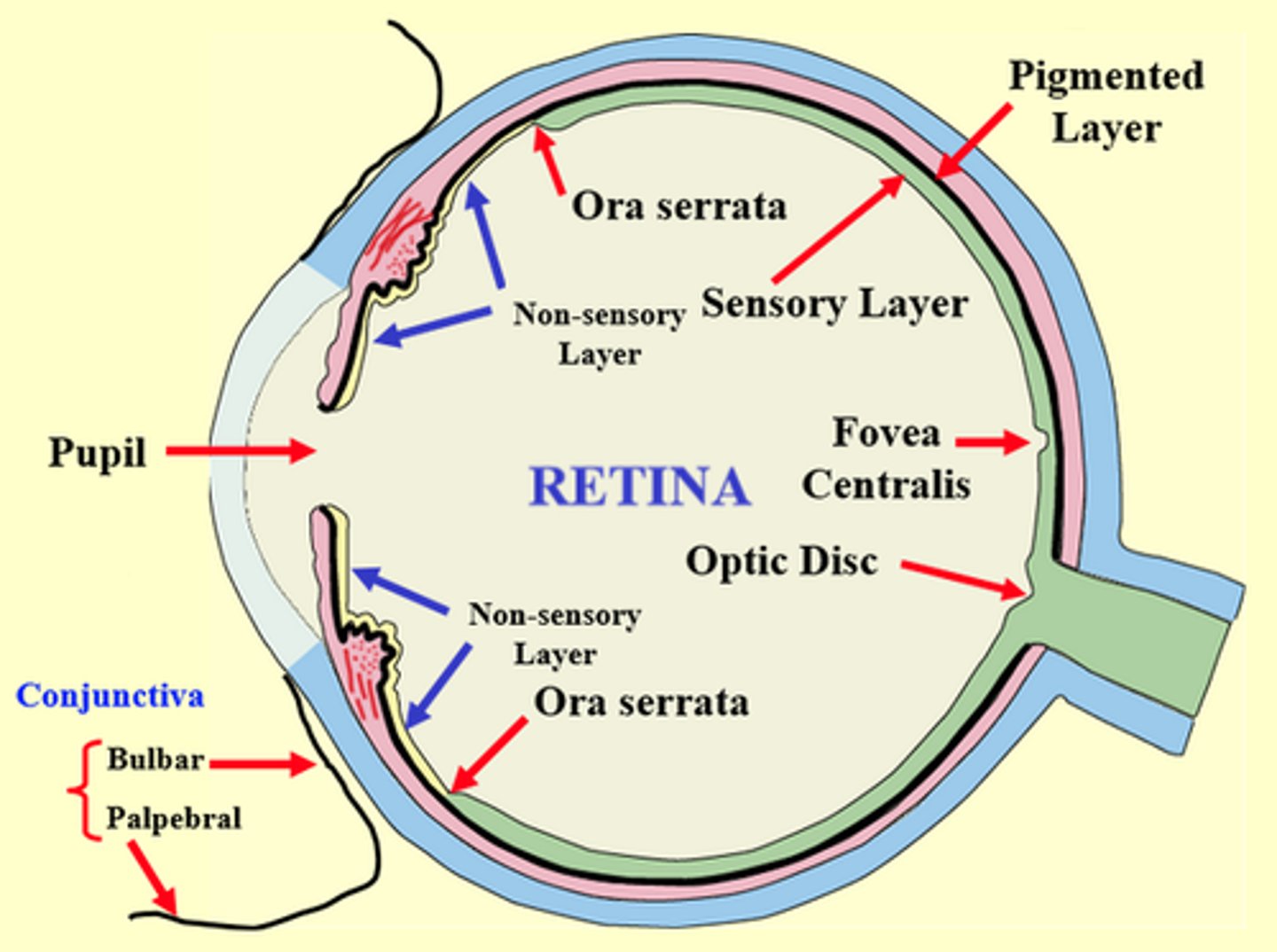
Ciliary and Iridial Retina
continuations of the the outer pigment cell layer of the retina over the inner surface of the ciliary body and iris; not light sensitive.
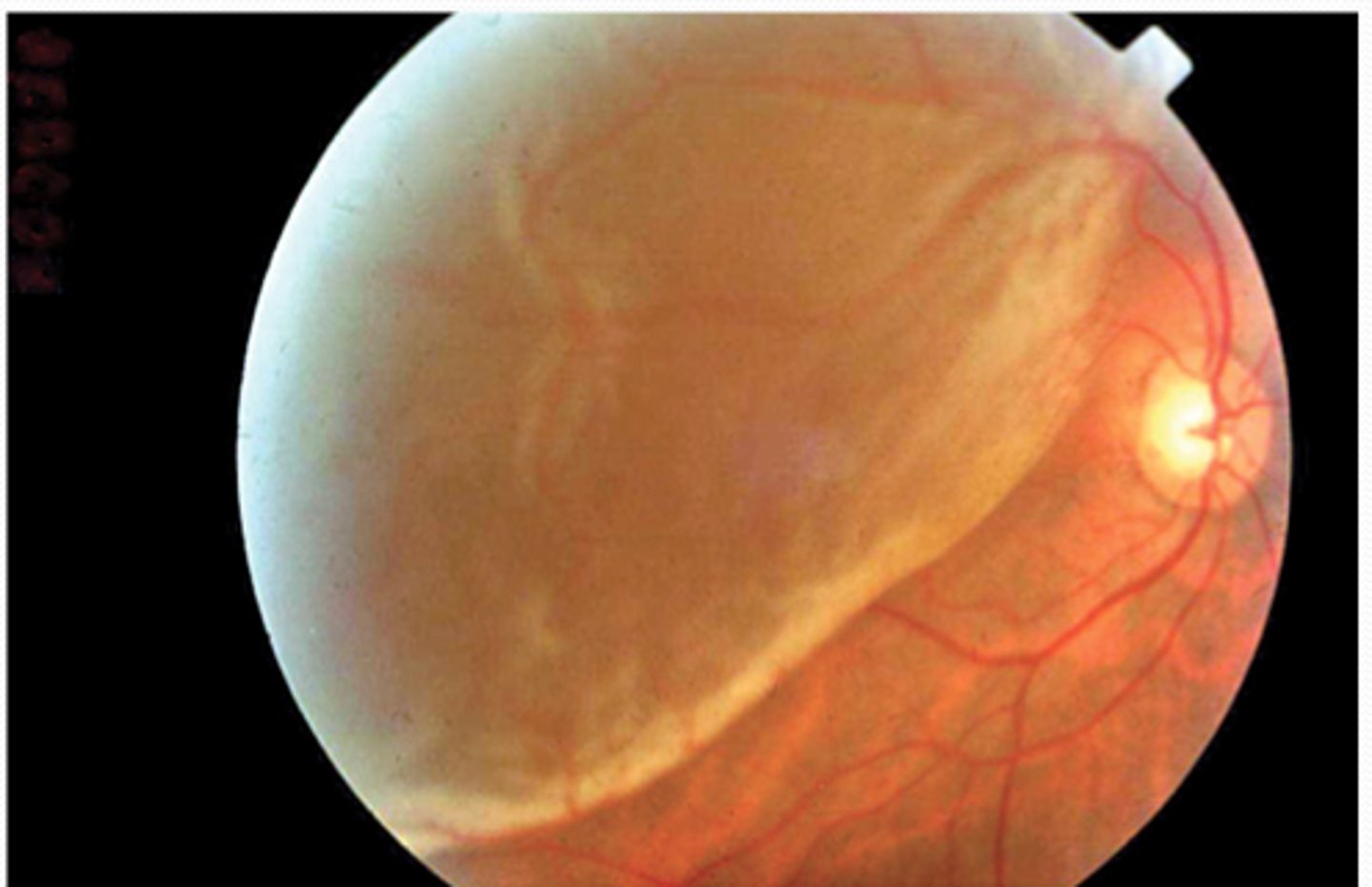
Retinal Detachment
separation between the pigment epithelium and the neural layers of the neural retina
Aqueous Humor
flows from the posterior chamber to the anterior chamber and is drained into the venous system at the scleral venous sinus (canal of Schlemm) at the iridocorneal angle
Vitreous Body
transparent jelly like filling the space between the lens and the retina, forms the posterior 4/5 of the eyeball
Conjunctiva
thin, vascular, transparent mucous membrane covering the sclera (bulbar) and the inner surfaces of the eyelids (palpebral)
blood supply of the eyeball
1. ophthalmic artery branches, from the internal carotid artery
2. ophthalmic veins which drain into facial vein or into the cavernous vein.
Levator Palpebrae Superioris
innervated by CN III, elevates upper eyelid
Lateral Rectus
abducts eye
Medial rectus
adducts eye
Superior Rectus
elevates/adducts eye
Inferior Retus
depress/adduct eye
Superior Oblique
- inserts posterior to the equator of the eye
- depresses
-abduction
Inferior Oblique
- inserts posterior to the equator of the eye
- elevates
-abduction
All the extra ocular muscles are innervated by CN III except
1. Lateral Rectus - CN VI
2. Superior Oblique - CN IV
What is the buttocks?
the gluteus maximus and the gluteus medius with superficial fascia
Gluteus Maximus
Origin: iliac crest, sacrum, sacrotuberous ligament
Insertion: iliotibial tract, gluteal tuberosity, femoral shaft
Main Action on Thigh: extension, lateral rotation
Innervation: inferior gluteal n.
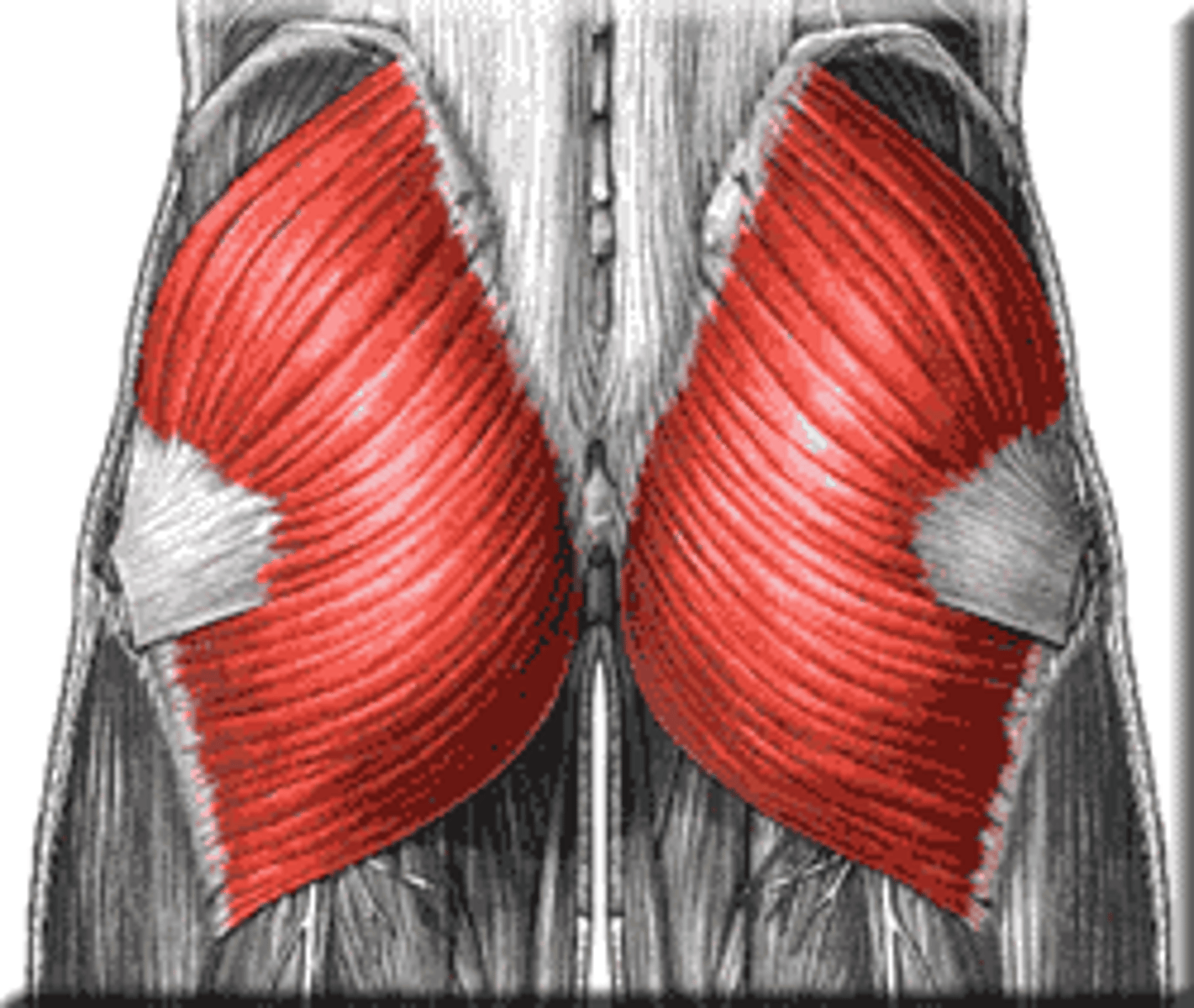
Gluteus Medius
Origin: ilium external surface
Insertion: greater trochanter
Main Action on Thigh: abduction, medial rotation; and prevents pelvic tilt with gait
Innervation: superior gluteal n.
Deep to gluteus maximus
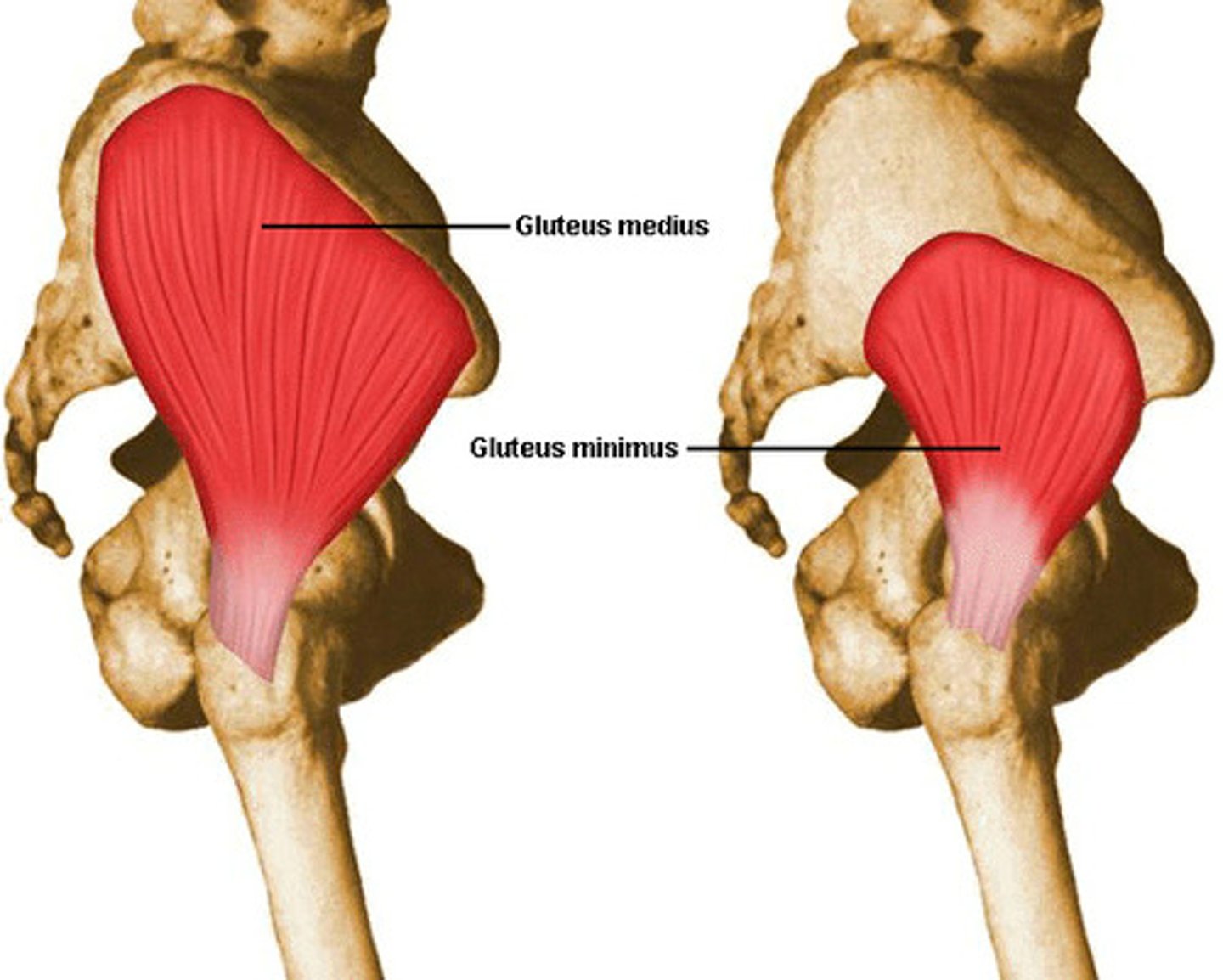
Gluteus Minimus
Origin: ilium external surface
Insertion: greater trochanter
Main Action on Thigh: abduction, medial rotation; and prevents pelvic tilt with gait
Innervation: superior gluteal n.
Deep to gluteus medius
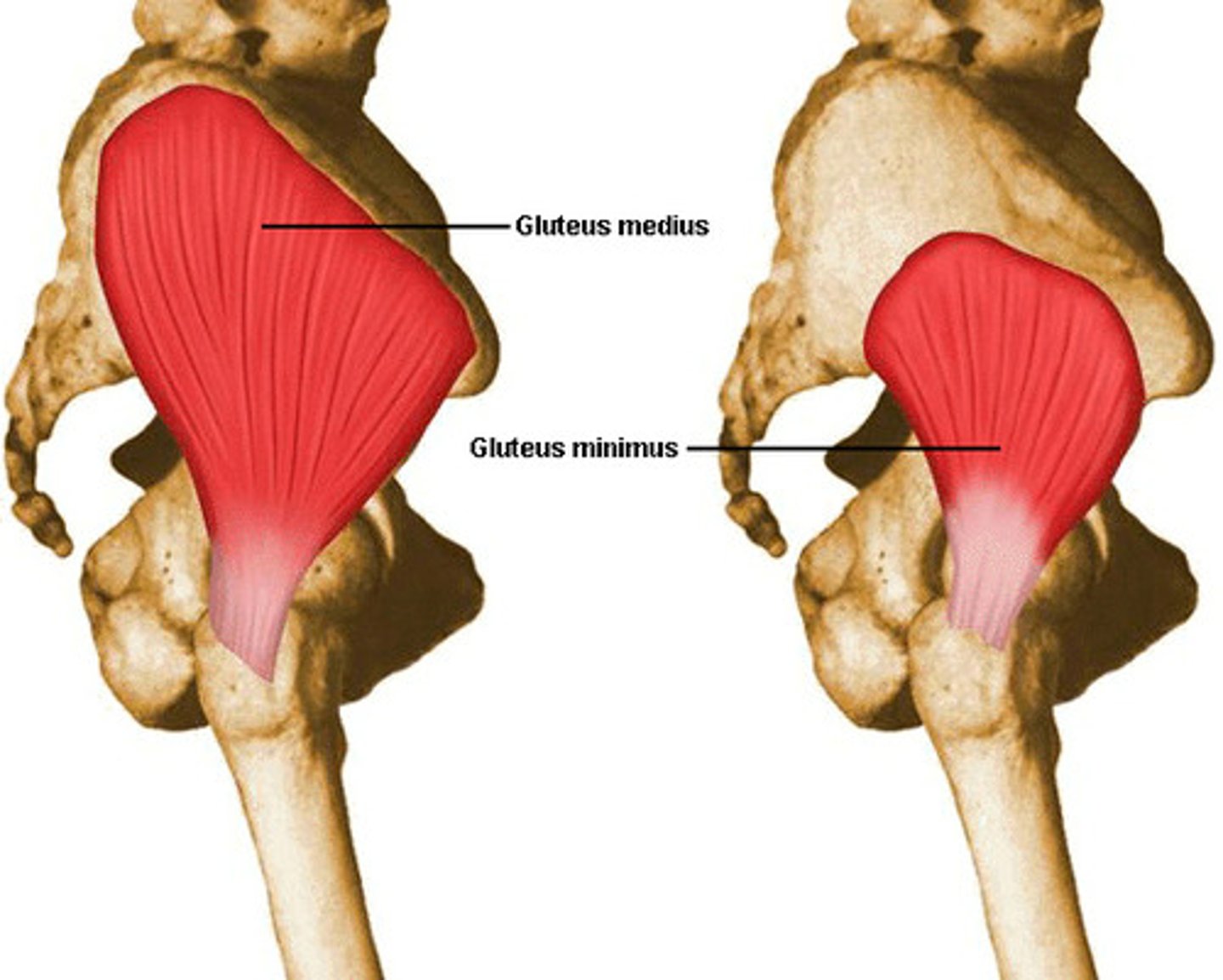
Piriformis
Origin: sacrum, sacrotuberous ligament
Insertion: greater trochanter
Main Action on Thigh: laterally rotates the thigh and stabilizes the femoral head in the acetabulum
Innervation: inferior gluteal n.
More medial to gluteus minimus muscle
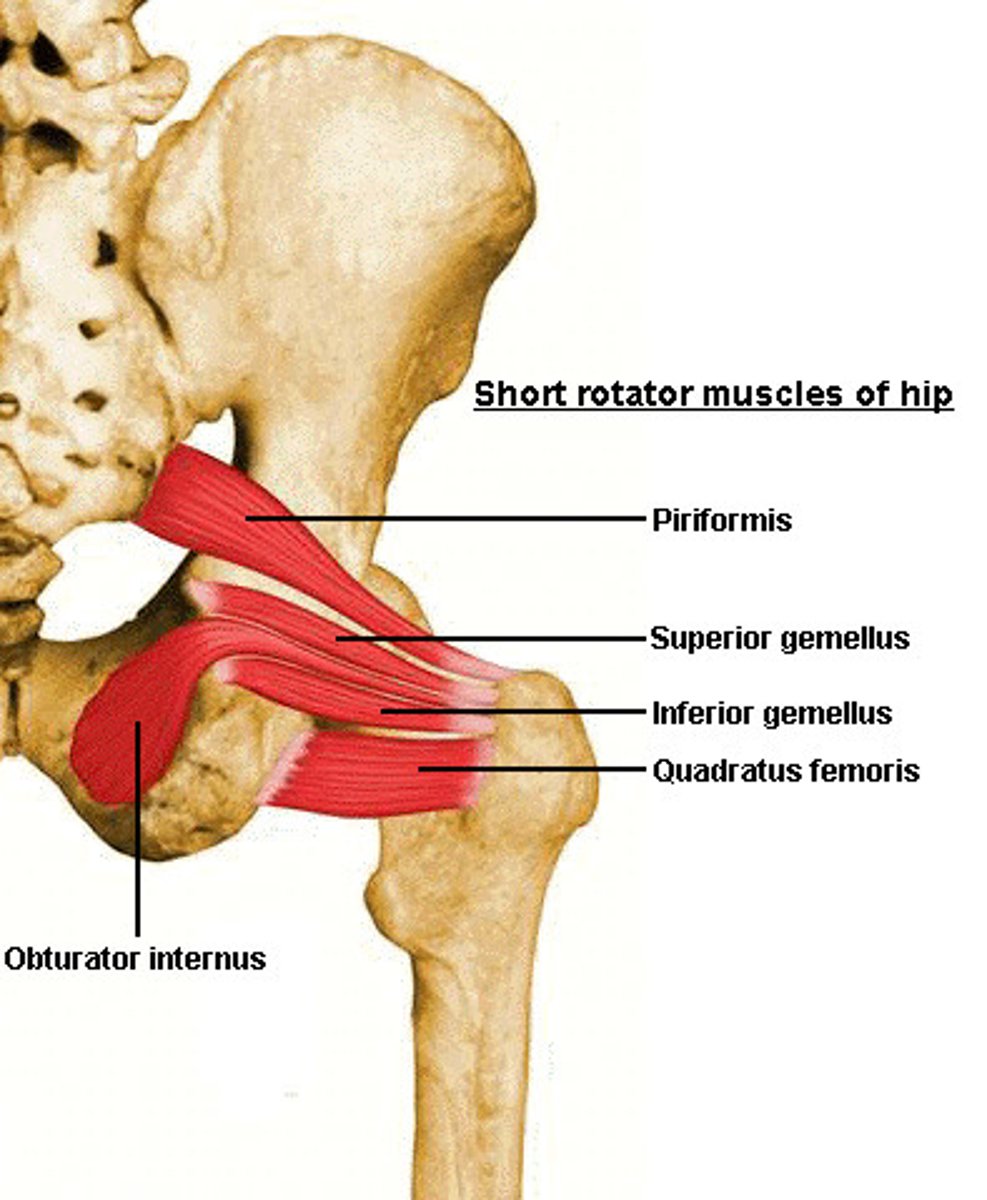
Gemellus Superior
Origin: ischial spine
Insertion: greater trochanter
Main Action: laterally rotate the thigh and stabilize the femoral head in the acetabulum
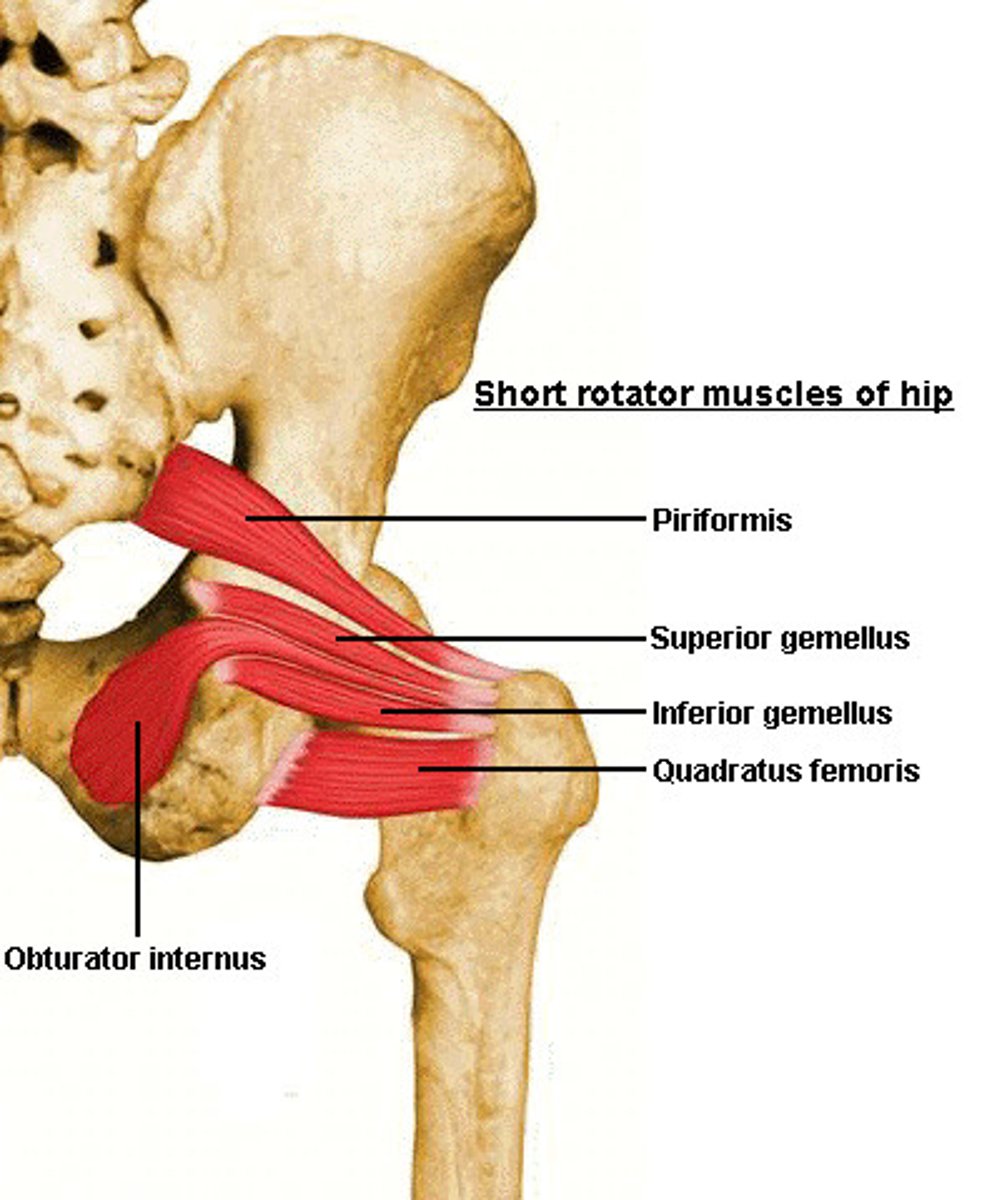
Obturator Internus
Origin: inner surface of obturator foramen
Insertion: greater trochanter
Main Action: laterally rotate the thigh and stabilize the femoral head in the acetabulum
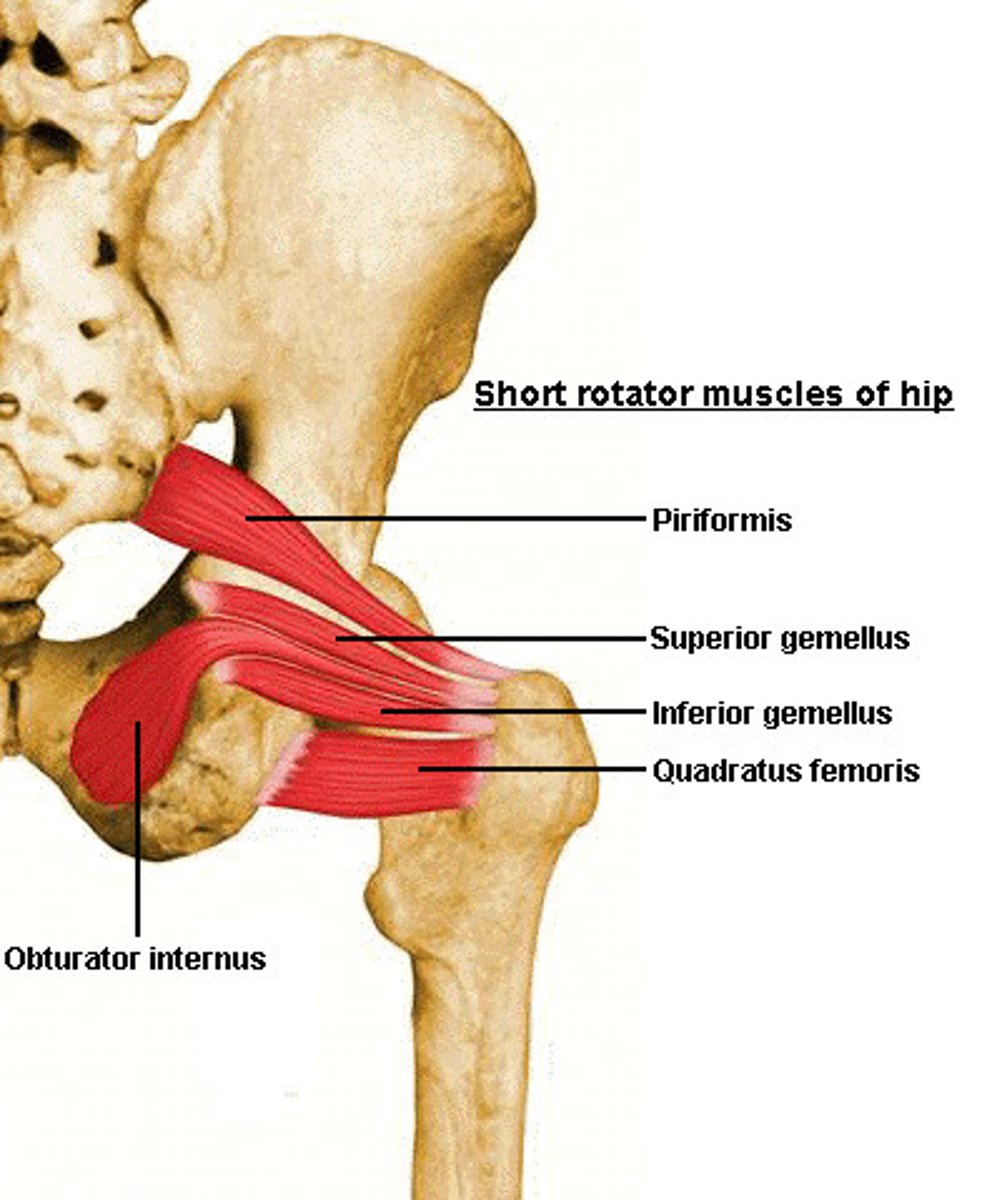
Gemellus Inferior
Origin: ischial tuberosity
Insertion: greater trochanter
Main Action: laterally rotate the thigh and stabilize the femoral head in the acetabulum
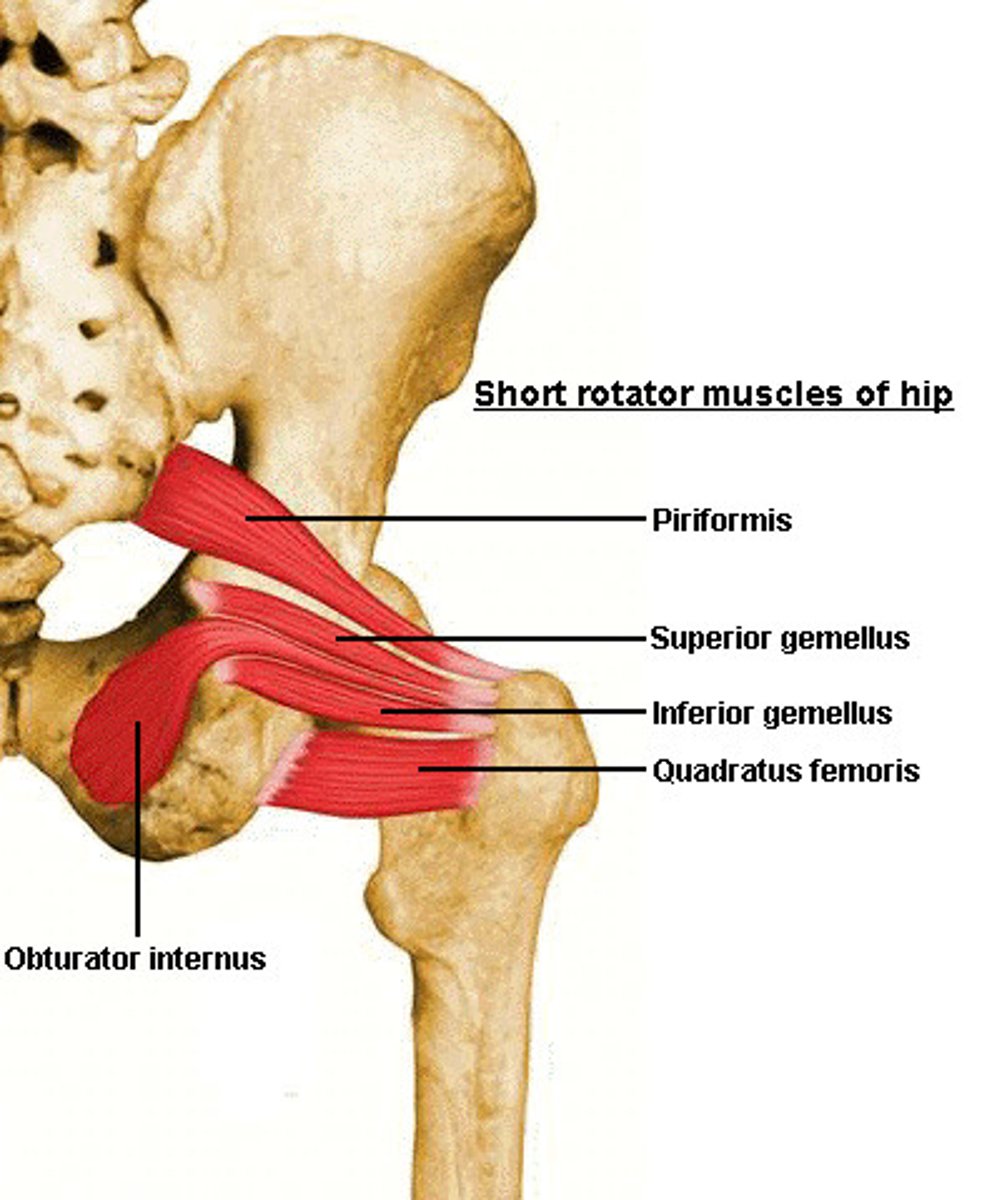
Obturator Externus
Origin: outer margins of obturator foramen
Insertion: greater trochanter
Main Action: laterally rotate the thigh and stabilize the femoral head in the acetabulum
Deep to quadratus femoris
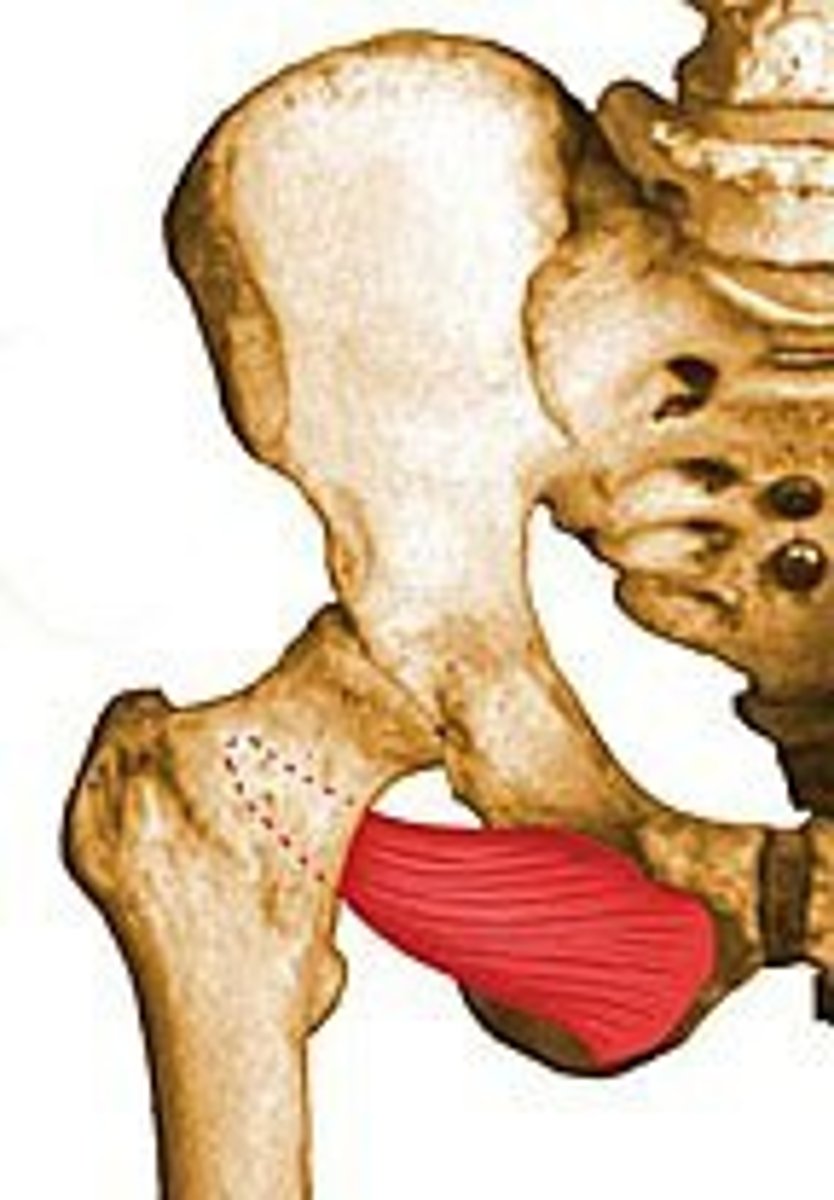
Quadratus Femoris
Origin: ischial tuberosity
Insertion: intertrochanteris crest of the femur
Main Action: laterally rotate the thigh and stabilize the femoral head in the acetabulum
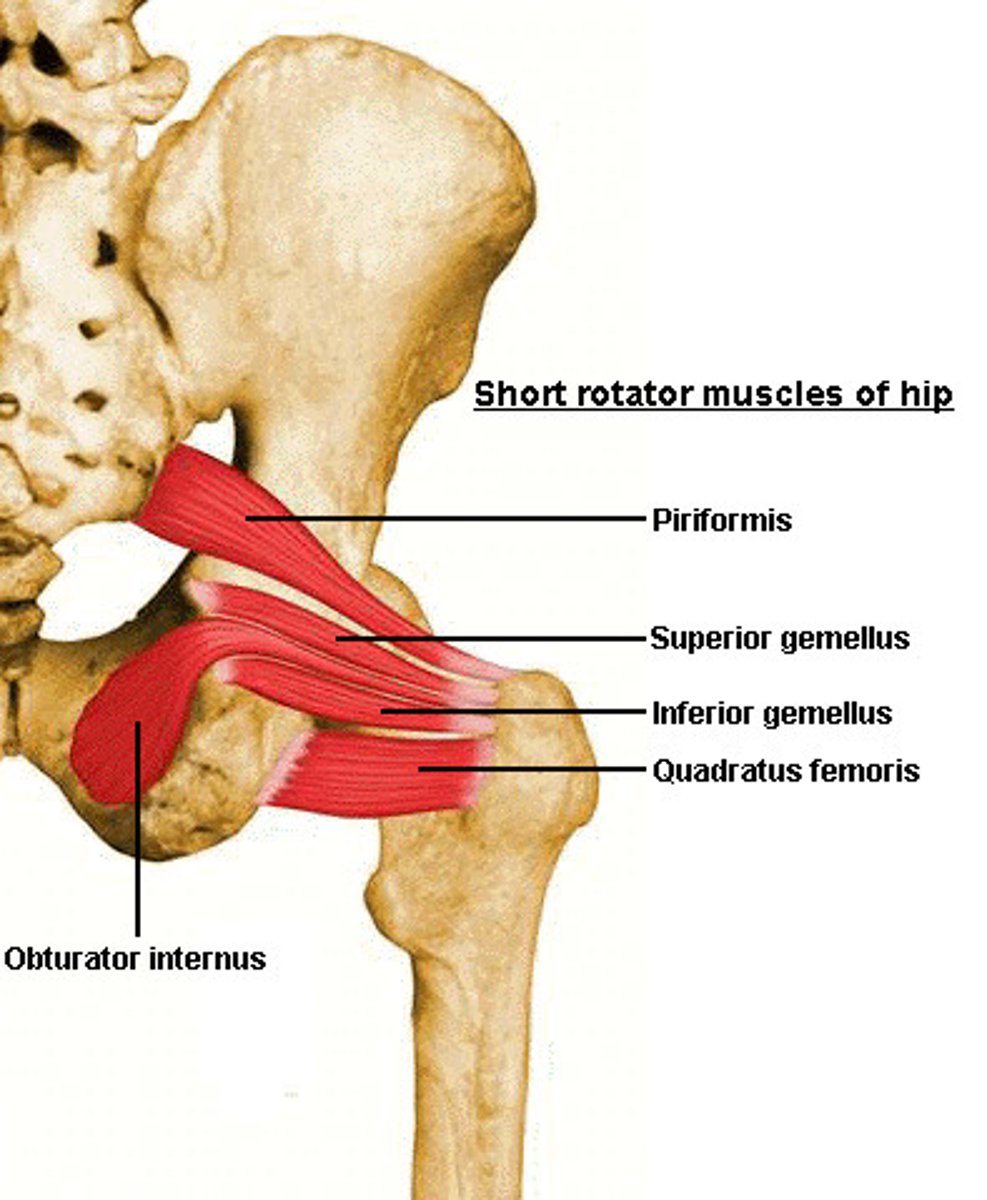
Sciatic Nerve
it is the tibia nerve and the common fibular nerve wrapped in a common connective tissue sheath. Enters the gluteal region via the greater sciatic foramen and passes inferably deep to the gluteus maximus. DOES NOT SUPPLY MUSCLES IN THE GLUTEAL REGIONS. instead it innervates the muscles of the posterior thigh, leg and foot
Sciatica
Compression of sciatic nerve causing back pain with radiation to posterior leg
Trochanteric Bursitis
Inflammation at the site where the gluteus medius inserts or the IT-band passes over the trochanter
Iliotibial Band Syndrome
Over use injury. Cause by this band rubbing against bone, often in the area of the knee.
Piriformis Syndrome
→compression of the sciatic nerve
→caused when piriformis muscle is too big squishes the nerve: or due to overuse and random spasms.
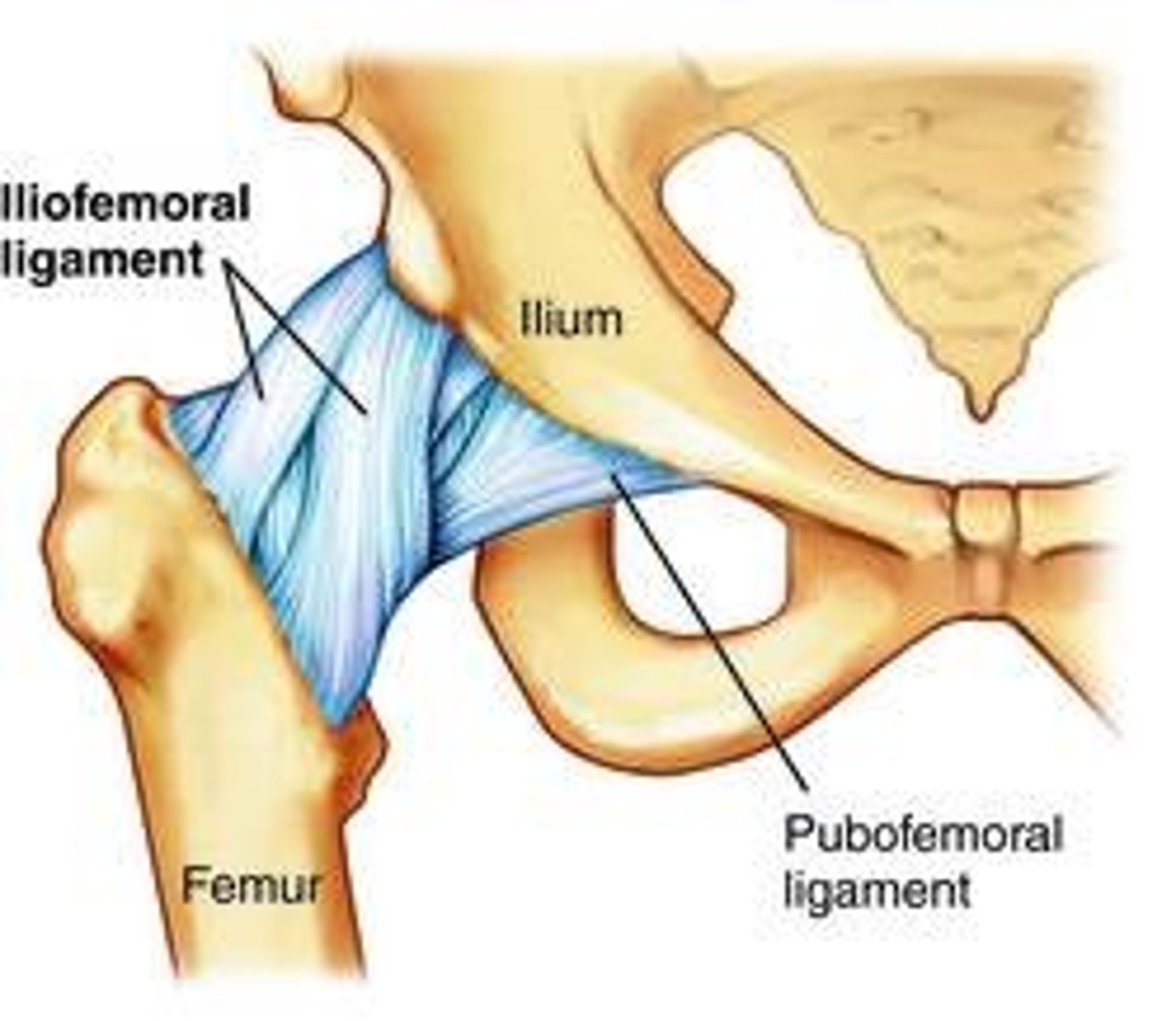
The iliofemoral ligament
found on the anterior part of the joint and prevents overextension and helps maintain erect posture by resisting the hip extension caused by bearing weight
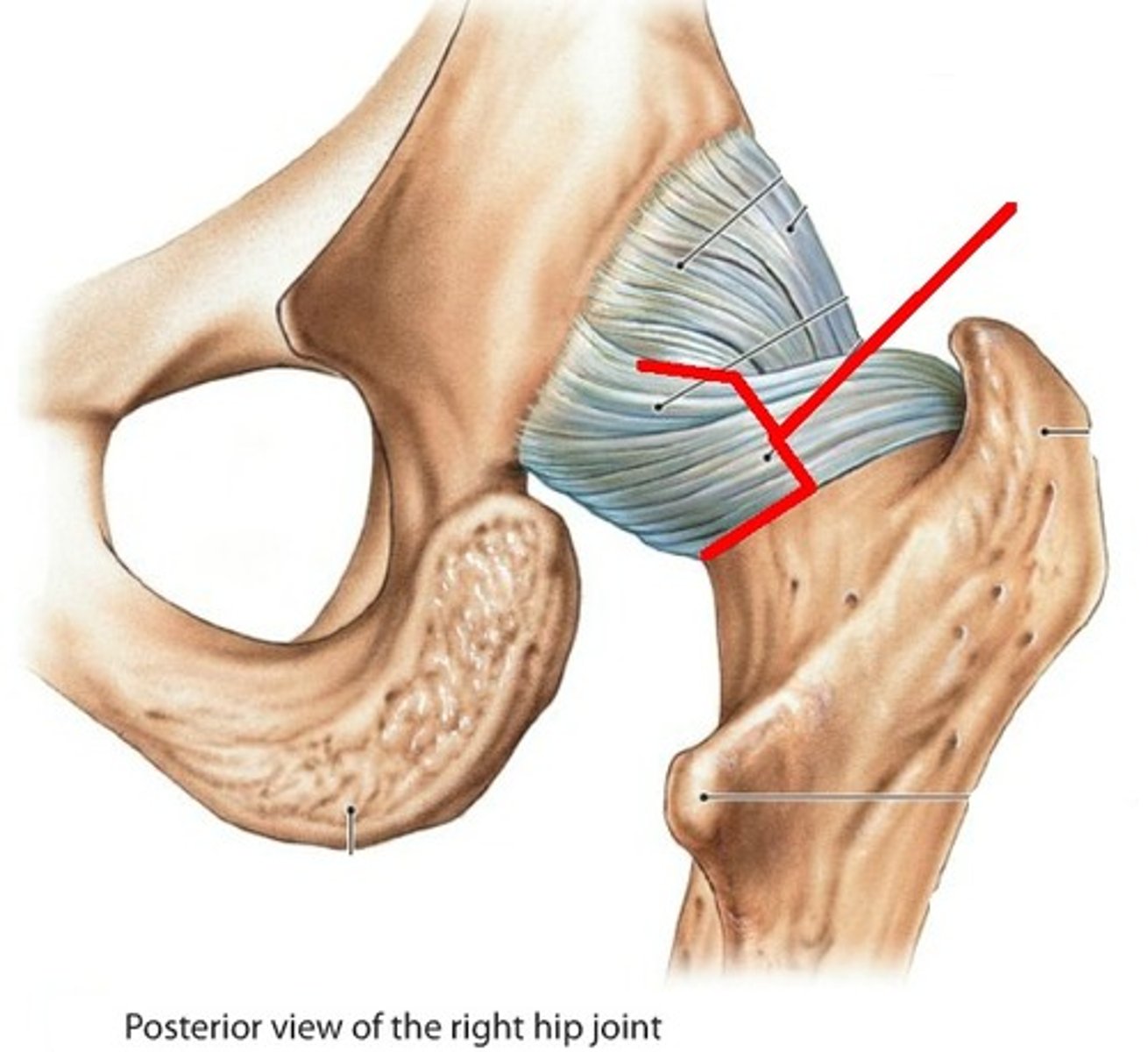
The ischiofemoral ligament
found posteriorly, and also limits extension
The pubofemoral ligament
found interiorly; prevents overabduction
Most of the blood supply of the head of the femur comes from the
medial and lateral femoral circumflex vessels, branches of the deep femoral artery or the femoral artery; these branches can be injured when the neck of the femur is fractured leading to aseptic necrosis of the head of the femur
The quadriceps femoris inserts onto the
tibial tuberosity
Deep Fascia
fascia lata in the thigh, and the crural fascia in the leg.
Along the lateral aspect of the knee and leg is called the
iliotibial tract
what do the fascia late and crural fascia do?
they help pump venous blood out of the lower limb; when the muscles of the lower limb contract, these fasciae prevent them from bulging outward and forces them to compress thin-walled veins. the fascia surrounding the lower limb also helps the various muscles to work more efficiently in unison as we walk and run
In the superficial fascia are the
superficial veins and cutaneous nerves.
what is the most important superficial vein?
the great saphenous vein; this vein drains blood from the medial aspect of the foot, leg, and thigh, and returns this blood to the femoral vein by passing through an opening in the fascia late of the proximal thigh called the saphenous opening
- the great saphenous vein can be found running just anterior to the medial malleolus at the ankle