Respiratory Tract Infections
1/125
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
126 Terms
Name 5 Upper respiratory tract infections (URTI)
• Sinusitis / rhinitis
• Otitis media
• Pharyngitis
• Tonsillitis
• Epiglottitis
Name 3 Lower respiratory tract infections (LRTI)
• Tracheitis / bronchitis
• Bronchiolitis
• Pneumonia / pneumonitis
Are viral/bacterial resp tract infections more common
Viral
VIRAL = cough, coryza, hoarse, myalgias, diarrhoeas, rashes, others sick
BACTERIAL = more severe, fever, not resolving
What’s the proper name for the common cold
Rhinosinusitis
Rhinosinusitis normal incubation period
1-3 days
Rhinosinusitis duration of symptoms
1-2 weeks
3 drug “classes” that give symptomatic relief for rhinosinusitis
Paracetamol, NSAIDs, antihistamines
6 possible viral causes of Rhinosinusitis
◦ Rhinoviruses
◦ Coronaviruses
◦ Adenoviruses
◦ Parainfluenza viruses; respiratory syncytial viruses
(could also be Influenza viruses or SARS-CoV-2)
What other symptoms may appear if sinusitis becomes bacterial
Sometimes superimposed bacterial infection (acute bacterial sinusitis) → sneezing, nasal discharge (sometimes purulent), headache, facial pain, etc.
What 3 things would lead you to suspect there is a bacterial infection with sinusitis
◦ No improvement or worsening after 8-10d
◦ High fever, significant facial pain
◦ Development of central nervous system features (emergency)
2 possible bacteria in sinusitis
◦ Streptococcus pneumoniae
◦ Haemophilus influenzae
Otitis media is what
Ear infection/inflammation
Otitis media is usually viral/bacterial (& give example of most likely cause)
Viral - Rhinovirus
Occasionally, Otitis media has a secondary bacterial infection caused by what 3 bacteria
◦ Streptococcus pneumoniae
◦ Haemophilus influenzae
◦ Moraxella catarrhalis
3 most common causes of Pharyngitis (2 viral, 1 bacterial)
◦ Glandular fever (Epstein-Barr virus); HIV
◦ B-haemolytic Streptococcus (eg. S. pyogenes)
Name 3 other bacteria that could cause Pharyngitis
Mycoplasma, anaerobes, Corynebacterium diphtheriae
Clinical scores may be helpful in determining the need for antimicrobial therapy.
What 4 points/symptoms are used to decide whether someone gets treated for strep

Acute epiglottitis is usually caused by what (be specific)
H. influenzae type b
Acute epiglottitis clinical presentation
Toxic, dysphagia, drooling of saliva
What 3 precautions must be taken with Acute epiglottitis treatment?
◦ Get specialist review (eg. ENT) promptly
◦ Secure airway; avoid unnecessary examination
◦ Early antibiotics
Give an example of an antibiotic you could use for Acute epiglottitis
Ceftriaxone
Now moving to Lower respiratory tract infections…
What’s another name for Laryngo-trachea-bronchitis
Croup
Croup is most often seen in which age group
Typically in younger children (< 6 yrs)
Croup symptoms
Characterised by a barking-type cough, hoarseness of voice, fever, agitation, stridor, etc
Croup is usually caused by what
Parainfluenza viruses
(Occasionally RSV)
Bronchiolitis is seen most in what age group
Typically in infants and young children
Bronchiolitis is seen most at what time of year
winter
Bronchiolitis is usually caused by what bacteria/virus
Usually caused by respiratory syncytial viruses (RSVs)
Symptoms of Bronchiolitis
Wheezing, cough, URTI symptoms
Proper name for whooping cough
Pertussis
Pertussis is caused by what bacteria/virus
Bordetella pertussis
Morbidity and mortality of pertussis is highest in what age group
Highest in infants
Symptoms of the Catarrhal stage (early stage - most infectious) of pertussis
Coughing spasms (wks-mths) characteristic inspiratory whoop in children; infants may develop apnoea and cyanosis; complications of pneumonia & encephalopathy, etc
What is treatment for pertussis
Early Rx (with macrolides) can reduce infectivity and duration of symptoms
True/False Immunity received after Pertussis lasts a lifetime
False - Immunity wanes over time (>10 yrs)
When might a booster vaccination be indicated for pertussis (2)
Pregnancy
Certain HCWs
Symptoms of Community-acquired pneumonia
cough, purulent sputum, dyspnoea, chest pain, fever, anorexia, sweats, etc.
What 2 viruses/bacteria generally cause community-acquired pneumonia
Streptococcus pneumoniae
Haemophilus influenzae (non-type b)
Name 4 atypical organisms that could cause community-acquired pneumonia
Legionella pneumophila; Mycoplasma pneumoniae; Chlamydophila pneumoniae; Coxiella burnetti (Q fever)
Name 3 viruses that could cause community-acquired pneumonia
Influenza viruses
SARS-CoV-1 / SARS-CoV-2
MERS-CoV
2 examples of Pneumonic complications of systemic viral infections
Measles, Varicella-zoster (chickenpox)
Name 4 other possible bacterial causes of community-acquired pneumonia
Staphylococcus aureus
Pseudomonas aeruginosa
Anaerobes
Klebsiella pneumoniae
When might you suspect Staphylococcus aureus as a cause for community-acquired pneumonia
Post-trauma or post-influenza
When might you suspect Pseudomonas aeruginosa as a cause for community-acquired pneumonia
cystic fibrosis
bronchiectasis
How would Anaerobes enter your system to cause community-acquired pneumonia
Aspirated
2 possible fungal causes of community-acquired pneumonia
Pneumocystis, Aspergillus
Which possible fungal cause of community-acquired pneumonia would only be seen in severely immuno-compromised patients
Aspergillus
True/False Mycobacterium tuberculosis could be a cause of community-acquired pneumonia
True
Streptococcus pneumoniae (major pathogen for community-acquired pneumonia) is gram +/- and what shape
Gram-positive diplococci
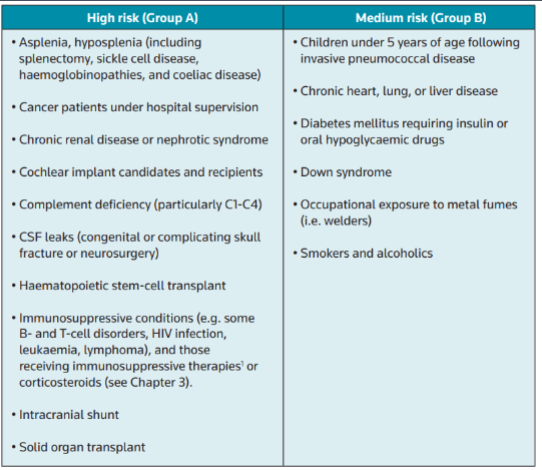
Risk groups for invasive pneumococcal disease (IPD)
Age
Co-morbidities
>65 yrs or <2 yrs
Chronic lung, cardiovascular, renal and liver diseases
Diabetes mellitus, alcohol abuse
Asplenia/hyposplenism
Immunosuppression (condition and/or treatment)
Post-influenza (secondary bacterial infection)
Streptococcus pneumoniae causes what type of pneumonia: Bronchopneumonia, Aspiration pneumonia, Lobar pneumonia
Lobar pneumonia
What can Streptococcus pneumoniae be treated with
Varying levels of susceptibility to penicillin
True/False Higher doses of penicillin/amoxicillin can overcome intermediate penicillin susceptibility in S. pneumoniae
True
What is co-amoxiclav a combo of
amoxicillin & clavulanic acid
Is co-amoxiclav (amoxicillin-clavulanate) superior to amoxicillin if S. pneumoniae is susceptible to both?
No — if Streptococcus pneumoniae is susceptible to amoxicillin, there is no benefit in using co-amoxiclav over amoxicillin alone
When should co-amoxiclav (amoxicillin + clavulanic acid) be used?
Amoxicillin alone can be broken down by β-lactamase enzymes produced by some bacteria
Clavulanic acid inhibits β-lactamase, protecting amoxicillin
Main indications: infections where β-lactamase–producing bacteria are likely. E.g. Haemophilus influenzae & Moraxella catarrhalis
Give 4 classes of drug treatments for S. pneumoniae RTI
Beta-lactams
Macrolides
Quinolones
Tetracyclines
Give 2 types of Beta-lactams used in the treatment of S. pneumoniae RTI (& give an example of each)
Penicillins (eg. penicillin, amoxicillin)
Cephalosporins (eg. ceftriaxone)
Give 2 examples of Macrolides used in the treatment of S. pneumoniae RTI
clarithromycin, erythromycin
Give an example of a Quinolone used in the treatment of S. pneumoniae RTI
levofloxacin
Give 2 examples of Tetracyclines used in the treatment of S. pneumoniae RTI
tetracycline, doxycycline
‘Atypical’ bacterial pathogens present slightly differently. How would symptoms differ
May have more prominent extra-pulmonary features eg. CNS, gastrointestinal, etc.
How would lab testing differ for ‘atypical’ bacterial pathogens
They don’t grow on standard media eg. blood agar; alternative methods of diagnosis
How would radiological features differ for ‘atypical’ bacterial pathogens
Perihilar infiltrates
Diffuse infiltrates, etc.
How would treatment differ for ‘atypical’ bacterial pathogens
Beta-lactams are ineffective; often requires Rx with macrolides or fluoroquinolones
What Investigations would you carry out for pneumonia
Clinical history and physical examination
Radiological eg. Chest X-ray
General laboratory: FBC, biochemistry, ESR, CRP, blood gas
Microbiological:
◦ Sputum for microscopy, culture, etc.
◦ Nasopharyngeal swab (PCR for eg. viruses)
◦ Blood culture
◦ Urine
Others: eg. bronchoscopy, biopsy
In investigation of pneumonia, what are you testing for in urine
Legionella & pneumococcal antigens
In investigation of pneumonia what culture medium is generally used
Usually on blood and chocolate agar
How is it decided if hospitalisation is necessary for pneumonia
CURB-65 criteria
Explain the CURB-65 criteria

What CURB65 score is considered Mild/Moderate/Severe CAP (Community-acquired pneumonia)
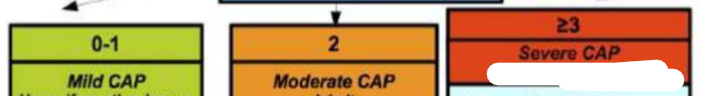
What CAP scored require admission
2+
How is mild CAP treated

How is moderate CAP treated
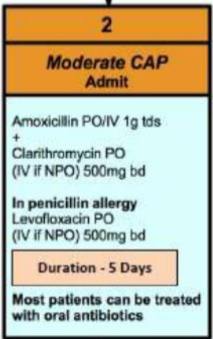
How is severe CAP treated


Fill in the antibiotics used in the treatment of CAP
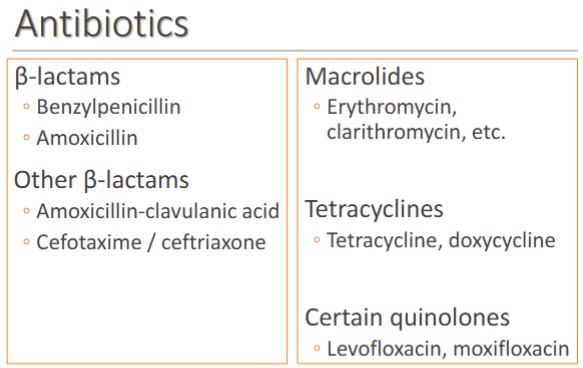
How does treatment change for S. pneumoniae vs H. influenzae/M. catarrhalis vs Atypical organisms
S. pneumoniae: often responds to high-dose penicillin/amoxicillin
H. influenzae/M. catarrhalis: β-lactamase-producer? → consider amoxicillin-clavulanic acid
Atypical organisms: Macrolides or quinolones
How does treatment change for mild vs moderate-severe cases
Mild cases:
◦ Amoxicillin / Amoxicillin-clavulanic acid Or
◦ Clarithromycin Or
◦ Doxycycline
Moderate to severe cases:
◦ Amoxicillin plus clarithromycin; Or
◦ Amoxicillin / Amoxicillin-clavulanic acid plus clarithromycin; Or
◦ Cefotaxime plus clarithromycin
Top 3 causal organisms of typical pneumonia
. Streptococcus pneumoniae
· Haemophilus influenzae
· Staphylococcus aureus
Top 3 causal organisms of atypical pneumonia
· Mycoplasma pneumoniae
· Chlamydia pneumoniae
· Legionella pneumophila
Which group of Legionella pneumophila causes the majority of legionellosis
Serogroup 1
Symptoms of Legionella infection
fever, cough, altered mental status, abdominal symptoms, headaches, hyponatraemia, elevated liver enzymes, etc.
3 groups @ high-risk for legionellosis
◦ Elderly patients
◦ Heavy smokers, chronic lung disease
◦ Steroids, other causes of immunosuppression
How is Legionella pneumophila usually acquired (transmitted)
Usually acquired via inhalation of aerosolised organisms after exposure to environmental sources eg. contaminated air-conditioning systems, Jacuzzis, cooling towers, etc.
How is Legionella pneumophila diagnosed
Difficult to culture (needs special medium)
Look for Legionella urine antigen (L. pneumophila serogroup 1)
PCR assay for respiratory samples
Treatment for Legionella pneumophila
Quinolones (eg. levofloxacin)
or
Macrolides (eg. clarithromycin, erythromycin)
Now we’re moving to Hospital-acquired pneumonia. What is the most common causal organism
Staphylococcus aureus (including MRSA)
Name 3 bacteria that could cause Hospital-acquired pneumonia
E. coli, Klebsiella pneumoniae, Pseudomonas aeruginosa
Do gram +/- bacteria cause Hospital-acquired pneumonia
Gram -
Infective exacerbation of COPD can be a cause of pneumonia. How would you spot this?
Acute change of symptoms beyond baseline levels:
Eg.
Change in purulence of sputum
Increase in sputum volume
Increase in dyspnoea
True/False Infective exacerbation of COPD would show consolidation on imaging
False - no consolidation
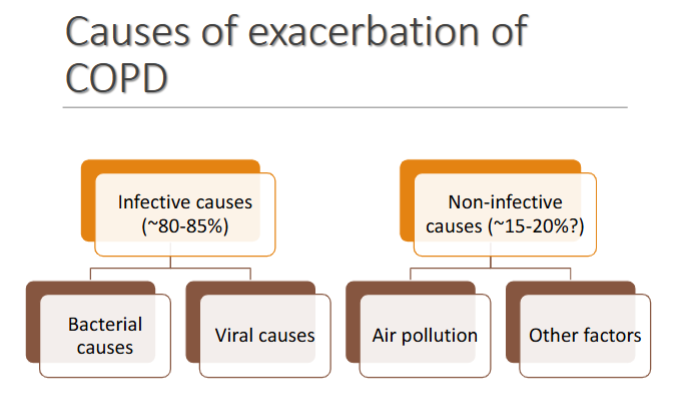
Most common bacterial causes of Infective exacerbation of COPD
Haemophilus influenzae (non-type b)
Streptococcus pneumoniae
Moraxella catarrhalis
What would be a bacteria that would cause an advanced disease Infective exacerbation of COPD
Pseudomonas aeruginosa
Main viral cause of Infective exacerbation of COPD
Rhinoviruses
Are there any other possible viral causes of an Infective exacerbation of COPD
Influenza and Parainfluenza viruses; RSV; others
Rx in infective exacerbation of COPD
Most guidelines recommend:
Beta-lactam (eg. amoxicillin or amoxicillin-clavulanate)
Or
Macrolide (eg. clarithromycin)
Or
Tetracycline (eg. doxycycline)
Influenza virus is a DNA/RNA virus
RNA
How many types of Influenza virus are there
3 types: A, B, C