IMED2001 - Antibiotics and Antibiotic Resistance (L7)
1/21
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
Antimicrobial therapeutics: general consideration
NOT ALL INFECTIONS REQUIRE ANTIMICROBIAL THERAPY:
- Host immune system controls most infections
.
DIFFERENT CLASSES OF MICROBES REQUIRE DIFFERENT THERAPEUTICS:
- Bacteria: antibiotics
- Fungi: antifungals
- Parasites: anti-parasitic agents
- Viruses: anti-virals
.
SOME CORE CONCEPTS APPLY TO ALL OF THESE:
- Selective toxicity, spectrum of activity, antimicrobial resistance, need for stewardship
.
ADJUNCT (NON-ANTIMICROBIAL) THERAPEUTICS ARE SOMETIMES NEEDED FOR INFECTIONS
- Adjunctive immune therapy e.g steroids to reduce inflammation in meningitis
- Removing the source of the infection (e.g surgical drainage)
Many antibiotics are derived from natural products
penicillin
Core concepts in antibiotic therapy
INDICATION FOR THERAPY:
- When do we treat a patient with an antibiotic
MODE OF ACTION:
- how do antibiotics work
SPECTRUM OF ACTION:
- which antibiotics for which bacteria?
ANTIBACTERIAL RESISTANCE:
- How does resistance evolve and spread amongst bacteria
PRINCIPLES OF USE AND STEWARDSHIP:
- Prevent emergence of antimicrobial resistance
- What antibiotic(s), what dose, for how long?
What are the indications for antibiotic therapy
TO TREAT A BACTERIAL INFECTION THAT:
- is severe, or
- is unlikely to resolve spontaneously (or with local treatment) or,
- may be followed by severe complications
.
TO PREVENT A BACTERIAL INFECTION IN SPECIFIC SITUATIONS. e.g,
- surgical prophylaxis (especially if implantable devices)
- prevent recurrent acute rheumatic fever
.
MIXED INFECTIONS ARE NOT UNUSUAL
- for example, sometimes viral respiratory infections may be assocaited with bacterial 'superinfection' that requires antibiotics (influenza virus + S. aureus or S. pneumoniae
.
Prophylaxis is a medical term for preventive care, encompassing actions taken to prevent disease, infection, or complications before they occur.
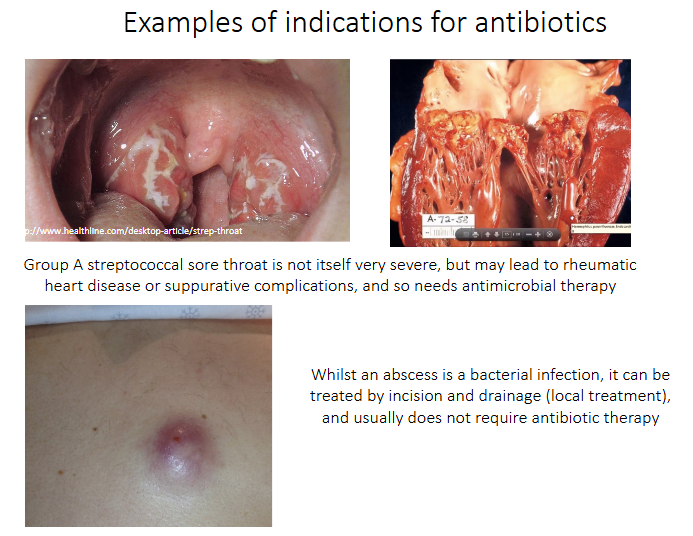
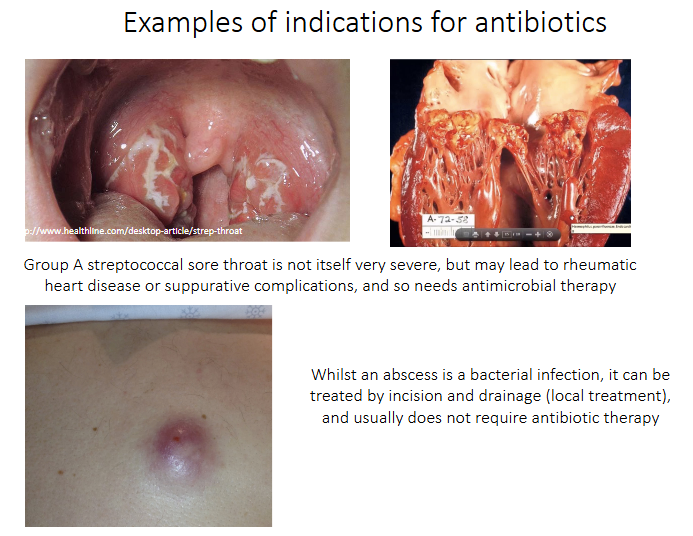
Examples of indications for antibiotics
- Group A streptococcal sore throat is not itself very severe, but may lead to rheumatic heart disease or suppurative compliccations, and so needs antimicrobial therapy
- Whilst an abscess is a bacterial infection, it can be treated by incision and drainage (local treatment), and usually does not require antibiotic therapy
Mode of action of antibiotics
- Antibiotics usually require 'support' from the host immune system to eradicate infection
.
Antibiotics work by inhibiting core metabolic processes in bacteria
- e.g synthesis of cell wall, protein, nucleic acid, other biochemical pathways
.
Antibiotics that target the same bacterial pathway may be antagonistic
- those that target different pathways may be synergistic
.
BACTERIA VARY IN SUSCEPTIBILITY TO ANTIBIOTICS ACCORDING TO THEIR:
- Metabolic activity, e.g actively dividing bacteir are more susceptible
- local environment. e.g bacteira in biofilms are more resistant
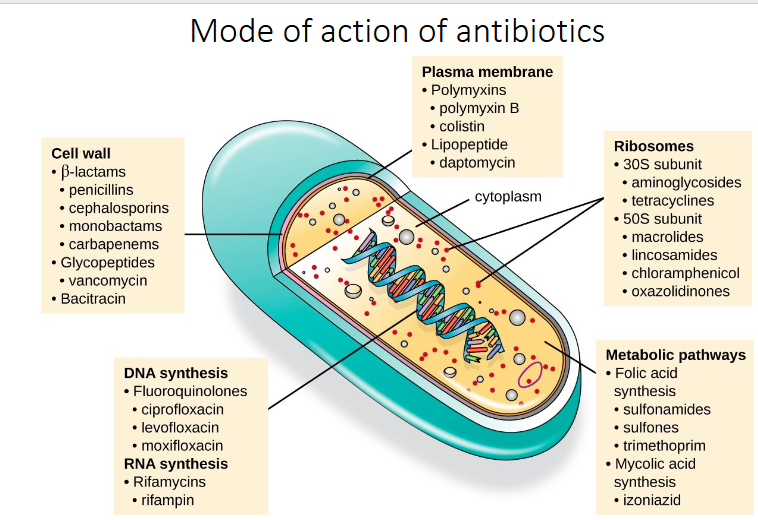
Mode of action of antibiotics diagram
DIAGRAM ON SLIDE 9
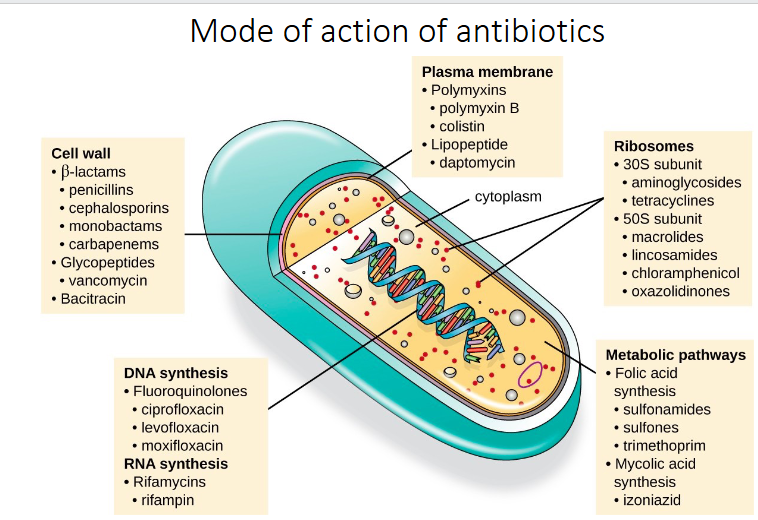
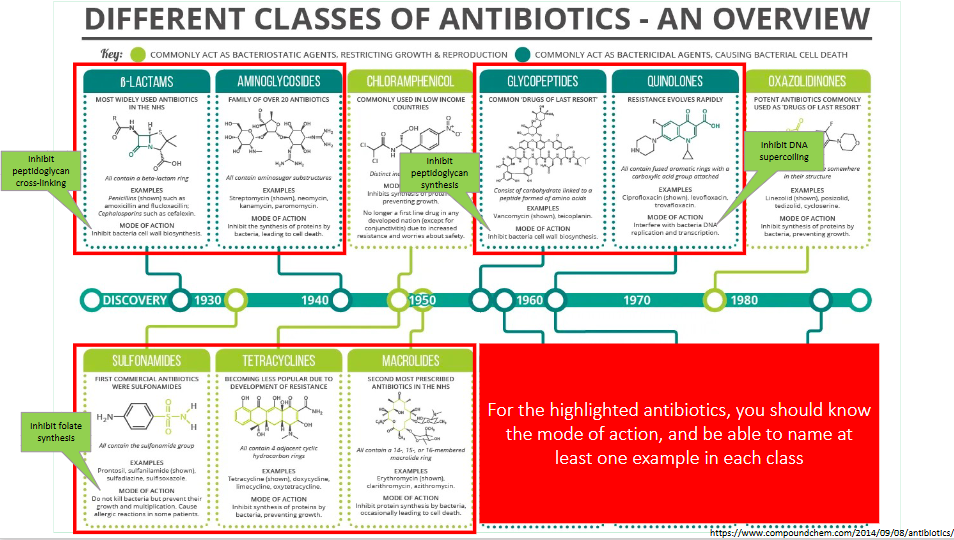
Need to know the antibiotics that are highlighted in red
- should know the mode of action, and be able to name at lesat one example in each class
.
- quinolones inhibit DNA gyrase which was involved in supercoiling of DNA
.
BACTERICIDAL AGENTS:
BETA-LACTAMS
all contain a beta-lactam ring
Mode of Action:
Inhibit cell wall biosynthesis by inhibiting peptidoglycan cross-linking
Examples: Penicillins, Cephalosporins
.
AMINOGLYCOSIDES:
all contain aminosugar substructures
Mode of action:
Inhibit synthesis of proteins by bacteria, leading to cell death
Examples: Streptomycin, Neomycin
.
GLYCOPEPTIDES:
consist of a carbohydrate linked to a peptide formed of amino acids
Mode of action:
Inhibit bacteria cell wall biosynthesis by inhibiting peptidoglycan synthesis
Examples: Vancomycin
.
QUINOLONES:
all contain fused aromatic rings with a carboxylic acid group attached
Mode of action:
Interfere with bacteria DNA replication and transcription (inhibit DNA supercoiling)
Examples: Ciprofloxacin
.
BACTERIOSTATIC AGENTS:
SULFONAMIDES:
all contain the sulfonamide group
Mode of action:
do not kill bacteria but prevent their growth and multiplication. Cause allergic reactions in some (inhibit folate synthesis)
Examples: Prontosil, Sulfadiazine
.
TETRACYCLINES:
all contain 4 adjacent cyclic hydrocarbon rings
Mode of action:
inhibit synthesis of proteins by bacteria, preventing growth
Examples: Tetracycline, Limecycline
.
MACROLIDES:
all contain a 14-, 15- or 16- membered macrolide ring
Mode of action: Inhibit protein synthesis by bacteria, occassionally leading to cell death
Examples: Erythromycin
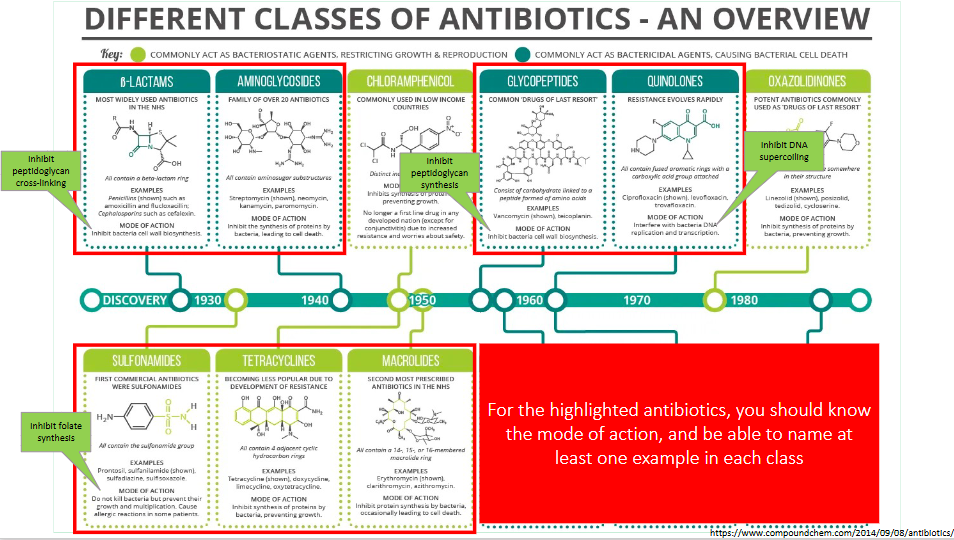
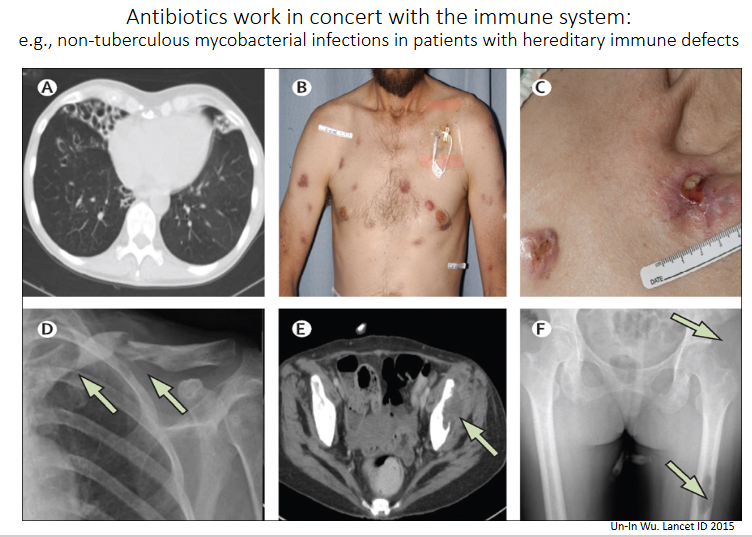
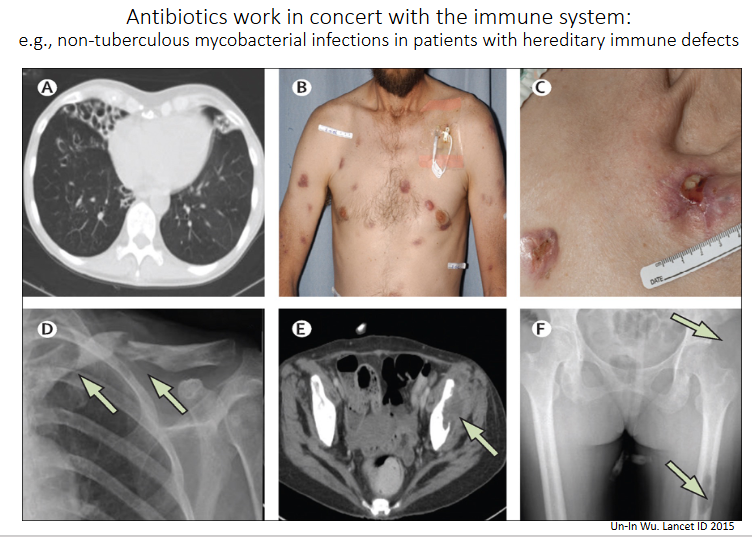
Antibiotics work in concert with the immune system
- e.g non-tuberculous mycobacterial infections in patients with hereditary immune defects
Spectrum of activity of antibiotics
- refers to the range of bacteria against which an antibiotic is active
.
BROAD SPECTRUM:
- active against both Gram positive and Gram negative
- useful for empiric therapy
- More likely to lead to spread of multi-resistant bacteria
.
NARROW SPECTRUM:
- active against (fewer) specific families of bacteria
- more targetted so less likely to lead to selection for resistance
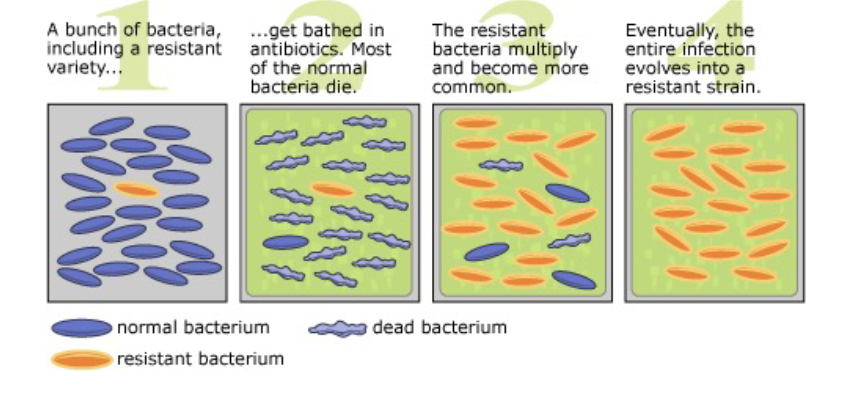
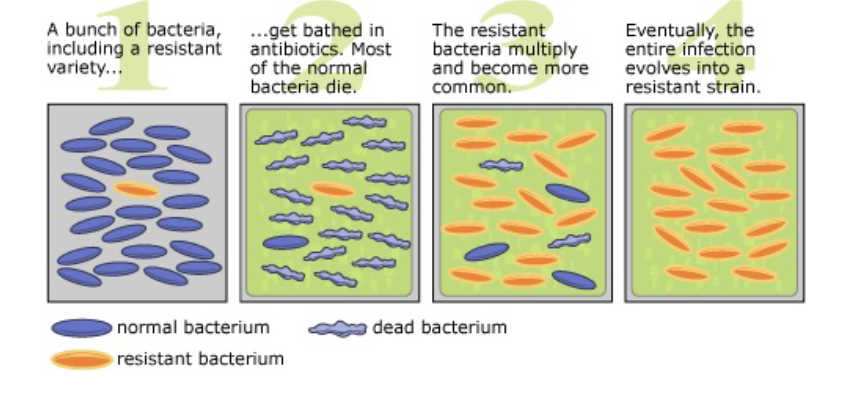
How does resistance spread in a bacterial population?
1. bunch of bacteria including a resistant variety
2. get bathed in antibiotics. Most of the normal bacteria die
3. The resistant bacteria multiply and become more common
4. Eventually, the entire infection evolves into a resistant strain
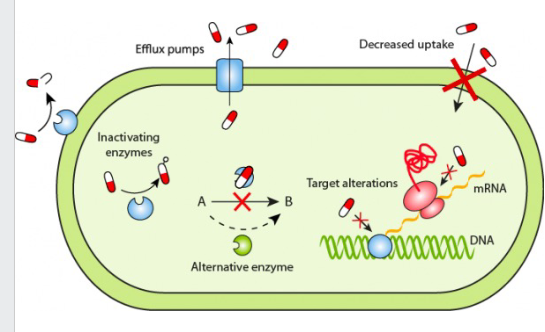
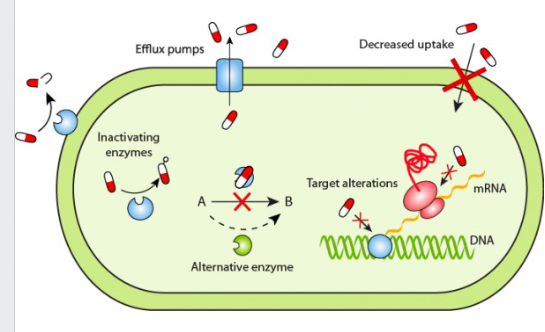
Mechanisms of Antibiotic Resistance
STOP THE ANTIBIOTIC FROM REACHING ITS TARGET:
- pump the antibiotic out (efflux pumps)
- Decrease permeability of the bacterial cell membrane
- Bacterial enzymes that inactivate antibiotics (e.g Beta-lactamase destroys the beta-lactam ring of penicillins)
- bacterial enzymes that modify (add chemical groups to) antibiotics, inhibiting their binding to target
.
MODIFY OR BYPASS THE TARGET OF THE ANTIBIOTIC:
- Camouflage the target by changing the structure of the target in the bacterium
- Bypass the target, e.g penicillin-binding protein (PBPs) are needed for bacterial cell wall synthesis and are the targets of beta-lactam antibiotics. S. aureus can acquire the resistance gene mecA which produces a new PBP with low affinity for beta-lactam antibiotics (MRSA: methicillin-resistant Staphylococcus aureus)
.
- some bacteria are naturally resistant to certain antibiotics (e.g bacteria without cell walls (mycoplasmas) are intrinsicaly resistant to antibiotics, such as Beta-lactams, that act on cell wall synthesis)
- in contrast, when bacteria which were previously susceptible to an antibiotic evolve resistance is called acquired resistance
.
- Look at the reaction where A goes to B. Antibiotics stops that, but some bacteria develop an alternative enzyme for that reaction
.
Penicillin-binding proteins (PBPs) are essential bacterial enzymes that construct the cell wall by cross-linking peptidoglycan, ensuring structural integrity and proper division. They are the primary targets of
-lactam antibiotics (e.g., penicillin), which inhibit them, leading to cell lysis. Resistance often arises through structural modifications in PBPs that lower antibiotic binding
Principles of use of antibiotics
- only use when indicated
- Use a narrow spectrum antibiotic when possible
- Choice depends on infecting organism and type and site of infection (antibiotics penetrate tissue/fluid variability) (e.g meningitis) (meningitis requires penetrating blood brain barrier)
- dose (higher doses less likely to select for partially resistant strains)
.
Duration of therapy
- fixed for certain conditions, e.g endocarditis (to prevent relapse of infection)
- In many cases can stop therapy when symptoms resolve
- longer duration -> continued antibiotic pressure -> increasing likelihood of selecting for resistant strains
- inadequate duration may lead to relapse of infection, not to resistance
.
Combination Therapy useful for:
- specific bacteria where risk of resistance emerging is high (e.g M. tuberculosis)
- Some specific severe infections e.g endocarditis

Understanding syndromic management and empiric treatment
- One microorganism can cause infection at many different sites in the body
- Infection at one site in the body can be caused by many different microorganisms
.
- Empiric treatment is the initiation of medical therapy—usually antimicrobials—based on clinical suspicion, patient risk factors, and local resistance patterns, rather than waiting for definitive laboratory results
- Syndromic management is an approach to treating STIs based on symptoms (syndromes) rather than laboratory tests, designed for high-volume or low-resource settings
.
- syndromic treatment is a type of empiric treatment

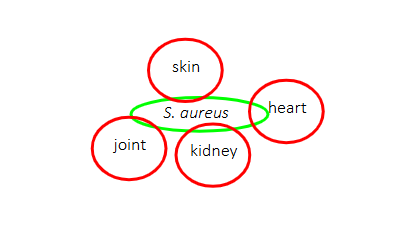
For example, in the case of Staph. aureus
DIAGRAM ON SLIDE 20
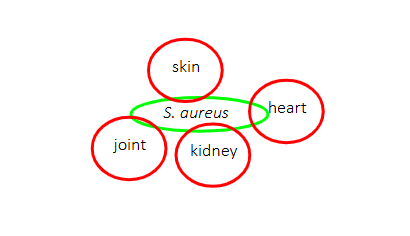
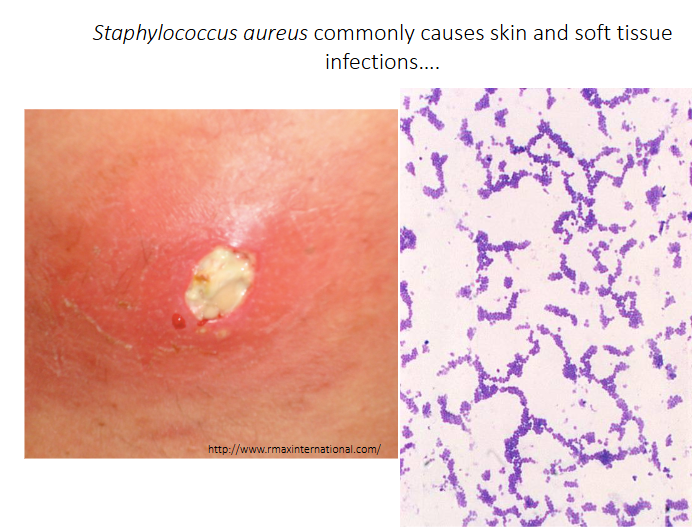
Staphylococcus aureus commonly causes skin and soft tissue infections
DIAGRAM ON SLIDE 21
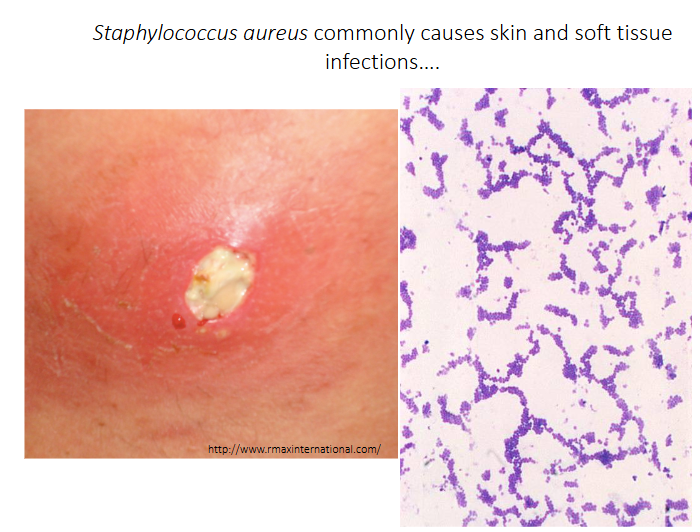
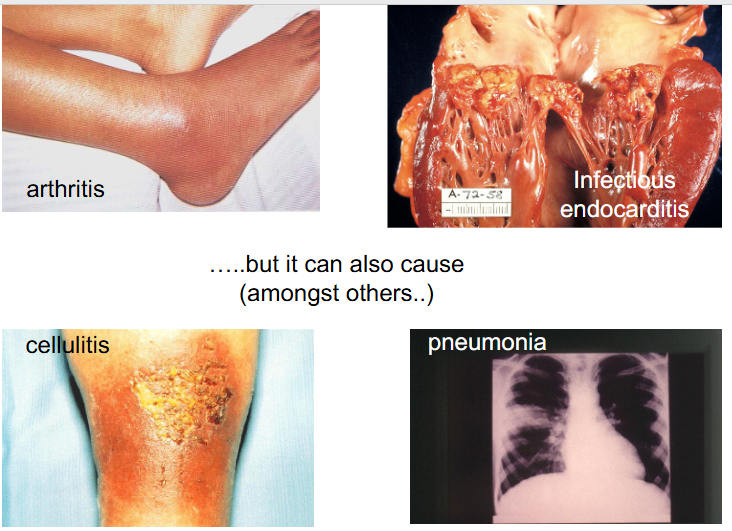
S. aureus can also cause (amongst others)
DIAGRAM ON SLIDE 22
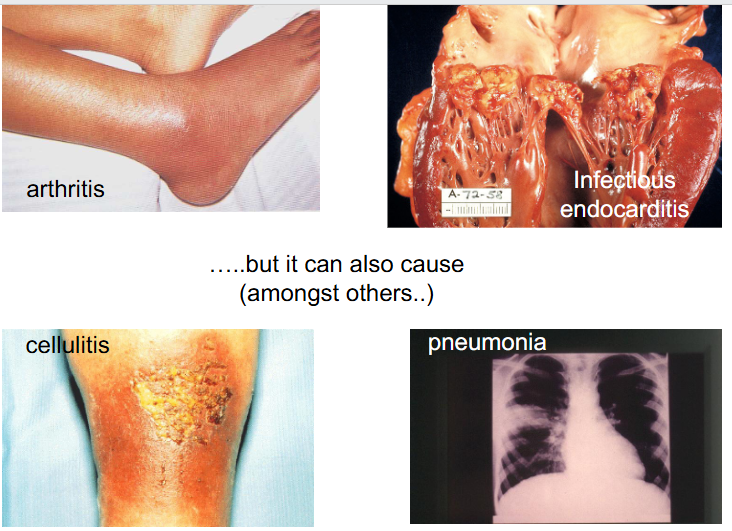
On the other hand
DIAGRAM ON SLIDE 23
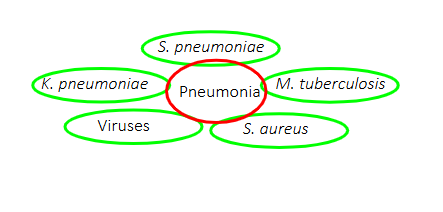
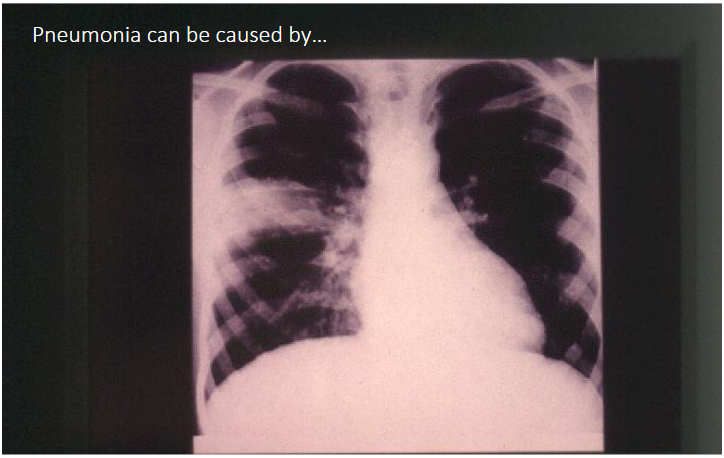
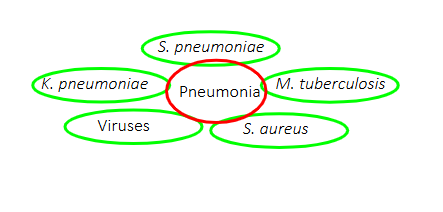
Pneumonia can be caused by
BACTERIA
- Streptococcus pneumoniae (gram-pos diplococci)
- Haemophilus influenzae (gram-neg bacilli)
- Klebsiella pneumoniae (gram-neg bacilli)
- Staphylococcus aureus (gram-pos cocci in clusters)
- Mycoplasma pneumoniae (no cell wall-therefore not affected by gram stain)
.
VIRUSES:
- RSV, influenza virus, coronaviruses, and others
.
- basically when we treat pneumonia we need to know what antibiotic or medicine to choose
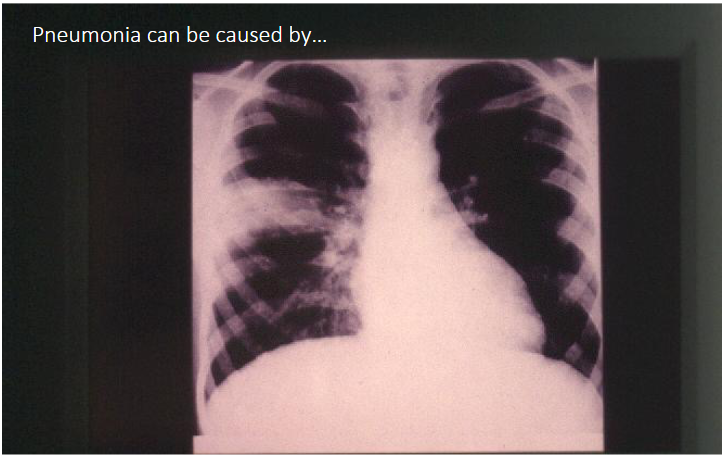

Infectious Syndromes
- infection of a particular body site. e.g infections of the lower respiratory tract, cause a set of commonly co-occuring symptoms and signs, e.g cough, fever, malaise, shortness of breath. We call these a syndrome
.
- Most infections are treated using a 'syndromic approach' - we don't know the actual cause of infection in the patient, so we need to treat the most common and important causes of the syndrome. This is called "empiric therapy"


Empiric vs Directed Therapy
EMPIRIC THERAPY:
- knowing the most common causes of a clinical syndrome allows appropriate initial (broad spectrum) antibiotic therapy
- inadequate intial antibiotic therapy is associated with treatment failure and death
- however, broad-spectrum antibiotic use causes the emergence of multi-resistant pathogens
.
DIRECTED THERAPY:
- if the specific causative organism is identified in the microbiology laboratory, we can target therapy to treat that organism
- avoid unnecessary antibiotic use (e.g virus)
- optimise therapy for the individual present

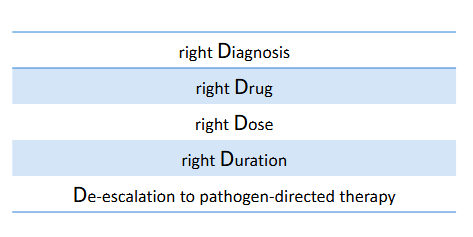
Antimicrobial Stewardship
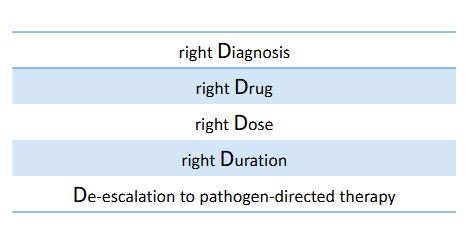
- Antimicrobial stewardship improves and measures the appropriate use of antimicrobials through the 5 D's
- in its broadest sense, stewardship encompasses any activity that promotes the judicious and appropriate use of antimicrobials in human medicine, veterinary medicine and animal agriculture around the globe
- Why is stewardship important? An estimated 700,000 people die of drug-resistant infections each year globally
.
- the last one basically means that if we do lab tests and find out its for isntance strep. we can narrow down the spectrum of antibiotics