Gastrointestinal Tract
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
82 Terms
Gastrointestinal Tract:
a continuous “tube” from the mouth to the anus, along with associated glands (liver, gall bladder, pancreas) needed for digestion
GI tube is divided into:
Upper GI Tract: Oropharynx, Esophagus, Stomach
Lower GI Tract: Intestines, Colon, Rectum
Peristalsis:
Coordinated symmetrical contraction and relaxation of muscles that propagates in a wave down the GI tube
Major GI functions:
Digestion and movement of food
Absorption of nutrients
Elimination of wastes
Mucosal immunity
Basic Structure of the GI Tube:
Mucosa
Submucosa
Muscularis
Serosa
Mucosa:
Inside of the tube Epithelium, Basement Membrane, Lamina Propria (connective tissue, small blood vessels, nerves and lymphatics), thin muscle layer
Submucosa:
Connective tissue, blood vessels, nerves, lymphatics, secretory glands
Muscularis:
2 layers of Smooth Muscle (circular inner layer, lengthwise outer layer)
Serosa:
Outside of the tube
Connective tissue with larger blood vessels, nerves and lymphatics
Regions of the GI tube:
Each organ of the GI Tube is divided into anatomical and functional regions
Esophagus
Stomach
Intestine
Colon
Diseases tend to occur in specific regions of each organ
Esophagus:
Cervical, Upper Thoracic, Mid Thoracic, Lower Thoracic
Stomach:
Cardia, Fundus, Body (Corpus), Antrum, Pylorus
Intestine:
Duodenum, Jejunum, Ileum
Colon:
Cecum, Ascending, Transverse, Descending, Sigmoid, Rectum
Dysphagia:
Difficulty swallowing
Dyspepsia:
Indegestion (upper abdomen discomfort with bloating & gas)
Reflux:
Regurgitation of stomach (gastric) fluids into the esophagus
GERD:
Gastroesophageal reflux disease, can injure the esophagus
Pyrosis:
Burning chest pain (heartburn), can mimic cardiac pain
Hematemesis:
Vomiting up blood
Significant upper GI hemorrhage (ruptured vessel) has fresh (red) blood
Slow bleed causes blood to be degraded by stomach acid, vomit has a “coffee ground” appearance
Melena:
Black tar-like stool caused by an upper GI bleed (need significant
and protracted GI bleed), term is specific for blood causing a dark stool. Many foods and medications can cause a black stool but are not melena
Fecal occult blood test:
Detects blood in stool samples, also called the Stool Guaiac test. Fresh blood (bright red) in the stool indicates a rectal or anal bleed (often hemorrhoids)
Esophagus: Congenital Defects:
Esophageal Atresia
Tracheo-Esophageal Fistula
Esophageal Stenosis
Esophageal Atresia:
Failure to develop and results in a “dead- end” pouch, results in vomiting
Tracheo-Esophageal Fistula:
Abnormal connection between lungs and GI tract, results in either food in the lungs (causes aspiration pneumonia) or bloating due to air in the stomach
Esophageal Stenosis:
Narrowing of the tube, results in Dysphagia (difficulty swallowing)
Acquired/Congenital Defect:
Lower Esophageal Sphincter (LES)
Hiatal Hernia
Lower Esophageal Sphincter (LES):
a thickening of esophageal wall and diaphragm muscles, prevents
stomach contents from entering esophagus. Relaxation of the LES can cause Reflux of gastric fluids. Many substances (alcohol, caffeine, tobacco, certain foods) can relax the normal muscle tone of the LES
Hiatal Hernia:
Defect in the opening of the diaphragm, causes part of the cardia region of stomach to protrude into the thoracic cavity. Can interfere with normal LES function and cause reflux
Esophageal Varices:
Dilation of veins in the distal (lower thoracic) esophagus
Caused by high pressure in the veins due to portal hypertension (caused by liver cirrhosis)
Rupture can cause massive bleeding and death, common cause of death in cirrhosis
Treated by Band Ligation: tie off the vessel with a surgical band
to stop blood flow, causes varices to regress
Esophagitis:
Inflammation of the Esophagus
Causes:
GERD (common cause) and infections (viral and fungal)
Symptoms
Dsyphagia and Pyrosis
GERD:
caused by chronic reflux due to LES dysfunction
Reflux of stomach acid damages and inflames the squamous epithelium of the esophagus, can cause fibrosis and narrowing
Long-term GERD causes metaplasia of the distal (lower thoracic) region from squamous to gastric epithelium: Barrett Esophagus
Esophagitis: Infections:
Often in immunocompromised
Viruses: Herpes, Cytomegalovirus (CMV)
Fungus: Candida albicans
Barrett Esophagus:
Metaplasia of the distal (lower thoracic) region from squamous
to glandular gastric epithelium
Caused by chronic reflux of gastric fluids that damage the
esophagus (GERD)
Chronic GERD can predispose to develop adenocarcinoma of esophagus
Esophageal Carcinoma: Two major types:
Squamous Cell Carcinoma (SCC), Adenocarcinoma (AC)
Both are uncommon cancers in the U.S.
Adenocarcinoma is more common type (> 60%)
Usually found in males >50 years old (4:1 M/F ratio)
Common in China, Iran, Russia, parts of Africa
Squamous Cell Carcinoma is more common globally
Male/Female ratio is almost equal
Symptoms: Dysphagia, weight loss, hematemesis, pain (but symptoms often non-specific and mild)
Risk factors: Diet & Environment
Nitrosamines in food (smoked & pickled foods): SCC
Excessive or long-term alcohol & tobacco use: AC, SCC
Possible environmental/occupational causes: SCC
Long-standing GERD: AC
Diagnosis & Prognosis:
Imaging, Endoscopy with biopsy
No effective treatment. Very poor 5-year survival, but
has improved (from 5% to 20%) by earlier detection 13
Squamous Cell Carcinoma:
Most in mid-upper (75%) part of esophagus (25% in lower)
Uncommon in the U.S.
Develops from squamous epithelium
Associated with diet & environment
Adenocarcinoma:
Found in the lower part of esophagus, near LES
More common in the U.S.
Develops from gastric glands in regions of Barrett esophagus
Associated with long-standing GERD
Stomach Regions:
Cardia
Fundus
Body (Corpus)
Antrum
Pylorus
Cardia:
region below the LES where the stomach begins
Fundus:
upper region that stores gas and undigested food
Body (Corpus):
largest part where the main digestion occurs
Antrum:
largest part where the main digestion occurs
Pylorus:
derived from the Greek word for ”gatekeeper”, it controls movement of food into the duodenum
Stomach Histology: Gastric Mucosa:
Folded into Gastric Pits that contain multiple cell types
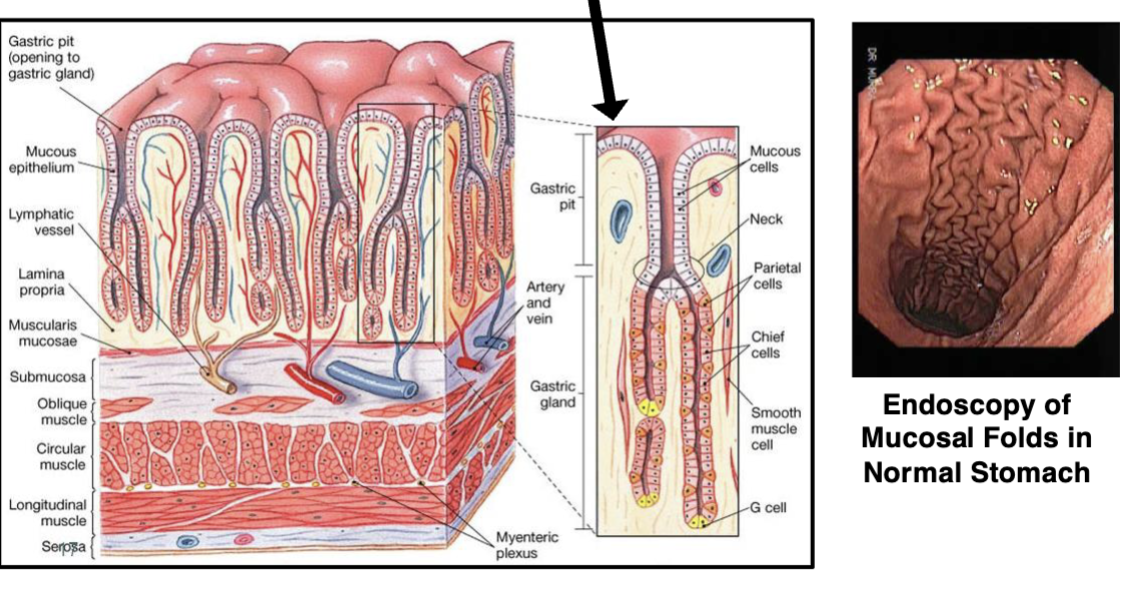
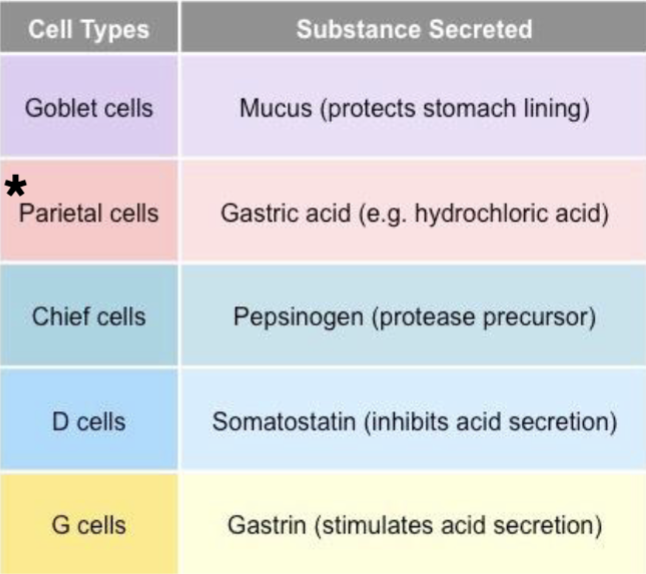
Stomach Cell Types: Parietal Cells:
Also secrete Intrinsic Factor, needed to absorb vitamin B12 (required for RBC production)
Protection of Gastric Mucosa: Required for protection:
Normal, intact blood flow to the stomach
Intact mucus layer and normal mucus production
Normal acid and bicarbonate (neutralizes acid) production
Normal hormone secretion (gastrin and somatostatin)
Protection of Gastric Mucosa: Damage can be caused by:
Infection with Helicobacter pylori
Increased acid production (often caused by certain foods)
Aspirin and other NSAIDs (Ibuprofen, Naproxen, etc.)
Smoking and excessive alcohol use
Ischemia and/or trauma
Acute Gastritis:
Relatively short duration, but can be severe
Usually caused by irritant exposure (high amount alcohol or NSAIDs) or trauma (burns, stroke, injuries)
Often results in pain, vomiting (possibly hematemesis), dyspepsia
Irritants often produce erosions of the mucosa (superficial ulcers)
Trauma often results in stress ulcers (multiple small ulcers)
Both usually self-limiting, resolves after irritant/trauma is removed
Severe acute gastritis can cause significant blood loss
Chronic Gastritis:
Long duration and often produce ulcers
Infection with Helicobacter pylori is the most common cause
Autoimmune Atrophic Gastritis:
destruction of the mucosa results in gastric atrophy. Most often occurs in the elderly, caused by autoantibodies to parietal cells, this can result in Pernicious Anemia:
Decreased intrinsic factor due to death of parietal cells, which leads to decreased vitamin B12 absorption in the gut, results in anemia
Peptic Ulcers:
The “umbrella” term for this chronic condition
Gastric ulcer: peptic ulcer in the stomach (20% of ulcers)
Duodenal ulcer: peptic ulcer in the duodenum (80% of ulcers)
Very common condition that affects about 10% of U.S. population
Most often seen in men over 50 years old
Smoking, alcohol and NSAID use are major risk factors
Helicobacter pylori is associated with >90% of cases (2005 Nobel Prize in Medicine was awarded for discovering this link between infection and ulcers)
H. pylori is a gram-negative bacterium that does not directly damage the mucosa, it alters the gastric mucosa to allow acid to produce an ulcer at infection site
Symptoms will vary depending on location of the ulcer
Gastric ulcers: epigastric pain 0.5 to 1 hour after a meal
Duodenal ulcers: epigastric pain 2 to 4 hours after a meal
Pathology of peptic ulcers:
Round (often solitary) with sharp “punched- out” appearance that can extend deep into submucosa
Peptic ulcers complications:
significant bleeding if ulcer erodes a blood vessel, or peritonitis if ulcer erodes stomach wall (perforation) into peritoneal cavity
Gastric cancer: Adenocarcinoma:
Accounts for 90-95% of all stomach cancers
Uncommon cancer in the U.S., Canada and western Europe, and
incidence is declining
Very common cancer world-wide, particularly in Latin America, China, Japan, Russia
Symptoms are vague: dyspepsia, vomiting, weight loss, pain
Risk factors: Nitrosamines in food, cigarette smoking, chronic H. pylori infection
Diagnosis: Imaging, Endoscopy with biopsy
Prognosis: No effective treatment, very poor 5-year survival
Gastric Cancer: Tumor Pathology:
Several different tumor growth patterns, small tumors may resemble a peptic ulcer:
Fungating tumor: Grows and fills the stomach lumen
Diffuse tumor: Infiltrates the stomach wall and encases it with cancer, producing a rigid, thick “leather bottle” appearance
Tumors often invade into the peritoneal cavity
Intestine:
Largest digestive organ: about 3.5x body length (average length of 22 feet)
Intestine major functions:
Food absorption, Ileum has extensive lymphoid tissue (Peyer’s Patches) that make large amounts of IgA (mucosal immunity)
Enterocytes have a very large surface area for absorption
Intestine Cell Types: Anoikis:
Epithelial enterocytes die by apoptosis, shed into lumen
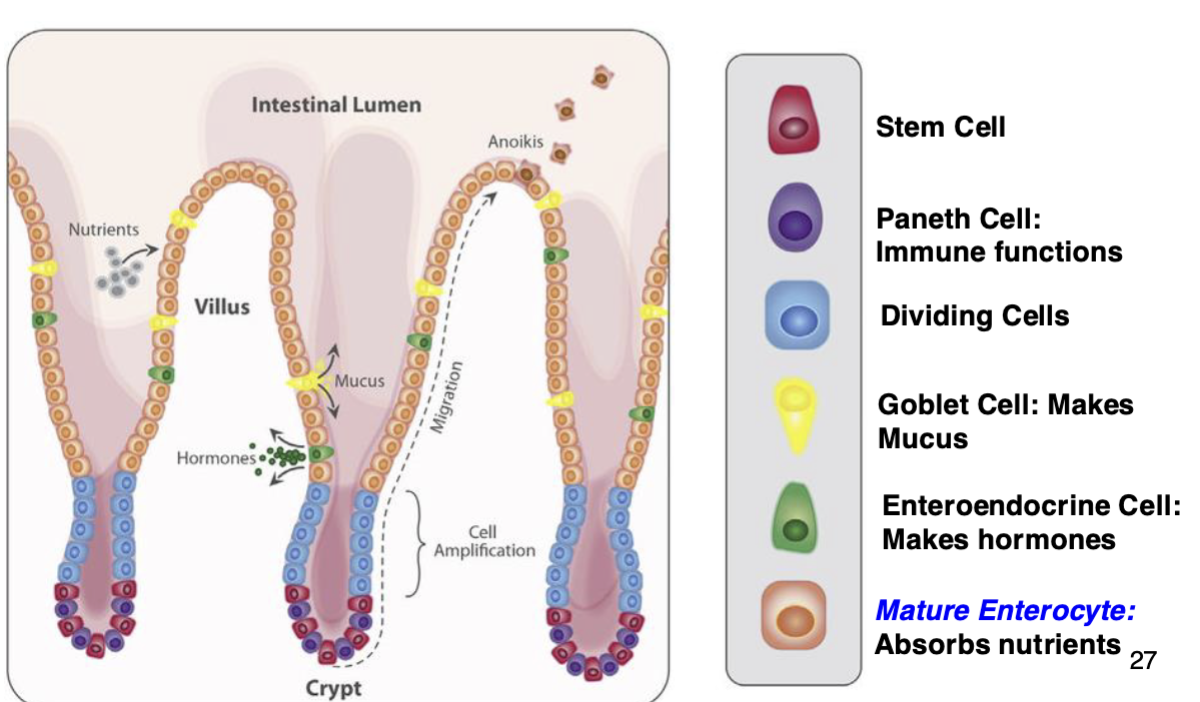
Intestinal Pathology: Tumors:
Very rare, <5% of all GI tumors are intestinal, and most are benign!
Intestinal Pathology: Gastroenteritis:
Infections, usually viral or bacterial, are extremely common and result in cramping, gas and diarrhea. Severe bacterial infections (cholera and salmonella) can be fatal if not treated promptly.
Celiac disease:
Immune reaction against the wheat protein Gliadin.
NOT a classic autoimmune disease (but has some characteristics)
T-cytotoxic cells responding to gliadin kill enterocytes and destroy villi
Most often occurs in the duodenum and jejunum
Results in decreased absorption and malnutrition
Treatment is to avoid gluten!
Intussusception:
A serious medical emergency in which part of the intestine slides into an adjacent part of the intestine/colon. Blocks food or fluid from passing, also can stop the blood supply to that part of the intestine.
Usually affects infants and young children, more often in males
In adults this can be caused by tumors, polyps or scar tissue
Treatment is surgery ASAP!
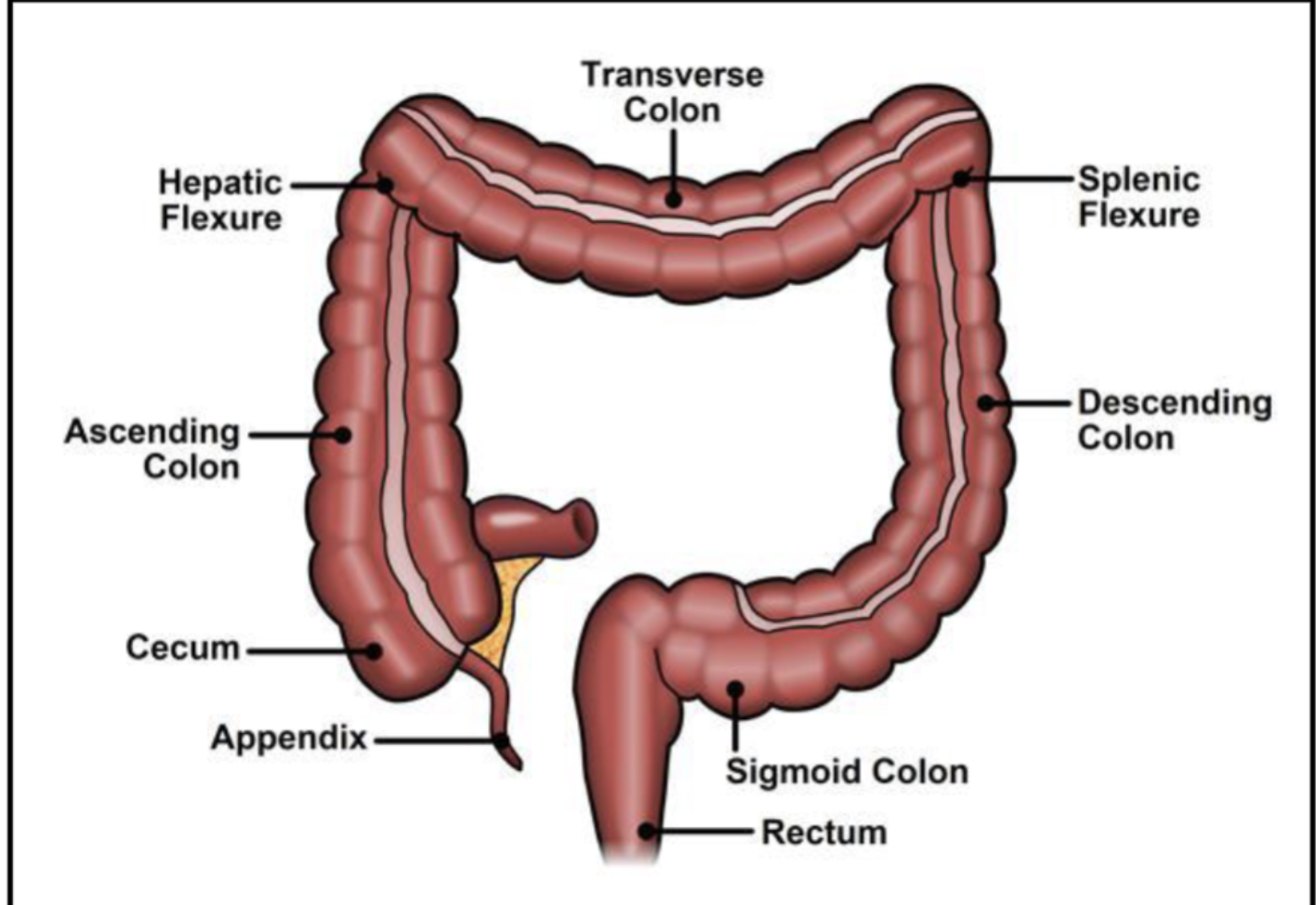
Colon & Rectum
Acute Appendicitis:
Very common, particularly those under 20 years old
Develops from an obstruction, primarily caused by:
Fecalith (hardened stool blocking lumen)
Hyperplasia of lymphoid tissue (Appendix is a lymphoid organ)
Obstruction leads to ischemia and overgrowth of gut bacteria
Classic symptoms: Pain in the right lower quadrant, fever, abdominal tenderness, nausea, leukocytosis (elevated white blood cell count)
Surgical treatment is required since rupture can cause peritonitis
Interval appendectomy: if appendix already ruptured, some people will be treated with antibiotics, followed for several weeks/months, then surgery when inflammation has subsided
Before modern surgery and antibiotics, this was almost always fatal
Inflammatory Bowel Disease (IBD):
Broad category that contains two distinct diseases: Crohn’s Disease (Regional Enteritis) and Ulcerative Colitis
Common features of BOTH Crohn’s Disease and Ulcerative Colitis:
Idiopathic diseases with both genetic and autoimmune components
Chronic relapsing diseases (cycles of remission then relapse)
Affects women more than men
Can affect almost any age from pre-teen to elderly, but peak incidence in people in their 20’s
Both cause intermittent diarrhea, but severity is variable ranging from mild to chronic severe disease
Medical treatment includes steroids, antibiotics and new targeted biologics (anti-cytokine drugs), response to therapy is also variable
NOTE: Don’t confuse IBD with Irritable Bowel Syndrome (IBS), IBS is very common and is defined by symptoms, it does not have the severity or tissue pathology of IBD
Crohn’s Disease (CD):
Also known as Regional Enteritis
Less common than Ulcerative Colitis
Usually presents with more severe symptoms and pathology
About 30% have lesions outside the GI tract (skin, eyes, joints)
Ulcerative Colitis (UC):
3-fold more common than CD
Disease usually starts with relatively mild symptoms
Excessive diarrhea is the classic manifestation of UC
Severe cases have bloody diarrhea, often with abdominal pain and fever
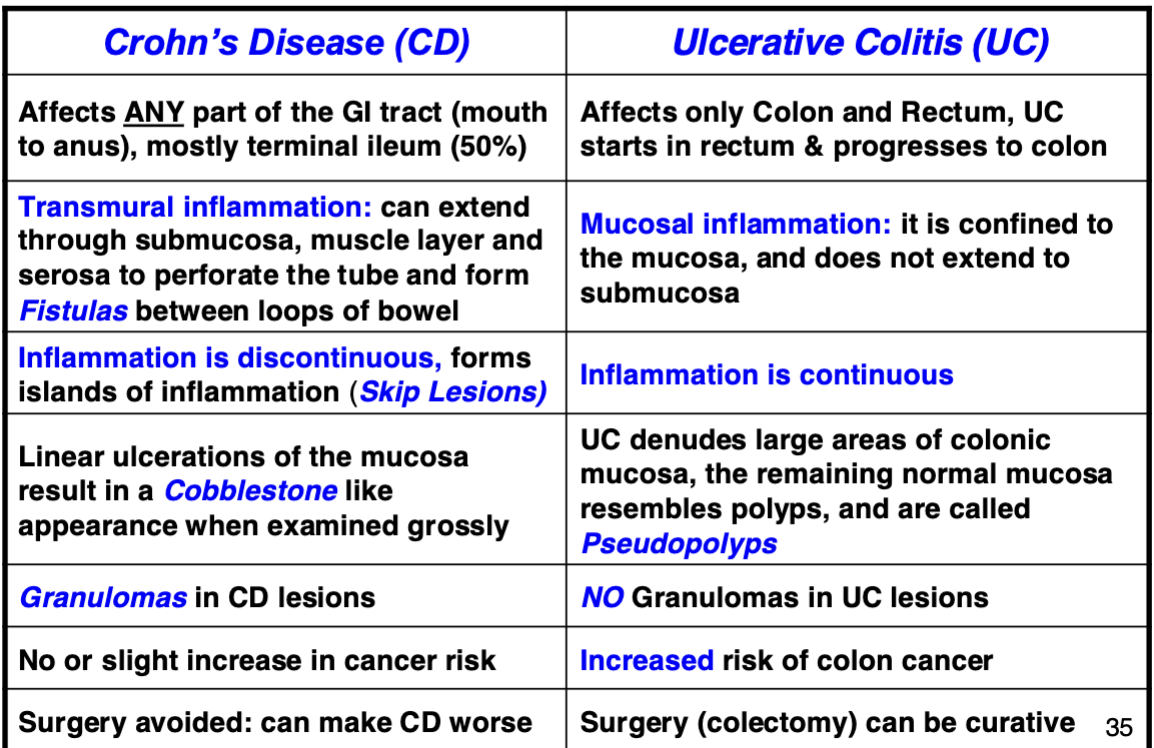
Comparison of CD & UC Pathology
Diverticulosis:
an abnormal outpouching in the wall of the colon
Very common, increases with age: 20% at age 40, >60% at age 60
Thought to be caused by increased pressures in the colon wall (hard dry feces due to diet) and/or weak spots in colon wall
Occur most often in distal colon (descending, sigmoid), can have just one or many diverticula
Diverticulitis:
Inflammation of diverticula, due to obstruction with hard feces. Symptoms are very similar to appendicitis but usually on the left side, Complications include
Rupture → peritonitis
Scarring → stricture and obstruction
Fistulas
Massive bleeding from erosion into a blood vessel
Treatment: Surgical removal if antibiotics fail
Colon Polyps:
Very common, incidence increases with age: 1% at age 25, >50% at age 70
Hyperplastic polyp:
most common non-cancerous polyp, small and flat
Polyps can be Sessile (flat) or Pedunculated (a stalk)
Adenomatous polyp:
most common pre-neoplastic polyp, polyps start as benign growths, but some can transform into cancer.
Nearly all colon cases develop from adenomatous polyps
Tubular Adenoma:
Pedunculated, about 80% of colonic adenomas are benign, but about 10-20% may develop into adenocarcinoma
Villous Adenoma:
Sessile, about 15% of colonic adenomas, but about 50% may develop into adenocarcinoma
Adenocarcinoma of the Colon:
accounts for > 95% of all colon cancers
3rd most common (non-skin) cancer in both men and women in U.S.
2nd leading cause of cancer deaths in both men and women in U.S.
Associated with a diet high in animal fat and low in fiber
Most cases (~65%) occur in distal colon (descending, sigmoid, rectum)
Most cases are diagnosed in older adults (60’s and 70’s)
Lynch Syndrome (Hereditary non-polyposis colorectal cancer) is an inherited early onset form (<1% cases) that develops in 30’s to 40’s
Symptoms are usually vague and non-specific:
1) Changes in bowel habits, constipation (more common) or diarrhea
2) Mild anemia (causes fatigue) due to slow blood loss around the tumor
3) Abdominal pain, can be diffuse or sharp
4) Unexplained weight loss
5) Blood in stool
Colon cancer staging:
based on depth of tumor invasion & number of cancer positive lymph nodes
TNM Cancer Staging: Tumor:
Size of tumor and if it has invaded nearby tissue
TNM Cancer staging: Nodes:
Number of lymph nodes positive for cancer cells
TNM Cancer staging: Metastasis:
Spread of cancer to another part of the body (often the liver)
Endoscopy:
Colonoscopy has helped greatly in the diagnosis and management of diseases of colon: Easier access = more biopsies = diagnosis
Prognosis is good if colon cancers are detected in Stage I or II, and screening colonoscopy has greatly reduced incidence (removal of pre-cancerous polyps) and improved survival by earlier detection