Ch 17 - Chemical Mediators
1/130
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
131 Terms
what dod the observation that factors present in blood could cause a physiological response in lab setting do in the field of pahramacology
catalyzed the growth of the pharmaceutical industry and the quest for biologically active molecules and compounds
factors in the early 1900s were what and how did this change as technology developed
only the simplest substances that were identifies (5-HT, histamine, etc.)
complicated structures were revealed (protaglandins, endothelin)
modern day state of factor identification
though the structure of many meidators have been identified, there are several with yet to be determined role and functions (NO)
hormones
released from a single endocrine gland and circulate in the bloof to affect other target tissues or cells
local hormone
a chemical messenger that conveys information from one cell to another (but can also be carried by blood)
relationshop between hormone and local hormone function
some hormones can act as local hormones, and some local hormones can act systemically
hormones that can act as local hormones example
hydrocortisone
local hormones that can act systemically examples
cytokines, histamine
what type of fatcor are mediators
local hormones are the mediators between a stimulus and a physiological response
mediator describes
local hormone
classes of local hormones
small molecules
peptides and proteins
a mediator must have the following characteristics (similar to Koch’s postulates)
must be produced and released by local cells and initiate a timely biological response at target tissues
administration of the mediator reproduces the same biological response
inhibiting the synthesis, release, or action of mediator attenuates or changes the biological response
histamine what class of mediator
small molecule
histamine was originally identified in ___ as _____
the allergic response the primary mediator of anaphylaxis
histamine chemical properties/class, what it’s derived from, and what enzyme is used to derive it
histamine is a basic amine derived from histidine by histidine decarboxylase
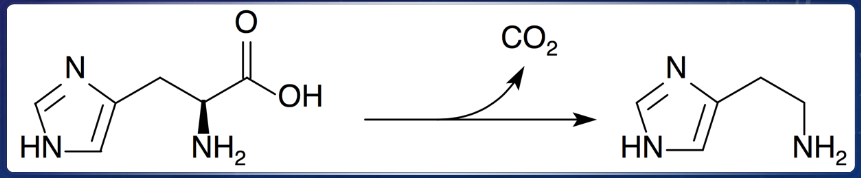
where is most histamine in the body generated
in granules in mast cells, basophils, and eosinophils (WBCs)
histamine distribution in body
present in most tissues but at high []s in tissues exposed to the outside world (lungs, skin, GI tract)
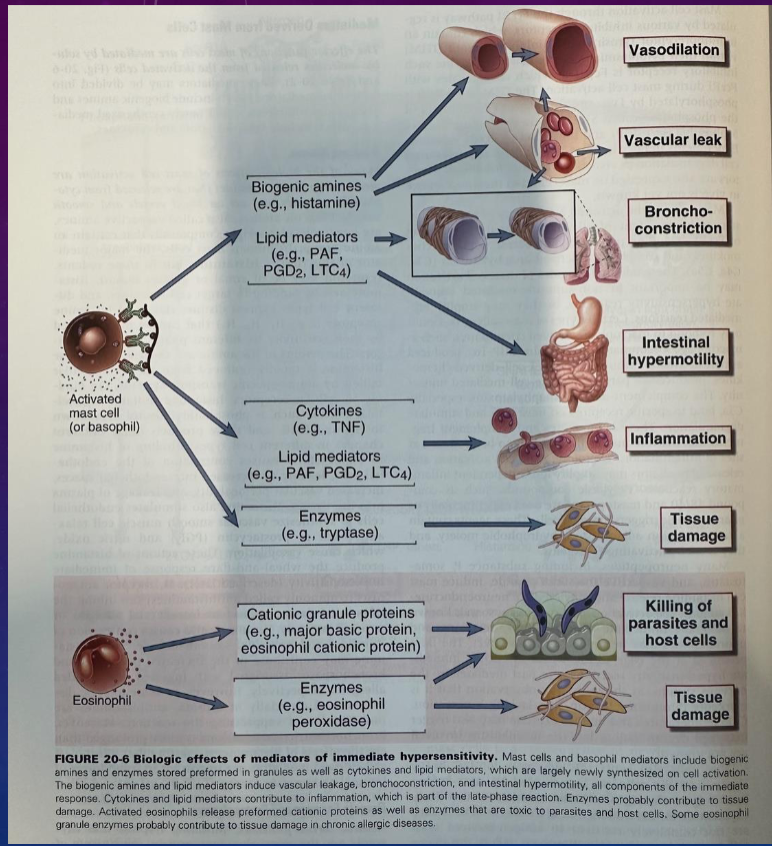
biological effects of mediators of immediate response (other side is my notes okay dont be mad)
biological effects of mediators of immediate response
eosiniphils and mast cells
have cross linking of Ab from ligand that triggers release from cell
release
histamines
lipid mediators
cytokines
other enzymes (not focus in this class)
mediators have diff effects on diff target tissues
lipid mediators and histamine have multiple physiological effects
vasodialation, vascular leaking, bronchoconst, intestinal hypermobility, inflammation
think of allergic reaction
runny eyes and nose related to these mediators, local reaction to certain allergens/irritants
some people
affect breathing
narrows airways, obstructive
histamine release stpes
exposure to an allergen activates the immune system, triggering histamine release
antigen → antigen presenting cell → T-cell activation → B-cell activation → IgE release → mast cell activation → histamine release
how is histamine removed from the body
mainly degraded, occurs mainly through metabolic inactivation by histaminase
what is another wy histamine can be released (non-specific response)
blunt trauma type of way
localized tissue damage can cause histamine release and trigger inflammation
what immunoglobin is associated with allergies and why
IgE is the one associated with allergies
reason is Fc region binds to receptors (Fc epsilon receptors) that are specific to histamine carrying cells
binding activates mast cells and causes histamine release
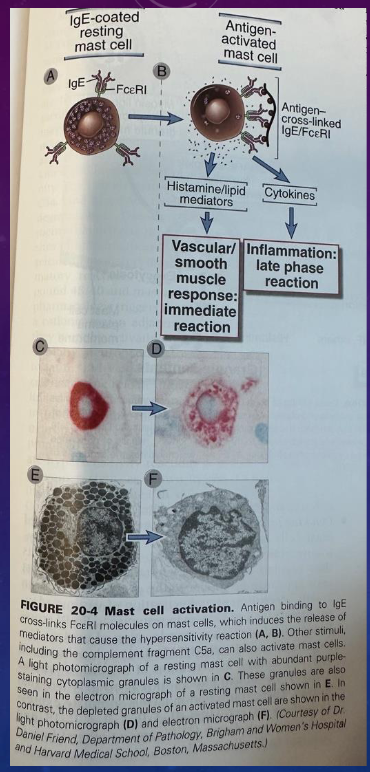
illustrating mast cell activation and histamine release
.
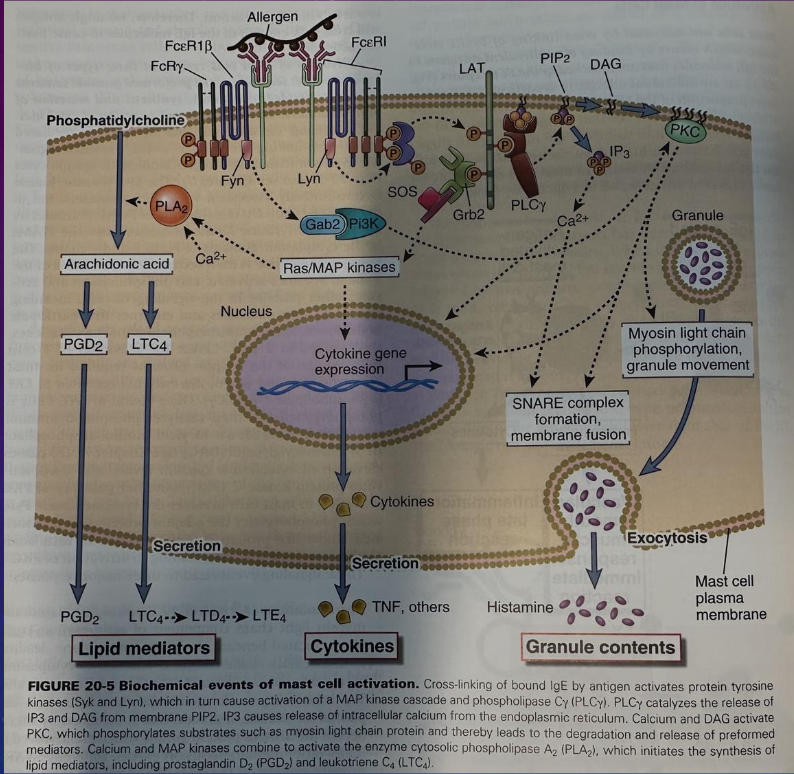
notes again sorry gang
no need to remember all this
know the top and bottom not the middle
a little redundant but shows the internal cellular responses responsible for the release of mediators
binding, crosslinking of receptors, cascade, production of PGD2 (release of lipid mediators), production of cytokines and release of granule contents
cytokines are made in response to the trigger while granule contents are already there but get released
cytokines and lipid mediators are delayed, enzymatic framework is alr there tho, just need to make it
granule contents are more immediate
picture represents a mast cell
histamine receptors are all what type
GPCR
how many histamine receptor homologs and how named
H1 - H4
what do histamine receptors fo
transduce signals though adenylyl cyclase and cAMP in peripheral tissues
actions of each histamine receptor homolog
H1 and H2 generally have stimulatory actions
H3 and H4 have inhibitory actions (however, tissue specific responses for H4 are not well characterized)
main antihistamine drug class and what are they used for
H1 antagonists, principal antihistamines used in the treatment or prevention on inflammation
physiological responses to histamine - H1
SM: contracts in response to H1 activation in bronchi, bronchioles, small intestine, and uterus
cardiovascular system: increases vasodilation, makes post capillary venules more permeable
physiological responses to histamine - H2
heart: increases CO (SV and heart rate)
GI tract: stimulates gastric secretions, especially gastric acid
histamine antagonists (both comp and non-comp are available) are all considered antagonists, but fall into what categories
sedative
non sedative
what is the diff between sedative and non-sedative histamine antagonists
sedative have CNS effects
what do histamine antagonists do
decrease mediated contraction of the smooth muscle of the bronchi, the intestine, and the uterus
apllication of histamine antagonists
not very good as bronchodilators but have clinical applications in anaphylaxis
Fexofenadine - class of drug, clinical uses
H1 blocker (antagonist)
clinical uses: hay fever, rhinities, skin rashes (hives), insect bites
Cimetidine - drug class, clinical uses
H2 blocker
clinical uses: peptic ulcers, reflux oesophagitis → through inhibition of gastric secretion
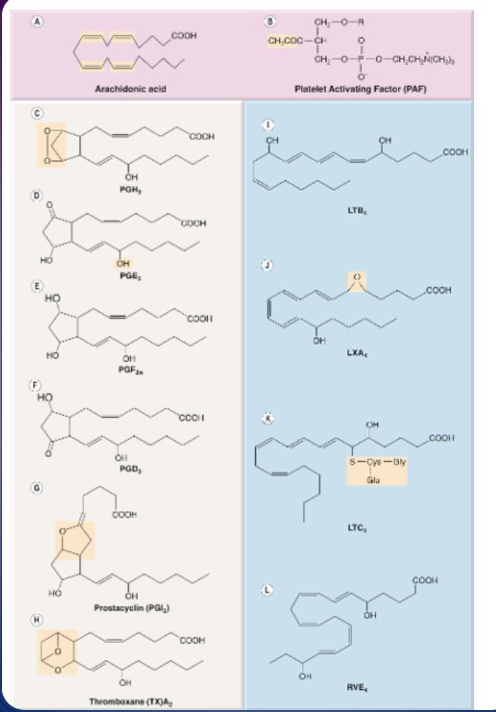
eicosanoid
general term for mediators that are generated from fatty acid precursors as required (ie. not stored for later use)
a precursor for several mediators
arachidonic acid
arachidonic acid is a precursor for
prostanoids
leukotrienes
lipoxins, and resolvins
prostanoids include
prostaglandin and thromboxanes
eicosanoids are synthesized from
arachidonic acid
synthesis pathway for prostaglandins
arachidonate is metabolized by cyclo-oxygenases (COX-1 or COX-2) to prostanoids
synthesis pathway for leukotrienes
5-lipoxygenase converts arachidonate to leukotrienes
eicosonoid synthesis
.
chemical feature of arachidonate that allows for it to be made into so many diff things
have unsaturated carbons (double bonds) which gives opportunity to add smth else
number of mediators
some double bonds can be changed to allow for addition of subsequent moeities to the molecule
“PG” indicates
prostaglandins
PGE_2 is (what it stands for/class of mediator)
a prostanoid, prostaglandin E2
what is PGE2 (functional meaning not what it stands for)
prominent in inflammatory responses and is a mediator of fever and pain
where is PGE2 made
generated by local tissues and blood vessels
what does PGE2 activate
three of the PG receptors
EP_1 receptors
EP_2 receptors
EP_3 receptors
what does activation of EP1 receptors do
contraction of bronchial and GI tract SM
what does activation of EP2 receptors do
relaxation fo bronchial, vascular, and GI tract SM
what does activation of EP3 receptors do
inhibition of gastric acid secretion, increased gastric mucus secretion, contraction of pregnant uterus and GI SM, inhibition of lipolysis and of autonomic NT release
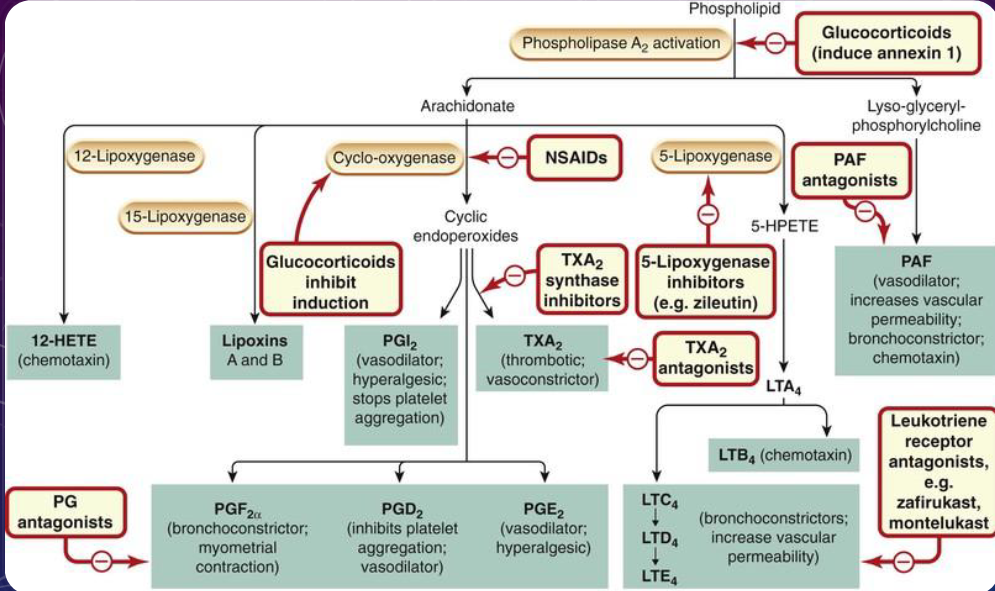
phospholipid inflammatory mediators (notes)
number of pathways and look at what happens when you start to interfere w the pathways
the precursor can be made into a bunch of things
bottom is all the PGs and leukotrienes
made by enzyme pathways
cyclo-oxygenase
can block at diff parts
NSAIDs - inhibit enzyme
other drugs we can use
leukotriene RECEPTOR antagonists - inhibiting reception
she mentioned another but I didnt catch it lowkey I think you need tk all
NSAIDs - stands for what and examples
non-steroidal anti-inflammatory drugs
aspirin, ibuprofen
what do NSAIDs do
inactivate COX enzymes to combat the inflammatory response, arachidonic acid is not metabolized to prostanoids, have side effects
misoprostol
PGE agonist (activates EP2/EP3 receptors)
clinical uses of misoprostol
the pregnant uterus is highly sensitive to misoprostol and will contract in response to threshold levels
early pregnancy - terminates pregnancy
late pregnancy - induces labor (ripens cervix)
post delivery - uterus clamping (stops bleeding)
additional uses
prevents gastirc acid secretion (used in combination with NSAIDs) to prevent NSAID-induced ulcers
LT
leukotrienes
LTs made by what and from what primarily
by WBCs
made from arachidonic acid by 5-lipoxygenase
LT synthesis cascade (from LTA_4)
LTA4 can be further converted to LTB4, LTC4, LTD4, LTE4, and LTF4
what are LTC4-F
cystinyl containing LTs
what does LTB4 do
is an important mediator of chemotaxis and activator of WBCs
CysLT
cysteinyl-containing LTs
CysLT cause
contraction of bronchial muscles and peripheral vasodilation
Montelukast
CysLT receptor agonist used to treat asthma
chemotaxis
chemical mediated movement - WBC drawn to an area where these are present
lipoxin
other small molecule mediator
acts on polymorphonuclear leukocytes to oppose the inflammatory response
also act as a high affinity antagonist to CysLT1 (therefor lipoxin analogues are being studied as antiasthmatics)
PAF
platelet activatig factor
other small molecule mediator
produced by platelets in response to thrombin and by activated immune cells
key mediator between inflammatory response and thrombosis and its additional function
PAF, also intiates the inflammatory response in allergic reactions
small molcecule mediators
histamine
eicosonoids (prostanoids, LTs, lipoxins and resolvins)
peptide and protein mediators length (# residues)
generally vary from three to about 200 aa residues in length (50 aa cut off for peptide to protein)
similarities between peptides and proteins
both udergo post-transcriptional modifications that often affect their biological activity
differences between peptides and proteins
proteins must adopt tertiary or quaternary structures that make them rigid (sterically hindered and functional groups are stabilized) wherease peptides are flexible
peptides and proteins are classificed into 4 categories (broadly) based on
biological activity
peptide and protein mediator classes
NTs and neuroendocrine mediators
hormones from non-neuronal sources
growth factors
immune system mediators
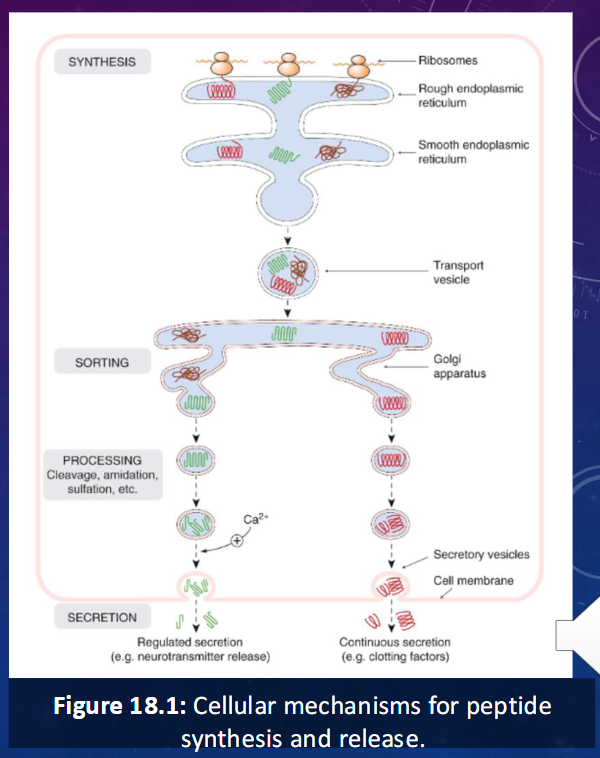
peptide synthesis steps
genes code for peptide structure (generally as a precursor molecule that has the desired peptide embedded)
preprohormone is translated, signal peptide is removed and preprohormone is converted to prohormone
prohormone contains complete hormone sequence plus other peptide sequences
prohormone is transferred to golgi apparatus where it is processed
prohormone is packaged into secretory vesicles
POMC (stands for)
pro-opiomelanocortin
POMC (definition)
a precursor peptide that is cleaved into hormones and peptide mediators
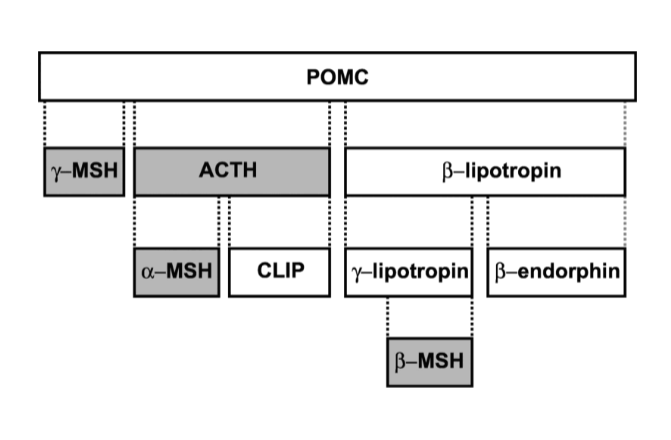
what does POMC give rise to
ACTH, MSH, and \beta-endorphin
ACTH
adrenocorticotrophic hormone
MSH
melanocyte-stimulating hormones
POMC gives rise to many molecules, what is their function
all have specific functions, but also work together in inflammatory response
processes that permit extensive diversity within peptide/protein families
geen splicing and post translational processing of prohormone
how does gene splicign contribute to peptide/protein diversity
a single gene can code for multiple proteins through differential expression of exons and introns, usually through experimental cues that govern differing trasncriptional start sites
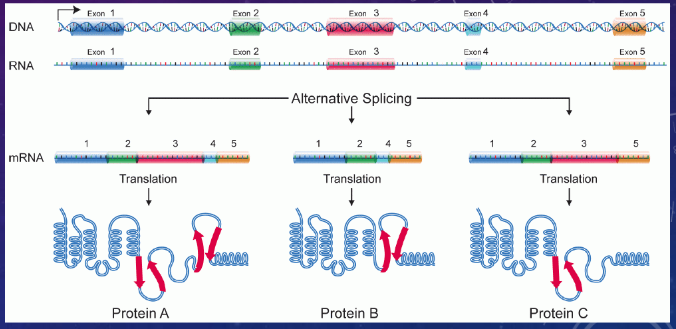
how do post-translational modifications contribute to peptide/protein mediator diversity
include peptides that cleave prohormones at different sites giving rise to similar but distinct peptides - usually tissue specific phenomenon
proteolytic cleavage of kininogens gives rise to
bradykinin and lysyl-bradykinin (kallidin)
bradykinin
a vasodilator and increases vascular permeability, also causes sustained contraction in SM
strong pain producing agent that is potentiated by prostaglandins
types of BK receptors
two main types
constitutively expressed B2
inflammatory response induced B1
icatibant
bradykinin antagonist
peptide analogue of bradykinin
seelctive competitive antagonist for B2 receptors
used to treat acute attacks of hereditary angioedema
B1 and B2 antagonists are known and may be developed for treating
inflammatory disorders
neuropeptides
often co-released during normal physiological responces with non-peptide neurotransmitters
most important neuropeptide
substance P
neurogenic inflammation
arises from the local release of neuropeptides from afferent neurons that affect mast cells (release histamine)
aprepitant
neurokinin NK1 receptor antagonist used to treat emesis
signalling molecules of the inflmmatory response
cytokines
cytokines
protein or polypeptide mediators synthesized and released by cells of the immune system during inflammation (via autocrine or paracrine mechanisms)
cytokines bind to what to do what
bind to specific kinase linked receptors with high affinity and intiate a signal transduction cascade to phosphorylate and activate downstream proteins
receptor expression for cytokines
not usually expressed unless in an inflammatory response