Neuro E2- CN disorders
1/75
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
76 Terms
What CN’s does the sense of smell depend on?
CN 1 and portions of CN V
Qualitative odor sensations are mediated by _____
CN I
Somatosensory overtones (warmth, coolness, sharpness, tingling & irritation) are mediated by ____
ophthalmic & maxillary divisions of CN V
What is the absent sense of smell?
anosmia
What is an abnormally intense smell?
hyperosmia
What is the hallucination of fecal odor known as?
Cacosmia
Which is more common- primary disorders of CN I or secondary dysfunction of CN I?
secondary
Where is there a high concentration of photoreceptors (rods/cones)?
fovea
Describe the pupillary pathway
light impulse travels up optic nerve → divides at chasm → arrive at pretectal nucleus → efferent signals sent via CN III → direct & consensual constriction
What does a sudden onset of blindness imply?
vascular event
What does a slow evolution of visual complaints imply?
inflammatory or neoplastic disease
What do transient or recurrent visual symptoms imply?
ischemia, embolic, MS, or myasthenia gravis
What is the inability to maintain conjugate gaze?
diplopia
What u/l loss of vision that resolves w/in ~20 minutes due to decreased blood flow to the retina (likely from embolism)?
transient monocular vision loss (TMVL)
What else is TMVL known as?
amaurosis fugax, optic neuritis, giant cell arteritis
What condition would a patient experience gray-black curtain that gradually descends in one eye, or blurring/fogging/dimming of vision?
TMVL
What do patients with TMVL also need to be evaluated for?
TIA/stroke
What is inflammation of the optic nerve that causes u/l vision loss, scotomata on visual field testing, & pupils that are slow to react?
optic neuritis
What is the treatment for optic neuritis?
steroids
What is inflammation of the external carotid artery at the superficial temporal artery that can extend to the ophthalmic artery, leading to blindness?
giant cell / temporal arteritis
What patients would likely hav optic neuritis?
MS patients aged 15-50
Who is giant cell arteritis MC in?
> 50 y/o (mean age is 70)
What condition?
pain over scalp at temporal artery w/ dec pulse or nodules
jaw pain/stiffness when chewing
pale optic disc
elevated ESR > 50 mm/hr
dx w/ temporal artery bx
Giant cell arteritis
What is the treatment for giant cell/temporal arteritis?
urgent prednisone burst to avoid vision loss, slowly taper over several months
What condition?
afferent pupillary defect & defective sensory system
pupils dilate instead of constricting with direct light
consensual reflex present (both eyes dilate)
disease oof retina or optic nerve
Marcus gunn pupil
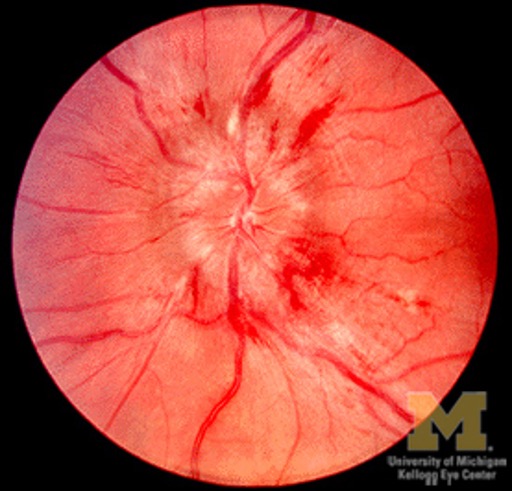
What condition?
sign of increased ICP
usually b/l (binocular vision disorder)
HA, N/V, other neuro dysfunction
urgent search for cause (HTN emergency, mass, etc)
Papilledema
What is the MC pituitary tumor?
prolactinoma
What condition?
tumor press on optic chiasm → gradual bitemporal hemianopsia
other sx: HA, galactorrhea, amenorrhea, acromegaly
Dx: MRI & prolactin levels
pituitary tumor
What is the treatment for pituitary tumors?
surgical excision & bromocriptine
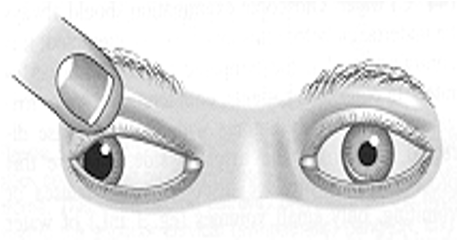
Which condition is diplopia, ptosis, dilation of pupil, & fixed position of eye downward and outward?
CN III palsy
What should all patients with new-onset CN III palsy with pupillary involvement be presumed to have until proven otherwise with expeditious MRA?
cerebral artery aneurysm (emergency if HA present)
In what patients is pupil-sparing CN III palsy most common in?
older patients (>50) due to diabetes related vascular infarction (or HTN)
What is the workup for pupil-sparing CN III palsy?
MRI & neuro referral to r/o aneurysm; usually resolves w/in 3 mos
What is unequal pupil sizes?
anisocoria
identifying abnormal pupil in aniscocoria
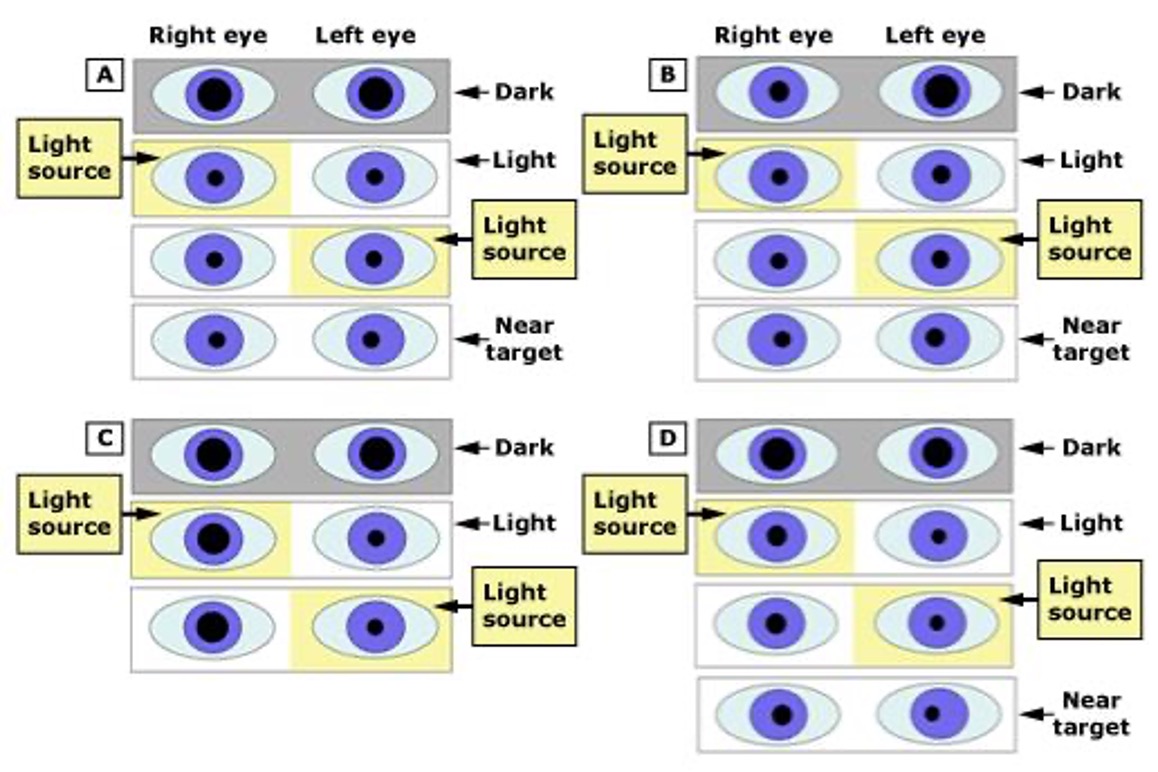
What condition is the interruption of cervical sympathetic nerves to the eye that causes ptosis, miosis, & anhidrosis on the involved side of face (also dilation lag or delayed eyelid elevation)?
Horner’s syndrome
How do you confirm the diagnosis of Horner’s syndrome?
Cocaine drop test / topical cocaine test
How does the cocaine drop test (topical cocaine test) work?
blocks reuptake of NE at sympathetic nerve synapse → causes pupillary dilation in eyes w/ intact innervation to increase degree of anisocoria(no effect in eyes w/ impaired innervation)
positive = anisocoria ≥ 0.8 mm
What all can be done for the workup of Horner’s syndrome?
cocaine test, CT/MRI, angiography (think lung tumor or carotid artery aneurysm)
Ptosis of the eyelid on the side of the small pupil indicates what condition?
horner’s syndrome
Ptosis of the eyelid on the side of the large pupil indicates what condition?
CN III palsy
What condition?
pupil accommodates to near vision but does NOT react to light directly or consensually
assoc w/ CNS syphillis, etc
argyll-robertson pupil
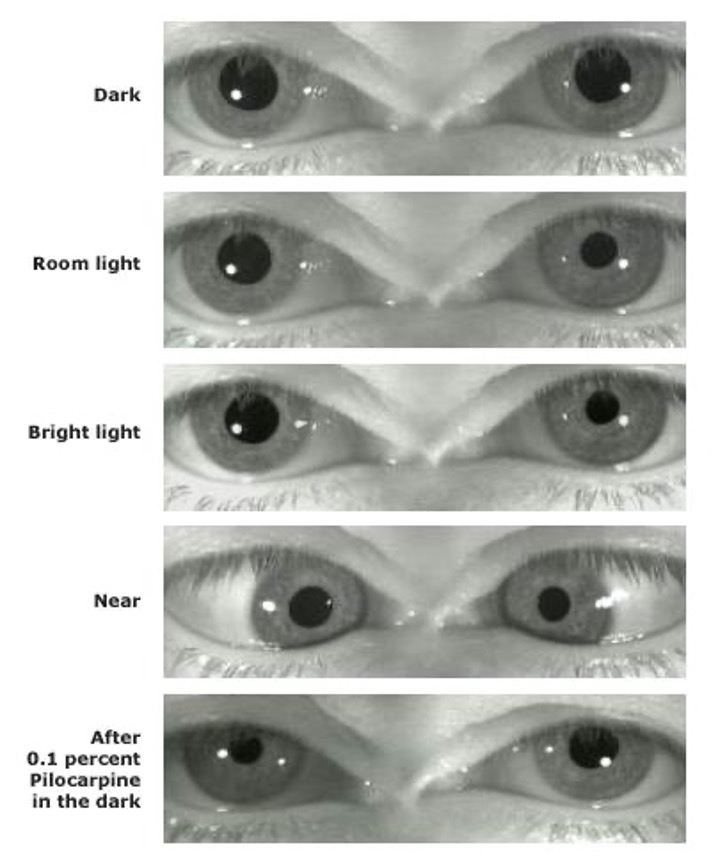
What condition is a tonic pupil with parasympathetic denervation that constricts poorly to light but reacts better to accommodation?
Adie’s pupil
What condition?
anisocoria more in dark (small pupil abnormal)
dilation lag, ptosis
cocaine test → small pupil does not dilate
Horner’s Syndrome
What condition?
anisocoria more in dark (small pupil abnormal)
cocaine test → both pupils dilate symmetrically
Physiologic anisocoria
What condition?
anisocoria more in light (large pupil abnormal)
sluggish to light, light near dissociation, isolated
0.1% Pilocarpine → large pupil constricts
Adie’s tonic pupil
What condition?
anisocoria more in light (large pupil abnormal)
ptosis / ophthalmoplegia
CN III palsy
What condition?
anisocoria more in light (large pupil abnormal)
sluggish to light, light near dissociation, isolated
0.1% pilocarpine → large pupil does not constrict
pharmacologic anisocoria
What is the MCC of vertical diplopia?
CN IV palsy
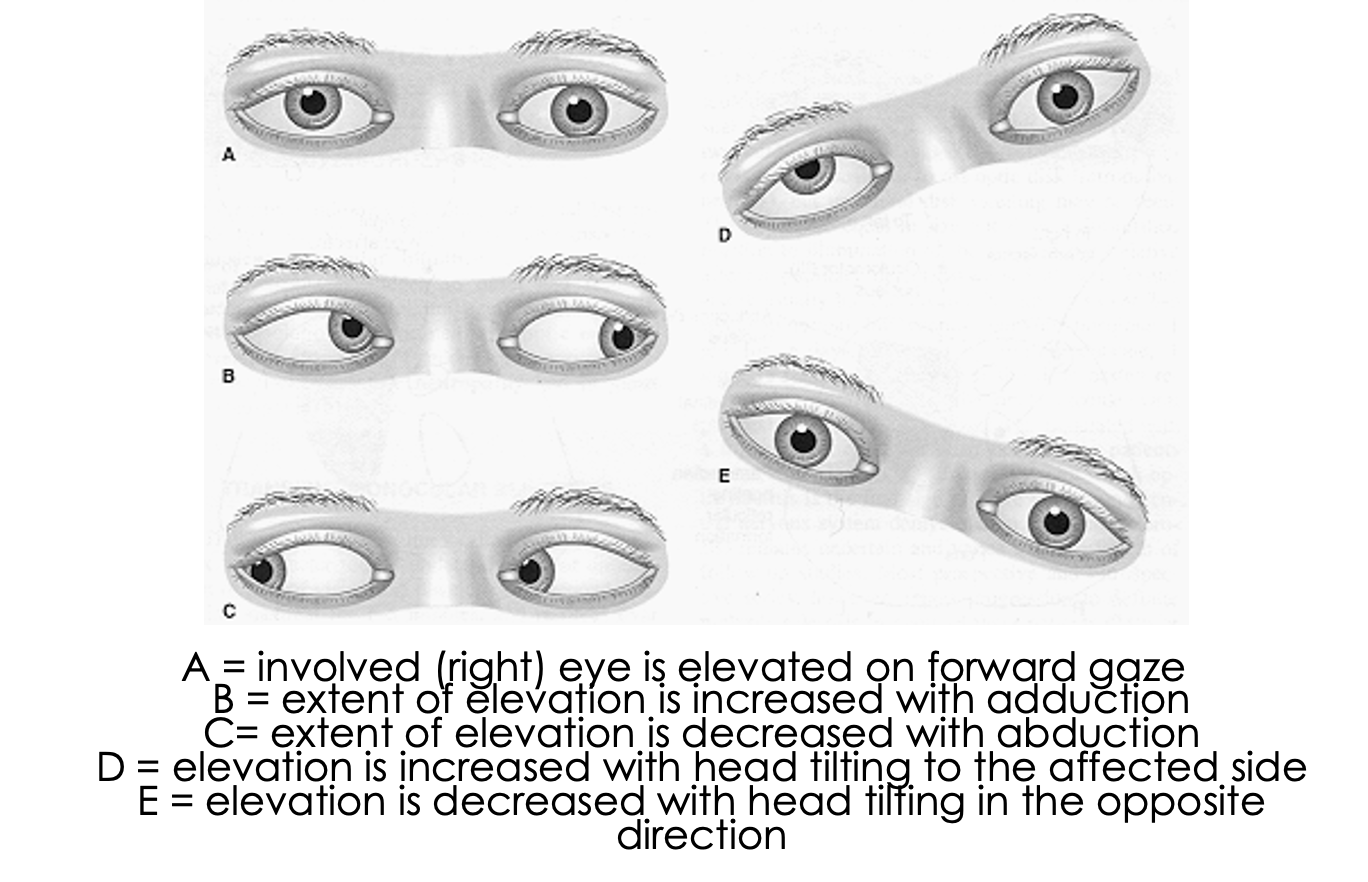
What condition?
(vertical) diplopia
eye deviates upward and slightly medially
MCC- blunt head trauma (other- microvascular infarct d/t DM, neoplasms, inflammation, infx)
CN IV palsy
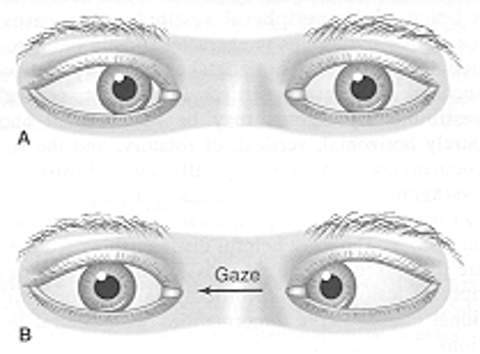
What condition?
affected eye adducted at rest & cannot abduct
MCCs: basal intracranial neoplasms, trauma, microvascular dz
CN VI palsy
What is bilateral CN VI palsy a sign of?
increased ICP (get urgent head CT)
What in the MCC of unilateral CN VI palsy in elderly?
microvascular infarction second to DM
What is a more common cause of CN VI palsy in children & young adults?
tumor
What is another name for trigeminal neuralgia?
Tic Douloureux
What condition?
microvascular compression of sensory fibers of trigeminal root by a blood vessel (usually superior cerebellar artery)
lancinating pain in distribution of 1+ branches of CN V (lower 2/3 of face)
very painful sharp electric spasms lasting s-mins, usually around eye, cheek, lower face
can be triggered by touch, draft of air, or sounds & pain occurs while brushing teeth/chewing, drinking, eating, shaving
Trigeminal neuralgia
What are treatment options of trigeminal neuralgia?
usually spontaneous recovery; can tx w/ carbamazepine, phenytoin, baclofen, gabapentin
What is another name for idiopathic facial nerve palsy?
Bell’s palsy
What condition?
possibly d/t reactivation of HSV
u/l facial paresis, prodromal aural pain, numbness in affected region, auditory hyperacusis, impaired taste on anterior 2/3 of tongue
sx divello over 1-3 days
Idiopathic facial nerve palsy
What is the treatment for Bell’s palsy?
complete spontaneous recover in most
prednisone burst & taper; acyclovir
no improvement & complete paralysis → ENT referral
What does facial paralysis with spared forehead muscles indicate?
central lesion (storke in one cerebral hemisphere)
What condition?
HSV re-eruption along CN VII
prodrome of pain, facial weakness, vesicular rash (in ear), dec hearing on affected side, N, loss of balance
MRI & NCV → inflammation & damage to CN VII
Ramsay-hunt syndrome
What is the treatment for Ramsey hunt syndrome?
antivirals (acyclovir), steroids, & pain control
What kind of hearing loss?
affects external auditory canal or middle ear
weber lateralize to side of lesion
rinne: BC>AC on side of lesion
conductive hearing loss
What kind of hearing loss?
lesions affecting inner ear or CN VIII
weber materializes away from lesion
rinne: AC > BC (both decreased) on side of lesion
sensorineural hearing loss
A diminished gag reflex & disturbed swallowing indicates what palsy?
CN IX
Asymmetric rise of uvula indicates what palsy?
CN X
Flaccid paralysis of tongue w/ atrophy & speech difficulties indicates what palsy?
CN XII
In a patient s/p stroke affecting the left CN IX, which direction would the uvula be deviated?
towards the right (the normal/strong side bc this side of the palate is pulled up higher)
In right CN XII dysfunction, which way will the tongue deviate?
towards the right (the paralyzed side because of weakened genioglossus muscle)
What is the MCC of injury to spinal accessory nerve?
medical procedures involving head and neck
What would injury to CN XI cause?
drooping shoulder, muscle atrophy, weak/limited elevation of arm/shoulder, shoulder pain and scapula (shoulder blade) winging
What medications can cause taste loss?
ACE inhibitors
What nerve is affected if there is altered sense of taste with somatosensory sensations (hot peppers)?
CN V
When would taste be lost on anterior 2/3 of tongue?
bell’s palsy
When would taste be loss on posterior 1/3 tongue?
CN IX dysfunction